Research Article, Int J Cardiovasc Res Vol: 7 Issue: 2
Echocardiographic Study of Paediatrics Patients in a Private Hospital in an Urban City in Nigeria
Barakat Adeola Animasahun* and Omonigho Ekhomu
College of Medicine, Lagos State University, Lagos, Nigeria
*Corresponding Author : Dr. B Adeola Animasahun
College of Medicine, Lagos State University, Lagos, Nigeria
Tel: +2348037250264
E-mail: deoladebo@yahoo.com
Received: February 08, 2018 Accepted: April 19, 2018 Published: April 24, 2018
Citation: Animasahun BA, Ekhomu O (2018) Echocardiographic Study of Pediatrics Patients in a Private Hospital in an Urban City in Nigeria. Int J Cardiovasc Res 7:2. doi: 10.4172/2324-8602.1000347
Abstract
Background: Most previous publications on echocardiography use in Nigeria emanate from public hospitals and academic settings. This study aims to elucidate the peculiarities of echocardiography use in an urban, private hospital study in pediatric patients.
Methods: Prospective and cross-sectional, involving a review of consecutive echocardiogram done at the Pediatric Cardiology unit of the Reddington multi-specialist hospital between February 2005 to January 2009. Data were analyzed using Statistical Package for Social Sciences (SPSS) version 20. Level of significance set at p<0.05.
Results: The age range of the subjects was three days to 256 months of age, with a mean age of 59.4 +/- 64months and a male to female ratio of 1: 1.1. Approximately thirty-seven percent of all the echocardiographs done were normal. The most common indication for echocardiography was heart murmurs. Ventricular septal defect was the most prevalent finding based on murmurs. All Patients whose indication for echocardiography was chest pain had normal findings. Congenital heart diseases constituted 108 (85%) of all the abnormal echocardiographic findings.
Conclusion: Our findings in this study generally seem to fall in line with the appropriate use of heart murmur as an indication for echocardiography. There is a high incidence of LVH in patients evaluated via echocardiogram for obesity. There is a similar distribution in congenital heart diseases as compared to other studies both in private and public settings, as well as developed countries compared to developing nations.
Keywords: Echocardiography; Children; Private hospital; Nigeria
Background
Echocardiography is the commonest imaging modality used in cardiology, because of its easy accessibility, non-invasive nature and highly diagnostic capability [1]. It is important for assessing cardiac structure, function and hemodynamics in those with cardiac disease, and for diagnostics in those expected of the same [1]. First introduced in the 1950s by Hertz and Edler [2], it has been used in Nigeria since 1976 [3]. Most previous publications on echocardiography use in Nigeria have been set primarily in public and academic settings and focused on adults mostly or with children as a hidden subset within the adult majority. The research questions are:
What are the patterns of cardiac findings in Pediatric patients in the studied private multi-specialist hospital?
Do the patterns of cardiac findings in Pediatric patients in the studied private multi-specialist hospital differ significantly from those found in public hospitals?
What are the criteria or indications for echocardiography in the subjects?
What are the echocardiographic findings for each indication for echocardiography in the subjects?
Our study is a retrospective review of a prospectively obtained data, it is descriptive and focuses on pediatric echocardiograms (ECHOs) done at the Reddington Multi-specialist hospital Pediatric cardiology department. Through this study, we seek to review the patterns of cardiac findings in pediatric patients in this private multispecialist hospital. We seek to elucidate the peculiarities to an urban, private hospital study in pediatric patients.
Methods/Study Design
This was a prospective and cross-sectional study, involving a review of consecutive echocardiograms done at the Pediatric Cardiology Unit of the Reddington multi-specialist hospital between February 2005 to January 2009.
The Reddington Multi-Specialist Hospital is a one-stop comprehensive tertiary hospital which provides a solution to various healthcare problems. It is located on the Victoria Island part of Lagos which is the commercial capital of Nigeria. The hospital provides care in all fields of Internal Medicine, including its special expertise in Cardiology, with its own Coronary and Intensive Care Unit. It also provides Renal Dialysis, Obstetrics and Gynecology, Paediatrics and Paediatric Cardiology, Surgery (including Endoscopy and Day-case Surgery), Ophthalmology, ENT (Ear, Nose, and Throat) Surgery, Radiology, and Psychiatry. The hospital has facilities for inpatient and outpatient care.
Echocardiography was done according to the American Standard on Echocardiography using a 2-D echocardiography machine with facility for colored Doppler and M-mode. The Paediatric cardiologists performed the echocardiography on all the study subjects. Details concerning the patient’s biodata, clinical presentation, and echocardiographic diagnosis, and other relevant information were recorded prospectively.
Ethical approval for the study was obtained from the ethical committee of the Reddington multi-specialist hospital.
The data were analyzed using Microsoft Excel supplemented by the Statistical Package for Social Sciences (SPSS) version20. The children’s age, sex, indication for echocardiography and echocardiographic findings were represented in tables and charts. Descriptive statistics were presented as percentages or means and standard deviations. Means of normally distributed variables were compared using the Student T test and proportions using Chi-square test. The level of significance set at p<0.05.
Results
There were 210 ECHOs done on children in the pediatric cardiology clinic and inpatient facilities of Reddington Multi- Specialist Hospital during the study period. Seven of the patients enrolled in the study had to be excluded due to incomplete data, and 203 subjects were included in our analysis. The highest numbers of ECHOs were done in the year 2007.
The subjects ranged in age from three days to 256 months of age, with a mean age plus standard deviation of 59.4 +/- 64 months over the four-year period with a male to female ratio of 1: 1.1. Approximately 37 percent (77) of all the ECHOs done were normal. Males consisted of 45.5% of abnormal ECHOs, while females accounted for 54.5% of all abnormal ECHOs.
The most common indication for ECHO referrals was heart murmurs, found in 101(49.5%) of the referrals (Table 1). Seventyfive (84.3%) of ECHOs performed with murmur as the indication for echocardiography were abnormal while others were normal (p=0.001). The pre-operative evaluation was the indication for echocardiography in 10 (4.9%) of all the echocardiography done for specific referrals. Up to 20 percent of patients analyzed with preoperative echocardiograms for adenoidal hypertrophy had abnormal findings. Seven out of twelve patients evaluated by ECHO for obesity were diagnosed with Left Ventricular Hypertrophy; 58.3% (p = 0.64) as shown in Table 2.
| Indication | Number (percent) |
|---|---|
| Murmur | 89 (43.8) |
| Breathlessness | 15 (7.4) |
| CHD | 12 (5.9) |
| Obesity | 12 (5.9) |
| Cyanosis | 11 (5.4) |
| Post-up check | 11 (5.4) |
| Cough | 10 (4.9) |
| AdenoidalHypertrophy | 10 (4.9) |
| Chest pain | 8 (3.9) |
| Cardiomegaly on CXR | 4 (2) |
| Bradycardia | 3 (1.5) |
| Dysmorphism | 3 (1.5) |
| Others | 14 (6.9) |
| Total | 203 (100) |
Table 1: Indication forechocardiography.
| Indications | Normal (%) | Abnormal (%) | p |
|---|---|---|---|
| Murmur | 14 (15.7) | 75 (84.3) | 0.005 |
| ACHD | 7 (58.3) | 5 (41.7) | 0.64 |
| Recurrent cough | 4 (40.0) | 6 (60.0) | 0.6 |
| Cyanosis | 3 (27.3) | 8 (72.7) | 0.21 |
| FTT | 1 (50.0) | 1 (50.0) | 1 |
| Adenoidal hypertrophy | 8 (80.0) | 2 (20.0) | 0.11 |
| Chest pain | 9 (100) | 0 (0.0) | 0.009 |
| Cardioegaly on CXR | 10 (90.9) | 1 (9.1) | 0.021 |
| Obesity | 5 (41.7) | 7 (58.3) | 0.64 |
| Breathlessness | 1 (6.7) | 14 (93.3) | 0.004 |
| Bradycardia | 0 (0.0) | 3 (100) | 0 |
| Dysmorphism | 1 (33.3) | 2 (66.6) |
FTT: Failute to thrive
Table 2: Some indications for echocardiography and findings in terms of normal versus abnoral.
Details of abnormality found on echocardiography with murmur as an indication for the echocardiography are enumerated in Table 3. This included Tetralogy of Fallot, Atrial septal defects (ASD) and Ventricular septal defects (VSDs). VSDs being the most prevalent finding based on murmurs. Thirty-nine percent of the abnormal ECHOs were VSDs.
| Findings | Number (%) |
|---|---|
| VSD | 39 (30.7) |
| ASD | 26 (20.5) |
| TOF | 12 (9.5) |
| LVH | 12 (9.5) |
| AVSD | 10 (7.9) |
| PDA | 7 (5.5) |
| PS | 5 (3.9) |
| TGA | 3 (2.3) |
| Cor pulmonale | 3 (2.3) |
| RHD | 2 (1.6) |
| Others | 8 (6.3) |
| Total | 127 (100) |
ASD: Atrial Septal Defect PDA: PatentDuctusArteriosus
TOF: Tetralogy of Fallot PS: PulonaryStenosis
LVH: Left Ventricular Hypertrophy TGA: Transposition of the great arteries
RHD: Rheumatic Heart Disease
Others = (One case each of Pericarditis, Double outlet right ventricle, Aortic stenosis, Pulmonary Hypertension, Dextrocardia, Complex Cyanotic Congenital Heart Disease, Dilated Cardiomyopathy and A-P window)
Table 3: Abnormal echocardiographic findings.
All Patients whose indication for echocardiography was chest pain had normal findings. The indication with the highest percentage of abnormal findings was breathlessness, with just 14 cases, but 93.3% of all subjects referred for breathlessness revealed an anomaly on ECHO. Echocardiographic findings in subjects with breathlessness as an indication for echocardiography were Left Ventricular Hypertrophy (LVH), and Cor-Pulmonale, with LVH being more prevalent, with 79% of the abnormal studies revealing LVH.
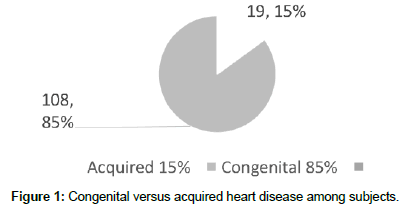
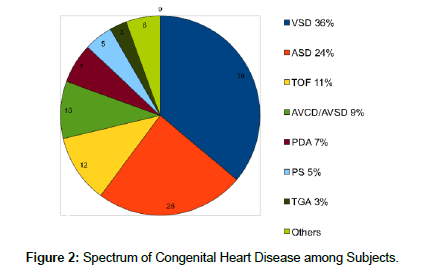
Congenital heart diseases constituted 108 (85%) of all the abnormal echocardiographic findings in this study (Figure 1). The most frequent congenital heart disease was Ventricular Septal defects (VSDs) in 39 (31%), followed by atrial septal defects (ASDs) in 21% (26) Tetralogy of Fallot (TOF) in 10% of the subjects with abnormal echocardiographic findings (Figure 2).
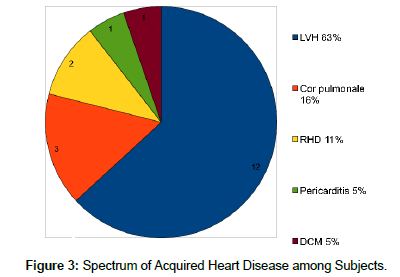
Acquired heart diseases were found in 15% of the cases with abnormal echocardiographic findings. Left ventricular hypertrophy was the most prevalent acquired finding, responsible for 12 (63%) of the acquired causes. Left ventricular hypertrophy was found in 10% of all the abnormal echocardiographic findings (inclusive of both acquired and congenital heart defects). Cor-Pulmonale was the second most prevalent acquired heart diagnosis, comprising approximately 16 percent [3] of these findings. Rheumatic Heart Disease (RHD) was found in two patients; about two percent of abnormal diagnoses and 10.5 percent of the acquired heart diseases found in this study (Figure 3).
Discussion
Cardiovascular disease has become a ubiquitous cause of morbidity and a leading contributor to mortality in most countries. It is now believed that at present the developing countries contribute a greater share of the global burden of cardiovascular disease than what is seen in developed countries [4].
Of the various diagnostic modalities, echocardiography remains the most readily available, non-invasive and highly diagnostic tool for assessing cardiac structure, function and hemodynamics in those with suspected cardiac disease [1]. Outlining appropriate indications for referral for this test in children may be more challenging for the general practitioner or pediatrician. Thus, appropriate use criteria were devised to assist in identifying appropriate indications for referral. Chest pain, syncope, and murmurs are considered the common indications for echocardiography, with murmurs quoted as the most common indication for echocardiogram referrals [1]. As was noted in our study, the most common reason for referral for echocardiography was heart murmurs with almost half of the referrals comprising this complaint. This goes along with findings in other studies; in a study comprising 209 subjects, 67% of referrals were made for heart murmurs [5]. As an indication for echocardiography, heart murmurs was shown to be high-yield as almost ninety percent of children who had echocardiography, due to auscultated heart murmurs had an abnormal finding. In another study on school children in Jos, out of 418 schoolchildren, four had heart murmurs, and three of those children with heart murmurs had pathologic heart murmurs. All three with pathologic heart murmurs were found to have congenital cardiac abnormalities [6]. This correlates with the AUC described, where murmurs score high on the appropriate use criteria spectrum, with only innocent murmurs without accompanying findings, standing as ‘Rarely appropriate’ for echocardiography, referrals without a preceding pediatric cardiologist’s assessment [1]. However this differs slightly within our demographic where the pediatric cardiologist is usually the echocardiographer, so that a referral for an echocardiogram is tantamount to a referral to the pediatric cardiologist, as opposed to the situation in most developed countries where echocardiograms may routinely be performed by echocardiographers who are not necessarily pediatric cardiologists as well, and pediatric cardiologists may even remotely read echocardiograms without necessarily evaluating the patients personally.
All patients evaluated by echocardiography for chest pain in our study had normal studies. This was similar to findings of Bensky, Wesley, & DuRant in a study evaluating the proficiency of primary care physicians (PCP’s) in determining appropriate echocardiography referrals, with 210 subjects studied, all indications for referral apart from murmur, including chest pain, revealed normal echocardiography [5] Campbell et al. [1] identified chest pain as relatively low-yield as an indication for referral for echocardiography. Criteria elevating chest pain to appropriate use included exertional chest pain, abnormal electrocardiogram, and family history of unexplained sudden death or cardiomyopathy [1] Our study, however, suggests that an echocardiography may not be the first best test for a complaint of chest pain, but it is still very important for ruling out possible and dangerous diagnoses after prudent, sequential work-up.
Our study demonstrated some significant findings in our patients referred for pre-operative evaluation before adenotonsillectomy for adenoidal hypertrophy and associated complications. Twenty percent of the patients referred for this indication had abnormal findings. This was not statistically significant, but it’s clinical relevance must be considered. Adenoidal hypertrophy causing upper airway obstruction can lead to cardiopulmonary complications such as pulmonary hypertension, right heart failure, and cor-pulmonale in children [7,8]. A study done on eighty children who underwent adenoidectomy showed statistically significant positive changes in echocardiography parameters of pulmonary artery pressure and right ventricular diastolic filling when pre-operative and postoperative echocardiography, on the subjects were compared [8]. This may suggest some reversibility in complication effect through the intervention of adenoidectomy.
Our results also highlighted specific findings associated with obesity with more than half of subjects evaluated for this indication having abnormal findings (58.3%). Out of twelve diagnoses of left ventricular hypertrophy, seven of these children were originally referred for obesity. While this was not statistically significant in our study, it is clinically significant to find such a high incidence. It is known that childhood obesity is predictive of adult obesity and is thus, associated with an increased risk of diabetes, hypertension, and hypercholesterolemia [9]. With the development of pulmonary consequences of obesity, some children may develop obesityhypoventilation syndrome and experience right-sided heart failure with right ventricular hypertrophy. Studies also show increased risk for dyslipidemia, and carotid-artery atherosclerosis in obese children [10]. Crowley et al. [11] study demonstrated a trend of higher BMIs in adolescents correlating with increases in left ventricular mass. Magner et al. [12] also conducted a study to assess geometric and functional changes of the heart in obese children compared with nonobese children and adolescents. They found thicker left ventricular (LV) walls and increased LV mass as well as impaired measures of systolic function, among obese children as compared with nonobese children [12]. Their study also showed impaired markers of LV longitudinal function among the obese children as assessed by 2D speckle-tracking echocardiography (2D-STE). These findings are similar to what we discovered in our study. All are emphasizing the significant impact of childhood obesity on cardiovascular outcome. Based on this we would recommend judicious surveillance in children with obesity, inclusive of blood pressures, and to consider screening echocardiograms to assess for LVH and prompt early preventative interventions.
Interestingly, there were only two diagnoses made of Rheumatic Heart Disease (RHD) in our study, suggesting a prevalence of approximately 0.99% in our study population. This is surprisingly high, considering the setting of our study. In other studies, lesser prevalence was discovered. Yilgwan’s and his colleagues [6] found no children with RHD, upon evaluation of 481 students; there was a 0% prevalence of RHD found in the students [6]. In 1972, Shaper described RHD as one of the commonest forms of heart disease in children and young adults in most tropical or developing countries, and as one of the most common cardiovascular diseases in adults [13]. Initial impressions were that the rheumatic fever (RF) and RHD appeared to be increasing. Risk factors of poor environmental hygiene, low socioeconomic standards, and lack of a comprehensive prophylactic program against streptococcal infections were cited as contributory to this rise [14]. However, a subsequent study by Ogunbi et al., concluding in 1978 showed an even lower incidence than ours at 0.08% with 11 cases found out of 12755 children screened [13]. A study in Jos on childhood acquired heart diseases (AHDs) by Bode-Thomas and her colleagues showed RHD to be the most common cause of all acquired heart diseases (AHD)s found at that institution comprising 57.7% of all AHDs found; a prevalence of 17.4% for that study population, considerably higher than most other studies [15]. Sadoh et al. did a study on 1764 primary school pupils in Edo state which showed a prevalence of 0.57/1000 pupils; showing a relatively lower RHD prevalence [16]. Danbauchi et al. published a study in 2003 looking at RHD in Zaria, showing 47 of subjects of all ages found to have RHD out of 600 echocardiograms done in that ECHO lab; a prevalence of 7.8% [17]. There seems to be a geographical variation in the spread of RHDs, with northern states appearing to have a higher prevalence. The prevalence of rheumatic heart disease is usually associated with socioeconomic status, with a directly proportional relationship between poverty and high RHD rates. However, we are surprised to find higher numbers within our urban population. A structural heart disease study done in 2005 in Lagos by Okoromah et al. showed that CHDs seemed to outnumber AHDs as heart diagnoses in children 4weeks-15 years of age [18]. The study also recorded pericarditis with effusion as the commonest cause of AHD comprising 31% of AHDs as compared to RHD which was responsible for 28.6% of diagnoses [18]. Comparatively, our study showed CHDs to significantly outnumber AHDs with CHDs accounting for 85% of diagnoses, as compared to 15% of our diagnoses as AHDs as seen in Figure 1. In our study, RHDs accounted for 11% of AHDs, ranking third in these diagnoses (Figure 2). Unlike other studies, ours seems to highlight other AHDs not commonly focused upon such as LVH and cor-pulmonale. The significance of this may be seen in the fact that a possible relationship is elucidated between LVH and obesity allowing us to consider the possible impact of Westernization, globalization, and influx of diseases seen more in developed countries, as a factor in AHDs, especially considering our demographic in an urban environment with a likely higher socioeconomic population.
In assessing probabilities for congenital heart disease, one of the criteria used is the Nadas criteria. The Nadas criteria identifies auscultatory findings as one of the strongest indicators of possible congenital heart disease comprising three of the four major criteria, and one of the five minor criteria. Abnormal ECGs, chest x-ray findings, abnormal blood pressures, and congestive heart failure comprise the other possible criteria. Abnormal ECG findings were also statistically significant, in our study, as an indicator for echocardiography referral. Thus, Nadas criteria may also be used to determine appropriate indicators for referrals for ECHO studies.
It is accepted that congenital heart diseases account for 8-12/1000 live births in developing countries (6), with an estimated incidence of 3.5/1000 in a much older study in Nigeria [19]. The disease burden in Nigeria becomes more meaningful when related to the birth rate in the country [20]. With the almost recent birth rate at 40/1000 as quoted by the World Bank from statistics reflecting 2013 [21], and a population of 173.6 million; approximately 6.9 million births occur annually. Congenital heart malformations may be found in up to 24,304 newborns across Nigeria annually. This burden becomes even more concerning when barriers to diagnosis, and correction, if necessary, are analyzed [20].
In our study the commonest cardiac diagnosis via ECHO was Ventricular septal defect (VSD) with 30% of diagnoses comprising this diagnosis. In a study done on subjects of all ages in Kano, VSD was the most prevalent congenital heart disease diagnosis; found in 45.9% of the patients [22]. Kolo et al. study in Ilorin similarly manifested VSDs as the most common diagnosis in studied subjects [23], as was also found in Chinawa et al. study in Enugu, where it was found in almost twenty percent of diagnoses [24]. A nine-year study in University of Benin Teaching Hospital (UBTH) also found VSDs as the most frequent defect at 55.1% in studied subjects [25]. However, this is not a new finding, as VSDs are known to be the commonest congenital heart defect globally, with cited incidence of 1.5-3.5 per 1000 live births [26]. In Nigerian hospital based audits, 35-55% of CHDs were found to be VSDs, while in the comprehensive collation of Nigerian echocardiography, lab data, the incidence was found to be at 28-46% [26]. This is significant as VSDs are also the most common CHD causing heart failure in childhood [26]. Spontaneous closure is the expected natural history in small and muscular VSDs, with spontaneous closure rates of up to 45.9% in a 3 years UBTH VSD study in 2010 [26]. However, large and non-muscular VSDs present a dilemma for the Nigerian pediatric cardiologist due to the lack of surgical capabilities for palliation and affordable options for transcatheter closures if appropriate [26]. The afore-mentioned study showed a mortality of 3.3% in patients with VSDs, who did not access surgical or interventional resolutions. Only 4.9% of the subjects in the study, with large VSD, were able to afford surgical closure before 2 years of life [26]. Initiatives to provide affordable centers for surgical palliations for children with significant VSDs would be beneficial to ameliorate the disease burden caused by VSDs and pre-empt the complication of heart failure for which the defect is noted.
ASDs were the second most common echocardiography finding. This was consistent with findings in the Ilorin study seen in 21% of patients [23], but contrasted with findings in Kano and University of Nigeria Teaching Hospital (UNTH) Enugu, where the findings were of TOF as the second most prevalent finding in their ECHO studies seen in 26.2%, and 12.7% respectively (22,24). In Yilgwan’s study, ASD was the only CHD found out of three children with abnormal heart echocardiography, making it the second most prevalent finding in that study as well [6].
TOF tied with LVH as the third most common echocardiography diagnosis in our study, comprising 10% of diagnoses. TOF is the most common cyanotic heart lesion beyond the neonatal period. Usually with a prevalence of 5 out of every 10,000 babies. Okoromah et al. study in 2008 of structural heart diseases revealed VSDs as most common CHD, followed by ASDs, and followed by TOF at 11.8% relative frequency [18]. A TOF study concluded in December 2014 in Lagos showed a prevalence of 4.9 per 10,000, similar to the expected prevalence [27]. The natural history of TOF reports a mortality rate approaching 50% in untreated patients, ranging from 30% at age two years, to 50% if still untreated by the age of 6 years. Only about 20% of patients can be expected to reach the age of 10 years [28]. In our study country, there is limited access to the curative surgery needed. These pediatric heart operations are not being done regularly in the country, thus, getting our patients to this vital care requires formidable means both for travel to an outside location, as well as to undergird the costs of the surgical procedure itself [29]. Establishment of cardiac centers where the surgeries can be done within Nigeria to undercut costs would be invaluable and go a long way to decreasing the burden of this problem and potential mortality for patients with this diagnosis.
Conclusion
Establishing criteria for referral for ECHO studies is an important endeavor to enable us appropriately manage resources and become more deliberate in our performance of studies while building our clinical diagnostic skills. Our findings in this study seem to fall in line with the appropriate use criteria for indications of heart murmurs.
Pre-operative echocardiograms for patients with adenoidal hypertrophy showed significant findings suggesting clinical relevance. Our study showed a high incidence of LVH in patients evaluated via echocardiogram for obesity. Our data on RHDs showed intermediate prevalence, yet relatively high considering our demographic and concomitant expectation for our socioeconomic group. More recent studies show a higher prevalence, however, with a possible geographic disparity in the prevalence in Nigeria. More Westernized impact is seen in penetration of diseases grouped under AHDs. More extensive studies would be needed to fully elucidate this possible phenomenon.
Our study showed the similar distribution in congenital heart diseases as compared to other studies both in private and public settings, as well as developed countries compared to developing nations. Ventricular septal defects were found to be the most prevalent. Possibly the most outstanding theme is the need for more resources to meet the heart disease burden, along with ways to improve access to care as well as the availability of surgical palliations for complex heart defects to improve mortality and morbidity experienced in this part of the world.
Acknowledgements
We gratefully acknowledge subjects described in this study, their parents, caregivers and other healthcare staff involved in their care.
Conflict of Interest
No conflict of interest among the authors.
References
- Campbell RM, Douglas PS, Eidem BW (2014) ACC/AAP/AHA/ASE/HRS/SCAI/SCCT/SCMR/SOPE 2014 Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology. J Am Soc Echocardiogr 27: 1247-1266.
- Edler I, Hertz CH (2004) The use of ultrasonic reflectoscope for the continuous recording of the movements of heart walls. Clin Physiol Funct Imaging 24: 118-136.
- Uwanuruochi K, Offia E, Ukpabi OJ (2015) Initial experience with echocardiography at the federal medical center, Umuahia, Nigeria Nig J Cardiol 12: 13-17.
- Reddy KS, Yusuf S (1998) Emerging epidemic of Cardiovascular Disease in Developing Countries. Circulation97: 596-601.
- Bensky AS, Wesley C, DuRant RH (1999) Primary Care Physicians' Use of Screening Echocardiography. Pediatrics 103.
- Yilgwan CS, Ige OO, Bode-Thomas F (2014) Clinical screening for heart disease in apparently healthy Nigerian school children. Nig J Cardiol11: 74-79.
- Tezer MS, Karanfil A, Aktas D (2005) Association between adenoidal-nasopharyngeal ratio and right ventricular diastolic functions in children with adenoid hypertrophy causing upper airway obstruction. Int J Pediatr Otorhinolaryngol 69: 1169-1173.
- Abdel-Aziz M (2011) Asymptomatic cardiopulmonary changes caused by adenoid hypertrophy. J Craniofac Surg 22: 1401-1403.
- Ogden CL, Yanovski SZ, Carroll MD (2007) The epidemiology of obesity. Gastroenterology 132: 2087-2102.
- Juonala M, Magnussen CG, Berenson GS (2011) Childhood adiposity, adult adiposity, and cardiovascular risk factors. N Engl J Med 365: 1876-1885.
- Crowley D, Khoury P, Urbina E (2011) Cardiovascular Impact of the Pediatric Obesity Epidemic: Higher Left Ventricular Mass is Related to Higher Body Mass Index. J Pediatr 158: 709-714e1.
- Mangner N, Scheuermann K, Winzer E (2014) Myocardial changes in childhood obesity. JACC Cardiovasc Imaging 7: 1198-1205.
- Ogunbi O, Fadahunsi HO, Ahmed I (1978) An epidemiological study of rheumatic fever and rheumatic heart disease in Lagos. J Epidemiol Community Health 32: 68-71.
- Antia AU, Reddy S (1971) Rheumatic heart disease in children in developing countries. Ghana Med J 10: 9-13.
- Bode-Thomas F, Ige OO, Yilgwan C (2013) Childhood acquired heart diseases in Jos, north central Nigeria. Niger MedJ 54: 51-58.
- Sadoh WE, Omuemu VO, Israel-aina YT (2013) Prevalence of Rheumatic Heart Disease among primary school pupils in Mid-Western Nigeria. East Afr Med J 90: 28-32.
- Danbauchi SS, Alhassan MA, David SO (2004) The spectrum of rheumatic heart diseases in Zaria, Northern Nigeria. Annals Afr Med. 3: 17-21.
- Okoromah CA, Ekure EN, Ojo OO (2008) Structural heart disease in children in Lagos: profile, problems and prospects. Niger Postgrad Med J 15: 82-88.
- Gupta B, Antia AU (1967) The incidence of Congenital Heart Disease in Nigerian Children. Br Heart J 29: 906-909.
- Jaiyesimi F (1982) Congenital Cardiac Malformations: A Serious Health Problem in Nigeria. Niger J Paediatr 9: 67-70.
- World Bank Data (2016) Nigeria.
- Sani MU, Mukhtar-Yola M, Karaye KM (2007) The spectrum of Congenital Heart Disease in a Tropical Environment: An Echocardiography study. J Natl Med Assoc 99: 665-669.
- Kolo PM, Adeoye PO, Omotoso AB (2012) The pattern of Congenital Heart Disease in Ilorin, Nigeria. Niger Postgrad MedJ 19: 230-234.
- Chinawa JM, Eze JC, Obi I (2013) Synopsis of congenital cardiac disease among children attending University of Nigeria Teaching Hospital Ituku Ozalla, Enugu. BMC Res Notes 6: 475.
- Ibadin MO, Sadoh WE, Osarogiagbon W (2005) Congenital Heart Diseases at the University of Benin Teaching Hospital. Niger J Paediatr 32: 29-32.
- Sadoh WE (2010) Natural history of ventricular septal defects in Nigerian children. SA J of Child Health 4: 16-19.
- Animasahun BA, Madise-Wobo AD, Omokhodion SI (2015) Children with Tetralogy of Fallot in an Urban Centre in Africa. J Cardiovasc Thorac Res 7: 168-171.
- Bhimji S (2015) Tetralogy of Fallot. Medscape.
- Falase B, Sanusi M, Majekodunmi A (2013) Open heart surgery in Nigeria; a work in progress. J Cardiothorac Surg 8: 1-9.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi