Research Article, Int J Cardiovasc Res Vol: 6 Issue: 6
Differential Analysis of Nitroglycerin Influence on Myocardium in Coronary Artery Disease Patients
Alekseev Mikhail* and Alekseev Aleksandr
Diagnostic Center - Juventa, Russia
*Corresponding Author : Alekseev Mikhail, Ph.D.
Diagnostic Center “Juventa”, Saint-Petersburg, Mejevaya street, 42, 197755, Russia
Tel: +78124348576, +79219137188
E-mail: Alex-skorost@mail.ru
Received: October 25, 2017 Accepted: November 25, 2017 Published: November 30, 2017
Citation: Alekseev M, Alekseev A (2017) Differential Analysis of Nitroglycerin Influence on Myocardium in Coronary Artery Disease Patients. Int J Cardiovasc Res 6:6. doi: 10.4172/2324-8602.1000330
Abstract
Objective: The mechanism of nitrates action and its positive influence on the myocardium is unclear and cause sharp debates. In current study we made an attempt to open new sides of nitrates and myocardium interaction.
Methods: We examined 14 patients with G-criterion during an episode of chest pain. In 10 cases, the angina pectoris was cut off using nitroglycerin 0.8 mg sublingually. The recordings were made during the angina pectoris and nearly 16 minutes after NTG administration. This gives us the dynamic of changes in myocardium during drug administration. In 11 cases the CAD was proved by coronary angiography, but another 3 patient had non-cardiac cause of chest pain. The G-criterion is calculated by mathematical division of standard deviation by average value of T-wave amplitude values from 60 seconds in each electrocardiographic channel. Then the G-criteria from all channels were compared by relation the maximum value in ischemic zone to minimum value non-ischemic to get the second order G-criteria (SOG-criteria).
Results: It was shown that the arrest of angina in 10 cases occurred in the 2-4th minutes after NTG administration, but, according to the G-criterion and SOG-criterion, the decrease of myocardium ischemia (-51%) was basically in the 4-8th minutes, and the duration of ischemia reduction lasted from between 2 and 8 minutes. We registered the opposite reaction on NTG administration in all 11 CAD patients: in ischemic zone of the myocardium the G-criterion decreased on average -28.4% and in normal zone the G-criterion increased +54.5%.
Conclusion: This study indicates the different response of ischemic and normal myocardium on the same dosage of NTG, which can be used as diagnostic criterion for ischemic zones. The assessment of NTG effect should be based not only on the subjective patient’s sensations, but also on the positive or negative evolution of objective criteria for myocardial ischemia.
Keywords: Nitroglycerin; DACG; T-wave amplitude; Statistical criterion; Angina pectoris; Coronary artery disease; Acute coronary syndrome
Objective
Acute coronary syndrome (ACS) is the most frequent manifestation of ischemic heart disease (IHD). Cardiovascular disease is now the most common cause of mortality worldwide, and among cardiovascular deaths, the majority are attributable to coronary artery disease (CAD).
Patients with ischemic heart disease can be divided into two large groups: patients with chronic coronary artery disease (CAD), who most commonly present with stable angina and patients with acute coronary syndromes (ACSs). The ACS group is composed of patients with acute myocardial infarction (MI) with ST-segment elevation (STEMI) on their presenting electrocardiogram (STEMI), and those with unstable angina (UA) and non-ST-segment elevation MI (NSTEMI). The relative incidence of UA/NSTEMI in comparison with STEMI appears to be increasing.
The diagnosis of UA is based largely on the clinical presentation. Stable angina pectoris is characterized by chest or arm discomfort that may not be described as pain but is reproducibly associated with physical exertion or stress and is relieved within 5–10 min by rest and/ or sublingual nitroglycerin. The discomfort is usually severe enough to be considered painful. Anginal “equivalents” such as dyspnea and epigastric discomfort may also occur. The examination resembles that in patients with stable angina and may be unremarkable.
In UA, ST-segment depression, transient ST-segment elevation, and/or T-wave inversion occur in 30–50% of patients, depending on the severity of the clinical presentation. In patients with the clinical features of UA, the presence of new ST-segment deviation, even of only 0.05 mV, is an important predictor of adverse outcome. T-wave changes are sensitive for ischemia but less specific, unless they are new, deep T-wave inversions.
An ischemic myocardium results when the supply of oxygenated blood through the coronary arteries becomes in adequate to meet the demands of cardiac muscle, leading to myocardial anoxia [1]. CVD can result from a quantitative or functional nitric oxide (NO) deficiency that can limit NO-dependent signal transduction pathways to the detriment of normal cellular function, and as such, delivery of low concentrations of exogenous NO would be an attractive therapeutic option [2].
Nitric oxide formation by endothelial NO synthase (NOS) plays an important role in the regulation of vasomotor tone in the pulmonary and systemic vascular beds [3-6]. The importance of NO in the regulation of vasomotor tone has been demonstrated in experimental animals and in human subjects by the use of NOS inhibitors [3,5-7]. NO is also produced by NOS independent mechanisms [8-10]. Nitrite can be produced by oxidation of NO under physiologic conditions [11-13]. However, NO generation by NOS may be rapidly depleted in ischemic conditions, because NOS is dependent upon the availability of oxygen [14,15].
At this time, the most commonly used NO agents at this time include isosorbide dinitrate, isosorbide-5-mononitrate and NTG, all of which are effective in reducing ventricular preload by increasing peripheral venous capacitance [15-17]. These drugs can decrease systemic vascular resistances, but it requires higher doses than in case of venous capacitance increasing [18-23]. These agents can reduce ventricular filling pressure and myocardial oxygen consumption [24] , and may can also improve systolic and diastolic ventricular function by improving coronary flow in patients with ischemic heart disease. The limitations of this class of agents are well known and potentially include adverse hemodynamic effects, drug tolerance, lack of selectivity, and limited bioavailability [25].
The current study is an attempt to solve the problem of objective assessment of patient’s complaints. Drug administration, for example, nitroglycerin can help us to determine the accuracy of chosen assessment method.
Materials and Methods
For this study we used the Digital Analytic Cardiography technology (DACG) [26], which is based on the in-depth analysis of temporal and amplitude parameters of well-known electrocardiographic (ECG) parameters. For this aim the common 12-channel electrocardiograph with the possibility of raw ECG data transfer was used. The fundamental differences between DACG technology and usual ECG diagnostic are: 1. The sensitivity of highresolution ECG device with resolution of less than 50 microseconds in time and of less than 5,0 microvolts in amplitude; 2. The duration of recording was 60 seconds to have sequence of ECG data parameters.
In each case silver/silver chloride electrodes were used: four limb leads and six precordial leads (V1-V6). The recording was made over 12 channels simultaneously for 60 seconds: two to four times before the NTG administration and 16 times after. We could record only 16 minutes not to disturb the usual protocol of cardiological care. Then the data were transferred from ECG device to the computer for analysis. The ECG signal records were processed by the original program pocket with calculating G-criterion.
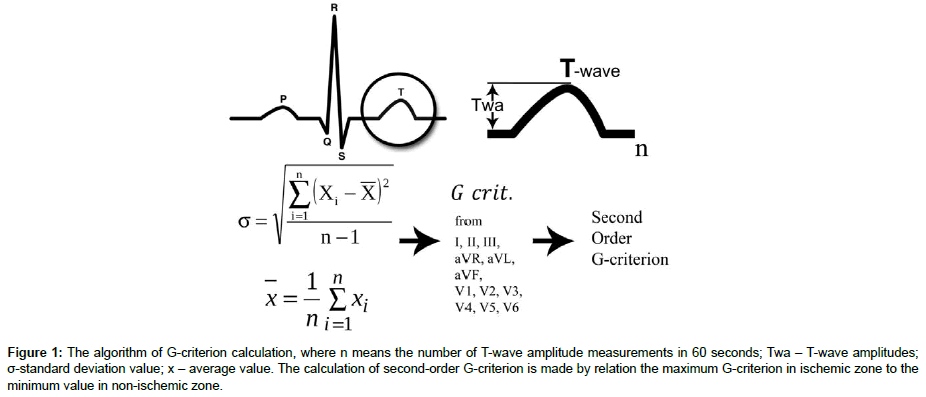
It is known, that the first ischemic changes are represented on the surface ECG by T wave abnormalities (hyperacute, inverted, biphasic and flat) and ST-segment changes (elevation, depression). For calculating the G-criterion we used the T-wave amplitude (Twa; positive, negative, the both waves in biphasic case) from each 12 channels. The number of T-waves in each case differs, because the recordings were made during 60 seconds and every patient had his own heart beat rate. After measuring the T-wave amplitudes from recording, we use the statistical characteristics: standard deviation and average value from the formulas (Figure 1). For calculation the G-criterion we relate mathematically the standard deviation of T-wave amplitudes (Twa) to the average value of the T-wave amplitudes from the same source of T-waves [27]. For convenience of result presentation we reduced the values to the one. Then we compared the G criteria from each channel, which reflected the different parts or walls of the heart muscle. The difference of G-criteria between channels gives us significantly quantitative characteristics of ischemic zones and non-ischemic zones in myocardium. We related the maximum or ischemic value of G-criterion from one channel to the minimum or non-ischemic value of G-criterion from another channel to calculate the second order G- criterion (SOG-criterion) [27].
Figure 1: The algorithm of G-criterion calculation, where n means the number of T-wave amplitude measurements in 60 seconds; Twa – T-wave amplitudes; σ-standard deviation value; x – average value. The calculation of second-order G-criterion is made by relation the maximum G-criterion in ischemic zone to the minimum value in non-ischemic zone.
For current study we examined 14 patients via G-criterion during the episode of chest pain. In 10 cases the angina pectoris ceased after administration of 0,8 mg nitroglycerin sublingually. The severity of chest pain was assessed by using 11-point numeric rating scale (NRS-11). The characteristics of patients are presented on Table 1. The recordings were made during the angina pectoris and nearly 16 minutes after NTG administration with fixing the results of G-criteria every 1 minute. This gave us the dynamic of changes in ischemic and normal myocardia during drug administration.
| With CAD | Male | Age | MI | Chest pain | PCI | ST-segment changes | T-wave changes | ||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Cause | NRS-11 | CA lesion | changes in mm | localisation | localisation | ||||||
| Patient B | male | 61 | - | Chest discomfort | 4 | + | RCA, LAD | -2,1 | V5-V6 | normal | |
| Patient S | female | 70 | + | Chest pain/dispnoe | 5 | + | LAD | -1,1 | V5-V6 | inversion | V4-V6 |
| Patient V | female | 77 | + | Chest pain | 8 | + | LAD | -0,7 | V6 | inversion | V2-V5 |
| Patient G | male | 79 | + | Chest pain | 9 | + | LCx | - | - | broad | V4-V6 |
| Patient I | male | 56 | - | Chest pain | 9 | + | LAD | -0,8 | V4-V5 | inversion | V3-V6 |
| Patient K | male | 44 | - | Chest pain | 5 | - | - | -0,2 | V6 | normal | |
| Patient Ph | male | 74 | + | Chest pain | 5 | + | RCA | -1,2 | V5-V6 | flat | III, aVF |
| Patient M | female | 74 | - | Chest pain | 7 | + | LAD, RD1 | -1,0 | V6 | broad | V5 |
| Patient Sl | female | 74 | - | Chest pain | 4 | + | RCA | descending | V5-V6 | inversion/flat | III/V3 |
| Patient A | male | 64 | + | Chest pain | 6 | + | LCx | - | - | normal | |
| Patient P | male | 59 | + | Chest pain | 7 | + | LCx | -1,0 | V6 | inversion/flat | V2-V3/V4 |
| Without CAD | |||||||||||
| Patient T | female | 51 | - | Chest pain | 8 | - | - | - | - | normal | |
| Patient St | male | 37 | - | Chest pain | 6 | - | - | - | - | normal | |
| Patient N | female | 51 | - | Chest pain | 6 | - | - | - | - | broad | V3 |
Table 1: The characteristics of chest pain patients. MI (myocardial infarction) in anamnesis. NRS-11 (Numeric Rating Scale) is an 11-point scale for self-reporting of pain. The data coronary angiography results are presented with significant coronary artery lesion above 50%. The ST-T changes were assessed according rest ECG test. In the bottom of the table are presented the characteristics of chest pain patients without CAD, but they also used nitroglycerin 0.8 mg.
In 11 cases, CAD was proved by coronary angiography, but another 3 patient had non-cardiac cause of pain. In cases of patients T. and St. were diagnosed intercostal neuralgia and the esophagitis in patient N. as a cause of acute chest pain. The results of coronary angiography are shown and only the arteries with coronary lesion above 50%.
Results
The patients with acute chest pain are presented on the Table 2. From 14 patients with chest pain 10 had positive subjective effect of the NTG administration, basically, between the 2nd and 4th minutes; 4 patients had no effect. The time of the beginning of NTG subjective effect was much more rapid, than the beginning of the decrease of ischemia by SOG-criterion. The decrease of SOG-criterion was registered in all CAD patients. The average time of NTG subjective effect was more than 20 minutes, the duration of the SOG criterion lowering lasted 2-8 minutes. After the lowering of ischemia the SOGcriterion began slowly increasing. The decrease of second order G-criterion in CAD patients is was on average 51%. We registered the regularity: the higher the second order G-criterion was, the more significant the second order G-criterion decreased after NTG administration.
| NTG efect subjectively | Second order G-criterion (SOG) | Normal or Non-Ischemic zone | Ischemic zone | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| With CAD | effect | time of effect | before | after | % of change | time of effect | lead | before | after | before | after | |
| Patient B | yes | 2 min. | 3,14 | 2,11 | -32,80 | 4 min | V3 | 3,42 | 3,56 | V6 | 10,76 | 7,89 |
| Patient S | mild yes | 2 min. | 4,6 | 3,21 | -30,22 | 2 min | V1 | 4,51 | 5,2 | V4 | 20,73 | 16,68 |
| Patient V | yes | 1 min. | 8,31 | 2,59 | -68,83 | 6 min | V3 | 2,42 | 6,34 | V6 | 19,37 | 16,44 |
| Patient G | mild yes | 3,5 min | 7,77 | 3,08 | -60,36 | 9 min | V2 | 2,26 | 4,28 | V5 | 16,32 | 13,2 |
| Patient I | yes | 2 min. | 7,27 | 2,82 | -61,21 | 8 min | V6 | 1,94 | 3,36 | V3 | 15,08 | 9,48 |
| Patient K | no | - | 6,27 | 3,52 | -43,86 | 13 min | V3 | 3,05 | 4,24 | V5 | 20,52 | 14,96 |
| Patient Ph | yes | 3 min. | 3,87 | 1,54 | -60,21 | 5 min | V2,V3 | 8,08 | 9,72 | V5 | 31,29 | 14,94 |
| Patient M | yes | 3 min. | 4,47 | 2,21 | -50,56 | 6 min | V2 | 2,54 | 4,02 | V5 | 15,27 | 8,92 |
| Patient Sl | yes | 2,5 min. | 3,19 | 1,85 | -42,01 | 9 min | V6 | 5,37 | 6,97 | V3,V4 | 14,09 | 12,95 |
| Patient A | yes | 2 min. | 3,59 | 1,58 | -55,99 | 3 min | V6 | 3,09 | 4,11 | V2 | 11,08 | 6,52 |
| Patient P | yes | 1,5 min. | 4,67 | 2,48 | -46,90 | 4 min | V2 | 3,06 | 5,38 | V5 | 14,3 | 10,81 |
| Without CAD | ||||||||||||
| Patient T* | no | - | 1,36 | 2,85 | +109,56 | 7 min | V2 | 5,82 | 11,71 | V4 | 4,43 | 3,2 |
| Patient St* | no | - | 1,87 | 2,57 | +37,43 | 5 min | V3 | 3,36 | 3,7 | V6 | 6,31 | 9,51 |
| Patient N* | no | - | 1,45 | 2,52 | +73,79 | 5 min | V2 | 6,04 | 4,44 | V5 | 8,79 | 11,19 |
Table 2: The individual changes of patients pain perception before and after NTG administration. It shows the time difference between the subjective effect and objective effect by second order G-criterion. We can see the percentage of lowering the G-criterion in ischemic zones and the opposite increase normal or non-ischemic zone of myocardium in all CAD patients. Patient T*, St* and N* without CAD have different reaction on NTG in two non-ischemic zones. It is registered the lowering of the second-order G-criterion (on average -51%) and the opposite effect on NTG administration in normal patients (+109,5%, + 37,4%, 73,8%).
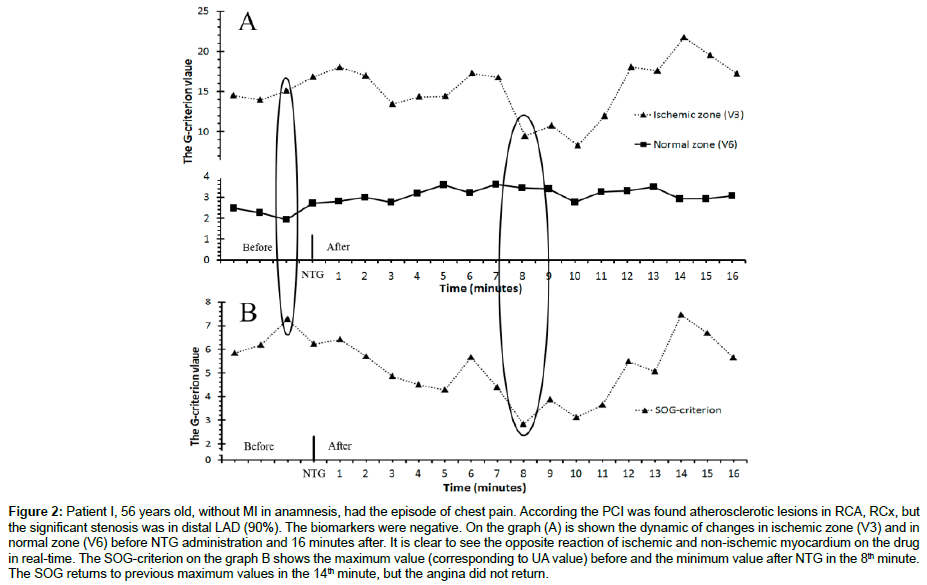
The precise examination of 11 cases with second order G-criterion lowering, we noticed one interesting fact: the G-criterion decreased in the ischemic zone, but, at the same time, we registered the increasing of G-criterion in non-ischemic zones in all cases. One of the examples is presented on Figure 2. Patient I, 56 years old, had a severe episode angina pectoris with positive subjective and objective effects of NTG. On the graph we see the decreasing the G-criterion in ischemic zone in leads V2-V3 from 15,08 to 9,48 (-37,14%), but the non-ischemic zone in leads V5-V6 shows the increasing of G-criterion, for example in V5 from 1,94 to 3,36 (+73,2%). The duration of the anti-ischemic effect was maximum 4 minutes, and after that, the SOG-criterion began gradually increasing to prior levels. The SOG-criterion returned to prior levels in the 16th minute.
Figure 2: Patient I, 56 years old, without MI in anamnesis, had the episode of chest pain. According the PCI was found atherosclerotic lesions in RCA, RCx, but the significant stenosis was in distal LAD (90%). The biomarkers were negative. On the graph (A) is shown the dynamic of changes in ischemic zone (V3) and in normal zone (V6) before NTG administration and 16 minutes after. It is clear to see the opposite reaction of ischemic and non-ischemic myocardium on the drug in real-time. The SOG-criterion on the graph B shows the maximum value (corresponding to UA value) before and the minimum value after NTG in the 8th minute. The SOG returns to previous maximum values in the 14th minute, but the angina did not return.
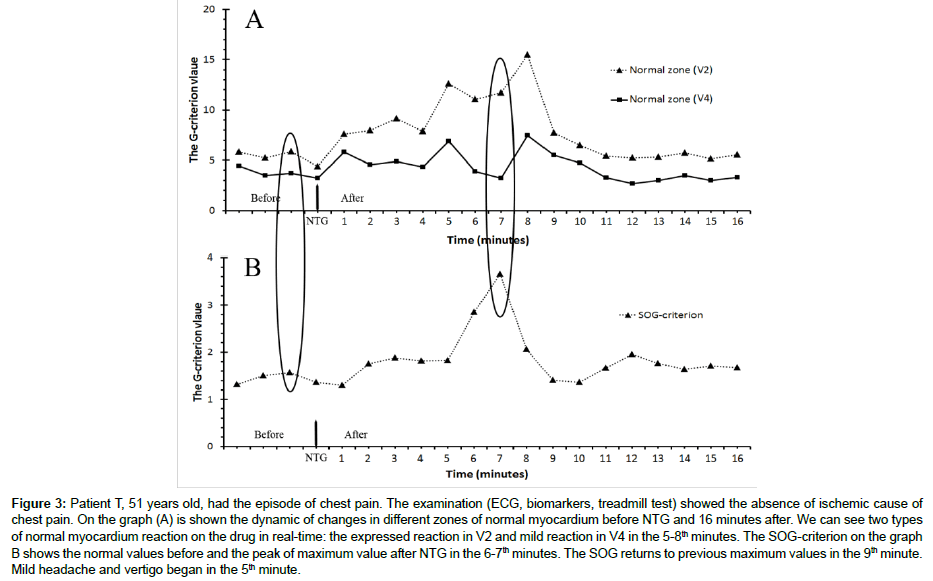
Of 14 patients, only 3 had normal value of second order G-criterion (1,42, 1,36) or II functional class (1,87). After the diagnostic protocol by ECG, stress test and biomarker testing, it was diagnosed the nonischemic cause of chest pain. There was no positive effect of NTG administration. At the same time we registered the opposite effect of second order G-criterion after NTG administration. The increasing was +73,8%, +109,6% and +37,4%, respectively. One of these cases, patient T., is presented on Figure 3. On the graph we can see that SOG-criterion was 1,36, the maximum value of G-criterion was in V4. In the 7th minute after the NTG administration the SOG-criterion increased to 2,85 (+109,56%). The increasing of G-criterion in V2 from 5,82 to 11,71 (+101,2%) and decreasing in V4 from 4,44 to 3,2 (-28%). It also noticeable, that in V2 the G-criterion increased significantly in the 10th minute up to 15,45, but in V4 increased significantly to 7,49, the SOG-criterion was 2,06. In other 2 cases the reaction of myocardium had the same trend, but with different percentage of changes.
Figure 3: Patient T, 51 years old, had the episode of chest pain. The examination (ECG, biomarkers, treadmill test) showed the absence of ischemic cause of chest pain. On the graph (A) is shown the dynamic of changes in different zones of normal myocardium before NTG and 16 minutes after. We can see two types of normal myocardium reaction on the drug in real-time: the expressed reaction in V2 and mild reaction in V4 in the 5-8th minutes. The SOG-criterion on the graph B shows the normal values before and the peak of maximum value after NTG in the 6-7th minutes. The SOG returns to previous maximum values in the 9th minute. Mild headache and vertigo began in the 5th minute.
In all patients with IHD the dynamic of SOG-criterion depends on G-criterion changes both in ischemic zone,where the G-criterion decreases, and in normal or non-ischemic one,where the G-criterion increases, after NTG administration. The return of SOG-criterion was fixed registered in the 12-14th minute in all CAD patients, excluding patient K. without subjective effect of NTG administration.
Discussion
The fact of quantitative correspondence of second order G-criterion and functional classes of CAD, which was revealed in our previous studies [26], and the fact of definite decrease of this criterion on NTG administration in CAD patients testify, that worked out G-criterion reflects clearly the ischemic status of myocardium with statistical accuracy. At the same time, the G-criterion proves quantitatively the positive anti-ischemic effect of nitrate administration and the individual features of each patient.
In this study, we analyzed the NTG administration at 0,8 mg and assessed the influence of NTG on the heart muscle, since this way of NTG administration has less effect on the arterial blood pressure [28-30].
The relief of angina pectoris in all cases with CAD, excluding Patient K., in the 1-2 minute after sublingual NTG administration can be clarified by various reasons. The influence of NO, as a neuromodulator, can be realized through the reflex action on the afferent nerve pathways. The studies suggested that the muscular cardiac algogenic effects of adenosine are mediated mainly by A1 receptors and the patients without CAD need substantially greater dosage of adenosine in experimentally-caused angina [31,32]. The NO can affect on the adenosine receptors and decrease the sensitivity to pain. Additionally, the emotive reaction or ‘placebo effect’ of drug administration also has the significant influence on pain perception. High incidence of this effect was reported in studies of assessing symptom relief [33], and also was reported that NTG-induced vasodilation could not be demonstrated [34,35].
The restoration of the ischemic status objectively according to the G-criterion nearly in the 12-14th minute after NTG administration (the return of SOG-criterion to baseline level in 10 cases) without symptoms of angina can be the corroboration of reflex and A1- receptor modulation mechanism of NTG. It means that the level of ischemia became as before NTG administration, but the pain was arrested. This fact raise the question: what is the trigger mechanism of angina pectoris? The only one fact of myocardial ischemia is not sufficient. As it is known, that 21% of CAD patients are asymptomatic [36,37].
A decrease of myocardial ischemia severity begins in the 4 to 6 minutes and has the maximum value in the 6th to 9th minutes in every CAD patient, excluding one case without positive NTG effect. The fact that sublingual administration of 0,8 mg NTG resulted in maximum blood concentration in nearly in the 5 minute speaks well to this observation. This amount of time is necessary for realization of nitrates’ effects, which include(s): direct relaxant effect on vascular smooth muscles and dilation of coronary vessels, which improves oxygen supply to the myocardium, the dilation of peripheral veins and arteries, reducing preload and afterload with further lowering of myocardial oxygen consumption.
The study also reports the fact of reliable opposite reaction on nitrates administration of ischemic and non-ischemic myocardium in all CAD patients. As it is shown in Table 2, the decrease of G-criterion in ischemic zone on average -28.4%, but in normal, or non-ischemic zone of myocardium we registered the increase of G-criterion +54.5% on average. It can be explained by anti-ischemic effect of nitrates in ischemic zone, but in normal zone the high non-physiological concentration of NO in combination with normal oxygen supply can cause the formation of the highly reactive and harmful radical, peroxynitrite (ONOO). This radical is produced by the reaction of superoxide and NO, and it influences the repolarization process and relaxation of non-ischemic myocardia, which is realized in increasing of T-wave amplitude instability (G-criterion) [38].
In the group of patients without CAD (3 patients), two types of reaction of myocardia were seen with on NTG administration. In one zone of myocardium, it had no reaction on to drug administration, but in another, it had the same one, like the non-ischemic zone in CAD patients. The time of the increase was from 6 to 8 minutes also, and its duration was 1 to 1.5 minutes. The same reaction is seen with on non-physiological concentrations of NO in normal myocardia. At the same time, the zones without significant reaction can be, potentially, the future ischemic zones.
The analysis of G-criterion from different leads allows precisely revealing revelation the ischemic zones, it severity and the influence of anti-ischemic drugs. As we showed in the study, it is important to assess the status not only the ischemia, but also the non-ischemic myocardia.
Conclusion
The anti-anginal effect of NTG begins in the 2th - 4th minutes after sublingual administration, and it can be the result of NO reflex action as neurotransmitter, because the duration of anti-anginal effect is much longer than the direct effect on myocardium. At the same time, the anti-ischemic effect of NTG begins later (in the 4th to 9th minute after NTG administration) and lasts 2 to 8 minutes.
The opposite response of G-criterion in ischemic and nonischemic myocardia after NTG administration allows utilizing this effect in pharmaceutical examination of patients as diagnostic test of IHD. For objectification of anti-ischemic effect of drugs (for example, nitrates), it is required to have dynamic control of myocardium and the severity of ischemic changes. The estimation of drug efficacy, based on the angina termination (subjective assessment), do not reflects the changes in the heart.
Acknowledgements
We thank our action group of like-minded persons for their contributions. Also, we thank the AMEDTEC Medizintechnik Aue DmbH Company for helping with the 12-lead ECG-device for our scientific needs. Special thanks are given to the staff of the Diagnostic Center “Juventa”.
Funding Sources
This research was supported by the personal funds of first author.
Conflict of interest disclosures
None
References
- Contro S, Haring OM (1952) Goldstein W Paradoxic action of amyl nitrite in coronary patients. Circulation 6: 250-256.
- Napoli C, Ignarro LJ (2003) Nitric oxide-releasing drugs. Annu Rev Pharmacol Toxicol 43: 97-123
- McMahon TJ, Hood JS, Bellan JA, Kadowitz PJ(1991) N omega-nitro-L-arginine methyl ester selectively inhibits pulmonary vasodilator responses to acetylcholine and bradykinin. J Appl Physiol 71: 2026-2031.
- Rees DD, Palmer RM, Schulz R, Hodson HF, Moncada S (1990) Characterization of three inhibitors of endothelial nitricoxide synthase in vitro and in vivo. Br J Pharmacol 101: 746-752.
- Bellan JA, Minkes RK, McNamara DB, Kadowitz PJ (1991) N omega-nitro-L-arginine selectively inhibits vasodilator responses to acetylcholine and bradykinin in cats. Am J Physiol Heart Circ Physiol 260: H1025-1029.
- McMahon TJ, Hood JS, Kadowitz PJ (1992) Pulmonary vasodilator response to vagal stimulation is blocked by N omega-nitro-L-arginine methyl ester in the cat. Circ Res 70: 364-369.
- Hauser B, Bracht H, Matejovic M, Peter R, Balasubramanian V et al. (2005) Nitric oxide synthase inhibition in sepsis? Lessons learned from large-animal studies. Anesth Analg 101: 488-498.
- Zweier JL, Samouilov A, Kuppusamy P (1999) Non-enzymatic nitric oxide synthesis in biological systems. Biochim Biophys Acta 1411: 250-262.
- Cosby K, Partovi KS, Crawford JH, Patel RP Reiter CD et al. (2003) Nitrite reduction to nitric oxide by deoxyhemoglobin vasodilates the human circulation. Nature Med 9: 1498-1505.
- Jansson EA, Petersson J, Reinders C, Sobko T, Björne H et al. (2007) Protection from nonsteroidal anti-inflammatory drug (NSAID)-induced gastric ulcers by dietary nitrate. Free Radic Biol Med 42: 510-518.
- Lauer T, Preik M, Rassaf T, et al. (2001) Plasma nitrite rather than nitrate reflects regional endothelial nitric oxide synthase activity but lacks intrinsic vasodilator action. Proc Natl Acad Sci USA 98: 12814-12819
- Heiss C, Lauer T, Dejam A, Kleinbongard P Hamada S et al. (2006) Plasma nitroso compounds are decreased in patients with endothelial dysfunction. J Am Coll Cardiol 47: 573-579.
- Kleinbongard P, Dejam A, Lauer T, Jax T, Kerber S et al. (2006) Plasma nitrite concentrations reflect the degree of endothelial dysfunction in humans. Free Radic Biol Med 40: 295-302.
- North AJ, Lau KS, Brannon TS, Wu LC, German Z, et al. (1996) Oxygen upregulates nitric oxide synthase gene expression in ovine fetal pulmonary artery endothelial cells. Am J Physiol Lung Cell Mol Physiol 270: L643-649
- Bogaert MG (1972) Organic nitrates in angina pectoris. Arch Int Pharmacodyn Ther 196 (Suppl 196): 125.
- Battock DJ, Levitt PW, Steele PP (1976) Effects of isosorbide dinitrate and nitroglycerin on central circulatory dynamics in coronary artery disease. Am Heart J 92: 455-458
- Silber S (1990) Nitrates: why and how should they be used today? Current status of the clinical usefulness of nitroglycerin, isosorbide dinitrate and isosorbide-5-mononitrate. Eur J Clin Pharmacol 38: S35-51.
- Johnson JB, Fairley A, Carter C (1959) Effects of sublingual nitroglycerin on pulmonary arterial pressure in patients with left ventricular failure. Ann Intern Med 50: 34-42
- Fremont RE (1961) The actions of organic nitrates on the cardiopulmonary and peripheral circulations. Angiology 12: 391-400.
- Mikulic E, Franciosa JA, Cohn JN (1975) Comparative hemodynamic effects of chewable isosorbide dinitrate and nitroglycerin in patients with congestive heart failure. Circulation 52: 477-482.
- Charuzi Y (1982) Use of nitroglycerin ointment in acute pulmonary edema and hypertension. Chest 82: 800.
- Palevsky HI, Fishman AP (1985) Vasodilator therapy for primary pulmonary hypertension. Annu Rev Med 36: 563-578.
- Bundgaard H, Boesgaard S, Mortensen SA, Arendrup H, Aldershvile (1997) Effect of nitroglycerin in patients with increased pulmonary vascular resistance undergoing cardiac transplantation. Scand Cardiovasc J 31: 339-342.
- Pearlman AS, Engler RL, Goldstein RA, Kent KM, Epstein SE (1980) Relative effects of nitroglycerin and nitroprusside during experimental acute myocardial ischemia. Eur J Cardiol 11: 295-313.
- Ignarro LJ, Napoli C, Loscalzo J (2002) Nitric oxide donors and cardiovascular agents modulating the bioactivity of nitric oxide: an overview. Circ Res 90: 21-28.
- Alekseyev M, Alekseyev A, Dowzhikov A, Labin S (2014) Digital Analytic Cardiography (DACG), a New method for quantitative tropism assessment of the myocardium. Int J Cardiovasc Res 3:6.
- Alekseev M, Alekseev A, Siegle R, Roder G (2016) Data processing apparatus for assessing a condition of a myocardium. Patent application PCT/EP2016/001193, DE.
- Mason DT, Braunwald E (1965) The effects of nitroglycerin and amyl nitrite on arteriolar and venous tone in the human forearm. Circulation 32: 755-766.
- Wilkins RW, Haynes FW, Weiss S (1937) The role of the venous system in circulatory collapse induced by sodium nitrite. J Clin Invest 16: 85-91.
- Ablad B, Johnsson G (1963) Comparative effects of intra-arterially administered hydralazine and sodium nitrite on blood flow and volume of forearm. Acta Pharmacol Toxicol (Copenh) 20: 1-15.
- Gaspardone A, Crea F, Tomai F, Versaci F, et al. (1995) Muscular and cardiac adenosine-induced pain is mediated by A1 receptors. J Am Coll Cardiol 25: 251-7.
- Sylven C (1993) Mechanisms of pain in angina pectoris--a critical review of the adenosine hypothesis. Cardiovasc Drugs Ther 7: 745-59.
- Master AM, Jaffe HL, Dack S (1939) The drug treatment of angina pectoris due to coronary artery disease. Am J M Sc 197: 774.
- Gorlin R, Brachfeld N, MacLeod C, et al. (1959) The effect of nitroglycerin on the coronary circulation in patients with coronary artery disease or increased left ventricular work. Circulation 19: 705-718.
- Ross RS, Ueda K, Lichtlen PR, et al. (1964) Measurement of Myocardial Blood Flow in Animals and Man by Selective Injection of Radioactive Inert Gas into the Coronary Arteries. Circ Res 15: 28-41.
- Community surveillance event rates. Atherosclerosis Risk in Communities (ARIC) Study Website.
- Boland LL, Folsom AR, Sorlie PD, Taylor HA, et al. (2002) Occurrence of unrecognized myocardial infarction in subjects aged 45 to 65 years (the ARIC study). Am J Cardiol 90: 927-931.
- Ferdinandy P, Schulz R. (2003) Nitric oxide, superoxide, and peroxynitrite in myocardial ischaemia-reperfusion injury and preconditioning. Br J Pharmacol 138: 532-43.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi