Short Article, J Pulm Med Vol: 2 Issue: 1
Clinical Practice Variability in the Management of Patients with Alveolar Proteinosis
Díaz SC*, Barbero E, Chiluiza D and Lobato DS
Department of Pneumological, Hospital Ramóny Cajal, Madrid, Spain
*Corresponding Author : Sánchez Díaz C
Department of Pneumological, Hospital Ramóny Cajal, Madrid, Spain
E-mail: c.sanchezdiaz91@gmail.com
Received: October 16, 2017 Accepted: January 30, 2018 Published: February 05, 2018
Citation: Baydur A, Koç M, Barbers R, May D (2018) Lung Compliance and Resistance Following Bronchial Thermoplasty in Severe Persistent Asthma: A Pilot Study and Discussion of the Physiology. J Pulm Med 2:1.
Abstract
Alveolar proteinosis is a diffuse lung disease characterized by the accumulation of an amorphous and lipoproteinaceous of inorganic powders and HIV infection. Characteristic bronchoalveolar lavage is diagnosticated (presence of positive PAS material in the alveoli (pulmonary surfactant). This disease can be congenital, primary/idiopathic (due to alteration of the stimulating factor of macrocytic colonies) or several clinical conditions like hematological diseases, inhalation proteinaceous material, PAS positive). Total lung lavage (TLL) is onsidered the gold standard treatment of this pathology.
Keywords: Proteinosis; Lung; Sex; Blood gases; Smoking; respiratory failure
Background
One problem related to alveolar proteinosis is the great variability in the management of the patients suffering alveolar proteinosis. A recent study in which 30 centers worldwide specialized in TTL were surveyed, reported that variability is specially significant in certain aspects of the technique, such as the time interval between the lavage of both lungs, the choice of the first lung to be washed, the position in which the technique is performed, contractions, methods and followup schedule, use of thoracic percussion and amount of fluid used in total [1]. In the present report we have analyzed our experience in TLL with special attention to these controversial aspects.
Our sample consists of 17 patients, with a mean age of 41.11 years old. The distribution by sex is 14 men (82.35%) and three women (17.64%). Fourteen were smokers (82.35%), 2 were not (11.76%) and the other one was not aware of smoking (5.8%). All patients were symptomatic before the procedure, but only 8 had a respiratory failure according to arterial blood gases (47.05%). Ten of the patients had a restrictive spirometric pattern before the procedure (58.8%), while the remaining 7 had a normal spirometry (41.17%). Fourteen patients had a diffusion (DLCO) disorder (82.35%), of the 3 remaining, this data was not available. All patients had radiological involvement (except for a patient whose this information was not available). Five of them had an alveolar pattern and 11 had an alveolointerstitial pattern. Eleven bipulmonary lavages were performed, 5 had no indication and the remaining one did not tolerate it.
Controversial Aspects
It is generally preferred to leave a time interval of 1-2 weeks between the lavage of both lungs; however, it has also been shown that bilateral simultaneous total lung lavage is a safe and effective technique, which improves symptoms, function pulmonary and gasometry of patients with alveolar proteinosis [2-4]. It is important the time interval or not?
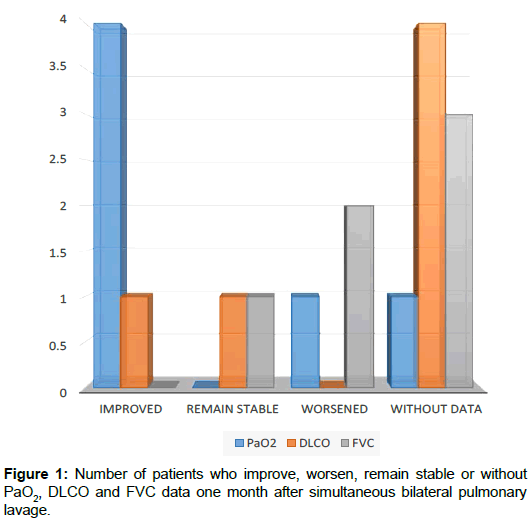
In our series of cases, in 6 patients bilateral lavage was simultaneous, one was bilateral, with one week between the lavage of both lungs and another was unilateral due to intolerance to the contralateral lung lavage. Four of the six patients who underwent bilateral simultaneous lavage, improved PaO2, one got worst and in the other do not have this data. The DLCO improved in one patient. Another one remained the same value and we do not have this information of the remaining four. We do not have FVC in three of these patients, 2 worsened, and the rest maintained the same. In the only patient who left one week between the lavage of both lungs, PaO2, DLCO, FVC and clinical was improved. We do not have radiological information. We do not have information on the evolution of the only patient who unilateral pulmonary lavage was performed, due to intolerance to the procedure (Figure 1).
The most accepted contraindications are coagulation disorders, anaesthetic risk, and cardiopulmonary instability. In our series of cases there was no contraindicated case for total lung lavage and there was only one case in which the procedure had to be stopped due to intolerance to it.
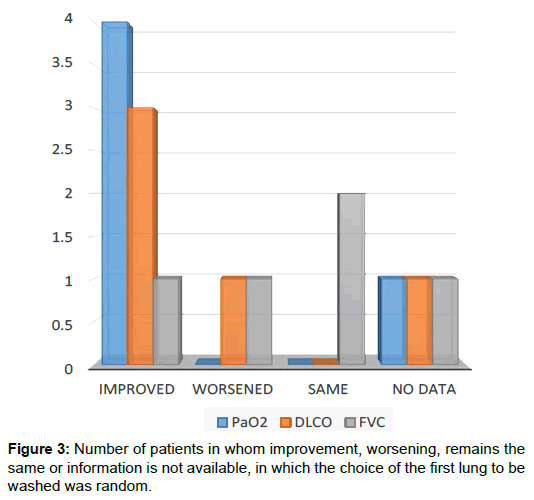
The first lung to be lavaged is the one that is most affected [5]. Three of the four patients in whom the choice of the first lung was not determined by radiological involvement, PaO2 improved, this data is unknown in the rest of them. Three of them improved the DLCO, while the rest worsened. FVC improved in one patient, remained stable in two and the rest is unknown. Clinically two improved, one worsened and another remained stable. Radiologically one remained the same and the others did not have such information.
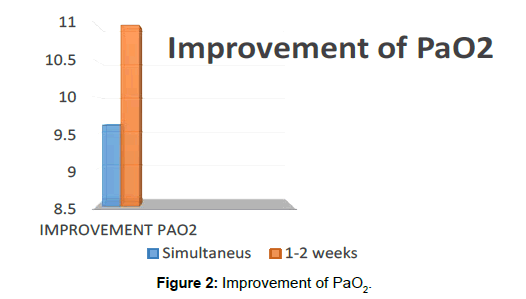
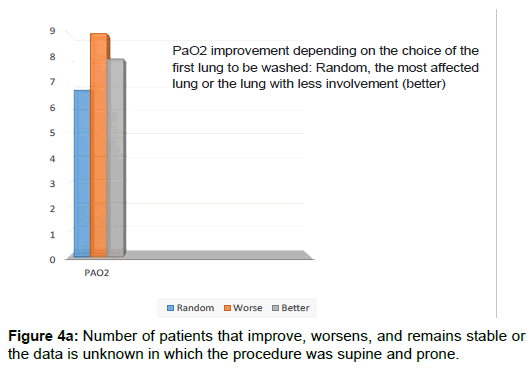
In two patients, we do not have radiological information about which lung is most affected. In the two patients in which the decision of the first lung to be washed was determined by compliance (starting with the most affected lung), in one of them PaO2 improved. We do not have any additional information. In one patient, the first lung washed, had less radiological involvement. The result was an improvement in PaO2 and FVC, however the DLCO worsened. He remained clinically and radiologically stable. The mean increase of PaO2 in patients in whom the first lung treated was random was 6.73, the improvement of PaO2 in the patient who started to wash the most affected lung was 9 points, the mean increase in PaO2 in the patient who started to wash the lung less affected was 8 points (Figure 2).
Regarding the position in which the technique should be performed, both prone and lateral decubitus are effective techniques [6,7].
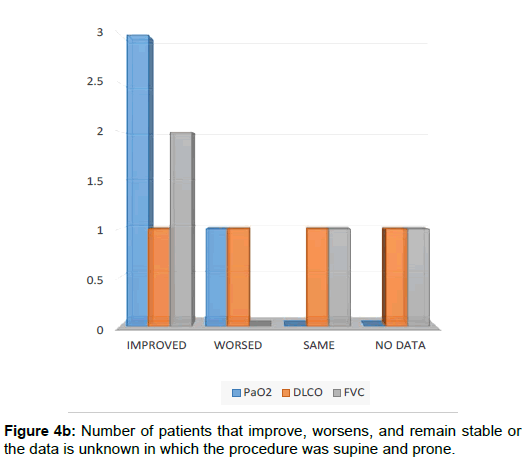
We only have position information in four patients, in which the position was prone and supine. The PaO2 improves in 3 patients, in one it worsens, the DLCO improves in 1 patient, it worsens in 1 patient, it remains stable in one patient and the data in the remaining patient is unknown. The FVC improves in two patients, in another it remains stable, in another we do not have the data. Clinically improve 3 and one worse, radiologically two remain stable, one improves and the rest we do not have the data.
The amount of fluid used to perform the WLL is critical. Although there is a general agreement about the aliquot of liquid for washing (about 800 ml of warm saline solution in adults) there is great variability in the total volume instilled by lung, ranging from 5 to 40 litters, with an average of 15.4 litters/lung [8-11]. The average of litters that were necessary to wash the left lung of the 9 patients of which we had this data is 15.55 L. the average of litres that were necessary to wash the right lung of the 9 patients of whom we had this Data is 16.55 L.
Regarding the methods and timing of follow-up, the literature describes that 50% of patients needs only one lavage, while the rest needs repeat washing in 6-12 months [12,13]. With the information available, we can affirm that three patients in whom the bilateral pulmonary lavage was simultaneous, did not need a new lavage until 10, 6 and 3 months respectively (6.33 on average). In a patient in whom the time interval between the lavage of both lungs (simultaneous or leaving 1-2 weeks) was unknown, he did not require another lavage until 28 months.
Regarding the first lung to be washed, we know that in a patient started by the lung less affected, he did not require another lavage until 48 months. In two other patients of whom we did not have radiological information it took 10 months and 3 months simultaneously until the next lavage. Another patient in which the decision of the first lung to wash was randomly (Figures 3, 4a and 4b) he needed 6 months until the next lavage.
It is stated in the literature that after each instillation a thoracic percussion of at least four or five minutes should be performed [14]. In our series of cases, no patient receives thoracic percussion.
Conclusions
- In our series of 17 cases, both bilateral simultaneous lung lavage and bilateral lung lavage leaving one week between the lavage of both lungs were safe procedures.
- In 4 of 6 patients (66.66%) in whom simultaneous bilateral total lung lavage was performed, PaO2 improved one month after the procedure.
- In the only patient in which there were 1-2 weeks between the lavage of both lungs, an improvement in PaO2 of 11 points was observed, higher than the mean improvement in PaO2 of patients in whom lavage was bilateral (mean of 9.62 points).
- Regarding the first lung to be washed, although the ascent of PaO2 is similar in patients who were randomly started with those who started with the most affected and compared with those who started with the least affected, the highest ascent Of PaO2 is observed in the patient in whom the most affected lung was started.
- Regarding the position, in all our patients the technique was performed in supine position and prone position, with good results, especially in the improvement of PaO2 and FVC.
- The average of liters that were necessary to wash the left lung of the 9 patients of which we had this data is 15.55 L. the average of liters that were necessary to wash for the right lung of the 9 patients of whom we had this Data is 16.55 L.
- Due to the characteristics of this study, we do not have enough information to know whether simultaneous bilateral lung lavage requires the use of more litters than bilateral lung lavage, leaving 1-2 weeks between both washes. We also do not know if the patients who started with the most affected lung required less liters than those who started randomly, or considering other criteria.
- In conclusion, our experience reflects the variability in the management of patients suffering alveolar proteinosis. It would be interesting to carry out a prospective study to analyze these issues.
References
- Campo I, Luisetti M, Griese M, Trapnell BC, Bonella F, et al. (2016) Whole lung lavage therapy for pulmonary alveolar proteinosis: a global survey of current practices and procedures. Orphanet J Rare Dis 11: 115.
- Silva A, Moreto A, Pinho C, Magalhães A, Morais A (2014) Bilateral whole lung lavage in pulmonary alveolar proteinosis--a retrospective study. Rev Port Pneumol 20: 254-259.
- Ichiwata T, Tokita S, Soma R, Kikuchi K, Akasaka K, et al. (2009) Unilateral total pulmonary lavage for pulmonary alveolar proteinosis and an algorithm to select lavage procedures. Nihon Kokyuki Gakkai Zasshi 47: 185-190.
- Campo I, Luisetti M, Griese M (2016) Whole lung lavage therapy for pulmonary alveolar proteinosis: a global survey of current practices and procedures. Orphanet J RareDis 11:115.
- Vymazal T, Krecmerova M (2015) Respiratory strategies and airway management in patients with pulmonary alveolar proteinosis: a review. Biomed Res Int 2015: 639543.
- Fernández del Campo R, Lozares Sánchez A, Francisco Corral G, Prieto del Portillo I, Rodríguez EP, et al. (2007) Bilateral bronchoalveolar lavage: a clinical case, method and discussion. Med. Intensiva vol.31 no.7 oct. 2007.
- Beccaria M, Luisetti M, Rodi G, Corsico A, Zoia MC, et al. (2004) Beneficio perdurable a largo plazo después del lavado pulmonar completo en la proteinosis alveolar pulmonar. Eur Respir J 5: 156-162.
- Claypool WD, Rogers RM, Matuschak GM (1984) Update on the clinical diagnosis, management, and pathogenesis of pulmonary alveolar proteinosis (phospholipidosis). Chest 85: 550-558.
- Larson RK, Gordinier R (1965) Pulmonary alveolar proteinosis: Report of six cases, Review of the literature, and formulation of a new theory. Ann Intern Med 62: 292.
- Beccaria M, Luisetti M, Rodi G, Corsico A, Zoia MC, et al. (2004) Long-term durable benefit after whole lung lavage in pulmonary alveolar proteinosis. EurRespir J 23: 526.
- Michaud G, Reddy C, Ernst A (2009) Whole-lung lavage for pulmonary alveolar proteinosis. Chest 136: 1678.
- Bonella F, Bauer PC, Griese M, Ohshimo S, Guzman G, et al. (2011) Pulmonary alveolar proteinosis: new insights from a single-center cohort of 70 patients. Respir Med 105: 1908.
- Zhao YY, Huang H, Liu YZ, Song XY, Li S, et al. (2015) Whole Lung Lavage Treatment of Chinese Patients with Autoimmune Pulmonary Alveolar Proteinosis: A Retrospective Long-term Follow-up Study. Chin Med J 128: 2714.
- Hammon WE, McCaffree DR, Cucchiara AJ (1993) A comparison of manual to mechanical chest percussion for clearance of alveolar material in patients with pulmonary alveolar proteinosis (phospholipidosis). Chest 103: 1409.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi