Case Report, J Clin Image Case Rep Vol: 1 Issue: 1
Hidden Hypopharyngeal Primary of HPV Associated Lymphoepithelial-Like Carcinoma Presenting with Lymph Node Metastasis
Olivier T Giger1 and Patrick Dubach2*
1Department of Pathology, University of Cambridge, Addenbrooke’s NHS Trust Hospital Cambridge, Switzerland
2Head of the Department of Otorhinolaryngology, Head Neck Surgery, Burgerspital Solothurn Schöngrünstrasse, Switzerland
*Corresponding Author : Patrick Dubach, MD
Head of Department of Otorhinolaryngology, Head and Neck Surgery, Burgerspital Solothurn, Schöngrünstrasse 42, 4500 Solothurn, Switzerland
Tel: 0041326273546
Fax: 0041326273444
E-mail: Patrick.dubach@spital.so.ch
Received: June 29, 2017 Accepted: July 10, 2017 Published: July 17, 2017
Citation: Giger OT, Dubach P (2017) Hidden Hypopharyngeal Primary of HPV Associated Lymphoepithelioma-Like Carcinoma Presenting with Lymph Node Metastasis. J Clin Image Case Rep 1:1.
Abstract
Background: Lymphoepithelial-like carcinoma of the pharynx is a recently described sub-entity of HPV-associated pharyngeal squamous cell carcinoma. This histological entity might become an important differential diagnosis of cervical lymph node metastasis to its well known EBV-associated epipharyngeal counterpart.
Methods and results: We report on a patient presenting with a cervical cystic mass. Clinical findings and fine needle aspiration cytology was compatible with a second branchial arch cyst. Consecutive excision showed a lymph node with poorly differentiated lymphoepithelial-like squamous cell carcinoma, suggestive for a metastasis of an oropharyngeal primary. The patient underwent pandendoscopy with suspected primary in the epi- or oropharynx as suggested by the molecular characteristics of the tumor. The primary tumor was finally identified as a HPV 16 associated lymphoepitheliallike carcinoma in the tongue base and vallecula.
Conclusion: The final diagnosis of a HPV16-associated lymphoepithelial-like carcinoma has recently gained interest in the literature and the presented manifestation in the vallecula is an important differential diagnosis to EBV-associated epipharyngeal lymphoepithelial carcinoma.
Keywords: Hypopharynx; Lymphoepithelial-like carcinoma; HPV16; Ultrasound; EBV
Introduction
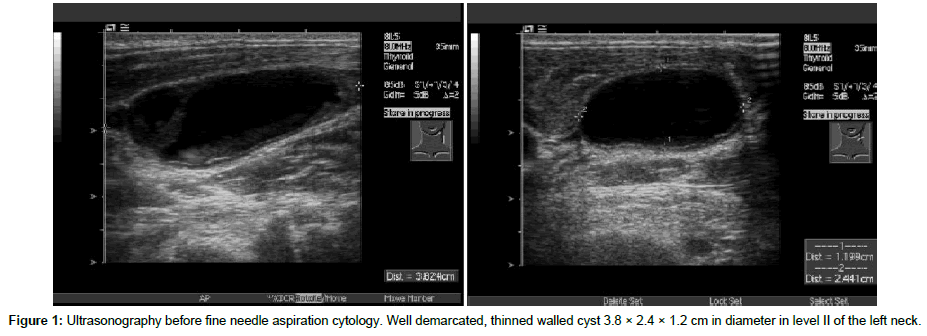
A 59 years old, healthy patient was referred by his family doctor because of a short history of painless neck mass. His personal history was unremarkable except for tonsillectomia at the age of nine. He was neither a smoker nor did he consume regularly alcohol. In the ultrasonography, a well demarcated cervical cyst (3.8 × 2.4 × 1.2 cm) compatible with second branchial arch cyst has been described (Figure 1).
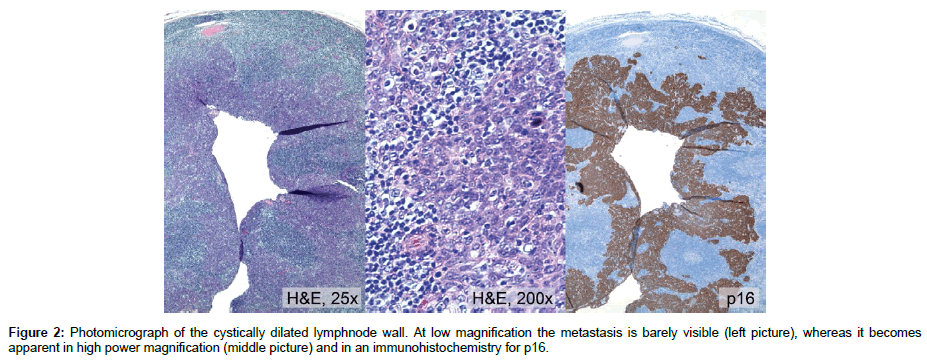
Following inconclusive fine needle aspiration cytology, a diagnostic resection was performed by the practicing ENT specialist. The histological sections showed a cystic lymph node metastasis. At low power magnification (25x; figure left) the cyst wall lining seemed normal, but in a higher magnification (200x) a layer consisting of poorly differentiated cells with a dense lymphocytic infiltrate became obvious compatible with a lymphoepithelial carcinoma with a so called “Schmincke” growth pattern (Figure 2). An extracapsular extension was not obvious. The infiltrating cells demonstrated immunohistochemically a squamous cell differentiation (p63 and CK 5/6 positivity). Furthermore the cells showed a strong reactivity for the cyclin dependent kinase p16. The EBER in-situ hybridization did not demonstrate Epstein-Barr virus gene integration in the tumor cells. In the subsequently performed HPV specific PCR, HPV16 DNA was detected and the tumor herein classified as a metastasis of a lymphoepithelial-like carcinoma [1] suggestive for a metastasis of an oropharyngeal primary (Figure 2).
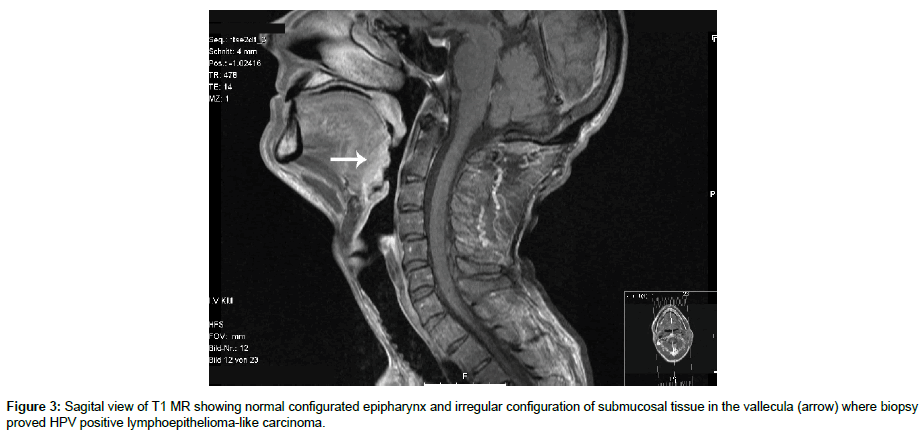
MR scan documented post-operative alterations in left sided level 2 after lymph node resection and normally configurated lymphoid tissue of the Waldeyer ring; however, with slight submucosal irregularities on the lingual surface of vallecula (Figures 3 and 4).
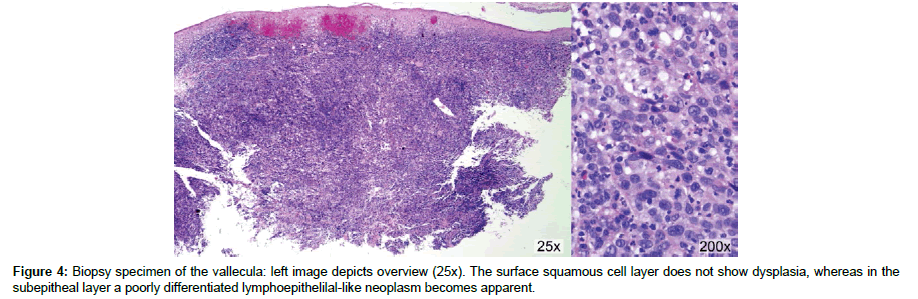
The panendoscopy, preceding directly modified radical neck dissection revealed a slightly irregular tongue base with an inconspicuous mucosal surface in the vallecula. Systematic sampling biopsies of the epipharynx, the tonsillar fossa, and the vallecula and tongue base resulted in the identification of a lymphoepithelial-like carcinoma in the left sided vallecula, staged after final histological analysis of the neck dissection as cT2 pN2b cM0; HPV associated lymphoepithelial-like carcinoma of the hypopharynx.’
Discussion
Squamous cell carcinomas of the head- and neck region (HNSCC) can manifest in about 13% of patients with a neck mass as the first and only clinical manifestation [2].
The non-keratizing squamous cell carcinomas of the pharynx have amply been described as undifferentiated nasopharyngeal carcinoma, lymphoepithelioma and lymphoepithelial-like carcinoma [1]. The latter is HPV-infection related and EBV negative has only recently described by Singh et al. in a cohort of 22 patients [1]. This stands in contrast to lymphoepithelioma of the nasopharynx which typically is associated to EBV integration [3]. Lymphoepithelioma can histologically be subdivided according to their phenotype into Regard-and Schmincke Type according to the describers [4,5]. The latter may be difficult to identify on routine H&E stained tissue slides due to the dens lymphocytic infiltrate, as in the here presented case.
Covered by inconspicuous mucosa such tumors are often difficult to identify by the endoscopist at gross examination and they are often only detected upon random biopsies in the oropharynx [2,6]. In our case, the cystic degeneration of the lymph node could have been indicative for a metastasis of an oropharyngeal carcinoma as previously described as a typical feature of such tumors [7]. Detection of EBV in neck metastasis has been described by Macdonald and colleagues as a biomarker for nasopharyngeal carcinoma 8. Recently, the role of HPV in pharyngeal carcinogenesis has become a major issue of research and HPV associated HNSCC with histologic appearance resembling EBVrelated lymphoepithelial carcinoma has only recently been described in tumors of the oropharyngeal region [1,9].
It has been shown in fine needle-aspiration study by Begum and colleagues that metastatic HNSCC are often HPV associated if the primary tumor was located in the oropharynx, whereas a HPV was only detected in a single case of a HNSCC of a different location [10]. They furthermore found a significant correlation of p16 expression in lymph node metastasis of SCC of the oropharynx. As such, HPV16 detection in neck metastasis of squamous cell carcinoma gain important role as a further biomarker in the work up of HNSCC.
Conclusion
We describe a unique case of a HPV16 associated lymphoepithelial-like carcinoma of the vallecula to illustrate the potential value of early molecular testing in the histologic work up in SCCHN diagnosed in a metastatic setting. Head and Neck lymph node metastases by squamous cell carcinomas of unknown primary demonstrating a lymphoepithelial growth pattern need further evaluation with p16 immunohistochemistry or molecular pathology based investigations such as EBER or HPV analysis. Early molecular tissue examination processing may assist the clinician to discover the primary tumor and may be decisive in the future for oncological HNSCC management. This is an important finding since HNSCC, especially if sub classified as lymphoepithelioma or lymphoepithelial-like squamous cell carcinoma are often difficult to detect on endoscopy for the clinician due a lack of surface epithelial involvement.
References
- Singhi AD, Stelow EB, Mills SE, Westra WH (2010) Lymphoepithelial-like carcinoma of the oropharynx: A morphologic variant of HPV-related head and neck carcinoma. Am J Surg Pathol 34: 800-805.
- Martin H, Romieu C (1952) The diagnostic significance of a lump in the neck. Postgrad Med 11: 491-500.
- Raab-Traub N (2002) Epstein-Barr virus in the pathogenesis of NPC. Semin Cancer Biol 12: 431-441.
- Schmincke A (1921) Über lympho-epitheliale Geschwülste. Beitr. Pathol Anat Allg Pathol 21: 161-170.
- Regaud C RL (1921) Sur uncas d'epithelioma epidermoide developpé dans le massif maxillaire superieur. Rev Laryngol Otol Rhinol 1921: 369-378.
- SE Mills MG, HF Frierson (2000) Squamous cell carcinoma variants: Tumors of the upper aerodigestive tract and ear. 26: 88-96
- Hoffmann M, Gottschlich S, Görögh T, Lohrey C, Schwarz E, et al. (2005) Human papillomaviruses in lymph node neck metastases of head and neck cancers. Acta Otolaryngol 125: 415-421.
- Macdonald MR, Freeman JL, Hui MF, Cheung RK, Warde P, et al. (1995) Role of Epstein-Barr virus in fine-needle aspirates of metastatic neck nodes in the diagnosis of nasopharyngeal carcinoma. Head Neck 17: 487-493.
- Zhang MQ, El-Mofty SK, Davila RM (2008) Detection of human papillomavirus-related squamous cell carcinoma cytologically and by in situ hybridization in fine-needle aspiration biopsies of cervical metastasis: A tool for identifying the site of an occult head and neck primary. Cancer 114:118-123.
- Begum S, Gillison ML, Nicol TL, Westra WH (2007) Detection of human papillomavirus-16 in fine-needle aspirates to determine tumor origin in patients with metastatic squamous cell carcinoma of the head and neck. Clin Cancer Res 13: 1186-1191
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi