Research Article, Res Rep Gastroenterol Vol: 4 Issue: 2
The Relation between Helicobacter Pylori Infection, Serum Ammonia and Hepatic Encephalopathy in Yemeni Cirrhotic Patients
Mansour A Al-Amrani1* and Ali Ahmed Al-Zaazaai2
1Department of Hepatology and Gastroenterology, Sana, Yemen
2Department of Clinical Pharmacy, Wenzhou Medical University, Zhejiang Province, China
*Corresponding Author : Mansour A Al-Amrani
Department of Hepatology and Gastroenterology, Faculty of Medicine in Sana'a, Yemen
Tel: 00967- 777112929
E-Mail: mansourendoscope@gmail.com
Received date: April 29, 2020; Accepted date: May 14, 2020; Published date: May 21, 2020
Citation: Al-Amrani MA, Al-Zaazaai AA (2020) The Relation between Helicobacter Pylori Infection, Serum Ammonia and Hepatic Encephalopathy in Yemeni Cirrhotic Patients. Res Rep Gastroenterol 4:1. doi: 10.37532/rrg.2020.4(1).111
Abstract
Introduction: Helicobacter pylori (H. pylori) infection in the group of patients with liver cirrhosis may affect the exacerbation of inflammatory injuries in the stomach, which could directly, and indirectly, lead to loss of liver function.
Aim of the study: Assessment of possible relation among H. pylori infection, serum ammonia, and hepatic encephalopathy in the middle of patients with liver cirrhosis.
Patients and methods: This study was conducted in the Hepatobiliary-Gastroenterology Specialized Research Center in Sana'a City Yemen. This is a prospective study and patients from April 2008 to April 2014 were collected. All patients with established Chronic Liver Disease (CLD) with hepatic encephalopathy.
Result:A total of 78 patients with liver cirrhosis included in the present study, there were selected, (n=42; 54%) were males and (n=36; 46%) were females. Clinical and demographic characteristics of the study patients were shown H.E grade had the most significant relationship with H. pylori state (p=0.000). There was a significant relation between stage A, B, C, and H. pylori state (p=0.09).
Conclusion:This study comes to more reliable and confident that is a highly significant association among H. pylori infection, Hepatic Encephalopathy, stage A, B, C, and serum ammonia in cirrhotic patients.
Keywords: Helicobacter pylori infection, Hepatic encephalopathy, Serum ammonia, cirrhotic patients
Introduction
Helicobacter pylori bacteria are rich in the urease enzyme and are recognized to produce ammonia from urea that is fast absorbed from the gastric lumen into circulation. Infection with these bacteria has been shown to be related to elevated blood ammonia levels and repeated attacks of obvious hepatic encephalopathy [1]. The most common biochemical irregularity in patients with chronic Hepatic Encephalopathy (HE) is hyperammonemia [2,3]. Elevated blood ammonia levels have similarly been implicated in the causality of HE [4]. Infection with these bacteria is one of the most common in the world. In highly developed countries, 50% of the population is infected, whereas in the developing countries the percentage reaches as much as 90% [5]. H. pylori infection in the assembly of patients with liver cirrhosis may impact the exacerbation of inflammatory injuries in the stomach, which could directly, and indirectly, lead to deficiency of liver function. This is mainly dangerous in patients with progressive liver disease [6].
In this regard, two theories have been postulated regarding the relationship between H. pylori infection and HE which showed that ammonia has still an essential role in the pathogenesis of hepatic encephalopathy [7]. HE in its numerous grades, according to the West Haven Criteria, is assessed to be present in 30%-45% of individuals with Liver Cirrhosis (LC), while approximately 60%-80% of these individuals show cognitive dysfunction in specified testing. All clinical appearances of HE is considered by the nonappearance of any physical cerebral changes and are possibly changeable by adequate therapeutic management [8,9]. Only a minority of gastroenterologists are prepared to test for HE. In a survey conducted in the USA, 38% of the members of the American Association for the Study of Liver Diseases had never tested for it, although the majority (84%) is aware of the medical problem and the need to test for it [10]. There are only a few data published so far from small prospective clinical studies on the role of H. pylori in subclinical HE, and their findings are inconsistent [11,12]. Elevated levels of ammonia could deteriorate hepatic encephalopathy. As a result, it can be suggested that Helicobacter Pylori infection may possibly contribute to the progress of hepatic encephalopathy [13]. A number of studies showed that ammonia levels both in gastric juice and blood were significantly developed in cirrhotic patients with H. pylori infection than those without [1,14]. The aim of our study was Assessment of possible relation among H. pylori infection, serum ammonia, and hepatic encephalopathy in the middle of patients with liver cirrhosis, and also an assessment of clinical and laboratory characteristics of cirrhotic patients (etiology, age, sex and stage of LC in relation to H. pylori infection.
Patients and Methods
This study was conducted in the Hepatobiliary-Gastroenterology Specialized Research Center in Sana'a City, Yemen. This is a prospective study and patients from April 2008 to April 2014 were collected. The total number of patients included in this study was 78 patients divided into age groups. They included 42 males and 36 females. According to the etiology of liver cirrhosis, the patients were categorized into the following groups: Group 1: HBV, Group 2: HCV, Group 3: schistosomiasis. Group 4: Autoimmune, Group 5: Idiopathic. Serum ammonia level was expressed as normal (Less than 60 micromol/L) were 10 patients – Mild elevation (60-100 micromol/L) were 38 patients – marked elevation (more than 100 micromol/L) were 30 patients. According to the stage of liver cirrhosis A, B, C, all patients with established Chronic Liver Disease (CLD) with HE. CLD was diagnosed on the basis of the clinical features like finger clubbing, palmar erythema, spider naevi, splenomegaly, hepatomegaly or shrunken liver, or the persistent elevation for more than 6 months of the liver enzymes. Plus a positive abdominal ultrasound for irregular liver margins, coarse liver appearance, and a dilated portal vein > 12mmor). To assess the severity of the liver disease, the patients were scored according to the Child-Pugh classification. This mark is established on the grade of encephalopathy, the existence of ascites, prothrombin time, and the serum levels of bilirubin, and albumin. Accordingly, the patients had either compensated liver disease (Class A, 5-6 points), moderate liver disease (Class B, 7-9 points), or severe liver disease (Class C, 10-15 points).
Diagnosis of viral etiology based on Hepatitis B surface antigen/ Hepatitis C Virus (HBsAg/HCV Ab PCR while Autoimmune depends on sever sero immune markers – ve viral marker hypergamaglobulinemia response to immunosuppressive therapy Schistosomiasis a liver disease depend on the sch.Ag, rectal snip. Whereas idiopathic CLD based on –ve viral, autoimmune markers, -ve evidence for schistosomiasis normal metabolic or even a liver biopsy. Assessment of HE was clinically as well as psychometric test diagnosis of H. pylori infection was made by stool Ag, Universal Backup Tool (UBT), Endoscopy with clo test or biopsy histopathology.
Ammonia measurement
Fasting venous blood samples were obtained from each patient to measure ammonia concentration (micromole/L), according to the manufacturer's instructions.
Inclusion criteria
All Yemeni patients with liver cirrhosis complaining of manifestations suggestive of hepatic encephalopathy whatever the grade. These patients are suffering from liver cirrhosis of different stages and due to different etiologies.
Exclusion criteria
Patients with liver cirrhosis with HCC, advanced renal and cardiac diseases
Statistical Analysis
Data were stored and analyzed by the statistical program, Statistical Package for the Social Sciences (SPSS) Version 16. All the quantitative variables corresponding age, blood ammonia levels, and so out were analyzed for mean+standard duration. Frequencies and proportions were calculated for the quantitative variables like gender, Child-Pugh grade (CP grade). Hyperammonemia was stratified amongst disease severity grade (CP grade) to see effect modification. Statistical significance was established at p value<0.05 was taken as a criterion standard.
Results
A total of 78 patients with LC included in the present study, there were selected, (n=42; 54%) were males and (n=36; 46%) were females. Clinical and demographic characteristics of the study patients were shown H. pylori state (Figure 1) had the most significant relationship with H.E grade, stage A, B, C, and serum ammonia (p=0.000, p=0.009, p=0.041 respectively) (Table 1).
H.pylori p valuesNegative –Positive +Count%Count%H.EGrade 1211%3253%0.000*Grade 21583%1830%significantGrade 316%1017% StageA633%47%0.009*B739%2542%significantC528%3152% Serum AmmoniaNormal528%58%0.041*Mild844%2237%significantMarked528%3355%
Table 1: Show the relation between H.E, stage, s. ammonia with H. pylori state.
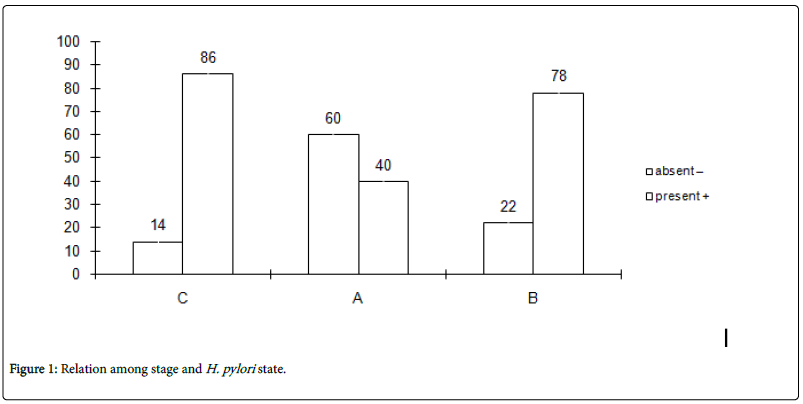
Figure 1: Relation among stage and H. pylori state.
Relation H. pylori with H.E grade 1, found patients (n=2; 11%) were negative, and (n=32; 53%) were positive. While in grade 2, found patients (n=15; 83%) were negative, and (n=18; 30%) were positive. Compared with grade 3, found patients (n=1; 6%) were negative, and (n=10; 17%) were positive (Table 1). Additionally, the present study shown H. E in grade 1 in autoimmune patients (n=3; 21%), HBV patients (n=2; 14%), HCV patients (n=12; 67%), idiopathic patients (n=8; 50%) and Schistosoma patients (n=9; 56%). On the other hand, H.E in grade 2 in autoimmune patients (n=6; 43%), HBV patients (n=11; 79%), HCV patients (n=3; 17%), idiopathic patients (n=6; 38%) and Schistosoma patients (n=7; 44%). This study found significant relationship between H.E and etiology of liver cirrhosis (p=0.005). Whereas shown non-significant relation among H. pylori infection with etiology of liver disease (p=0.250).Moreover,in the stage (A, B, C) there was non-significant correlation between Child-Pugh class and etiology in liver cirrhosis (p=0.920). Similarly, there was nonsignificant association between serum ammonia and etiology in liver cirrhosis (Table 2).
ETIOLOGYP valuesAutoimmuneHBVHCVIdeopathicSchistosomalCount%Count%Count%Count%Count%H.EGRADE 1321%214%1267%850%956%0.005GRADE 2643%1179%317%638%744%SignificantGRADE 3536%17%317%213%00% H. pyloriNegative –429%536%16%319%531%0.25Positive+1071%964%1794%1381%1169%Non-significantSerum AmmoniaNormal00%321%422%16%213%0.373Mild750%536%528%956%425%Non-significantMarked750%643%950%638%1063% A214%214%211%319%16%0.92StageB750%643%844%425%744%Non-significant C536%643%844%956%850%
Table 2: The relation between H. pylori, H.E, stage, serum ammonia with etiology.
In Figure 1: We found percentage relation H. pylori (positive +) with stage C were higher than stage B and stage C. whereas, percentage H. pylori (negative -) with stage C were lesser than stage A and stage B.
Despite the fact, there were non-significant among etiology (autoimmune, Hepatitis B virus (HBV), Hepatitis C Virus (HCV), idiopathic, Schistosoma), serum ammonia (Figure 2), H.E, H. pylori, and stage (Child-Pugh class),with age (Table 3). On the other hand, there was non-significant difference between H. pylori, etiology (autoimmune, HBV, HCV, idiopathic, Schistosoma), serum ammonia, H.E, and stage (Child-Pugh class), with sex (Table 4). The present study found non-significant in relation among patients H.E, and serum ammonia (p=0.435). This study shown relation serum ammonia level with H.E grade which shown percentage in grade 1 expressed as normal (Less than 60 micromol/L) were (n=3; 30%) patients – Mild elevation (60-100 micromol/L) were (n=15; 50%) patients – marked elevation (more than 100 micromol/L) were (n=16; 42%) patients. In the other hand, percentage in grade 2 expressed as normal (Less than 60 micromol/L) were (n = 4; 40%) patients – Mild elevation (60-100 micromol/L) were (n=13; 43%) patients – marked elevation (more than 100 micromol/L) were (n=16; 42%) patients. Moreover, percentage in grade 3 expressed as normal (Less than 60 micromol/L) were (n=3; 30%) patients – Mild elevation (60-100 micromol/L) were (n=2; 7%) patients – marked elevation (more than 100 micromol/L) were (n=6; 16%) patients (Table 5).
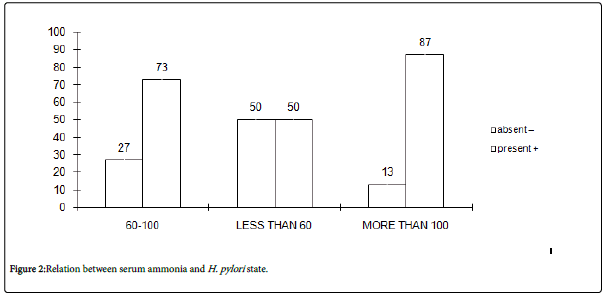
Figure 2: Relation between serum ammonia and H. pylori state.
AGEp values20-60 yearsfewer than 20 yearshigher than 60 yearsCount%Count%Count%EtiologyAutoimmune1322%150%00%0.178HBV1220%00%212%Non-significantHCV1119%00%741% Ideopathic1322%00%318% Schistosomal1017%150%529% Serum AmmoniaNormal610%00%424% Mild2542%00%529%0.334Marked2847%2100%847%Non-significantH.EGrade 12746%00%741%0.555Grade 22441%150%847%Non-significantGrade 3814%150%212% H. pyloriNegative–1322%00%529%0.6Non-significantPositive +4678%2100%1271% StageA915%00%16% 0.839B2339%150%847%Non-significantC2746%150%847%
Table 3: Relation among H. pylori, H.E, stage, serum ammonia, etiology with age.
Table 4: shown relation among H. pylori, H.E, stage, serum ammonia and etiology with sex.
Table 5: Relation between H.E and serum ammonia.
In Figure 2: We found percentage H. pylori (positive +) with serum ammonia more than 100 were 87%, less than 60 were 50% and 60 -100 were 73%. Compared, H. pylori (negative -) with serum ammonia more than 100 were 13%, less than 60 were 50% and 60-100 were 27%.
Discussion
The pathogenesis of H.E is still poorly understood, but raised systemic ammonia concentration as a consequence of shunting of ammonia-rich portal blood away from the liver and impaired urea genesis have long been causally implicated in its development. H. pylori urease activity in the cirrhotic stomach has been proposed to represent a significant source of ammonia, contributing to the development of H.E. This study showed patients were H.E grade the most significant relationship with H. pylori state (p=0.000). Another study by DR. JAHANGIR LIAQUAT(15) et al. found the H. pylori was observed to be rising with the severity of hepatic encephalopathy [15]. Similarly, the study by El-seida [16], et al. exposed a highly significant association between H. pylori infection and MHE in cirrhotic patients [16].
However, the above study confirms with our study. In the present study, we found a significant association between stage (A, B, C) and H. pylori state. The Previous study by Sherweet M. Ibrahim [17] et al. found a non-significant difference in Child-Pugh class, hepatic encephalopathy grade and precipitating factors of HE between H pylori-positive and negative groups [17]. Whereas, our study found a significant relation between Child-Pugh class and H. pylori state (p=0.009). On the other hand, the previous study by Ibrahim [17] et al. opposed with our study. Additionally, the study by Masood [18] et al. found Patients with HE and H. pylori infection exposed a significant decrease in blood ammonia levels after anti-H. pylori treatment (p< 0.001) [18]. The current study found H. pylori and blood ammonia levels were significantly increased with the severity and mark of hepatic encephalopathy, which proposes that H. pylori infection may have a role in the pathogenesis of hepatic encephalopathy. Consequently, our study confirms with the above study by Masood et al. However, because of the inadequate number of published studies and procedural errors of the studies included in the past, more enormous randomized studies are necessary in order to supplementary confirm this association. But come to our study more reliable and confident. A Previous study by Pogorzelskaa [6] shown H. pylori infection was diagnosed in 69 (46.9%) patients, usually among those chronically infected with HBV or HCV. The incidence of H. pylori infection among patients with post-inflammatory liver cirrhosis was significantly higher (P=0.001), as compared with patients with alcoholic liver cirrhosis [6]. However, the previous study by Pogorzelskaa et al. opposite our study which found non-significant relation between H. pylori infection patients with etiology of liver cirrhosis. Another study by AvinashA[19] et al. Presence of MHE had a non-significant relationship with age, sex, Child-Pugh grade, and cause of cirrhosis [19]. But, different from our study which shown found a significant relationship between HE and causes of liver cirrhosis (p= 0.005).In our study, we found non-significant between stages, serum ammonia with the etiology of liver cirrhosis. On the other hand, the present study showed non-significant relation among H. pylori, H.E, stage, serum ammonia, etiology with age.Another study by Rekha [11] shown there was no statistically significant difference between the two groups (p > 0.05). The blood ammonia values are shown in Child-Pugh A, B, and C class of patients were non-significant different (p > 0.05) in the positive or negative of H. pylori infection [11]. However, the above study confirms with our study. The present study found non-significant relation among H. pylori, H.E, stage, serum ammonia and etiology with sex. Another study by Mohamed [20] shown non-significant groups regarding Age and Sex. This confirms with our study about non-significant for age and sex.The present study showed a nonsignificant relation between H.E and serum ammonia. It is concluded that Helicobacter pylori do not contribute significantly to blood ammonia levels and the severity of hepatic encephalopathy which confirms with our study. In the present study shown Figure 3: relation H. pylori state with etiology which found percentage H. pylori (positive +) with HCV (94%) were higher than others etiology.
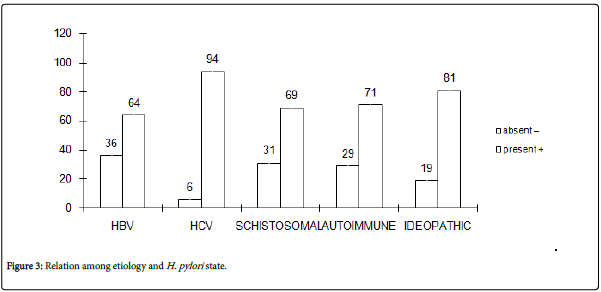
Figure 3: Relation among etiology and H. pylori state.
In Figure 3:Shown relation H. pylori state with etiology which found percentage H. pylori (positive +) with HCV (94%) were higher than other etiology. Compared, percentage (H. pylori negative -) with also HCV (6%) was lesser than others etiology but with HBV were higher than other etiology.
Compared, percentage (H. pylori-negative -) with also HCV (6%) was lesser than other etiology but with HBV was higher than other etiology. Moreover, Another study by Pogorzelskaa [6] et al shown Figure 4. Helicobacter pylori infection in different groups of patients. Hepatitis B Virus(HBV); Hepatitis C Virus(HCV); Primary Biliary Cirrhosis (PBC) which found, hepatitis B virus higher than others [6].
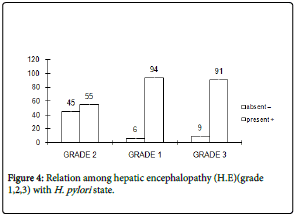
Figure 4: Relation among hepatic encephalopathy (H.E)(grade 1,2,3) with H. pylori state.
In Figure 4: This study found percentage relation H. pylori (positive +) with grade 1 were higher than grade 2 and grade 3. Whereas, percentage H. pylori (negative -) with grade 1 were lower than grade 2 and grade 3.
Conclusion
This study comes to more reliable and confident that is a highly significant association among H. pylori infection, hepatic encephalopathy, stage A B C and serum ammonia in cirrhotic patients. But found non-significant relation H. pylori infection with the etiology of liver disease. Whereas found a significant relationship between H.E and etiology of cirrhosis. Therefore, H. pylori infection is an effective curable risk factor for the clinical controlling of hepatic encephalopathy. There may be a role of anti-H. pylori therapy in patients of hepatic encephalopathy and should be studied additional.
Acknowledgment
For our colleagues Professor Dr. Mansour A. Al-Amrani, PhD. of Hepatology and Gastroenterology, Faculty of Medicine in Sana'a Yemen. The authors would like to thank the professor. Dr. Xiao Jian. Clinical Pharmacology from Wenzhou Medical University, Wenzhou Zhejiang Province, PR China who helped in arranging this paper for publication.
Authors’ Contribution
Prof. Dr.Mansour A. Al-Amrani: Study concept and design, data acquisition, interpretation; manuscript drafting, study supervision, the idea of the manuscript, collection, writing and literature review.
Dr. Ali Al-Zaazaai: Revision of the manuscript for important intellectual content, analysis, and publishing.
Financial Support
This research received a specific grant from Professor Mansour Al- Amrani.
Conflict of Interest Statement
A statement is declared for no conflict of interest.
References
- Gubbins GP, Moritz TE, Marsano LS (1993) The Veterans Administration Cooperative Study Group No. 275. Helicobacter pylori is a risk factor for hepatic encephalopathy in acute alcoholic hepatitis: The ammonia hypothesis revised. Am J Gastroenterol 88: 1907-1909.
- Quero JC, Michael G, , , Schalm SW, et al. (2000) Screening of Subclinical hepatic encephalopathy. Semin Liver Dis 32: 748-753.
- Dhiman RK, Saraswat VA, Verma M (1995) Figure connection test: a universal test for assessment of mental state. J Gastroenterol Hepatol 10:14-23.
- Michael G, , ,
- Schiff ER, Sorrell MF, Willis CM (1999) Schiff’s Disease of the Liver (8th ed) Philadelphia: Lippincott-Raven, p:144.
- Pogorzelsk J, Magda T, Alicja K, Tadeusz WT, Robert F (2017) Helicobacter pylori infection among patients with liver cirrhosis. Eur. J. Gastroenterol. Hepatol 29:1161-1165.
- Mitchell H, Katelaris P (2016) Epidemiology, clinical impacts and current clinical management of Helicobacter pylori infection. Med J Aust 10: 376–380.
- Abdel-Hady H, Zaki A, Badra G, Lotfy M, Selmi C, et al. (2007) Helicobacter pylori infection in hepatic encephalopathy: Relationship to plasma endotoxins and blood ammonia. Hepatol Res 37: 1026-1033.
- Stewart CA, Smith GE (2007) Minimal hepatic encephalopathy. Nat Clin Pract Gastroenterol Hepatol4: 677-685.
- Häussinger D, Schliess F (2008) Pathogenetic mechanisms of hepatic encephalopathy. Gut 57: 1156-1165.
- Bajaj JS, Etemadian A, Hafeezullah M, and Saeian K (2007) Testing for minimal hepatic encephalopathy in the United States: An AASLD survey . Hepatology 45: 833-834.
- Rekha C, Phanidhar S, Sagar AV, Revathi A, and Asra WA (2007) Role of Helicobacter pylori and hyperammonemia in subclinical hepatic encephalopathy in cirrhosis of liver. Indian J Clin Biochem 22 : 136-139.
- Kini D, Aggarwal R, Saraswat VA, Naik SR (2001) Role of Helicobacter pylori infection in hyperammonemia and subclinical hepatic encephalopathy in cirrhosis of liver. Indian J Gastroenterol 20: 237-240.
- Dasani BM, Sigal SH, and Lieber CS (1998) Analysis of risk factors for chronic hepatic encephalopathy: the role of Helicobacter pylori infection. Am J Gastroenterol 93: 726-731.
- Chakrabarti P, Zullo A, Hassan C, Pandit A, Chowdhury A, et al. (2002) Helicobacter pylori, gastric juice, and arterial ammonia levels in patients with cirrhosis. J Clin Gastroenterol 34:578-81.
- DR.Jahangir L, MR.Iftikhar K, and MR.Mukhtiar A (2012) HELICOBACTER PYLORI & HEPATIC ENCEPHALOPATHY. Professional Med J 19: 063-067.
- Seham S. El-seida, Fatma A. Attiaa, Mona Abd El-Raoufa, et al. (2015) The role of Helicobacter pylori in minimal hepatic encephalopathy. Egypt J Intern Med 27:26-31.
- Salama MG, Sami EW, Sherweet MI, and Yosri EM (2012) Helicobacter Pylori Infection / Hepatic Encephalopathy Inter-Relationship before and after its Eradication. Afro-Egypt J Infect Endem Dis 2: 69-76.
- Dr Huma M, Dr Humna F, Dr Sharoon S (2019) Study to evaluate role of helicobacter pylori infection in the pathogenesis of minimal hepatic encephalopathy and effect of its eradication at mayo hospital lahore.Indo Am J P Sci 06: 14955-14959.
- Avinash A, Alok G, Mam C, Sciddhartha K (2011) Role of Helicobacter pylori infection in the pathogenesis of minimal hepatic encephalopathy and effect of its eradication. Indian J Gastroenterol 30:29-32.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi