Clinical Image, J Clin Image Case Rep Vol: 5 Issue: 9
Dead Man Sign of ECG- a Unique Predicting Sign of Acute Coronary Syndrome
Mayank Yadav*
Department of Advanced Cardiac Center, PGIMER, Sector 12 Chandigarh, India
*Corresponding Author: Mayank Yadav
Department of Advanced Cardiac Center, PGIMER, Sector 12 Chandigarh, India
E-mail: mayank001.my@gmail.com
Received: September 03, 2021 Accepted: September 17, 2021 Published: September 24, 2021
Citation: Yadav M (2021) Dead Man Sign of ECG- a Unique Predicting Sign of Acute Coronary Syndrome. J Clin Image Case Re 5(9): 183.
Keywords: Bradyarrhythmias, Tachyarrhythmias, Thrombolytics
Introduction
This case represents inferior wall MI with unique dead man sign which predict the culprit artery and level of the block. This sign is commonly associated with the course of bradyarrhythmias and tachyarrhythmias.
Inferior wall of heart receives it blood supply from posterior descending artery branch of right coronary artery in about 70% people and in 10% it is the branch of left circumflex artery in rest 20% it receives dual blood supply form both RCA and LCX [1].
Inferior wall MI consists of 40% of all acute myocardial infarction and occurs commonly due to acute obstruction of right coronary artery with mortality rate less than 10%. Diagnosis of inferior wall infarction is made by 12 lead ECG showing ST segments elevation in leads II, aVF, III with or without reciprocal changes in lead I and a VL [2]. RV infarction is coexisted with 10-50% of inferior wall infarction and is usually diagnosed by presence of ST segment elevation in right sided chest leads from RV4-V6.In the absence of right sided leads diagnosis of right ventricular infarction is made by ST segment elevation in lead V1 with segment depression in lead V2 [3]. ST elevation myocardial infarction is treated with primary coronary intervention or thrombolytics depending upon the time duration from symptoms onset. If door to balloon time is less than 90 mins primary percutaneous intervention is the treatment of choice and rest cases are treated with thrombolytics followed by elective percutaneous intervention.
Case Presentation
We admitted a 52 years old man with the complain of chest pain and ECG was done (Figure 1) ECG is showing sinus rhythm with ventricular rate of 60 min with ST segment elevation in inferior leads (II, aVF, III) and ST segment elevation in lead V1 with ST segment depression in V2 and reciprocal ST segment depression in leads I and aVL. So, diagnosis of inferior wall myocardial infarction with Right ventricular infarction was made as there was ST segments elevation in lead III was more than lead II (III>II) and ST segment elevation in V1 with segment depression in V2 is highly specific of RV infarction when right sided chest leads are not available.
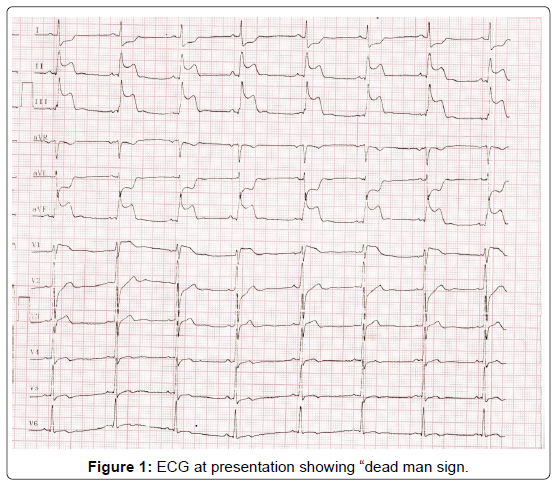
Figure 1: ECG at presentation showing “dead man sign.
Patient developed seizure like activity while taking another ECG (Figure 2) and polymorphic broad complex ventricular arrhythmia was captured in ECG which was terminated with DC shock of 150 J. As chest pain was of more than 2 hours duration so thrombolytics were administered and Post thrombolysis ECG was repeated (Figure 3).
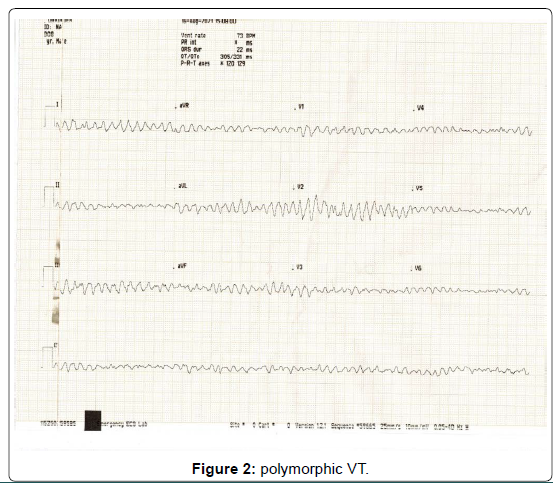
Figure 2: polymorphic VT.
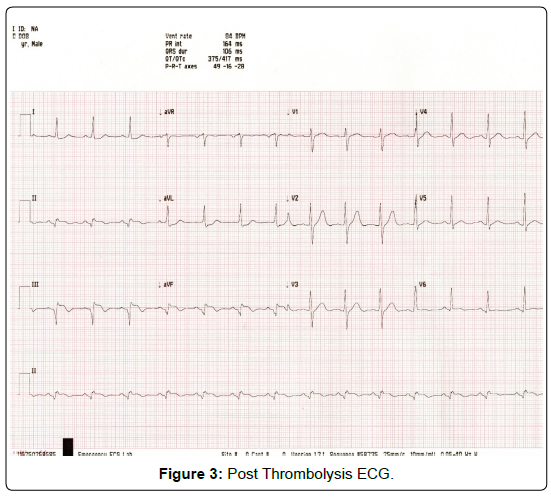
Figure 3: Post Thrombolysis ECG.
Following thrombolysis there was complete resolution of chest pain with more than 50% resolution ST segment elevation in inferior leads and in lead V1 suggestive of successful thrombolysis. Patient underwent coronary angiography which was showing normal Right coronary artery, LAD and LCX artery (Figure 4-6).
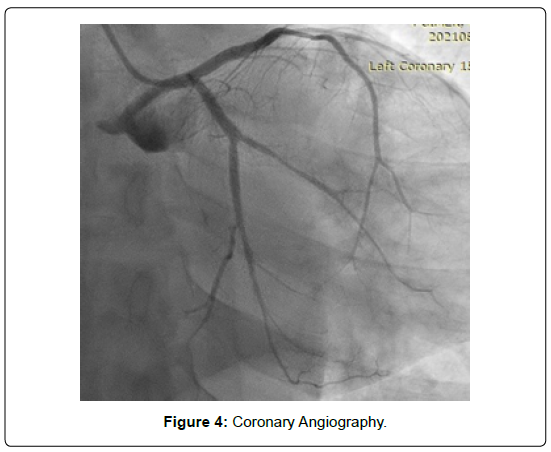
Figure 4: Coronary Angiography.
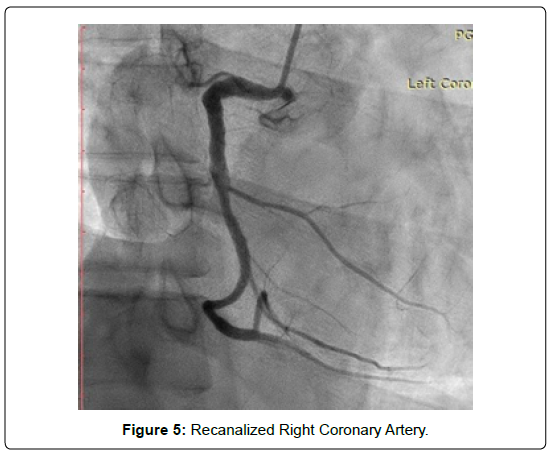
Figure 5: Recanalized Right Coronary Artery.
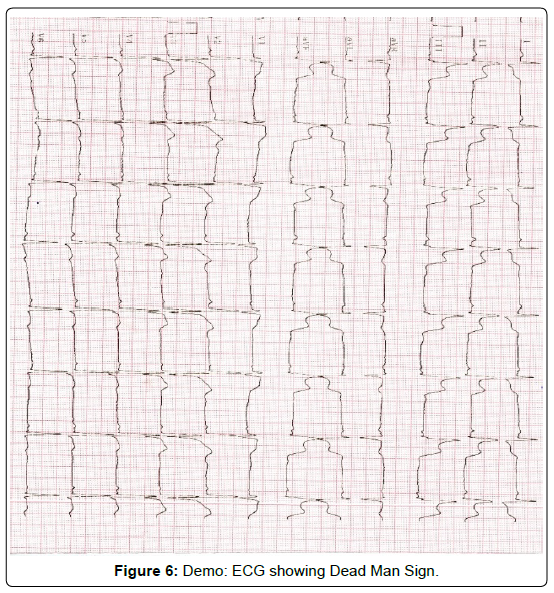
Figure 6: Demo: ECG showing Dead Man Sign.
The interesting finding present here in this ECG is that ST segment elevation in aVF and ST segment depression in aVL combinedly giving appearance of a “DEAD MAN SIGN” (dead man lying on ground). This ECG sign is associated with total or near total occlusion of right coronary artery.
Discussion
Dead man sign of ECG is suggestive of total or near total occlusion of proximal right coronary artery with course of bradyarrhythmia and tachyarrhythmia (supraventricular or ventricular tachyarrhythmias). In this case patient presented with bradycardia with the heart rate of 55/min but later he developed broad complex ventricular arrhythmia which is typically associated with dead man sign when seen with inferior wall myocardial infarction [4]. Patient received thrombolytics as presentation was more than 2 hours. following thrombolysis ST segment elevation subsided more than 50%. However proximal right coronary artery obstruction was normal on coronary angiography as patient already received thrombolytics with resolution of ST segment elevation following thrombolysis is suggestive of successful thrombolysis.
Conclusion
In conclusion this case demonstrates inferior wall myocardial infarction with RV myocardial infarction with the heart rate of 55 min later on patient developed polymorphic broad complex Ventricular tachyarrhythmia demonstrating the usual presentation seen with the dead man sign in ECG with inferior wall myocardial infarction.
References
- Shriki JE, Shinbane JS (2012) Identifying, characterizing, and classifying congenital anomalies of the coronary arteries. Radiographics 32: 453-68.
- Aydin F, Turgay Yildirim O (2018) Acute Inferior Myocardial Infarction Caused by Lightning Strike. Prehosp Disaster Med 33(6): 658-659.
- Konstam MA, Kiernan MS, Bernstein D (2018) Evaluation and Management of Right-Sided Heart Failure: A Scientific Statement from the American Heart Association. Circulation 137: 20.
- Ahamad Tramboo N (2016) A New ECG Sign. Int J Clin Med Imaging 3(1).
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi 