Research Article, J Aging Geriatr Med Vol: 1 Issue: 3
Underuse of Implantable Loop Recorders in Elderly Patients with Syncope and Unexplained Falls
Susanne C. de Ruiter1, Jeske J. Walgers1, Els Doejaaren1, Tjeerd Germans2, Jaap H. Ruiter2 and René W.M.M. Jansen1*
1Department of Geriatric Medicine, Northwest Clinics, Alkmaar, the Netherlands
2Department of Cardiology, Northwest Clinics, Alkmaar, the Netherlands
*Corresponding Author : René Jansen, MD, PhD
Department of Geriatric Medicine, Northwest Clinics Alkmaar, Wilhelminalaan 12, 1815 JD Alkmaar, The Netherlands
Tel: +31-72-5482380
Fax: +31725482197
E-mail: r.w.m.m.jansen@nwz.nl
Received: April 28, 2017 Accepted: June 12, 2017 Published: June 19, 2017
Citation: de Ruiter SC, Walgers JJ, Doejaaren E, Germans T, Ruiter JH, et al. (2017) Underuse of Implantable Loop Recorders in Elderly Patients with Syncope and Unexplained Falls. J Aging Geriatr Med 1:3.
Abstract
Background: Implantable loop recorders (ILRs) may improve detection of cardiac causes of syncope. Their use in elderly patients is not clear.
Methods: Observational study including patients ≥65 years with unexplained syncope and/or falls undergoing cardiac evaluation, comparing patients with and without cardiac causes on baseline characteristics, indications for pacemaker/ILR, and mortality (mean follow-up ≥1 year). All electrocardiograms (ECGS) were retrospectively re-evaluated.
Results: 374 of a total of 419 patients (mean age 80, SD 6 years) underwent cardiac evaluation. 121 patients had a proven/suspected cardiac cause for the syncope/fall. Ten patients underwent pacemaker/ICD and twelve patients ILR implantation, leading to a diagnosis in five. Sixty patients were advised to undergo ILR implantation after a next event; only three received an ILR during follow-up, although eleven experienced symptoms. Within the group of patients that underwent a cardiac evaluation, there was a higher mortality rate in the cardiac group versus the other causes group (p=0.03). The cardiac group had significantly more ECG abnormalities. Also patients with a cardiac evaluation had more ECG abnormalities (p=0.02). Based on the initial ECG, respectively 9 and 72 patients with a cardiac evaluation had an indication for pacemaker and ILR, but only five patients received a pacemaker and five patients received an ILR. Nine patients without cardiac evaluation (20%) had an indication for ILR based on their ECG.
Conclusions: A substantial number of elderly syncope and fall patients had ECG abnormalities suggestive of a cardiac cause, with an indication for ILR/pacemaker implantation, but only a small number received a device. A cardiac evaluation and early ILR implantation should be considered more often in the diagnostic work-up of unexplained syncope and falls in the elderly.
Keywords: Syncope; Falls; Very elderly; Implantable loop recorders
Introduction
Syncope is a common problem in the elderly. Its incidence increases rapidly ≥70 years of age, up to 81.2 per 1000 patient years above the age of 80 years [1]. Due to transient loss of consciousness following rapid global cerebral hypo perfusion, syncope results in a loss of muscle tone. Per definition, this is of short duration with spontaneous complete recovery [2]. Since 30-50% of patients have retrograde amnesia, and less than 50% of syncopal events are witnessed, many patients will present with a fall rather than loss of consciousness, however [3-5]. In the evaluation of falls in the elderly, syncope should therefore always be considered as a possible cause for the fall [6].
The consequences of falls and syncope range from loss of confidence, fear of falling, and depressive illness, to fractures and subsequent institutionalization [7,8]. Costs of falling increase with advancing age to almost 15.000 euros in patients ≥85 years [9]. Therefore, a rapid diagnosis and successful intervention are very important to prevent recurrence. However, even if state-of-the-art diagnostic procedures are followed in specialized clinics, about 35% of all syncope patients are left without a good explanation for their syncope [10].
Cardiovascular disorders are an important risk factor for syncope and falls, particularly in the elderly. Rhythm and/or conduction disorders (RCDs) may easily be missed in the initial evaluation [11]. Implantable loop recorders (ILRs) substantially increase the diagnostic yield compared with a conventional work-up for syncope [12,13]. The updated ESC guidelines for syncope therefore recommend early use of ILRs [1]. To date, little is known about the use of ILRs in the evaluation of unexplained syncope and falls in geriatric patients [13-15].
The main objective of this study was to determine the diagnostic yield of the cardiac evaluation of elderly patients with unexplained syncope and falls, and to evaluate the use and diagnostic yield of ILRs in these patients. We expected that all patients with an indication for an ILR would be detected, and that all suitable patients would subsequently receive an ILR.
Methods
We performed an observational study at the Fall and Syncope day Clinic (FSC) of the Northwest Clinics, Alkmaar, The Netherlands. This is a multidisciplinary diagnostic pathway for elderly patients with unexplained falls and/or syncope, involving geriatricians, cardiologists and neurologists, based on the current ESC guidelines on syncope and (inter)national guidelines on the evaluation of falls [1,16,17]. Details of this two-day program have been described elsewhere [6]. In the current study, we included patients aged ≥65 years from November 2011 until May 2016. Because of the large overlap between syncope and falls in elderly subjects, and the fact that these events are often indistinguishable, both patients presenting with syncope and unexplained falls were included.
Specific patient consent and ethical board approval were not requested, since this study used archival data of standard geriatric evaluations and had no implications on therapeutic decisions. No sensitive patient data were used.
If patients were suspected of a life-threatening condition, they would be referred to the cardiac emergency department; otherwise they were evaluated at the FSC. All FSC patients underwent a comprehensive geriatric assessment, including medical history, eyewitness account if available, medication review, and physical examination. A nurse practitioner and physiotherapist investigated mental, nutritional, and functional state. Additionally, laboratory tests, orthostatic and postprandial blood pressure measurements, and a 12-lead electrocardiogram (ECG) were taken. In case the geriatrician suspected a cardiac cause for syncope or falls, patients underwent an additional evaluation by the cardiologist, including 24-hour Holter ECG recordings, echocardiogram, and if indicated tilt testing with carotid sinus massage. A final diagnosis and advice for treatment were devised after reaching consensus in the multidisciplinary team, based on all available information.
The cardiologist determined whether patients were a candidate for ILR or pacemaker implantation. All patients who received a pacemaker or ILR, or who were a candidate for ILR implantation in case of recurrent syncope, were followed by the cardiologist for a period of at least one year. At follow-up visits, clinical characteristics of syncopal events, falls, and treatment changes administered for syncope, were collected.
We also reviewed the hospital records of all included patients on August 24th 2016, to determine mortality. Although we had no access to the national death registration (CBS, Heerlen, the Netherlands), in general nearly all deaths are recorded in the hospital records.
In the current study, we compared baseline characteristics of patients in whom the cardiologist concluded that a cardiac cause was proven or suspected as the cause for the syncope or fall (the cardiac group), with those of patients in whom the cardiologist had ruled out a cardiac cause for the syncope or fall (the other causes group). Patients who did not undergo a full cardiac evaluation were excluded from the analysis. Diagnoses and advice for treatment and/or follow-up in the cardiac group were evaluated. For patients with an indication for pacemaker or ILR, we also evaluated the outcome of follow-up visits. Mortality was evaluated for different subgroups.
In addition, a cardiologist specialized in RCDs, retrospectively re-evaluated baseline ECGs of all patients (including those who did not undergo a full cardiac evaluation) according to the current recommendations for ILR implantation, to see if any patients with an indication for ILR were missed in the initial FSC evaluation [1,12].
Statistical analysis
Statistical analyses were performed using SPSS for Windows, version 20 (SPSS, Inc., Chicago, IL, USA). We used Student’s t-Test, Mann-Whitney U-Test, and Pearson’s Chi-Square Test or Fisher’s Exact Test when indicated to compare subjects’ characteristics. Twotailed p-values <0.05 were considered statistically significant.
Results
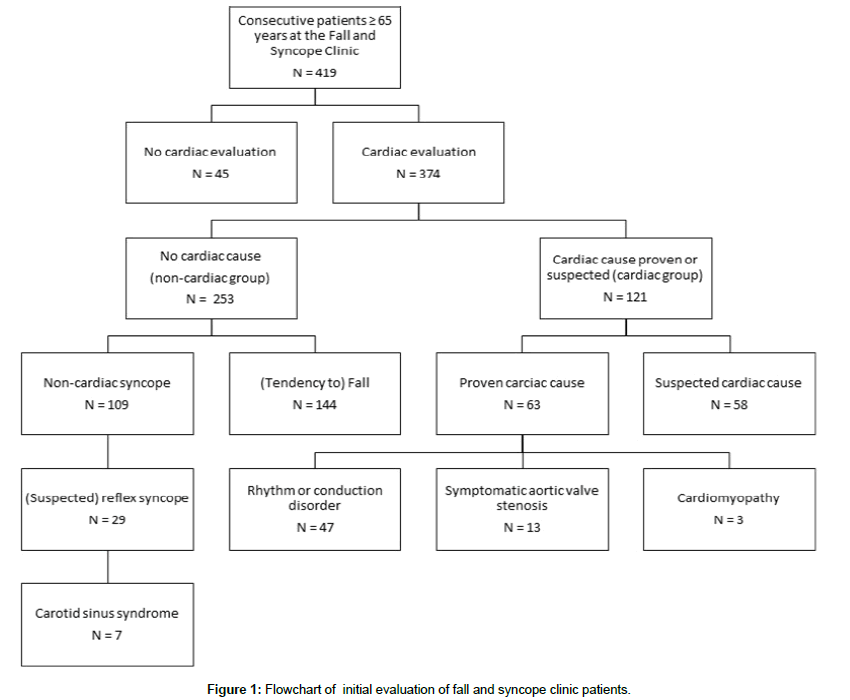
We included 419 patients for evaluation of unexplained syncope and/or falls. Figure 1 shows the initial evaluation, Figure 2 shows the advice given and Figure 3 shows the follow-up in these patients.
Based on the initial work-up, the geriatrician concluded that a cardiac cause was unlikely in 45 patients, and these were not referred for further cardiac evaluation. This included only three syncope patients. One was diagnosed with severe orthostatic hypotension in end-stage Parkinson’s disease. The other one was recently evaluated by the cardiologist, who did not find any explanations for the syncope. Thirty-three patients were diagnosed with falling due to several noncardiac conditions, and the remaining patients with dizziness or a tendency to fall. One additional syncope patient did not undergo cardiac evaluation due to miscommunication; no explanation for the syncope was found in this patient. Baseline characteristics and the results of the retrospective ECG analysis of these 45 patients are included in the Supplemental Appendix.
A full cardiac evaluation was performed in 374 patients. A cardiac cause for the syncope or fall was ruled out by the cardiologist in 253 patients (68%, the other causes group). This group included 109 patients with a non-cardiac syncope; 29 of these patients were diagnosed with (suspected) reflex syncope, including 7 patients with carotid sinus syndrome. The remaining 144 patients presented with a (tendency to) fall.
In 121 patients (32%) the cardiologist concluded that a cardiac cause for the syncope or fall was proven or suspected (the cardiac group). Of this group, 83 patients had a proven syncope. The remaining patients presented with near-syncope or a fall where syncope was suspected (but could not be proven) as the cause of the fall. In the cardiac group, RCDs were diagnosed in 47 patients; these included sinus bradycardia, sinus pause, sick sinus syndrome, atrial fibrillation with pauses, non-sustained ventricle tachycardia, third degree AV-block, and trifascicular block. Symptomatic aortic valve stenosis was found in 13 patients. Three patients were diagnosed with a cardiomyopathy. In the remaining 58 patients of the cardiac group a cardiac cause was strongly suspected, but not proven.
Baseline characteristics and medication of the patients that underwent a full cardiac evaluation are shown in Table 1 and Table 2. We included very elderly patients, mainly females, with a mean age of almost 80 years, and multiple comorbidities. Patients in the cardiac group were significantly older than patients in the other causes group (81 versus 79 years, p=0.05). As expected, the cardiac group had a higher prevalence of structural heart diseases and congestive heart failure (p=0.009).
| CG (N=121) | OCG (N=253) | p-value | |
|---|---|---|---|
| Mean age (SD) in years | 80.6 (6.2) | 79.2 (6.6) | 0.05 |
| Female gender | 82 (67.8%) | 168 (66.4%) | 0.79 |
| Mean no. of comorbidities (SD) | 10.8 (5.8) | 11.5 (5.6) | 0.19 |
| History of hypertension | 80 (66.1%) | 117 (67.6%) | 0.78 |
| History of hypercholesterolemia | 21 (17.4%) | 65 (25.7%) | 0.07 |
| History of type 2 Diabetes Mellitus | 22 (18.2%) | 54 (21.3%) | 0.48 |
| History of cerebrovascular accident | 33 (27.3%) | 55 (21.7%) | 0.24 |
| History of ischemic heart disease | 33 (27.3%) | 63 (24.9%) | 0.62 |
| History of rhythm or conduction disorder | 36 (29.8%) | 65 (25.7%) | 0.41 |
| History of atrial fibrillation | 31 (25.6%) | 55 (21.7%) | 0.4 |
| Pacemaker / ICD before evaluation FSD | 3 (2.5%) | 13 (5.1%) | 0.24 |
| History of congestive heart failure | 18 (15.0%) | 20 (7.9%) | 0.03 |
| History of structural heart disease | 30 (24.8%) | 35 (13.8%) | 0.009 |
| History of peripheral vascular disease | 14 (11.6%) | 28 (11.1%) | 0.85 |
| History of chronic respiratory disease | 19 (15.7%) | 50 (19.8%) | 0.34 |
| History of chronic kidney disease | 8 (6.6%) | 26 (10.3%) | 0.25 |
| History of Parkinson(ism) | 2 (1.7%) | 12 (4.7%) | 0.14 |
| History of epilepsy | 3 (2.5%) | 6 (2.4%) | 0.95 |
| History of fractures | 55 (45.5%) | 101 (39.9%) | 0.31 |
| Known cognitive impairment or dementia | 19 (15.7%) | 25 (9.9%) | 0.1 |
| History of psychiatric disorders | 24 (19.8%) | 56 (22.1%) | 0.61 |
| Institutionalized | 11 (9.1%) | 16 (6.3%) | 0.33 |
| Dependent on others for activities of daily living | 28 (23.1%) | 56 (22.9%) | 0.96 |
| Dependent on others for instrumental ADL | 56 (46.3%) | 97 (38.3%) | 0.14 |
| Use of walking device | 70 (57.9%) | 126 (49.8%) | 0.15 |
Table 1: Patient characteristics of the cardiac group (CG) and other causes group (OCG)
| CG (N=121) | OCG (N=253) | p-value | |
|---|---|---|---|
| Mean no. of medications (SD) | 6.6 (3.6) | 7.1 (3.7) | 0.24 |
| Antihypertensive agents | 90 (73.2%) | 165 (65.2%) | 0.08 |
| - Diuretics - ACE inhibitors / ARBs - Beta blockers - Calcium channel blockers |
47 (38.8%) | 84 (33.2%) | 0.29 |
| 59 (48.8%) | 111 (43.9%) | 0.38 | |
| 38 (31.4%) | 81 (32.0%) | 0.91 | |
| 35 (28.9%) | 34 (13.4%) | 0 | |
| Antiarrhythmic drugs | 25 (20.7%) | 39 (15.4%) | 0.21 |
| Oral anticoagulants / heparins | 69 (57.0%) | 145 (57.3%) | 0.96 |
| Lipid lowering drugs | 50 (41.3%) | 126 (49.8%) | 0.12 |
| Anti-diabetic drugs | 19 (15.7%) | 46 (18.2%) | 0.55 |
| Alpha adrenergic antagonists | 7 (5.8%) | 20 (7.9%) | 0.46 |
| Benzodiazepines | 23 (19.0%) | 53 (20.9%) | 0.66 |
| Antipsychotics | 1 (0.8%) | 7 (2.8%) | 0.45 |
| Antidepressants | 16 (13.2%) | 40 (15.8%) | 0.51 |
Table 2: Medication use in the cardiac group (CG) and other causes group (OCG).
There was a trend towards a higher use of antihypertensive drugs in the cardiac group compared with the other causes group, however this was not significant (73% versus 65%, p=0.08). This was explained by a difference in the use of calcium channel blockers (29% versus 13%, p=0.000). Of note is the fact that the use of lipid lowering drugs was lower in the cardiac group, though not significantly (41% versus 50%, p=0.12).
Cardiac devices and follow-up
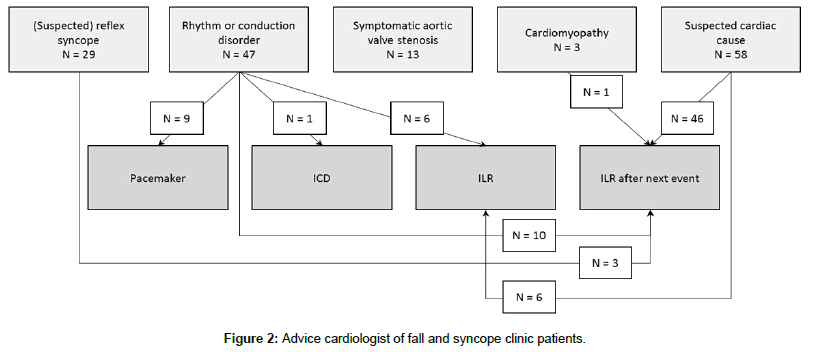
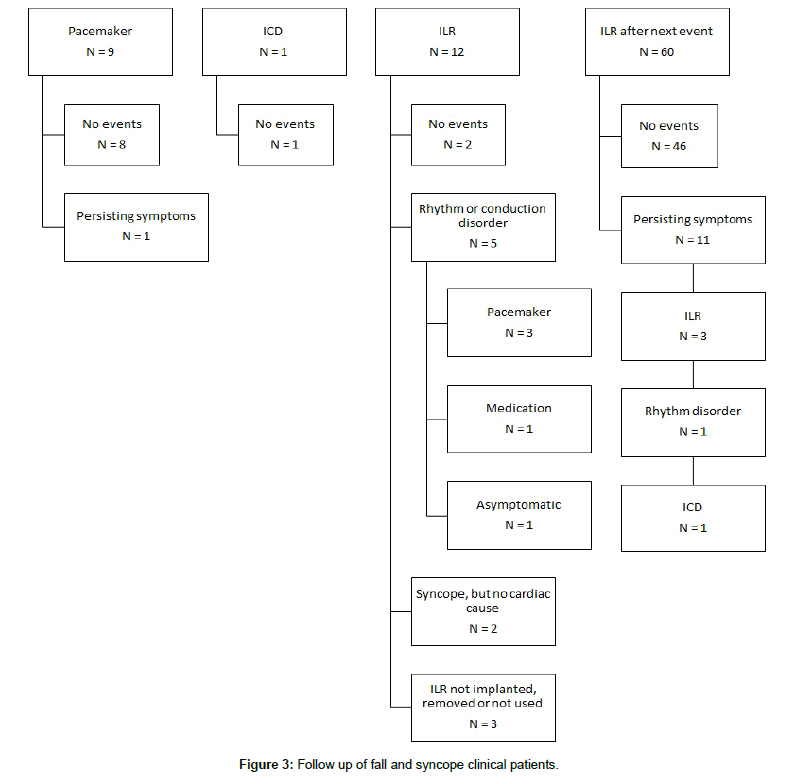
Figure 2 shows the advice given by the cardiologist regarding the implantation of cardiac devices, and Figure 3 shows the follow-up in patients receiving a device. After the FSC evaluation, nine patients with an RCD received a pacemaker and one patient with an RCD received an implantable cardioverter defibrillator (ICD). During ≥1 year follow-up, only one patient had persisting symptoms of syncope and falls.
A total of twelve patients received an ILR after the FSC evaluation; six patients with an RCD and six with a suspected cardiac cause for the syncope. During ≥1 year follow-up, ILR registration led to a (definite or further) diagnosis in five patients (Figure 3). Three patients received a pacemaker for symptomatic pauses. One patient received medication for atrial fibrillation. The other had asymptomatic pauses, without recurrence of syncopal events. Out of the remaining seven patients who received an ILR, two patients suffered through several syncopal events without registration of an RCD, one patient forgot to use the ILR when having complaints, two patients had no recurrence of syncope during 30 months of follow-up. The ILR was removed in one patient shortly after implantation, because the ILR caused too much irritation. The last patient did not appear for the implantation of the ILR.
Implantation of an ILR was advised only after recurrence of syncope in 57 patients of the cardiac group: ten patients with an RCD, one patient with a cardiomyopathy, and 46 patients with a suspected cardiac cause (Figure 2). Three additional patients from the other causes group (all with suspected reflex syncope) received the same advice. Therefore, in total 60 patients were advised to receive an ILR after recurrence of a syncopal event. A waiting policy was often advised because of a low number of syncopal events, or because of patients’ preferences. In nine patients the effect of lowering the dose of cardiovascular medication was awaited before deciding to implant an ILR. During a mean of one year follow-up, 46 patients did not mention any complaints (Figure 3). Eleven patients did suffer from new events. However, only three patients received an ILR, which led to a diagnosis of ventricle tachycardia in one of these patients, who received an ICD six months after the initial FSC evaluation.
Mortality
Overall, 51 out of 419 patients died in the period between their initial evaluation and August 24th 2016. There was no significant difference in mortality between the group that underwent a full cardiac evaluation and the group that did not (42 patients (11%) versus 9 patients (20%), p=0.10). Within the group of patients that underwent a cardiac evaluation, there was a higher mortality rate in the cardiac group versus the other causes group (20 patients (17%) versus 22 patients (9%), p=0.03).
There were two deaths in the group that received a pacemaker, ICD, or ILR immediately after the initial evaluation. Eight out of sixty patients who received the advice to wait for implantation of an ILR after a next event, died (13%), but this did not significantly differ from mortality rates among the other patients with a cardiac cause (p=0.24), patients who underwent cardiac evaluation (p=0.57), or the total group of patients (p=0.80).
ECG evaluation
Table 3 lists the results of the retrospective evaluation of baseline ECGs in all patients undergoing a full cardiac work-up. As would be expected, (relevant) ECG abnormalities, especially multiple disorders at the same time, were significantly more often present in the cardiac group (p=0.000). Rhythm disorders (p=0.000) and ventricular hypertrophy (p=0.04) were also more frequent in the cardiac group.
| CG (N=121) | OCG (N=253) | p-value | |
|---|---|---|---|
| ECG abnormalities | 107 (88.4%) | 179 (70.8%) | 0 |
| Relevant abnormalities | 84 (69.4%) | 125 (50.6%) | 0 |
| Multiple abnormalities | 69 (57.5%) | 94 (37.3%) | 0 |
| Rhythm disorder | 65 (54.6%) | 84 (33.3%) | 0 |
| Conduction disorder | 54 (45.4%) | 105 (41.7%) | 0.5 |
| Left or right ventricular hypertrophy | 33 (28.7%) | 47 (19.0%) | 0.04 |
| Ischemic disorder | 7 (6.0%) | 17 (7.0%) | 0.74 |
| Repolarization disorder | 52 (43.7%) | 93 (37.1%) | 0.22 |
| Miscellaneous | 2 (1.7%) | 4 (1.6%) | 1 |
| Suggestive of syncope | 37 (30.8%) | 28 (11.1%) | 0 |
| Indication for Pacemaker | 8 (6.7%) | 1 (0.4%) | 0.001 |
| Indication for ILR | 33 (27.5%) | 39 (15.4%) | 0.006 |
Table 3: ECG review of the cardiac group (CG) and other causes group (OCG).
ECG abnormalities suggestive of a cardiac cause for the fall or syncope were found in 37 patients (31%) of the cardiac group versus 28 patients (11%) of the other causes group (p=0.000). Based on the initial ECG, 8 patients (7%) of the cardiac group and 1 patient (0.4%) of the other causes group would have had an indication for pacemaker (p=0.001), but only 5 patients (56%) did receive one. An indication for ILR implantation, based on the initial ECG, was present in 33 patients (28%) of the cardiac group and 39 patients (15%) of the other causes group (p=0.006). Three of these patients (4%) received a pacemaker instead, five patients (7%) received an ILR, and 17 patients (24%) were advised to wait for recurrence of syncope before implantation. The other 47 patients (65%) did not receive a cardiac device.
There were more ECG abnormalities in the group that underwent cardiac evaluation compared with the 45 patients who were not referred to a cardiologist, (77% versus 60%, p=0.02). The prevalence of relevant abnormalities was not at all different between patients with and those without cardiac evaluation (56% versus 51%, p=0.54). It is noteworthy that ten patients (22%) who did not undergo further cardiac evaluation, had ECG abnormalities suggestive of a cardiac cause for their fall or syncope. Nine of these patients would have had an indication for ILR implantation based on their initial ECG.
Discussion
Cardiovascular disorders are an important risk factor for syncope and falls in the elderly. ILRs may play an important role in the diagnostic work-up of these patients, when a cardiac cause is suspected or when the cause of a syncope or fall remains unexplained [1,12]. In our study, a multidisciplinary evaluation, including a full cardiac work-up, revealed a (suspected) cardiac cause in about one third of very elderly patients presenting with unexplained falls and syncope. However, only a small number of these patients received a device following the initial evaluation (8% pacemaker/ICD, 10% ILR). Although sixty patients were advised to receive an ILR after a next event, only three patients did eventually receive an ILR. This number is much lower than we expected, especially considering the fact that 18% of these patients still suffered from symptoms. In addition, in retrospection, 72 patients who underwent cardiac evaluation had an indication for an ILR according to current guidelines, based on their initial ECG, but only 12 of these 72 patients (17%) received an ILR.
In our study, the overlap between syncope and falls was significantly larger in the group with cardiac causes. Importantly, about half of these patients had a history of fractures. Implantation of an ILR was considered only at the end of a series of investigations, including echocardiography, external loop recorder monitoring, tilt testing, and carotid sinus massage. If an ILR is implanted early in the diagnostic work-up, a reduced number of tests might be needed to reach a diagnosis, and complications and costs from recurrent falls and/or syncope might be avoided, because a diagnosis is reached earlier [18]. In this study, ILR implantation led to a diagnosis in 6 out of 15 patients. Symptomatic treatment for cardiac causes (with pacemakers or adjustment of medication) may then be feasible, even in elderly patients [19]. These discrepancies between clinical practice and standardized indications for an ILR have been described before in patients with unexplained syncope in a study of syncope units [20]. In this study, the estimated indications were four times higher than the actually implanted ILRs.
The geriatricians refrained from further cardiac evaluation in 45 patients in our study, because a non-cardiac explanation for the syncope or fall was found. These patients did not significantly differ from patients who were referred to the cardiologist in baseline characteristics, cognitive function, or dependency in (instrumental) activities of daily living (see Supplemental Appendix), so these characteristics are unlikely to have played a part in the decision to refrain from performing a full cardiac evaluation. However, our data show that caution is needed when a likely non-cardiac cause is found. One would expect few ECG abnormalities in this group, but the prevalence of relevant ECG abnormalities did not differ from the group that did undergo cardiac evaluation. An abnormality of the baseline ECG has been shown to be an independent predictor of cardiac syncope, and is associated with increased mortality [12]. In retrospection, almost one quarter of patients not referred to the cardiologist showed signs of a cardiac cause for the syncope or fall on their initial ECG.
Mortality was significantly higher in patients with a cardiac cause for their syncope or fall. There was a significant difference in age between the cardiac group and the group with other causes, however, which might explain the difference in mortality. Furthermore, although almost all deaths are recorded in the hospital records, it may be that if a patient was under care of their general practitioner, we were not informed that the patient had died. Therefore, no clear conclusions can be drawn on this point.
Another limitation of this study is the heterogeneity of its population, due to a significant number of comorbidities, and the fact that patients were seen by a large number of different physicians involved in our clinical pathway. The initial intention of our multidisciplinary day clinic was to refer all patients back to their general practitioner following evaluation, but it turned out that patients with (suspected) cardiac causes, especially when there is an indication for ILR, have to be followed by a geriatrician, cardiologist, or dedicated nurse practitioner. This resulted in different follow-up methods across our population, according to the diagnosis reached at the end of the initial evaluation.
Conclusions
A (suspected) cardiac cause was found in about one third of very elderly patients in this study. Although a substantial higher number of patients presented with ECG abnormalities suggestive of a cardiac cause, only few received an ILR. If an ILR was implanted, a diagnosis was reached in the majority of patients. While awaiting the results of prospective studies on this subject, we conclude that a cardiac evaluation and early ILR implantation should be considered more often in the diagnostic work-up of unexplained falls and syncope in the elderly.
Acknowledgement
The authors thank G.J.M. Tahapary, MD, PhD cardiologist, for his advice in this study, and T. van der Ploeg, statistician, for advice and assistance with the statistical analysis.
References
- Ruwald MH, Hansen ML, Lamberts M, Hansen CM, Højgaard MV, et al. (2012) The relation between age, sex, comorbidity, and pharmacotherapy and the risk of syncope: a Danish nationwide study. Europace 14: 1506-1514.
- Guidelines for the diagnosis and management of syncope (2009) The task force for the diagnosis and management of syncope of the European Society of Cardiology. Eur Heart J 30: 2631–2671.
- Shaw FE, Kenny RA (1997) The overlap between syncope and falls in the elderly. Postgrad Med J 73: 635-639.
- Ungar A, Mussi C, Del Rosso A, Noro G, Abete P, et al. (2006) Diagnosis and characteristics of syncope in older patients referred to geriatric departments. J Am Geriatr Soc 54: 1531-1536.
- Dey AB, Stout NR, Kenny RA (1997) Cardiovascular syncope is the most common cause of drop attacks in the elderly. Pacing Clin Electrophysiol 20: 818-819.
- Wold JHF, Ruiter JH, Cornel JH, Vogels RLC, Jansen RWMM (2015) A multidisciplinary care pathway for the evaluation of falls and syncope in geriatric patients. Eur Geriatric Med 6: 487-494.
- Tinetti ME, Williams CS (1997) Falls, injuries due to falls, and the risk of admission to a nursing home. New Engl J Med 337: 1279-1284.
- Khera S, Palaniswamy C, Aronow WS, Sule S, Doshi JV, et al. (2013) Predictors of mortality, rehospitalization for syncope, and cardiac syncope in 352 consecutive elderly patients with syncope. J Am Med Dir Assoc 14: 326-330.
- Hartholt KA, Polinder S, Van der Cammen TJ, Panneman MJ, Van der Velde N, et al. (2012) Costs of falls in an ageing population: A nationwide study from the Netherlands (2007-2009). Injury 43: 1199-1203.
- Croci F, Brignole M, Alboni P, Menozzi C, Raviele A, et al. (2002) The application of a standardized strategy of evaluation in patients with syncope referred to three syncope units. Europace 4: 351-355.
- Sarasin FP, Hanusa BH, Perneger T, Louis-Simonet M, Rajeswaran A, et al. (2003) A risk score to predict arrhythmias in patients with unexplained syncope. Academic Emer Med 10: 1312-1317.
- Brignole M, Vardas P, Hoffman E, Huikuri H, Moya A (2009) Indications for the use of diagnostic implantable and external ECG loop recorders. Europace 11: 671-687.
- Furukawa T, Maggi R, Bertolone C, Ammirati F, Santini M, et al. (2011) Effectiveness of remote monitoring in the management of syncope and palpitations. Europace 13: 431–437.
- Parry S, Matthews I (2010) Implantable loop recorders in the investigation of unexplained syncope: a state of the art review. Heart 96: 1611-1616.
- Parry SW, Matthews I (2010) The implantable loop recorder in older patients with syncope: is sooner better?. Age Ageing 39: 284-285.
- Guidelines on “Preventie van valincidenten bij ouderen” (2004) Alphen aan den Rijn: Van Zuiden Communications B.V, Netherlands.
- Kenny RA, Rubenstein LZ, Tinetti ME, Brewer K, Cameron KA, et al. (2011) Summary of the updated American Geriatrics Society / British Geriatrics Society clinical practice guideline for prevention of falls in older persons. J Am Geriatr Soc 59: 148-157.
- Solbiati M, Costantino G, Casazza G, Dipaola F, Galli A, et al. (2016) Implantable loop recorder versus conventional diagnostic workup for unexplained recurrent syncope. Cochrane Database Syst Rev 4: CD011637.
- Salih H, Monsel F, Sergent J, Amara W (2012) Long-term follow-up after implantable loop recorder in patients with syncope: results of a French general hospital survey. Ann Cardiol Angeiol (Paris) 61: 331-337.
- Vitale E, Ungar A, Maggi R, Francese M, Lunati M, et al. (2010) Discrepancy between clinical practice and standardized indications for an implantable loop recorder in patients with unexplained syncope. Europace 12: 1475-1479.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi