Research Article, Int J Ophthalmic Pathol Vol: 7 Issue: 3
Frontalis Sling Surgery Using DCR Silicon Stents for Correction of Ptosis with Poor Levator Action: Single-Centre Experience from Saudi Arabia
Al-Wadaani FA*
Department of Ophthalmology, College of Medicine, King Faisal University, Al Ahsa, Eastern Province-Saudi Arabia
*Corresponding Author : Fahd A Al-Wadaani
Department of Ophthalmology, College of Medicine, King Faisal University, Al Ahsa, Eastern Province-Saudi Arabia
Tel: +009655939366
E-mail: dr_wadani@yahoo.com
Received: September 09, 2018 Accepted: September 29, 2018 Published: October 05, 2018
Citation: Al-Wadaani FA (2018) Frontalis Sling Surgery Using DCR Silicon Stents for Correction of Ptosis with Poor Levator Action: Single-Centre Experience from Saudi Arabia. Int J Ophthalmic Pathol 7:3. doi: 10.4172/2324-8599.1000224
Abstract
Background: When levator function is poor or absent, frontalis sling is one of the preferred methods of treatment of ptosis. Various materials have been used for frontalis slings with varying results.
Aim: To find an effective, easily available and, lasting frontalis sling material with minimal complications.
Materials and Methods: Retrospective study in which DCR Silicone stents were used for brow suspension in cases of ptosis with poor Levator action (less than 5 mm) in the form of a single rhomboid like in FOX method with slight modification, done between 2012 to 2016.
Results: Retrospectively all the records of these patients were retrieved and the surgical results studied and analyzed. Mean follow up period was 2.6 years. Good long term functional results (assessed in terms of eyelid height, skin crease depth, eyelid contour and patient satisfaction) were achieved in 33 eyelids [90%].Under correction was noticed in 3 eyelids [8%]. Re-surgery was done for these patients and all of them improved well. Lagophthalmos and mild corneal exposure were noticed in 6 eyelids which improved after the use of artificial tear eye drops and ointments.
Conclusion: This method proved to be a simple, less expensive and effective method with minimal complications.
Keywords: Frontalis Sling Surgery; Ptosis; Ophthalmoplegia; Saudi Arabia
Introduction
Ptosis is an abnormal drooping of upper eyelid in relation to globe [1]. The normal position of the upper lid is between the superior limbus and upper pupillary margin [2] (covering about 1-2 mm of upper cornea). Ptosis may be congenital or acquired. Congenital ptosis is usually unilateral (70%-75% of ptosis) and is non-hereditary. Rarely congenital ptosis may be due to sympathetic paralysis (Congenital Horner’s syndrome) [3]. Acquired ptosis is divided into four main types and these are neurogenic, Apo neurotic, mechanical and myogenic. Ptosis, when present, always produces a cosmetic problem. In children it may be associated with astigmatism and can result in deprivation amblyopia in cases where it covers the pupil. Treatment is surgical correction. There are various surgical procedures to correct ptosis. In children surgery should be performed when accurate evaluation can be done and the child is able to cooperate postoperatively. However, when there is danger of amblyopia or chin elevation with resultant torticollis, it should be performed as early as possible. Primary goal of the surgery is elevation of the lid and maintenance of symmetry. The best results are obtained when the surgeon is able to balance the lids in primary position [2]. Levator function is the pivotal factor in planning surgery for ptosis. When levator function is poor or absent, frontalis sling is one of the preferred methods [4]. Various materials have been used for frontalis sling. Smith and Cherubini used 4/0 silk. Frieden Wald, et al. used a similar material but the technique was slightly different. Crawford has described the use of autologous fascia lata (AFL) which continues to be the gold standard for sling surgery [4,5]. Some surgeons prefer nonautologous material because surgery can be done under local anesthesia in adult patients and a second incision (in leg) can be avoided. It is also preferred when AFL is not available (as in very young children with short legs). The other materials used are skin, silicone band, Silicone rods etc. [5-8].
Methods
The study was carried out between 2012 to 2016 and a single surgeon was involved in carrying out all the surgeries. Approval from the ethics committee of the hospital was obtained prior to the procedure. A total of 27 patients (37 eyes) with moderate to severe ptosis were included in the study. All patients had poor (4 mm or less) levator action. Two patients (both more than 50 yrs old) were having chronic progressive external ophthalmoplegia (CPEO) with bilateral ptosis. The rest were all of congenital type. 2 patients, aged less than 4 years with severe congenital ptosis, one had bilateral ptosis with chin elevation and the other with upper lid severe ptosis were also included. All other patients were between 8 to 30 years of age. Most of the congenital cases were done under general anesthesia barring few who cooperated to be operated under local anesthesia. Both adult cases with CPEO were operated under local anesthesia. In this study, DCR (dacryocystorhinostomy) stents were used for frontalis suspension, which has the advantage of being easily available and at the same time being a relatively non-degradable and less reactive, was expected to have good long term functional benefits.
Fox pentagon procedure with modification was used in all cases. Instead of two direct stab incisions over the lid, we made a superficial transverse incision, including in it skin and superficial fibers of orbicularis muscle at about 4 mm from lid margin and then within this incision two stab 2 mm cuts, corresponding to medial and lateral limbus, were made to the depth of tarsus. Two bone depth incisions along the upper border of eye brows were made, each about one cm from the lateral and medial brow margins. Finally a one cm bone depth incision was made on the forehead, about one and a half cm from the mid-point of an imaginary line joining the two eye brow incisions. The tube was then hooked or tied to a 3-0 silk suture attached to a 26 mm cutting needle. The needle was first passed from the forehead incision to the lateral brow incision and with little traction; the silicon tube would follow it. The needle was then passed deep to include the orbital septum and then to exit at lateral limbal level incision in the lid incision. From here the needle and thus thereby the tube was made to pass under the orbicularis (at tarsus depth) to exit next in the medial deep cut (corresponding to the medial limbus) on the lid incision. From here, the needle and thereby the silicon tube was passed up deep to orbital septum to come out at medial eyebrow incision. Finally it was made to exit at the forehead incision where it meets the other end. The two ends are pulled to attain a lid height corresponding to the upper limbus (with expected fall of 1 mm or more postoperatively in sitting or standing position). Then the two ends were tied together making five to six knots together which was then buried deep through a pocket under the frontalis muscle. This pocket over the knot was sutured with 6-0 vicryl. Forehead wound was closed with non-absorbable interrupted sutures and the horizontal lid incision closed with 6-0 continuous silk sutures. Brow incisions were not sutured. Finally frost suture was applied to lower lid and the eye patched for 24 hrs. Patient was put on systemic broad spectrum antibiotic and an analgesic for 7 days post operatively. Frost suture was removed next day and patient was put on frequent artificial tear eye drops during the day and ointment during night. Lid and forehead sutures were removed on 5th day. Patient was followed at one month, 3 months and then 6 monthly for an average of two to two and a half years.
Results
The records of all these patients were retrieved and studied. The patients were followed for one to four years with a mean follow up period of 2 and half years. Among 27 patients (37 eyes) included in the study, 10 were females and the rest were males, although it does not depict the true gender distribution of the disorder because only the cases with poor levator action with good Bell's phenomenon were enrolled for this surgery. Ages of our patients ranged from 2 years to 62 years. The youngest patient in our study was a 2 year old child with moderate to severe degree of bilateral congenital ptosis with chin elevation. The next youngest was approximately 3 and a half years old with unilateral severe ptosis (pupil covered). Both were subjected to temporary sling surgery using same material to avoid ocular torticollis and deprivation amblyopia (Table 1).
| Age in years | No. of patients | Unilateral | Bilateral | Total no. of eyes involved |
|---|---|---|---|---|
| 0 - 4 | 02 | 01 | 01 | 03 |
| 5 - 10 | 09 | 06 | 03 | 12 |
| 11 - 20 | 11 | 07 | 04 | 15 |
| 21 - 30 | 03 | 03 | 00 | 03 |
| 31 - 50 | 00 | - | - | - |
| 51 - 60 | 02 | 00 | 02 | 04 |
Table 1: Age and Laterality.
Most of the patients in our series were in the age group of five to twenty years. Also, most of the cases were unilateral. This does not depict the actual laterality of the disorder, since only those patients enrolled for this surgery that had (1) moderate to severe degree of ptosis, (2) poor LPS function but with good preserved Bell's phenomenon. Two patients were more than 50 years of age, both being males and had chronic progressive external ophthalmoplegia (CPEO). On each follow up visit, patients were assessed to evaluate the functional results and also to look for any complications associated with the surgery. Good functional results were assessed in terms of eyelid height (MRD I), skin crease depth, eyelid contour and patient satisfaction. Marginal reflex distance more than 3 mm in postoperative patients, a good skin crease and a satisfied patient were each taken as a good result respectively during each follow up visit (Table 2).
| Complications | No. of cases | Percentage |
|---|---|---|
| Lagophthalmos with mild Corneal exposure | 06 | 16% |
| Wound infection | 03 | 8% |
| Granuloma formation | 01 | 3% |
Table 2: Complications.
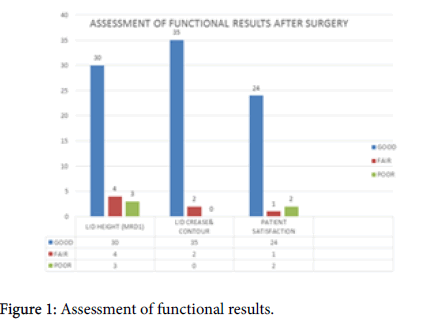
Good long term functional results were achieved in most of the cases. In roughly 80 to 90% of cases, adequate eyelid height, skin crease depth and proper eyelid contour were achieved. The overall patient satisfaction was also very good. In 3 of the cases where adequate lid height was not obtained in the first surgery, re-surgery was done and all showed satisfactory improvement (Figure 1). In 6 cases (eyes) there was mild to moderate lagophthalmos with mild corneal exposure, which was managed conservatively. Wound infection was found in 3 cases in our series, which was mild and was treated by systemic and topical antibiotics. One patient developed granuloma over the forehead wound, which was excised.
Discussion
Ocular In cases of poor LPS action, accessory elevators have always been used for elevating the lids 8. Frontalis sling surgery is the most commonly performed surgery for this group [9]. Although none of the surgical procedures gives perfect results, it helps to alleviate the severity of the condition [10]. AFL is the best material for frontalis suspension. It is non-degradable and allows fibrovascular in-growth leading to bio-integration without significant inflammation [11-14]. AFL has good long term functional results with maintenance of lid height and well-formed skin crease. There are only occasional reports of post-operative wound infection. El-Toukhy et al. using AFL showed one wound infection out of 34 eyelids [3%]. The Wasserman et al. showed 2 infections out of 24 eyelids [8%] [15]. Deenstra et al. demonstrated 12 cases of exposure keratopathy with no wound infection out of 119 eyelids [16]. Contrary to this, use of preserved fascia lata has a recurrence rate of 50% after 8-9 years of surgery 8. Different non autologous materials have also been used, including - silicone rod, monofilament nylon, polypropylene, polyester and expanded polytetrafluroethyleneCarter et al. using silicon rod showed 3 cases of extrusion and, 4 cases of recurrences out of 61 eyelids [11%]. Wasserman, et al. using nylon showed 9 cases of recurrences and one infection out of 13 eyelids [16-18].
In our study of 37 eyes, good lid height was achieved in 81% and in other 11% cases fair lid height was achieved (this included the two cases of elderly patients with CPEO, where only fair lid height was aimed at during surgery to avoid post-operative exposure keratopathy because of associated elevation deficit). Good lid crease and contour with satisfactory cosmesis was attained in more than 94% of cases, which is much better compared to previous studies, probably in part due to the horizontal incision given across the lid. On the whole, good functional results were achieved in 90% of cases which almost matches AFL (autogenous fascia lata) sling (92%).
Silicone stent being relatively non-biodegradable, not much inflammatory reaction is seen since there is better bio-integration with the tissues. In our study, we had only 6 cases with mild corneal exposure keratopathy in the immediate post-operative period due to early lagophthalmos which improved with topical tear drops and ointment. The lagophthalmos, improved within 6 – 8 weeks, with meticulous use of artificial tear drops during the day and ointment at night (with eye patching during night as per need, for initial one or two weeks) during this time. Wound infection which has been reported in many studies with the use of various synthetic materials was seen in only 3 cases in the forehead wound in our series. It did not seem to have any relation with the sling material, as it was superficial (probably related to external stitches) which improved within few days with local antiseptics and systemic antibiotics.
Conclusion
Silicone DCR stents tube is good alternative to AFL as a frontalis sling material as its functional results (90%) almost match that of AFL. In addition it has lesser complications compared to many other synthetic sling materials available. Compared to AFL, it has the advantage of avoiding second incision in the leg and can be done under local anesthesia.
References
- Kanski JJ (2007) Clinical ophthalmology. (3rd edtn) Buterworth – Heimemann, London.
- Vaughan D, Asbury T (1992) General Ophthalmology. (13th edtn) Prentic Hall International Inc. USA.
- Albert DM, Jakobiec FA (2014) Principles and Practice of Ophthalmology. (1st edtn) WB Saunders Company.Philadelphia – Lodone.
- Putter AM (1984) Basic Oculoplastic Surgery. In: Peyman GA, Sanslers DR, Goldbag MF. Principles and Practice of Ophthalmology. 1st Indian ed. WB Saunders Company, Philadelphia.
- Concad B, Harry KJ (1961) An Atlas of Ophthalmic Surgery. (1st edtn) JB Lippincott Company, Philadelphia.
- Miller Stephen JH (1990) Parsons Disease of the Eye. (16th edtn) Churchill Livingstone. London.
- Ahn J, Kim NJ, Choung HK, Hwang SW, Sung M, et al. (2008) Frontalis sling operation using silicone rod for the correction of ptosis in chronic progressive external ophthalmoplegia. Br J Ophthalmol 92: 1685-1688.
- Gonnering RS (1994) Basic and Clinical Science Course. Am Acad Ophthalmol 95: 127-189.
- Mehmood H (2001) Levator Resection. A Feasible Option in Congenital Ptosis with Poor Levator Function. Paki J Ophthal 17: 3-5.
- Malik HM (1995) Correction Of Congenital Ptosis Using Silicone Material for Frontalis Suspension. Paki J Ophthal 11: 115-117.
- Gonnering RS (1994) Calnil Kenneth Nerad Jeffery A. Basic and Clinical Science Course. Am Acad Ophthalmol 95: 127-189.
- Mustarde JC (1980) Repair and Reconstruction in the Orbital Region. (2nd edtn) Edinburgh; Churchill Livingstone.
- Mehta P, Patel P, Olver JM (2004) Functional results and complications of Mersilene mesh use for frontalis suspension ptosis surgery. Br J Ophthalmol 88: 361-364.
- Beard C. Ptosis. (3rd edtn) St Louis, CV Mosby.
- El-Toukhy E, Salaem M, El-Shewy T, Abou-Steit M, Levine M (2001) Mersilene mesh sling as an alternative to autogenous fascia lata in the management of ptosis. Eye (Lond) 15: 178-182.
- Wasserman BN, Sprunger DT, Helveston EM (2001) Comparison of materials used in frontalis suspension. Arch Ophthalmol 119: 687-691.
- Manners RM, Tyers AG, Morris RJ (1994) The use of Prolene as a temporary suspensory material for brow suspension in young children. Eye (Lond) 8: 346-348.
- Esmaeli B, Chung H, Pashby RC (1998) Long-term results of frontalis suspension using irradiated, banked fascia lata. Ophthal Plast Reconstr Surg 14: 159-163.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi