Case Report, Int J Cardiovasc Res Vol: 7 Issue: 4
Septal Bulge as a Cause of Tako-Tsubo Syndrome
Pavlovic J*, Holy J, Hrabos V and Sembera Z
Krajská Zdravotní a.s., Masarykova Nemocnice v Ústí nad Labem, Klinika Kardiologie, Sociální PéÄÂe 3316/12A, 400 11, Czech Republic
*Corresponding Author : Pavlovic Jan MD
Krajská Zdravotní a.s., Masarykova Nemocnice v Ústí nad Labem, Klinika Kardiologie, Sociální PéÄÂe 3316/12A, 400 11, Czech Republic
Tel: +420 737 420 893
E-mail: janpavlovic@seznam.cz
Received: July 11, 2018 Accepted: August 06, 2018 Published: August 10, 2018
Citation: Pavlovic J, Holy J, Hrabos V, Sembera Z (2018) Septal Bulge as a Cause of Tako-Tsubo Syndrome. Int J Cardiovasc Res 7:4.. doi: 10.4172/2324-8602.1000358
Abstract
Even though the coincidence of LVOT obstruction and TTS has been described as early as 17 years ago and several articles have been published on this topic, some important unresolved questions and controversies regarding pathogenesis still remain. We present one case report and bring an updated concise summary of the existing knowledge.
Keywords: Tako-tsubo syndrome; Dynamic LVOT obstruction; Septal bulge; Sigmoid septum; Acute coronary syndrome
Abbreviations
ACS: Acute Coronary Syndrome; DSE: Dobutamine Stress Echocardiography; LVEF: Left Ventricular Ejection Fraction; LVOT: Left Ventricular Outflow Tract; CMR: Cardiac Magnetic Resonance; SS: Sigmoid Septum; TTE: Transthoracic Echocardiography; TTS: Tako-tsubo Syndrome
Introduction
With regard to the results of recently published studies [1-5] TTS can no longer be deemed a benign disease. Thus, early diagnosis and knowledge of the pathogenesis is important as it has therapeutic consequences. TTS is an infrequent diagnosis and publications concerning LVOT obstruction are single case reports or studies on small numbers of patients. In this paper we present a case report and an updated view on the role of septal bulge, a common finding especially in elderly patients with arterial hypertension, in the pathogenesis of LVOT obstruction and TTS.
Case Report
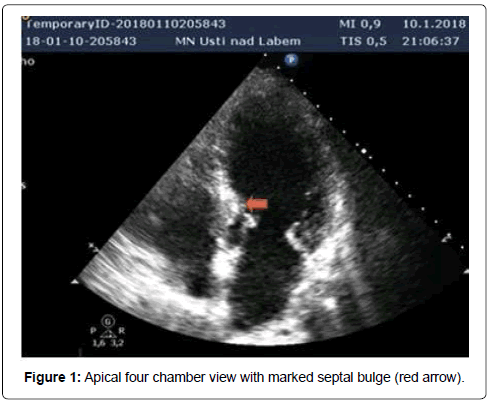
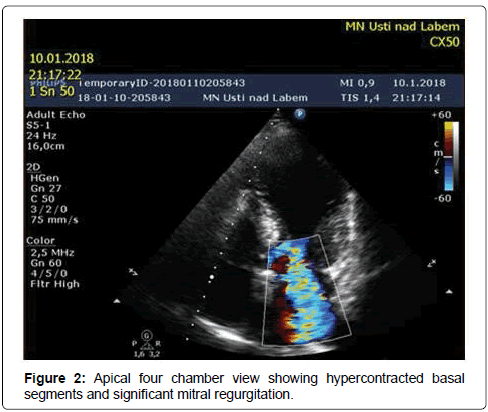
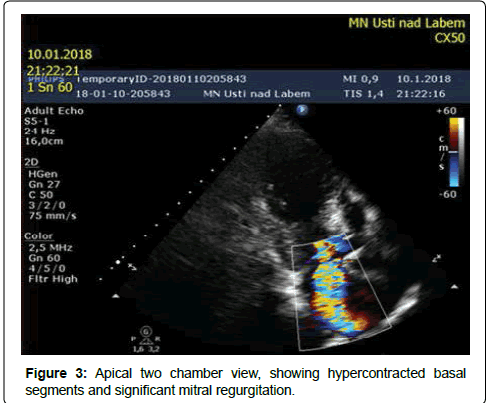
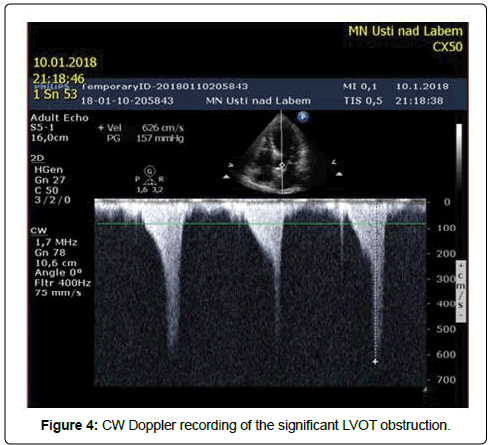
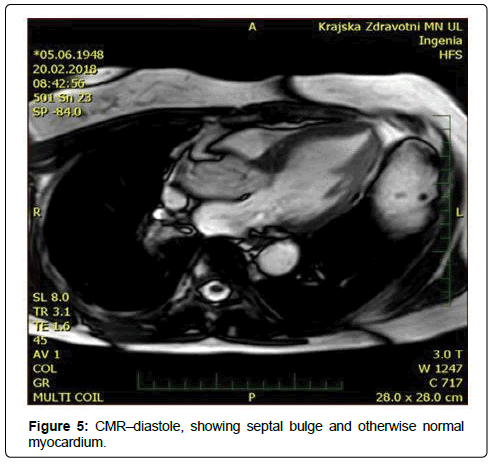
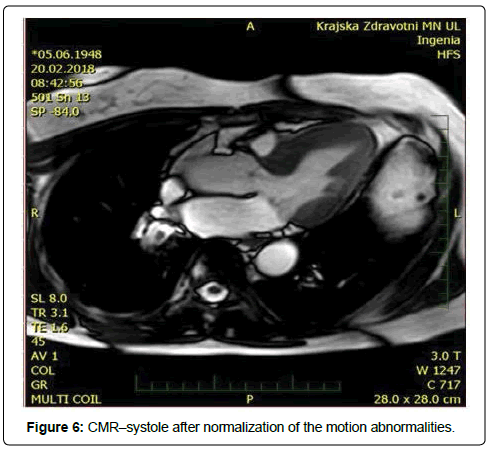
Our patient was a 69-years-old woman with treated hypercholesterolemia who was admitted for an episode of typical chest pain. It appeared during walking uphill, and then she sat down and experienced presyncope. Before this episode the patient was treated for gastroenteritis with diarrhea. On admission, her ECG showed borderline ST elevations of 2 mm in V1-V3 and borderline ST depressions in leads I and a VL. At first she was misdiagnosed as ACS in the regional hospital (and was given, besides other treatment, nitrates). Subsequently the TTE was performed (Figures 1-4) and revealed a kinesis of the apical and mid segments of the left ventricle with hyper kinesis of all basal segments, LVEF of 35%-40%, septal bulge of 13-14 mm thickness and major LVOT obstruction (maximal gradient of 190 Torr), accentuated by Valsalva maneuver, systolic anterior movement of mitral valve with significant mitral regurgitation and significant tricuspid regurgitation with pulmonary hypertension (maximal transtricuspid gradient of 40 Torr). Then, coronary angiography was performed with normal finding. Out of laboratory examinations, the only abnormity was elevated hs Troponin T (365 ng/l) on admission with continuous decrease afterwards and borderline value of Urea (8 mmol/l) on admission. On ECG the repolarization changes developed into deep negative T waves in anterolateral leads with ST depressions, prolongation of QTc (600 ms) and the patient had intermittent sinus bradycardia. That is why, she was not given betablocker. Both, the akinesis of the LV and the valve regurgitations have completely resolved in 2 weeks. Afterwards CMR was performed, showing normal thickness of the myocardial walls, except for the basal septum, normal kinetics of LV and no sign of structural disorder of the myocardium: no oedema or late enhancement. (Figures 5 and 6). It was the only patient with coincidence of TTS and LVOT obstruction out of 4 patients with tako-tsubo syndrome examined at our institution in the period since 5/2015 to 5/2017.
Discussion
The incidence of TTS is relatively low: in most studies it is around 1%-3% of all patients referred as suspected acute coronary syndrome, but the precise incidence is unknown [6]. Of these patients only minority has dynamic LVOT obstruction – in three studies [7-9] it was 18%, 19% and 19.6% respectively up to 33% in study of Kawaji [10] and therefore it is difficult to collect a statistically significant number of patients with both TTS and LVOT obstruction.
Controversy still exists whether the LVOT obstruction is primarily caused by septal bulge, acute geometric remodeling and basal LV hypercontractility [1,7,11] or by systolic anterior motion of the mitral valve leaflet [12]. Coincidence of LVOT obstruction and TTS has been described already by Villareal et al. in three case reports [1]. (1) and septal bulge has been proposed among possible causes of LVOT obstruction as early as by Fukuda et al. and Iida et al. [13,14].
In 2013 a systematic study on 64 patients [15] actually proved the potential of sigmoid septum to produce LVOT obstruction during dobutamine infusion: in 40 subjects, an LVOT obstruction occurred during the DSE and it was defined as latent obstruction.
The largest sample of patients with the coincidence of all three conditions (TTS, SS and LVOT obstruction) has been studied in works of Mahmoud et. al. [16], Núnez et al. [9], Kawaji et al. [10], Merli et al. [17] and of De Backer et al. [8] with 8, 10, 9, 4 and 6 patients respectively.
In the study of Mahmoud et al. [16] among 10,366 patients referred for coronary angiography, the study population consisted of 3,909 patients with suspected ACS. Thirty-two patients presented with TTS, resulting in a prevalence of 0.8% in population of ACS.Eight women exhibited LVOT obstruction - a prevalence of 25% among TTS cases. All patients with intraventricular pressure gradient had systolic anterior motion of the mitral valve and septal bulge. Prevalence of septal bulge was 100% in patients with Tako-tsubo syndrome and LVOT obstruction versus 29% in patients without LVOT obstruction.
In the study of Núnez et al. [9] half of the patients had significant left ventricular hypertrophy (LVH). The obstruction gradient was detected in 58.8% of patients with LVH (n=10) and 0% in the group without LVH. In the study of De Backer [8] prevalence of septal bulge in the patients with TTS and LVOT obstruction was 83.3 (n=5) and 26.9% in patients without LVOT obstruction (n=7).
In our study [18,19] we have analyzed a population of 2143 patients admitted between years 2004 and 2009 for suspected ACS and found 11 patients (0.5%) who met the revised Mayo Clinic’s diagnostic criteria for TTS [20]. Three of them had septal bulge, but only in one patient LVOT obstruction was detected (9%). It was a woman with LVOT obstruction in the acute stage of TTS, which turned into a latent obstruction, provocable by nitroglycerine after resolution of motion abnormalities.
We have simplified the results of the mentioned studies so as to address purely the correlation between TTS, LVOT obstruction and sigmoid septum in Table 1. Total number of patients with TTS and LVOT obstruction in these studies is 25 and 24 of them had sigmoid septum or septal hypertrophy (96.7%). However in the study of Kawaji et al. [10] the authors could not identify any baseline characteristics predisposing to the occurrence of LVOT obstruction.
| Author, year | Sigmoid septum/septal bulge (basal/midventricular septal thickening) with or without septal hypertrophy | Transient dynamic LVOT or intraventricular obstruction |
|---|---|---|
| Merli 2006 | 4 | 4 |
| Mahmoud 2008 | 8 | 8 |
| Núnez 2009 | 10 | 10 |
| DeBacker 2014 | 6 | 5 |
Table 1: Selected studies of patients with coincidence of TTS, LVOT obstruction and SS or septal hypertrophy.
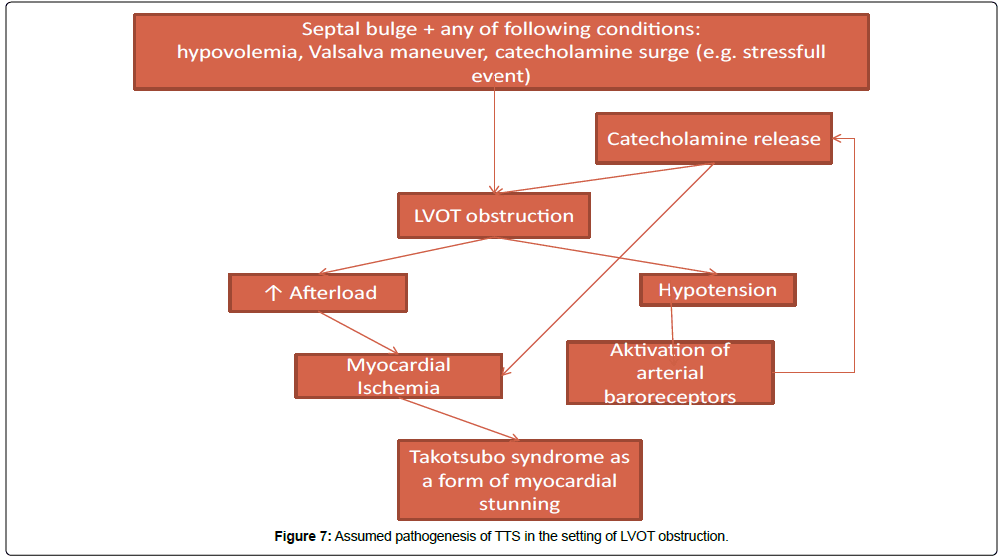
The results of presented studies encourage to speculate, whether there is first obstruction and then TTS or vice versa. Hyperkinesis of basal segments is always present in TTS but, according to the mentioned studies, in case of concomitant LVOT obstruction it is almost never without septal bulge. This suggests that the combination of septal bulge and conditions like hypovolemia or Valsalva maneuver alone is sufficient to cause LVOT obstruction and TTS. It is likely, that the actual cause of LV motion abnormities is diffuse ischemia due to pressure overload boosted by catecholamines leading to a form of myocardial stunning – an idea presented already in a case report of a patient with hypertrophic cardiomyopathy by Bougard et al. 22 years ago [21]. We outline a probable pathogenetic scheme in Figure 7.
Given the proposed pathogenesis it would seem logical to treat TTS with betablockers. Studies, performed to date, do not support long term treatment with betablockers however [3,22] as they do not seem to prevent recurrences of TTS. But the use of short acting betablockers in the setting of TTS and acute heart failure is recommended [2] although this recommendation is not based on a statistical evidence of a mortality benefit.
Conclusion
Our case report, in accordance with findings of other authors, shows, that septal bulge, together with any condition increasing the gradient across LVOT (like hypovolemia or Valsalva maneuver) has the potential to cause tako-tsubo syndrome. It can serve as part of evidence providing theoretical basis for administration of beta blockers at least in a subgroup of patients with TTS.
References
- Villareal RP, Achari A, Wilansky S, Wilson JM (2001) Anteroapical stunning and left ventricular outflow tract obstruction. Mayo Clin Proc. 76:79-83
- Ghadri JR, Wittstein IS, Prasad A, Sharkey S, Dote K, et al. (2018) International Expert Consensus Document on Takotsubo Syndrome (Part II): Diagnostic Workup, Outcome, and Management. Eur Heart J 39: 2047-2062.
- Ghadri JR, Ruschitzka F, Luscher TF, Templin C (2014) Takotsubo cardiomyopathy: still much more to learn. Heart 100: 1804-1812.
- Templin C, Ghadri JR, Diekmann J, Napp LC, Bataiosu DR, et al. (2015) Clinical Features and Outcomes of Takotsubo (Stress) Cardiomyopathy. N Engl J Med 373 :929-938
- Tornvall P, Collste O, Ehrenborg E, Jarnbert-Petterson H (2016) A case-control study of risk markers and mortality in Takotsubo stress cardiomyopathy. J Am Coll Cardiol 67: 1931-1936.
- Lyon AR, Bossone E, Schneider B, Sechtem U, Citro R, Underwood SR, Sheppard MN, et al. (2016) Current state of knowledge on Takotsubo syndrome: a Position Statement from the Taskforce on Takotsubo Syndrome of the Heart Failure Association of the European Society of Cardiology. Eur J Heart Fail 18: 8-27.
- Tsusihashi K, Ueshima K, Uchida T, Oh-mura N, Kimura K, et al. (2001) Transient left ventricular apical ballooning without coronary artery stenosis: a novel heart syndrome mimicking acute myocardial infarction. J Am Col Cardiol 38:11-18
- De Backer O, Debonnaire P, Gevaert S, Missault L, Gheeraert P, et al. (2014) Prevalence, associated factors and management implications of left ventricular outflow tract obstruction in takotsubo cardiomyopathy: a two-year, two-center experience. BMC Cardiovasc Disord 14: 147.
- Núnez-Gil IJ, García-Rubira JC, Luaces M (2009) Outflow tract obstruction and Takotsubo syndrome. Am Heart J 158: e5–e6.
- Kawaji T, Shiomi H, Morimoto T, Tazaki J, Imai M, et al. (2015) Clinical Impact of Left Ventricular Outflow Tract Obstruction in Takotsubo Cardiomyopathy. Circulation J 79: 839-846
- Chandrasegaram MD, Celermajer DS, Wilson MK (2007) Apical ballooning syndrome complicated by acute severe mitral regurgitation with left ventricular outflow obstruction–case report. J Cardiothorac Surg 2: 14.
- Liang JJ, Janish CD, Bishu KG, Reeder GS (2014) Dynamic left ventricular outflow tract obstruction in apical ballooning syndrome Takotsubo cardiomyopathy. Perfusion. 30: 82-84
- Fukuda N, Asai M, Tominaga T, Irahara K, Mikawa T, et al. (1984) Noninvasive studies of dynamic left ventricular outflow obstruction in patients with sigmoid septum. J Cardiogr 14: 445.
- Iida K, Sugishita Y, Ajisaka R, Matsumoto R, Higuchi Y, et al. (1986) Sigmoid septum causing left ventricular outflow tract obstruction: A case report. J Cardiography 16: 237-247
- Tano A, Kasamaki Y, Okumura Y, Ohta M, Kofune T, et al. (2013) Major determinants and possible mechanism of dobutamine-induced left ventricular outflow tract obstruction in patients with a sigmoid ventricular septum. J Cardiol 61: 428-435.
- El Mahmoud R, Mansencal N, Pilliere R, Leyer F, Abbou N, et al. (2008) Prevalence and characteristics of left ventricular outflow tract obstruction in Tako-Tsubo syndrome. Am Heart J 156: 543-548.
- Merli E, Sutcliff S, Gori M, Sutherland GG (2006) Tako-Tsubo cardiomyopathy: New insights into the possible underlying pathophysiology. Eur J Echocardiogr 7: 53-61.
- PavloviÄ J, HlaváÄÂek K, Feuereisl R, SurovÄÂík R, Frídl P, et al. (2010) Role of a dynamic LVOT obstruction in the pathogenesis of takotsubo syndrome. Cor Vasa 52: 695-699
- SurovÄÂík R, Feuereisl R, Frídl P, HlaváÄÂek K, Jebavý P, et al. (2009) Stresová (takotsubo) kardiomyopatie. Interv Akut Kardiol 8: 292-296.
- Kawai S, Kitabake A, Tomoike H, Takotsubo Cardiomyopathy Group (2007) Guidelines for diagnosis of takotsubo (ampulla) cardiomyopathy. Circulation J 71:990-992
- Bougard M, Heuse D, Friart A (1996) Myocardial stunning in hypertrophic cardiomyopathy with normal coronary arteries. Int J Cardiol 56: 71-73
- Singh K, Carson K, Usmani Z, Sawhney G, Shah R, et al. (2014) Systematic review and meta-analysis of incidence and correlates of recurrence of Takotsubo cardiomyopathy. Int J Cardiol 174: 696-701.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi