Research Article, J Pulm Med Vol: 5 Issue: 2
Foreign Body in Craniofacial Orifices in Children: Query Parental Indictment
1Department of ENT, University of Port Harcourt Teaching Hospital, Rivers State, Nigeria
2Department of ENT, Chukwuemeka Odumegwu Ojukwu Teaching Hospital, Anambra state, Nigeria
*Corresponding Author: Osuji AE Department of ENT, University of Port Harcourt Teaching Hospital, Rivers State, Nigeria Tel: +2348030849107 E-mail: osujiliz@yahoo.com
Received Date: 09 June, 202; Accepted Date: 23 June, 2021; Published Date: 30 June, 2021
Citation: Osuji AE, Nwankwo BE (2021) Foreign Body in Craniofacial Orifices in Children: Query Parental Indictment, J Pulm Med 5:2
Abstract
Introduction: The increasing economic and pecuniary pressure on families incurred by contemporary lifestyle in a continuously evolving world has led parents especially mothers to engage in jobs that are very time mortgaging. This leads to reduced supervision of growing children among several families. Concurrently, the prevalence of foreign body in craniofacial orifices in children is on the increase, without any audacious attempt to decode the raison d'être. Besides, early childhood explorative tendencies of putting objects in their craniofacial orifices further predispose children to foreign body aspiration and ingestion. This study highlights some circumstances about the lodging of foreign body in the craniofacial orifice in children seen in our hospital, to ascertain the dynamics of a parental factor in children putting objects in their craniofacial orifices.
Keywords: Foreign Body
Abstract
Introduction: The increasing economic and pecuniary pressure on families incurred by contemporary lifestyle in a continuously evolving world has led parents especially mothers to engage in jobs that are very time mortgaging. This leads to reduced supervision of growing children among several families. Concurrently, the prevalence of foreign body in craniofacial orifices in children is on the increase, without any audacious attempt to decode the raison d'être. Besides, early childhood explorative tendencies of putting objects in their craniofacial orifices further predispose children to foreign body aspiration and ingestion. This study highlights some circumstances about the lodging of foreign body in the craniofacial orifice in children seen in our hospital, to ascertain the dynamics of parental factor in children putting objects in their craniofacial orifices.
Patients and methods: The study was carried out in the University of Port Harcourt Teaching hospital (UPTH), Rivers State, Nigeria, among patients who presented to the Ear, Nose and Throat Clinic of UPTH with foreign body in the Ear, Nose or Throat, from July 2018 to June 2019. The data collected were age and sex of the children, occupation of parents, and the social history of some patients. The data was presented in simple tables and figures.
Results: This was a retrospective analysis of the 57 cases of foreign body in the craniofacial orifices (Ear, Nose and Throat) seen in the Ear, Nose and Throat (ENT) clinic of the University of Port Harcourt Teaching Hospital, Rivers State, Nigeria. Among these 57 cases were 36 males and 21 females. 8(14%) were adults, while 49(86%) of the patients were of paediatric age, with their age ranging from 1-14 years. 29 (59.2%) of the paediatric patients were less than 5 years. Among this paediatric population analysed, the age category of 3-4 years had the highest number of foreign bodies in the craniofacial orifices in 15 subjects (30.6%), followed by 1-2 years age category with foreign body in 14 (28.6%) subjects. The age category of 5-6 followed with foreign bodies. The ear was the orifice with the highest number of foreign bodies in 11 (22.4%) subject, 35 (61.4%) in the general population, and also in the paediatric population with 27 (55.1%) objects retrieved from the ear.
Conclusion: Foreign body ingestion and aspiration are common among children under 5 years, its possibility is further enhanced when mothers or primary caregivers are encumbered with other responsibilities that limit their active supervision of these children. Therefore, an increase in the level of societal awareness and parental sensitization as regards the prevention and likely complications of foreign body ingestion and aspiration, coupled with adequate counselling of by clinicians will help to reduce the prevalence of foreign body in the craniofacial orifices in children.
Keywords
Foreign body; Aspiration; Ingestion; Port harcourt; Children; craniofacial orifice.
Introduction
With the increasing economic and pecuniary pressure on families incurred by contemporary lifestyle in a continuously evolving world, parents especially mothers have increasingly engaged in jobs that are time mortgaging. This leads to reduced supervision of growing children among several families. At the same time, the prevalence of foreign body in craniofacial orifices in children is on the increase, without any audacious attempt to decode the raison d'être. Foreign body in craniofacial orifices are relatively common in children less than 5 years [1] and it has been attributed to the immature swallowing and protective reflexes in this age group [2]. This is in addition to early childhood explorative tendencies of putting objects in their craniofacial orifices which further predisposes them to foreign body aspiration or ingestion [3].
The craniofacial orifices refer to the physiological openings in the human head through which access is gained into the body’s digestive tract, airway, or ear cavity. Foreign body ingestion occurs when a non-edible substance gains entrance through the mouth and is lodged at the base of the tongue, vallecula, hypopharynx, oesophagus, or any other part of the digestive tract [1]. Most foreign bodies in the digestive tract are expelled spontaneously without complications, but, some cases may require surgical or endoscopic removal in some children, with a possibility of complications [1]. On the other hand, foreign body aspiration occurs when an edible or non-edible substance, gains entrance through the mouth or the nose, to become lodged in the laryngopharynx, larynx, trachea, bronchi, or any other part of the airway [4]. Foreign body aspiration has been identified as a major cause of morbidity and mortality in children and accounts for up to 7% of pre-hospital deaths in children aged 0-5 years [2].
This study highlights some of the factors relating tolodging of foreign body in the craniofacial orifice in children seen in our hospital, to ascertain the dynamics of parental factor in children putting objects in their craniofacial orifices. It also tries to highlight the need for counselling of parents or guardians in the prevention and management of foreign body ingestion and aspiration in children.
Patients and Methods
The study was carried out in the University of Port Harcourt Teaching Hospital (UPTH), Rivers State, Nigeria. The patients who presented to the Ear, Nose and Throat Clinic of UPTH with foreign body in their ear, nose or throat from January 2018 to June 2019 were collated. After due permission was obtained, their medical records were retrieved from the hospital medical records department. The data collected were age and sex of the children, occupation of parents, and location of occurrence of foreign body insertion. The adult subjects were excluded from the analysis in this study, to focus on findings from paediatric cases (Figures 1-4).
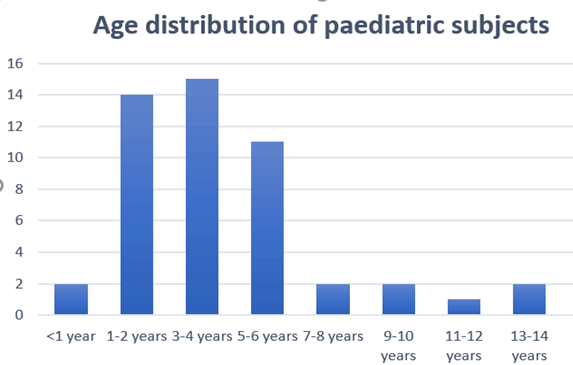
Figure 1: Age distribution of paediatric subjects
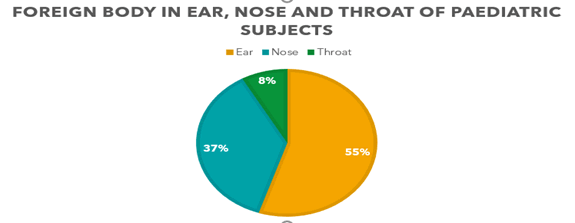
Figure 2: Distribution of foreign bodies in the craniofacial orifices of paediatric subjects.
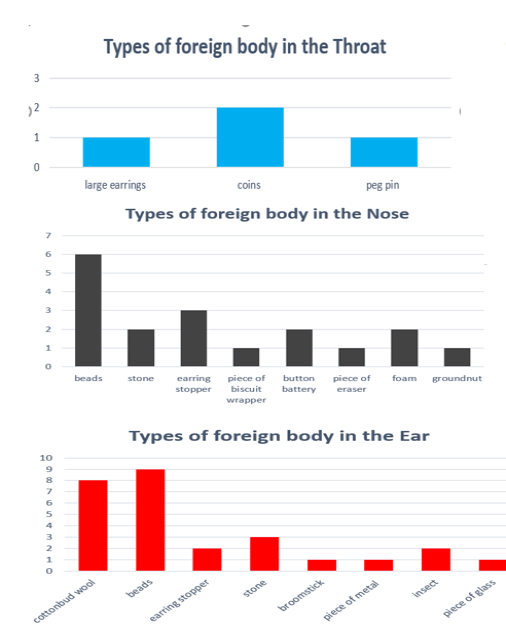
Figure 3: types of foreign bodies in the Ear, Nose and Throat of all study subjects
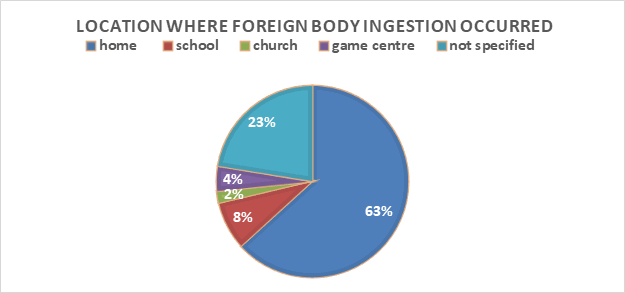
Figure 4: location where foreign body ingestion incident in the paediatric subjects occurred
Results
This was a retrospective analysis of the 57 cases of foreign body in the ear, nose and throat seen in the Ear, Nose and Throat (ENT) clinic of the University of Port Harcourt Teaching Hospital within a 12 month period from July 2018 to June 2019. Among these 57 cases were 36 males and 21 females. 8(14%) were adults, while 49(86%) of the patients were of paediatric age, with their age ranging from 1-14 years. 29 (59.2%) of the paediatric patients were less than 5 years. In subjects older than 18 years, cotton wool was the commonest type of foreign body, and ear was the commonest site of foreign body lodgement. The ear was the orifice with the highest number of foreign bodies in 35 (61.4%) subjects. Out of the 35 subjects, 27 (55.1%) were of the paediatric population. After noting types of the foreign body seen in the general study population, further analysis of data was focused on the 49 paediatric subjects (Table 1). Among this paediatric population analysed, the age group of 3-4 years had the highest number of subjects, 15 (30.6%) with a foreign body in the craniofacial orifices, followed by 1-2 years age group,14 (28.6%), and then the 5-6 age group followed, with 11 (22.4%) subjects with foreign bodies. There was no record of a subject within the age of 15-18 years that had a foreign body in this study. Among the fathers of the 49 children in this study, 2 fathers are unemployed, while among the mothers, 5 are housewives.
Table 1: The occupation of paediatric subject/tsâ?? parents.
Discussion
Foreign body in craniofacial orifices in children is a re-occurring decimal especially in the Paediatric Ear, Nose and Throat clinic, and contributes a significant percentage of ENT emergencies in the pediatric population [4]. Any attempt to understand factors that could inadvertently be contributing to the incidence can facilitate action in the right direction to curb the occurrence of foreign body ingestion and aspiration. This study has attempted to x-ray numerous factors in line with the patients, their parents or guardians, their environments where foreign body ingestion occurred, the objects ingested or aspirated, and the craniofacial orifice involved.
This study shows a male preponderance in the incidence of foreign body aspiration. This has been attributed to the increased adventurous nature of male children, and this was a similar finding by Ankur et al in India [3]. In this study, children aged 1-6 years had the highest incidence of foreign body in craniofacial orifices. Rishi et al in 2017 noted a similar finding, however, their study showed a greater preponderance in children less than 5 years. They opined that this is the age of exploration in children, thus the greater incidence of foreign body in craniofacial orifices in this age group [5].
The Ear was the commonest site of foreign body lodgment in our study, followed by the nose; however, this was mostly in the older paediatric population of 9-14 years, where cotton wool from cotton buds was the single most common foreign body in the ear. In the younger paediatric population of fewer than 9 years, there were different objects noted as aural foreign bodies, especially in the age group of 1-6 years among whom bead was the commonest foreign body in the ear. This finding was similar to the study by Said et al in 2013 [6]. However, this is contrary to the study by Rishi et al, and Ankur et al, where the nose was the commonest site of foreign body lodgment. Objects lodged as foreign bodies in the craniofacial orifices, have been reported to either be self-inflicted by the patient or perpetrated by other children [7]. Selfinflicted foreign bodies in ear and nose are common in children with Attention Deficit Hyperactivity Disorders (ADHD) [7].
Coins were the commonest object found in the throat in this study, Similar to reports from some previous studies [5,8]. This may be because the size of the coin is relatively larger than other craniofacial orifices, thus cannot be accommodated in the nose or ear, when compared to the throat. Beads were the commonest object found in the ear and nose. This shows that these ornaments of beautification in some cases end up in child’s orifices. This could mean that parents or guardian use of ornament around children may be liable for increased predisposition to the ingestion or aspiration of these ornaments by their children. As much as beads, earrings, and such ornaments may implicate the mother or female guardian, in recent times these ornaments are no longer restricted to females. The presence of these ornaments constitutes increased risk of foreign body aspiration if not safely handled around children, and the parents ought to be sensitive to this possibility [9].
Considering the location where the foreign body ingestion incident occurred, the home had the highest occurrence of FB in the craniofacial orifice of children. It may not be surprising that the home which should be a haven for these children posed an increased risk of foreign body aspiration and ingestion because it depends on the availability of objects, and absence of watchful parents or caregivers [9]. In the event of this, it can be presumed that the guardian or parents of these children should take responsibility to ensure safety and prevent foreign body aspiration or ingestion. However, the extent to which this safety can be achieved depends on the attentiveness of the parents or guardian to this responsibility of safeguarding the children, rather than just being physically present around the children. Also, the level of awareness of the parents to the risk and effect of foreign body aspiration in children has been deemed highly necessary [10]. This awareness of safety seems to be more appreciable in parents with good literacy level than in parents with a low level of literacy, but at the same time, safeguarding children against foreign body ingestion and aspiration cannot be achieved without the presence of a guardian or parent [9]. Game centres/Play zones were particularly associated with a high risk of coin ingestion and button battery aspiration in this study. This calls for increased awareness of parents who take children to such fun places. Irrespective of the location of foreign body ingestion occurrence, this study noted a high incidence in children whose parents have a relatively low level of literacy [3,8,10].
Connelly R. et al, 2016 classified Socio economic class using occupation according to National Statistics Socio Economic Classification (NS-SEC) and stated that “Occupation is the most powerful single indicator of the level of material reward, social standing and life chances” [11]. This study noted that the incidence of foreign body in craniofacial orifices in children cuts across Socio economic class of parents, like the report by other researchers [3,4,10]. Besides, both parents working increased incidence more than one parent working. In this study, the subjects’ parents had different occupations, showing that foreign body aspiration or ingestion in children is not limited to subjects whose parents are in a particular line of occupation. Ankur M. et al, in 2011 reported a higher incidence with low socioeconomic class and a higher incidence in the urban area [3]. This study similarly noted a higher incidence with low socio economic class but could not ascertain the difference in incidence among rural and urban area because it was carried out in an urban setting. The incidence in children with high socio economic class parents could be attributed to the long absence of parents from children probably due to job demands, which necessitates the employment of low socio economic class individuals to care for children. Whereas high incidence in low socio economic class can be attributed to a low level of literacy, which often predominates in the low socio economic class among the society. Consequently, parental low level of literacy has been implicated as a major underlying factor in the predisposition of children to a foreign body in craniofacial orifices. In line with this finding, a higher incidence has been noted in children whose mothers are housewives, and a high incidence in children whose parents have a low level of literacy [3,6].
Provision of a safe environment and safe practices coupled with the vigilance of primary caregivers around children can be said to be the common denominator in curbing the incidence of foreign body in craniofacial orifices in children. Parental ability to take responsibility for the safety of children should be pre-eminent irrespective of parents’ socio economic class, or child’s location at home, or in another environment. The need for parental education in this subject matter cannot be overemphasized. Beyond the removal of foreign body, clinicians should emphasize on educating parents on their pivotal role in curbing foreign body lodgment in children's ear, nose and throat, thereby stemming the tide of blaming it on the children. As much as foreign body ingestion and aspiration is common among children under 5 years, the possibility of it occurring is further enhanced if primary caregivers are unaware or are encumbered with responsibilities that limit their active supervision of the children.
Conclusion
Foreign body ingestion and aspiration is common among children under 5 years, but its likelihood is heightened when parents or guardians are laden with other responsibilities that limit their active supervision of their children. Therefore, an increase in the level of societal awareness and parental sensitization as regards the prevention and likely complications of foreign body ingestion and aspiration, coupled with adequate counseling of by clinicians will help to reduce the incidence of foreign body ingestion and foreign body aspiration in children.
References
- Lee JH (2018) Foreign body ingestion in children. Clin Endosc 2(51):129-136.
- Zaupa P, Saxena AK, Barounig A, Höllwarth ME (2009) Management strategies in foreign-body aspiration. Ind J Pediat 76:157-161.
- Ankur M, Dibakar H, Sirshak D, Mainak D, Jayanta S, et al. (2011). Ear, Nose and Throat foreign bodies in children: A search for socio-demographic correlates. Int j paediat otorhinolaryng 75(4):510-512
- Afolabi O, Alabi B, Segun-busari S, Dunmade A, Ologe F (2009) Paediatric aural foreign bodies: A challenge to caregivers, Int J Otorhinolar 11(1).
- Rishi B, Manita P, Ramesh P (2017) Types of foreign body in ear, Nose and Throat in Western Part of Nepal. Glob J Otolaryngol 4(3):555640
- Said M, Wahid F, Kamran M (2013) Ear, nose and throat foreign bodies: An analysis of 150 cases. P J M H S 7(4).
- Perera H, Fernando S, Yasawardena A, Karunaratne I (2009) Prevalence of attention deficit hyperactivity disorder (ADHD) in children presenting with self-inserted nasal and aural foreign bodies. Int J Paediatr Otorhinolaryngol 7(10):1362â??1364.
- Heim SW, Maughan KL (2007) Foreign bodies in the ear, Nose, and Throat. American Family Physician.
- OA Afolabi, AG Salaudeen, BS Alabi, AO Lasisi (2010) Correlation of aural foreign bodies with handedness: An observational study in a Nigerian tertiary hospital J Clin Med Res 2(5):79â??82.
- Ologe FE, Dunmade AD, Afolabi OA (2007) Aural foreign body in children. Ind J Pediatr 74:755â??758
- Connelly R, Gayle V, Lambert PS (2016) A review of occupation based social classifications for social survey research. Methodolog Innovat 9(1).
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi 