Clinical Image, Int J Cardiovasc Res Vol: 9 Issue: 7
Multiple Intracardiac Thrombi Complicated By Ischemic Stroke In A Young Patient With SARS-Cov-2 Infection
Rime Benmalek, Zeine El Abasse, Anas Maaroufi and Rachida Habbal
Department of Cardiology, Hospital University Center Ibn Rochd, Casablanca, Morocco
*Corresponding Author: Dr. Rime Benmalek
Resident in Department of cardiology, Hospital University Center Ibn Rochd, Casablanca, Morocco
Tel: +212 607 717 951
E-mail: Rime.benmalek@gmail.com
Received:November 04, 2020 Accepted: November 23, 2020 Published: November 30, 2020
Citation: Benmalek B, El Abasse Z, Maaroufi A, Habbal R (2020) Multiple Intracardiac Thrombi Complicated by Ischemic Stroke in a Young Patient with SARSCov-2 Infection. Int J Cardiovasc Res 9:7. doi: 10.37532/icrj.2020.9(7).424
Abstract
Coronavirus disease-2019 (COVID-19) is known to predispose patients to thrombotic disease, especially venous thromboembolism. However, arterial thrombosis is exceptionally described and can be associated with other additional risk factors increasing the risk for thromboembolism, making the management of these patients challenging.
Keywords: Corona Virus
Discussion
COVID-19 is a disease associated with a pro-thrombotic state resulting in arterial and venous venous thrombo-embolic complications, both clinically apparent and subclinical, usually due to excessive inflammation, platelet activation, endothelial dysfunction, hypoxia and stasis [1,2]. Most available reports in the literature focused on venous thromboembolic events occurring in critically ill patients, and few studies described arterial events in stable patients. These arterial complications are rarely a direct consequence of the virus itself and are usually associated with other conditions promoting the risk for thromboembolism such as atherosclerosis, hypertension, and AF. Our case reports a young patient presenting with a stroke revealing both COVID-19 and an underlying unknown severe MS with multiple large intracardiac thrombi, which, can alone be responsible for her neurovascular complication. However, the role of SARS-CoV-2 in the pathogenesis of this arterial event can’t be ruled-out for sure. Fizzah et al. [3] study clearly demonstrated a higher thrombus burden in patients with COVID-19 presenting with ST-Segment Elevation Myocardial Infarction (STEMI) compared with STEMI patients who are not infected. These patients had higher incidence of multiple thrombotic culprit lesions as well as stent thrombosis, higher thrombus grade, lower resultant myocardial blush grade, and associated increased use of thrombus aspiration and GP IIb/IIIa inhibitors [3].
The pathophysiology of stroke in COVID-19 patients is still unknown but is more likely due to an increased systemic inflammatory response leading to endothelial and hemostatic activation [2], in addition to the affinity of the SARS-CoV-2 for Angiotensin-converting enzyme 2 receptors, that are expressed in endothelial and arterial smooth muscle cells in the brain, allowing the virus to damage intracranial arteries [4]. Recent studies have identified the impact of COVID-19 on the incidence of stroke [5]. In the meta-analysis of Tsivgoulis et al. [6] the authors estimated a pool rate of ischemic stroke (0.016, Confidence Interval [CI] : 0.008-0.025, I2 : 47%, p=0.111) based on 5 cohort studies including 4460 positive COVID-19 cases, and they found that the COVID-19 positive stroke patients were younger, had a more severe stroke syndrome and higher cryptogenic etiology than the COVID-19 negative stroke patients. These data about COVID-19 impact on stroke could be justified by the neurotropic and neurovirulence of the virus [5,7].
In our case, the hypothesis of COVID-19 being responsible of the multiple cardiac thrombi can be evoked, but is less likely than the role of MS and AF, thus, a causal relationship between SARSCoV- 2 and ischemic stroke can’t be confirmed in our patient since she had competing vascular risk factors and mechanisms. However, the interaction between the two pathologies is a plausible hypothesis since the viral infection may have precipitated the cardiac thrombi formation and the ischemic stroke.
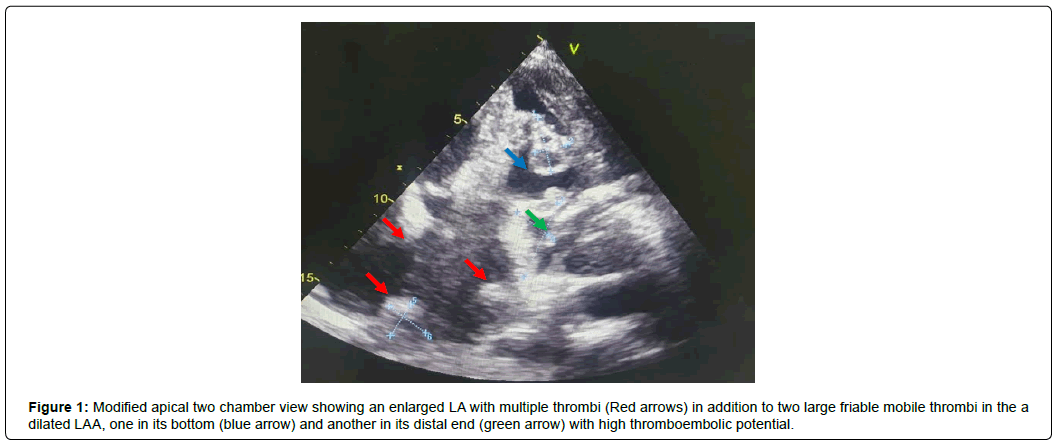
Early therapeutic anticoagulation with heparin has shown benefice in reducing thromboembolism in patients with COVID-19- associated ischemic stroke but must be balanced against the risk of hemorrhagic transformation of the acute infarct [8]. In our patient, a surgical approach is also indicated depending on the evolution of her viral infection and her response to AC, however, the outcome remains uncertain due the association between the active SARS-CoV-2 infection, the severe mitral valvular disease and the multiple large thrombi that may require thrombectomy (Figure 1). No similar case was found in the current literature to help us guide the therapeutic strategy in our patient.
References
- Levi M, Thachil J, Iba T, Levy JH (2020) Coagulation abnormalities and thrombosis in patients with COVID-19. Lancet Haematol. 7:e438-e440.
- Bikdeli B, Madhavan MV, Jimenez D, Chuich T, Dreyfus I, et al. (2020) COVID-19 and thrombotic or thromboembolic disease: implications for prevention, antithrombotic therapy, and follow-up. J Am Coll Cardiol. 75:2950-2973.
- Masi P, Hekimian G, Lejeune M, Chommeloux J, Desnos C, et al. (2020) Systemic inflammatory response syndrome is a major contributor to COVID-19-associated coagulopathy: insights from a prospective single center cohort study. Circulation. 142:611-614.
- Carod-Artal FJ (2020) Neurological complications of coronavirus and COVID-19. Rev Neurol. 70:311-322.
- Brouwer MC, Ascione T, Pagliano P (2020) Neurologic Aspects of covid-19: A Concise Review. Infez Med. 28:42-45.
- Tsivgoulis G, Katsanos AH, Ornello R, Sacco S (2020) Ischemic stroke epidemiology during the COVID-19 pandemic: navigating uncharted waters with changing tides. Stroke. 51:1924-1926.
- Orozco-Hernández JP, Marín-Medina DS, SánchezDuque JA (2020) Manifestaciones neurológicas de la infección por SARS-CoV-2. Semergen. 46:106–108
- Beyrouti R, Adams ME, Benjamin L, Cohen H, Farmer SF, et al. (2020) Characteristics of ischaemic stroke associated with COVID-19. J Neurol Neurosurg Psychiatry. 91:889–891.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi