Case Report, Int J Cardiol Res Vol: 14 Issue: 1
Double Trouble-Lignocaine Induced Complete Heart Block in QRBBB-ACS
Rupendra Nath Saha*
Department of Cardiology, All India Institute of Medical Sciences (AIIMS), New Delhi, India
*Corresponding Author: Rupendra Nath Saha
Department of Cardiology, All India Institute of Medical Sciences (AIIMS), New Delhi, India
E-mail: rupendra.ncp@gmail.com
Received date: 03 September, 2024, Manuscript No. ICRJ-24-147155;
Editor assigned date: 06 September, 2024, PreQC No. ICRJ-24-147155 (PQ);
Reviewed date: 20 September, 2024, QC No. ICRJ-24-147155;
Revised date: 14 February, 2025, Manuscript No. ICRJ-24-147155 (R);
Published date: 21 February, 2025, DOI: 10.4172/2324-8602.1000604.
Citation: Saha RN (2025) Double Trouble-Lignocaine Induced Complete Heart Block in QRBBB-ACS. Int J Cardiol Res 14:1.
Abstract
Arrhythmia is one of the most common causes of fatality in Acute coronary syndrome. We are presenting a case of ACS with QRBBB on presentation which was started on lignocaine infusion post angioplasty for prevention of ventricular tachycardia, which resulted in an iatrogenic complete heart block, which reverted on stopping the drug. The exaggerated toxicity of the drug was blamed on the long duration of the drug infusion and co-existing ischemic hepatitis.
Keywords: Coronary, Heart, Hepatitis, Drug
Introduction
Coronary Artery Disease (CAD) is one of the most common cardiovascular illnesses impacting the global human population. This disease is the leading cause of death in both developed and developing countries. An arrhythmia complicating would often be the cause of mortality. Lifestyle, environmental, and hereditary variables all contribute to the risk of developing cardiovascular disease.
Case Presentation
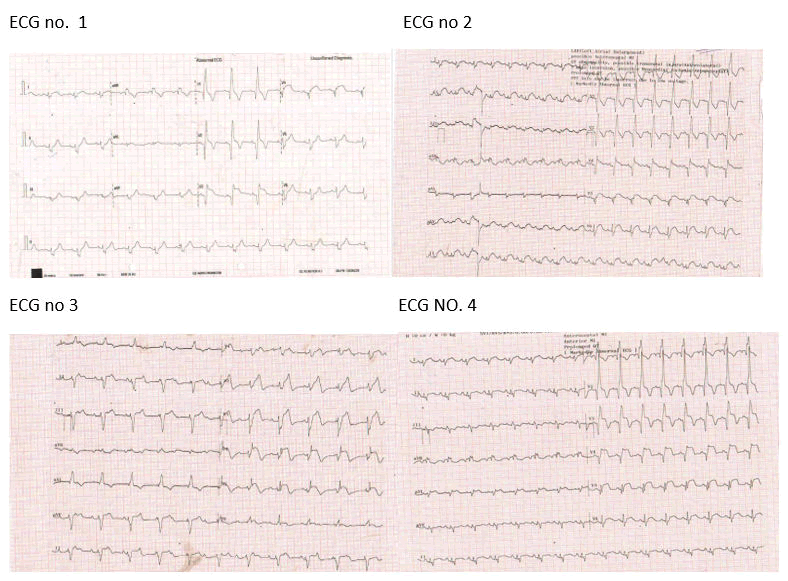
A 49-year-old gentleman, presented with sudden onset compressive chest pain for the last 10 hours. Clinical examination revealed him to be in shock with cold and clammy peripheries. ECG was suggestive of qRBBB pattern in precordial leads with corresponding ST depression in inferior leads and ST elevation in aVR (ECG no. 1). Echocardiography suggested hypokinetic anterior, anterolateral walls and apex with an ejection fraction of 35%-40%. He was diagnosed to have an extensive anterior wall myocardial infarction and was wheeled in for primary angioplasty. Invasive coronary angiography was suggestive of proximal LAD 100% occlusion with grade V thrombus. He developed wide complex ventricular tachycardia on the table, which was managed with defibrillator shock. Subsequently, primary angioplasty to LAD was done with two drug-eluting stents, establishing TIMI III flow. He was having recurrent NSVT runs post PTCA in ICU monitor and ECG was suggestive of frequent VPCs (ECG no. 2). Thus, was started on lignocaine infusion at a rate of 1 mg/kg/hr. His blood investigations were suggestive of ischemic hepatitis and hence were decided to be managed conservatively. Lignocaine infusion was continued for 36 hours when he developed a complete heart block (ECG no. 3). Immediately, the lignocaine infusion was stopped, and he was observed for any symptoms. He reverted to normal sinus rhythm (ECG no. 4) within an hour. He was initiated on beta blockers and discharged after two more days of rehabilitation. He was followed up in our OPD after two weeks, where he was reported to be completely asymptomatic and carrying out his daily activities as usual (Figure 1).
Figure 1: ECG scan numbers.
When an anterior Myocardial Infarct (MI) occurs, the most common cause of new Right Bundle Branch Block (RBBB) is proximal occlusion of the left anterior descending coronary artery with impaired circulation of the septal arteries supplying the bundle branches. Because the right ventricle is located anteriorly, rightprecordial Q waves can be hidden when the aberrant septal forces linked to an anteroseptal MI are neutralised by activating the right ventricular free wall [1]. As a result, irregular Q waves in the right precordial leads are particularly noticeable during RBBB, exhibiting the traditional qRBBB pattern. The right ventricle activates later, showing the anomalous septal forces in most patients with an anteroseptal myocardial infarction. Acute qRBBB myocardial infarction is a dangerous variation of acute coronary syndrome that requires immediate detection and the implementation of reperfusion therapy due to its high in-hospital mortality and morbidity rate. Ventricular tachyarrhythmias (12%), total heart block (13%), heart failure (69%), and cardiogenic shock (52%) were all quite prevalent [2]. According to current recommendations, reperfusion treatment in prior MI is accompanied by LBBB or STEMI, not RBBB. Applying the Hirulog and Early Reperfusion or Occlusion-2 (HERO-2) databank, Wong et al. evaluated the various bundle branch blocks present in the early stages of MI to identify their prognostic relevance. 6.9% of patients with normal conduction, 11.4% with RBBB at randomisation, and 16.7% with new RBBB within 60 minutes of admission were found to have expired within 30 days. They agreed that early after fibrinolytic therapy, new BBB (including LBBB) and RBBB accompanying anterior acute MI at presentation are independent predictors of increased 30-day mortality [3].
Lignocaine is a tertiary amide class IB Vaughan-Williams antiarrhythmic agent, most popularly used for its local anaesthetic properties. Intravenous (IV) lidocaine was initially documented in the literature in 1950 [4] to treat a ventricular tachycardia episode during cardiac catheterisation; however, its antiarrhythmic properties were not widely utilised until the 1960’s during cardiac surgery. Since then, it’s been a widespread choice for ventricular arrhythmia associated with acute myocardial infarction, very much so due to its short elimination half-life compared to Amiodarone. CNS side effects are known for adverse effects of Lignocaine (1-10%), which include headache, dizziness, and radiculopathy; CVS side effects are much less known [5]. Few case reports exist on its capability to cause brady arrhythmias and heart blocks. Hilleman et al. reported a case of Mobitz type II heart block [6] following lignocaine administration in ordinary therapeutic doses in non-ischemic myocardium. Lichstein et al. reported a case of high-grade AV block following lignocaine usage in a patient with trifascicular block disease [7].
Discussion
Thus, in our case, though lignocaine had to be used for the prevention of a fatal ventricular tachyarrhythmia in a post-ischemic, irritated myocardium, it led to a transient complete heart block. The contributing factors to such maleficent behaviour of the drug might be attributed to the compromised liver function owing to the ongoing ischemic hepatitis; a baseline affected conduction system disease with QRBBB, and continuation of a prolonged infusion of lignocaine for more than 24 hours as beta blockers could not be initiated due to persistence of cardiogenic shock. Though the ideal way of monitoring and thus preventing such episodes would be continuous monitoring for a drug level of lignocaine in blood, such investigation on a routine basis is rarely feasible in our country. In such a scenario, thus it becomes the onus of the treating physician to keep a high alert for such an adverse effect.
Learning point
- Lignocaine can have the adverse effect of causing symptomatic high-grade AV blocks, which are reversible on stopping the drug.
- Compromised liver function, baseline conduction disease, and prolonged infusion are all aggravating factors for such a side effect.
- QRBBB-ACS has a very high mortality due to its inherent nature of causing fatal arrhythmias and cardiogenic shocks, and thus, it to be managed with utmost importance.
Conclusion
Thus QRBBB-ACS is one of the most challenging cases of myocardial infarction to manage and one should be aware of the side effects of lignocaine so commonly used.
Declaration of Interest
None.
References
- Klein A, Baranchuk A (2020) Identification of high-risk patients based on electrocardiogram during acute anterior ST-elevation myocardial infarction: The qRBBB pattern. Can J Cardiol 36: 1708-1709.
[Crossref] [Google Scholar] [PubMed]
- Paul A, Bhatia KS, Alex AG, Thomson VS, Mani T, et al. (2020) Electrocardiographic predictors of mortality in acute anterior wall myocardial infarction with right bundle branch block and right precordial Q-waves (qRBBB). Can J Cardiol 36: 1764-1769.
[Crossref] [Google Scholar] [PubMed]
- Wong CK, Stewart RA, Gao W, French JK, Raffel C, et al. (2006) White, for the Hirulog and early reperfusion or occlusion (HERO-2) trial investigators, prognostic differences between different types of bundle branch block during the early phase of acute myocardial infarction: Insights from the Hirulog and Early Reperfusion or Occlusion (HERO)-2 trial. Eur Heart J 27: 21â??28,
[Crossref] [Google Scholar] [PubMed]
- Southworth JL, Mckusick VA, Pierce EC 2nd, Rawson Jr. FL (1950) Ventricular fibrillation precipitated by cardiac catheterization; Complete recovery of the patient after 45 minutes. J Am Med Assoc 143: 717-720.
[Crossref] [Google Scholar] [PubMed]
- Stephanie A, Kluwer W (2024) Lidocaine (local and regional anesthetic) and (systemic): Drug informationIn: Up-to-Date.
- Hilleman DE, Mohiuddin SM, Destache CJ (1985) Lidocaine-induced second-degree mobitz type II heart block. Drug Intell Clin Pharm 19: 669-673.
[Crossref] [Google Scholar] [PubMed]
- Lichstein E, Chadda KD, Gupta PK (1973) Atrioventricular block with lidocaine therapy. Am J Cardiol 31: 277-281.
[Crossref] [Google Scholar] [PubMed]
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi