Research Article, Int J Cardiovasc Res Vol: 8 Issue: 6
Assessment of Left Ventricular Diastolic Function and Left Atrial Deformation in Normotensive Type 2 Diabetes without Microvascular Complications
Wafaa S El-Sherbeny* and Suzan B Elhefnawy
Department of Cardiology, Faculty of Medicine, Tanta University, Egypt
*Corresponding Author: Wafaa S. El-Sherbeny
Department of Cardiology, Faculty of Medicine, Tanta University, Egypt
E-mail: wfelsherbeny@gmail.com
Received: November 07, 2019 Accepted: December 02, 2019 Published: December 09, 2019
Citation: El-Sherbeny W, Elhefnawy SB (2019) Assessment of Left Ventricular Diastolic Function and Left Atrial Deformation in Normotensive Type 2 Diabetes without Microvascular Complications. Int J Cardiovasc Res 8:6.
Abstract
Introduction: The goal of the investigation is to estimate left ventricular (LV) diastolic function in normotensive type II diabetes mellitus patient without microvascular complications and by using 2D-speckle tracking echocardiography (STE) for early discovery of LA dysfunction in those individuals. A total of 40 cases suffering from type 2 DM (group I) and 40 normal healthy individuals with sex and age matched were involved as the control group (group II). 2D-echocardiography, Doppler and tissue Doppler imaging were measured to evaluate LV diastolic function, measurement of peak atrial longitudinal strain (PALS) using 2D-STE
Results: The present work confirmed that E/A ratio was significantly lowered in case group compared with control group, there were a significantly decrease in the case group than the healthy control individuals in both the average early diastolic velocity (Em) of the septal mitral valve annulus (Septal E`) and lateral mitral valve annulus (lateral E`). The ratio (E/E`) by TDI was elevated significantly (P=0.001) in diabetic patients versus control group (15.92 ± 3.01 m/sec in the case group and 8.95 ± 0.99 m/sec in the healthy group). global PALS was dropped significantly (p=0.001)in diabetic patients in comparison with control group, diabetic peoples with duration of 11 to 15 years had more incidence of diastolic dysfunction(DD) with increasing the grade of DD. Patients with HbA1c ≥ 7.5% had more prevalence of DD with increasing the grade of DD than patients with HbA1c<7.5% (p=0.014).
Conclusion: Diastolic function was impaired in diabetic patients despite absence of CAD and other features of CAD. The grade of DD increase with increased level of HbA1c and duration of diabetes, impaired left atrial function in normotensive diabetic patients with preserved LV systolic function may be prone to develop microvascular complication
Keywords: Diabetes mellitus; Diastolic dysfunction; Left atrial strain; Speckle tracking
Abbreviations
LV: Left Ventricle; LA: Left Atrium; STE: Speckle Tracking Echocardiography; LVEF: Left Ventricular Ejection Fraction; PALS: Peak Atrial Longitudinal Strain; PACS: Peak Atrial Contraction Strain; DD: Diastolic Dysfunction; CAD: Coronary Artery Disease; ROI: Region of Interest; ACR: Albumin Creatinine Ratio; LVEDV: Left Ventricular End Diastolic Volume; LVESV: Left Ventricular End Systolic Volume; DT: Deceleration Time; IVRT: Isovolumetric Relaxation Time; TDI: Tissue Doppler Imaging; LVDD: Left Ventricular Diastolic Dysfunction.
Introduction
Diabetes mellitus prevalence is rising all over the world, there by becoming an increasingly powerful threat to global health, where they prospected that by the year 2025 more than 5% of the world population will be affected by diabetic disease (The World Health Organization projects) [1].
Both the American College of Cardiology and the American Heart Association established that since diabetes is of great importance to the advance of heart dysfunction thus it has been considered as one of the main risk factors for inducing cardiac dysfunction [2].
Several reports found that the frequency of heart failure with preserved left ventricular ejection fraction in diabetic subjects is elevated even in non-hypertensive and coronary artery disorder [3]. The incidence of left ventricular (LV) diastolic dysfunction (DD) in asymptomatic diabetic subjects was averaged 20-75%. This wide range variation connected with nominated patient and the used diagnostic tool for diagnosis of diastolic dysfunction such as the echocardiographic markers [4-6].
It is assumed that a first impediment in type II DM is diastolic dysfunction (DD), which considered the initial stage in the development of diabetic heart disease. Deficiencies in both systolic and diastolic utility, even in the absence of hypertension, LV hypertrophy and CAD, is the main characteristics of diabetic cardiomyopathy [7].
One of the important markers for the severity of DD is the rise in left atrial (LA) volume with/or without LV filling pressures, many investigations proposed that the level of higher LV filling pressures may not entirely clarify LA failure and that LA myocardial fibrosis and remodelling which responsible for LA dysfunction in patients with HFpEF [8–12]. The main characteristics of using of two-dimensional (2D) speckle tracking echocardiography(STE) represented in a quantitative estimation of the longitudinal myocardial LA anomalies and provide additional information for early detection of LA dysfunction in inpatients with DM [13-15] thus mediating the cardiovascular risk in these subjects.
The goal of this investigation is to define whether there is any linked among type II DM and diastolic failure, even in the nonsymptomatic patients, early discovery of LA failure in such subjects by STE.
Subjects and Methods
Study population
The present investigation was a prospective study. Eighty subjects with variable ages, sex group will enrol in this study. They were divided as 40 cases are suffering from diabetes mellitus type 2 (group I) and forty normal subjects with nearly the same age and sex were included as the control group (group II).
Patients with Type II DM>3 years duration with normal left ventricular ejection fraction (LVEF: ≥ 50%), presence of therapeutic treatment for DM. All the subjects had normal electrocardiogram, negative exercise test, free of angina symptoms.
The study was conducted during the period from July 2015 to April 2016. Written informed consent was taken from each patient. The study was approved by the ethical committee of Faculty of Medicine, Tanta University.
Exclusion criteria
The following groups of patients were excluded: Patient with previous myocardial infarction, coronary artery disease, LV systolic dysfunction, Non sinus rhythm, previous stroke, Hypertensive patients, valvular heart disease, patients with microvascular complications such as neuropathy, retinopathy, or nephropathy and those with albumin-to-creatinine ratio of >0.25 in spot urine.
Methods
All individuals were subjected to the following: Proper history taking, proper general and local examination, resting standard 12 lead surface electrocardiogram (ECG), exercise test (Treadmill test or dobutamine echo), laboratory investigation, transthoracic echocardiographic examination include Conventional 2D-echocardiography, 2D-Speckle tracking echocardiography, Doppler and tissue Doppler imaging (TDI).
Transthoracic echocardiographic examination: All subjects were examined in the left lateral decubitus position, using a system a vivid 9 with a 2.5-MHz multifrequency transducer. Electrocardiograms were recorded simultaneously. Based on American Society of Echocardiography, measurements were performed
Two-dimensional transthoracic echocardiography: Within this technique, calculation by Simpson’s method of the left ventricular ejection fraction (systolic function) with the use of apical 4-chamber view; and LVEF ≥ 50% was considered as normal.
Pulsed-Wave Doppler (PWD): A pulsed-wave Doppler (PWD)- derived transmitral inflow velocity was obtained in the apical 4-chamber view, where the volume sample was placed at the mitral valve leaflet tips. Measurements included the transmitral early diastolic rapid filling (E-wave) and atrial contraction late filling (A-wave) velocities to calculate E/A ratio, isovolumteric relaxation time (IVRT) and deceleration time (DT) [16]
Tissue Doppler Imaging (TDI): This was performed by activating TDI function in the same machine. The ECG was recorded. TDI was performed with 2 mm sample volume placed at lateral side and septal side of mitral annulus from apical 4-chamber view.
The lateral and septal late diastolic (A`) and early diastolic (E`) velocities were measured E/E` was calculated as E/ e’ ratio correlates with LV filling pressure [16].
Measurement of LA longitudinal strain: LA speckle tracking longitudinal strain measured using conventional 2D grey scale echocardiography [17–19]. during breath hold, three consecutive heart cycles were recorded. The frame rate was set between 60 and 80 frames per second. Recordings were processed using acoustictracking software (Echo Pac; GE). GE), allowing off-line semiautomated analysis of speckle-based strain. LA endocardial border was first traced manually at end systole and subsequently the software automatically delineated this region of interest (ROI) into six segments in both four- and two-chamber views, the ROI adjusted manually to include the whole LA myocardial thickness, automated segmental tracking quality was assessed. In patients in whom some segments were excluded because of the impossibility of achieving adequate tracking. Peak atrial longitudinal strain (PALS), measured at the end of the reservoir phase were calculated by averaging the values observed in all accepted LA segments (global PALS) in fourand two-chamber views [17–19].
Laboratotry investigation
A-Glycosylated hemoglobin (Hb A1C): the goal for people with diabetes is a hemoglobin A1C less than 7%. The higher the hemoglobin A1C, the higher the risks of developing complications related to diabetes.
B-Microalbumin-to-creatinine ratio: The urine albumin test or microalbumin/creatinine ratio (ACR) is used to screen people with chronic condition such as diabetes and hypertension, both of them have risk of developing chronic kidney disease.
Statistical analysis
Statistical presentation and analysis of the present study was conducted, using the mean, standard deviation and chi-square test by SPSS V.20.
Results
Forty patients with type 2 DM more than 3 years (group I) (case group) (LVEF ≥ 50%) with a mean age 54.8 ± 7.3 years, 22 men (55%) and 18 women (45%) and 40 healthy subjects (group II) (control group), with a mean of (50.98 ± 4.61) years. 23 males (57.5%) and 17 females (42.5%).
Echocardiographic data
Left ventricular end diastolic volume (LVEDV) was averaged (78.35 ± 19.01 ml), P=0.171 in the case group, in comparison with control group (74.1 ± 4.1 ml).
The mean of left ventricular end systolic volume (LVESV) in the case group was ( 34.38 ± 8.1 ml) and in the control group was (31.63 ± 4.69 ml), P value=0.067.
The mean ejection fraction (EF%) in the case group was (57.01 ± 5.38%) and in the control group was (57.48 ± 4.99%) With regarding to EF%, the results revealed to non-significant variation among the two groups.
LV diastolic parameters
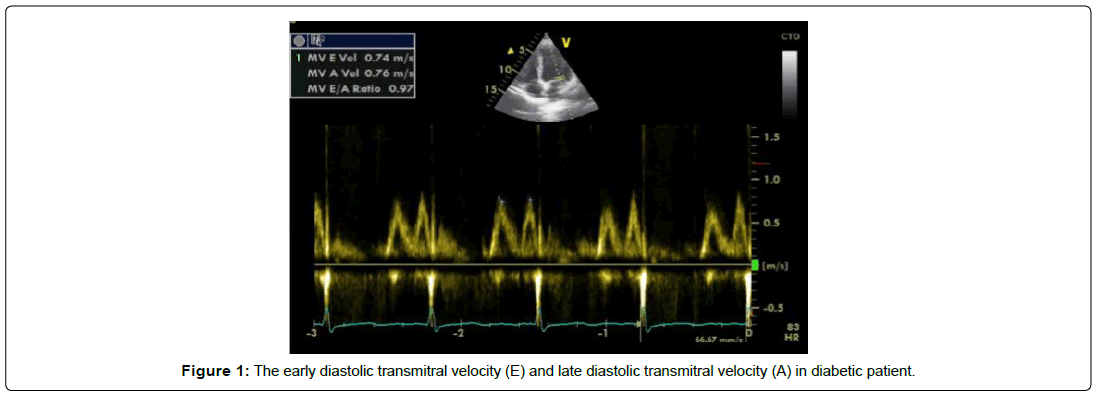
Most of diabetic patients had different grades of diastolic dysfunction: The mean mitral valve peak E wave velocity was lower significantly in the case group compared to control group (P value=0.000). No significant differences between both groups as regard the mean mitral valve peak A wave velocity (P value=0.687).
Concerning the (E/A ratio) high significant differences (P=0.000) among the two groups was recorded. As seen in Table 1 and Figure 1.
| DM | Control | t test | p value | ||
|---|---|---|---|---|---|
| E Wave (m/s) | Range | 0.5–1.32 | 0.56–1.14 | 59.377 | 0.000 |
| Mean ± SD | 0.62 ± 0.13 | 0.87 ± 0.15 | |||
| A Wave (m/s) | Range | 0.56 – 0.92 | 0.45 – 0.95 | 0.163 | 0.687 |
| Mean ± SD | 0.71 ± 0.08 | 0.70 ± 0.12 | |||
| E/A (cm/sec) | Range | 0.65 – 1.8 | 1.19 – 1.42 | 89.251 | 0.000 |
| Mean ± SD | 0.89 ± 0.23 | 1.24 ± 0.05 | |||
| DT (m/sec) | Range | 122–210 | 128 – 190 | 7.405 | 0.008 |
| Mean ± SD | 173.95 ± 23.37 | 158.36 ± 27.69 | |||
| IVRT (m/sec) | Range | 41–210 | 76–105 | 3.998 | 0.012 |
| Mean ± SD | 89.81 ± 29.86 | 102.16 ± 6.29 | |||
Table 1: Comparison between two groups regarding to pulsed wave Doppler parameters.
In addition, there was a significant variation between the case and the control group as regard IVRT and DT Table 1.
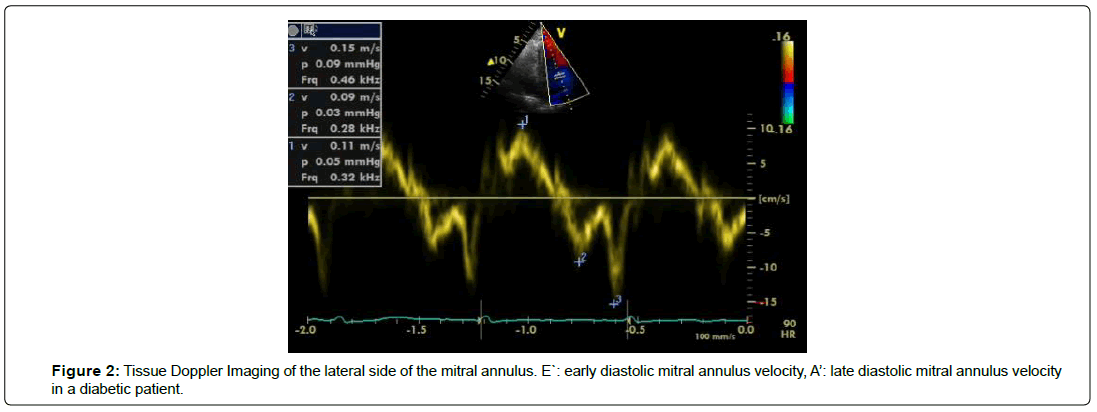
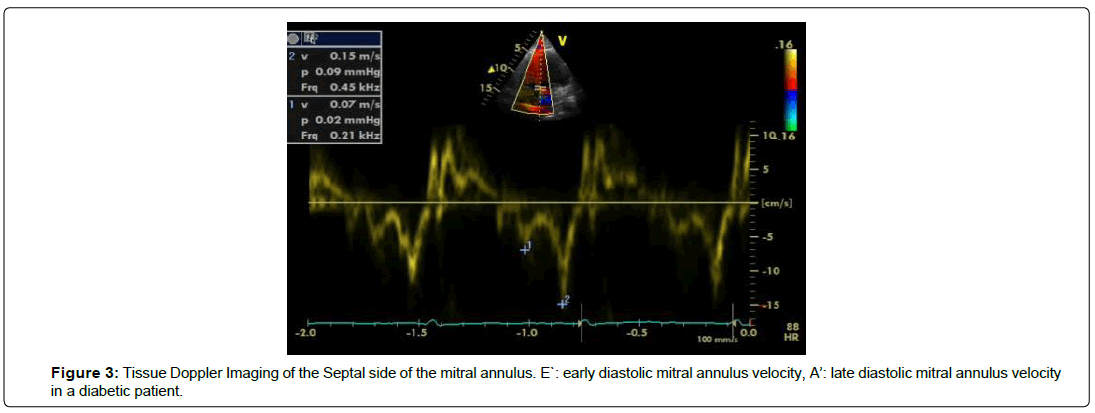
Lower E` velocity at either septal or lateral side of mitral annulus in the case group compared to controls. The values pointed to a highly significant variations (p=0.001) among the two groups. There was no significant variation among the case and the control groups as regard A` velocity ( p=0.638). The mean E/E` ratio by TDI was 15.92 ± 3.01 m/sec in the case group and 8.95 ± 0.99 m/ sec in the control group, with a significant difference (p=0.001) was recorded among the two studied groups as demonstrated in Table 2 and Figures 2 and 3.
| DM | Control | t test | p value | |||
|---|---|---|---|---|---|---|
| Septal | E`velocity (m/sec) | Range | 0.2 – 0.8 | 0.6 – 0.17 | 21.488 | 0.001 |
| Mean ± SD | 0.039 ± 0.012 | 0.098 ± 0.022 | ||||
| A` velocity (m/sec) | Range | 0.04 – 0.15 | 0.05 – 0.15 | 0.223 | 0.638 | |
| Mean ± SD | 0.94 ± 0.026 | 0.92 ± 0.021 | ||||
| E/E` ratio | Range | 9.5 – 21.3 | 6.5 – 10.6 | 19.269 | 0.001 | |
| Mean ± SD | 15.92 ± 3.01 | 8.95 ± 0.99 | ||||
| Lateral | E` velocity (m/sec) | Range | 0.3 – 0.9 | 0.7 – 0.17 | 19.507 | 0.001 |
| Mean ± SD | 0.051 ± 0.012 | 0.106 ± 0.022 | ||||
| A` velocity (m/sec) | Range | 0.03 – 0.14 | 0.04 – 0.14 | 0.252 | 0.617 | |
| Mean ± SD | 0.084 ± 0.024 | 0.086 ± 0.021 | ||||
| E/E` ratio | Range | 9.5 – 21.3 | 5.8 – 9.7 | 15.894 | 0.001 | |
| Mean ± SD | 12.69 ± 2.64 | 8.25 ± 0.89 | ||||
Table 2: Comparison between both groups regarding tissue Doppler imaging parameters.
Relationship between grades of diastolic dysfunction and HbA1c: Patients with HbA1c ≥ 7.5% had more prevalence of diastolic dysfunction with increasing the grade of diastolic dysfunction than subjects with HbA1c<7.5%, where the data pointed to a significant difference (P=0.014) between the two studied groups, as seen in Table 3.
| Variables | Diastolic dysfunction Absent |
Impaired (or abnormal) relaxation(grade 1 diastolic dysfunction) | Pseudo normal pattern(grade 2 diastolic dysfunction) | Total percentage from patient (%) | p value |
|---|---|---|---|---|---|
| HBA1c (< 7.5%) (n=28) |
(18) 64.3% | (7) 25% | (3) 10.7% | 70% | 0.014 |
| HBA1c ( ≥ 7.5%) (n=12) |
(2) 16.7% | (5) 41.6% | (5) 41.7% | 30% | |
| Duration of diabetes mellitus 6-10 years (n=24) |
(16) 66.7 | (6) 25% | (2) 8.3 | 60% | 0.027 |
| Duration of diabetes mellitus 11-15 years (n=16) |
(4) 25% | (7)43.8% | (5) 31.2% | 40% |
Table 3: Relationship between grades of diastolic dysfunction and HbA1c & duration of diabetes mellitus.
Relationship between grades of diastolic dysfunction and duration of diabetes mellitus: Matching persistence of diabetes for a period of 6-10 years or from 11 to 15 years with diastolic failure, subjects with 11 to 15 years duration of diabetes showing high incidence of diastolic failure with increasing the grade of diastolic failure. There was a statistically significant difference (p=0.027) between two groups Table 3.
Left atrium longitudinal strain measurements
The mean four and two chamber PALS were lower in case group compared to control group, with high significant variations (p=0.001) among the two groups, as well as global PALS strain was (18.12 ± 4.50) in case group and (23.57 ± 4.06) in control group with significantly difference (p=0.001) between two groups (Table 4).
| DM | control | t test | p value | ||
|---|---|---|---|---|---|
| PALS 4 chamber | Range | 10 – 27 | 13 – 30 | 3.338 | 0.001* |
| Mean ± SD | 19.94 ± 5.0 | 23.63 ± 4.90 | |||
| PALS 2 chamber | Range | 10 – 25 | 13.5 – 28.5 | 3.766 | 0.001* |
| Mean ± SD | 18.20 ± 4.16 | 21.67 ± 4.07 | |||
| PALS global % | Range | 10.4 – 25.5 | 14.9 – 28 | 5.684 | 0.001* |
| Mean ± SD | 18.12 ± 4.50 | 23.57 ± 4.06 | |||
Table 4: Comparison between diabetic and control group as regard peak atrial longitudinal strain.
Discussion
Several investigators have established that the frequency of heart dysfunction in diabetic individuals is rise even in patients not suffering from coronary artery disease and hypertension. Some authors showed that patients suffering from DM demonstrating a high incidence of pre-clinical diastolic failure [3].
In the current work, diastolic function was inspected by TDI and transmitral left ventricular diastolic filling patterns.
The advantages of TDI than conventional PW Doppler methods in being higher in sensitivity for discovery of left ventricular failure, in addition to its capability for determination of myocardial tissue velocities in the longitudinal direction, and the peak early diastolic myocardial velocity (E′) replicates the global left ventricular diastolic function [20].
The goal of the current work is to assess left ventricular diastolic function in normotensive patients complaining from diabetes mellitus type II without microvascular complications, and early estimation of LA failure in diabetic individuals.
Diastolic dysfunction
The present study demonstrated that MVE velocity and (E/A ratio) were dropped significantly in case group than control subjects with (P=0.000).
The IVRT showing significant difference between case and control groups. The mean DT was showing significant difference (P=0.008) among the case and control groups.
These results were concordant with results obtained by Mishra et al. [21] and results obtained by Ernande et al. [22] who enrolled and compared diabetes mellitus (DM) type 2 patients with organized blood pressure and without overt heart disease with 88 age-matched controls, reported that the (E/A ratio) in the diseased group was significant inferior (p<0.001) as matched with control subjects. The mean IVRT was differed significantly among the patient’s groups.
The results of the present study were concordant with results obtained by Dikshit et al. [23] who reported that an initial marker of diabetic cardiomyopathy is the higher incidence of diastolic failure in diabetic patients.
The present study demonstrated that septal and lateral early diastolic mitral annulus E` velocity was a significant lower (p=0.001) in case group matched with control group.
The mean transmitral to early diastolic velocity ratio (E/E`) was demonstrating a high significant difference between the case and control group which reflect elevated LV filling pressure.
These results were consistent with numerous studies in asymptomatic diabetic patients which showed high prevalence of LV DD [23,24].
The obtained data from the current work were concordant with results obtained by Ofstad et al. [25] who studied T2DM patients not exhibiting clinical symptoms of heart dysfunction and 100 non-diabetic controls matched for age, found that the mean (E/E`) ratio was lower in control group, while it recorded a higher value in diabetic patients which considered as an indication for increasing LV filling pressure in diabetic group.
The obtained finding from the current work also concordant with results obtained by Suran et al. [26] who studied normotensive middleaged T1DM patients not showing a history of heart dysfunction or coronary artery illness, and compared to 48 healthy controls.
Relationship between grades of diastolic dysfunction and duration of diabetes mellitus
The present study demonstrates that diabetic patients suffering for a period of 11 - 15 years had high incidence of diastolic failure with increasing the score of diastolic failure. The significant relationship among the duration of DM and the sternness of DD in this group of patients speculated that the etiology of DD must be the DM., LV DD consider to be early first stage of diabetic cardiomyopathy.
This result was concordant with result obtained by from [4] found that a duration of diabetes ≥ 4 years was unconventionally accompanying with LV diastolic failure (E/e>15) with probabilities ratio 1.91.
The study of Masugata et al. [27] reported that there was an association among the duration of diabetes and E/A ratio in type 2 diabetic subjects and demonstrated a significant negative correlation (r=-0.62, p<0.001). Which are in the same line of our results.
This study found that the higher level of glycosylated hemoglobin the more prevalence of DD in case group which was consistent with result obtained by Sharavanan et al. [28].
Left atrium strain measurement
This study found that global PALS were reduced significantly in diabetic group compared to control group. The impairment of LA function in diabetic patients due to subendocardial fibrosis that affect left atrium lead to reduction of left atrial longitudinal systolic strain, same finding of previous study [8,15].
These results were consistent with the results of Santos et al. [11] who used two-dimensional speckle tracking echocardiography for evaluating pump function, outlet and LA reservoir in HFpEF patients in sinus rhythm and healthy controls individuals and found that failure in all stage of LA function, and systolic LA strain was diminished independent of history of AF or LA size. LA failure may be a marker of sternness and play a pathophysiological role in HFpEF.
The results of the present study were concordant with results obtained by Georgievska-Ismail et al. [29] who enrolled 218 patients with HFPEF, depending on the presence of diabetes mellitus divided into two groups (with or without). The study found PALS and PACS were lower significantly in diabetic patients and its diminished values were liked significantly with the sternness of diabetes.
In the study of Mendillo et al. [30] demonstrated that impairment of LA deformation in patient with high blood pressure and/or diabetes with normal LA dimension and proposed that early abnormalities in LA strain may come first variations in traditional 2D measures of LA function, the findings of the current investigation are in coordination with that results, in our study, we showed that a decrease in global PALS in patient suffering from DM, where it significantly liked with reduced diastolic function.
Limitations
In the current work, we tried to exclude ischemia and coronary artery illness by non-invasive symptom-limited routine implementation test and wall motion valuation by transthoracic echocardiography. In spite of the subjects had treadmill exercise and wall motion test and normal resting ECG, the applied tools do not exclude the presence of atherosclerosis. Coronary angiography in asymptomatic patients was not done due to ethical reasons Hypertension was left out with clinical follow-up; ambulatory blood pressure recordings were not offered due to financial complications. The study was applied to a small number of participants, who were fine categorized, moderately controlled type 2 diabetes patients without any clinical symptoms revealed to the presence of major and/or minor diabetic problems. All the assessments were done only once for the control and the patients groups; though, the valuation of the results was estimated accurately assessment of LA function by 2DSTE is rapid and easy, but difficulty to obtained ROI particularly in the area of auricle and outlet of pulmonary veins leads to incorrect measurements.
Conclusion
Diastolic function was impaired in diabetic patients despite absence of CAD and other features of CAD, The grade of DD increase with increased level of HbA1c and duration of diabetes, impaired left atrial deformation mechanics assessed by 2DSTE in normotensive diabetic patients with preserved LV systolic function may be prone to developed microvascular complication.
References
- Fisman EZ, Tenenbaum A (2008) Cardiovascular Diabetology: Clinical, Metabolic and Inflammatory Facets. Adv Cardiol 45: 82–106.
- Hunt SA, Baker DW, Chin MH, Cinquegrani MP, Feldman AM, et al. (2001) ACC/AHA guidelines for the evaluation and management of chronic heart failure in the adult. Circulation 104(24): 2996-3007.
- Kazik A, Wilczek K, Poloñski L (2010) Management of diastolic heart failure. Cardiol J 17: 558-565.
- From AM, Scott CG, Chen HH (2010) The development of heart failure in patients with diabetes mellitus and pre-clinical diastolic dysfunction a population-based study. J Am Coll Cardiol 55: 300–305.
- Galderisi M (2006) Diastolic dysfunction and diabetic cardiomyopathy: evaluation by Doppler echocardiography. J Am Coll Cardiol 48: 1548–1551.
- Kiencke S, Handschin R, von Dahlen R, Muser J, Brunner‐LaRocca HP, et al. (2010) Pre-clinical diabetic cardiomyopathy: prevalence, screening, and outcome. Eur J Heart Fail 12: 951–957.
- Boudina S, Abel ED (2007) Diabetic cardiomyopathy revisited. Circulation 115: 3213-3223.
- Morris DA, Gailani M, Vaz Perez A, Blaschke F, Dietz R, et al. (2011) Left atrial systolic and diastolic dysfunction in heart failure with normal left ventricular ejection fraction. J Am Soc Echocardiogr 24: 651–662.
- Blume GG, Christopher J, Mcleod CJ, Seward JB, Pellikka PA, et al. (2011) Left atrial function: physiology, assessment, and clinical implications. Eur J Echocardiogr 12: 421–430.
- Rosca M, Lancellotti P, Popescu BA, Piérard LA (2011) Left atrial function: pathophysiology, echocardiographic assessment, and clinical applications. Heart 97: 1982–1989.
- Santos AB, Kraigher-Krainer E, Gupta DK, Claggett B, Zile MR, et al. (2014) Impaired left atrial function in heart failure with preserved ejection fraction. Eur J Heart Fail 16: 1096–1103.
- Kadappu K, Boyd A, Eshoo S, Haluska B, Yeo AET, et al. (2012) Changes in left atrial volume in diabetes mellitus: more than diastolic dysfunction? Eur Heart J Cardiovasc Imaging 13: 1016– 1023.
- Morris DA, Takeuchi M, Krisper M, Köhncke C, Bekfani T, et al. (2015) Normal values and clinical relevance of left atrial myocardial function analysed by speckle-tracking echocardiography: multicenter study. Eur Heart J Cardiovasc Imaging 16: 364–372.
- Mondillo S, Cameli M, Caputo ML, Lisi M, Palmerini E, et al. (2011) Early detection of left atrial strain abnormalities by speckle-tracking in hypertensive and diabetic patients with normal left atrial size. J Am SocEchocardiogr 24: 898–908.
- Muranaka A, Yuda S, Tsuchihashi K, Hashimoto A, Nakata T, et al. (2009) Quantitative assessment of left ventricular and left atrial functions by strain rate imaging in diabetic patients with and without hypertension, Echocardiography 26:262-271.
- Nagueh SF, Appleton CP, Gillebert TC, Marino PN, Oh JK, et al. (2009) Recommendations for the evaluation of left ventricular diastolic function by echocardiography. Eur J Echocardiogr 10: 165–193.
- Cianciulli TF, Saccheri MC, Lax JA, Bermann AM, Ferreiro DE (2010) Two-dimensional speckle tracking echocardiography for the assessment of atrial function. World J Cardiol 2: 163–170.
- Mor-Avi V, Lang RM, Badano LP, Marek Belohlavek, Cardim NM, et al. (2011) Current and evolving echocardiographic techniques for the quantitative evaluation of cardiac mechanics: ASE/EAE consensus statement on methodology and indications endorsed by the Japanese Society of Echocardiography. J Am SocEchocardiogr 24: 277–313.
- Vianna-Pinton R, Moreno CA, Baxter CM, Lee KS, Tsang TSM, et al. (2009) Two-dimensional speckle-tracking echocardiography of the left atrium: feasibility and regional contraction and relaxation differences in normal subjects. J Am Soc Echocardiogr 22: 299–305.
- Miki T, Yuda S, Kouzu H, Miura T (2013) Diabetic cardiomyopathy: pathophysiology and clinical features. Heart Fail 18: 149-66.
- Mishra TK, Rath PK, Mohanty NK, Mishra SK (2008) Left ventricular systolic and diastolic dysfunction and their relationship with microvascular complications in normotensive, asymptomatic patients with type 2 diabetes mellitus. Indian Heart J 60: 548–553.
- Ernande L, Rietzschel ER, Bergerot C, De Buyzere ML, Schnell F, et al. (2010) Impaired myocardial radial function in asymptomatic patients with type 2 diabetes mellitus: a speckle-tracking imaging study. J Am SocEchocardiogr 23: 1266-1272.
- Dikshit ND, Wadia PZ, Shukla DK (2013) Diastolic dysfunction in diabetes mellitus. Natl J Med Res 3: 249-252.
- Aguilar D, Deswal A, Ramasubbu K, Mann DL, Bozkurt B (2010) Comparison of patients with heart failure and preserved left ventricular ejection fraction among those with versus without diabetes mellitus. Am J Cardiol 105: 373–377.
- Ostad AP, Urheim S, Dalen H, Orvik E, Birkeland KI, et al. (2015) Identification of a definite diabetic cardiomyopathy in type 2 diabetes by comprehensive echocardiographic evaluation: A cross-sectional comparison with non-diabetic weight-matched controls. Journal of Diabetes 7: 779-790.
- Suran D, Sinkovic A, Naji F (2016) Tissue Doppler imaging is a sensitive echocardiographic technique to detect subclinical systolic and diastolic dysfunction of both ventricles in type 1 diabetes mellitus, BMC Cardiovascular Disorders 16: 72-79.
- Masugata H, Senda S, Goda F, Yoshiharab Y, Yoshikawab K, et al. (2008) Left ventricular diastolic dysfunction in normotensive diabetic patients in various age strata. Diabetes Res Clin Pract 79: 91–96.
- Sharavanan TKV, Prasanna KB, Ekanthalingam S (2016) A study on the prevalence of diastolic dysfunction in type 2 diabetes mellitus in a tertiary care hospital. IAIM 3(7): 216-221.
- Georgievska-Ismail L, Zafirovska P, Hristovski Z (2016) Evaluation of the role of left atrial strain using two- dimensional speckle tracking echocardiography in patients with diabetes mellitus and heart failure with preserved left ventricular ejection fraction, Diabetes & Vascular Disease Research 13(6): 384-394.
- Mondillo S1, Cameli M, Caputo ML, Lisi M, Palmerini E, et al. (2011) Early detection of left atrial strain abnormalities by speckle-tracking in hypertensive and diabetic patients with normal left atrial size. J Am Soc Echocardiogr 24: 898–908.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi