Research Article, Int J Cardiovasc Res Vol: 7 Issue: 4
Hypertension and Associated Factors in Brazilian Adult Population: National Health Survey-2013
Patrícia de Menezes Marinho1*, Risia Cristina Egito de Menezes1, Sabrina Joany Felizardo Neves1, Alfredo Dias de Oliveira-Filho1, Vanessa Sá Leal2, Juliana Souza Oliveira2, Giovana Longo-Silva1, Maria Alice Araújo Oliveira1, Emília Chagas Costa2and Francisco de Assis Costa1
1Federal University of Alagoas, Alagoas, Brazil
2Federal University of Pernambuco, Pernambuco, Brazil
*Corresponding Author : Patrícia de Menezes Marinho
Faculty of Nutrition, Federal University of Alagoas, Avenida Lourival Melo Mota, s / n - Tabuleiro dos Martins. CEP 57072-900 - Maceió / AL, Brazil
Tel: (82) 3412-1166
E-mail: patricia_mmarinho@hotmail.com
Received: May 25, 2018 Accepted: August 09, 2018 Published: August 14, 2018
Citation: Marinho PdM, Menezes RCED, Neves SJF, Oliveira-Filho ADD, Leal VS, et al. (2018) Hypertension and Associated Factors in Brazilian Adult Population: National Health Survey-2013. Int J Cardiovasc Res 7:4. doi: 10.4172/2324-8602.1000359
Abstract
Background: Hypertension is an important public health problem in Brazil, and has been affecting individuals of different ages and social strata.
Objective: To determine the prevalence of hypertension and its associated factors in Brazilian adult population.
Methods: Cross-sectional study involving Brazilian adults aged 18 years and older. Data were obtained from the National Health Survey conducted in 2013. A multistage sampling method was used to select a national representative sample of the Brazilian population. The selected sociodemographic variables studied were: sex, age, race, marital status and education level. Behavioral variables included physical activity, smoking status, self-perceived health status and reported salt intake self-perceived. Body Mass Index calculated from weight and height values obtained during household visits. Comorbidities diabetes type 2, high blood cholesterol, cardiovascular diseases, stroke and chronic renal failure were assessed by self-report.
Results: Hypertension increased with age in both sexes, and the men were more likely than women to have that disease in all age categories analyzed. Male sex, older age, not living with partner, low educational level, physically inactive, smoking, overweight, diabetes type 2 and high blood cholesterol were associated with hypertension.
Conclusion: These results reinforce the need for adoption and implementation of measures, based on strategies for prevention, treatment and control of hypertension, still present in expressive way in Brazil and different parts of the world.
Keywords: Hypertension; Prevalence; Mortality; Morbidity; Adult; Brazil
of undiagnosed, untreated and uncontrolled people with hypertension usually common in weak health systems [1,2].
It is estimated that CVD will become the leading cause of death and disability, globally, by 2020 [3]. The trend of increasing hypertension prevalence seems to prevail among developing countries. In Latin America, the prevalence of hypertension-given the broad diversity of the region-ranges from 13.4 to 45.5%, and this rates are likely to triple by 2030 [4-6].
In 2013 in Brazil, the study found that the prevalence of adults with high blood pressure was 22.8%, higher in men (25.8%; 95% CI: 24.8-26.7) than in women (20.0%; 95% 19.3-20.8%) [7]. According to the 2010 national census, of the 190 million people in Brazil (130 million adults), 160 million live in urban areas while 30 million live in rural areas [8]. Nowadays the Brazilian population is estimated to be of more than 202 million [9] and once rapid unplanned urbanization is one of the main factors that contribute to the development of hypertension and its complications, extensive and updated data about the prevalence of hypertension and its associated factors would be of urgent public health importance, especially due to an exponential increase in the CVD burden [1].
Thus, considering the complexity, multi-causality, and that the available data on hypertension in 2013 until then refer to the prevalence, and considering that the factors associated with the disease have not yet been adequately elucidated in this population, the deepening and understanding of these predictors constitute justification for this work. In this way, this study aimed to determine the prevalence of hypertension and its associated factors in Brazilian adult population.
Methods
This is a cross-sectional population-based study involving Brazilian adults aged 18 years and older. Data were obtained from the National Health Survey, a nationally representative household survey conducted by the Brazilian Institute of Geography and Statistics (IBGE) and Ministry of Health in 2013 [10]. A multistage sampling method was used to select a national representative sample of the Brazilian population. The primary sampling units were census tracts based on the 2010 census and randomly selected from the IBGE national master sampling plan. Within each census tract households were randomly selected from a national registry of addresses. Within selected households a randomly selected respondent aged 18 years or older was invited to take part in the survey.
Initially, 79,875 households were selected. Upon completion of data collection, the final sample size was 64,348 households with an overall response rate of 78%. Person-level survey weights were calculated taking into account the probability of selection as well as non-response rates. For the purpose of this study, the data of adults selected within each domicile to answer the individual interview and whose blood pressure was measured were analyzed. Thus, our sample consisted of 59.402 individuals.
Respondents were classified as having hypertension if systolic blood pressure measurement of ≥ 140 mmHg or a diastolic measurement of ≥ 90 mmHg (n=12.662 adults). Blood pressure was measured by trained professionals using a properly calibrated automatic device. Details on the procedures performed in the measurement of blood pressure can be found in previous publication [11].
The selected sociodemographics variables studied were sex, age, race, marital status and education level. Behavioral variables included physical activity (inactive, <10 min/wk; insufficient, 10–149 min/ wk; active, ≥150 min/wk of moderate-intensity equivalent physical activity); smoking status (current, former, none); and evaluation health status (very good, good, regular, bad, too bad) and reported salt intake (very low, low, appropriate, high, very high) were ascertained by self-perceived. Body Mass Index (BMI) calculated from weight and height values obtained during household visits. Overweight, categorized as yes and no, was assessed according to BMI cut-off points. In the individuals aged between 18 and 59 years, the values ≥ 25 kg/m2 were considered overweight [12]. For those aged 60 or over [13], we considered values>27 kg/m2. Diabetes type 2, high blood cholesterol, cardiovascular diseases, stroke, chronic renal failure, were ascertained by self-report.
Statistical analysis
In all of the analyses, the effects of complex sampling were considered. First, we described participant characteristics by weighted frequencies. Hypertension prevalence in the population was then calculated at a 95% confidence interval (CI). To identify factors related to hypertension prevalence, we calculated prevalence ratio (PR) using bivariate analysis and calculated the adjusted PR by a multiple regression of Poisson model with robust variance. In this model, all of the variables were analyzed simultaneously. We preferred to use this more conservative model that included all of the variables to allow for better confounding adjustment. Other models that included only the most significant variables were tested and did not change the significance of the variables. Associations were considered to be statistically significant when p<0.05. The STATA software version 13.0 was used for all of the calculations.
Ethical Aspects
The National Health Survey-2013 was approved by the Brazilian National Commission on Ethics in Research (CONEP) of the National Health Council (CNS). All participants signed a term of free and informed consent.
Results
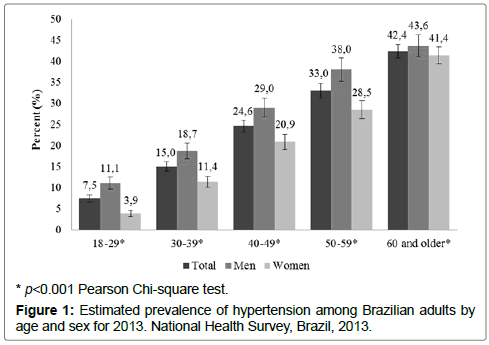
In 2013, hypertension increased with age for both sexes, being that Brazilian men were more likely than women to have hypertension in every age category. The difference in the prevalence of hypertension between men and women increased with age (with the exception of the 60 and over age group where rate were 2.2%), from 7.2% among those aged 18-29, to 7.3% among those 30-39, to 8.9% among those 40-49, to 9.5% among those 50-59 (Figure 1).
The prevalence of hypertension was also significantly higher among black adults (27.5%, 95% CI 25.48-29.63, p<0.001), and among married or living as if married individuals (23.7%, 95% CI 20.33- 22.23, p<0.001). Among the Brazilian population, there is an inverse association between schooling and hypertension: while than 24% (95% CI 22.71-25.35, p<0.001) of the individuals with 5-8 schooling years and more reported having hypertension, the same condition was observed among 40.8% (95% CI 38.88-42.79, p<0.001) of the adults with up to 4 years of schooling (Table 1).
| Variables | Total | Hypertension | (CI 95%)2 | p value** | ||
|---|---|---|---|---|---|---|
| N1 | %² | n1 | %2 | |||
| Sociodemographics | ||||||
| Age groups, years | <0.001 | |||||
| 18-29 | 13,822 | 25.7 | 901 | 7.5 | (6.75-8.43) | |
| 30-39 | 14,003 | 21.5 | 1,846 | 15.0 | (13.92-16.11) | |
| 40-49 | 11,370 | 18.2 | 2,622 | 24.6 | (23.18-26.08) | |
| 50-59 | 9,030 | 16.4 | 2,786 | 33.0 | (31.26-34.8) | |
| ≥ 60 | 11,177 | 18.2 | 4,507 | 42.4 | (40.74-44.03) | |
| Race/ethnicity * | <0.001 | |||||
| Asian | 525 | 0.9 | 110 | 23.3 | (17.49-30.43) | |
| Latin | 29,066 | 42.0 | 5,901 | 21.8 | (20.81-22.78) | |
| Native Americans | 412 | 0.4 | 78 | 18.6 | (13.15-25.66) | |
| White | 23,828 | 47.5 | 5,208 | 22.7 | (21.76-23.74) | |
| Black | 5,568 | 9.2 | 1,364 | 27.5 | (25.48-29.63) | |
| Marital status | <0.001 | |||||
| Not living with partner | 25,507 | 39.0 | 5,713 | 21.3 | (20.33-22.23) | |
| Living with partner | 33,895 | 61.0 | 6,949 | 23.7 | (20.33-22.23) | |
| Education level, years* | <0.001 | |||||
| ≤ 4 | 7,624 | 16.1 | 2,927 | 40.8 | (38.88-42.79) | |
| 5-8 | 15,068 | 29.7 | 3,387 | 24.0 | (22.71-25.35) | |
| 9-11 | 18,237 | 37.5 | 2,896 | 16.9 | (15.91-17.99) | |
| >11 | 8,474 | 16.6 | 1,358 | 18.0 | (16.54-19.54) | |
| Behavioral aspects | ||||||
| Self-perceived health status | <0.001 | |||||
| Very good | 7,315 | 13.2 | 1,108 | 14.8 | (13.3-16.35) | |
| Good | 31,188 | 52.7 | 5,780 | 20.4 | (19.57-21.3) | |
| Regular | 17,052 | 28.2 | 4,572 | 28.9 | (27.58-30.22) | |
| Bad | 3,084 | 4.7 | 960 | 32.0 | (29.06-35.01) | |
| Too bad | 763 | 1.2 | 242 | 34.6 | (28.93-40.79) | |
| Self-perceived salt intake | <0.001 | |||||
| Very low | 1,848 | 2.9 | 604 | 32.4 | (28.45-36.66) | |
| Low | 14,053 | 22.5 | 3,830 | 28.7 | (28.45-36.66) | |
| Appropriate | 35,450 | 60.5 | 6,675 | 20.5 | (19.69-21.36) | |
| High | 6,977 | 12.3 | 1,365 | 21.4 | (19.85-23.13) | |
| Very high | 1,074 | 1.9 | 188 | 18.0 | (14.56-21.93) | |
| Physical activity | <0.001 | |||||
| Yes | 17,799 | 31.7 | 2,901 | 17.7 | (24.33-25.95) | |
| No | 41,603 | 68.3 | 9,761 | 25.1 | (16.69-18.7) | |
| Smoking | <0.001 | |||||
| No | 50,716 | 85.2 | 10,522 | 22.1 | (21.43-22.79) | |
| Yes | 8,686 | 14.8 | 2,140 | 26.5 | (24.74-28.43) | |
CI 95%- 95% confidence interval.
1Number of subjects in the non-weighted sample;
2Prevalence and 95% confidence intervals (CI 95%) calculated under weights due to the sampling design;
* The totals differ due to losses in the variable;
** p value of Pearson Chi-square test.
Table 1: Sociodemographics and behavioral characteristics, comorbidities and prevalence rate of hypertension among Brazilian adults. National Health Survey, Brazil,2013.
The prevalence of hypertension was significantly high (p<0.001) among individuals with bad (32.0%, 95% CI 29.06-35.01) or too bad (34.6%, 95% CI 28.93-40.79) self-perceived health status. Behavioral associated factors for self-reported hypertension such as being physically inactive was more likely to be identified among hypertensive patients (p<0.001). However, it was observable higher prevalence of high blood pressure among adults who reported selfperception of very low salt consumption. Cigarette smoking was significantly associated with hypertension in the bivariate analysis (Table 1).
Overweight individuals had a higher prevalence of hypertension (26.9%, 95% CI 26.0-27.86 vs 17.9%, 95% CI 17.12 to 18.74, p<0.001). Overweight was significantly higher (p<0.001) in women compared to men (55.0%, 95% CI 54.01-56.03 vs 52.5%, 95% CI 51.29-53.63). Diabetes type 2, high blood cholesterol, cardiovascular diseases, stroke and chronic renal failure, were significantly associated (p<0.001) with hypertension (Table 1).
In the multivariate analysis, male sex, older age, not living with partner, low educational level, physically inactive, smoking, overweight, diabetes type 2 and high blood cholesterol remained associated with hypertension (Table 2).
| Variables | Total | Hypertension | (CI 95%)2 | p value** | ||
|---|---|---|---|---|---|---|
| N1 | %2 | n1 | %2 | |||
| Comorbidities | ||||||
| Overweight* | <0.001 | |||||
| No | 27,381 | 46.2 | 4,715 | 17.9 | (17.12-18.74) | |
| Yes | 32,021 | 53.8 | 7,947 | 26.9 | (26.0-27.86) | |
| Diabetes type 2* | <0.001 | |||||
| No | 48,660 | 92.9 | 9,971 | 21.8 | (21.13-22.58) | |
| Yes | 3,628 | 7.1 | 1,411 | 42.2 | (39.25-45.11) | |
| High blood cholesterol* | <0.001 | |||||
| No | 43,567 | 85.3 | 9,031 | 21.9 | (21.13-22.6) | |
| Yes | 7,266 | 14.7 | 2,128 | 32.9 | (30.87-35.07) | |
| Cardiovascular diseases | <0.001 | |||||
| No | 57,174 | 95.8 | 11,989 | 22.4 | (21.77-23.13) | |
| Yes | 2,228 | 4.2 | 673 | 30.0 | (27.11-33.14) | |
| Stroke | <0.001 | |||||
| No | 58,436 | 98.5 | 12,291 | 22.5 | (21.81-23.15) | |
| Yes | 966 | 1.5 | 371 | 41.3 | (35.53-47.35) | |
| Chronic renal failure | <0.001 | |||||
| No | 58,566 | 98.6 | 12,415 | 22.6 | (21.98-23.34) | |
| Yes | 836 | 1.4 | 247 | 30.5 | (25.53-35.92) | |
1PR: prevalence ratios calculated under weights due to the sampling design;
2CI 95%: 95% confidence intervals (CI 95%) calculated under weights due to the sampling design;
*Adjusted for all other variables in the table
Table 2: Multiple regression of Poisson to hypertension among Brazilian adults, according to sociodemographics, behavioral and comorbidities. National Health Survey, Brazil, 2013.
Discussion
The prevalence of hypertension observed in Brazil in 2013 is similar to the prevalence rates of self-reported hypertension observed in the period between 2006 and 2011 in Brazil [4]. In the 2000’s, the pooled prevalence estimates of self-reported hypertension in Brazil obtained through home surveys was 25.2% [14]. In a study aimed to compare hypertension prevalence in seven major Latin American cities, the overall weighted prevalence of hypertension was 16.3%, ranging from 13.4% to 44.2%, while the prevalence of self-reported hypertension was 32.8% in the United States in 2011 among adult individuals [5,15]. The prevalence observed in our study was similar to that described in nationwide studies [16-18].
The prevalence of hypertension by the analyzed sociodemographic characteristics was higher among those aged ≥ 60 years, and among black adults, men, married or living as if married individuals, and among people with low educational levels. The prevalence of hypertension has increased with age in both sexes and was higher in men than in women at all ages. This difference increased with age. Since global prevalence of overweight is higher among women than men [19], we assessed the association between overweight and sex. Similarly, our study shows that overweight was more prevalent among women than men. Multivariate regression analysis also showed that diabetes type 2 and high blood cholesterol were significantly associated with hypertension. Overall, most of the present study’s findings align with several epidemiological studies that have revealed an association between hypertension sociodemographic, clinical, and lifestyle factors [18,20-22].
We also found a significant inverse linear relationship between self-perceived consumption of salt and hypertension prevalence rate in Brazil, but this relationship was not maintained in the final model. Still, draws attention the fact that traditionally, high salt intake has been identified as a risk factor for the occurrence of hypertension, and that the current guidelines [23,24] and several studies [25,26] are categorically recommend a low salt intake as a way to reduce blood pressure. It is worth noting that hypertension is considered a lifestyle disease, and the success of your treatment is directly related to accession lifestyle guidelines recommended by health professionals. In a study with 10.773 adults-designed to assess adherence to lifestyle recommendations by individuals who were aware of their hypertension-Kim and Kong noted that reducing salt intake was only slightly higher among those aware of their condition status [27- 29]. Thus, we believe that the inverse association similar between a associated factor of hypertension and its prevalence observed in our study suggests a change in the pattern of behavior motivated by diagnosis or awareness of the disease, in addition to knowledge of the implications of the lifestyle of hypertensive patients on the clinical manifestations of the disease. Thus, monitoring of the health service and the perception of hypertension appear to have led to a reduction in self-perceived daily salt consumption. Although previous studies have shown that better control of blood pressure reflects improvements in awareness of hypertension and lifestyle changes may be associated with newly diagnosed hypertensive patients, reductions of the entire population in daily salt consumption among hypertensive patients were not commonly reported in the literature.
Additionally, we verified that the self-perceived health despite having been significantly associated with hypertension in the bivariate analysis, this relationship also did not remain in the final explanatory model. As an independent predictor of mortality, poor self-perceived health status can lead to a lower engagement in preventive health practices and disease treatment [30]. In addition, changes in selfreported health can induce life-style changes which may have a delayed effect on health. Harrington and his colleagues found that the food quality is influenced by the core life behaviors and poor general state of self-perceived health is associated with poor-quality diet [31], which is contrary to the results observed when self-perceived consumption of salt. However, as this study looked at self-perceived consumption of salt intake, it may be that individual perception simply plays the medical discourse, not representing the total real consumption practiced by individuals.
Our study had limitations. For example, the cross-sectional design does not allow establishing cause and effect relationships, which makes it difficult to assess whether the factors identified as associated with hypertension are a consequence of preceded by the occurrence of the disease. Therefore, it is suggested to carry out studies with longitudinal drawings, in order to establish the temporal relationship among causal factors and the study outcome. In addition, it should be noted that although the procedures were standardized and the professionals trained, blood pressure measurement was performed using a digital automatic device, not traditional stethoscope [32,33]. Regarding self-reported morbidities, it is known that this method may result in an underestimation of the prevalence of injuries among individuals, however self-report morbidity remains one of the most widely used methods in clinical and public health research, and it has been found to be significantly associated with important outcome measures such as mortality, general health status, physical well-being, emotional well-being, among others [30,34].
Conclusion
Overall, hypertension is prevalent in about one-fifth of Brazilian adults, and being more predominant in men. The factors that presented a consistent association and greater chance of disease were: male sex, older age, not living with partner, low educational level, physically inactive, smoking, and overweight, diabetes type 2 and high blood cholesterol. These results reinforce the need for adoption and implementation of measures, based on strategies for prevention, treatment and control of hypertension in various sectors, which contribute to promotion and maintenance of healthy, lifestyles, as well reducing the burden of disease and complications, still present in expressive way, in Brazil and different parts of the world.
Funding
The National Health Survey was funded by the Ministry of Health (MS) and executed by Brazilian Institute of Geography and Statistics (IBGE). The author PM receives scholarship from Fundacao de Amparo à Pesquisa do Estado de Alagoas (FAPEAL).
Conflict of Interests
The authors declare no conflicts of interest.
References
- World Health Organization (2013) A global brief on hypertension: silent killer, global public health crisis. Geneva, Switzerland.
- Campbell NR, Lackland DT, Niebylski ML (2014) High blood pressure: why prevention and control are urgent and important: a 2014 fact sheet from the World Hypertension League and the International Society of Hypertension. J Clin Hypertens (Greenwich) 16: 551-553
- Abegunde DO, Mathers CD, Adam T, Ortegon M, Strong K (2007) The burden and costs of chronic diseases in low-income and middle-income countries. Lancet 370: 1929-1938.
- Andrade SS, Malta DC, Iser BM, Sampaio PC, de Moura L (2014) Prevalence of self-reported arterial hypertension in Brazilian capitals in 2011 and analysis of its trends in the period between 2006 and 2011. Rev Bras Epidemiol 17: 215-226.
- Hernández-Hernández R, Silva H, Velasco M, Pellegrini F, Macchia A, et al. (2010) Hypertension in seven Latin American cities: the Cardiovascular Risk Factor Multiple Evaluation in Latin America (CARMELA) study. J Hypertens 28: 24-34.
- Pramparo P (2002) The epidemiology of hypertension in South America. J Hum Hypertens 16: S3-S6.
- Malta DC, Santos NB, Perillo RD, Szwarcwald CL (2016) Prevalence of high blood pressure measured in the Brazilian population, National Health Survey, 2013. Sao Paulo Med J 134:163-70.
- Brazilian Institute of Geography and Statistics (2013) Atlas of the demographic census 2010. Rio de Janeiro: IBGE. Brazil
- Instituto Brasileiro de Geografia e Estatística (2014) Estimativas da população residente no Brasil e unidades da federação com data de referência em 1º de julho de 2014
- Instituto Brasileiro de Geografia e Estatística (2013) Ministério da Saúde. Pesquisa Nacional de Saúde - PNS 2013: percepção do estado de saúde, estilos de vida e doenças crônicas. Rio de Janeiro: IBGE.
- Instituto Brasileiro de Geografia e Estatística. Ministério da Saúde. Instituto Brasileiro de Geografia e Estatística. Pesquisa Nacional de Saúde: 2013. Ciclos de Vida. Brasil e grandes regiões. Rio de Janeiro: IBGE; 2015
- World Health Organization (1995) Physical status: The use and interpretation of anthropometry. Geneva, Switzerland.
- The Nutrition Screening Initiative (1994) Incorporating nutrition screening and interventions into medical practice: a monograph for physicians. Washington D.C. US: American Academy of Family Physicians, The American Dietetic Association, National Council on Aging Inc.
- Picon RV, Fuchs FD, Moreira LB, Riegel G, Fuchs SC (2012) Trends in Prevalence of Hypertension in Brazil: A Systematic Review with Meta-Analysis. PLoS One 7: 1-10.
- Fan AZ, Strasser SM, Zhang X, Fang J, Crawford CG (2015) State Socioeconomic Indicators and Self-Reported Hypertension Among US Adults, 2011 Behavioral Risk Factor Surveillance System. Prev Chronic Dis 12: 1-8.
- Li D, Lv J, Liu F, Liu P, Yang X, et al. (2015) Hypertension burden and control in mainland China: Analysis of nationwide data 2003-2012. Int J Cardiol 184: 637-644.
- Kim HJ, Ki Y, Cho Y, Jun B, Oh KW (2014) Trends in the prevalence of major cardiovascular disease risk factors among Korean adults: results from the Korea National Health and Nutrition Examination Survey, 1998-2012. Int J Cardiol 174: 64-72.
- Gao Y, Chen G, Tian H, Lin L, Lu J, et al. (2013) Prevalence of hypertension in China: a cross-sectional Study. PLoS One 8: 1-8.
- Ng M, Fleming T, Robinson M, Thomson B, Graetz N, et al. (2014) Global, regional, and national prevalence of overweight and obesity in children and adults during 1980-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 384: 766-781.
- El Bcheraoui C, Memish ZA, Tuffaha M, Daoud F, Robinson M, et al. (2014) Hypertension and Its Associated Risk Factors in the Kingdom of Saudi Arabia, 2013: A National Survey. Int J Hypertens 2014: 1-8.
- Supiyev A, Kossumov A, Utepova L, Nurgozhin T, Zhumadilov Z, et al. (2015) Prevalence, awareness, treatment and control of arterial hypertension in Astana, Kazakhstan. A cross-sectional study. Public Health 129: 948-953.
- Zhang J, Huang Q, Yu M, Cha X, Li J, et al. (2013) Prevalence, awareness, medication, control, and risk factors associated with hypertension in Bai ethnic group in rural China: the Yunnan Minority Eye Study. PLoS One 8: 1-9.
- Eckel RH, Jakicic JM, Ard JD, de Jesus JM, Houston Miller N, et al. (2014) AHA/ACC Guideline on Lifestyle Management to Reduce Cardiovascular Risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 129: S76-S99.
- Sociedade Brasileira de Cardiologia / Sociedade Brasileira de Hipertensão / Sociedade Brasileira de Nefrologia (2010) VI Diretrizes Brasileiras de Hipertensão. Arq Bras Cardiol 95: 1-51.
- Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, et al. (2001) DASH-Sodium Collaborative Research Group. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med 344: 3-10.
- He FJ, Li J, Macgregor GA (2013) Effect of longer term modest salt reduction on blood pressure: Cochrane systematic review and meta-analysis of randomised trials. BMJ 346: 1-15.
- Egan BM, Zhao Y, Axon RN (2010) US trends in prevalence, awareness, treatment, and control of hypertension, 1988-2008. J Am Med Assoc 303: 2043-2050.
- Neutel CI, Campbell NRC (2008) Changes in lifestyle after hypertension diagnosis in Canada. Can J Cardiol 24: 199-204.
- Kim Y, Kong KA (2015) Do Hypertensive Individuals Who Are Aware of Their Disease Follow Lifestyle Recommendations Better than Those Who Are Not Aware? PLoS One 10: 1-13.
- Idler EL, Benyamini Y (1997) Self-rated health and mortality: a review of twenty-seven community studies. J Health Soc Behav 38: 21-37.
- Harrington J, Fitzgerald AP, Layte R, Lutomski J, Molcho M, et al. (2011) Sociodemographic, health and lifestyle predictors of poor diets. Public Health Nutr 2011; 14: 2166-2175.
- Beevers G, Lip GY, O’Brien E (2001) ABC of hypertension: blood pressure measurement. Part II-conventional sphygmomanometry: technique of auscultatory blood pressure measurement. Brit Med J 322: 1043-1047.
- Pan F, Zheng D, He P, Murray A (2014) Does the position or contact pressure of the stethoscope make any difference to clinical blood pressure measurements: an observational study. Medicine 93: 1-5.
- Bombak AE (2013) Self-Rated Health and Public Health: A Critical Perspective. Front Public Health 1: 1-4.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi