Research Article, J Trauma Stress Disor Treat Vol: 7 Issue: 4
Impact of Trauma and Living Conditions on Psychopathology of Ambulance Personnel - A Comparison between German and Palestinian Ambulance Drivers
Jasmin Wittmann1, Abdel Aziz Mousa Thabet2 and Youssef Shiban3*
1Department of Psychology, Bielefeld University, Bielefeld, Germany
2Al Quads University, School of Public Health, Child Institute, Gaza
3Department of Clinical Psychology; PFH – Private University of Applied Sciences, Göttingen, Germany
*Corresponding Author : Youssef Shiban
PFH – Private University of Applied Sciences, Weender Landstraße 3-7, 37073 Göttingen, Germany
Tel: +4955154700445
E-mail: shiban@pfh.de
Received: August 17, 2018 Accepted: September 12, 2018 Published: September 20, 2018
Citation: Wittmann J, Thabet AAM, Shiban Y (2018) Impact of Trauma and Living Conditions on Psychopathology of Ambulance Personnel: A Comparison between German and Palestinian Ambulance Drivers. J Trauma Stress Disor Treat 7:2. doi: 10.4172/2324-8947.1000190
Abstract
The prevalence and the types of traumas experienced by people differ significantly depending on the situation people live in, e.g., in a generally safe environment or in a stressful one. The current study compares German and Palestinian ambulance drivers investigating their overall history of traumas, symptoms of posttraumatic stress, and levels of anxiety and depression. Participants completed a series of questionnaires measuring stress, trauma, depression, and anxiety. The data from both groups were compared. As expected, the Palestinian group had experienced more traumata, demonstrated higher levels of posttraumatic stress symptoms, and had higher scores on the depression and anxiety scales than the German ambulance drivers. There were significant relationships between PTSD and depression, between PTSD and anxiety as well as between depression and anxiety in both samples. Our results indicate a clear need for a further investigation regarding the impact of multiple traumas on the psychological well-being of Palestinian ambulance drivers.
Keywords: PTSD; Trauma; Anxiety; Depression
Introduction
Post-Traumatic Stress Disorder (PTSD) is a prevalent disorder which has attracted a great amount of research aiming to understand its basic mechanisms and hopes to develop effective treatments for patients suffering from PTSD. The American Psychiatric Association classified trauma- and stress-related disorders – and by association PTSD – as their own separate category in the fifth edition of its Diagnostic and Statistical Manual of Mental Disorders (DSM 5). One necessary diagnostic criterion for PTSD is the exposure to a catastrophic event involving either threatened death or injury, or a threat to the physical integrity of oneself or others.
As exposure to a traumatic event is essential for developing PTSD, it is important to assess the frequency of such events in the lifetime of different samples. Furthermore, it has been determined that the number of traumatic experiences is a powerful predictor of PTSD. Karam et al. reported that exposure to multiple traumatic events is most common among persons suffering from PTSD [1-3].
Some people have a higher risk of experiencing multiple traumatic events due to their occupation. For example, police officers, firefighters, or ambulance drivers, who face an increased risk of experiencing a catastrophic or life-threatening event [4]. Professional emergency service personnel and firefighters have one of the most dangerous and stressful occupations, due to the many threats they face while working. These occupations carry with them the responsibility of protecting the public and all of these jobs have the potential of causing serious physical and psychological harm to the employee. Emergency service personnel often report physical symptoms of distress, particularly after involvement in critical incidents. Physical exhaustion, sleep disturbances, nausea and gastrointestinal problems are some of the commonly physical symptoms reported by them. Their chronic exposure to traumatic events and job-related stressful situations put them at increased risk of developing PTSD and other mental health problems [5,6]. Emergency service personnel are subjected to higher rates of stress responses and report higher levels of PTSD, ranging from 16%-24% compared to the general population that has a lifetime prevalence rate of 6%-9% for PTSD [7]. Persistent re-experiencing of the traumatic event, avoidance of trauma-related stimuli, and increased emotional arousal can be experienced months to years after the event occurred. Ambulance personnel are a part of Palestinian society and experienced the effect of war and conflict during 2014 war on Gaza, lasting a total of 50 days (8 July to 26 August 2014). In summary, it can be stated that ambulance officers experience a high risk of trauma exposure due to their occupation, which has associated consequences on psychological well-being.
Against this background, further research might target the question of whether or not living in a war zone or a stressful environment has influence on the probability of PTSD development after experiencing a traumatic event, corrected for trauma exposure in the general population. People living under such circumstances are faced daily with high-stress situations as opposed to people living in secure surroundings, who rarely experience traumatic situations. German and Palestinian ambulance drivers are exposed to a higher risk of experiencing a trauma because of their occupation. While the German sample lives in an almost secure surrounding, the Palestinian sample lives in a war zone. The question is whether this fact influences the likelihood of developing PTSD after experiencing a traumatic event. The aim of this study was to investigate whether there is a difference between Palestinian and German ambulance drivers when comparing their overall history of traumas and posttraumatic stress symptoms, as well as their levels of anxiety and depression. We hypothesize that the Palestinian group has experienced more traumas because they live in a war zone (e.g., they were all working in Gaza during the 2014 Israel–Gaza conflict). Furthermore, we expect to find higher levels of anxiety and depression and a higher number of posttraumatic stress symptoms in this group as well.
Method
Participants
One hundred forty four Palestine and German relief forces working as part of a medical or ambulance service were investigated. The inclusion criterion was to be part of a relief force, working with either a medical or ambulance service. This criterion was assessed via one questionnaire. The Palestinian sample was recruited at the Palestinian Red Crescent Emergency Department in Gaza City. Written informed consent of joining the study was given by the participants after reading the letter of approval from the Head of Emergency Department. Forty-one male participants were interviewed at their workplace. The interview lasted for 40 minutes per person. The Palestine sample consisted of 41 participants (all male, aged between 22 and 61, M=40.2, SD=10.2). The German participants were recruited through personal connections to local ambulance drivers and adverts posted in medical departments. There was no interview in the German sample. One hundred and three German participants filled in the questionnaire, 53 of them were excluded from the study because they did not finish the questionnaire. The final German sample consisted of 50 participants (80% male, aged between 16 and 59, M=35.7, SD=10.5).
Measures
Participants filled in a demographic questionnaire (age, sex, family status, residence, and current occupation), the Gaza Traumatic Events Checklist – 51 Days war on Gaza [8] translated into German by the authors, the Davidson PTSD Scale [9] to assess PTSD symptoms, the Hamilton Anxiety Scale [9,10] to measure the severity of anxiety, and the short form of the Beck Depression Inventory [11,12] to assess symptoms of depression.
The Gaza Traumatic Events Checklist – 51 Days war on Gaza consisted of 28 items. The checklist was developed to reflect the particular circumstances of the regional conflict, which could not be captured by other war trauma measures, and has been reported previously [13]. The 28 Items cover three domains of events that are typical of the war in Gaza: (1) personally witnessing acts of violence (e.g., killing of relatives, home demolition, bombardment, or injuries); (2) experiencing loss or injury of family and other close persons; and (3) being personally the target of violence (e.g., being shot, injured, or beaten up by soldiers). The respondents rated whether they had been exposed to each of these events as (0) ‘no’ or (1) ‘yes’. A total score was estimated. Responses to these items were highly internally consistent (Cronbach’s alpha=.82).
The Davidson PTSD Scale is a 17 item self-report measurement that assesses the 17 DSM-IV symptoms of PTSD. Items are rated on a 5-point Likert scale (from 0=“not at all” to 4=“every day”). In addition to the 17 items, two further questions ask about the duration of the problems experienced (“How long have you been having these indicated problems?”) with specific answer categories – “Less than one month”- “One to three months” –“more than six months,” as well as the moment when the participants began experiencing problems (“How soon after the traumatic event did the problems occur?”) with the answer categories “within six months” and “after six months and later”.
The HAM-A (Hamilton Anxiety Rating Scale) consists of 14 items, each defined by a series of symptoms, and measures both psychic anxiety (mental agitation and psychological distress) and somatic anxiety (physical complaints related to anxiety). Answers are given on a 5-point Likert scale (from 0=“not at all” to 4=“extremely”). The summed values provide a scoring ranging from 0 to 56. A score of 17 or less represents mild anxiety, a score between 18 to 24 mild to moderate anxiety, and a score of 25 and above moderate to severe anxiety. The scale predates the current definition of a generalized anxiety disorder. An inter-rater reliability of .89 and the internal consistency of .83 are given [11-15]. Available data indicates validity correlations of .50 to .80 with a global anxiety rating [16].
The Beck Depression Inventory (BDI) is one of the most widely used instruments to assess depression. The main aim of the BDI is to measure depression symptoms and severity in persons age 13 and older. This inventory was validated in Palestine culture [17]. In the current study, participants completed the short form BDI, BDI-SF, which consists of 13 items. The severity of depression is classified on the basis of the total score. In a normal community sample, a BDI score ≤ 4 suggests no or minimal depression, 5 to 7 represents mild to moderate depression, 8 to 15 is moderate to severe, and ≥ 16 indicates a severe level of depression. The reliability was determined on the basis of internal consistency (Cronbach’s alpha). Overall, the results were determined to be satisfactory for both the total sample (.84) and for each gender (men: .85, women: .83), as well as the convergent and divergent validity.
Results
Number of traumatic events
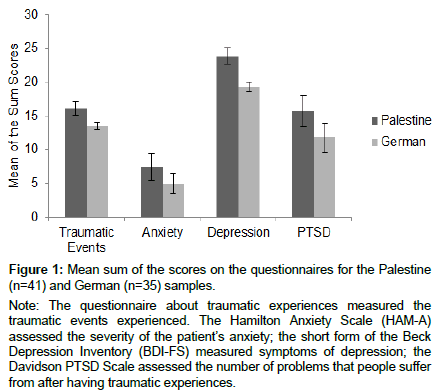
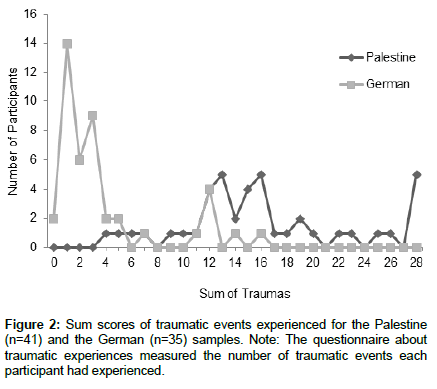
As depicted in Figure 1, the number of traumatic events experienced was higher in the Palestinian group than in the German group, t(89)=8.06, p<.001, d=1.72, with an average of about 16 traumatic events in the Palestine group and 6 events in the German group. Furthermore, the German sample averaged a maximum of three traumatic events, while the Palestinian group averaged a maximum of more than 12 traumatic events, as shown in Figure 2.
Figure 1: Mean sum of the scores on the questionnaires for the Palestine (n=41) and German (n=35) samples.
Anxiety
Figure 1 also illustrates the average anxiety levels of both groups. It is clearly visible from the figure that the Palestinian group demonstrated higher anxiety scores when compared to the German group. This was confirmed by a significant t-test, t(88)=3.24, p<.002, d=0.73.
Depression
Figure 1 shows the mean scores from the BDI-FS. As it can be seen, the scores of the two groups differ in this dimension. These plotted differences were confirmed by a significant t-test, t(88)=3.31, p<.002, d=0.76.
Posttraumatic stress symptoms
Figure 1 also suggests that both groups differ in their amounts of posttraumatic stress symptoms. The statistical analysis confirmed that the Palestinian group had significantly higher levels of posttraumatic symptoms, t(89)=4.65, p<.001, d=0.99.
Relationship between trauma, PTSD, depression and anxiety
Table 1 shows the Spearman correlation between the different scales for the German and the Palestinian sample. In the Palestinian group there were no statistically significant relationships between the total sum of traumas and PTSD, depression and anxiety. The correlation test showed that there were statistically significant positive relationships between the total score of PTSD and both depression (r=.67, p<.01) and anxiety (r=.83, p<.01). In addition, there was a positive correlation between depression and anxiety (r=.68, p<.01). In the German sample, the total sum of traumas significantly correlated with the variables PTSD (r=.56, p<.01), depression (r=.32, p<.05) and anxiety (r=.39, p<.01). The correlation test also showed a significant relationship between depression and anxiety (r=.65, p<.01), as well as between the sum of PTSD symptoms and anxiety (r=.57, p<.01).
| Country | GTECa | BDI-SFb | D-PTSDc | HAM-Ad | |
|---|---|---|---|---|---|
| Palestine | GTEC | - | - | - | - |
| BDI-SF | .006 | - | - | - | |
| D-PTSD | .097 | .669** | - | - | |
| HAM-A | .128 | .685** | .836** | - | |
| Germany | GTEC | - | - | - | - |
| BDI-SF | .318* | - | - | - | |
| D-PTSD | .564** | .539** | - | - | |
| HAM-A | .390** | .654** | .574** | - |
Table 1: Inter-correlations between the variables sum of trauma, depression, PTSD and anxiety for Palestinian (n=41) and for German participants (n=50).
Discussion and Conclusion
The study investigated whether there was a difference between a German and a Palestinian group of healthcare employees and ambulance drivers when comparing the numbers of traumatic events they experienced, their posttraumatic stress symptoms, and their levels of depression and anxiety. The results confirm that the Palestinian healthcare employees experienced greater than 50% more traumatic events than the German group, and have more symptoms of posttraumatic stress, anxiety, and depression. These results were in line with our hypotheses.
The correlation between the scales shows a significant relationship between PTSD and depression, PTSD and anxiety, and depression and anxiety in both samples. These findings are in line with the current research. It is well established that the concepts of depression and anxiety are intertwined with one another and it is difficult to differentiate between the symptoms of each disorder. Some of the symptoms experienced by people suffering from these disorders overlap, although the core symptoms of anxiety and depression are distinguishable from one another [18]. Regarding the state of the research, the correlation between the depression scale and the anxiety scale in our sample is not surprising. Research also indicates a significant comorbidity between PTSD and major depression. They both can be single consequences of experiencing a trauma but they can also appear in a comorbid fashion [19]. Our study revealed a statistically significant relationship between PTSD and depression in both samples. The third correlation between PTSD and anxiety also appeared to be significant in the German and the Palestinian group. Postulate that some people are more sensitive to anxiety and are therefore more at risk of developing PTSD [20]. This view, indicating a relationship between PTSD and anxiety, can be supported by our study.
Surprisingly, in the Palestinian sample there were no significant correlations between the sum of traumas and all the other scales, in comparison to the German sample. Karam et al. argue that exposure to multiple traumas increases the risk of developing PTSD, and therefore a direct relationship between the sum of traumas and the higher scores on the other scales was expected. These results indicated that the PTSD and mental health problems in the Palestinian sample could be due to previous wars, trauma, siege and stress. In contrast to these findings, the scores on the depression, anxiety and PTSD scales in the German sample correlated with the reported sum of traumas.
The specific kinds of traumatic events experienced were not assessed in this study, and it is possible that the risk of PTSD varies with the type of event experienced [1,2]. Furthermore, we have not yet been able to distinguish the extent to which the occupation and the overall stressful environment influences the development of PTSD symptoms.
The traumatic experience questionnaire developed by the Palestinian research group was mostly focused on assessing events related to military actions, which could have caused a certain data distortion.
It would be interesting to see how the differences between the two groups might influence their capacity for emotional learning, and how these differences affect the risk of developing mental disorders such as PTSD.
Author Note
We would like to thank the participants and our interns for the support and the valuable comments. No potential competing financial interests exist.
References
- Cloitre M, Stolbach BC, Herman JL, Kolk B, Pynoos R, et al. (2009) A developmental approach to complex PTSD: Childhood and adult cumulative trauma as predictors of symptom complexity. J Trauma Stress 22: 399-408.
- Karam EG, Friedman MJ, Hill ED, Kessler RC, McLaughlin KA, et al. (2014) Cumulative traumas and risk thresholds: 12â€Âmonth PTSD in the World Mental Health (WMH) surveys. Depress Anxiety 31: 130-142.
- Ullman SE, Filipas HH (2001) Predictors of PTSD symptom severity and social reactions in sexual assault victims. J Trauma Stress 14: 369-389.
- Skogstad M, Skorstad M, Lie A, Conradi H, Heir T, et al. (2013) Work-related post-traumatic stress disorder. Occupy Med 63: 175-182.
- Haslam C, Mallon K (2003) A preliminary investigation of post-traumatic stress symptoms among firefighters. Work & Stress 17: 277-285.
- Wagner D, Heinrichs M, Ehlert U (1998) Prevalence of symptoms of posttraumatic stress disorder in German professional firefighters. American Journal of Psychiatry 155: 1727-1732.
- Diagnostic and statistical manual of mental disorders (DSM-5®) American Psychiatric Association (2013). American Psychiatric Pub.
- Thabet AA, Thabet S (2015) Stress, trauma, psychological problems, quality of life, and resilience of Palestinian Families in the Gaza Strip. Clinical Psychiatry 1: 1-11.
- Davidson JR, Book S, Colket J, Tupler L, Roth S, et al (1997) Assessment of a new self-rating scale for post-traumatic stress disorder. Psychol Med 27: 153-160.
- Hamilton M (1976) ECDEU Assessment manual for psychopharmacology (193-198) Rockville, Maryland.
- Hamilton M (1996) Hamilton Anxiety Scale (HAMA) In CIPS (Ed.), Internationale Skalen für Psychiatrie. Göttingen.
- Beck A, Steer R, Brown G (2000) BDI-FS Screen for medical inpatients: Manual. Psychological Corporation. San Antonio, TX.
- Kliem S, Brähler E (2013) Beck Depressions-Inventar - Fast Screen (BDI-FS), Pearson Assessment, Frankfurt.
- Thabet AA, Karim K, Vostanis P (2006) Trauma exposure in pre-school children in a war zone. Br J Psychiatry 188: 154-158.
- Beneke M (1987) Methodological investigations of the Hamilton anxiety scale. Pharmacopsychiatry 20: 249-255.
- Snaith R, Baugh S, Clayden A, Husain A, Sipple, M (1982) The Clinical Anxiety Scale: an instrument derived from the Hamilton Anxiety Scale. Br J Psychiatry 141: 518-523.
- Thabet L, Thabet AA, Abdul S, Vostanis P (2007) Mental health problems among orphanage children in the Gaza Strip. Adoption & Fostering 31: 54-62.
- Agudelo D, Buela-Casal G, Spielberger CD (2007) Anxiety and depression: the problem of the differentiation through the symptoms. Salud Mental 30: 33-41.
- Shalev AY, Freedman S, Peri T, Brandes D, Sahar T, et al (1998) Prospective study of posttraumatic stress disorder and depression following trauma. Am J Psychiatry 155: 630-637.
- Marshall GN, Miles J, Stewart SH (2010) Anxiety Sensitivity and PTSD Symptom Severity Are Reciprocally Related: Evidence from a Longitudinal Study of Physical Trauma Survivors. J Abnorm Psychol 119: 143-150.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi