Research Article, J Clin Exp Oncol Vol: 7 Issue: 4
Immediate Breast Reconstruction with Laparoscopic Harvested Omental Flap after Breast Cancer Surgery
Sandbichler P*, Pittl T, Pointner S, Paulmichl A and Hiehs S
Department for General Surgery and Radiology, Hospital St.Vinzenz, Austria
*Corresponding Author : Sandbichler P
Department for General Surgery and Radiology, Hospital St.Vinzenz, Sanatoriumstr.43, A-6511 Zams, Austria
Tel: 0043 664 600855810
E-mail: peter.sandbichler@krankenhaus-zams.at
Received: June 06, 2018 Accepted: July 04, 2018 Published: July 11, 2018
Citation: Sandbichler P, Pittl T, Pointner S, Paulmichl A, Hiehs S (2018) Immediate Breast Reconstruction with Laparoscopic Harvested Omental Flap after Breast Cancer Surgery. J Clin Exp Oncol 7:4. doi: 10.4172/2324-9110.1000223
Abstract
Here we present a rarely used technique for breast reconstruction after complete or subtotal subcutaneous mastectomy for breast cancer utilizing a laparoscopically harvested omental flap.
The procedure was performed in selected patients with multicentric carcinomas, large, central tumors (also post treatment with neoadjuvant chemotherapy), tumors with extensive intraductal components, diffuse carcinomas in situ and in patients desiring the procedure. To date, 65 of these procedures (39 complete and 26 partial mastectomies) have been performed. After the sentinel node biopsy, laparoscopy was performed in order to estimate the size of the omentum. The omentum was dissected, preserving the right gastroepiploic vessels as the pedicle of the omental flap.
After performing the subcutaneous mastectomy through an infra mammary incision, a subcutaneous tunnel was created, and the omentum pulled out through a 2-3 cm paraxyphoidal incision, and placed within the breast defect.
The cosmetic result was excellent to satisfactory in the majority of cases. There was one loss of the omental flap due to fat necrosis, and one gastric perforation was managed laparoscopically. In three patients, an additional augmentation with lipofilling became necessary. Small skin necrosis could be conservatively treated. Postoperative radiation in patients with positive lymph nodes and subtotal mastectomy was performed without complications. There was no local recurrence to date.
In selected patients, this technique produces good results, creating a breast with a natural, soft consistency, and with minimal donor site morbidity. It provides an esthetically appealing supplement to the established methods. Difficulties include preoperative estimation of the size of the omentum. However, if the volume should be inadequate in the beginning, it frequently increases within the first six months. Also this technique can only be applied for unilateral reconstruction.
Keywords: Breast cancer; Tumors; Laparoscopy; Oncoplastic surgery
Introduction
More than 70% of breast cancer patients can be treated in a breast-preserving manner with good results, to which modern neoadjuvant chemotherapies and the reduction of the tumor-free margin (no ink on tumor) also contribute [1]. However, a significant percentage of breast pathologies remain which require complete or subtotal removal of the breast parenchyma. These are the domain of oncoplastic surgery, which can achieve good cosmetic results with various flap plastics or breast implants. However, in some cases large defects of the donor site with potential morbidity can occur [2-5].
As an additional option for autologous breast reconstruction, the omentum majus is also an option. In 1963, for example, Kiricuta reconstructed breast and thorax defects with an omentum flap [6]. The laparoscopic preparation of the omentum majus to cover a soft tissue defect was described by Saltz et al. [7]. Later on, Cothier- Savey et al. and Jimenez et al. reported breast reconstructions with laparoscopically prepared omentum flap [8,9]. This technique was mainly investigated in the Far East, whereby Zaha et al. recently reported a series of 200 cases with good results [10-13].
In Europe, only one group has reported a small number of breast reconstructions using a free omentum flap [14]. We started breast reconstruction in 2014 with a laparoscopically prepared, vascular pedicled omentum flap and report a series of 65 cases after total or subtotal subcutaneous mastectomy.
Materials and Methods
From November 2014 until December 2017, 65 patients with ages between 26 and 72 years were treated. In 39 of the patients, a complete subcutaneous mastectomy was performed, while the other 26 patients underwent only a partial subcutaneous mastectomy. Indications for the procedure were an extended DCIS (ductal carcinoma in situ), remaining multicentric carcinoma after neoadjuvant chemotherapy, large tumors with positive hormone receptor status in small breasts or the desire of patients with small carcinomas to avoid radiation therapy. Patients with skin-infiltrating tumors and inflammatory carcinomas were excluded. Furthermore, large abdominal operations, especially those of oncological nature, were considered as exclusionary criteria. 14 patients with multicentric carcinomas had neoadjuvant chemotherapy. In 27 of all cases, postoperative radiotherapy was necessary (Table 1).
| Patients Characteristics | |
|---|---|
| Patients | |
| N (#of patients) | 65 |
| Avg. age | 53 |
| Min. age | 26 |
| Max. age | 72 |
| Type of Mastectomy | |
| Total Mastectomy | 60% |
| Partial Mastectomy | 40% |
| Cancer Type | |
| Tis | 19 (29%) |
| pT1a | 2 (3%) |
| pT1b | 8 (13%) |
| pT1c | 22 (34%) |
| pT2 | 7 (11%) |
| ypTx | 7 (11%) |
| N+ | 13 (20%) |
| Therapy | |
| Postmastectomy radiotherapy | 27 |
| Neoadjuvant chemotherapy | 14 |
| Surgery | |
| Avg. surgery time (min) | 154 |
| Max. surgery time (min) | 195 |
| Min. surgery Time (min) | 117 |
Table 1: General overview of the patient set.
Surgical procedure
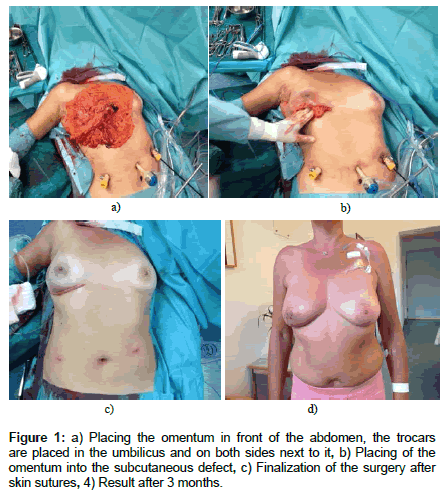
The sentinel node (SN) biopsy was usually performed first, except in neoadjuvantly treated patients in which the SN biopsy had already been performed pretherapeutically. Laparoscopy was then performed to estimate the size of the omentum. The laparoscopic trocar was inserted through the umbilicus. Two additional 5 mm working trocars were placed next to the camera trocar on both sides.
The omentum majus was then removed from the greater curvature of the stomach while preserving the right gastroepiploid vessels, which serve as the vascular pedicle. The mobilization continued into the spleen hilus in order to gain as much tissue as possible. Subsequently, the omentum was detached from the transverse colon, starting laterally, and the preparation was carried out up to the right flexure. An inframammary skin incision was made, which was later used to perform the subcutaneous mastectomy. A clamp was used to subcutaneously build a tunnel into the direction of the xyphoid and the clamp was inserted into the abdomen under laparoscopic vision, after which the incision was extended to approximately 3-4 cm. The omentum was then carefully pulled out of the abdomen through this tunnel and placed in front. The subcutaneous mastectomy was then performed via the infra mammary incision. Depending on the size of the omentum or the oncological necessity, the mastectomy was done completely or partially.
Retromamillary tissue was sent in separately for histological frozen section examination. In the case of partial resections, the cutoff margins were also examined. If the SN node biopsy was positive, an axillary dissection was performed and the extent of the resection adapted to the size of the omentum, since radiation is necessary in these cases.
After the breast resection, the omentum was swiveled into the subcutaneous defect, taking care that the stem of the vessel was not twisted. After insertion of a suction drainage, the wound was closed. The average operating time was ~154 min (117-195) (Figure 1).
Results
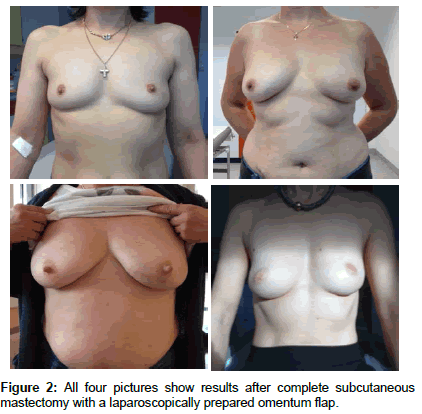
In all 65 cases of complete or subtotal subcutaneous mastectomy for breast cancer utilizing a laparoscopically harvested omental flap, an oncological R0 resection was possible. Excellent to good cosmetic results were achieved in the vast majority of these cases, especially after subtotal mastectomies (Figure 2).
In nine patients, the omentum was not sufficiently large after complete subcutaneous mastectomy. In three of these cases, the interfering incongruence could be permanently compensated by means of lipofilling. Three patients were satisfied with the situation and correction procedures are planned for the remaining three.
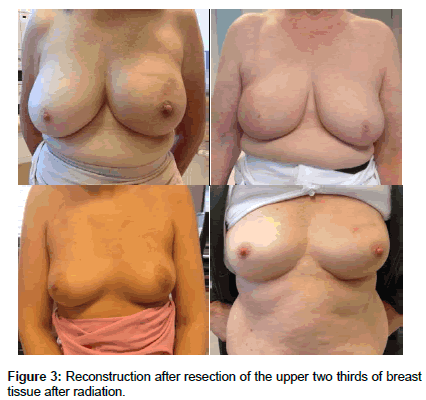
In the case of subtotal mastectomies, the extent of resection was adapted, if oncologically possible, to the size of the omentum, which could easily be inserted into all quadrants and led to predominantly good results. The following postoperative radiotherapy did not lead to any permanent changes in the implanted adipose tissue (Figure 3). In the first few postoperative weeks, the omentum was often indurated. Within the first three months, however, it became softer and eventually reached the same consistency as the other breast, so that no palpatory difference was noticeable. In some cases, the volume of omentum also increased by up to 20% within the first six months.
In three cases, antihormonal therapy resulted in considerable weight gain with enlargement of the contralateral breast. Skin necroses occurred in only five patients and predominantly in smokers, which healed completely without surgical intervention. The ample blood supply of the omentum may be a contributing factor for the relatively low number of skin necrosis cases. In one patient, the omentum had to be removed due to multiple fatty tissue necroses that occurred despite intact blood circulation. A gastric perforation that occurred after a week in one patient was successfully treated laparoscopically. It was noticeable that in none of the cases infection-related complications occurred, which could be due to the unique antibacterial quality of the omentum [15]. Hernia in the area of paraxyphoidal incision has not occurred so far, nor have any local relapses.
Discussion and Conclusion
Breast reconstruction with laparoscopically harvested omentum flap has been described in the past, especially in the Far East. Zaha et al. presented the world’s largest series with 200 patients [13]. However, there are only a few studies on this topic in Europe up to this point [14]. The advantages of this method are the small donor site defect of the omentum, comparable to a laparoscopic cholecystectomy. In addition, the nature of the omentum, which in most cases guarantees a natural shape and consistency of the operated breast, plays an important role. Although the technique can only be applied to unilateral reconstruction, the easy availability and minimal changes due to postoperative radiation, with a low overall complication rate, as well as a fast postoperative convalescence are of great benefit for patients.
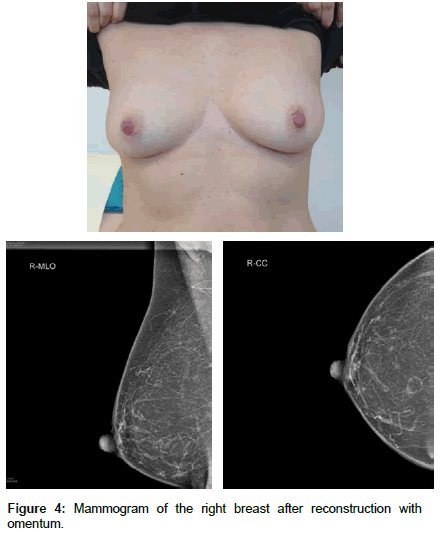
This case series has also shown that the size of the omentum is difficult to estimate preoperatively, so that for complete mastectomies a careful selection and also corresponding information of the patients about possible corrective interventions is necessary. Corrective interventions are planned after six months at the earliest, as the implanted omentum can increase in size during this time. We have therefore proceeded, if oncologically possible, to adjust the extent of the mammary gland resection to the volume of the omentum, thus achieving excellent esthetic results in all quadrants of the breast [13]. Mammographic examinations of the operated breast can be reliably assessed due to the constitution of the omentum (Figure 4).
Regarding oncological safety, Zaha was able to achieve a very low local recurrence rate with an observation period of 90 months [13]. No local recurrence has yet occurred in the patients described in this case series, although our follow-up time from max. 37 months is currently still too short.
In summary, we believe this surgical method is a valuable addition to the autologous reconstructive spectrum with a low complication rate, low donor site related morbidity and good to very good esthetic results. A prerequisite is a meticulous selection of patients, since the size of the omentum is difficult to determine preoperatively.
References
- Moran MS, Schnitt SJ, Giuliano AE, Harris JR, Khan SA, et al. (2014) Society of Surgical Oncology-American Society for Radiation Oncology consensus guideline on margins for breast-conserving surgery with whole-breast irradiation in stages I and II invasive breast cancer. J Clin Oncol 32: 1507-1515.
- Hoffmann J, Wallwiener D (2009) Classifying breast cancer surgery: a novel, complexity-based system for oncological, oncoplastic and reconstructive procedures, and proof of principle by analysis of 1225 operations in 1166 patients. BMC Cancer 9: 108.
- Munhoz AM, Montag E, Fels KW, Arruda EG, Sturtz GP, et al. (2005) Outcome analysis of breast-conservation surgery and immediate latissimus dorsi flap reconstruction in patients with T1 to T2 breast cancer. Plast Reconstr Surg 116: 741-752.
- Hamdi M, Van Landuyt K, Monstrey S, Blondeel P (2004) Pedicled perforator flaps in breast reconstruction: a new concept. Br J Plast Surg 57: 531-539.
- Kronowitz SJ, Feledy JA, Hunt KK, Kuerer HM, Youssef A, et al. (2006) Determining the optimal approach to breast reconstruction after partial mastectomy. Plast Reconstr Surg 117: 1-11.
- Kiricuta I (1963) The use of the great omentum in the surgery of breast cancer. Presse Med 71: 15-17.
- Saltz R, Stowers R, Smith M, Gadacz TR (1993) Laparoscopically harvested omental free flap to cover a large soft tissue defect. Ann Surg 217: 542-546.
- Cothier-Savey I, Tamtawi B, Dohnt F, Raulo Y, Baruch J (2001) Immediate breast reconstruction using a laparoscopically harvested omental flap. Plast Reconstr Surg 107: 1156-1163.
- Jimenez AG, St Germain P, Sirois M, Hatheway M, Lethbridge R (2002) Free omental flap for skin-sparing breast reconstruction harvested laparoscopically. Plast Reconstr Surg 110: 545-551.
- Guan D, Lin H, Lv Z, Xin Y, Meng K, et al. (2015) The oncoplastic breast surgery with pedicled omental flap harvested by laparoscopy: initial experiences from China. World J Surg Oncol 13: 95.
- Zaha H, Inamine S, Naito T, Nomura H (2006) Laparoscopically harvested omental flap for immediate breast reconstruction. Am J Surg 192: 556-558.
- Zaha H, Inamine S (2010) Laparoscopically harvested omental flap: results for 96 patients. Surg Endosc 24: 103-107.
- Zaha H, Abe N, Sagawa N, Unesoko M (2017) Oncoplastic surgery with omental flap reconstruction: a study of 200 cases. Breast Cancer Res Treat 162: 267-274.
- van Alphen TC, Fechner MR, Smit JM, Slooter GD, Broekhuysen CL, et al. (2017) The laparoscopically harvested omentum as a free flap for autologous breast reconstruction. Microsurgery 37: 539-545.
- Chandra A, Srivastava RK, Kashyap MP, Kumar R, Srivastava RN, et al. (2011) The anti-inflammatory and antibacterial basis of human omental defense: selective expression of cytokines and antimicrobial peptides. PLoS One 6: e20446.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi