Research Article, Res J Opt Photonics Vol: 2 Issue: 2
Study and Applications of Laser Light
Gupta SK1*, Jangam H2 and Sharma N2
1Department of Physics, Parishkar College of Global Excellence, Jaipur, India
*Corresponding Author : Sumit Kumar Gupta
Assistant Professor, Department of Physics, Parishkar College of Global Excellence, Jaipur, India
Tel: 919784271105
E-mail: sumitguptagit@gmail.com
Received: May 25, 2018 Accepted: June 11, 2018 Published: June 18, 2018
Citation: Gupta SK, Jangam H, Sharma N (2018) Study and Applications of Laser Light. Res J Opt Photonics 2:2.
Abstract
This work gives an idea about the originality of laser beams and how we benefit from them in the treatment and the recovery of patients. Some of the important medical lasers are NeodymiumYAG Laser (Nd: YAG) is used in laparoscopic surgery, the Carbon Dioxide Laser (CO2) is one of the most widely used in surgical operation especially in gynecologic surgery. Moreover it is used as scalpel, the Argon Laser (Ar+) is used for ophthalmology and the Dye Laser is recently used in the treatment of cancer tumor. We know that Argon and Dye Lasers beams produce intense visible light that can be seen by the naked eye. For this reason they can be easily controlled and directed by the surgeons and physician. But beams of Carbon Dioxide and YAG Lasers are invisible and they are located in the Zone of the infrared region. For this reason we use the beams of Helium Neon lasers that have red colour with energy very low. So we use these lasers simultaneously with the above mentioned lasers beams to allow the operator to adjust spot size and operation distances efficiently. This enables the surgeons and physicians to accomplish more serious operations and to obtain more satisfactory results. From the field study of the laser instruments used in ophthalmology hospitals in Khartoum State it’s clear that the laser instruments used there are, Argon Laser, Yag Laser and Excimer Laser Instruments.
Keywords: Laser light, Radiation
Introduction
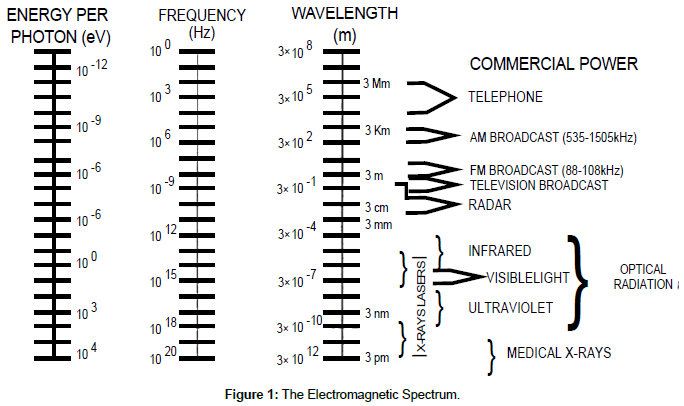
The word laser is an acronym for Light Amplification by the Stimulated Emission of Radiation. Laser light today covers a wide range of wavelengths, which includes the visible range of the electromagnetic spectrum [1]. Figure 1 Light Amplification by the Stimulated Emission of Radiation was originally described as a theoretical concept by Albert Einstein in 1917, but it was not until 1954 that the first “stimulated” emissions of microwave radiation (Maser) were generated by J.P Gorden and C.H. Townes at Bell Laboratories. Theoretical calculations for the construction of a visible light Maser or Laser were published in 1958. The first Laser was built in 1960 by T.H. Maiman. His laser consisted of a pink ruby rod with silvered ends for mirrors inserted in a helical coil of a photographic flash lamp, which generated millisecond pulses of coherent 694 nm Ruby Laser (red) light [2]. Today lasers have entered almost all fields of science and have made a wide step of progress in many of them. Laser has become the modern technique of the 20th century. In medicine, it became the “beam that heals” and has been utilized in nearly every discipline of medicine, in diagnosis, therapy, surgery and medical instrumentation. In order to realize the full advantages of using a laser beam, one should understand the process of interaction between the beams one uses and the spot one needs to treat. One should know something about beam properties, its origin and the requirements needed to provide such a beam; also one should know how to handle the laser system and how to work safely, with an awareness or all possible hazards and, therefore, taking all necessary precautions to avoid harm to oneself and damage to treated area.
The purpose of this paper is to provide such information in a simple form and also to describe several types of lasers that find interest in the different fields of medicine, together with some applications.
Laser Power
Power Density
The rate of laser energy delivery is called power and is measured in watts. The wattage is equal to the amount of energy, measured in joules, divided by the duration of exposure, measured in seconds.
Watts (W)=Joules (J)/Seconds (S) (1)
An important factor in the effective application of the laser is a concept of power density, or irradiance. Power density is defined as the amount of power that is concentrated into a spot, or watts/cm2.
Power density=Watts/Spot Size (cm) (2)
The spot size of a laser beam depends on several variables, including the focal length of the lens, the wavelength of the laser, and the transverse electromagnetic mode of the beam.
The focal length of the lens determines the size of the beam spot. A lens with a short focal length can provide a smaller spot size, thus increasing the intensity of the beam. A CO2 laser with a 50-mm lens can produce a spot size of 0.1 mm, whereas a 400-mm lens can produce a spot size of 0.8 mm. Thus the shorter 50-mm lens can concentrate the power in a smaller spot area.
The wavelength of the laser also limits the spot size and beam focusing. When all other factors are equal, shorter wavelengths can generate smaller spots. Thus, an argon laser at 488/514 nm can produce a much smaller spot than the CO2 laser can at 10,600 nm. The choice of laser should be based on the specific effects of the laser on the tissue rather than based on its spot-size capabilities.
The transverse electromagnetic mode (TEM) determines the precision of the spot by the power distribution over the spot area.
TEM01 mode is an example of a common multimode distribution, meaning that the spot has a cool area in the center of the beam. The most common and fundamental mode is the TEM00, which produces an even power distribution over the spot, with most of the power concentrated in the center and the rest decreasing in intensity towards the periphery of the beam. The spot size of a TEM00 beam is the region that has approximately 86% of the total beam power.
Fluency
Fluency is one of the most important and critical concepts that affect precision during laser surgery. It involves three properties: watts, time, and spot size (or area). The tissue effect will vary if any of these parameters are changed.
Fluency=Watts × Time/Spot size (cm) (3)
A laser beam can impact tissue at 100 W for 1 second, thereby delivering 100 J to tissue. Another beam can impact tissue at 1 W for 100 s, thereby also delivering 100 J to tissue. The difference in tissue effect is that more adjacent tissue damage will occur with the longer duration of impact because of the laser’s tissue-heating effects. Using the highest appropriate wattage for the shortest time minimizes any damage to adjacent healthy tissue [3].
Mode of Operation
The output of a laser may be a continuous constant-amplitude output (known as CW or continuous wave); or pulsed, by using the techniques of Q-switching, and Modelocking.
Continuous wave operation
In the continuous wave (CW) mode of operation, the output of a laser is relatively consistent with respect to time. The population inversion required for lasing is continually maintained by a steady pump source [4].
Pulsed operation
In the pulsed mode of operation, the output of a laser varies with respect to time, typically taking the form of alternating ‘on’ and ‘off’ periods. In many applications one aims to deposit as much energy as possible at a given place in as short time as possible.
Q-switching
Extremely high power levels can be obtained by using a technique Known as q-switching that momentarily stores excess energy. A shutter is placed in the optical path to prevent laser emission until a very large population inversion has built up. When the shutter is opened the electrons is rapidly fall to the ground state releasing a tremendous pulse of energy that lasts only a few nanoseconds. Powers in the megawatt range can be produced by this technique. Q-switching is commonly used with ruby and neodymium solid laser.
Modelocking
A modelocked laser emits extremely short pulses on the order of tens of picoseconds down to less than 10 femtoseconds. These pulses are typically separated by the time that a pulse takes to complete one round trip in the resonator cavity.
Laser-Tissue Interaction
When laser energy is delivered to tissue four specific interactions can occur: reflection, scattering, transmission or absorption. The extent of the interaction depends on the wavelength of the laser, fluency, and tissue types.
Reflection
The laser beam has no effect on the target when it is reflected off the impact site (Figure 2), but it can cause harm where the beam eventually hits.
Scattering
The distribution of the laser light energy within the tissue can be altered when the beam is scattered through the tissue (Figure 3). If the scattered energy is ultimately absorbed, then it will be converted to heat. The laser beam can also backscatter, causing potential hazard.
Transmission
Some laser wavelengths can be transmitted through certain tissue but have little or no thermal effect (Figure 4).
Absorption
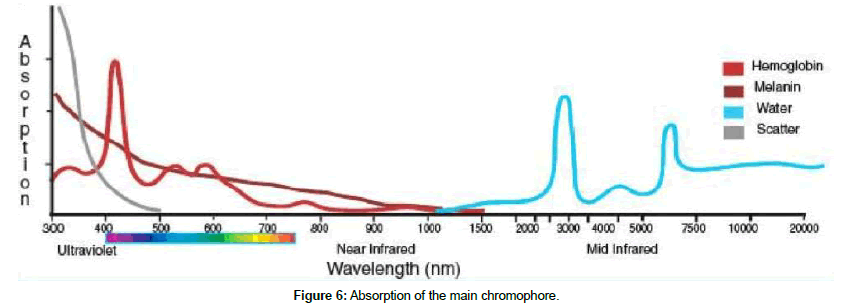
As the tissue absorbs the laser energy, heat energy is produced and tissue damage occurs (Figure 5). Each tissue has specific absorption characteristics base on its composition and chromophore content. The principal chromophores present in mammalian tissue are hemoglobin, melanin, water and protein.
Infrared light is absorbed primarily by water, while visible and ultraviolet light are primarily absorbed by hemoglobin and melanin, respectively. As wavelength decreases toward the violet and ultraviolet, scatter or absorption from covalent bands in protein limits penetration depth in the range (Figure 6).
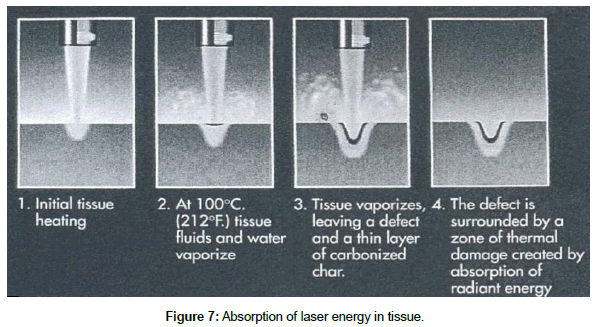
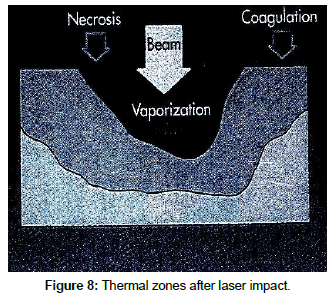
When laser light strikes tissue and absorption takes place, the cellular water is super-heated to over 100°C. Intracellular protein is destroyed as the heat continues to build. The water inside the cell then turns to steam. Since 1 g of steam occupies more space than does 1 g of water, the cellular membrane bursts under this extreme pressure. Debris and smoke (laser plume) is spewed from the tissue. Adjacent tissue is warmed by the intense heat produced it the point of incidence. The degree of thermal damage depends upon the temperature to which the laser energy heats the tissue. Table 1 notes the changes that occur as the laser beam is absorbed. The mechanism of thermal laser surgery is illustrated in Figure 7. At the immediate laser- tissue impact site there is a zone of vaporization. Immediately adjacent to this site is a zone of necrosis caused by the thermal spread. Farther from the impact site is a zone of coagulation as thermal injury decreases (Figure 8).
| Temperature | Visual change | Biological change |
|---|---|---|
| 37-60°C | No visual change | Warming, welding |
| 60-65°C | Blanching | Coagulation |
| 65-90°C | White/grey | Protein denaturation |
| 90-100°C | Puckering | Drying |
| 100°C | Smoke plume | Vaporization, carbonization |
Table 1: Tissue changes with temperature increases.
The depth of penetration of the laser beam depends upon the laser wavelength, color and consistency of the tissue, power of the beam, duration of beam exposure, and beam spot size. As the laser beam cuts through tissue, it will continue to heat and destroy deeper tissues. If there is concern about accidental damage to adjacent tissues, a backstop may be used. Materials such as wet sponges, quartz rods, or titanium rods can be used as back-stops.
Laser surgery can be divided into three broad categories regarding tissue response: Thermal, mechanical, and chemical effects. Approximately 85% of lasers used today produce a thermal effect at the tissue level. These lasers cut, coagulate, vaporize, and ablate tissue from the interaction site where the thermal response originates. The mechanical effect on tissue is produced by some lasers as the laser beam generates sonic energy that mechanically disrupts tissue. Breaking apart kidney stones in the ureter or disrupting the posterior capsule within the eye are examples of this type of mechanical effect. The chemical effect of some lasers is produced as the laser energy activates light-sensitive drugs to disrupt and change tissue. This process is used in photodynamic therapy to selectively destroy malignant cells [5].
Medical Lasers with Applications
Properties of medical lasers
Brief properties of some medical lasers with several applications are given for lasers discussed in the previous sections of this chapter.
The ruby laser
The Ruby laser emits red light with a wavelength of 694 nm, early ruby laser systems were use retinal surgery, but weren’t used widely for dermatologic work until the development of Q-Switching technology in the mid 1980’s for tattoo treatments. Ruby laser light is strongly absorbed by blue and black pigment, and by melanin in skin and hair. Modern ruby laser system are available in Q-Switched mode, with an articulating arm, “free running” (millisecond range) mode with a fiber optic cable delivery, or as dual mode lasers. Current uses include
Treatment of tattoos (Q-switched mode).
Treatment of pigmented lesions including freckles, liver spots, Nevus of Ota (Q-switched mode).
Laser Hair Removal (free-running mode).
The neodymium: YAG laser
The laser output is in the near infrared spectrum at wavelength 1060 nm. It has a poor absorption by blood, i.e. absorption coefficient, a=4 cm-1 and is less absorbed by water (a~0.1 cm-1) .Hence it can penetrate rather deep into the tissue and is transmitted through clear liquids. This allows its use in the eye and other water-like filled cavities such as the bladder. The Nd: YAG beam has a high degree of scattering upon impact with tissue. The homogeneous zone of thermal coagulation and nicrosis from the impact site but precise control is not possible. The laser beam is also used to coagulate vessels up to about 4 mm in diameter. These characteristics make the Nd: YAG laser an excellent tool for tissue coagulation but very crude, unprecise tool for cutting due to tissue damage. For treatments sapphires tips, diamond or quartz are used to improve precision and to allow better control to avoid excessive tissue destruction. Major specialties of the laser use is in the treatment of menorrhagia, e.g. uncontrolled bleeding from uterus. A laser fiber is passed into the uterus via a hysteroscope to coagulate the endometrium. The pulsive form of Nd: YAG output, i.e. the Q-switched and the mode-locked form, has found a growing use in ophthalmology both for eye diagnosis and treatment. Laser can differentiate between a faulty neural system and a disturbed optical system of the eye. Thus a predictive ability is provided when considering operations such as cataract removal, vitrectomy, corneal transplant and glaucoma surgery [6,7].
The helium: neon laser
Due to the low output power of the laser beam, the laser is mostly used in students’ laboratory for teaching. In medicine, it has been used normally as aiming beam. Since the beams of some powerful lasers, as CO2 and Nd: YAG lasers are invisible to the eye, the red beam of He: Ne laser allows the operator to adjust spot size and operating distance before the operating beam is switched.
The argon-laser
The laser beam is visible as a bright blue-green light of wavelength 488-515 nm. It is better absorbed by blood (a=34 cm-1) than the Nd: YAG laser, but its absorption in water (a<0.001cm-1) is less than of Nd: YAG laser. It is easily transmitted through clear aqueous tissues. Certain tissue pigments such as chromogens, melanin and hemoglobin will absorb argon laser light very effectively. This localization of heat generation will be a highly effective coagulator. The first significant medical application of this selective absorption characteristic was in the treatment of diabetic retinopathy in 1965. The argon laser light is absorbed by the retinal pigment epithelium and the generated heat is then used to photocoagulate the retina. Dermatology and plastic surgery are the other major areas of applications of argon laser therapy. The laser light is more heavily absorbed by the pigmented tissue or pigmented lesion than by the surrounding tissue. A valuable application is the treatment of port-wine stains. Like other power output lasers, the argon laser beam when focused to a very small spot (or when its power is increased sufficiently), its power density is high enough to result in vaporization of the target. Medical argon ion lasers are of power as high as 15 W. The beam is easily delivered to the site through optical fibers which can be coupled to operating microscope or hand pieces or to a variety of endoscopes.
The carbon dioxide laser
The laser emission is in the mid infrared wavelength of 10.6 μm. This range is heavily absorbed by water (a=230 cm-1). The biological tissue is composed of 70% to 90% water and its absorption to CO2 radiation is independent on the tissue color unlike its absorption to argon ion laser light. Due to this high degree of absorption, most of the incident energy is sharply absorbed i.e. having a very short penetration depth (~0.01 mm), limiting the lateral damage of the tissue and leaving a very small zone of coagulation and necrosis. This makes the CO2 laser a precise surgical instrument. The major applications of CO2 laser is in cutting, vaporization and coagulation. A focused spot of the laser beam will allow a precise cut (laser scalpel) leaving a dry bloodless areas of damage. The depth of the cut is determined by the power density and the time of irradiation. Dry incisions heal in much the same way as conventional wounds. Vaporization can be performed with focused or defocused beams. It helps in removing tissue of one cell layer at a time from its delicate structure. When cutting, vessels up to 0.5 mm in diameter can be coagulated instantly; larger vessels can be treated with a defocused beam. Precision welding of arteries for microsurgery and anastomosis of small vessels and nerves can be achieved. The CO2 laser has found widespread applications in medicine, including most of its branches i.e. gynecology, otolaryngology, neurosurgery, plastic surgery, ophthalmology, and others. Surgical CO2 lasers typically of 30W output and can go as high as 100 W. The beam is delivered with the aid of an articulating arm and hand pieces, or coupled to an operating microscope. Recently, fiber optics has become available.
The dye laser
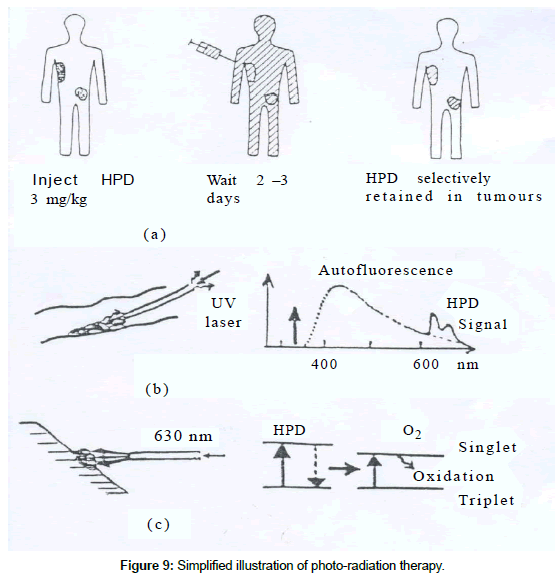
The dye fluorescence covers a broad spectrum of colors. The dye laser is used where a selective absorption characteristics of tissue upon certain wavelength is required in therapy; for example, in the treatment of port-wine stains, tattoos and other pigmented tissue. Currently, dye laser is used in photo radiation therapy (PRT), a new possibility for cancer tumor detection and treatment. This involves the use of a photosensitizing agent (tumor seeking agent), such as haematoporphyrin derivative (HPD) in combination with laser radiation. It spreads, but is selectively retained in tumor tissue after two to three days. When activated by ultraviolet radiation its emission is characterized by dual peaked fluorescence light distributed in the red spectral region (about 630 nm) superimposed on the natural fluorescence (auto fluorescence) spectrum of the tissue (the broad band emission in Figure 9).
Tumor marking.
Tumor detection using laser-induced fluorescence.
Tumor destruction by the selective release of singlet oxygen.
The spectral red lines of HPD identify the tumor and allow standard biopsy specimens to be taken at the-correct location. When laser radiation of 630 nm is delivered to HPD molecule, it absorbs it and transfers it to an oxygen molecule which gets excited. This excited molecular oxygen (singlet) is known to be a strong toxic agent. It oxidizes the surrounding (tumor) tissue. The laser radiation needed for this induced chemical process is normally provided by using a dye laser pumped by an argon-ion laser. Another application of dye lasers involves the pulsed type. They have been used to fragment gallstones and kidney stones. These are typically microsecond pulses, emitting energy 50-100 mJ at wavelengths in the blue-green region. Laser radiation is delivered to the stone by an optical fiber passed through one of the channels of an endoscope The laser lithotripter (stone breaker) have several advantages over the acoustic shockwave lithotripter currently used for kidney stones.
Clinical laser applications
In this section we will demonstrate the laser surgery, the advantage and disadvantage of the use of laser, and some of the medical fields where laser is currently used.
Laser surgery: It is a type of surgery that uses the cutting power of a laser beam to make bloodless cuts in tissue or remove a surface lesion such as a skin tumor. There are a number of different types of lasers that differ in emitted light wavelengths and power ranges and in their ability to clot, cut, or vaporize tissue when using laser in medicine, potential advantages for both surgeons and patients are provided. These advantages are No-touch technique, Possibility of operating in inaccessible regions, Dry surgical field with sterilization of the operative site, Reduced blood loss, Reduced oedema and pain yielding more rapid recovery of the patient., Limited fibrosis and stenosis, Limited damage of the adjacent tissue (for a few tens of micrometers) – Precision, Reduced postoperative pain and No evidence of causing genetic damage or cancer [8-10].
There are also disadvantages, at the present state of the technique, in the application of the laser tool as high cost, complexity of the laser surgical unit and reliability and safety problems.
Gynecology: Gynecologists were among the specialists who first truly appreciated the potential of the laser. One of the first lasers they used was the CO2 laser, which they found tremendously effective in treating patients with erosion of the cervix. New gynecological applications were introduced and with instrumentation refinements, the laser advanced laparoscopic surgery to a fine art. The laser was then found useful for cutting, coagulating and vaporizing during intraabdominal procedures. Also, the laser was coupled with the hysteroscope to perform surgery within the uterus. Other clinical applications continue to be developed by innovative gynecologists who strive to provide less invasive less complicated procedures to benefit their patients. Many different wavelengths are being used effectively for a variety of gynecological applications, including lower tract, laparoscopic, hysteroscopic, and intraabdominal procedures.
Urology: Lasers were first experimentally used in urology within gas-filled bladders. The laser was inserted through conventional rigid cystoscopies with special deflecting prisms or shutoff windows to conduct the laser energy. Advances have led to the development of cystoscopes accessories and quartz fibers to conduct the beam through a fluid-filled bladder. In the 1970s, A.Hofstetter successfully performed Nd: YAG laser cystoscopy to irradiate bladder tumors. This accomplishment led to tremendous advances in treating recurrent bladder tumors and initiated the development of other urological laser applications. A variety of laser wavelengths are used today to successfully treat many urological conditions. The CO2, Nd: YAG, frequency doubled YAG and argon lasers are commonly used for different procedures.
General surgery: The laser has been slow to gain acceptance in the field of general surgery because conventional methods offer accessibility and visibility, and the physician feels comfortable with traditional surgical tools that are easy to control during procedure. Instrument a development has advanced to meet the needs of the physician to incise or excise diseased tissue precisely and with fewer complications using minimally invasive techniques. Therefore, the general surgeon has not had a great desire to accept other tools, such as the laser. Because the laser has not been as quickly accepted by general surgeons as it has by other specialists, its fate is still being determined. Unfortunately for general surgeons, the laser has allowed endoscopists, cardiologists, radiologists and internal medicine specialists to perform the needed surgery from within organs or structures, thus eliminating the need for the general surgeon and incisional procedures. During the late 1980s and early 1990s, laparoscopy was aggressively introduced to the general surgeon. Laparoscopic cholecystectomy became the preferred procedure over the open upper-abdominal method. Laser technology was the tool of choice for these beginning procedures since the physicians who developed this laparoscopic technique were also skilled in using the laser. CO2 lasers are used in surgical operations, such as, otolaryngology. This is the branch of medical Science, which deals with problems of the ENT and the oral cavity. The output power of these lasers is of the order of 50 W in the CW mode. Several problems in the neck and head can treat with laser radiation. By using conventional surgical method, there is a possibility of losing a large quantity of blood. However, while doing surgical operations with lasers, it is imperative that the eyes of the patients are well protected. Protective materials such as cotton, sponge swabs etc are usually used for protecting certain vital organs like nerves, veins and arteries from unduly getting heated while the nearby tissue is being worked upon. Lasers are also used in brain surgery for cutting tissues, boring holes in the skull and vaporizing lesions and cauterizing blood vessels. The damage around the region, which is treated, is less than 1 mm. This is extremely important since the least amount of tissue should be removed or destroyed in the brain. Using CO2 lasers, neurosurgical coagulation of blood vessels up to l mm in external diameter can be done.
Dermatology: Laser is already being successfully used for cauterization and local treatment of skin growths and skin deformities.
Laser treatment provides two major advantages over conventional treatment in case of burn injuries and skin grafting. They are the area, which has been treated remains sterile and hence provides an ideal bed for immediate skin grafting and the blood loss is minimal.
Laser finds wide application in dermatology especially in Homeostasis, which means stopping of bleeding and Removal of hair, tattoos, warty keratosis, cell carcinomas, freckles, acne and various growths, both benign and malignant. CO2 lasers have been used for treating skin tumors. Another application of laser more specifically photo medicine, is in the surgical treatment of port wine stains (PWS). A port wine stain is a defect in the skin, which is manifested by discolored or blotchy and darkened patches in the skin. The most commonly used laser in the treatment of PWS is the pulsed argon laser.
Cardiology: Another important area of medical application of lasers is the laser assisted balloon angioplasty, which has become very common in clearing blocked arteries. In balloon angioplasty, a tiny deflated balloon, housed in a thin catheter, is threaded through the artery in the blocked region. When it reaches the right spot the balloon is inflated to open up the vessel by compressing the obstructing plaque against the walls of the artery. This method is less expensive and less prone to complications, as compared to conventional bypass surgery. The disadvantage with balloon angioplasty is that the vessel can close again because there is no permanent removal of the clot. About an estimated 30% case need repetition of the process. This technique is of no use in case of totally blocked arteries. Lasers have helped in overcoming this problem. Lasers can pave the way for the balloon or clear the arteries on their own. In laser-assisted angioplasty, an Ar+ laser delivers the energy through the catheter and disposable balloon. The balloon helps in inflating the site for blood flow cessation and centering the optical fiber, which transmitting the laser and the opening the vessel. Taking turns, the balloon and the laser, clear the path for each other, through the block.
Ophthalmology: Laser has become a common tool now in photocoagulation such as the one used to reattach a detached retina. For example, the green beam of argon ion laser is focused on a certain point of the retina. The beam penetrates through the lens of the eye and the vitreous chamber without being absorbed. But the beam gets strongly absorbed by the red blood cells of the retina and the resultant thermal effect leads to reattachment of retina. In the past, highpowered xenon lamps were also often used to concentrate enough heat in the area of the unattached retina. The problem faced here was that the optical power could not be focused sharply.
Photocoagulation: The laser produces a pulse of light energy as directed by the surgeon, which is passed to the eye under treatment. The pulse of light is focused by the lens of the patients’ eye to produce a minute lesion or coagulation of the tissue of the retina and the choroids (the vascular membrane of the eyeball between the sclera and retina). The retina is so welded to the choroids by a series of these lesions through several repeated pulses from the laser. The amount of energy required for coagulation is different for different patients. The two lasers are commonly used in ophthalmology, are the ruby laser of 0.69 μm and argon ion laser of 488 to 514 nm .
Treatment of corneal ulcers: The other application of lasers in the treatment of eye disease is in corneal ulcers. Here, an argon-ion laser is used in combination with a fluorescein dye. The infected site is dyed with the fluorescein dye by using antibodies, specific for the infecting organism, labeled with the dye. Fluorescein absorbs argon laser strongly and raises the temperature of the organism, thereby destroying it, without damaging the surrounding tissues.
Laser in the treatment of glaucoma: Glaucoma is caused by an increase in pressure inside the eye, which destroys nerve cells and causes vision loss. Conventional surgery to treat this condition is to cut a channel in the eye to drain out the excess fluid. However, this procedure is biset with a 5% risk of blindness. There are several drugs that could be administered to reduce the pressure. But they also cause serious side effects such as increase in blood pressure and bronchospasms. Laser surgery seems to give no side effect [11,12].
Gastroenterology: Gastrointestinal diseases primarily include ulcers and tumors of the esophagus, Stomach liver, gallbladder and intestine. The intestine further consists of the jejunum, ileum, colon, and rectum. According to the position of these organs, the gastrointestinal tract is subdivided into an upper and a lower tract. Most intestinal tumors are reported to occur inside the colon or the rectum. In general, any kind of ulcer or tumor can be treated with lasers if it is accessible with endoscopic surgery. Gastroenterology is one of the major domains of the CW Nd: Y AG laser only in photodynamic therapy are dye lasers applied. There exist mainly two indications for laser therapy: gastrointestinal hemorrhages and benign, malignant Since CW Nd: YAG laser is acting thermally; it can stop bleeding by means of coagulation. The CO2 laser is not suitable for clinical gastroenterology, since it is not transmitted through optical fibers which belong to the mandatory equipment of successful endoscopic surgery. By way of summary, performance data of the lasers described in this chapter are gathered in Table 2 [13-15].
| Laser type | Wavelength nm | Power range W (J\S) | Mode | Efficiency |
|---|---|---|---|---|
| Ruby | 694 | (>30) | pulsed | 0.1% |
| Nd: YAG | 1060 | 5-120 | CW and Q- switched | 1-3% |
| Doubled Nd: glass | 503 | (>3) | Pulsed | 0.1% |
| He:Ne | 682.8 | 10-3 to 10-2 | CW | 0.02% |
| Argon ion | 458-515 | 0.001-25 | CW and pulsed | 0.1% |
| CO2 | 10600 | 0.1-100 | CW and pulsed | 10-20% |
| Dye | 400-700 | 0.001-6 | CW | 0.5% |
Table 2: Characteristics of medical lasers.
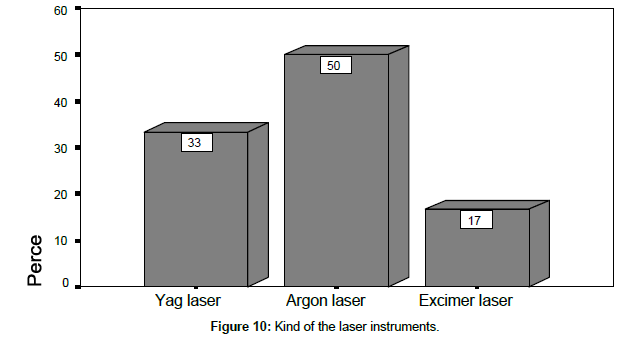
From Table 3 it is clear that the Argon laser instrument is the most widely used laser instrument. It is used at the rate of 50% compared with the Yag laser instrument which is used at the rate of 33.3% and the Excimer laser which is used at the rate of 16.7%. This is illustrated in Figure 10.
| Laser Instrument | Purpose of instrument | Number of treated sessions | Frequency | Percent |
|---|---|---|---|---|
| Yag laser | Capsuletomy | 1 session | 4 | 33.3 |
| Argon laser | Pan retinal photocoagulation | More than 1 session | 6 | 50.0 |
| Excimer laser | Lasik | 1 session | 2 | 16.7 |
| Total | 12 | 100.0 |
Table 3: Kinds of the laser instruments.
From Table 4 it is also clear from the above analysis that the price of the laser instruments is high and because they are very expensive they are found only in specialized centers of ophthalmology [16].
| Price | Frequency | Percent |
|---|---|---|
| Expensive | 12 | 100.0 |
Table 4: Price of the instruments.
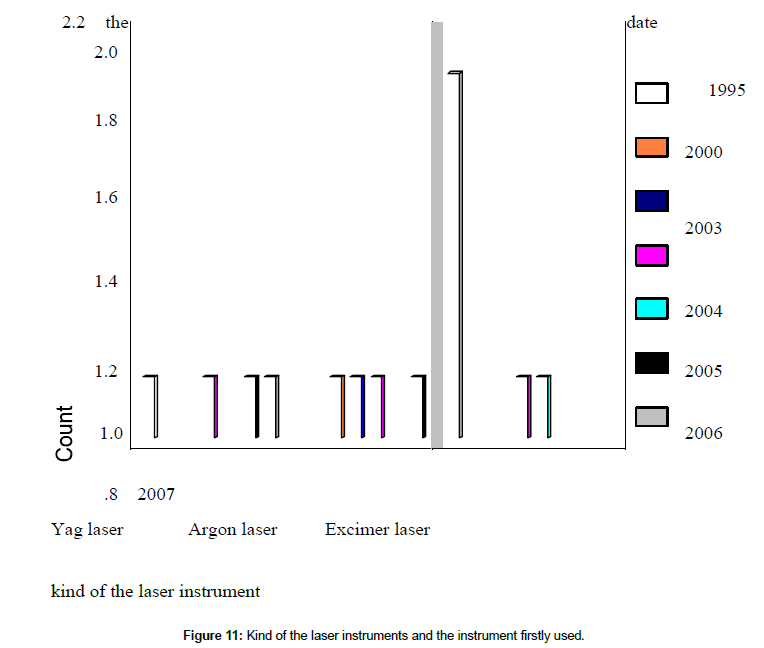
From Table 5 we find that the first laser instrument used in the Khartoum state is the Yag laser instrument which was firstly used in 1995. No other laser instrument was used until the years 2000- 2003 when the Argon laser instrument was firstly used. After 2003 another laser instrument (Excimer laser instrument) began to be used together with Argon laser and Yag laser instruments in specialized ophthalmology hospitals (Figures 11 and 12).
| Kind of the laser instrument | The instrument firstly used | Total | |||||||
|---|---|---|---|---|---|---|---|---|---|
| 1995 | 2000 | 2003 | 2004 | 2005 | 2006 | 2007 | |||
| Yag laser | Count | 1 | 1 | 1 | 1 | 4 | |||
| % of Total | 8.3% | 8.3% | 8.3% | 8.3% | 33.3 % | ||||
| Argon laser | Count | 1 | 1 | 1 | 1 | 2 | 6 | ||
| % of Total | 8.3% | 8.3% | 8.3% | 8.3% | 16.7% | 50.0 % | |||
| Excimer | Count | 1 | 1 | 2 | |||||
| laser | % of Total | 8.3% | 8.3% | 16.7 % | |||||
| Total | Count | 1 | 1 | 1 | 3 | 1 | 2 | 3 | 12 |
| % of Total | 8.3% | 8.3% | 8.3% | 25.0% | 8.3% | 16.7% | 25.0% | 100.0 % | |
Table 5: Kind of the laser instruments the instrument firstly used.
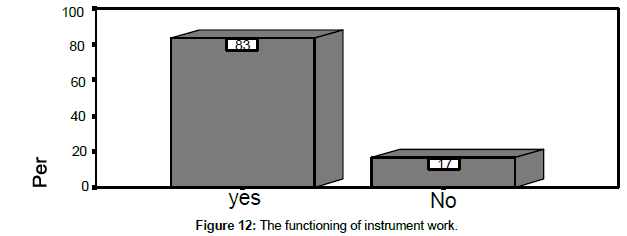
In the Table 6 we notice that the rate of the instruments functioning well is 83.3% and the rate of those don’t work due to the lack of the spare parts and experienced engineers and technicians is 16.7% (Table 7).
| Answer | Frequency | Percent |
|---|---|---|
| Yes | 10 | 83.3 |
| No | 2 | 16.7 |
| Total | 12 | 100.0 |
Table 6: The functioning of instrument work.
| Answer | Frequency | Percent |
|---|---|---|
| Yes | 3 | 25.0 |
| No | 9 | 75.0 |
| Total | 12 | 100.0 |
Table 7: The availability of the repairing centers.
From Table 8 we notice that the laser instruments repairing centers are not available according to what is needed. There is a shortage at the rate of 75%. The rate of what is really available is 25%. That is because there are not enough experienced medical Engineers and technicians to repair these instruments. The shortage of the spare parts is about 75% (Table 8).
| Answer | Frequency | Percent |
|---|---|---|
| Yes | 3 | 25.0 |
| No | 9 | 75.0 |
| Total | 12 | 100.0 |
Table 8: The availability of the spare parts.
Status of Laser Development in India
The research and development work in the field of lasers started in our country 28 years back on a very small scale at a few research laboratories of the Defence Research & Development IISc, Bangalore. Later, a number of research laboratories and teaching institutions also entered into this area. A Study Group on Lasers, constituted in 1971 by DRDO, and INSA Laser Committee constituted under the Chairmanship of Prof. P Venkateswarlu in 1976 (the author was a member of the two committees) made detailed studies to assess the status of R&D work on laser at both international and national levels and gave suitable recommendations for development of lasers and laser systems in the country. In 1988, Dr DD Bhawalkar, Director, Centre for Advanced Technology (CAT), Indore, gave a status report on lasers to the Science Advisory Council to the Prime Minister. Very briefly the current status of the laser work in the country is outlined below: Ruby, Nd:YAG and Nd:Glass Lasers Laser rods of ruby, Nd:glass, flash lamps and hard coated laser mirrors, have been developed indigenously at the Defence Science Centre (DSC), Delhi, and the solid sate lasers giving peak power output of a few megawatts have been developed for Defence applications. BARC has also developed these lasers with mainly imported components, Laser range finders with Nd:YAG or Nd:glass as the active element have been developed at Instruments Research Development Establishment(IRDE), Dehradun and DSC. CAT, is developing a high power Nd:glass laser for atomic energy application, Helium- Neon Laser Helium-Neon lasers of low power output (2-5 mW) with lifetimes of a few thousand hours have been developed at IISc, NPL, and Bharat Electronics Ltd., Bangalore. The technology has been transferred by NPL to M/s Laser Instruments, New Delhi and by BARC, Bombay to ECIL, Hyderabad. they started production of these lasers commercially about 20 years back but stopped production since their performance is far from satisfactory. BEL also made an attempt about 10 years back and stopped production due to lack of sufficient technology Carbon Dioxide Laser Carbon dioxide lasers giving an output power in the range 10-100 W have been developed at BARC IIT, Kanpur, IRDE and DSC, Central Electronics Ltd. (CEL) and Jyoti Ltd. have started commercial production of these lasers around 1975 but have stopped production by 1982. CAT has developed transverse carbon dioxide laser with 3.5 kW power. Semiconductor Laser BARC and Solid State Physics Laboratory (SPL), Delhi have developed low power gallium-arsenide lasers with a view to use them for applications in communication and ranging. BARC demonstrated communication over 20 Km distance using laser. Further work is necessary to develop these lasers with heterostructures and to improve their efficiency. Materials Basic laser materials like ruby, Nd:phosphate glass and lithium niobate are being developed at DSC for Defence applications, Central Glass and Ceramics Research Institute, Calcutta (CGCRI), has also developed good quality Nd:silicate glass for commercial applications. The development of gallium-arsenide and Nd:YAG crystals is under process at SPL. Several establishments and institutes like DSC, IRDE, IISc, NPL, BARC, IIT, Kanpur and BEL have established optical workshops including coating facilities to fabricate laser components. Good experience has been gained to fabricate laser rods and hard coated laser morrors at DSC Fibre-Optic Communication In 1980, a panel on Optical Fibre Communication System constituted by the Electronics Commission recommended the introduction of optical fibre communication in India. With this in view, CGCRI took up an R&D project on indigenous development of optical communication fibre. In 1982, a System Appraisal Group for Optical Fibre and Cables comprising representatives of the Department of Electronics, Ministry of Defence, IIT, De/hi, Telecommunication Research Centre (TRC) and Hindustan Cables Ltd. recommended setting up of R&D and manufacturing facilities of optical fibres and cables at HCL through collaborative arrangement. It was decided to manufacture at HCL the multimode graded index fibre with’ 3 to 5 db/km loss and bandwidth up to 100 MHz. Similarly, the production of optical fibre has been started at OPTEL, Bhopal with foreign collaboration. In 1983, a Committee on Optical Fibres and Cables (COFC) was constituted by the Ministry of Communication to finalise the technical specifications for optical fibres and cables required not only for communications, but also for Defence and other sectors. The Department of Communications has successfully installed the optical fibre cable and an 8 Mb system to provide junctions between two exchanges in the Pune Telephone system. TRC has taken up a design of an indigenous 34 Mb system to be installed between Thana and Powai in the Bombay Telephone system. Efforts are on1e way to introduce optical fibre communication several trunk routes in the country. Facilities for 93 characterisation of optical fibres have been set up at HCL and IIT, Delhi. Organisation, Bhabha Atomic Research Centre, National Physical Laboratory, IIT, Kanpur.
The Laser Future
The possibility that one day the classic sheet metal cutting machine would be fitted with a fiber laser is not something unconceivable, according to Trump. The metal machining giant says that recent developments would not dissuade the company from believing that this was not impossible. In India CO2 lasers are the most popular choice in the sheet metal industry. However, Theron says that the future of laser in the Australian sheet-metal and fabrication industry might not always be dominated by the CO2 laser. Time and willingness on the part of metal fabricators and process to invest in newer technology suited to the application at hand could see solidstate laser partially unseat the CO2. Scientific Research Lasers have opened new fields of investigation in science and technology. It has given physics a versatile tool for the study of interaction of light and matter. The powerful beam of laser has become an important tool for spectroscopic analysis. A laser system, known as microprobe, is used for exciting emission from solid samples for spectrographic analysis. In 1928, Prof. CV Raman discovered a new phenomenon, known as Raman Effect. by which molecular structures of different substances can be investigated by passing monochromatic light through them. He found that when light passes through a transparent substance, it is scattered and emerges with a change of frequency caused due to the vibration of molecules in the substance. This produces additional lines (known as Raman lines) in the scattered light spectrum. The discovery of laser is a great boon for recording the Raman spectra. The use of lasers has enabled recording of Raman lines within seconds, which otherwise would require long exposure times of or few hours using ordinary light sources. The analysis of Raman lines gives the fundamental properties of the substances. Similarly, lasers can also be used for analyzing liquids. A laser beam, when passed through a liquid, gives several colors (wavelengths) and the process is called fluorescence. The study of the fluorescence spectra thus obtained gives the properties of the liquids. Lasers offer attractive possibilities in terms of the exploration of molecular structure and determination of nature of chemical reactions. A laser beam can initiate and hasten a chemical reaction. Since different reactions require different wavelengths of light, a ‘tunable’ laser (i.e., a source whose wavelength can be altered as in radio tuning) is of immense help to a chemist. Tunable lasers, particularly dye lasers, now cover the entire visible spectrum and have revolutionized optical spectroscopy. In photochemistry, lasers with short duration pulses are highly useful for inducing and monitoring ultrafast chemical reactions more efficiently than by any conventional method. Laser also finds application in biological research. Using laser techniques, biological studies have been carried out in enzymes, proteins, cellular components and isolated cells, microorganisms, tissue culture, isolated physiological systems individual organs, etc. Using a ruby laser coupled with a microscope, single cells have been irradiated with laser beams focused on to a spot of the order of one micron to destroy individual chromosomes, thus making available a highly delicate instrument for genetic studies. It is also possible to produce laser beams as narrow as the diameter of a protein molecule and use it to alter genetic properties of living organisms [17-19].
Conclusion
The aim of this work is to show the different methods of the applications of laser in medicine. Lasers are classified according to their active medium. Some of the important medical lasers are; Neodymium-YAG Laser (Nd-YAG), Argon Laser (Ar+), Carbon Dioxide Laser (CO2), and Dye Laser. Laser has special properties that makes it more important and useful than many other substances or instruments that are used in medicine. Some of its properties are, laser light has small divergence of beam & it has high energy. It has proved its great ability and benefits in the different fields of medicine especially surgery because it reduces blood loss due to the operation cutting, and including most of its branches i.e. gynecology, ophthalmology, dermatology, and others. Moreover laser has short pulses of light. This reduces pain and yields more rapid recovery to the patient. As the laser beam is very tiny the damage in adjacent tissues is very limited. In laser operations the surgeon uses few instruments. This enables the surgeon to have a clear vision of the spot of the operation. Laser operation causes no wounds so the patient can leave the hospital immediately after the operation. Laser operations have become more efficient, perfect and accurate due to the application of the computer control. The relationship between the different laser beams and the tissues depends on the properties of the laser beam according to its wavelengths, and its intensity. The laser instruments were firstly used in the Khartoum state science 1995. Now the laser instruments which are used in the specialized ophthalmology hospitals are: Argon Laser, Yag Laser and Excimer Laser Instruments. The number of the Excimer laser instruments is few because it is not found in many hospitals because the cost of its treatment is too expensive for the patients. The difficulties that face the wide use of the laser instruments are due to: The shortage in the repairing centers of the medical engineers and technicians and the lack of spare parts. In general lasers have many hazards, some of the important hazards are: radiation, explosive, electrical, and toxic hazards. Due to these hazards it is very important that all the safety precautions requirements should be available in the hospital where the laser system is used. These safety precautions are: laser instrument should only be used by qualified and experienced technicians, surgeons and physicians. The laser instruments must be kept away from those who misuse them. These instruments must be occasionally checked, tested and maintained [20].
References
- Kandela SA (1991) Laser physics in medicine, AL Hekima, Bagdad, Iraq.
- http:// www.arab-eng.org/vb/t55706.html.
- Ball K (2016) Lasers the perioperative challenge, 2nd Edtn, Nabcy L. Coon, USA.
- Steen WM (2015) Laser materials processing, 2nd Edtn, Springer, Berlin, Germany.
- Mayers RA (2011) Encyclopedia of lasers & optical technology, 1st Edtn, Academic Press, Elsevier, United States.
- http://www.shorelaser.com/aboutlasermed.html.
- Hecht J (1971) The laser and applications layers, Francis, London.
- Hecht J (2003) Laser guide, Donnelly and Son Company, Chicago, Illinois, United States.
- Svelto O (2009) Principles of Lasers, 4th Edtn, London, Springer, Berlin, Germany.
- Verdeyen JT (2000) Laser electronics, 3rd Edtn, New Jersey, United States.
- Javan A, Bennett WR, Herriot DR (2005) Population inversion and continuous optical maser oscillation in a gas discharge containing a He-Ne mixture. Phy Rev Lett 6: 106-110.
- Silfast WT (2004) Laser fundamentals, 2nd Edtn, Cambridge University Press, London.
- Nambiar KR (2004) Laser principle’s types and applications, New age international P limited, Hyderabad, Telangana.
- Ready JF (1997) Industrial applications of laser, 2nd Edtn, Academic press, USA.
- Duarte FJ (2009) Tunable laser applications,2nd Edtn, CRC Press, United States.
- Duarte FJ (2016) Tunable Laser Applications, 3rd Edtn, CRC Press, United States.
- https://www.forbes.com/forbes/2007/0423/042.html#2d382874b680
- teHighEnergyLaserSystems/Pages/JointHighPowerSolidStateLaser.aspx
- https://en.wikipedia.org/wiki/Los_Angeles_Times
- http://www.foxnews.com/tech/2011/04/08/navy-showboats-destructive-new-laser-gun.html?test=faces
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi