Research Article, Int J Ophthalmic Pathol Vol: 10 Issue: 0
Keratoconus screening in Basic School Children using keratoconus suspect criteria in Aljaded Althawra (Aljazeera State)
Diana Mohammed1*, Alnazir Mohammed2
1Department of Ophthalmology, Alrustaq Hospital, Alrustaq, Oman
2Department of Ophthalmology, Makkah eye complex, Khartoum, Sudan
*Corresponding Author: Diana Mohammed
Department of Ophthalmology, Alrustaq Hospital, Alrustaq, Oman
E-mail: dndnmasanko1982@yahoo.com
Received: September 21, 2021 Accepted: October 21, 2021 Published: October 28, 2021
Citation: Mohammed D, Mohammed A (2021) Keratoconus Screening in Basic School Children using Keratoconus Suspect Criteria in Aljaded Althawra (Aljazeera State). Int J Ophthalmic Pathol S4.
Abstract
Prolonged Objectives: Keratoconus screening in Basic Children School using Keratoconus suspect criteria & to detect specificity and sensitivity of each criteria in Aljaded Althawra. Also, to identify the risk factors of keratoconus.
Material and Methods: This study is a community based cross sectional analytical study conducted in Aljaded Althawra – Alkamleen locality– Aljazeera state – between Nov 2014 – April 2015. Four hundred students (800 eyes), age between 5 - 15 years old were examined 58.2%were males, and 41.8% were females. Visual acuity, slit lamp, fundus examination was taken. KC was detected from study sample according to keratoconus suspect criteria & corneal topography done to detect KC.
Result: 45 (11.25%) 90 eyes had keratoconus suspect Criteria. Male 68.9 %, female was 31.1 %. Peak’s age group was 9-12 years old (48,9%). VKC 76 eyes (84.4%), CVA less than normal 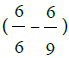 21 eyes (23.3%), real cylinder (– 4.0) or more 8eyes (8.9%), KC in fellow eye 14(15.6%) and family history of KC & frequent change of glasses 0.0%. The risk factor associated with KC, rubbing eye 71.1%, history of wearing glasses 31.1% & family history of refractive error 31.1%.14 eyes (15.5%) were KC, males (57.1%) & females 42.9%. 11 eyes (14.5%) had VKC,7 eyes (33.3%) had CVA less than normal
21 eyes (23.3%), real cylinder (– 4.0) or more 8eyes (8.9%), KC in fellow eye 14(15.6%) and family history of KC & frequent change of glasses 0.0%. The risk factor associated with KC, rubbing eye 71.1%, history of wearing glasses 31.1% & family history of refractive error 31.1%.14 eyes (15.5%) were KC, males (57.1%) & females 42.9%. 11 eyes (14.5%) had VKC,7 eyes (33.3%) had CVA less than normal 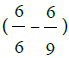 , 6 eyes (75.0%) had real cylinder (– 4.0) or more,4 eyes (28.6%) had KC in fellow eye,0 eyes (0.0%) had family history of KC & frequent change of glasses.
, 6 eyes (75.0%) had real cylinder (– 4.0) or more,4 eyes (28.6%) had KC in fellow eye,0 eyes (0.0%) had family history of KC & frequent change of glasses.
Conclusion: Results of this study suggested strong association between KC and high cylinder (– 4.0) or more in autorefractometer reading & CVA less than normal 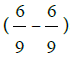 and KC in fellow eye according to p value and sensitivity & specificity but there is no relation to VKC. Keratoconus was more related to rubbing eyes, Hx of wearing glasses and family history of refractive errors. Screening of KC with corneal topography allows early detection and management.
and KC in fellow eye according to p value and sensitivity & specificity but there is no relation to VKC. Keratoconus was more related to rubbing eyes, Hx of wearing glasses and family history of refractive errors. Screening of KC with corneal topography allows early detection and management.
Keywords: Keratoconus, Eye Disease, Eye Rubbing
Introduction
Keratoconus is a bilateral non-inflammatory corneal ectasia with
an incidence of approximately 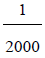 in general population [1,2]. It is
characterized by central and para- central corneal stromal thinning
and subsequent conical ectasia. This conical distortion of the cornea
results in irregular astigmatism with associated reduction in visual
performance. It typically presents in adolescence and progresses in a
variable manner.
in general population [1,2]. It is
characterized by central and para- central corneal stromal thinning
and subsequent conical ectasia. This conical distortion of the cornea
results in irregular astigmatism with associated reduction in visual
performance. It typically presents in adolescence and progresses in a
variable manner.
Worldwide, it occurs in all ethnic groups, with males and females affected equally. Keratoconus is typically bilateral, but asymmetric with the worse eye continuing to have a poorer prognosis as the condition progresses [1]. The occurrence of keratoconus is usually an isolated condition, but it has been reported to occur with increased frequency in a number of ocular and systemic disorders. Ocular associations include VKC [1,3], retinitis pigmentosa, blue sclera, aniridia, ectopia lentis and Leber’s congenital amaurosis. Systemic associations include atopy, magnesium deficiency, Down’s syndrome, Turner syndrome, connective tissue disorders (such as Marfan’s, Ehlers-Danlos, osteogenesis imperfecta and pseuodoxanthoma elasticum), mitral valve prolapse, Laurence-Moon-Biedl syndrome, Rieger’s syndrome and neurofibromatosis. It has been particularly linked to various forms of ocular trauma such as hard contact lens wears, allergic eye disease and especially eye rubbing [1,2]. An inverse relationship between severity of the condition and diabetes has been reported [4].
A genetic predisposition to keratoconus has been observed [5,6] with the disease reported with increased incidence in some family groups [7] and reports of concordance in identical twins. Despite extensive laboratory and clinical research, the etiology of keratoconus is poorly understood. It is thought to include biochemical, physical and genetic factors; however, no single proposed theory explains the various clinical features. It is, therefore, likely that the development of keratoconus is the final common pathway for several different disorders.
Criteria of Keratoconus Suspect
• Myopic children not corrected to 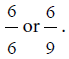
• Astigmatism more than (- 4.0) or more.
• History of frequent change of glasses.
• History of VKC.
• Family history of keratoconus.
• Had kerat
Materials and Methods
This study is a community based cross sectional analytical study conducted among the student of the basic school in 1st, 4th and 7th classes in Aljaded Althawra –Alkamleen locality– Aljazeera state – between November 2014 – April 2015
A total of 400 student were studied. This sample size of the study group was calculated uses this equation
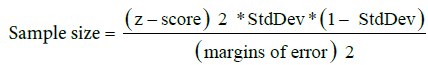
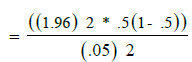
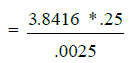
= 384.16
Parameters investigated included Includes in terviewing (patients’ demography, presentin g symptoms &duration, family history of ker atoconus, refractive error, past history of ker atoconus, vkc, wear spectacle & frequency of change or contact lens &its type), visual aq unity, clinical and slit-lamp microscopic exam inations all these done in field. Then patients had suspected kc according to kc suspect crit eria were referred to Makkah Omdurman eye hospital & AL Faisal eye center to do corne al Topography.
Data were statistically analyzed using the Statistical Package for the Social Sciences;
(SPSS) for windows, version 21. Results obtained were presented in tables and figures. Sensitivity and specificity of each criteria were obtain (Table 1).
| Positive (+) | Negative (-) | |
|---|---|---|
| Disease (+) | a | b |
| No Disease(-) | c | d |
Table 1: Sensitivity and specificity of each criteria were obtain.
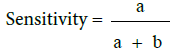
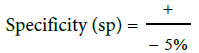
*Low sensitivity, high specificity: Positive test means the disease is likely. A negative test is not very helpful, because sensitivity is low
*High sensitivity, low specificity: Negative test means the disease is not likely. A positive test is not very helpful, because sensitivity is low.
*High sensitivity, high specificity: Ideal test. A positive test result means condition likely. A negative test result means condition is unlikely low.
The confidence interval of 95% and the P. value is ≤ 0.05, 0.05
stander deviation and major error (confidence interval) of 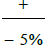 is used in this study. Ethical approval was obtained from locality
of state, research and Ethics committee of SMSB, and Makkah eye
hospital – Sudan.
is used in this study. Ethical approval was obtained from locality
of state, research and Ethics committee of SMSB, and Makkah eye
hospital – Sudan.
Results
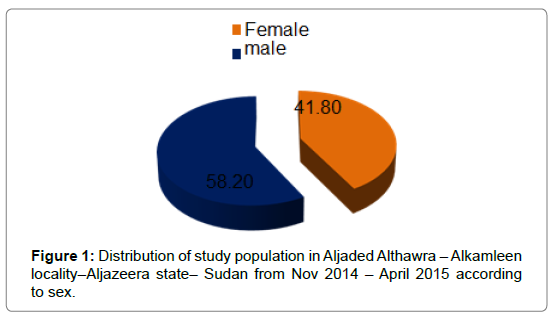
Total number of students in the area is 10374, males were 6300(60.7%) & females were 4074(39.3%) in 26 school (15 for boys & 11 for girls) 400 (800 eyes) students were examining in 6 school (3 for boys &3 for girls) whom were selected randomly. Males were 233(58.2%) while females were 167(41.8 %) (Figure 1).
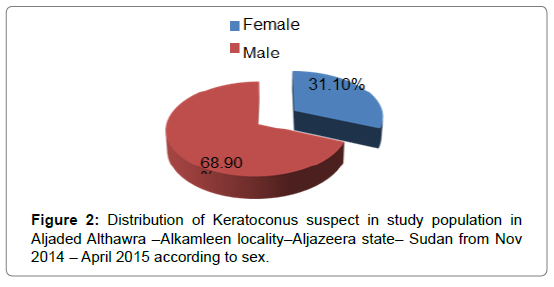
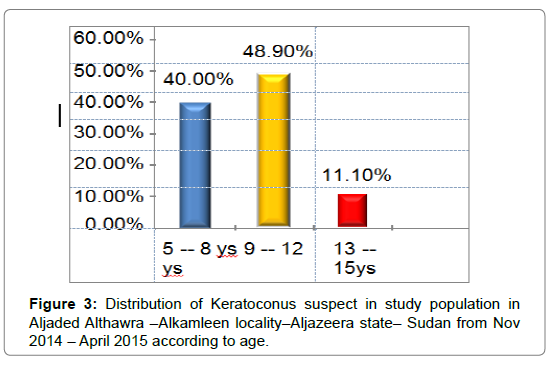
Forty-five (11.25%) students were found to have keratoconus suspect Criteria. Males were 31(68.9 %) while females were 14 (31.1%). (Figure 2) shows 18 of examined people aged from 5-8 (40.0%), 22 aged from 9-12(48.9%) and 5 aged from 13-15 (11.1%). (Figure 3) Peak’s age group was 9-12 years old (48,9%).
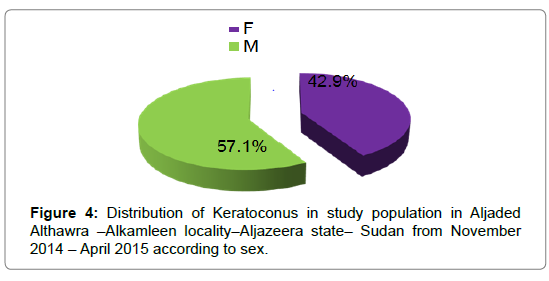
The risk factors that associated with keratoconus found in the study population include; Eye rubbing, Hx of wearing glasses, family history of refractive errors and wearing contact lens were found 32(71.1%), 14(31.1%), 14(31.1%) and 0(0.0%) of the study population respectively and were found 7(21.9%), 5(35.7%), 4(28.5%) and 0(0.0%) had keratoconus pattern respectively, (Table 2). Regarding the relationship between keratoconus suspect criteria and corneal topographic KCP. We found 14 eyes (15.5%) show positive KCP. Males were 8 eyes (57.1%) & females were 6(42.9%) (Figure 4). Peak age 5 - 8 (50 %) (Figure 5).
| Risk factor | F* | P* | KCP | |
|---|---|---|---|---|
| F* | P* | |||
| Rubbing eyes | 32 | 71 | 7 | 22 |
| Hx of wearing glasses | 14 | 31 | 5 | 36 |
| Family history of refractive errors | 14 | 31 | 4 | 29 |
| Hx of wearing contact lens | 0 | 0 | 0 | 0 |
| Note: *F = Frequency. P = Percentage | ||||
Table 2: Distribution of Keratoconus suspect in study population in AL jaded Althawra –Alkamleen locality–Aljazeera state– Sudan from Nov 2014 – April 2015 according to risk factors of KC.
Eleven eyes (14.5%) had VKC out of 76 eyes (84.4%) (Table 3).
Seven eyes (33.3%) had CVA less than normal 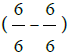 out of 21 eyes (23.3%) (Table 4). Six eyes (75.0%) had real cylinder (- 4.0) or more,
out of 8eyes (8.9%) (Table 5). Four eyes (28.6%) had KC in fellow eye
out of 14(15.6%) (Table 6). Zero eyes (0.0%) had family history of KC
& frequent change of glasses.
out of 21 eyes (23.3%) (Table 4). Six eyes (75.0%) had real cylinder (- 4.0) or more,
out of 8eyes (8.9%) (Table 5). Four eyes (28.6%) had KC in fellow eye
out of 14(15.6%) (Table 6). Zero eyes (0.0%) had family history of KC
& frequent change of glasses.
| KCP | VKC | |||
|---|---|---|---|---|
| +VE | -VE | Total | p | |
| +VE | 11 | 3 | 14 | 0.5 |
| -VE | 65 | 11 | 76 | |
| Total | 76 | 14 | 90 |
Table 3: Relation between KC & VKC of study population in Aljaded Althawra –Alkamleen locality–Aljazeera state– Sudan from November 2014 – April 2015.
| KCP | CVA | |||
|---|---|---|---|---|
| +VE | -VE | Total | P | |
| +VE | 7 | 7 | 14 | 0.01 |
| -VE | 14 | 62 | 76 | |
| Total | 21 | 69 | 90 |
Table 4: Relation between KC & CVA less than normal (6/6 -6/9) of study population in Al jaded Al thawra –Al kamleen locality– Aljazeera state– Sudan from Nov 2014 – April 2015.
| KCP | Cyl | |||
|---|---|---|---|---|
| +VE | -VE | Total | P | |
| +VE | 6 | 8 | 14 | 0 |
| -VE | 2 | 74 | 76 | |
| Total | 8 | 82 | 90 |
Table 5: Relation between KCP & Real cylinder (–4.0) or more of study population in AL jaded Althawra –Alkamleen locality– Aljazeera state– Sudan from Nov 2014 – April 2015.
| KCP | Fellow | |||
|---|---|---|---|---|
| Eye | ||||
| +VE | -VE | Total | P | |
| +VE | 14 | 0 | 14 | 0 |
| -VE | 0 | 76 | 76 | |
| Total | 14 | 76 | 90 |
Table 6: Relation between KCP & Fellow eye KC of study population in Aljaded Althawra –Alkamleen locality–Aljazeera state– Sudan from Nov 2014 – April 2015.
Regarding sensitivity and specificity of each criteria. VKC
had sensitivity of 79% & specificity of 14%. CVA less than normal 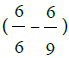 had sensitivity of 50% & specificity of 82%. Real cylinder
(- 4.0) or more had sensitivity of 43% & specificity of 97%. KC in fellow
eye had sensitivity of 29% & specificity of 87%. Family history of KC
and frequent change of glasses had sensitivity of 0% & specificity of
0% (Table 7).
had sensitivity of 50% & specificity of 82%. Real cylinder
(- 4.0) or more had sensitivity of 43% & specificity of 97%. KC in fellow
eye had sensitivity of 29% & specificity of 87%. Family history of KC
and frequent change of glasses had sensitivity of 0% & specificity of
0% (Table 7).
| Criteria | Sensitivity | Specificity |
|---|---|---|
| Hx VKC | 79% | 14% |
| CVA less than normal (6/6 – 6/9) | 50% | 82% |
| Real cylinder (- 4.0) or more | 43% | 97% |
| KC in fellow eye | 29% | 87% |
| Frequent change of glasses | 0% | 0% |
| Family history of KC | 0% | 0% |
Table 7: Demonstration of sensitivity & specificity of each criteria of study population in Aljaded Althawra –Alkamleen locality– Aljazeera state– Sudan from Nov 2014 – April 2015.
Discussion
Keratoconus has well-described clinical signs, but early forms of the disease may go undetected unless the anterior corneal topography is studied. Early disease is now best detected with video keratography. With the advent of computer-assisted corneal topographic analysis, the challenge has been to reliably quantify the minimal topographic criteria necessary for the diagnosis of keratoconus hat clinicians can use universally and reproducibly. This has become particularly relevant for ruling out early keratoconus when screening was done.
Aljaded althawra is located in the revolution north of the island with the boarder with the state of Khartoum and the region is home to a host of different Sudanese tribes. In this community based cross sectional analytical study, 400 students were examined whom were randomly selected of population in targeted age group. We found that 45 had keratoconus suspect criteria, 68.9% were males & 31.1% were females (Figure 2).
There are many risk factors associated with keratoconus. In this study one of the risk factors is rubbing eyes which were found in 32(71.1). Seven (21.9%) of them had positive topographic KCP (Table 2). Compare to 24.4% in a study from India by Agrawal et al., evaluated 274 patients of KC and revealed a higher prevalence of allergy in these patients [8]. Other risk factors were contact lens wearing but, in this study, no one had 0(0.0%) (Table 2). Also, there was 14(31.1%) had history of wearing glasses. Fourteen (31.1%) had family history of wearing glasses. Five (35.7%) & 4(28.5%) of them had positive topographic KCP respectively (Table 2).
In this study we found 45 (11.25%) had keratoconus suspect criteria, 14 eyes (15.5%) of them had positive topographic KCP. Show greater prevalence in males 8(57.1%) than females 6(42.9%) (Figure 5). Compare to two studies from north India [9,10] and one from western India [11] where keratoconus was noted more often in males. While the central India study found a higher prevalence in women [12].
We found in this study there is 76 eyes (84.4%) had VKC, 11eyes (14.5%) had positive topographic KCP (Table 3). And this result shows no relationship between VKC & KC (P value =0.5) opposite to Totan et al., studied the incidence of KC in VKC and found KC in 26.8% by quantitative evaluation of video- keratography (VKG) maps [13].
We found there are 21 eyes (23.3%) had CVA less than normal 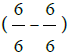 . (Table 4) and 14 eyes (15.6%) had KC in fellow eye (Table
6). Seven eyes (33.3%) and 4eyes (28.6%) respectively- had positive
topographic KCP. This result shows relationship between these
criteria and KC (p value =0.01). Founding these criteria in a patient
raises the possibility to get KC.
. (Table 4) and 14 eyes (15.6%) had KC in fellow eye (Table
6). Seven eyes (33.3%) and 4eyes (28.6%) respectively- had positive
topographic KCP. This result shows relationship between these
criteria and KC (p value =0.01). Founding these criteria in a patient
raises the possibility to get KC.
About the fourth criteria which characterize by high cylinder (- 4.0) or more in auto refractometer reading. We found 8 eyes (8.9%) had this criteria, 6 eyes (75%) of them had positive topographic KCP (Table 5). This result show strong relationship between this criteria and KC (p value =0.00) which raises the possibility to get KC. Regarding family history which is one of the criteria. In this study no one had this criteria 0 eyes (0.00%). Compare to The US Collaborative longitudinal Evaluation of Keratoconus study reported a rate of 13.5% and study from occupied Palestine where the prevalence is higher, it was 21.7%. About the last criteria which are frequent change of glasses. In this study no one had this criterion 0 eyes (0.00%).
In this study the sensitivity and specificity criteria show. VKC
had high sensitivity (79%) &low specificity (14%) this means KC is
not likely. The CVA less than normal 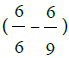 , real cylinder (- 4.0)
or more and KC in fellow eye had low sensitivity (50%, 43%, 29%
respectively) & high specificity (82%, 97%, 87% respectively). This
means KC is likely. The family history of KC & frequent change of
glasses had sensitivity of 0% & specificity of 0% (Table 7).
, real cylinder (- 4.0)
or more and KC in fellow eye had low sensitivity (50%, 43%, 29%
respectively) & high specificity (82%, 97%, 87% respectively). This
means KC is likely. The family history of KC & frequent change of
glasses had sensitivity of 0% & specificity of 0% (Table 7).
Conclusion
This study shows keratoconus among children between 5 -15
years old. In Aljded Althawra is 15.5%. In this study KC show greater
prevalence in males than females and peak age 5 -8 years. The risk
factors associated with KC in the study include, rubbing eyes, history
of wearing glasses and family history of wearing glasses. This study
shows strong relationship between keratoconus and high cylinder
(-4.0 or more) in auto refractometer reading, CVA less than normal 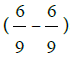 and KC in fellow eye. They can be used in diagnosis of KC because their sensitivity & specificity suggest KC. Also show
no relationship between VKC and keratoconus according to its
sensitivity & specificity.
and KC in fellow eye. They can be used in diagnosis of KC because their sensitivity & specificity suggest KC. Also show
no relationship between VKC and keratoconus according to its
sensitivity & specificity.
Recommendation
This research is a primary study with limited fund so we recommend further wide community-based studies in this population & in screening of keratoconus. As keratoconus is a treatable disease so we advise initiating national program for early detection and treatment to prevent complications and blindness and to encourage Ministry of education and health to introduce screening program of keratoconus as primary eye care in schools which done annually. Also, to provide corneal topography machine to all eye hospitals and to be included in National Health Insurance. We recommend to increase awareness among citizens about the importance of early detection of the disease.
References
- Krachmer JH, Feder RS, Belin MW (1984) Keratoconus and related noninflam- matory corneal thinning disorders. Surv Ophthalmol 28: 293-322.
- Rabinowitz YS (1998) Keratoconus. Surv Ophthalmol 42: 297-319.
- Tabbara KF (1999) Ocular complications of vernal keratoconjunctivitis. Can J Ophthalmol 34: 88-92.
- Kuo IC, Broman A, Pirouzmanesh A, Melia M (2006) Is there an association between diabetes and keratoconus? Ophthalmol 113: 184-190.
- Hammerstein W(1974) Genetics of conical cornea. Albrecht Von Graefes Arch KlinExp Ophthalmol 190: 293- 308.
- Edwards M, McGhee CN, Dean S (2001)The genetics of keratoconus. Clin Experiment Ophthalmol 29: 345-351.
- Zadnik K, Barr JT, Edrington TB, Everett DF, Jameson M, et al. (1998) Baseline findings in the Collaborative Longitudinal Evaluation of Keratoconus (CLEK) Study. Invest Ophthalmol Vis Sci 39:2537-2546.
- Agrawal VB. Characteristics of keratoconus patients at a tertiary eye center in India. J Ophthalmic Vis Res 6: 87-91.
- Fatima T, Acharya MC, Mathur U, Barua P (2010) Demographic profile and visual rehabilitation of patients with Keratoconus attending contact lens clinic at a tertiary eye care centre. Cont Lens Anterior Eye 33: 19-22.
- Sharma R, Titiyal JS, Prakash G, Sharma N, Tando R et al. (2009) Clinical profile and risk factor for Keratoplasty and develop- mental of hydrops in north India patients with keratoconus. Cornea 28: 367-370.
- Agrawal VB (2011) Characteristic of Keratoconus patients at a tertiary eye centre in india. J Ophthalmic Vis Res 6:87-89.
- Jonas JB, Nangia V, Matin A, Kulkarni M, Bhojwani K (2009)Prevalence and association of Keratoconus in rural Maharashtra in central India: The central India Eye Medical Study. Am J Ophthalmol 148:760-765.
- Totan Y, Hepşen IF, Cekiç O, Gündüz A, Aydin E (2001) Incidence of keratoconus in subjects with vernal keratoconjunctivitis: A videokeratographic study. Ophthalmol 108:824-827.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi