Research Article, Int J Cardiovasc Res Vol: 9 Issue: 2
Two Dimensional Speckle Tracking Echocardiography Assessment of Left Ventricular Remodeling in Patients after Myocardial Infarction
Moustafa Kamal Eldin Ibrahim*, Khalid A. El-khashab and Tamer M. Ragab
Department of Cardiology, Fayoum University, Egypt
*Corresponding Author: Dr. Moustafa Kamal Eldin Ibrahim Khalil Saad
Faculty of Medicine, Fayoum University, Gamma St., Keman Square, Fayoum, Egypt
Tel: 002-01011404855
E-mail: moustafa19688@mail.com
Received: March 7, 2020 Accepted: April 04, 2020 Published: April 11, 2020
Citation: Ibrahim MKE, El-khashab KA, Ragab TM (2020) Two Dimensional Speckle Tracking Echocardiography Assessment of Left Ventricular Remodeling in Patients after Myocardial Infarction. Int J Cardiovasc Res 9:2. doi: 10.37532/icrj.2020.9(2).397
Abstract
Background: Adverse Left Ventricular Remodelling (LVR), defined as progressive ventricular dilatation, distortion of chamber shape, myocardial hypertrophy and deteriorating function, begins in some patients who suffered from Acute Myocardial Infarction (AMI), sometimes even after successful Percutaneous Coronary Intervention (PCI). If uninterrupted, it could lead to Congestive Heart Failure (CHF) and a poor clinical outcome. Aims: This study aims at evaluating the value of Speckle Tracking Echocardiography (STE) in predicting LVR after successful PCI in AMI patients. Materials and Methods: Eighty-four AMI patients had a complete echocardiographic study, including speckle tracking, performed two days after PCI and then two months afterwards. The patients were then divided into two groups based on the presenceh of remodelling; R+ (remodelling) group and R- (non-remodelling) group. Results: At the baseline study, group R+ showed significantly lower strain parameters than group R-. These included Global Longitudinal Strain (GLS) (-11.14 ± 0.5 VS -16.78 ± 0.4, p�?0.0001), longitudinal strain rate (-1.01 ± 0.05 VS -1.07 ± 0.04, p�?0.0001), Culprit Longitudinal Strain (CulLS) (-9.74 ± 0.59 VS -15.68 ± 0.49, P�?0.0001), and culprit longitudinal strain rate (-0.95 ± 0.05 VS -1.02 ± 0.04, P�?0.0001). In the follow up study, all of the strain parameters studied were again significantly lower in the R+ than the R- group. The most sensitive and specific parameters were the GLS and CulLS (sensitivities of 91.7% and 95.8% respectively and specificities of 95% and 96.7% respectively). Conclusion: Our findings show that impaired indices of LV deformation detected two days after successful PCI for AMI may provide a predictive value in early detection of LV remodelling.
Keywords: Left ventricular remodeling; Acute myocardial infarction; Speckle tracking echocardiography.
Introduction
Improvement in the early diagnosis, invasive and medical treatment of AMI lead to a reduction in the mortality rates associated with early and late complications of AMI. However, even complete revascularization does not exclude the risk of adverse LVR [1].
LVR is characterized by progressive enlargement and change in the shape of the LV cavity leading to systolic dysfunction. It occurs, as an adaptation to the tissue infarction, as a result of macro and microscopic changes at the cardiomyocyte, leading to structural and functional changes. LVR is associated with worse outcomes and predisposes to heart failure [2].
Although various studies evaluated multiple clinical factors and routine echocardiographic parameters to try to detect LVR as a consequence of myocardial infarction, there are still gaps in our data, and some of the clinical factors or diagnostic parameters failed to identify patients prone to LVR [3].
STE is an echocardiographic method for evaluating and measuring global and regional strain (longitudinal, circumferential, radial and transverse), the precise indices of ventricular function. The main advantages of STE over strain assessment based on Doppler tissue imaging are that measurements are angle independent, and that it can distinguish active from passive movement of wall segments. Strain-based parameters have been validated in experimental and human studies as sensitive indicators of regional and global cardiac function [4].
Our aim was thus to evaluate the value of STE in the prediction of LVR in AMI patients after primary PCI.
Methods
This study was a prospective cohort study conducted in Fayoum University Hospital, including patients from the emergency department and the in-patient cardiology department, after approval of the research and ethical committee.
Eighty-four patients diagnosed with AMI were included. Inclusion criteria included typical chest pain, elevated Cardiac Biomarkers (troponin and CK-MB) and ST segment elevation on the Electrocardiogram (ECG). All patients underwent PCI with stent implantation according to the ACC/AHA guidelines for STEMI. Prediction factors included number of diseased vessels and time to reperfusion. All patients then had a complete echocardiographic study (including 2D echo, a conventional Doppler study, Tissue Doppler imaging (TDi), and STE), performed two days after PCI. The following parameters were measured: End-Diastolic Volume (EDV), End-Systolic Volume (ESV), Ejection Fraction (EF) and Wall Motion Score Index (WMSI) (by conventional 2D echo); E & A waves, E;A ratio & Deceleration Time (DT) (by Doppler); s’, e’ & a’ waves (by TDI); GLS, Longitudinal Strain Rate (LSr), Global Circumferential Strain (GCS), Circumferential Strain Rate (CSr), CulLS and Culprit Longitudinal Strain Rate (CulLSr) (by STE). The patients were then followed up after two months, where a new echocardiographic study was performed and all the above parameters were re measured. The occurrence of LVR was looked for specifically. LVR was defined as ≥ 20% increase in the end diastolic or end systolic volumes of the LV on follow up echocardiography in comparison to the baseline echocardiography. The patients were then divided into two groups according to the occurrence of remodeling; Remodeling (R+) group and Non-remodeling (R-) group.
Exclusion criteria included history of prior myocardial infarction, heart muscle disease (cardiomyopathy) with regional or global hypokinesia, valvular heart disease, significant arrhythmias (including atrial fibrillation), previous pacemaker or cardioverter defibrillator implantation, previous Coronary Artery By-pass Grafting (CABG) or PCI, and very poor image quality [5].
All patients received best guideline directed medical therapy as per the ACC/AHA guidelines for STMEI, including aspirin 75-100 mg once daily, ticagrelor 90 mg bid, a high dose statin, a beta blocker (dosed according to heart rate and BP), and a Renin-Angiotensin- Aldosterone System (RAAS) inhibitor (dosed according to BP).
Data entry and statistical analysis
Data was collected, coded and analyzed using SPSS (Statistical Package for Social sciences) software (Version 25) on Windows 7, and a simple descriptive analysis in the form of percentage distribution, means and S.D. (Standard Deviation) was executed. Categorical data was analyzed by computing percentages, and consequent differences were tested statistically by applying Chi square tests for comparisons between groups; students’ T-test to compare between two groups, a p-value of<0.05 was considered statistically significant.
Results
This study was conducted on eighty-four patients from the emergency and in-patient departments of Fayoum University Hospital in the duration from May 2017 till September 2018.
Basic characteristics in both groups (R+, R-), were as follows: the mean age of R+ group was 58.9 ± 9.3 and that of the R- group was 58.3 ± 6.9. In the R+ group 70.8% were males and 29.2% were females, while in the R- group 68.3% were males and 31.7% were females. Regarding different risk factors, in the R+ group, 62% were smokers, 54% were diabetic and 58% were hypertensive, while in the R- group, 56% were smokers, 48% were diabetic and 56% were hypertensive [Table 1].
| Variables | Patients with remodeling (R+) (N=24) | Patients without remodeling (R-) (N=60) | P-value# | ||
|---|---|---|---|---|---|
| Mean | ± SD | Mean | ± SD | ||
| Age | 58.92 | 9.38 | 58.32 | 6.99 | 0.749 |
| Variables | N | % | N | % | P-value## |
| Sex | |||||
| Male | 17 | 70.8 | 41 | 68.3 | 0.823 |
| Female | 7 | 29.2 | 19 | 31.7 | |
| Smoking | |||||
| Yes | 15 | 62.5 | 34 | 56.7 | 0.624 |
| No | 9 | 37.5 | 26 | 43.3 | |
| Hypertension | |||||
| Yes | 14 | 58.3 | 34 | 56.7 | 0.889 |
| No | 10 | 41.7 | 26 | 43.3 | |
| Diabetes | |||||
| Yes | 13 | 54.2 | 29 | 48.3 | 0.629 |
| No | 11 | 45.8 | 31 | 51.7 | |
Table 1: Basic characteristics and risk factors in both groups.
Regarding the angiographic results in both groups, the only statistically significant difference was in the time to reperfusion which was longer in the R+ than the R- group, with a mean of 18.75 ± 8.8 hours and 5.55 ± 2.45 hours, respectively, and a p value of˂0.0001. On the other hand, there were no statistically significant differences between both groups regarding the number of diseased vessels or the infarct related artery (IRA); in the R+ group 50% had the LAD, 16% had the LCX and 33% had the RCA as the IRA, while in the R- group 48% had the LAD, 21% had the LCX and 30% had the RCA as the IRA [Table 2].
| Variables | Patients with remodeling (R+)(N=24) | Patients without remodeling (R-)(N=60) | P-value# | ||
|---|---|---|---|---|---|
| Mean | ± SD | Mean | ± SD | ||
| Number of diseased vessels | 1.83 | 0.82 | 1.77 | 0.76 | 0.725 |
| Time to reperfusion | 18.75 | 8.89 | 5.55 | 2.45 | <0.0001 |
| Variables | N | % | N | % | P-value## |
| IRA | |||||
| LAD | 12 | 50 | 29 | 48.3 | 0.868 |
| LCX | 4 | 16.7 | 13 | 21.7 | |
| RCA | 8 | 33.3 | 18 | 30 | |
Table 2: Angiographic results in both groups.
The basic echocardiographic results in the baseline echocardiography study showed that only the WMSI was statistically significant, where its value was higher in the R+ than the R- group, with a mean of 1.58 ± 0.08 and 1.23 ± 0.07 respectively, and a p value of˂0.0001. The EF, EDV and ESV were less in the R+ than in the Rgroup, but there was no statistically significant difference [Table 3].
| Variables | Patients with remodeling (R+)(N=24) | Patients without remodeling (R-)(N=60) | P-value# | ||
|---|---|---|---|---|---|
| Mean | ± SD | Mean | ± SD | ||
| Two days after PCI | |||||
| EF | 50.63 | 2.03 | 51.29 | 3.96 | 0.322 |
| EDV | 87.25 | 9.04 | 89.55 | 8.15 | 0.261 |
| ESV | 43.08 | 4.91 | 43.7 | 5.94 | 0.654 |
| WMSI | 1.58 | 0.08 | 1.23 | 0.07 | <0.0001 |
| After 2 months | |||||
| EF | 50.67 | 2.27 | 54.81 | 4.17 | <0.0001 |
| EDV | 106.36 | 11.32 | 87.59 | 8.23 | <0.0001 |
| ESV | 52.46 | 6.08 | 39.69 | 5.98 | <0.0001 |
Table 3: Basic echocardiographic results in both groups.
The follow up echocardiography study showed that there was a statistically significant difference between both groups regarding the EF, EDV and ESV; the EF was less in the R+ than the R- group (mean values of 50.6 ± 2.27 and 54.8 ± 4.1 respectively, with a p value of ˂0.0001), the EDV was higher in the R+ than the R- group (mean values of 106.3 ± 11.3 and 87.5 ± 8.2 respectively, with a p value 0f˂0.0001), and the ESV was higher in the R+ than the R- group (mean values of 52.4 ± 6 and 39.6 ± 5.9 respectively, with a p value of˂0.0001).
The Doppler study done at the baseline echocardiography, showed many statistically significant differences between both groups regarding the A, E/A and DT values, where the A wave was lower in the R+ than the R- group (67.5 ± 2.5 and 74.2 ± 2.5 respectively, with a p value of˂0.0001), the E/A ratio was higher in the R+ than the R- group (1.2 ± 0.03 and 1.08 ± 0.08 respectively, with a p value of˂0.0001), and the DT was less in the R+ than the R- group (151.8 ± 8.8 and 183.1 ± 6.8 respectively, with a p value of˂0.0001). There was no statistically significant difference in the E wave value between both subgroups.
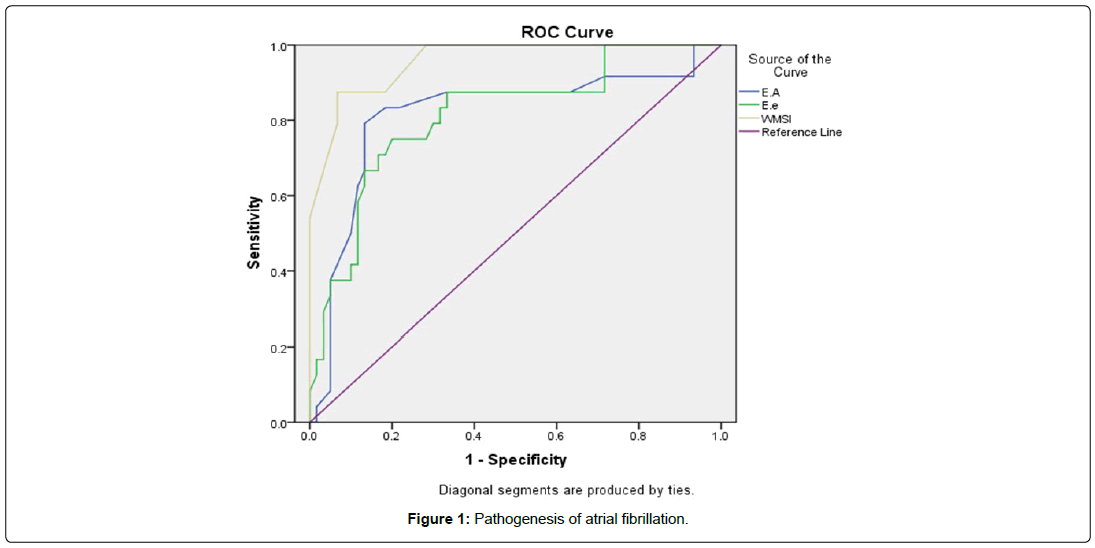
In regards to the TDI study, the e’ was significantly lower in the R+ than the R- group (5.2 ± 0.3 and 6.2 ± 0.6 respectively, with a p value of˂0.0001), and the E/e’ ratio was significantly higher in the R+ than R- group (15.5 ± 1 and 13.02 ± 1.4 respectively, with a p value of˂0.0001). The a’ and s’ values did not show significant differences between both groups [Table 4 and Figure 1].
| Variables | Patients with remodeling (R+)(N=24) | Patients without remodeling (R-)(N=60) | P-value# | ||
|---|---|---|---|---|---|
| Mean | ± SD | Mean | ± SD | ||
| E | 81.04 | 3.06 | 80.18 | 4.94 | 0.431 |
| A | 67.54 | 2.57 | 74.27 | 2.52 | <0.0001 |
| E/A | 1.2 | 0.03 | 1.08 | 0.08 | <0.0001 |
| DT | 151.83 | 8.82 | 183.17 | 6.83 | <0.0001 |
| Tissue Doppler | Mean | ±SD | Mean | ±SD | P-value# |
| e' | 5.24 | 0.33 | 6.22 | 0.64 | <0.0001 |
| E/e' | 15.52 | 1.01 | 13.02 | 1.49 | <0.0001 |
| a' | 8.59 | 0.38 | 8.65 | 0.4 | 0.554 |
| s' | 6.69 | 0.35 | 6.84 | 0.41 | 0.138 |
Table 4: Doppler results two days after PCI in both groups.
The STE data derived from the baseline study, showed statistically significant difference in the following values:
The GLS was lower in the R+ than the R- group (mean values of -11.14 ± 0.59 and -16.78 ± 0.49 respectively, with a p value of˂0.0001).
The LSr was lower in the R+ than the R- group (mean values of -1.01 ± 0.05 and 1.07 ± 0.04 respectively, with a p value of˂0.0001).
The CulLS was lower in the R+ than the R- group (mean values of -9.74 ± 0.59 and -15.68 ± 0.49 respectively, with a p value of˂0.0001).
The CulLSr was lower in the R+ than the R- group (mean values of -0.95 ± 0.05 and -1.02 ± 0.04 respectively, with a p value of˂0.0001).
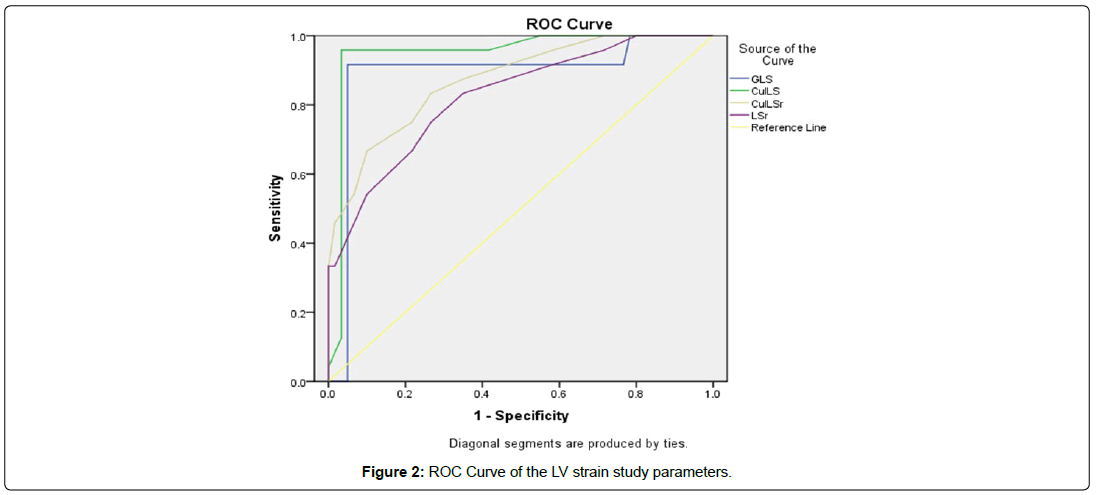
However, the GCS and the CSr did not show a statistically significant difference between both groups [Table 5 and Figure 2].
| Variables | Patients with remodeling(N=24) | Patients without remodeling(N=60) | P-value# | |||
|---|---|---|---|---|---|---|
| Mean | ± SD | Mean | ± SD | |||
| Two days after PCI | ||||||
| GLS | -11.14 | 0.59 | -16.78 | 0.49 | <0.0001 | |
| LSr | -1.01 | 0.05 | -1.07 | 0.04 | <0.0001 | |
| GCS | -16.62 | 0.38 | -16.71 | 0.57 | 0.492 | |
| CSr | -1.23 | 0.05 | -1.24 | 0.06 | 0.06 | |
| CulLS | -9.74 | 0.59 | -15.68 | 0.49 | <0.0001 | |
| CulLSr | -0.95 | 0.05 | -1.02 | 0.04 | <0.0001 | |
| After 2 months | ||||||
| GLS | -11.48 | 0.59 | -17.9 | 0.51 | <0.0001 | |
| LSr | -0.99 | 0.05 | -1.14 | 0.04 | <0.0001 | |
| GCS | -17.03 | 0.39 | -17.32 | 0.57 | 0.023 | |
| CSr | -1.26 | 0.05 | -1.29 | 0.06 | 0.01 | |
| CulLS | -10.14 | 0.59 | -16.63 | 0.49 | <0.0001 | |
| CulLSr | -0.96 | 0.08 | -1.1 | 0.04 | <0.0001 | |
Table 5: Speckle Tracking Echocardiography (STE) results in both groups.
In the follow up LV deformation study done after 2 months, all the parameters showed a statistically significant difference, where:
The GLS was lower in the R+ than the R- group (mean values of -11.48 ± 0.59 and -17.9 ± 0.51 respectively, with a p value of˂0.0001).
The LSr was lower in the R+ than the R- group (mean values of -0.99 ± 0.05 and -1.14 ± 0.04 respectively, with a p value of˂0.0001).
The GCS was lower in the R+ than the R- group (mean values of -17.03 ± 0.39 and -17.32 ± 0.57 respectively, with a p value of˂0.023).
The CSr was lower in the R+ than the R- group (mean values of -1.26 ± 0.05 and -1.29 ± 0.06 respectively, with a p value of˂0.01).
The culprit longitudinal strain (CulLS) was lower in the R+ than the R- group (mean values of -10.14 ± 0.59 and -16.63 ± 0.49 respectively, with a p value of˂0.0001).
The CulLSr was lower in the R+ than the R- group (mean values of -0.96 ± 0.08 and -1.1 ± 0.04 respectively, with a p value of˂0.0001).
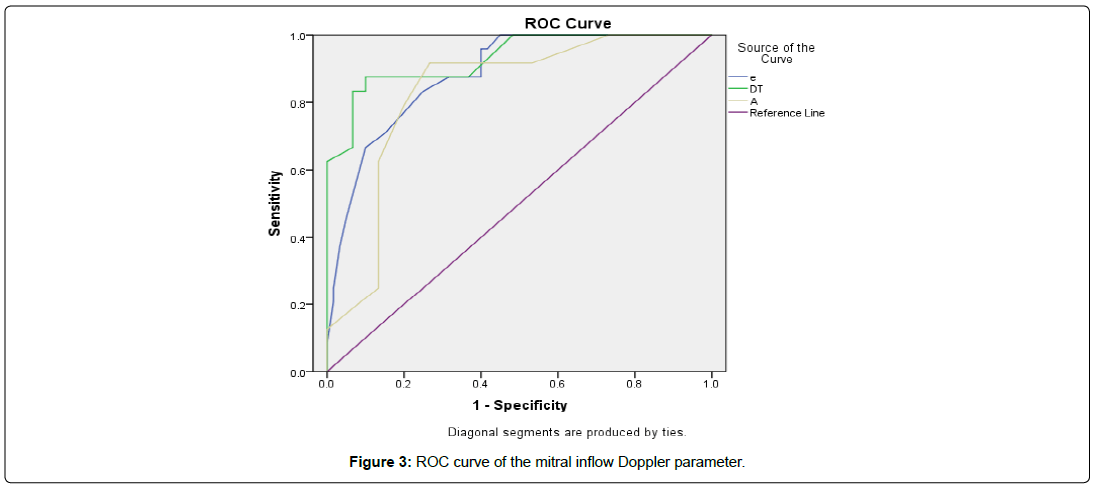
The receiver operating characteristics (ROC) curves of variables, which were significantly different, from the baseline study, showed a significant difference between the R+ and R- groups. The most sensitive and specific parameters were the CulLS and the GLS, where both showed sensitivities of 95.8% and 91.7% respectively, and specificities of 96.7% and 95% respectively. Out of the nonstrain derived parameters, the WMSI and the DT showed the highest specificity, where the specificities were 90% and 93.3% respectively [Table 6 and Figure 3].
Discussion
Prevalence of adverse ventricular remodelling
The goal of this study was to analyse the prevalence, clinical characteristics, and predictors of LVR after AMI in the era of primary PCI and modern medical therapy. Despite aggressive treatment, including reperfusion and anti-remodeling strategies, ventricular enlargement is still common. Our study shows that out of the eightyfour patients with AMI, twenty-four patients (30%) suffered from LVR. In a study done by Liszka et al. [6] adverse LVR was detected in 27% of the AMI population of the study. In a meta-analysis by Huttin et al. [7] including 23 prospective studies, it was found that despite the high success rate of revascularization by PCI, adverse LVR occurred in one third of the patients following AMI (12 to 44%). The variability in the prevalence of remodeling between our study and other studies, although minor, may be due to differences in study populations, and timing of imaging [8].
Therefore, despite modern treatment, our data suggest that LVR remains a frequent event. It is important to consider that adequate reperfusion in patients with AMI salvages myocardium and reduces mortality. However, successful restoration of epicardial coronary patency does not always cause adequate reperfusion at the microvascular level (phenomenon of no-reflow) [9].
Time to reperfusion
Our study shows that there was a significant longer mean time from first symptoms occurrence to reperfusion in the group of AMI patients who suffered from adverse LVR, where the mean duration was 18.75 hours ± 8.89 versus 5.55 hours ± 2.45 in the non-remodeling subgroup, with a p value of˂0.0001. This result is comparable to the results of a study done by Hsiao et al. [10] in which the door to balloon time was longer in the remodeling group. Also this same finding was detected by Liszka et al. [6] but other studies done by Bolognese et al. [11] and cerisano et al. [12] did not detect such a finding.
The first symptoms-reperfusion time consists of three parts: a) time to first medical contact, b) time to medical center and c) door to balloon time. The relatively long overall time to reperfusion found in our study was mainly due to patients’ unnecessary emergency call delay despite clear symptoms or ambiguous and atypical general symptoms, which were not primarily recognized as serious cardiovascular symptoms (e.g. gastrointestinal-like symptoms in inferior wall ischemia). The LVR occurring despite successful reperfusion may be a consequence of a lower number of viable cardiomyocytes in the infarct area at the time of reperfusion, which is not sufficient to prevent adverse remodeling [13,14].
Wall motion score index
Our study shows that there was a significantly higher WMSI value in the remodeling group than in the non-remodelers. This finding is comparable to the results of a study done by Loboz-Grudzien et al. [15] who found that a WMSI value of ≥ 1.5 was predictive of progressive left ventricular dilatation (PLVD) after myocardial infarction.
In a study done by Eek et al. [16] it was found that a WMSI value of more than 1.44 indicated an infarct size of more than 12% of the myocardium (infarct size was calculated by infarct volume as a percentage of total myocardial volume, quantified by MRI). Final infarct size is a strong predictor of mortality and major adverse cardiovascular events. Current reperfusion therapy is effective, resulting in a relative reduction of infarct size achieved, typically 40% by thrombolysis and 60% by primary PCI. The reduced mortality rate observed in the reperfusion era is largely attributable to a reduction of final infarct size. This WMSI value is comparable to the cutoff value in our study which is 1.4, at which both the sensitivity and specificity for the prediction of LV adverse remodeling were 87.5% and 93.3% respectively.
Doppler echocardiography
In the study done by Cerisano et al. [12] it was found that the assessment of LV filling pattern on Doppler echocardiography provides additional and important information in the setting of AMI, allowing identification of patients at high risk for progressive LV dilation after AMI. A restrictive filling pattern, as expressed by a short DT, was the most powerful predictor of LV remodeling, and the degree of LV dilation was related to the severity of impairment of LV filling.
Previous studies have demonstrated that infarct size is one of the major factors that promote LV remodeling [17,18]. On the other hand, the size of the infarct zone has been shown to influence the diastolic filling pattern, with the large infarcts exhibiting a “restrictive” filling pattern. Therefore, a short DT, indicative of a restrictive filling pattern, might simply reflect an increasing infarct size and consequently a higher risk of LV dilation [19,20].
In agreement with the aforementioned observations, our study showed that the R+ group (with remodeling) showed a significantly lower value of the A wave, shorter DT and a higher E/A value. The tissue Doppler also showed a significantly lower e` and a higher E/e` values in the R+ group.
Our results thus also suggest a restrictive filling pattern in the R+ group, with the DT being the most specific Doppler parameter (at a cutoff value of 172.5ms, sensitivity of 87.5% and specificity of 90%) for detection of LVR after 2 months.
Our study thus shows that early noninvasive assessment of trans-mitral flow velocity by Doppler echocardiography allows identification of patients at high risk for progressive LV dilation within 2 months after reperfused AMI. A restrictive filling pattern is a powerful predictor of LV remodeling, with the deceleration time being the most Doppler specific parameter.
Speckle tracking echocardiography derived strain parameters
There have been extensive studies about GLS, GCS and LSr, CSr proposing them as predictors for reworking. However, most of these studies had the limitation of small patient number. Some studies demonstrated that GLS may be a powerful prognosticator for reworking, others claimed GCS to be the best prognosticator, and other studies even claimed that circumferential strain rate was the simplest predictor of transforming.
Our study shows that, out of the various strain parameters measured 2 days after PCI, the GLS, LSr, CulLS and therefore the CulLSr were significantly lower within the subgroup of patients that afterwards suffered from adverse LV remodeling.
It was demonstrated that GLS predicts remodeling, where remodeling was defined as>15% increase in EDV. They targeted only anterior wall infarctions with a patient population of fifty. Lacalzada et al. [21] also illustrated that GLS predicts remodeling in STEMI in a study including ninety-seven low risk patients. Only 20 out of 97 patients developed remodeling in their study. A large study by Joyce et al. [22] reported an association between GLS and adverse LV dilatation after STEMI in 1,041 patients. The population was divided into 2 groups depending on their GLS (above or below -15%). Patients with baseline GLS less than –15.0% exhibited greater LV dilatation at 3- and 6-month follow-ups compared with patients with GLS equal to or above -15.0%. This is almost similar to our study that showed that at a cutoff value of -14%, the sensitivity and specificity of GLS to predict LV remodeling were 91.7% and 95% respectively.
On the opposite hand, Bonios et al. [23] stated that in their research on potential predictors of LV remodeling in patients with acute anterior wall myocardial infarction, apical CS was a stronger predictive marker of LV remodeling as compared to LS. One potential pathophysiological explanation of this finding is that LV CS plays a more pivotal role in maintaining LV structure, hence a worse circumferential CS might contribute to LV remodeling. In support of this hypothesis are the results of the study by Aikawa et al. [24] where, in patients with an anterior infarction, apical regional wall stress was an independent predictor of subsequent LV remodeling after AMI. But it’s worth mentioning that in both of these studies, only patients with anterior myocardial infarction were included.
The VALIANT Echo study, in contrary to our study, demonstrated that circumferential strain rate was predictive of LVR but GLS and LSr were not. That study investigated 603 patients with LV dysfunction or heart failure after myocardial infarction. Only 311 cases had adequate image quality to allow assessment of all longitudinal and circumferential strain and strain rate. The GLS and LSRs were derived only from the mean of apical 4- and 2-chamber views. Probably, the mean value of all complete 12 segments was not representative of worldwide values. It is worth mentioning that those patients were enrolled before the systematic use of primary PCI and other guideline-based anti-remodeling therapies [7].
In our study, we also investigated the CulLS, CulLSr which were defined as the average longitudinal strain and strain rates of the territories of the culprit vessels, and both showed significant difference between the groups of remodelers and non-remodelers (both were significantly lower). These results are in partial concordance with the results of the study by Hsiao et al. [10] which demonstrated that, out of both of these values, only the CulLSr showed a significant difference (was significantly lower within the adverse remodeling group).
What is the best parameter for prediction of adverse LV remodeling? In our study, the CulLS and therefore the GLS (longitudinal strain parameters) were the most sensitive and specific parameters for the prediction of LVR with sensitives of 95.8% and 91.7% respectively and specificities of 96.7% and 95% respectively. Gjesdal et al. [25] discovered that the GLS level identified by 2D STE is closely correlated to myocardial infarct size as determined by contrast-enhanced resonance imaging during chronic ischemic heart condition. A strain value of -15% has 83% sensitivity and 93% specificity at the worldwide level and 76% sensitivity and 95% specificity at the territorial level (territory of the culprit vessel) to spot infarction.
Longitudinal strain is more sensitive to early cardiac attack and circumferential strain may be preserved initially. This is often because subendocardium is more susceptible to ischemia. Because longitudinal fibers are in the subendocardial region and circumferential fibers are within the mid-wall region of the myocardium, thus the longitudinal fibers are more vulnerable to ischemia, resulting in cardiac long-axis systolic dysfunction which is reflected by impaired GLS. Consequently, it is reasonable that GLS is an early marker for cardiac dysfunction and GCS gets impaired in advanced patients with decompensated heart failure, which may explain why GCS was not found to be an early predictor of adverse LVR in our study. This hypothesis should be further verified [26].
Limitations
Our cohort of patients was relatively small, and it was limited to patients with few complications. Patients who required mechanical ventilation were difficult to be included due to poor image quality.
Deformation imaging based on speckle tracking technique relies on above-average image quality for good data extraction, and continuous endocardial border motion would be the major determinant in enrollment.
Conclusion
Adverse LV remodeling occurred in 30% of AMI patients even after PCI. The 2D STE proved to be a promising, feasible, and noninvasive modality to evaluate myocardial deformation in this cohort. In our study, CulLS and GLS were the most sensitive and specific predictors of adverse LV remodeling.
Ethics
This study was reviewed and approved by the Fayoum University- Faculty of Medicine (Research Ethical Committee). The official approval was obtained from the general director of hospital and the manager of the outpatient clinic and the head of the Cardiology department.
Consent to participate
The study was performed after explaining its objectives and confidentiality was expressed to the participants. Written consent was taken from the participants as an agreement to join the study before clinical examination and laboratory investigation. All participants had the right to not participate in the study.
Declaration
The authors declare that this manuscript did not previously publish or considered for publication in any other journal. The authors do not hold any stocks or shares, fees, funding or salary from any organization that may in any way gain or lose financially from the publication of this manuscript, either now or in the future.
Competing Interests
There is no conflict of interest as there are no commercial or financial relationships from any institution or organization that could be construed as a potential conflict and all the expenses are covered by the authors.
References
- Funaro S, Galiuto L, Boccalini F, Cimino S, Canali E et al. (2011) Determinants of microvascular damage recovery after acute myocardial infarction: Results from the Acute Myocardial Infarction Contrast Imaging (AMICI) multi-centre study. Eur J Echocardiogr 12: 306-312.
- Arnold SV, Spertus JA, Masoudi FA, Daugherty SL, Maddox TM et al. (2013) Beyond medication prescription as performance measures: optimal secondary prevention medication dosing after acute myocardial infarction. J Am Coll Cardiol 62: 1791-1801.
- Seropian IM, Sonnino C, Van Tassell BW, Biasucci LM, Abbate A et al. (2015) Inflammatory markers in ST-elevation acute myocardial infarction. Eur Heart J Acute Cardiovasc Care 5: 382-395.
- Marwick TH, Leano RL, Brown J, Sun JP, Hoffmann R et al. (2009) Myocardial strain measurement with 2-dimensional speckle-tracking echocardiography: definition of normal range. JACC Cardiovasc Imaging 2: 80-84.
- Ingul CB, Malm S, Refsdal E, Hegbom K, Amundsen BH et al. (2010) Recovery of function after acute myocardial infarction evaluated by tissue Doppler strain and strain rate. J Am Soc Echocardiogr 23: 432-438.
- Liszka J, Haberka M, Tabor Z, Finik M, Gąsior Z (2013) Two dimensional speckle tracking echocardiography assessment of left ventricular remodeling in patients after myocardial infarction and primary reperfusion. Arch Med Sci 6: 1091-1100.
- Huttin O, Coiro S, Selton-Suty C, Juillière Y, Donal E et al. (2016) Prediction of Left Ventricular Remodeling after a Myocardial Infarction: Role of Myocardial Deformation: A Systematic Review and Meta Analysis. PLoS ONE 11: e0168349.
- Na HM, Cho GY, Lee JM, Cha MJ, Yoon YE et al. (2016) Echocardiographic predictors for left ventricular remodeling after acute ST elevation myocardial infarction with low risk group: speckle tracking analysis. J Cardiovasc Ultrasound 24: 128-134.
- Farah E, Cogni AL, Minicucci MF, Azevedo PS, Okoshi K et al. (2012) Prevalence and predictors of ventricular remodeling after anterior myocardial infarction in the era of modern medical therapy. Med Sci Monit 18: CR276-281.
- Hsiao JF, Chung CM, Chu CM, Lin YS, Pan KL et al. (2016) Two-Dimensional Speckle Tracking Echocardiography Predict Left Ventricular Remodeling after Acute Myocardial Infarction in Patients with Preserved Ejection Fraction. PLoS ONE 11: e0168109.
- Bolognese L, Neskovic A, Parodi G, Cerisano G, Buonamici P et al. (2002) Left ventricular remodeling after primary coronary angioplasty. Circulation 106: 2351-2357.
- Cerisano G, Bolognese L, Carrabba N, Buonamici P, Santoro GM et al. (1999) Doppler-derived mitral deceleration time. An early strong predictor of left ventricular remodeling after reperfused anterior acute myocardial infarction. Circulation 99: 230-236.
- Nicolosi GL, Golcea S, Ceconi C, Parrinello G, Decarli A et al. (2009) Effects of perindopril on cardiac remodeling and prognostic value of pre-discharge quantitative echocardiographic parameters in elderly patients after acute myocardial infarction: the PREAMI echo substudy. Eur Heart J 30: 1656-1665.
- Bertini M, Mollema SA, Delgado V, Antoni ML, Ng AC et al. (2009) Impact of time to reperfusion after acute myocardial infarction on myocardial damage assessed by left ventricular longitudinal strain. Am J Cardiol 104: 480-485.
- Loboz-Grudzien k, Kowalska A, Brzezinska B, Sokalski L, Jaroch J (2007) Early predictors of adverse left ventricular remodelling after myocardial infarction treated by primary angioplasty. Cardiol J 14: 238-245.
- Eek C, Grenne B, Brunvand H, Aakhus S, Endresen K et al. (2010) Strain echocardiography and wall motion score index predicts final infarct size in patients with non-ST-segment-elevation myocardial infarction. Circ Cardiovasc Imaging 3: 187-194.
- Gaudron P, Eilles C, Kugler I, Ertl G (1993) Progressive left ventricular dysfunction and remodeling after myocardial infarction: potential mechanisms and early predictors. Circulation 87: 755-763.
- Pipilis A, Meyer TE, Ormerod O, Flather M, Sleight P (1992) Early and late changes in left ventricular filling after acute myocardial infarction and the effect of infarct size. Am J Cardiol 70: 1397-1401.
- Grabka M, Wita K, Tabor Z, Paraniak-Gieszczyk B, Chmurawa J et al. (2013) Prediction of infarct size by speckle tracking echocardiography in patients with anterior myocardial infarction. Coron Artery Dis 24: 127-134.
- Popovic AD, Neskovic AN, Marinkovic J, Lee JC, Tan M et al (1996) Serial assessment of left ventricular chamber stiffness after acute myocardial infarction. Am J Cardiol 77: 361-364.
- Lacalzada J, de la Rosa A, Izquierdo MM, Jiménez JJ, Iribarren JL et al. (2015) Left ventricular global longitudinal systolic strain predicts adverse remodeling and subsequent cardiac events in patients with acute myocardial infarction treated with primary percutaneous coronary intervention. Int J Cardiovasc Imaging 31: 575-584.
- Joyce E, Hoogslag GE, Leong DP, Debonnaire P, Katsanos S et al. (2014) Association between left ventricular global longitudinal strain and adverse left ventricular dilatation after ST-segment-elevation myocardial infarction. Circ Cardiovasc Imaging 7: 74-81.
- Bonios MJ, Kaladaridou A, Tasoulis A, Papadopoulou E, Pamboukas C et al. (2014) Value of apical circumferential strain in the early post-myocardial infarction period for prediction of left ventricular remodeling. Hellenic J Cardiol 55: 305-312.
- Aikawa Y, Rohde L, Plehn J, Greaves SC, Menapace F et al. (2001) Regional wall stress predicts ventricular remodeling after anteroseptal myocardial infarction in the Healing and Early Afterload Reducing Trial (HEART): an echocardiography-based structural analysis. Am Heart J 41: 234-242.
- Gjesdal O, Helle-Valle T, Hopp E, Lunde K, Vartdal T et al. (2008) Noninvasive separation of large, medium, and small myocardial infarcts in survivors of reperfused ST-elevation myocardial infarction: a comprehensive tissue Doppler and speckle-tracking echocardiography study. Circ Cardiovasc Imaging 1: 189–196.
- Abate E, Hoogslag GE, Leong DP, Bertini M, Antoni ML et al. (2014) Association between multilayer left ventricular rotational mechanics and the development of left ventricular remodeling after acute myocardial infarction. J Am Soc Echocardiogr 27: 239-248.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi