Short Article, Int J Cardiovasc Res Vol: 9 Issue: 8
A Rare Case of a Giant Primary Cardiac Angiosarcoma Revealed by Superior Vena Cava Syndrome and Right Heart Failure
Zeine El Abasse*, Rime Benmalek, Nassour Brahim and Choukrani Hanane
Department of Cardiology, Hospital University Center Ibn Rochd, Casablanca, Morocco
*Corresponding Author: Dr. Zeine El Abasse Department of Cardiology, Hospital University Center Ibn Rochd, Casablanca, Morocco Tel: 0627781863 E-mail: 0627781863
Received: October 23, 2020 Accepted: December 01, 2020 Published: December 08, 2020
Citation: Abasse ZE, Benmalek R, Brahim N, Hanane C (2020) A Rare Case of a Giant Primary Cardiac Angiosarcoma Revealed by Superior Vena Cava Syndrome and Right Heart Failure. Int J Cardiovasc Res 9:8.. doi: 10.37532/icrj.2020.9(8).427
Abstract
Primary cardiac tumors are very rare with an incidence ranging from 0.0017% to 0.003% according to surgery and autopsy reports [1]. Among them, only 25% are malignant and nearly 75% are sarcoma and around 40% are angiosarcomas [2]. Sarcomas are often metastatic and have a poor prognosis even after surgical removal with an average mean survival of 6 months [3].
Keywords: cardiac tumors
Introduction
Primary cardiac tumors are very rare with an incidence ranging from 0.0017% to 0.003% according to surgery and autopsy reports [1]. Among them, only 25% are malignant and nearly 75% are sarcoma and around 40% are angiosarcomas [2]. Sarcomas are often metastatic and have a poor prognosis even after surgical removal with an average mean survival of 6 months [3].
Case Report
We report the case of a 35 years-old female with no known medical history, who presented to the emergency department with severe exertional dyspnea associated with dry cough, asthenia, anorexia, dizziness and facial swelling that started 2 months ago. Physical examination found a normotensive patient (blood pressure at 120/70 mmHg) with tachycardia (heart rate at 115/min), with moderate bilateral lower limb edema, a distended jugular vein and mild dilatation of superficial neck and facial veins associated to upper chest and face swelling evoking a Superior Vena Cava (SVC) syndrome (Figure 1a) as well as shifting dullness and hepatomegaly. 12-leads Electrocardiogram (ECG) showed diffuse low voltage. Transthoracic Echocardiography (TEE) revealed a giant rounded irregular mass (82x94 mm) in the right atrium occupying the entire atrial chamber resulting in tricuspid orifice obstruction (mean gradient= 13 mmHg), in addition to a significant pericardial effusion with a Right Ventricule (RV) diastolic collapse (Figure 1 b.c.d). Chest and abdominal Computed Tomography (CT) scan revealed an hypodense right atrial mass of irregular morphology and confirmed its extrinsic compression of the tricuspid valve and the RV in addition to an occlusion of the SVC with the presence of collateral circulation to the azygos system. Moreover, pulmonary nodules compatible with metastasis, hepatomegaly and significant polyserositis (pericardial, peritoneal and pleural effusions) were found. Biopsy of the cardiac mass was performed and came positive for primary cardiac angiosarcoma. The patient was candidate for surgical resection but unfortunately, she died because of massive pulmonary embolism and aggravation of her tamponade that was reluctant to several attempts of pericardiocentesis.
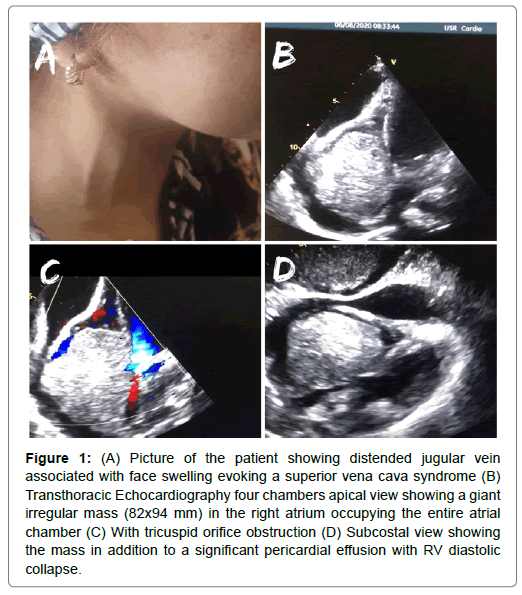
Figure 1: (A) Picture of the patient showing distended jugular vein associated with face swelling evoking a superior vena cava syndrome (B) Transthoracic Echocardiography four chambers apical view showing a giant irregular mass (82x94 mm) in the right atrium occupying the entire atrial chamber (C) With tricuspid orifice obstruction (D) Subcostal view showing the mass in addition to a significant pericardial effusion with RV diastolic collapse.
Discussion
Primary malignant cardiac tumors are extremely rare, angiosarcoma is the most commonly seen histological subtype and is known by its destructive nature. Right-sided sarcomas are usually more infiltrative with early metastasize but present with congestive heart failure until late stage of the disease [4]. They can cause obstructive and systemic symptoms, arrhythmias, pericardial effusion and systemic embolization [5,6]. The diagnosis approach is based on TTE, CT, magnetic resonance imaging, histopathology and immunohistochemistry.
The prognosis of this tumor is poor especially in young patients [4] such ours, with a mean survival of 3.8 ± 2.5 months without surgical resection [3,7]. Survival up to 3 years has been reported in a few cases [8,9], and was correlated to the location of the tumor (left-heart location had better prognosis) and early complete surgical resection, which was confirmed by the Mayo clinic serie where a better median survival in the event of R0 resection than R1 resection was found, thus showing the importance of wide resection in these patients [10].
Treatment guidelines for this pathology are not yet established since most of the literature on cardiac angiosarcomas is based on clinical cases or single-institution studies, however given the tumor’s high fatality rate, an aggressive approach using a combination of surgery, chemotherapy, radiation, and/or transplantation showed survival improvement in these patients [11]. Since Right-sided sarcomas are more infiltrative, some authors recommended the use of neoadjuvant chemotherapy to reduce tumor size before total surgical resection, by reporting a median survival time of 27 months, with 1 exceptional case of a patient still alive 9.5 years after surgery [12]. According to a more recent study, the use of doxorubicin/ifosfamide before surgery was associated to an improved median survival to 15.5 months for right-sided tumors and 20 months for the the left-sided ones [13]. Moreover, the adjunction of radiation therapy has led to reports of survival up to 3 years [14]. Therefore, a multidisciplinary approach including neoadjuvant chemotherapy, radiation and radical surgical resection will give patients with primary cardiac angiosarcoma the best chance of survival.
References
- Cook RJ, Ashton RW, Aughenbaugh GL, Ryu JH (2005) Septic pulmonary embolism: presenting features and clinical course of 14 patients. Chest. 128:162-166.
- Goswami U, Brenes JA, Punjabi GV, LeClaire MM, Williams DN, et al. (2014) Associations and outcomes of septic pulmonary embolism. Open Respir Med J. 8:28-33
- Liu S, Xie J, Chen Y, Yang J, Zhang J, et al. (2014) Presenting features and clinical course of 34 patients with septic pulmonary embolism caused by right-sided infective endocarditis. Chin Med J (Engl). 127:2735-2739.
- Huang RM, Naidich DP, Lubat E, Schinella R, Garay SM, et al. (1989) Septic pulmonary emboli: CT-radiographic correlation. AJR Am J Roentgenol. 153:41-45
- Iwasaki Y, Nagata K, Nakanishi M, Harada H, Kubota Y, et al. (2001) Spiral CT findings in septic pulmonary emboli. Eur J Radiol. 37:190-194.
- Lee SJ, Cha SI, Kim CH, Park JY, Jung TH, et al. (2007) Septic pulmonary embolism in Korea: microbiology, clinicoradiologic features, and treatment outcome. J Infect. 54:230-234.
- Ali A, Raza S, Khan R, Bechard D, Kaszala K, et al. (2012) Septic pulmonary embolism in a patient with defibrillator lead endocarditis. Am J Respir Crit Care Med. 185:e2.
- Habib G, Lancelotti P, Antunes MJ, Bongiorni MJ, Casalta JP, et al. (2015) 2015 ESC Guidelines for the management of infective endocarditis: The task force for the management of infective endocarditis of the European Society of Cardiology (ESC) endorsed by: European Association for Cardio-Thoracic Surgery (EACTS), the European Association of Nuclear Medicine (EANM). European Heart Journal. 36:3075-3128.
- Song XY, Li S, Cao J, Xu K, Huang H, et al. (2016) Cardiac septic pulmonary embolism: A retrospective analysis of 20 cases in a Chinese population, Medicine (Baltimore). 95: e3846.
- Aslam AF, Aslam AK, Thakur AC, Vasavada BC, Khan IA, et al. (2005) Staphylococcus aureus infective endocarditis and septic pulmonary embolism after septic abortion. Int J Cardiol. 105:233-235.
- Davis KA, Huang G, Petty SA, Tan WA, Malaver D, et al. (2020) The Effect of preexisting anticoagulation on cerebrovascular events in left-sided infective endocarditis. Am J Med. 133:360-369.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi