Research Article, J Physiother Rehabil Vol: 2 Issue: 1
Characteristics, Distribution and Behavior of Sensory Responses of the Straight Leg Raise Test in Asymptomatic Individuals
Mark Gugliotti1*, Peter Douris1, John Handrakis1,2, Michael Shacklock3, Alessandro Asaro1, Robert Garrick1, Gleb Kartsev1 and Yiyu Lin1
1Department of Physical Therapy, New York Institute of Technology, Old Westbury, New York, USA
2Department of Physical Therapy, New York Institute of Technology, VA RR&D National Center for the Medical Consequences of Spinal Cord Injury, James J. Peters VA Medical Center, Bronx, New York, USA
3Neurodynamic Solutions, Adelaide, Australia
*Corresponding Author : Mark Gugliotti
Department of Physical Therapy, New York Institute of Technology, Old Westbury, New York, United States of America
Tel: 631-929-7276
Fax: 631-929-7276
E-mail: mgugliot@nyit.edu
Received: January 25, 2018 Accepted: February 07, 2018 Published: February 13, 2018
Citation: Gugliotti M, Douris P, Handrakis J, Shacklock M, Asaro1 A, et al. (2018) Characteristics, Distribution and Behavior of Sensory Responses of the Straight Leg Raise Test in Asymptomatic Individuals. J Physiother Rehabil 2:1.
Abstract
Objectives: The purpose of our study was to examine the characteristics, distribution, and behavior of sensory responses of the straight leg raise (SLR) test in asymptomatic individuals. We hypothesized that: �?? The sensory response would be along the sciatic nerve distribution and its distal tributaries �?? No significant difference in sensory response would exist between limbs.
Method: The range of motion (ROM), quality, quantity, and distribution of sensory responses were measured in 47 asymptomatic individuals during the SLR test. Passive ankle dorsiflexion and passive neck flexion were used as neural sensitizing maneuvers.
Results: The mean ± SD ROM for passive terminal hip flexion was 81 ± 18.5° and 80 ± 17.8° for left and right hips, respectively. All sensory responses experienced were along the sciatic nerve distribution. The mean ± SD of all sensory responses for the left and right lower extremities were respectively as follows: stretching was 6.25 ± 1.75 and 6.63 ± 2.09 cm (p=0.11); burning was 4.28 ± 3.07 and 6.70 ± 5.39 cm (p=0.15); tingling was 2.65 ± 3.06 and 2.63 ± 3.05 cm (p=0.98); and numbness was 2.80 ± 0.14 and 0.60 ± 0.14 cm (p=0.06).
Conclusion: There are no significant differences in sensory response between limbs during the SLR test in asymptomatic individuals. Sensory responses were along the sciatic nerve distribution and its distal tributaries. These responses were intensified with the addition of passive ankle dorsiflexion suggesting it is an effective neural sensitizing maneuver when performing the SLR test.
Keywords: Neurodynamics; Straight leg raise; Sciatic nerve; Neural mobilization; Manual therapy; Mechanosensitivity; Structural differentiation; Sensory response
Introduction
Neurodynamic tests generally are used by clinicians to develop clinical hypotheses in the assessment of the mechanical and physiological function of neural tissue in patients with neuromusculoskeletal problems [1-4]. These tests assist the clinician when examining for possible mechanosensitivity of the neural tissues to forces such as tension, compression, and/or sliding with respect to their surrounding tissues [3,5,6]. In the healthy situation, the neural tissues ought to tolerate normal mechanical forces and move appropriately. In previous studies involving neurodynamic tests in asymptomatic individuals, the tests normally elicit a sensory response that quickly abates when the force is withdrawn [7,8]. The response usually consists of stretching in a specific area of the limb and can sometimes cause burning, tingling, and/or numbness to occur. Any inability to tolerate these normal mechanical forces may result in an adverse clinical response. This may be suggestive of a symptomatic pathological process such as neuritis or radiculitis, neuropathy or radiculopathy and/or underlying pathology or other clinical disorder [6,9-16]. The straight leg raise test (SLR) is the most widely used of the neurodynamic tests. It moves the neural structures from the tibial nerve through the sciatic nerve and spinal cord [17-23]. The test is used to evaluate the mechanical and physiologic responses of the sciatic nerve and its proximal and distal tributaries to application of movement and tension [1,2,4,7,8]. It is a passive maneuver performed by the clinician while the patient lies supine. First published in 1880 by Lazaravić, then Forst, in homage to his mentor Charles Lasègue, the test was described as a method in determining if an individual’s source of sciatic pain was caused by muscular compression [22,24]. Forst and Lasègue’s contemporaries disagreed and suggested the response to the SLR test was due to stretching of the sciatic nerve [25-27]. Current studies and reviews have shown the SLR test to be beneficial in the diagnosis of lumbosacral pathologies such as lumbar disc herniation and lumbar radiculopathy [10,28-34]. Nerve root and peripheral nerve compression can increase the mechanosensitivity of the local nerve tissue and impair its mechanical function [6,16,35,36]. Alterations in mechanosensitivity may manifest in patients during the SLR test in the form of reproduction of the patient’s clinical symptoms, which may include pain, burning, tingling, and/or numbness. [3,4,8,10]. The normal sensory response to the SLR test has not been widely documented in the literature. Research shows that the distribution of sensory response related to the SLR is limited to the posterior thigh along the sciatic nerve distribution [5,37-39]. Although each study yielded similar findings, their methodologies varied greatly and not all works underwent the rigors of a formal peer-reviewed process prior to publication. The purpose of our study was to examine the normal sensory response and distribution of the SLR test on asymptomatic individuals. We hypothesized that the sensory response would: 1) be along the sciatic nerve distribution and its distal tributaries; and 2) not significantly differ between limbs.
Materials and Methods
Participants
Forty-seven asymptomatic individuals between the ages of 40 and 60 years with a mean age of 49.9 (6.3) were recruited from the local community through IRB-approved flyers. All participants provided written informed consent to participate in this study. Participants were excluded if any of the following were present: history of musculoskeletal injuries within the past 6 months, limitations in hip, ankle or cervical range of motion (ROM) preventing full participation, current or prior history of cervical/lumbar radiculopathy, current pregnancy, or any other health related issues that may interfere with the individual’s ability to safely participate in this study. The study was approved by the Biomedical and Health Sciences Institutional Review Board of the New York Institute of Technology (BHS-1116). All 47 individuals (26 males, 21 females) participated in this study. In order to standardize each individual’s responses, the principal investigator (PI) provided instructions for the outcome measurement tool used. Four individual 10cm visual analogue scales (VAS) depicting sensory responses of stretching, burning, tingling, and numbness were used to document the intensity of each sensory response. The PI reviewed the scales with each participant and described each sensory response to ensure accurate responses. A body chart depicting the left and right lower extremity was reviewed and used to document the distribution of all sensory responses. Once the SLR and neural sensitizing maneuvers were completed, each participant was asked to rate the intensity and quality of their responses using the appropriate VAS. Every individual was asked to mark the location of his or her perceived sensory responses on the body chart. Leg dominance was also documented at this time. This was determined by asking what leg they would choose to kick a ball. The variables measured in this study were hip flexion ROM and the quality, quantity, and distribution of sensory responses; all just prior to the participant’s limit of tolerance and available range.
Procedures
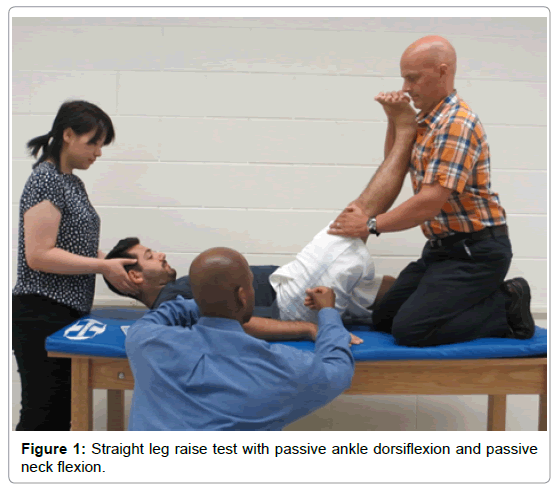
Participants were asked to lie supine on a standard treatment table with their head resting flat while their trunk and limbs were in a neutral position. The greater trochanter was palpated to determine the axis of rotation for proper placement of the goniometer. The stationary arm was aligned with the mid-line of the trunk while the moving arm was aligned with the lateral femoral condyle [40]. The leg to be tested was fully supported by one hand of the PI while the other hand maintained ventral pressure on the distal thigh just above the knee. This was to ensure full knee extension was maintained throughout the SLR [4,7,8]. A neutral ankle position of approximately 10° of plantar flexion without bias of inversion or eversion was maintained. The leg was then passively lifted from the table in the sagittal plane and raised until the individual’s initial onset of sensory response. The SLR was then advanced until the individual’s limit of tolerance. The limit of tolerance was subjectively decided by each individual and based upon the intensity of the sensory response (stretching, burning, tingling, numbness) they experienced at the end of hip flexion ROM. The angle of hip flexion was measured at that point. In order to structurally differentiate tissue response, the neural sensitizing movements of passive ankle dorsiflexion (DF) and passive neck flexion (PNF) were sequentially implemented to determine if either would cause an alteration in the individual’s sensory response [4-8] (Figure 1). The combination of sensitizing maneuvers was only held momentarily to avoid any discomfort. Once DF and PNF were released and the limb was lowered, each participant marked the intensity and quality of their responses using the appropriate VAS.
Intra-tester reliability
The ROM of hip flexion for 10 individuals (8 men and 2 women) was performed separately from the main study to establish intratester reliability of the operator. A standard 8-inch goniometer was used to measure hip flexion from 0° to 90°. Standardized placement of the stationary and moving arms was utilized [40]. The same operator performed ROM measurements throughout the entire study and no methods of blinding were applied.
Statistical analysis
All data analysis was performed using SPSS (Version 22.0, IBM, Armonk, NY, USA.) Hip flexion ROM (°) and sensory response (cm) for both lower extremities were analyzed using paired t-tests. Significance was set at an alpha level of 0.05. Intra-tester reliability was calculated using the intra-class correlation coefficient (ICC) model 2.1.
Results
Intra-tester reliability
The intra-tester reliability for hip flexion ROM during the SLR test was ICC = 1.0.
SLR test
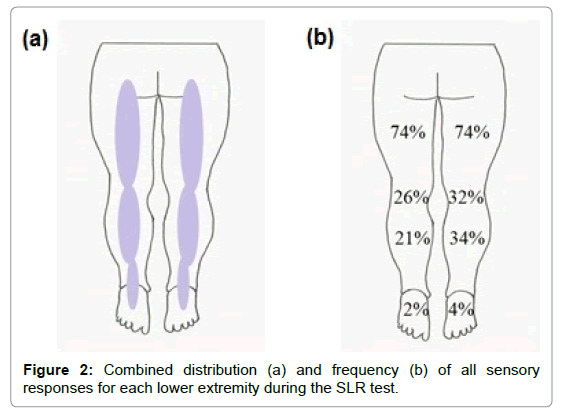
The mean end ROM for hip flexion was 81 ± 18.5° and 80 ± 17.8° for left and right hips, respectively. Hip flexion ROM was not different (p = .556) between limbs. The frequency and intensity for each individual sensory response experienced within the left and right lower extremities are depicted in Table 1. No significant difference in sensory response between limbs was found. The sensation of stretch was the most frequently reported response during the SLR test. The combined distribution and frequency of all sensory responses were reported along the posterior and plantar aspects of each lower extremity (Figure 2). Sensory responses were most prominent in the posterior aspect of the thigh. Finally, the frequency at which passive ankle dorsiflexion increased the local sensory response intensity was 98% for the left lower extremity and 89% for the right lower extremity. The frequency at which passive neck flexion increased the local sensory response intensity was 11% for both lower extremities. Forty individuals reported right limb dominance (85%) while only seven reported left limb dominance (14%).
| Descriptors | Frequency | Frequency | Intensity | Intensity | |
|---|---|---|---|---|---|
| Left LE (%) | Right LE (%) | Left LE (Mean ± SD) | Right LE (Mean ± SD) | T-Test Results | |
| Stretching (cm) | 98% | 98% | 6.25 ± 1.75 | 6.63 ± 2.09 | p = 0.11 |
| Burning (cm) | 32% | 28% | 4.28 ± 3.07 | 6.70 ± 5.39 | p = 0.15 |
| Tingling (cm) | 19% | 15% | 2.65 ± 3.06 | 2.63 ± 3.05 | p = 0.98 |
| Numbness (cm) | 4% | 12% | 2.80 ± .141 | 0.60 ± .141 | p = 0.06 |
Table 1: Individual sensory response frequency and intensity in each lower extremity (LE) during SLR test.
Discussion
This is a multi-parameter study of responses to the SLR in asymptomatic individuals involving a broad range of variables; quality, quantity and distribution of sensory responses and range of motion and, to some extent, symmetry. We hypothesized that the sensory response would, 1) be along the sciatic nerve distribution and its distal tributaries; and 2) not significantly differ between limbs. Hip flexion ROM during the SLR test ranged from 44° to 135°. These values support previous findings of responses to the SLR test at ranges between 30°-150° [1,38,41-44]. Because of this wide range, the use of structural differentiation maneuvers such as passive ankle dorsiflexion and passive neck flexion may be beneficial when attempting to confirm neural tissue involvement. The distributions and frequencies of sensory responses were reported by all participants to be along the posterior aspect and plantar surface of both lower extremities. These findings are consistent with responses reported in previous studies [5,39]. The intensity of the sensory responses was further enhanced with the use of a distant sensitizing maneuver. The frequency at which passive ankle dorsiflexion increased the local sensory response intensity was 98% for the left lower extremity and 89% for the right lower extremity.
Ankle dorsiflexion has been described as an effective means of increasing sensory response intensity making it useful in structural differentiation [43,45-47]. The disparity of sensitizer effect between limbs may be accounted for by limb dominance. It has been suggested that habitual asymmetric use of the lower extremities during daily and recreational function may create asymmetries in the tolerance of the neural tissues to movement and possibly promote ease during dominant leg testing [48]. The frequency at which passive neck flexion increased the local sensory response intensity was 11% for both lower extremities. Although passive neck flexion has been shown to be more effective as a distant sensitizer during upper limb neurodynamic and Slump tests, it has been used during SLR testing for the same purpose [37,49-51]. A key aspect of diagnosis with neurodynamic tests is whether the patient response differs from the known normal response. Here we describe in detail the normal response for clinical comparison with patient responses. Since our clinical experience is that the SLR test can produce pain, stretching, burning, tingling, and/ or numbness in patients, a key feature of classifying the patient’s test response as abnormal would be reproduction of the patient’s clinical symptoms, or part thereof.
Limitations
This study only examined the normal sensory response and distribution of the SLR test in middle-aged individuals. Whilst other studies show generally similar results to the present study, what would help in contextualizing and strengthening this study is more studies with similar results on different samples, such as younger and older populations and more comprehensive reporting of methods [38-39]. A limitation of this study is sample in terms of size (n=47) and lack of broadness for age (40-60 years). A small sample naturally reduces generalizability. Also, possibly older or younger people can present with less range of movement which may reduce the ability of a neurodynamic test to produce the same neurodynamic responses that would occur in populations of other ages. The willingness of each individual to tolerate any sensory response beyond their selfperceived limit of sensory response intensity may have additionally influenced our outcomes.
Another consideration was our oversight to monitor for any compensatory movements of the pelvic and lumbar regions during the SLR test. It has been suggested that posterior pelvic tilting and loss of lumbar lordosis can contribute to increased hip flexion during the SLR test [5,20,51,52]. It is therefore prudent to stabilize the pelvis and lumbar spine thus minimizing their influence. Finally, 28% of our participants came from diverse cultural backgrounds where, in some cases, English was not the first language spoken. Although a family member was present for reliable translation, it is possible that dialogue between researchers and participants may have been inadvertently altered or misinterpreted.
Conclusion
The results of this study provide evidence that there are no significant differences in the distribution and intensity of sensory responses between lower extremities during the SLR test in asymptomatic individuals. When performing the SLR test, the normal distribution of the sensory response is posterior, along the sciatic nerve distribution and its distal tributaries. This response can be amplified by performing a distant sensitizing maneuver such as passive ankle dorsiflexion or, to a lesser degree, passive neck flexion. These maneuvers can also assist the clinician in the process of structural differentiation when attempting to determine associated tissue involvement.
References
- Butler D (2000) The Sensitive Nervous System. Noigroup Publication, Adelaide, Australia.
- Butler D (2008) The Neurodynamic Techniques. Noigroup Publication, Adelaide, Australia.
- Shacklock M (1995) Neurodynamics. Physiotherapy 81: 9-16.
- Shacklock M (2005) Clinical Neurodynamics. A new system of musculoskeletal treatment, (1st ed.) Elsevier, London, England.
- Boyd B, Wanek L, Gray A, Topp K (2009) Mechanosensitivity of the lower extremity nervous system during straight-leg raise neurodynamic testing in healthy individuals. J Orthop Sports Phys Ther 11: 780-790.
- Kobayashi S, Shizu N, Suzuki Y, Asai T, Yoshizawa H (2003) Changes in nerve root motion and intraradicular blood flow during an intraoperative straight-leg-raising test. Spine 28: 1427-1434.
- Breig A, Troup J (1979) Biomechanical considerations in the straight leg raising test. Cadaveric and clinical studies of the effects of medial hip rotation. Spine 4: 242-250.
- Butler D. (1991) Mobilisation of the Nervous System, (1st ed.) Churchill Livingston, Melbourne, Australia.
- Vanti C, Bonfiglioli R, Calabrese M, Marinelli F, Guccione A, et al(2011) Upper limb neurodynamic test 1 and symptoms reproduction in carpal tunnel syndrome. A validity study. Man Ther 16: 258-263.
- Majlesi J, Togay H, Unalan H, Toprak S (2008) The sensitivity and specificity of the slump and the straight leg raising test in patients with lumbar disc herniation. J Clin Rheumatol 4: 87-91.
- Asbury AK, Fields HL (1984) Pain due to peripheral nerve damage: a hypothesis. Neurology 34: 1587-1590.
- Kuslich SD, Ulstrom CL, Michael CJ (1991) The tissue origin of low back pain and sciatica: a report of pain response to tissue stimulation during operations on the lumbar spine using local anesthesia. Orthop Clin North Am 22: 181-187.
- Chacur M, Milligan ED, Gazda LS, et al (2001) A new model of sciatic inflammatory neuritis (SIN): induction of unilateral and bilateral mechanical allodynia following acute unilateral peri-sciatic immune activation in rats. Pain 94: 231-244.
- Bove Gm, Ransil BJ, Lin HC, Leem JG (2003) Inflammation induces ectopic mechanical sensitivity in axons of nociceptors innervating deep tissues. J Neurophysiol. 90: 1949-1955.
- Chen C, Cavanaugh JM, Song Z, Takebayashi T, Kallakuri S, et al. (2004) Effects of nucleus pulposus on nerve root neural activity, mechanosensitivity, axonal morphology, and sodium channel expression. Spine 29: 17-25.
- Dilley A, Lynn B, Pang SJ (2005) Pressure and stretch mechanosensitivity of peripheral nerve fibres following local inflammation of the nerve trunk. Pain 117: 462-472.
- Beith I, Robins E, Richards P (1995) An assessment of the adaptive mechanisms within and surrounding the peripheral nervous system, during changes in nerve bed length resulting from underlying joint movement. In: Shacklock M (ed), Moving in on Pain. Butterworth-Heinemann, Oxford, United Kingdom.
- Coppieters MW, Alshami AM, Babri AS, Souvlis T, Kippers V, et al (2008) Strain and excursion of the sciatic, tibial and plantar nerves during a modified straight leg raising test. J Orthop Res249: 1883-1889.
- Alshami A, Babri A, Souvlis Tand Coppieters M (2008) Strain in the tibial and plantar nerves with foot and ankle movements and the influence of adjacent joint positions. J Appl Biomech 24: 368-376
- Breig A (1978) Adverse mechanical tension in the central nervous system. Almqvist and Wiksell, Stockholm, Sweden.
- Coppieters M, Andersen L, Johansen R, Giskegjerde P, Høvik M, et al (2015) Excursion of the sciatic nerve during nerve mobilization exercises: an in vivo cross-sectional study using dynamic ultrasound imaging. J Orthop Sports Phys Ther. 10: 731-737.
- Rade M, Könönen M, Vanninen R, Marttila J, Shacklock M, et al (2014) Young investigator award winner: In vivo magnetic resonance imaging measurement of spinal cord displacement in the thoracolumbar region of asymptomatic subjects: part 1: straight leg raise test. Spine 16: 1288-1293.
- Rade M, Könönen M, Vanninen R, Marttila J, Shacklock M, et al (2014) In Vivo MRI measurement of spinal cord displacement in the thoracolumbar region of asymptomatic subjects: part 2 - comparison between unilateral and bilateral straight leg raise tests. Spine 16: 1294-1300.
- Lazarević LK (1881) Ischias postica contunnii—jedan prilog za njenu diferencijalnu dijagnozu. Srpski arhiv za celokupno lekarstvo 7: 23–35.
- Forst JJ (1881) Contribution à l’EÃŒÂtude clinique de ia sciatique: thèse pour le doctorat en meÃŒÂdecine. Paris: FaculteÌ de MeÃŒÂdecine de Paris.33.
- Sjoeqvist O (1947) The mechanism of origin of Lasègue's sign. Acta Psychiatr Scand22: 290-297.
- Wilkins RH, Brody IA, (1969) Lasègue’s sign. Arch Neurol 21: 219-220.
- Capra F, Vanti C, Donati, R, Tombetti S, O’Reily C, et al (2011) Validity of the straight-leg raise test for patients with sciatic pain with or without lumbar pain using magnetic resonance imaging results as a reference standard. J Manipulative Physiol Ther 4: 231-238.
- Edgar MA, Park WM (1974) Induced pain patterns on passive straight-leg raising in lower lumbar disc protrusion. J Bone Joint Surg Br 56-B: 658-667.
- JÓ§nsson B, StrÓ§mqvist B (1995) The straight leg raising test and the severity of symptoms in lumbar disc herniation. Spine 1: 27-30.
- Scaia V, Baxter D, Cook C (2012) The pain provocation-based straight leg raise test for diagnosis of lumbar disc herniation, lumbar radiculopathy, and/or sciatica. A systematic review. J Back Musculskelet Rehabil 25: 215-223.
- Speed C (2004) Low back pain. BMJ 328: 1119-1121.
- Urban LM (1981) The straight-leg-raising test: a review. J Orthop Sports Phys Ther 3: 117-133.
- van den Hoogen HJ, Koes BW, Devillé W, van Eijk JT, Bouter LM (1996) The interobserver reproducibility of Lasègue’s sign in patients with low back pain in general practice. Br J Gen Pract 46: 727-730.
- Howe JF, Calvin WH, Loeser JD (1976) Impulses reflected from dorsal root ganglia and from focal nerve injuries. Brain Res 116: 139-144.
- Howe JF, Loeser JD, Calvin WH (1977) Mechanosensitivity of dorsal root ganglia and chronically injured axons: a physiological basis for the radicular pain of nerve root compression. Pain 3: 25-41.
- Herrington L, Bendix K, Cornwell C, Fielden N, Hankey K (2008) What is the normal response to structural differentiation within the slump and straight leg raise tests? Man Ther 13: 289-294.
- Miller A (1978) Neuro-meningeal limitation of straight leg raising. In: Daziel B, Snowsill J (eds) Proceedings of the Fifth Biennial Conference of the Manipulative Therapists’ Association of Australia.
- Slater H (1989) The effect of foot and ankle position on the SLR responses. In: Jones H, Jones M, Milde M (eds) Proceedings of the Sixth Biennial Conference of the Manipulative Therapists’ Association of Australia.
- Clarkson H Joint (2013) Motion and Function Assessment. A Research-Based Practical Guide. (3rd ed.) Williams & Wilkins, Philadelphia, PA.
- Andersson GBJ, Deyo RA (1996) History and physical examination in patients with herniated lumbar discs. Spine 21: 10-18.
- Fahrni WH (1966) Observations on straight leg-raising with special reference to nerve root adhesions. Can J Surg 1: 44-48.
- Hall T, Zusman M, Elvey R (1998) Adverse mechanical tension in the nervous system? Analysis of straight leg raise. Man Ther 3: 140-146.
- Sweetham B, Anderson J, Dalton E (1974) The relationships between little finger mobility, lumbar mobility, straight leg raising and low back pain. Rheumatol Rehabil 13: 161-166.
- Boland R, Adams R (2000) Effects of ankle dorsiflexion on range and reliability of straight leg raising. Aust J Physiother 46: 191-200.
- Gajdosik RL, LeVeau BF, Bohannon RW (1985) Effects of ankle dorsiflexion on active and passive unilateral straight leg raising. Phys Ther 10: 1478-1482.
- Vroomen P, de Krom M, Knottnerus J (2000) Consistency of history taking and physical examination in patients with suspected lumbar nerve root involvement. Spine 1: 91-97.
- Boyd BS, Villa PS (2012) Normal inter-limb differences during the straight leg raise neurodynamic test: a cross sectional study. BMC Musculoskelet Disord 13: 245-254.
- Maitland GD (1985) The slump test: examination and treatment. Aust J Physiother 6: 215-219.
- Walsh J, Flatley M, Johnston N, Bennett K (2007) Slump test: sensory responses in asymptomatic subjects. J Man Manip Ther 4: 231-238.
- Lew PC, Puentedura EJ (1985) The straight-leg-raise test and spinal posture. In: Proceedings of the Fourth Biennial Conference of the Manipulative Therapists’ Association of Australia.
- Mooney V, Robertson J (1976) The facet syndrome. Clin Orthop Relat Res 115: 149-156.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi