Research Article, J Trauma Stress Disor Treat Vol: 9 Issue: 2
A Pilot Evaluation of a 2 Hour Intervention Breathing Method in Multiply Traumatized Individuals
Harald Walach*1,2,3, Michael A. Persinger+ and Patrick Palucki4
1Medical University Poznan, Dept. Gastroenterology, Poznan, Poland
2University Witten-Herdecke, Dept. Psychology, Witten, Germany
3Holistic Coaching & Research, Berlin, Germany
*Corresponding Author: Dr. Harald Walach
University Witten-Herdecke, Dept. Psychology
Witten, Germany
Email: harald.walach@uni-wh.de
Received: January 17, 2020 Accepted: March 18, 2020 Published: March 25,, 2020
Citation: Walach H, Persinger MA, Palucki P (2020) A Pilot Evaluation of a 2 Hour Intervention Breathing Method in Multiply Traumatized Individuals. J Trauma Stress Disor Treat 9:2.
Abstract
Objective: Many trauma sufferers seek out alternative treatments. We report the results of a pilot observational outcome study of a 2-hour intensive breathing and awareness intervention in eleven multiply traumatized individuals, 9 of whom completed the intervention and the 30 day follow-up questionnaire.
Methodology: Observational outcome evaluation using a mixedmethods approach: Outcome was documented by applying the Profile of Moods State Questionnaire and a qualitative questionnaire.
Results: Effect size for POMS-Total score from pre-measurement to follow-up was high d=1.4, and was even higher for some subscales, such as “tense” (d=2.7) or “negative mood” (d=2.0). Only the subscale “vigour” did not show an effect. Qualitative questionnaire data after about one month supported the quantitative data: all nine participants reported good effects, some even dramatic improvements.
Conclusion: This small pilot study documents beneficial effects of this breathing method which should be studied more formally in a randomized study.
Keywords: Psychological trauma, PTSD, Breathing method, Mindfulness, Imagination, Outcome evaluation, Alternative therapies, Neoshamanism, Post-traumatic growth
Keywords
Psychological trauma, PTSD, Breathing method, Mindfulness, Imagination, Outcome evaluation, Alternative therapies
Introduction
Childhood psychological trauma is a comparatively frequent if extremely worrying danger of growing up. In a random sample of USAmerican children 30% had suffered trauma, and 14% of them up to three or more traumatic events [1]. Sexual trauma and abuse is, next to physical violence, among the most frequent causes of childhood trauma. Unsurprisingly, childhood trauma is associated with a 30% increased risk of later psychological or psychiatric disturbance [1]. Psychological treatment options exist and are considered effective for post-traumatic stress disorder [2,3]. Meta-analyses of existing treatments document medium to large effect sizes for treatments such as mode-deactivation treatment, a specialized form of cognitive behavioural treatment for adolescents [4], and for trauma specific therapies [5]. Against no treatment controls trauma focused therapies have large effect sizes, with prolonged exposition (PE) demonstrating the largest effect size (g=1.43), followed by Cognitive Processing Therapy (CPT; g=1.07) and by Eye Movement and Desensitization Treatment (EMDR; g=0.63). These effect sizes dwindle towards zero when the comparison standard is a trauma-focused Cognitive Behavioural Therapy. They are still sizeable, when the comparison is against supportive therapies, with effect sizes between g=0.66 and g=1.37, and against other, non-specific therapies, with effect sizes between half a standard deviation and g=0.89 [5]. This shows that successful psychological treatments for trauma, post-traumatic stress disorders and their sequelae have been developed, thoroughly researched, and made available in health services systems of various countries over the past decades. Despite this positive and promising state of the art of trauma therapy, the fact remains that many do not seek out such treatments or do not profit from them. A Cochrane review [6] estimated much smaller treatment effects of around half a standard deviation than Cusack and colleagues and Lenz and others, and found that drop-out rates are significantly higher for psychological treatments than for treatment as usual. These dropout rates can be seen as proxy estimators for the fact that effects of manualized treatments are measured across groups of people, and not across single individuals. While the average trauma-sufferer might profit to a large degree, unfortunately the average sufferer does not exist, but only individual sufferers of trauma with a wide variety in terms of history, background and resources. Some will profit from the therapies offered, some will not, and some will even deteriorate. Even though therapies might be, on average, very effective, there will always be single patients that will not profit. Thus, the search for effective approaches on a general and individual basis for individuals with traumatic life experiences or multiple traumata is still on.
Many trauma sufferers who do not benefit from such standard treatments seek out alternatives. Often they are drawn to the open or grey market of unregulated therapies. Such methods are generally under research. One such method is the so called Palucki-method, named after her inventor Ilona Palucki (IP). It is as breathing and mindfulness- based approach inspired by neo-shamanistic insights. Within the neo-shamanistic approach imaginative and breathing techniques have been variably used to treat traumatic subjects [7,8]. While in the classical shamanic view the shaman travels the netherworld or other worlds on behalf of the patient to find the fragmented soul and brings it back, in the method studied here the work is done by therapist and patient together. While the therapist uses soft and deep breathing techniques to focus attention on the physical and psychological states, she also teaches the patients to use their imagination to let go of symbols or representations of their traumatic experiences with their breath. In that respect such approaches are to some extent similar to the mode-deactivation therapy [4], or mindfulness- based approaches in which a calm psychological state, induced through mindful breathing is used to confront the traumatic experiences and images associated with them and allow them to pass by. Such an approach was studied here [9].
Methodology
The purpose of this pilot evaluation was to study the acceptability and potential effects of a single intervention of the imagination and mindfulness based Palucki method in self-referred traumatised individuals who had suffered from one or multiple traumatic experiences in the past, mostly severe physical abuse, sexual abuse, life-threatening experiences or a mixture of them. Most of the individuals who took advantage of the offer had had experience with one or more conventional therapeutic approaches without lasting success. The research was conducted in the late Dr. Michael A. Persinger’s lab at the Laurentian University in Ontario, Canada, who had also organized ethical approval. Potential participants were invited via public channels and offered one session of this method for free. They gave written informed consent, and were required to fill in a demographics questionnaire at the beginning of the study, as well as a Profile of Moods State [10] immediately before t1, after t2 and approximately 10 days after the treatment t3. Still 3 to 8 weeks after the treatment (on average after 39 days) participants also filled in an open questionnaire about the effects they had observed after the healing session. The open questionnaires were submitted to a content analysis. Questionnaires were given out by and handed in to research assistants who were independent. The only role of the therapist, IP, was to make sure that the individuals seeking treatment were indeed suffering from the sequelae of a traumatic experience and to deliver one treatment of her method to the individuals in single sessions.
The session lasted from about 1.5 to three hours and was individually geared to the person’s experience. The treatment started typically with a deep breathing technique followed by some imaginative elements and ended by verbal processing of the experience. The essence of the treatment is finding out about the core traumatic experience, giving it an imaginary representation and then using breathing and self-affirmations to distance the image and with it the experience from the center of the self. This makes the immediate grip of the traumatic experience less threatening and loosens it up, which, as a consequence, gives the trauma survivor some freedom to deal with it.
Results
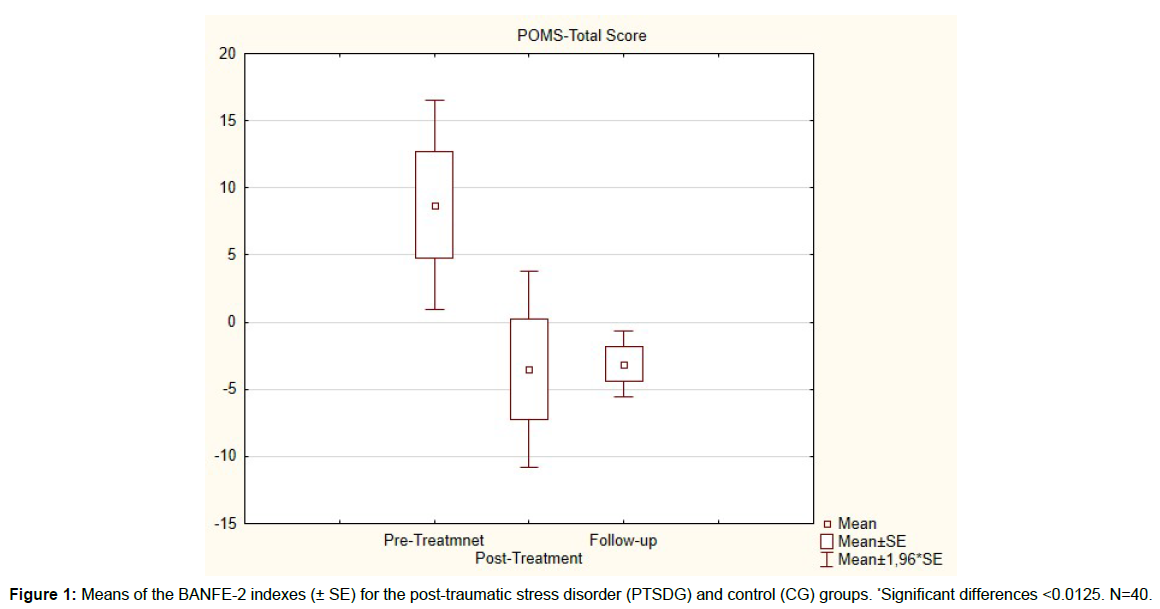
Eleven individuals were included and two did not complete the study. One arrived too late to follow the instructions of the treatment, and one person did only return the t-2 questionnaire but did not come back for the follow-up questionnaire. Nine individuals provided full data. The median age was 39 years (mean: 36.4 years, 8.5 years standard deviation; 23-47 years), and 8 of these were female. All had at least completed high school and 4 of them had a graduate education. Five were in the low- income stratum below 20.000 CAD, two had between 50k and 100k annual income, the rest was in between. Nine considered “Mind over matter real”, eleven had déjà-vu experiences, nine had out-of-body experiences or lucid dreams and six believed in life after death. Thus, the sample can be considered high in extraordinary experiences. The Table 1 reports the POMS summary scales before, immediately after treatment and about 9 days after the treatment. As can be seen, all scores changed clearly for the better. Effect sizes are generally large, except for “Vigour”. This is supported by an orienting non-parametric Friedman test for time-trend on the POMS-Total Score (Box Plot represented in the Figure 1; Chi2=8.2; df=9/2; p<0.016), with single Wilcoxon tests confirming that the major effect was between t1 and t2 (z=2.4; p<0.02), and then remained stable (z=0.0; p=1.0).
| Baseline - t1 (n= 11) |
After - t2 (n= 10) |
Follow-Up - t3 (n=9) | Effect Size d for Pre-Post | Effect Size d for Pre- Follow-up | |
|---|---|---|---|---|---|
| Tense | 3.8 (3.6) | 0.4 (0.8) | 0.3 (0.5) | 1.5 | 2.7 |
| [1.4-6.2] | [-0.2-1.0] | [-0.05-0.7] | |||
| Depressed | 3.3 (3.4) | 0.5 (1.6) | 0.4 (0.7) | 1.1 | 1.1 |
| [1.0-5.6] | [-0.6-1.6] | [-0.1-1.0] | |||
| Anger | 1.1 (1.9) | 0.2 (0.6) | 0.1 (0.3) | 0.7 | 0.9 |
| [-0.2-2.4] | [-0.2-0.6] | [-0.1-0.4] | |||
| Vigour | 6.5 (4.2) | 8.3 (6.0) | 6.3 (3.2) | 0.35 | -0.05 |
| [3.7-9.4] | [4.0-12.6] | [3.9-8.8] | |||
| Fatigue | 6.1 (3.4) | 4.8 (4.2) | 2.9 (3.0) | 0.3 | 1 |
| [3.8-8.3] | [1.8-7.8] | [0.6-5.2] | |||
| Confusion | 1.0 (1.8) | -1.1 (1.4) | -0.6 (0.9) | 1.3 | 1.2 |
| [-0.2-2.2] | [-2.1—0.1] | [-0.6 - -1.2] | |||
| Negative Mood * | 15.3 (11.0) | 4.8 (6.8) | 3.2 (1.2) | 1.2 | 2 |
| [7.8-22.7] | [-0.07 – 9.7] | [0.5 – 6.0] | |||
| POMS Total** | 8.7 (13.1) | -3.5 (11.7) | -3.1 (3.8) | 1 | 1.4 |
| [-0.1 – 17.6] | [-11.9 – 4.9] | [-6.0 - -0.2] |
*: Sum of all subscales without vigour
**: Sum of all subscales with vigour subtracted
Table 1: POMS – Summary Scales Before (t1), Immediately After (t2) and at 9 Day Follow-up (t3); means (standard deviations) [95%-confidence intervals].
The analysis of the qualitative data from the follow-up questionnaires showed that all participants continued employing the deep breathing technique they learned, releasing stress, becoming more present and sending negative thoughts and emotions away through the breath. Physical symptoms that had bothered the participants previously were, as a rule, not completely gone, but much relieved, such as tooth clenching, pains and stomach ache, and all but one participant reported that the breathing helped them to relieve the symptoms themselves. Some reported drastic changes after the treatment, such as no longer feeling the pain and the shame, when thinking of the trauma, having forgiven her and the perpetrators, feeling love and connectedness with life and others. Even those who felt only comparatively small changes reported that the treatment had left them changed and gave them the instrument they needed to take care of themselves, by breathing and regulating their emotions.
Discussion
For those 9 of the 11 participants that stayed with the treatment and returned questionnaires this single treatment session for participants with self-reported, multiple traumatic experiences in their past has been effective in relieving their symptoms, improving their mood and providing them with methods to help themselves and regulate their emotions. Another person benefitted from the treatment but did not provide follow-up data. This speaks to the fact that the therapist has some method on offer that can be accepted by patients. Especially the deep breathing technique was mentioned as helpful. The fact that the effects did not go away at follow-up, but rather increased in most cases and some stability of effects was documented by the qualitative follow-up questionnaires suggests that this is not just a short lived effect. Effect sizes are large and reported changes are impressive. They compare well with effect sizes of established trauma therapies that range between g=0.64 and g=1.43 against no-treatment comparison standards [5]. Although this is an uncontrolled study, effect sizes between d=1.4 and d=2.0 in the summary measures seem to be worthwhile.
What might explain such a comparatively swift improvement, considering that most effective treatments that are manualized take 12 or more sessions to reach their effect?
Is it the healer-therapist, or her method that produces changes? This cannot be determined based on this small pilot study, which has, of course, also some draw-backs. There was no clear-cut diagnostic information and no status-information that would have helped ascertain the severity of the problems. There was no control except the fact that most of the participants had already sought conventional help without much success. A controlled trial would therefore be a natural next step. One would have also liked a more clinically focused outcome measure. But the POMS describe present mood, and the fact that the mood had stabilized at follow-up together with the qualitative data make it plausible that there was a stable clinically relevant change.
It is reasonable to assume that the change observed did not happen just by accident and is likely not an artefact, as various data sources converge to a similar finding. Thus, one session of such a neo-shamanic treatment by IP was effective in relieving some of the stress and the suffering of these trauma survivors. Imagination and breathing are techniques that activate the parasympathetic system mediating powerful relaxation responses [11,12]. It is well known that a high resting heart rate is a predictor for trauma sufferers to develop chronic problems [13]. Conversely, it is reasonable to assume that reducing high autonomic arousal might be beneficial. Breathing is directly impacting heart rate and autonomic arousal [14,15]. Hence it is possible that breathing techniques can interfere with this dynamic and entrain parasympathetic arousal which counteracts stress and can, via the anti-inflammatory response [16], also impact immunological functions, general expectations, anxieties and bolster self-efficacy [17]. We also know that in a large proportion of trauma sufferers post-traumatic growth can be triggered [18]. Decisive factors for post-traumatic growth are acceptance, reappraisal, spirituality, and religious coping. It is likely that the Palucki method, using methods to confront the trauma and integrate it can support such reappraisal and coping processes and thus stimulate post-traumatic growth. In a recent study it was mainly higher hope that explained post-traumatic growth [19]. Thus, taken together, it is possible that hope, together with parasympathetic arousal through specialized breathing techniques and reappraisal via confronting the trauma through imagination triggers post-traumatic growth and integration of traumatic experiences, relieving stress and symptoms.
It goes without saying that a single, small observational cohort is not enough to provide any definitive answer. But it is enough to show that the method is acceptable to trauma sufferers and that it helps improve their mood and provides them with an instrument to deal with their heightened arousal. This was the goal of this small study and it paves the way for a more solid and broader research.
Conclusion
A single 1.5 to 3 hour treatment that teaches sufferers from traumatic events a deep breathing technique and some imagination to get rid of their negative emotions seems to be indeed effective. A deeper scrutiny of this method is therefore recommended.
Acknowledgement
This study was funded by Herrmann Marnett who funded Ilona Palucki’s expenses for the study. The late Michael A. Persinger made this research possible in his lab, and provided the ethical clearance. Mandy Scott is acknowledged for having collected the data and organized the study. Nikolaus von Stillfried ist acknowledged for consulting.
References
- Copeland WE, Shanahan L, Hinesley J, Chan RF, Aberg KA, et al. (2018) Association of childhood trauma exposure with adult psychiatric disorders and functional outcomes. JAMA Netw Open 1: e184493.
- Cusack K, Jonas DE, Forneris CA, Wines C, Sonis J, et al. (2016) Psychological treatments for adults with posttraumatic stress disorder: A systematic review and meta-analysis. Clin Psychol Rev 43: 128-141.
- Foa E, Keane TM, Friedman MJ, Cohen JA. (Eds.). (2009). Effective Treatments for PTSD: Practice Guidelines from the International Society for Traumatic Stress Studies; 2nd Edition. Chichester: Wiley-Blackwell.
- Swart J, Apsche J (2014) Mode deactivation therapy meta-analysis: Reanalysis and interpretation. Int J Behav Consult Ther 9: 16-21.
- Lenz AS, Haktanir A, Callender K (2017) Meta-Analysis of Trauma-Focused Therapies for Treating the Symptoms of Posttraumatic Stress Disorder. Journal of Counseling & Development 95: 339-353.
- Roberts NP, Roberts PA, Jones N, Bisson J (2016) Psychological therapies for post-traumatic stress disorder and comorbid substance use disorde. Cochrane Database Syst Rev
- Daigger M (2015) Imaginative Techniken in der Psychotraumatherapie: Die "innere Rettungsaktion" bei früh und komplex traumatisierten Patienten unter besonderer Berücksichtigung schamanischer Ideen. Trauma - Zeitschrift für Psychotraumatologie und ihre Anwendungen 13: 72-83.
- Ingerman S (1991) Soul Retrieval. Mending the Fragmented Self. San Francisco: Harper.
- Treleaven DA (2018) Trauma-Sensitive Mindfulness: Practices for Safe Healing. New York: Norton.
- Dworkin RH, Turk DC, Farrar JT, Haythornthwaite JA, Jensen MP, et al. (2005) Core outcome measures for chronic pain clinical trials: IMMPACT recommentatioins. Pain 113: 9-19.
- Benson H (1975) The Relaxation Response. New York: Morrow.
- Stefano GB, Fricchione GL, Slingsby BT, Benson H (2001) The placebo effect and relaxation response: neural processes and their coupling to constitutive nitric oxide. Brain Research Reviews 35: 1-19.
- Bryant RA, Harvey AG, Guthrie RM, Moulds ML (2000) A prospective study of psychophysiological arousal, acute stress disorder, and posttraumatic stress disorder. J Abnorm Psychol 109: 341-344.
- Grossman P, Taylor EW (2007) Toward understanding respiratory sinus arrhythmia : Relations to cardiac vagal tone, evolution and biobehavioral functions. Biol Psychol 74: 263-285.
- Grossman P, Wilhelm FH, Spoerle M (2004) Respiratory sinus arrhythmia, cardiac vagal control and daily activity. Am J Physiol Heart Circ Physiol 287: H728-H734.
- Tracey KJ (2007) Physiology and immunulogy of the cholinergic antiinflammatory pathway. J Clin Invest 117: 289-296.
- Pacheco-López G, Engler H, Niemi MB, Schedlowski M (2006) Expectations and associations that heal: Immunomodulatory placebo effects and its neurobiology. Brain Behav Immun 20: 430-446.
- Prati G, Pietrantoni L (2009) Optimism, Social Support, and Coping Strategies As Factors Contributing to Posttraumatic Growth: A Meta-Analysis. Journal of Loss and Trauma 14: 364-388.
- Kaye-Tzadok A, Davidson-Arad B (2016) Posttraumatic growth among women survivors of childhood sexual abuse: Its relation to cognitive strategies, posttraumatic symptoms, and resilience. Psychol Trauma 8: 550-558.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi