Short Communication, J Physiother Rehabil Vol: 3 Issue: 2
Narrative-based Medicine for Development of Home Exercise to Prevent Surgery in Hip Osteoarthritis: Consideration of Pericapsular Soft Tissue as a Pain Generator
Kazuo Hayashi1* and Toshiharu Tsunoda2
1Arthritis Center, Fukuoka Wajiro Hospital, Fukuoka, Japan
2Department of Orthopedic Surgery, Asama General Hospital, Nagano, Japan
*Corresponding Author : Kazuo Hayashi
Department of Arthritis Center, Fukuoka Wajiro Hospital, Fukuoka, Japan
Tel: +8109045169461
Fax: +810926915315
Email: hayashis@giga.ocn.ne.jp
Received Date: 13 May, 2019; Accepted Date: 30 May, 2019; Published Date: 5 June, 2019
Citation: Hayashi k, Tsunoda T (2019) Narrative-based Medicine for Development of Home Exercise to Prevent Surgery in Hip Osteoarthritis: Consideration of Pericapsular Soft Tissue as a Pain Generator. J Physiother Rehabil 3:2.
Abstract
In many cases of hip osteoarthritis (OA), patients exhibit symptoms that are discordant with radiography and magnetic resonance imaging findings. We have observed two distinct types of pain in hip OA: motion pain and walking pain. Motion pain typically improves with exercise therapy, whereas walking pain may require surgery. Many patients with motion pain have Kellgren-Lawrence grade 3 or 4 findings. Therefore, the combination of narrative-based medicine and evidence-based medicine is important for selecting the most suitable treatment for patients with hip OA.
Keywords: Hip osteoarthritis; Home exercise; PSTR exercise; Harris Hip Score (HHS)
Limitations of Evidence-based Medicine in hip OA
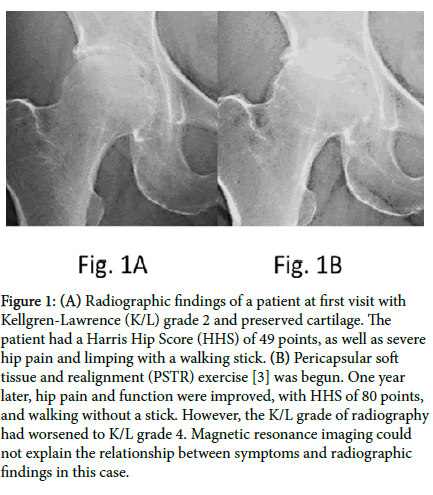
A major problem at our clinic during patients’ first visit is their understanding of the explanation of their hip pain received at hospitals they have visited previously. Most patients with hip osteoarthritis (OA) have received advice from doctors explaining that the exposed subchondral bone secondary to loss of cartilage from the joint surface is contacted, causing hip pain that can only be relieved by surgery. We always consider whether this is indeed the case, because we have observed many cases of patients with contact of the subchondral bone secondary to complete loss of cartilage who report no hip pain and no limitations in activities of daily living. In addition, we observed a patient with hip OA in which radiographic findings at first visit indicated Kellgren-Lawrence (K/L) Grade 2 [1], with preserved cartilage (Figure 1A).
Figure 1: (A) Radiographic findings of a patient at first visit with Kellgren-Lawrence (K/L) grade 2 and preserved cartilage. The patient had a Harris Hip Score (HHS) of 49 points, as well as severe hip pain and limping with a walking stick. (B) Pericapsular soft tissue and realignment (PSTR) exercise [3] was begun. One year later, hip pain and function were improved, with HHS of 80 points, and walking without a stick. However, the K/L grade of radiography had worsened to K/L grade 4. Magnetic resonance imaging could not explain the relationship between symptoms and radiographic findings in this case.
This patient had a Harris Hip Score (HHS) [2] of 49 points, and exhibited severe hip pain and limping with a walking stick. Pericapsular soft tissue and realignment (PSTR) exercise [3] was begun. One year later, hip pain and function were improved, resulting in HHS of 80 points, and walking without a stick. However, the K/L grade based on radiography had worsened to Grade 4 (complete loss of cartilage, Figure (1B). Magnetic resonance imaging findings were not able to explain the relationship between symptoms and radiographic findings in these cases. Overall, we have found that many patients’ problems cannot be explained by evidence-based medicine in hip OA.
Narrative-based Medicine in Hip OA
We have analyzed the details of patients’ complaints over 12 years, revealing the following mechanisms of hip pain:
A: Motion pain
1: Patients have either no pain or very slight pain on some days.
2: Patients complain of hip pain while standing and when taking the first few steps, with decreased hip pain as they continue walking.
3: Patients who walk for more than 20 minutes each way for work, in addition to bus, subway, or train travel, either have no pain or very slight pain during walking to work in the morning. However, they complain of hip pain while walking home from work or during the evening at home, and sometimes experience intense thigh pain or calf pain at night.
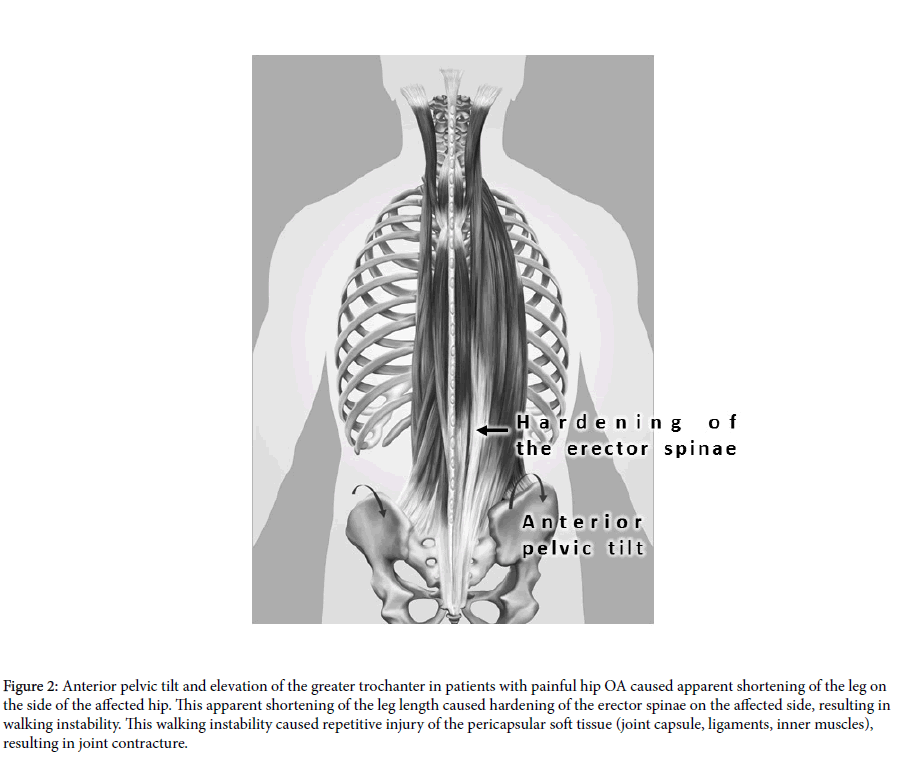
4: Motion pain appears to result from joint contracture. Anterior pelvic tilt and elevation of the greater trochanter in patients with painful hip OA causes apparent shortening of the leg on the side of the affected hip. This apparent shortening of leg length causes hardening of the erector spinae on the affected side, resulting in instability while walking (Figure 2). This walking instability causes repetitive injury of pericapsular soft tissue (joint capsule, ligaments, inner muscles), resulting in joint contracture. Moreside et al. reported the effects of the erector spinae in patients with moderate to severe hip OA [4].
Figure 2: Anterior pelvic tilt and elevation of the greater trochanter in patients with painful hip OA caused apparent shortening of the leg on the side of the affected hip. This apparent shortening of the leg length caused hardening of the erector spinae on the affected side, resulting in walking instability. This walking instability caused repetitive injury of the pericapsular soft tissue (joint capsule, ligaments, inner muscles), resulting in joint contracture.
B: Walking pain
1: There are no days on which patients have no pain or very slight pain.
2: Patients complain of more intense hip pain during walking than pain while standing and when taking the first few steps.
3: Patients who walk for more than 20 minutes each way for work in addition to bus, subway, or train travel, have moderate to severe walking pain while walking to work in the morning. Sometimes these patients need a stick, or to rest while walking. They have walking pain for most of the day.
4: Walking pain is caused by contact with the subchondral bone secondary to loss of cartilage from the joint surface. Patients with severe walking pain may require surgery.
PSTR exercise can improve pain and functioning in patients with motion pain, whereas patients with walking pain typically require surgery. Many patients with motion pain have radiographic findings of K/L Grade 3 or 4. We have reported that symptoms improved markedly as a result of PSTR exercises in patients with K/L Grade 3 or 4 in which joint cartilage was lost [3]. Radiographic findings are unable to determine the indication for exercise therapy or surgery. In a previous study, we reported that a narrative-based approach with patients is necessary for determining an indication for exercise therapy or surgical treatment [5]. In another study, we found no difference in magnetic resonance imaging findings between patients with motion pain and those with walking pain in a sample of 1077 patients [3].
Consideration of Pain Generators in OA
Previous studies reported that bone-related causes of pain in OA include subchondral microfracture, bone stretching with elevation of the periosteum due to osteophyte growth, bone remodeling and repair, bone marrow lesion, and bone angina caused by decreased blood flow and increased intra-osseous pressure [6]. The subchondral bone and synovium may be responsible for nociceptive stimulation, and peripheral neuronal sensitization is an important feature, resulting in pain during daily activities such as walking [7]. Witt et al. [8] conducted a review, reporting that, in animal studies, the subchondral bone was innervated with substance P immunoreactive nociceptive fibers that may be involved in pain generation in OA. However, Fortier et al. [9] reported that the normal subchondral bone nerve supply was obliterated in areas of advanced arthritis, with cartilage loss, bony eburnation, and cyst formation. In addition, hypercellular infiltrates in cystic cavitations in the subchondral bone stained intensely for substance P, but true neurofilaments were found to be absent in horses.
We propose that further investigation regarding potential differences in the mechanisms between motion pain and walking pain will be important for determining the most suitable treatment for each patient. The relationship between the characteristics of hip pain (motion pain or walking pain) and innervation of the subchondral bone should be investigated in future studies.
Conclusion
The combination of narrative-based medicine and evidence-based medicine is important for selecting the most suitable treatment for each patient with hip OA.
Acknowledgment
The PSTR exercises were ones in books published by Teruo Ooyati (Osaka, Japan). We thank Benjamin Knight, MSc., from Edanz Group for editing a draft of this manuscript.
References
- Kellgren JH (1957) Radiological assessment of osteoarthrosis. Ann Rheum Dis 16: 494-502.
- Harris WH (1969) Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J Bone Joint Surg Am 51: 737-755.
- Hayashi K (2018) Dramatic effects of new home exercises for patients with osteoarthritis of the hip: pericapsular soft tissue and realignment exercises. J Physiother Phys Rehabil 3: 162-173.
- Moreside J (2018) Altered erector spinae activity and trunk motion occurs with moderate and severe unilateral hip OA. J Orthopaed Res 36: 1826-1832
- Hayashi K (2019) New strategies for development of home exercise to prevent surgery in patients with hip osteoarthritis: considerations of pericapsular soft tissue as a pain generator. Acta Scientific Orthpaedics 2: 14-19
- Salaffi F (2014) The sources of pain in osteoarthritis: a pathophysiological review. Reumatismo 66: 57-71
- Dieppe PA (2005) Pathogenesis and management of pain in osteoarthritis. Lancet 365: 965-973
- Witt (2014) The anatomy of osteoarthritic joint pain. Clin Anat 27: 451-454.
- Fortier LA (1997) Distributional changes in substance P nociceptive fiber patterns in naturally osteoarthritic articulations. J Rheumatol 24: 524-530.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi