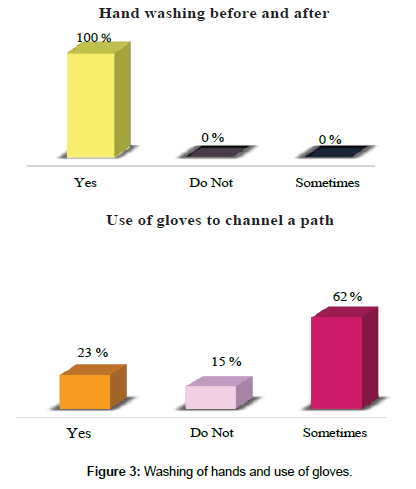Research Article, J Clin Image Case Rep Vol: 2 Issue: 1
Management of Peripheral Vascular Catheters by the Nursing Professional in Adult Patients of the Internal Medicine Area of the San Vicente De Paul Hospital
Tapia Paguay María Ximena1*, Castillo Andrade Rocío Elizabeth1, Montenegro Tapia Samantha Abigaíl2, Tito Pineda Amparo Paola1 and Imbaquingo Pozo Leidy Fernanda1
1Universidad Técnica del Norte UTN, Ibarra- Ecuador
2Universidad de las Américas UDLA, Quito-Ecuador
*Corresponding Author : Tapia Paguay María Ximena
Universidad Técnica del Norte UTN, Ibarra-Ecuador
Tel: +593 995171079; +593062615133
E-mail: mxtapia@utn.edu.ec; mariaxi_2@hotmail.com
Received: November 20, 2017 Accepted: February 06, 2018 Published: February 13, 2018
Citation: Ximena TPM, Elizabeth CAR, Abigaíl MTS, Paola TPA, Leidy IP (2018) Management of Peripheral Vascular Catheters by the Nursing Professional in Adult Patients of the Internal Medicine Area of the San Vicente De Paul Hospital. J Clin Image Case Rep 2:1.
Abstract
Intravenous access is one of the most frequent practice and a very important part of nursing work, and one of the problem that have caused many complications such as phlebitis and others. The objective of this study is to evaluate the management of peripheral vascular catheters by the nursing professional in adult patients of the area of internal medicine of quantitative, non-experimental design, of observational, descriptive and transversal type. A survey was applied to nursing professionals and an observation guide during the procedure; information was entered into a database in the Excel program; and their results were: 13 professionals surveyed; show that there is excellent knowledge in the application of standards of biosafety, antisepsis, salinization of pathway and care in catheter handling, according to the results of the observation guide with a sample of 82 patients, it was verified that there are norms that are not being fulfilled: How is it; leave the puncture site visible and cure the pathway, while compliance with the labeling of the route, change of circuits every 72 h, clean and dry catheter fixation, change of infusion solutions every 24 h and 19 phlebitis patients were identified. It is concluded that there is no relationship between the results of the survey and those of the observation guide since the nursing staff has knowledge about the correct management of the catheter but does not apply them completely to the patient.
Keywords: Peripheral venous catheter; Management; Nursing professional; Knowledge
Introduction
The use of the peripheral venous route is one of the procedures mostly used in the hospital institutions in order to have at the disposal of the health personnel a way of access for the attention of the patient during his hospital stay or during an emergency favoring the administration of medicines and the restoration of body fluids [1].
At present there are many patients and situations that can receive intravenous therapy. From the first day and until the end of a life, there is the possibility of applying it, using very varied locations with dwell times that can be short or prolonged, in medical and surgical care situations, as well as in the prevention and treatment of any health situation [2].
Peripheral venous catheters are the most frequently used devices for vascular access and although the incidence of local or systemic infections associated with their use is usually low, they cause great morbidity because of the frequency with which they are used [3].
Nursing professionals take an important part in this process. It is interesting to emphasize the fact that it is performed through peripheral venous vessels, as the mostly used for its versatility, to pose fewer serious complications and to be less bloody than other alternatives such as the one performed through central or arterial venous vessels, developing the nurses an intense activity around it and the responsibility that this type of procedures may be used for the patients [2]. Taking into account, points that will help to improve the time of permanence of the device in the patient avoiding complications:
a)Fixing method: The fixation with horizontal strip of plaster has not been able to be implanted in the CHUA (Albacete University Hospital Complex) and have indicated the need to return to the traditional "tie", provided that the tape does not fall on the point of puncture.
b)The salinization of the peripheral pathways every 8 h will be done with mono doses syringes of 3 cc saline.
c)Changes of serum system every 3 days [4].
General Objective
To evaluate the quality in the management of peripheral vascular catheters by the nursing professionals in an adult patients in field of internal medicine.
Specific Objectives
a)Describe the most common practices in the management of the peripheral venous catheter by the nursing staff.
b)Identify the main complications due to inadequate management of a peripheral venous catheter.
c)Establish parameters that help the nursing professional to correctly manage the peripheral venous catheter.
Methodology
The research was developed under a non-experimental quantitative, observational, descriptive and transverse cohort design. The Population and Sample constituted by all the professionals of nursing that work in the area of Internal Medicine of the Hospital San Vicente de Paul and adult patients hospitalized. The sample was randomly selected for convenience.
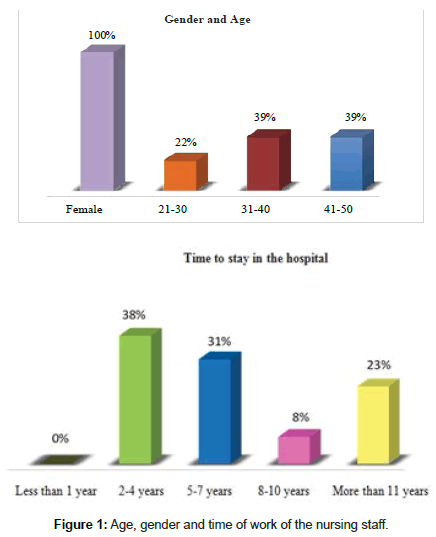
100% belong to the female gender of which 22% are between 21-30 years of age, 39% between 31-40 years and the same percentage for 41 to more years, related to working time in the area 38 % are working from 2 to 4 years, followed by 31% who work from 5 to 7 years and the rest work more than 11 years (Figure 1).
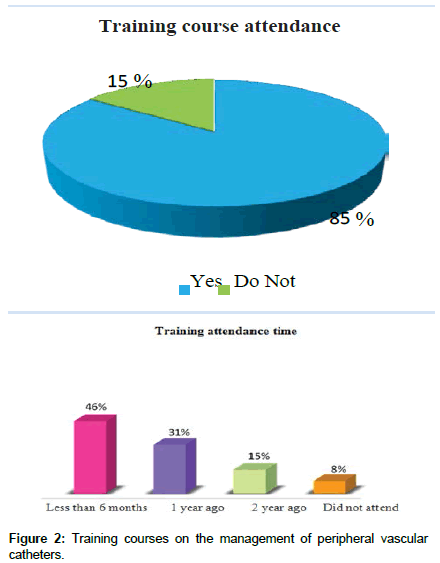
85% have attended training courses in this subject, while 15% have not attended this type of courses, in relation to the time of attending trainings 46% have a time of 6 months, on 31 % 1 year ago (Figure 2).
100% of the nursing staff perform hand washing before and after the application of the peripheral venous catheter, in 62% the use of gloves for this procedure is sometimes followed by 23% that if they use gloves at the time of channeling one way and finally 15% do not use gloves during the procedure, i.e., they are exposed to contact with patient fluids during the channeling (Figure 3).
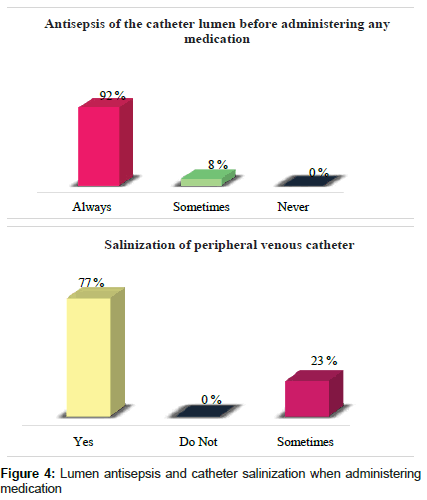
92% performed the antisepsis of the lumen of the peripheral venous catheter at the time of administering with some medication followed by 8% sometimes performed; in addition 77% performed the venous catheter salinization followed by 23% (Figure 4).
77% wash the route with 10 ml of saline solution 0.9%, with 3 ml, in a similar percentage of 8% and in the same way 8% does not perform the washing of the route, in the following Figure 54% monitor the catheter each administering medication, followed by 45% do it each shift (Figure 5).
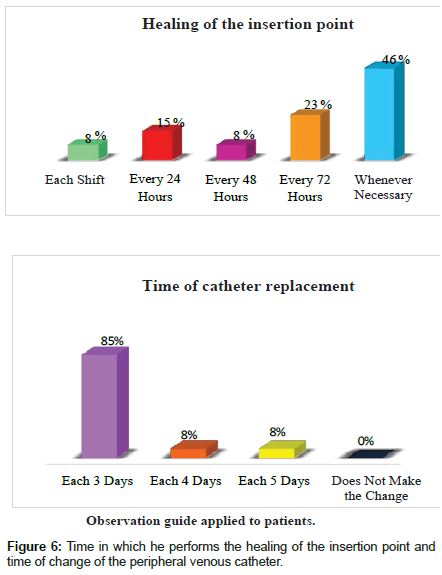
Performs the peripheral venous catheter insertion point every time it is necessary, followed by 23% who do it every 72 h, 15% every 24 h and lastly 8% do it every shift and every 48 h. Regarding the time to change the venous catheter, 85% performed the change every 3 days followed by 8% who performed every 4 days, in the same percentage they performed every 5 days (Figure 6).
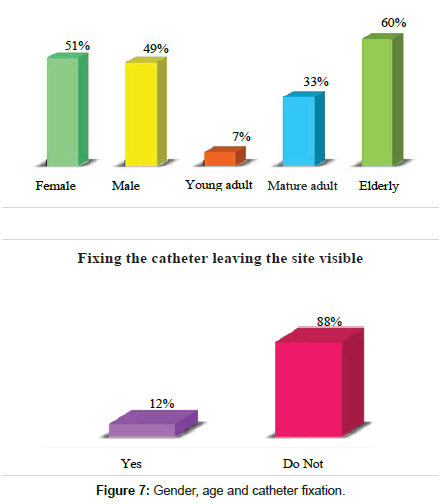
A percentage of 51% belong to the female gender, while in 49% belong to the male gender, regarding the catheter fixation 88% that according to the fixation of the catheter did not leave the puncture site visible while 12% if they left the puncture site visible (Figure 7).
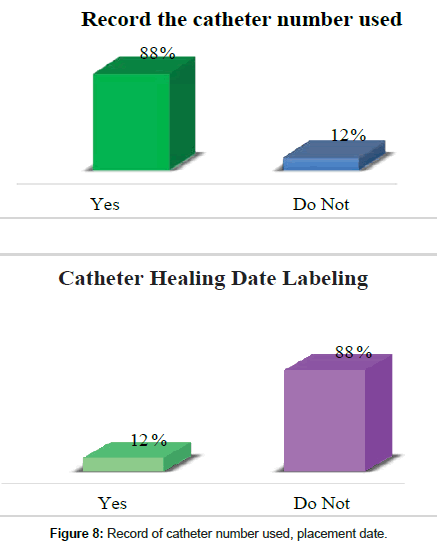
88% if they correctly register the catheter number used, date of placement, time and initials of the person in charge while 12% do not perform or the registry is incomplete. In 88%, the peripheral venous catheter cutoff date was not applied, while 12% labeled the pathway healing date (Figure 8).
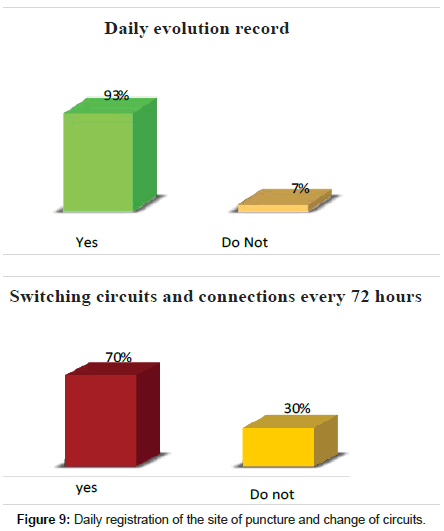
93% did the correct registration of the puncture site on the nursing sheet in this case the evolution sheet, while 7% did not register the puncture site; that 70% if they make the change of circuits and connections every 72 h as established by the norm, while 30% do not make the change or make the change after 72 h (Figure 9).
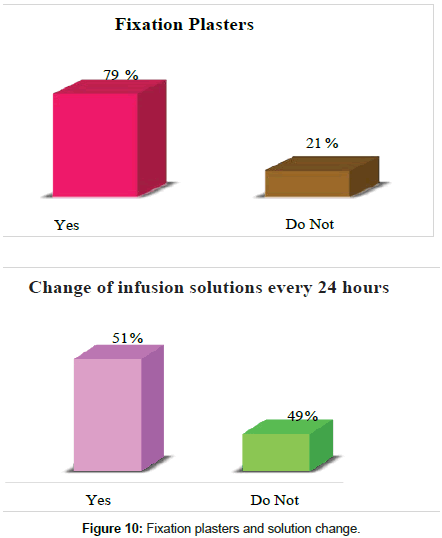
79% of the patients had clean and dry catheter fixation plasters while 21% did not, 51% had infusion solutions every 24 h and 49% did not have the solution. Infusion changed (Figure 10).
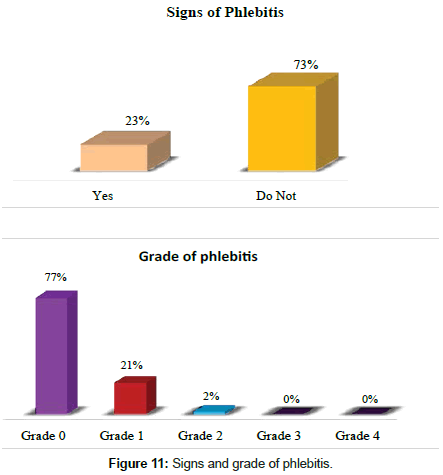
In 73%, there are no signs of phlebitis at the puncture site, where as in 23%, signs of phlebitis are observed. Regarding the phlebitis scale, 77% did not present phlebitis while 21% had phlebitis grade 1; i.e., with erythema with or without pain in the access area, with 2% having phlebitis grade 2 pains in the access area with erythema or edema (Figure 11).
Discussion
Continuous and periodic training of nursing professionals should be clear and specific objective of the authorities in peripheral venous catheter placement, 71% of nurses and nursing assistants have not received any training regarding management of venous catheters, peripheral intravenous catheters, thus this indicates a considerable degree of ignorance regarding the catheter management activities that should be performed by professional nurses and nursing auxiliaries [5]. As compared to this study, in our institution most of the professionals are trained in the management of the peripheral venous catheter, while a low percentage is not trained i.e. their knowledge is reduced according to this topic. Teaching should be conducted within a period of no more than one month, which allows the care provided to the patient should be safe, effective, efficient and timely [6]. Staff should correctly apply biosecurity standards at the time of channeling and management of a peripheral venous catheter, according to WHO [7]. Hand hygiene is the primary measure of reducing infections. The biosecurity measures applied by the nurse in the peripheral route canalization in the emergency services applied to 30 nursing professionals, of whom 50% performed hand washing before and after the procedure and the other 50%, did not wash of their hands [8]. The safe use of gloves in venipuncture by nursing workers shows that the 20 people observed, 45% of the workers used gloves in the execution of said procedures and another 55% did not use them, the reasons for the majority of nurses do not use gloves in the execution of peripheral venous puncture: inadequate adaptation of the material in terms of size and loss of tactile sensitivity; excess of activities and shortage of workers, lack of continuous education in the services, perception of self-sufficiency due to developed ability that leads to consider that the activity of peripheral venous puncture poses no risk to health, even knowing this is important to protect oneself from the fluids emitted by the patient [9]. In the protocol of the Puerto Montt clinic in Chile published in 2011 establishes that the connections and accesses with valve should be disinfected with alcohol to 70% prior to the administration of medications or the insertion of a connection , this means to say that in the institution there is a high percentage of nursing professionals that if they applies the norm and complies with the established protocols for the management of venous catheters peripherals while in a low percentage, they only performs it in some occasions, and they ignore the norm although they knows it very well the complications that can lead to this activity not being performed [10].
It is suggested that the application of catheter irrigation with 0.9% saline solution aims at maintenance of catheter permeability and according to recommendations of the Infusion Nursing Society (INS) this irrigation should occur in the following situations: after collection of blood samples through the peripheral venous catheter, before and after administering incompatible solutions or medication, always after the administration of medications, after intermittent therapies and when the patient does not need continuous infusion of fluids, this activity is one of the more important because it is the one that keeps the catheter permeable while it is in the patient without continuous hydration [11].
The recommendation of the 5 ml syringe is dictated by the fact that syringe with this volume and above this size have a small pressure, which is important to reduce the possibility of vessel injury, the nursing professionals surveyed have a low knowledge about the salinization of the route especially in the amount with which it is performed, since in this institution most of the medication is administered diluted [11].
Look for signs of phlebitis through observation and assess puncture site in search of signs of phlebitis every 8 hours: heat, pain, redness, increase in volume, daily and whenever it is appropriate to administer a drug, i.e. the majority of nursing professionals are meeting the standard of monitoring catheter patency, and the other part is doing so but in a wrong way [12]. It is suggested that the insertion point will be palpated through the cuff every 24 h and in case of pain or fever not affiliated the cure will be lifted, the dressings of the peripheral venous catheters will be changed every 72 h. The dressing will also be changed when it is dirty, wet or detached, there are different studies that claim that the less manipulation there is in the pathway the less risk of phlebitis, that is to say that in our institution most of the professionals are meeting the norm since they perform healing only when necessary [13]. suggest that there is no need to replace peripheral catheters more frequently than every 72-96 h to reduce the risk of infection and phlebitis in adults, in the institution applied the surveys in a greater percentage have knowledge about the change of peripheral venous catheter each 3 days, the other percentage do so on the fourth or fifth day due to lack of material in the institution [14].
In continuing the discussion about the results obtained in this study, the observation guide performed in the investigation was referred in the protocol of maintenance of venous routes of Spain that to fix the catheter to the skin and to avoid mobilizations with the consequent entry of germs to the blood flow, transparent dressing or a tie with adhesive strips that must be sterile to meet the recommended asepsis criteria. As for the ties must be taken into account that in their placement is not covered the insertion point to be inspected, in this case the institution and the service applied the observation guide did not have the supplies i.e. the dressing transparent to fix the catheter for such reason the insertion point [15] was not visible.
In article standards for the use of continuous venous therapy suggests to record in a visible place the date of placement and healing of the catheter. The majority of nursing professionals do not perform this activity because they report that between less catheter manipulation and less phlebitis, or if they perform the cure but do not record the healing date with the initials of the person who performed it, so does another research which results in 77% of nurses do not register corresponding, 23% if it registers the procedure and stresses that: the nursing record integrates the process of management and evolution of the procedure and care of the patient: jointly leaves written record of the act of attention that reflects the professional practice. The clinical history of the patient is a legal document and therefore all activities should be recorded in detail, i.e., if the catheter is permeable, if the route was reanalyzed and the scoring of the phlebitis scale [8].
Systematic change of the peripheral intravenous catheter every 72 h in adults is recommended in children and at-risk catheters are not recommended because routine replacement does not prevent infection. Most professionals do the change at 72 h complying with the protocol of management of the peripheral venous catheter, in a low percentage do not make the change, i.e., they perform after 72 h professionals say that it is difficult to comply with the norms since they do not have the sufficient inputs for the patients [14]. According to a study where 36.4% of patients hospitalized with venoclisis have phlebitis and 63.6% do not. However, it is worrying that there are still a percentage of patients who have phlebitis, so we must as nurses consider solutions, taking into account that phlebitis arises primarily from a physical, chemical or mechanical rather than an infectious phenomenon.
The safety of the patient as a priority in the processes, is the basis of health care today, without forgetting the safety of health professionals, it can be deduced that the patient who enters the hospital is exposed to a series of diseases, being it is important for the nursing professionals to have scientific knowledge in carrying out their procedures and to comply with appropriate aseptic standards [12].
Conclusion
a)100% belong to the female gender whose average age ranges from 36 to 40 years, of which 38% are working from 2 to 4 years in the institution, followed by 31% labor from 5 to 7 years, with 23% working for more than 11 years.
b)85% of nursing professionals have attended training courses while 15% have not attended; of those who have attended there is a high percentage that are trained constantly in a time less than 6 months.
c)According to the results of the survey, there is a high percentage that shows that the nursing professionals has a good knowledge of the application of biosecurity, antisepsis, salinization and care related to the management of the peripheral venous catheter, contributing to the decrease in incidence of phlebitis and complications with phlebitis.
d)The same does not happen with the results of the observation guide since it was noted that there are standards that are not being fulfilled in their entirety, such as: leaving the puncture site visible, labeling cure date, while there is a high percentage in compliance with the registration of the number of catheter used, date of placement, time and initials of the person in charge, change of circuits and connections every 72 h, clean and dry catheter fixation plasters, change of infusion solutions every 24 h.
e)We identified 19 patients with signs of phlebitis, i.e., 23% of the sample of which 21% had phlebitis grade 1 and 7% phlebitis grade 2.
f)There are contradictions between the results of the survey and those of the observation guide since nurses have knowledge about the correct management of the catheter but do not apply them completely to the patient. This is because the hospital does not have the materials needed to fulfill these activities.
g)Nursing professionals in the area of internal medicine at the Hospital San Vicente de Paúl with the socialization of results of this research is committed to comply with the protocol of management of the peripheral venous catheter and thus improve care for patients by decreasing the incidence of phlebitis in this area.
Acknowledgement
a)To the authorities of the Hospital San Vicente de Paúl, for the opening for the realization of this study.
b)To the nursing staff for the collaboration in the surveys and in the observation sheet.
c) Patients for openness in this research.
References
- Nursing Coordination (2012) Peripheral venous catheter insertion guide. Clinic of the University of the Sabana.
- Juan Carlos Bellido Vallejo MICG (2006) Guide of care in peripheral venous accesses and central peripheral insertion. General Nursing procedures and protocols.
- Herrera C (2015) Procedure for the installation of peripheral venous maintenance. Network Regional Clinics.
- Del Ejido Fernández MDLCCNBRA (2012) Channeling, maintenance and use of peripheral venous via. Protocol of Nursing.
- Gallardo Y (2013) Nursing care in the management of peripheral and central catheters.
- Véliz E, Fica VT (2014) Evaluation of conditions of management of peripheral catheters in adult patients. Rev Chilena Infectol 31: 666-669.
- Health Omdl (2010) Peripheral catheters. WHO.
- CACR (2013) Incidence of phlebitis in hospitalized patients with venoclisis-medical services. Private University Antenor Orrego.
- LCG (2012) Peripheral vein maintenance.
- Huelin Maciá TM, MdlP (2011) Maintenance of venous lines. Library of houses.
- Dopico Silva L, Oliveira Tinoco F (2007) Recommendations for the use of saline solution 0.9% in perineal venous catheters. Semiannual Electronic J Nursing.
- And DO (2014) Protocol for the prevention of physical, chemical and infectious phlebitis in sampling.
- Moros M (2006) Participation of the Nursing Professional in the prevention of phlebitis in hospitalized patients. Caracas
- Ciccioli F, Peak JL (2011) Guidelines for the Prevention of Intravascular Catheter-Related Infections, 2011. Centers for Disease Control and Prevention.
- Ministries of Health, Social Services and Equality (2014) Clinical Practice Guidelines on Intravenous Therapy with Non-Permanent Devices.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi