Case Report, Int J Ophthalmic Pathol Vol: 8 Issue: 1
Endoscopic Trans-Sinus Approach for Biopsy of the Inferior Rectus Muscle
Shani Golan1*, Ashutosh Kacker2 and Gary Lelli1
1Department of Ophthalmology, New York Presbyterian Hospital, Weill Cornell Medical College, New York, USA
2Department of Otolaryngology, New York Presbyterian Hospital, Weill Cornell Medical College, New York, USA
*Corresponding Author : Shani Golan
Department of Ophthalmology, New York Presbyterian Hospital, Weill Cornell Medical College, New York, USA
E-mail: shanigola2@gmail.com
Received: February 13, 2019 Accepted: February 22, 2019 Published: March 04, 2019
Citation: Golan S, Kacker A, Lelli G (2019) Endoscopic Trans-Sinus Approach for Biopsy of the Inferior Rectus Muscle. Int J Ophthalmic Pathol 8:1. doi: 10.4172/2324-8599.1000228
Abstract
We describe a case of a 68 year-old female presenting with a posterior left inferior rectus muscle mass. The patient underwent biopsy of the mass via an endoscopic trans-sinus approach, only rarely discussed previously in the literature. The Pathology results obtained from the muscle showed atrophic and fibrotic muscle with mild chronic inflammatory infiltrate, compatible with the diagnosis of inflammatory process. The patient was started with oral prednisone for idiopathic orbital inflammation.
Keywords: Biopsy, Inferior rectus muscle, Trans-sinus
Introduction
Minimally invasive endonasal techniques to approach the posterior orbit have been previously described [1-4], but only rarely [2] as an approach to biopsy the inferior rectus muscle.
We describe a case of a 68 year-old female presenting with a posterior left inferior rectus muscle mass. The patient underwent biopsy of the mass via an endoscopic trans-sinus approach-only rarely discussed previously in the literature [1]. Collection and evaluation of protected patient health information was HIPAA-compliant.
Case Report
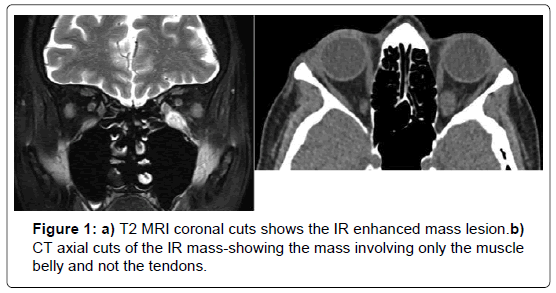
A 68-year-old year old female with a history of controlled hypothyroidism, dyslipidemia and osteoarthritis presented for evaluation of painless binocular vertical diplopia of 6 weeks duration. On examination BCVA was 20/25 OD and 20/30 OS. Anterior and posterior segment examination was normal. Left hypotropia with supraduction limitation was noted. Laboratory tests and contrastenhanced MRI of the orbits were obtained. The tests showed inflammatory markers in the normal range (ESR and CRP) and negative acetylcholine receptor antibodies. Contrast-enhanced MRI of the orbits showed isolated enlargement of the left inferior rectus muscle with the appearance of an intrinsic mass lesion within the muscle, sparing the muscle insertion (Figures 1a and b). Suspecting a systemic process, CT chest/abdomen/pelvis was subsequently ordered to look for primary disease. These tests revealed hepatosplenomegaly.
Flow cytometry of the peripheral blood was consistent with marginal zone lymphoma. Bone marrow biopsy was also consistent with marginal zone lymphoma. A repeat MRI preformed 1 month later showed stability of the inferior rectus muscle mass. For diagnostic purposes, the patient underwent biopsy of the inferior rectus mass via an endoscopic trans-sinus approach. The Procedure was performed under general anesthesia (Video 1).
Procedure
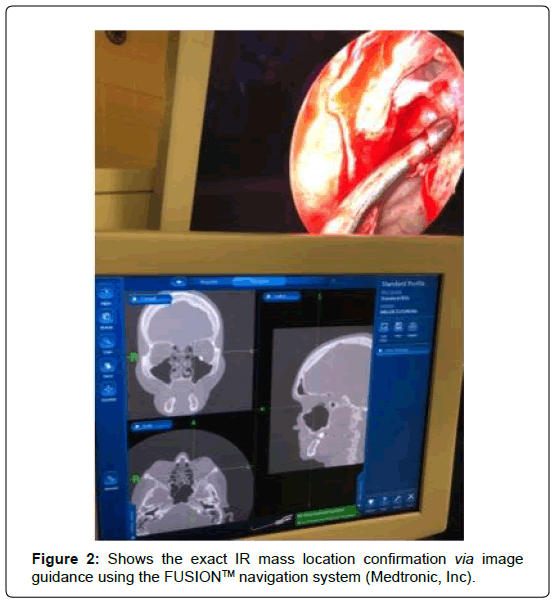
Endoscopic sinus surgery was performed-The orbital floor and medial strut were identified visually and with anatomic guidance, using the FUSION™ navigation system (Medtronic, Inc.) The medial strut was bured and removed exposing the orbital periosteum. The identification of the inferior rectus muscle was carried after the orbital periosteum was opened with a ball seeker and forced duction testing was performed on the left inferior rectus. Once identified image guidance was used to confirm the location of the inferior rectus mass at the posterior orbit (Figure 2).
Biopsies of the muscle were obtained and sent for pathologic correlation (frozen section revealed muscular tissue with lymphoid infiltrate). Hemostasis was obtained with thrombin soaked neurosurgical cottonoids.
The procedure time was recorded to be 70 minutes in total, which included approximately 20 minutes for processing and review of the frozen section specimen.
The Pathology results obtained from the inferior rectus muscle showed atrophic and fibrotic muscle with mild chronic inflammatory infiltrate. Immunostaining demonstrated a mixture of CD20+ B cells and CD3+ T cells, compatible with the diagnosis of inflammatory process.
The patient was started with oral prednisone for idiopathic orbital inflammation.
Discussion and Conclusion
Herein we report the use of the endonasal endoscopic approach for biopsy of the inferior rectus muscle. The endoscopic trans-sinus approach was previously reported as an approach to the lateral and posterior orbit [1-4]. It is direct and efficient, with a total operative time of 70 minutes in our case. The use of image guidance afforded the surgeons the opportunity to accurately biopsy the mass. Other techniques were considered, and included a direct EOM approach with disinsertion of the inferior rectus [4-6], although the mass was felt to be too far posterior to allow reasonable access. An orbital floor approach [6] was also contemplated, and while possible, the space within the posterior orbit was expected to be quite tight and there was concern for the inability to navigate the small space and obtain an adequate biopsy. Last, a modified Caldwell-Luc procedure [7] could be performed, but would create a more invasive option, with likely longer healing and longer operative times.
References
- Dziedzic TA, Anand VK, Schwartz TH (2015) Endoscopic endonasal approach to the lateral orbital apex: case report. J Neurosurg Pediatr 16: 305-308.
- Curragh DS, Halliday L, Selva D (2018) Endonasal approach to orbital pathology. Ophthalmic Plast Reconstr Surg 34: 422-427.
- Miller NR, Agrawal N, Sciubba JJ (2008) Image-guided transnasal endoscopic resection of an orbital solitary fibrous tumor. Ophthal Plast Reconstr Surg 24: 65-67.
- Shafi F, Zaidi S, Mehta P, Ahluwalia HS, Ahmed SK (2016) Endoscopic medial rectus sling: A window into the intraconal orbital apex. Ophthalmic Plast Reconstr Surg 32: 233-236.
- Kralik SF, Kersten R, Glastonbury CM (2012) Evaluation of orbital disorders and cranial nerve innervation of the extra ocular muscles. Magn Reson Imaging Clin N Am 20: 413-434.
- Eade EL, Hardy TG, McKelvie PA, McNab AA (2018) Review of extraocular muscle biopsies and utility of biopsy in extraocular muscle enlargement. Bjophthalmol 19.
- Park MW, Kim SM, Amponsah EK, Lee SK (2015) Simple repair of a blow-out fracture by the modified caldwell-luc approach. J Craniofac Surg 26: e306-307.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi