Case Report, Res Rep Gastroenterol Vol: 1 Issue: 1
Inverted Meckels Diverticulum as the cause of Intussusception in Adults
Shenouda M, Reid J, DeRogatis MJ*, Gaspard S and Hinika G
Dignity Health California Hospital Medical Center, Los Angeles, California, United States
*Corresponding Author : Michael DeRogatis
Dignity Health California Hospital Medical Center, Los Angeles, California, United States
Tel: 4849035655
Email: michael.derogatis@gmail.com
Received: September 29, 2017 Accepted: October 10, 2017 Published: October 15, 2017
Citation: Shenouda M, Reid J, DeRogatis MJ, Gaspard S, Hinika G (2017) Inverted Meckel’s Diverticulum as the cause of Intussusception in Adults. Res Rep Gastroenterol 1:1
Abstract
We present the case of a 20 year old female with acute, worsening cramp-like abdominal pain. Computed tomography (CT) of the abdomen and pelvis with intravenous contrast demonstrated a long segment of ileoileal intussusception and a separate, shorter and more distal ileoileal intussusception. Surgical treatment with exploratory laparotomy and pathological examination of the resected ileal segment showed ileal intussusception with telescoping Meckel’s diverticulum. The lead point of intussusception was a lipomatous lesion of heterotopic gastric tissue. Although Meckel’s diverticulum is a known cause of intussusception, it rarely presents in the 2nd decade of life.
Keywords: Meckel’s diverticulum; Ileoileal intussusception; Gastrointestinal tract
Introduction
Intussusception occurs when a segment of the intestine telescopes into another segment proximally or distally. The pathophysiology underlying pediatric intussusception differs from adult intussusception. In pediatric patients, intussusception is caused by either physiological or benign tumors. However, in adults, it is mostly due to pathological conditions [1]. Adult intussusceptions are also known to be rarer compared to the incidence of pediatric intussusception. Meckel’s diverticulum is the most common congenital anomaly of the gastrointestinal tract. However, Meckel’s diverticulum only accounts for 4% of intussusceptions and occurs in less than two-percent of the population [2]. It is usually clinically silent and uncommon in adults, but can lead to many complications including bleeding, obstruction, intussusception, diverticulitis, and perforation. Ectopic tissue, found in half of the cases, consists of gastric tissue (60-85%) and pancreatic tissue (5-16%) [3]. Meckel’s diverticulum is a true diverticulum resulting from persistence of the vitelline duct [4]. Indications for surgery are painless bleeding, bowel obstruction, and Meckel’s diverticulitis [2].
Meckel’s diverticulum generates intussusception by serving as a pathological lead point for bowel to invaginate into an adjacent intestinal segment. Without urgent treatment, this condition can be fatal within a few days [5]. Open laparotomy is the treatment of choice for adult intussusception caused by Meckel’s diverticulum [6]. Surgery is the mainstay of treatment for adult intussusception, where as non-surgical reduction is preferred in children [7]. Majority of the pediatric intussusceptions can be usually treated with pneumatic or hydrostatic reductions [8]. Intussusception among children is mostly manifested as a sudden onset of intermittent abdominal pain with associated symptoms of nausea, vomiting, painless bloody stool and palpable abdominal mass. Adult intussusception can be manifested as acute, subacute or chronic non-specific symptoms [9]. Therefore, it is easier to miss the diagnosis of intussusception among adults.
Case report
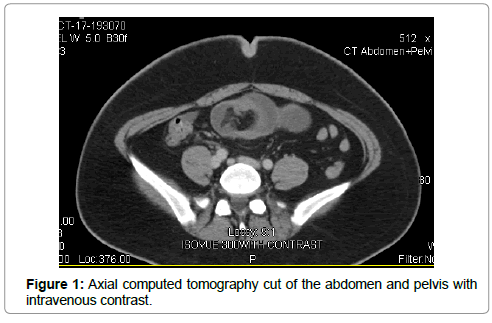
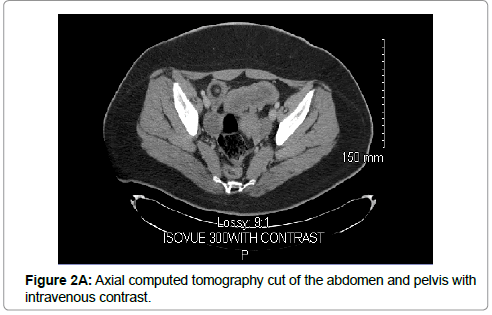
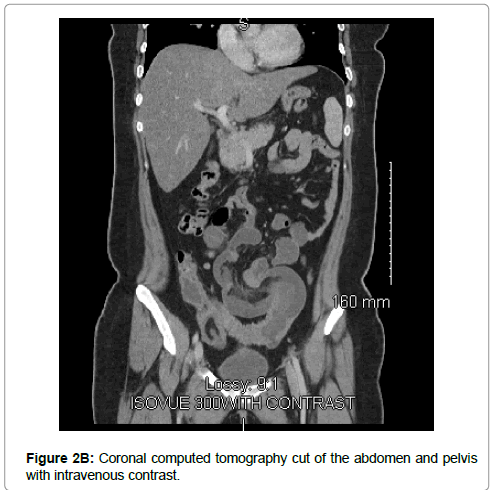
The patient is an otherwise healthy 20-year-old female, who presented to the hospital after two days of cramp-like abdominal pain associated with nausea and vomiting. It consistently worsened over the period of one day, necessitating a visit to the emergency department (ED). Upon examination in the ED, she was nauseated and had dull, aching abdominal pain. The patient had mild tachycardia in the low 100s. There was mild and diffuse tenderness to palpation of the abdomen with no palpable mass appreciated. Initial laboratory values were significant for an elevated white blood cell count of 16,300/mcL. Abdominal and pelvic CT scans with intravenous contrast showed evidence of ileoileal intussusception and mesenteric adenitis (Figure 1, 2A, 2B). When it was clear that she was not improving, the plan was made for exploratory laparotomy, possible small bowel resection.
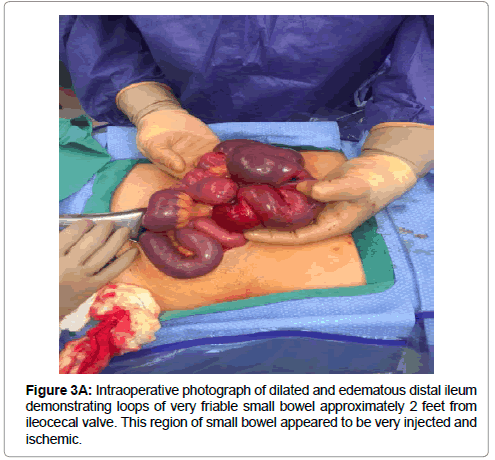
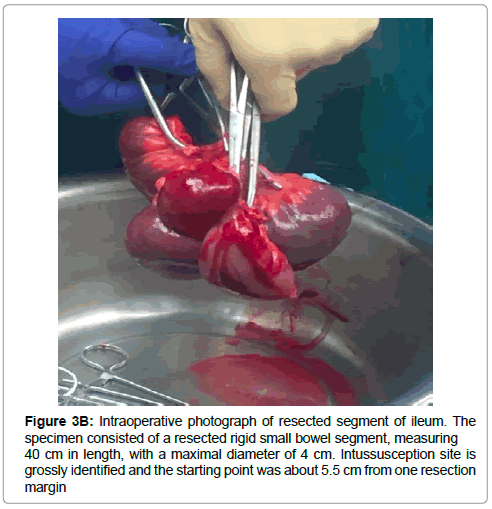
Risk, benefits, and complications of surgery were explained in detail to the patient and written consent was obtained. Procedure was done under general anesthesia. Midline abdominal incision was made and carried down to the fascial level with electrocautery. Upon entering the abdomen, the distal ileum was dilated and edematous. Loops of very friable thickened small bowel approximately 2 feet away from ileocecal valve was noted, highly suggestive of an intussusception (Figure 3A). This region of small bowel appeared to be very injected and ischemic in appearance. A point proximal to the dilated ileum was chosen as a resection point. A defect in the mesentery was made with a hemostat and the small bowel was transected with one firing of the GIATM stapler (Medtronic, Minneapolis, MN). An area of viable small bowel just distal to the distended loops was then chosen for the distal resection point and the bowel was transected in a similar fashion. The specimen was then removed by dividing the mesentery between clamps (Figure 3B). Once the specimen was passed off, the edges of the mesentery were checked for hemostasis. A stapled sideto- side, functional end-to-end stapled anastomosis was created. The small-bowel enterotomies were then closed with a single firing of the GIATM stapler in the perpendicular fashion and the staple lines were oversewn in a Lembert suture pattern with 2-0 Vicryl (Ethicon, Somerville, NJ) suture. The anastomosis was felt to be widely patent at the conclusion of the anastomosis. The abdomen was then copiously irrigated with 3 L of warm saline solution. The liver and spleen were palpated and no masses were appreciated. The fascia and skin were approximated. The patient was extubated and transferred to the PACU in a stable condition. Postoperatively, the patient was kept nothing by mouth. Her diet was advanced when she had flatulence on postoperative day 4. She was discharged home on postoperative day 6 without any complications. At 2 weeks follow up, staples were removed and the incision was clean, dry, and intact. At six weeks follow up, the patient was back to her normal activities.
Gross pathological examination of the specimen showed a resected rigid small bowel segment, measuring 40 cm in length, with a maximal diameter of 4 cm. The Intussusception site was grossly identified and the starting point was about 5.5 cm from one resection margin. A bloody Meckel’s diverticulum was identified inside of the resected small bowel, which measured 31 cm in length with diameters ranging from 1.5-2.5 cm. The distal tip of the telescoping Meckel’s diverticulum had a blind end, with an infarcted mass measuring 3.3 cm in length and a maximal diameter of 1.5 cm. The microscopic pathological examination of sections through the telescoping Meckel’s diverticulum showed extensive hemorrhagic infarction. Sections through the mass lesion at the lead point of intussusception showed a lipomatous lesion with hemorrhagic infarction. Scattered benign glands were present, consistent with heterotopic gastric tissue. There was no evidence of malignancy.
Discussion
In adults, intussusception is a rare cause of acute abdominal pain and bowel obstruction. Unlike pediatric intussusception, which is idiopathic in 90% of the cases, intussusception among adults is secondary to a lead point, arguably due to pathological abnormality in 70-90% of the cases [10]. Adult intussusception is shown to be caused secondary to processes such as lipoma, postoperative adhesions, Meckel’s diverticulum, inflammatory polyps, human immunodeficiency virus, endometriosis, Henoch-Sconlein purpura and primary or metastatic malignancy [9,11,12]. Transient adult intussusception is known to be present in patients with Crohn’s disease and Celiac disease as non-lead point intussusceptions [13,14]. Symptomatology of intussusception is predominantly abdominal pain with associated constitutional symptoms such as nausea, vomiting and gastrointestinal bleeding. Intussusception should be considered in the presence of small bowel obstruction. Intussusception creates internal prolapse of the proximal bowel, causing the mesentery to fold within the lumen of the adjacent distal bowel impairing peristalsis. This mechanism causes obstruction of the bowel contents and impairs the mesenteric blood supply to the affected segment, thus leading to ischemia of the bowel wall [9].
Even though a controversy still remains regarding the appropriate surgical intervention of adult intussusception, Nagorney and colleagues advocate for initial reduction of small bowel intussusception due to the extremely low risk of primary malignancy of the small bowel and subsequent limited surgical resection as the preferred treatment [15]. However, Marinis and colleagues recommend reduction of enteric intussusception when there is proven benign etiologies of the intussusception and the presence of viable and non-ischemic bowel [9].
Our patient, with adult intussusception due to Meckel’s diverticulum, initially presented with vague abdominal symptoms leading to a wide array of differential diagnoses. Despite the rarer incidence of adult intussusception secondary to Meckel’s diverticulum, it is important to always include this diagnosis in the differentials while conducting the proper workup for associated conditions and malignancies. Due to the delayed presentation of the patient after the initial start of abdominal pain, ischemia of the bowel did not allow for initial reduction. Therefore, bowel resection with primary anastomosis was the only indicated surgical procedure. Without early intervention, this condition can result in high morbidity and mortality.
References
- Erkan N, Haciyanli M, Yildirim M, Sayhan H, Vardar E, et al. (2005) Intussusception in adults: an unusual and challenging condition for surgeons. Int J Colorectal Dis 20: 452-456.
- Anderson DJ (2000) Carcinoid tumor in Meckel's diverticulum: laparoscopic treatment and review of the literature. J Am Osteopath Assoc 100: 432-434.
- Martin J P, Connor P D, Charles K (2004) Meckel's Diverticulum. Am Fam Physician 61: 1037-1042.
- Elsayes KM, Menias CO, Harvin HJ, Francis IR (2007) Imaging manifestations of Meckel's diverticulum. AJR Am J Roentgenol 189: 81-88.
- Shapkina AN, Shapkin VV, Nelubov IV (2006) Intussusception in children: 11-year experience in Vladivostok. Pediatr Surg Int 22: 90-904.
- Ediz A, Salih P, Emre G, Feridun S (2002) Laparoscopy-assisted Resection of Complicated Meckel's Diverticulum in Adults. Surg Laparosc Endosc Percutan Tech. 12: 190-194.
- Lu T, Chng Y (2015) Adult Intussusception. Perm J 19: 79-81.
- Khorana J, Singhavejsakul J, Ukarapol N, Laohapensang M, Wakhanrittee J, et al. (2015) Enema reduction of intussusception: the success rate of hydrostatic and pneumatic reduction. Ther Clin Risk Manag 11:1837-1842.
- Marinis A, Yiallourou A, Samanides L, Dafnios N, Anastasopoulos G, et al. (2009) Intussusception of the bowel in adults: a review. World J Gastroenterol 15: 407-411.
- Yakan S, Caliskan C, Makay O, Denecli AG, Korkut MA (2009) Intussusception in adults: clinical characteristics, diagnosis and operative strategies. World J Gastroenterol 15: 1985-1989.
- Ludvigsson JF, Nordenskjöld A, Murray JA, Olén O (2013) A large nationwide population-based case-control study of the association between intussusception and later celiac disease. BMC Gastroenterol 13: 89.
- Choi YS, Suh JP, Lee IT, Kim JK, Lee SH, et al. (2012) Regression of giant pseudopolyps in inflammatory bowel disease. J Crohns Colitis 6: 240-243.
- Kim YH, Blake MA, Harisinghani MG, Archer-Arroyo K, Hahn PF, et al. (2006) Adult intestinal intussusception: CT appearances and identification of a causative lead point. Radiographics 26: 733-744.
- Knowles MC, Fishman EK, Kuhlman JE, Bayless TM (1989) Transient intussusception in Crohn disease: CT evaluation. Radiology 170: 814.
- Nagorney DM, Sarr MG, McIlrath DC (1981) Surgical Management of Intussusception in Adults. Ann Surg 193: 230-236.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi