Review Article, J Virol Antivir Res Vol: 7 Issue: 2
Broadly Neutralizing Antibodies between HIV Vaccination and Treatment the Beginning of the End?
Mohannad Naser, Hebatullah Hassan, Nada Hisham and Manal Baddour*
Department Microbiology and Immunology, Alexandria University, Alexandria Governorate, Egypt
*Corresponding Author : Manal Baddour
Department Microbiology and Immunology, Alexandria University, Alexandria Governorate, Egypt
E-mail: manal.baddour@alexmed.edu.eg
Received: June 26, 2018 Accepted: September 12, 2018 Published: September 19, 2018
Citation: Baddour M (2018) Broadly Neutralizing Antibodies between HIV Vaccination and Treatment the Beginning of the End?. J Virol Antivir Res 7:2. doi: 10.4172/2324-8955.1000183
Abstract
For many years, HIV has been a major concern for both health professionals and researchers. Some of the HIV infected individuals develop broadly neutralizing antibodies (bNAbs). Different studies have shown that these bNAbs can be used in HIV prevention and treatment. BNAbs mostly act on four main sites (sites of vulnerability) on the viral spike of the conserved epitope known as CD4-Binding Site, First and Second Variable Domains (V1/V2) of the Env trimer, Third Variable Domain (V3)/Oligomannose Glycan Patch Involving Asn332 Glycan and Membrane Proximal External Region (MPER). Reverse vaccinology is considered a different concept of HIV prevention through figuring out the structure of bNmAbs. Although several trials were done in the field of HIV vaccination, none of them showed great success. However, there are other approaches paving the way for delivering an effective vaccine such as delivery of genes encoding neutralizing antibody which is known as antibody gene transfer. Another promising method is to target specific germ line precursor B cells to produce bNAbs against HIV by certain immunogens and there are a lot of trials doing on that nowadays. Concerning HIV treatment, research is also now directed to using these broadly neutralizing antibodies. Depending on the idea that antagonizing the CD4 cell and its co receptor can abolish the infection, many clinical trials have been done to find out a promising HIV antibody therapy. There are antibodies against CD4 cells such as Ibalizumab, and others against the coreceptor CCR5 such as Pro140 which are used in HIV therapy trials. The story does not end there, there are other concerns, due to HIV latency inside several body cells, targeting these HIV reservoir cells is indispensible. This can be achieved through antibody based molecules called CD3-targeted-bispecific-DARTs. Also an important aspect to be considered is to prevent the HIV cell to cell infection. Within this short review, we will discuss different approaches targeting HIV therapy and vaccination.
Keywords: HIV Vaccination; HIV therapy; Neutralizing antibodies; Vaccines
Introduction
HIV continues to be a major global public health issue. In 2016, an estimated 36.7 million people were living with HIV – with a global HIV prevalence of 0.8% among adults. Around 30% of these people do not know that they are infected with the virus [1].
Since the start of the epidemic, an estimated 78 million people have become infected with HIV and 35 million people have died of AIDSrelated illnesses. In 2016 alone, 1 million people died of AIDS-related illnesses [1].
Most of these infected individuals develop a humoral immune response weeks to months after infection, but it is strain specific and therefore instead of conferring immunity, it induces viral mutation [2,3]. Ten to thirty percent of these individuals will develop broadly neutralizing antibodies (bNAbs). Such antibodies can act antivirally against a wide spectrum of viruses by targeting relatively conserved regions on the HIV envelope trimmer spike. However, a minority (~1%) will produce antibodies with extensive breadth and potency (these are termed “elite neutralizers”) [2,4]. This process can take between 2 to 4 years. Yet, these are insufficient to control viral replication [5], because the native HIV1 Envs have several characteristics that could limit their ability to elicit bNAbs such as; protection of the conserved structures by variable loops [6-8], remarkable genetic diversity [9], a glycan shield [10], steric occlusion [11] and conformational masking [12].
However, human antibodies that effectively neutralize HIV1 target the HIV1 viral spike, a trimeric heterodimer composed of gp120 Env, which is involved in recognizing the CD4 receptor, and of gp41 transmembrane glycoprotein, which in turn is responsible for fusing the viral and target cell membranes [13,14].
These neutralizing Abs co-evolve together with the viruses. Eventually, mature bNAbs have unusual characteristics, particularly high somatic hyper mutations, extremely long heavy-chain complementarity determining region 3 (HCDR3) loops, and polyreactivity [3]. Moreover, isolation of the corresponding monoclonal antibodies has been facilitated by identification of favorable donors with potent bnAb containing sera and by development of improved methods for human antibody generation. Molecular studies of recombinant Envtrimers, alone and in interaction with bNAbs, are providing new insights that are fueling the development and testing of promising immunogens aimed at the elicitation of bNAbs [15].
Such bNAbs will play a significant role in guiding the new structurebased immunogenic designs and also contribute to both HIV-1 prevention and treatment fields.
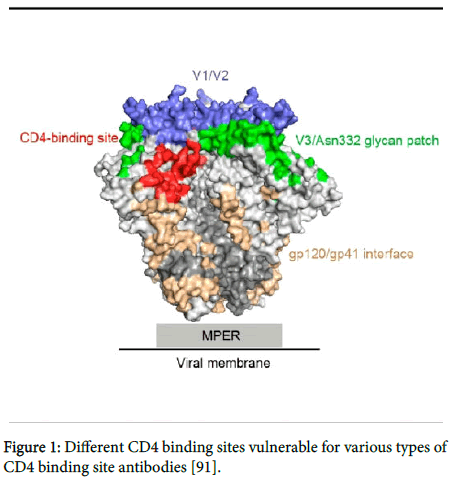
Most broadly neutralizing antibodies can be placed into four categories on the basis of the location on the viral spike of the conserved epitopes that they recognize Figure 1 [16].
Figure 1: Different CD4 binding sites vulnerable for various types of CD4 binding site antibodies [91].
Sites of Vulnerability
CD4-Binding site
The CD4-binding site is one of the conformational epitopes responsible for CD4 receptor binding. It is recessed and surrounded by glycans and variable regions which make it a conserved and protected site [17]. Despite being functionally conserved it is accessible to CD4 and the CD4bs antibodies. VRC01, a bNAb targeting CD4bs, is one of the most promising candidate vaccines and has neutralized 91% of 190 pseudoviruses with a 0.33μg/mL geometric mean IC50 [18,19]. As VRC01-class bNAbs were found in the sera of many donors, it was proposed that the human immune system can recognize vulnerable CD4-binding sites, yet the amounts produced are insufficient to control the infection. Consequently, the CD4-binding site on the Envtrimer is considered a great target for vaccine design [18].
First and second variable domains (v1/v2) of the envtrimer
This epitope includes the trimer apex of the Env quaternary structure and is highly variable. To escape neutralization, the bNAbs have developed a special and long CDRH3 “hammer-head” structure that allows antibodies to bind to the underlying protein surface (residues 165–171, as well as an Asn160 glycan). PGDM1400, is known to be one of the most efficient bNAbs which recognize V1/V2 domain, bearing a broad (83%) and potent cross-clade neutralizing activity with a median IC50 of 0.003 μg/mL [20].
Third variable domain (v3)/oligomannose glycan patch involving asn332 glycan
The V3-glycan epitopes are considered the “supersite of vulnerability” and depend on the N332 glycan [21], with several bNAbs identified to date. The first glycan-dependent bNAb to be identified was 2G12. A glycan cluster is a target of humoral immune recognition, and a glycan cluster-shielded Envtrimer is one of the classical viral evasion mechanisms [22]. Targeting these epitopes is an attractive site for vaccine development.
Membrane proximal external region (MPER)
MPER is a highly conserved region of gp41 and plays an important role in the viral fusion process [23]. It is a vulnerable site, and thus a valuable tool for HIV-1 vaccine design for the induction of neutralizing antibodies. However, the structural flexibility of the MPER is responsible for its poor immunogenicity in neutralization studies [24]. Several reports suggest that the MPER is relatively inaccessible to antibodies in the pre-fusion conformation and is exposed only transiently after CD4 binding [25-28].
A promising start
One of the most important early vaccine trials was the RV144 trial with a 31% (P=0.04) reduction in infection that correlated with the presence of antibodies that bind to the V1/V2 region of the envelope spike [29,30]. However, the antibody response induced by the vaccine did not neutralize primary HIV-1isolates, and it has been proposed that the effects were mediated instead by antibody-dependent cellular cytotoxicity (ADCC) [31].
bNAbs as vaccines
Antibodies play a crucial role as passive as well as active immunization against HIV. The combination of poor pharmacokinetic properties and limited overall breadth and potency made passive immunization with first generation bNAbs unfavourable [32-34]. Despite several achievements, there was little enthusiasm for the possibility of an antibody-based vaccine, because all of the initially characterized antibodies were unusual. There were several problems faced, including; having three combining sites, instead of the usual two (2G12 targeting V3) [35,36], being self-reactive (2F5 and 4E10 targeting MPER) [37,38] and finally, being a phage-derived antibody generated by random pairing of heavy and light chains that may have never existed in nature (b12 targeting CD4bs) [39]. Most important, however, the amount of these antibodies required for complete protection in macaques was thought to be too high to be achieved by vaccination [40]. Later on second-generation bNAbs with greater neutralization breadth and potency were developed against HIV-1. They proved to be far more effective than first-generation bNAbs in Human clinical trials as displayed in Table 1.
| Antibody binding site | Antibody | Example of clinical trials | Location Population | Phase | Recruitment status Primary purpose | References |
|---|---|---|---|---|---|---|
| CD4 binding site | VRC01 | NCT02716675 | United States, Brazil, Peru, Switzerland Estimated enrollment: 2700 participants | Phase 2 | Still recruiting Prevention | [79] |
| 3BNC117 | NCT02018510 | United states, Germany Actual enrollment: 49 participants |
Phase 1 | Completed Prevention | [80] | |
| VRC07-523lS | NCT03015181 | United States Actual enrollment: 26participants | Phase 1 | Active Non- recruiting Prevention | [81] | |
| N6 | Planned for clinical trial | [82] | ||||
| gp41 (membrane proximal external region) | 10e8 | Planned for clinical trial | [83] | |||
| Gp120-41 interface | 8ANC195 | Not yet planned for clinical trial | [84] | |||
| V1/V2-glycan | CAP256-VRC26 | Planned for clinical trial | [85] | |||
| PG9 | UK Actual enrollment: 21 participants |
Phase 1 | Active Non-recruiting Prevention | [86] | ||
| V3-glycan | PGT121 | NCT02960581 | United States Estimated enrollment: 63 participants |
Phase 1 | Enrolling by invitation Prevention | [87] |
| 10-1074 | NCT02511990 | United States, Germany Actual enrollment: 33 participants |
Phase 1 | Completed Prevention | [88] | |
| Combinations | 3BNC117+10-1074 | NCT02824536 | United States Actual enrollment:24 participants | Phase 1 | Active Non-recruiting Prevention | [89] |
| PGDM1400 and CAP256-VRC26.25 | Planned for clinical trial | [90] |
Table 1: Shows recent clinical trials using different antibodies categorized by their binding sites to achieve protection against HIV infection.
Reverse vaccinology (RV)
Reverse vaccinology refers to a reversed approach whereby starting from the known structure of bnMAbs and using them as a template, the epitope recognized by the Ab is in vitro reconstructed [41,42]. However, because HIV particles contain only a small number of proteins useful for vaccination purposes, which require a particular tertiary or quaternary conformation to be effective vaccine immunogens, this approach seems to have failed to deliver an effective, preventive HIV-1 vaccine after prolonged intensive research [43].
Germline targeting approach
Germline targeting is a vaccine priming strategy through which the affinity maturation of specific germline-precursor B cells is initiated by preferentially activating bnAb precursors [44,45]. Activating naïve B cells that express specific germline BCRs is the main purpose of germline targeting immunogens. This is achieved through: activating bnAb-precursor B cells, selecting productive (bnAb-like) somatic mutations, and finally producing memory B cells that can be boosted subsequently to select additional productive mutations [46-48].
Unfortunately, there are some limitations to the germ-line targeting approach. The limited number of available “germline-targeting” immunogens is still an obstacle and the search for additional “germline-targeting” immunogens is very active through different strategies by several groups. Also in humans, there will be competition between the B cells that express the desired BCR and a majority of B cells that bind outside the desired epitope. Moreover, it has been found in several studies that repeated immunizations with the “germline targeting” immunogen will not lead to extensive somatic hypermutation in HC and LCs and will not lead to the development of bNAbs due to viral diversity and lacking detectable affinity for supersite-bnAb germline precursor [48,49]. Additional Env variants will be required for boosting [46,50].
Furthermore, although the immunogens employed during the boost will amplify the desired B-cell clone stimulated during the prime, they will also stimulate undesirable B-cell lineages denovo [51].
Antibody gene transfer
Genetic delivery of antibody molecules: Passive transfer of monoclonal antibodies can successfully prevent HIV1 infection in humans as shown in clinical trials. However, considerable challenges regarding the cost and scaling up of the antibody product are causes of concern. So, using vector -based delivery of genes encoding antibody molecules as a means to produce sufficient levels of antibodies over a sustained period of time, is a suggested alternative approach [52].
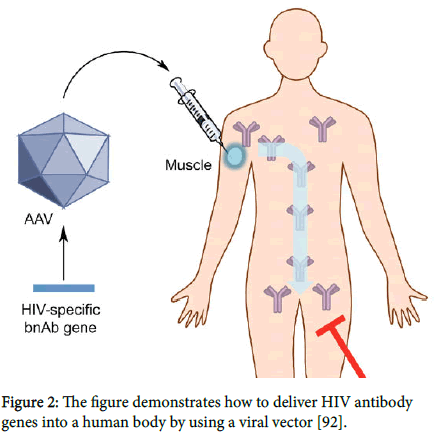
Vectored ImmunoProphylaxis (VIP): It is a gene therapy approach for generating vaccine-like protection by delivering genes (through a single injection of adeno associated virus based vectors (AAVs)) encoding nAbs into nonhematopoietic tissues, such as muscles as an alternative to traditional vaccination methods, as depicted in Figure 2 [53,54]. The advantage of this approach lies in the direct provision of nAbs through transgene expression in host cells, bypassing the reliance on the natural immune system for mounting desired humoral immune responses. VIP extends the application of monoclonal antibodies (mAbs) from passive immunization to a new form of gene therapy that is based on transfer of antibody genes and their subsequent expression in host tissues [55,56].In fact, two recent studies in animal models have demonstrated that VIP against HIV is feasible, paving the way for more clinical testing in humans [55,56].
Figure 2: The figure demonstrates how to deliver HIV antibody genes into a human body by using a viral vector [92].
Some concerns in VIP approach are: constitutive expression could induce immune responses against the VIP antibody and/or the F2A linker, in turn, leading to reduced antibody production and other unknown effects. So, as a safety precaution, it is desirable to develop a regulated expression system, such as the dimerizer-regulated gene expression system [57-59] to switch antibody expression on and off.
Treatment modalities: Based on the fact that ART is known for its ability to interfere with the virus life cycle to prevent replication, it is postulated that using FCFc receptor-mediated effector mechanism, bNAbs can neutralize the free virus and kill the infected cells. Despite obstacles in effective HIV vaccine design, several bNAbs are considered alternative approaches for HIV-1 therapy during chronic infection.
Multiple antibody-engineering technologies are suggested to produce neutralizing antibodies against HIV-1. Research is now directed to find rational antibody combinations or engineered antibodies (eAbs) as a therapy for HIV-1 infection [60].
Viral load is a major obstacle as it rebounds quickly in the infected individuals treated by either high or low dose of neutralizing therapeutic antibody. That is because of the outgrowth of pre-existing or de novo viral escape variants. So, elimination of the virus and virus-infected cells in vivo is very challenging once these resistant mutants rapidly emerge [61].
The relationship between broadly neutralizing immunity and disease progression is never correlated with the rapid virus escape, and decrease in the humoral responses along the course of the disease [61].
Targets for therapeutic bNAbs
Antibodies against CD4: HIV mediates its entrance mainly through a CD4 receptor together with its co- receptors CCR5 and CXCR4 [62]. An allogenic stem cell transplantation with 32bp homozygous deletion in the CCR5 allele to an HIV patient with acute myeloid leukemia led to undetectable HIV viral load even with discontinuation of the antiretroviral therapy [63]. Based on the same principle, it is proposed that by targeting the CD4 receptor or one of its co-receptors, HIV infection could be controlled. Some monoclonal antibodies were developed against human CD4 cellular receptor such as Ibalizumab (iMab), 6H10 and 13B8-2 [64-66]. Others were developed against CCR5 co-receptor such as the humanized mAb PRO140 [64]. The role of these antibodies in HIV therapy is still limited. Nevertheless, the second generation iMab which is a mAb that has broad and potent activity against HIV-1 by binding mainly to domain 2 (D2) of CD4 on host target cells and inhibiting a mechanical extension which occurs in beta strand between D1 and D2. This process is dependent on both time and the infectivity of the virus [64,68]. This leads to inhibition of post-CD4 binding events required to infect cells [69]. Another example of second generation mAb is PRO140 which is a monoclonal antibody directed against the CCR5 CoR (CCR5 antagonist), and it potently inhibits CCR5-mediated HIV-1 entry without blocking the natural activity of CCR5 in vitro [70].
Accordingly, these antibodies may provide new alternatives in both HIV treatment and prevention [64,65]. Triple- and quadruplemonoclonal antibody (Mab) combinations have been used to substantially improve the neutralization breadth of the treatment, as compared with the delivery of single Mab [71].
Engineered, bispecific antibodies are potentially promising candidates for HIV-1 prevention and therapy.
In 2013, Pace et al. [72], created bispecific antibodies that combine Ibalizumab (iMab) with anti-gp120 bNAbs. Two of these bispecific bNAbs are PG9-iMab and PG16-iMab.
Further concerns facing antibody therapy
Reservoir targeting: Even with potent ARVs and undetectable HIV-1 levels in the blood, HIV- 1 persists in reservoirs within multiple organ systems, including the reticuloendothelial system and is never fully eradicated [73]. Accordingly, once infection is established, the high replication and mutation rates present major obstacles to the immune system as it attempts to clear the infection [74]. Thus in order to target these reservoir cells CD3-targeted bi-specific DARTs were developed. The dual-affinity re-targeting (DART) scaffold is a bispecific, antibody based modality offering better stability and manufacturability. It has the ability to bind viral envelope with CD3- binding specificity to recruit and activate cytotoxic T cells. Accordingly, CD3-targeted bi-specific DARTs are antibody-based molecules that elicit a cell-mediated killing mechanism which is different from the Fc effector-competent bNAbs. HIVxCD3 DART molecules specifically redirect cytotoxic T cells to Env-expressing target cells and induce their lysis [75-77]. They showed enhanced potency against various HIV reservoir cells [78].
Cell to cell transmission: HIV-1 is consistently less susceptible to neutralization by multiple classes of bNAbs. The susceptibility is dependent upon both the viral strain and epitope targeted by the antibody. An important fact to be considered is that cell to cell infection cannot be prevented by some bNAbs even at high concentrations, and this is a major concern for antibody-based therapeutics and protection strategies (Table 2) [75].
| Number of Population | Location | Examples of clinical trials | Binding site | Antibody |
|---|---|---|---|---|
| 24 participants | Thailand | NCT02664415 | CD4 binding site | VRCO1 |
| 5 participants | USA | NCT01056393 | Conformational epitope on CD4 cell | Ibalizumab |
| 12 participants | USA | NCT00219986 | Monoclonal Antibodycocktail (C2F5, C2G12, C4E10) | |
| 10 participants | USA | PMC2045579 | Gp41 | 2G12, 2F5, and 4E10 |
| 14 participants | Switzerland | 15880120 | ||
| 300 participants | USA | NCT02859961 | Host CCR5 receptor | PRO 140 |
| 28 participants | NCT02355184 | |||
| 30 participants | NCT02483078 | |||
| USA | NCT02446847 | Gp41 | 3BNC117 |
Table 2: Clinical trials to treat HIV infection using bNAbs targeting different epitopes in HIV virion and CD4 cells.
Conclusions
Despite all efforts to find a highly effective vaccine against/treatment for HIV, the situation is still far from being resolved. With the unleashing of viral immunopathogenesis and discovery of bNAbs, the hope for a better outcome was heightened. Many ongoing and planned trials aiming at curbing the AIDS pandemic are undertaken. Virus reservoirs and cell to cell transmission are still formidable barriers to complete eradication. Germline targeting approaches, reverse vaccinology and genetic delivery of antibody molecules through antibody gene transfer or vectored immunoprophylaxis are among the novel vaccination modalities attempted but with moderate success. Any success in such attempts will have major impact on the public health concern.
References
- HIV/AIDS fact sheet (last updated November 2017)
- Barry SM, Mena Lora AJ, Novak RM (2014) Trial, error and breakthrough: A review of HIV vaccine development. J AIDS Clin Res 5: 359.
- Van Gils MJ, Sanders RW (2013) Broadly neutralizing antibodies against HIV-1: Templates for a vaccine. Virol 435: 46-56.
- Girard MP, Picot V, Longuet C, Nabel GJ (2013) Report of the cent gardes HIV vaccine conference: The B-cell response to HIV. part 1: broadly neutralizing antibodies fondation mérieux conference center, Veyrier du Lac, France, 5-7 November 2012. Vaccine 31: 2979-2983.
- Haynes BF, Moody MA, Liao HX, Verkoczy L, Tomaras GD (2011) Cell responses to HIV-1 infection and vaccination: pathways to preventing infection. Trends Mol Med 17: 108–116.
- Wyatt R, Kwong PD, Desjardins E, Sweet RW, Robinson J, et al. (1998) The antigenic structure of the HIV gp120 envelope glycoprotein. Nature 393:705–1110.
- Julien JP, Cupo A, Sok D, Stanfield RL, Lyumkis D, et al. (2013) Crystal structure of a soluble cleaved HIV-1 envelope trimer. Science 342: 1477–8310.
- Lyumkis D, Julien JP, de Val N, Cupo A, Potter CS, et al. (2013) Cryo-EM structure of a fully glycosylated soluble cleaved HIV-1 envelope trimer. Science 342: 1484–9010.
- McBurney SP , Ross TM. (2008) Viral sequence diversity: Challenges for AIDS vaccine designs. Expert Rev Vaccines 7:1405–1710.
- Wei X, Decker JM, Wang S, Hui H, Kappes JC, et al. (2003) Antibody neutralization and escape by HIV-1. Nature 422: 307–1210.
- Klein JS, Gnanapragasam PN, Galimidi RP, Foglesong CP, West AP, et al. (2009) Examination of the contributions of size and avidity to the neutralization mechanisms of the anti-HIV antibodies b12 and 4E10. Proc Natl Acad Sci USA 106: 7385–9010.
- Kwong PD, Doyle ML, Casper DJ, Cicala C, Leavitt SA, et al. (2002) HIV-1 evades antibody-mediated neutralization through conformational masking of receptor-binding sites. Nature 420: 678–8210.
- Wyatt R, Sodroski J (1998) The HIV‑1 envelope glycoproteins: fusogens, antigens, and immunogens. Science 280: 1884–1888.
- Pantophlet R , Burton DR. (2006) GP120: Target for neutralizing HIV‑1 antibodies. Ann Rev Immunol 24, 739–769.
- Burton DR , Hangarter L (2016) Broadly neutralizing antibodies to HIV and their role in vaccine design. Annu Rev Immunol 34: 635-659.
- Kwong PD, Mascola JR (2012) Human antibodies that neutralize HIV‑1: identification, structures, and B cell ontogenies. Immunity 37: 412–425.
- Zhou T, Xu L, Dey B, Hessell AJ, Van Ryk D, et al. (2007) Structural definition of a conserved neutralization epitope on HIV-1 gp120. Nature. 15: 445:732.
- Wu X, Yang ZY, Li Y, Hogerkorp CM, Schief WR, et al. (2010) Rational design of envelope identifies broadly neutralizing human monoclonal antibodies to HIV-1. Science 329: 856–861.
- ZhouT, Zhu J, Wu X, Moquin S, Zhang B, et al. (2013) Multi Donor analysis reveals structural elements, genetic determinants, and maturation pathway for HIV-1 neutralization by VRC01-class antibodies. Immunity 39: 245–258.
- Sok D, van Gils MJ, Pauthner M, Julien JP, Saye-Francisco KL, et al. (2014) Recombinant HIV envelope trimer selects for quaternary-dependent antibodies targeting the trimer apex. Proc Natl Acad Sci USA 111: 17624–17629.
- Kong L, Lee JH, Doores KJ, Murin CD, Julien JP, et al. (2013) Supersite of immune vulnerability on the glycosylated face of HIV-1 envelope glycoprotein gp120. Nat Struct Mol Biol 20: 796–803.
- Pancera M, Zhou T, Druz A , Georgiev IS, Soto C, et al. (2014) Structure and immune recognition of trimeric pre-fusion HIV-1 Env. Nature, 514: 455–461.
- Irimia A, Serra AM, Sarkar A, Jacak R, Kalyuzhniy O, et al. (2017) Lipid interactions and angle of approach to the HIV-1 viral membrane of broadly neutralizing antibody 10E8: Insights for vaccine and therapeutic design .Plos Pathogen 1006212.
- Montero M, Van Houten NE, Wang X, Scott JK (2008) The Membrane-Proximal External Region of the Human Immunodeficiency Virus Type 1 Envelope: Dominant Site of Antibody Neutralization and target for vaccine design. Microbiol Mol Biol Rev 72: 54-84.
- Dimitrov AS, Jacobs A, Finnegan CM, Stiegler G, Katinger H, et al. (2007) Exposure of the membrane-proximal external region of HIV-1 gp41 in the course of HIV-1 envelope e glycoprotein-mediated fusion. Biochem 46: 1398–1401.
- Frey G, Peng H, Rits-Volloch S, Morelli M, Cheng Y, et al. (2008) A fusion-intermediate state of HIV-1 gp41 targeted by broadly neutralizing antibodies. Proc Natl Acad Sci USA 105: 3739–3744.
- Rathinakumar R, Dutta M, Zhu P, Johnson WE, Roux KH (2012) Binding of anti-membrane-proximal gp41monoclonal antibodies to CD4-liganded and -unliganded human immunodeficiency virus type 1 and simian immunodeficiency virus virions. J Virol 86: 1820–1831.
- Chakrabarti BK, Walker LM, Guenaga JF,Ghobbeh A, Poignard P, et al. (2011) Direct antibody access to the HIV-1 membrane-proximal external region positively correlates with neutralization sensitivity. J Virol 85: 8217–8226.
- Rerks-Ngarm S, Pitisuttithum P, Nitayaphan S, Kaewkungwal J, Chiu J, et al. (2009) Vaccination with ALVAC and AIDSVAX to prevent HIV-1 infection in Thailand. N Engl J Med 361: 2209.
- Haynes BF, Gilbert PB, McElrath MJ, Zolla-Pazner S, Tomaras GD, et al. (2012) Immune-correlates analysis of an HIV-1 vaccine efficacy trial. N Engl J Med, 5: 366-1275.
- Bonsignori M, signori M, Pollara J, Moody MA, Alpert MD, et al. (2012) Antibody-dependent cellular cytotoxicity-mediating antibodies from an HIV-1 vaccine efficacy trial target multiple epitopes and preferentially use the VH1 gene family. J virol 86: 11521.
- TrKola A, Kuster H, Rusert P,Joos B, Fischer M, et al. (2005) Delay of HIV-1 rebound after cessation of antiretroviral therapy through - passive transfer of human neutralizing antibodies. Nat Med. 11: 61522.
- Joos B, TrKola A, Kuster H,Aceto L, Fischer M, et al. (2006) Long-Term Multiple-Dose Pharmacokinetics of Human Monoclonal Antibodies (MAbs) against Human Immunodeficiency Virus Type 1 Envelope gp120 (MAb 2G12) and gp41 (MAbs 4E10 and 2F5) Antimicrob. Agents Chemother 50: 1773-1179.
- Mehandru S, Vcelar B, Wrin T, Stiegler G, Joos B, et al. (2007) Adjunctive passive immunotherapy in human immunodeficiency virus type 1-infected individuals treated with antiviral therapy during acute and early infection. J Virol 81: 11016-1131.
- Trkola A, Purtscher M, Muster T, Ballaun C, Buchacher A, et al.(1996) Human monoclonal antibody 2G12 defines a distinctive neutralization epitope on the gp120 glycoprotein of human immunodeficiency virus type 1. J Virol 70: 1100.
- Calarese DA, Scanlan CN, Zwick MB, Deechongkit S, Mimura Y, et al. (2003) Antibody domain exchange is an immunological solution to carbohydrate cluster recognition. Science 300: 20-65.
- Haynes BF, Fleming J, St Clair EW, Katinger H, Stiegler G, et al. (2005) Cardiolipin polyspecific autoreactivity in two broadly neutralizing HIV-1 antibodies. Science 308: 1906.
- Yang G, Holl TM, Liu Y, Li Y, Lu X, et al. (2013) Identification of autoantigens recognized by the 2F5 and 4E10 broadly neutralizing HIV-1 antibodies. J Exp Med 210: 241.
- Burton DR, Pyati J, Koduri R, Sharp SJ, Thornton GB, et al. (1994) Efficient neutralization of primary isolates of HIV-1 by a recombinant human monoclonal antibody. Science 266: 10-24.
- Mascola JR, Nabel GJ (2001) Vaccines for the prevention of HIV-1 disease. Current Opinion in Immunology 13: 489.
- Burton DR (2002) Antibodies, viruses and vaccines. Nat Rev Immunol 2: 706-713.
- Walker LM, Burton DR (2010) Rational antibody-based HIV-1 vaccine design: Current approaches and future directions. Curr Opin Immunol 22: 358–366.
- Van Regenmortel MHV (2016) Structure-Based Reverse Vaccinology Failed in the Case of HIV Because it Disregarded Accepted Immunological Theory. Int J MolSci 17: 1591.
- Dimitrov DS (2010)Therapeutic antibodies, vaccines and antibodyomes.mAbs 2: 347-356.
- Xiao X, Chen W, Feng Y, Zhu Z, Prabakaran P, et al. (2009) Germline-like predecessors of broadly neutralizing antibodies lack measurable binding to HIV-1 envelope glycoproteins: Implications for evasion of immune responses and design of vaccine immunogens. Biochem Biophys Res Commun 390: 404-409.
- Dosenovic P, Von BL, Escolano A, Jardine J, Freund NT, et al. (2015) Immunization for HIV-1 Broadly Neutralizing Antibodies in Human Ig Knockin Mice. Cell 161: 1505–1515.
- Jardine JG, Ota T, Sok D, Pauthner M, Kulp DW, et al. (2015) HIV-1 VACCINES. Priming a broadly neutralizing antibody response to HIV-1 using a germline-targeting immunogen. Science 349: 156-161.
- Steichen JM, KulpD W, Tokatlian T, Escolano A, Dosenovic D, et al. (2016) HIV vaccine design to target germline precursors of glycan-dependent broadly neutralizing antibodies. Immunity 45: 483-496.
- Liao HX, Liao HX, Lynch R, Zhou T, Gao F, et al. (2013) Co-evolution of a broadly neutralizing HIV-1 antibody and founder virus. Nature 496: 469–476.
- Escolano A, Steichen JM, Dosenovic P, Kulp DW, Golijanin J, et al. (2016) Sequential Immunization Elicits Broadly Neutralizing Anti-HIV-1 Antibodies in Ig Knockin Mice . Cell 166: 1445-1458.
- Stamatatos L, Pancera M, McGuire AT (2017) Germline Targeting Immunogens. Immunol Rev 275:203-216.
- Zhang Z, Li S, Gu Y, Xia N (2016) Broadly neutralizing antibodies and the search for an HIV-1 vaccine: The end of the beginning. Int J MolSci 17:E1901.
- Berkhout B, Sanders RW (2012) Gene therapy as a vaccine for HIV-1. Expert Opin Biol Ther 12:1315-1321.
- Balazs AB, West AP (2013) Antibody gene transfer for HIV immunoprophylaxis. Nat Immunol 14:1-5.
- Balazs AB, Chen J, Hong CM, Rao DS, Yang L, et al. (2012) Antibody-based protection against HIV infection by vectored immunoprophylaxis. Nature 481:81-84.
- Johnson PR, Schnepp BC, Zhang J, Connell MJ, Greene SM, et al. (2009) Vector-mediated gene transfer engenders long-lived neutralizing activity and protection against SIV infection in monkeys. Nat Med 15:901-906.
- Rivera VM, Gao GP, Grant RL, Schnell MA, Zoltick PW, et al. (2005) Long-term pharmacologically regulated expression of erythropoietin in, primates following AAV-mediated gene transfer. Blood 105:1424-1430.
- Nguyen M, Huan-Tu G, Gonzalez-Edick M, Rivera VM, Clackson T, et al. (2007) Rapamycin-regulated control of antiangiogenic tumor therapy following raav-mediated gene transfer. Mol Ther 15:912–920.
- Fang J, Yi S, Simmons A, Tu GH, Nguyen M, et al. (2007) An antibody delivery system for regulated expression of therapeutic levels of monoclonal antibodies in vivo. Mol Ther 15:1153-1159.
- Sun M, Li Y, Zheng H (2016) Recent Progress toward Engineering HIV-1-Specific Neutralizing Monoclonal Antibodies. Front Immunol 30:39.
- Shingai M, Nishimura Y, Klein F, Mouquet H, Donau OK, et al. (2013) Antibody-mediated immunotherapy of macaques chronically infected with SHIV suppresses viraemia. Nature 503:277-280.
- Liu R, Paxton WA, Choe S, Ceradini D, Martin SR et al. (1996) Homozygous defect in HIV-1 coreceptor accounts for resistance of some multiply exposed individuals to HIV-1 infection. Cell 86:367-77.
- Hütter G, Nowak D, Mossner M, Ganepola S, Müßig A, et al. (2009) Long-Term Control of HIV by CCR5 Delta32/Delta32 Stem-Cell Transplantation. N Engl J Med 360:692-698.
- Pace C, Markowitz M (2015) Monoclonal antibodies to host cellular receptors for the treatment and prevention of HIV-1 infection. Curr Opin HIV AIDS 10:144-150.
- Spreen WR, Margolis DA, Pottage JC (2013) Long-acting injectable antiretrovirals for HIV treatment and prevention. Curr Opin HIV AIDS 8:565-571.
- Burkly L, Mulrey N, Blumenthal R, Dimitrov DS (1995) Synergistic inhibition of human immunodeficiency virus type 1 envelope glycoprotein-mediated cell fusion and infection by an antibody to CD4 domain 2 in combination with anti-gp120 antibodies. J Virol 69:4267-4273.
- Benkirane M, Corbeau P, Housset V, Devaux C (1993) An antibody that binds the immunoglobulin CDR3-like region of the CD4 molecule inhibits provirus transcription in HIV-infected T cells. EMBO J 12:4909-4921.
- Perez JR, Alonso CA, Berkovich R, Franco D, Chen MW, et al. (2014) Probing the effect of force on HIV-1 receptor CD4. ACS Nano 8:10313-10320.
- Jacobson JM, Kuritzkes DR, Godofsky E, DeJesus E, Larson JA, et al. (2009) Safety, pharmacokinetics, and antiretroviral activity of multiple doses of ibalizumab (formerly TNX-355), an anti-CD4 monoclonal antibody, in human immunodeficiency virus type 1-infected adults. Antimicrob Agents Chemother 53:450-457.
- Dau B, Holodniy M. (2009) Novel targets for antiretroviral therapy. Drugs 69:31-50.
- Kong R, Louder MK, Wagh K, Bailer RT, Camp A, et al. (2015) Improving neutralization potency and breadth by combining broadly reactive HIV-1 antibodies targeting major neutralization epitopes. J Virol 89:2659-2671.
- Pace CS, Song R, Ochsenbauer C, Andrews CD, Franco D, et al. (2013) Bispecific antibodies directed to CD4 domain 2 and HIV envelope exhibit exceptional breadth and picomolar potency against HIV-1. Proc. Natl Acad Sci USA 110:13540-13545.
- Finzi D, Blankson J, Siliciano JD, Margolick JB, Chadwick K, et al. (1999) Latent infection of CD4+ T cells provides a mechanism for lifelong persistence of HIV-1, even in patients on effective combination therapy. Nat Med 5:512-517.
- Barry SM, Lora AJM, Novak RM. (2014) Trial, Error and Breakthrough: A Review of HIV Vaccine Development J AIDS Clin Res 5:11.
- Smith SA, Derdeyn CA (2017) New connections: Cell to cell HIV-1 transmission, resistance to broadly neutralizing antibodies, and an envelope sorting motif. J Virol 91: e00149-17.
- Chichili GR, Huang L, Li H, Burke S, He L, et al. (2015) A CD3xCD123 bispecific DART for redirecting host T cells to myelogenous leukemia: pre-clinical activity and safety in non–human primates. Sci Trans Med 7: 289ra82.
- Wong R, Pepper C, Brennan P, Nagorsen D, Man S, et al. (2013) Blinatumomab induces autologous T cell killing of chronic lymphocytic leukemia cells. Haematologica 98:1930-1938.
- Schiller J, Chackerian B (2014) Why HIV virions have low numbers of envelope spikes: implications for vaccine development. PLoS Pathog 10:e1004254.
- US National library of Medicine (2018) Study record detail USA.
- US National library of Medicine (2016) Study record detail USA.
- US National library of Medicine (2018) Study record detail USA.
- Huang J, Kang BH, Ishida E, Zhou T, Griesman T, et al. (2016) Identification of a CD4-Binding-Site Antibody to HIV that Evolved Near-Pan Neutralization Breadth. Immunity 45:1108-1121.
- Yu Y, Tong P, Li Y, Lu Z, Chen Y (2014) 10E8-like neutralizing antibodies against HIV-1 induced using a precisely designed conformational peptide as a vaccine prime. Sci China Life Sci 57:117-127.
- Scharf L, Wang H, Gao H, Chen S, McDowall AW, et al. (2015) Broadly Neutralizing Antibody 8ANC195 Recognizes Closed and Open States of HIV-1 Env. Cell 162: 1379-1390.
- Doria RNA, Schramm CA, Gorman J, Moore PL, Bhiman JN (2014) Developmental pathway for potent V1V2-directed HIV-neutralizing antibodies. Nature 509:55-62.
- US National library of Medicine (2018) A Phase 1, Randomized, Blinded, Dose-escalation Study of rAAV1-PG9DP Recombinant AAV Vector Coding for PG9 Antibody in Healthy Male Adults. Study record detail USA.
- US National library of Medicine (2017) A Clinical Trial of the Safety, Pharmacokinetics and Antiviral Activity of PGT121 Monoclonal Antibody (mAb) in HIV-uninfected and HIV-infected Adults. Study record detail USA.
- US National library of Medicine (2018) A Study of the Safety, Pharmacokinetics and Antiretroviral Activity of 10-1074. Study record detail USA.
- U.S National library of Medicine ( 2017) 3BNC117 and 10-1074 in HIV Uninfected Adults. Study record detail USA.
- Julg B, Tartaglia LJ, Keele BF, Wagh K, Pegu A, et al. (2017) Broadly neutralizing antibodies targeting the HIV-1 envelope V2 apex confer robust protection against a clade C SHIV challenge. Sci Transl Med 9:e1321.
- Zhang Z, Li S, Gu Y, Xia N (2016) Antiviral Therapy by HIV-1 Broadly Neutralizing and Inhibitory Antibodies. Int J Mol Sci 17:11.
- Yang L, Wang P (2014) Passive Immunization against HIV/AIDS by Antibody Gene Transfer. Viruses 6: 428-447.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi