Research Article, J Vet Sci Med Diagn Vol: 7 Issue: 1
Our Approach to Intervertebral Disc Disease in Dogs: A Review of the Current Literature
Nikola Heblinski1* and Hugo Schmökel2
1Veterinary, Resident ECVS, Evidensia Specialistdjursjukhuset Strömsholm, Djursjukvägen 11, 73494 Strömsholm, Sweden
2Chief Veterinarian, Diplomate ECVS, Phd, Evidensia Specialistdjursjukhuset Strömsholm, Djursjukvägen 11, 73494 Strömsholm, Sweden
*Corresponding Author : Nikola Heblinski
DVM, Resident ECVS, Evidensia Specialistdjursjukhuset Strömsholm, Djursjukvägen 11, 73494 Strömsholm, Sweden
Tel: +0046 220 458 00
E-mail: nikola.heblinski@gmx.de
Received: December 19, 2017 Accepted: January 19, 2018 Published: January 24, 2018
Citation: Heblinski N, Schmökel H (2018) Our Approach to Intervertebral Disc Disease in Dogs: A Review of the Current Literature. J Vet Sci Med Diagn 7:1. doi: 10.4172/2325-9590.1000246
Abstract
Intervertebral disc disease is a common disorder affecting the spinal cord of canine patients. The clinical appearance of intervertebral disc disease can vary significantly and outcome as well as prognosis may be strongly dependent on the location, the severity and the duration of the disease. Over the past 60 years a lot of research had been done on this topic in order to achieve a better understanding and also to improve the treatment options and outcome of intervertebral disc diseases in dogs. This review summarizes the clinical appearance, the classification system, diagnostic possibilities, surgical intervention and prognosis and gives a broad overview over the current literature on intervertebral disc diseases in our canine patients.
Keywords: Intervertebral disc disease; Dogs; chondrodystrophic; Hansen type
Introduction
In the 1950ies ground setting work was published regarding intervertebral disc disease (IVDD) in dogs. Olsson and Hansen, both working at the University of Stockholm, presented their results of extensive clinical and histological investigations in mainly chondrodystrophic patients with IVDD [1,2]. This data was later widened by the work of Funkquist introducing surgical decompression of intervertebral disk extrusions (IVDE) using a laminectomy, and comparing these surgical results with conservative treatment of dogs affected by an IVDE [3,4]. Since then, numerous publications have provided more clinical knowledge and led to modifications of decompression techniques; but still little has been changed in the clinical approach of IVDE. Recently, however, new research using advanced imaging techniques has given more detailed descriptions of the different variations of the disease. This has further improved the prognostic accuracy of treatment and outcome. Therefore, it is the objective of this review to summarize current published data and evidence for the classification, prognosis and treatment of IVDE in dogs.
Classification of IVDD and IVDE in Dogs
The main work of Hansen is based on the histology of degenerated intervertebral discs in chondrodystrophic dogs and is still valid and in use [5]. According to Hansen, complete ruptures of the annulus fibrosus (AF) with extrusion of nucleus pulposus (NP) are classified as Hansen type 1 (IVDE); while partial ruptures of the AF with some degree of AF protrusion are classified as Hansen type 2 (IVDD) [1].
IVDE Hansen Type l
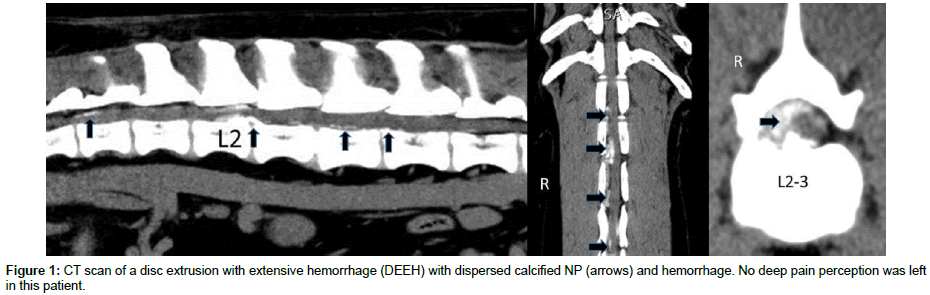
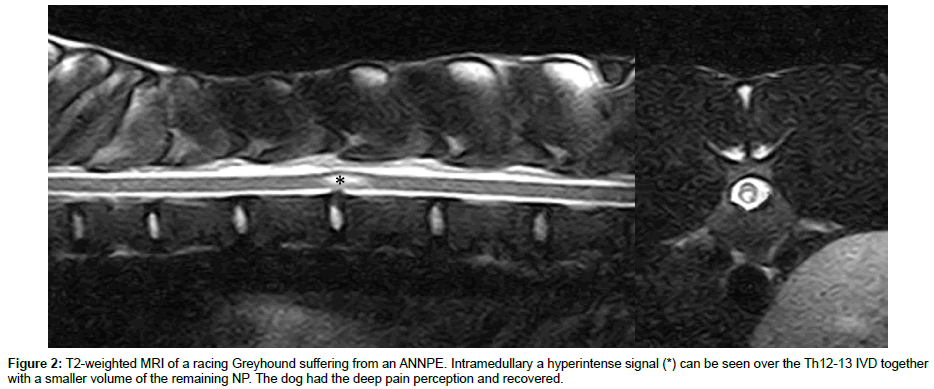
Funkquist introduced 1962 a sub-classification of the Hansen type l based on the length of dispersion of the extruded NP. She proposed three subtypes, subtype l and 2 with only a short dispersion of extruded NP within the spinal canal and subtype 3 with a longer dispersion over three or more vertebrae. Recently, in a study using MRI scans, subtype l and 2 have been described as nondispersed and dispersed IVDE respectively [6]. Further, patients with a herniation classified as subtype 3 have shown a poorer outcome when treated conservatively, in comparison to subtype l and 2 [3]. A very similar form of the Funkquist IVDE type l subtype 3, with long dispersion of NP, has been described clinically and myelographically by Tartarelli and co-workers [7]. Myelography in these patients showed significant compression of the spinal cord over several vertebrae, making extensive hemilaminectomies necessary to relieve the compressed nervous tissue. Tartarelli and co-workers intraoperatively found considerable hemorrhage within the epidural space. Therefore, the term disk extrusion with extensive hemorrhage (DEEH) was proposed for the Funkquist IVDE type l subtype 3 [7]. To identify the extrusion of NP and bleeding in DEEH, computed tomography (CT) has been described to be a reliable diagnostic technique (Figure 1) [8]. According to some studies, a smaller percentage of patients with DEEH recover in comparison to patients with the classical Hansen type l IVDE (subtype 1 and 2) [3,9]. The necessity of extensive decompression in many cases of DEEH and the severity of the clinical signs makes it reasonable to categorize the DEEH as a different clinical entity of the Hansen IVDE type l (Table 1). Another form of Hansen type 1 IVDE described in the literature is the acute IVDE of non-degenerated NP. This has been observed in both dogs and cats. In the event of trauma, the AF of the disc can acutely rupture and viscous non-degenerated NP extrudes under significant pressure, leading to intramedullary contusion damage, often with severe clinical signs. Two subtypes have recently been described; the acute non-compressive nucleus pulposus extrusion (ANNPE) and the intradural/intramedullary IVDE (IIVDE) [10]. In most cases of ANNPE, no residual NP is identified during imaging, making a surgical decompression ineffective [11]. But in an event of IIVDE sometimes intradural nucleus material can be found, making a surgical intervention necessary. Dogs and cats with an acute IVDE should therefore be assessed with an MRI to detect any intramedullary changes (Figure 2). Should there be a loss of deep pain perception (DPP) and a hyperintense intramedullary signal found in a T2-weighted sequence of the MRI, the prognosis is guarded [6,12,13]. This form of traumatic IVDE has in the literature also been called high velocity-low volume IVDE, and sometimes Hansen type 3 [11,14,15].
| Type | Name in Literature | Extruded Material | Clinical Features |
|---|---|---|---|
| Type 1 a | Hansen type 1 Subtype 1 and 2 |
Degenerated NP | Acute to slow progressing onset, mainly chondrodystrophic breeds |
| Type 1 b | DEEH Hansen 1 subtype 3 Dispersed IVDE |
Degenerated NP | Peracute/acute onset, often severe symptoms, NP often over 3 or more vertebrae |
| Type 1 c | ANNPE, Traumatic IVDE, High velocity-low volume IVDE, Hansen 3 |
Non-degenerated NP | Peracute onset with trauma, often severe symptoms |
| Type 1 d | IIVDE | Non-degenerated NP | Peracute onset with trauma, often severe symptoms |
| Type 1 e | HNPE | Mildly degenerated NP | Peracute/acute onset, often no pain, mainly in the cervical spine |
| Type 1 f | Far lateral IVDE | Degenerated NP | Radicular pain |
Table 1: Summary of the different common forms of IVDE Hansen type l.
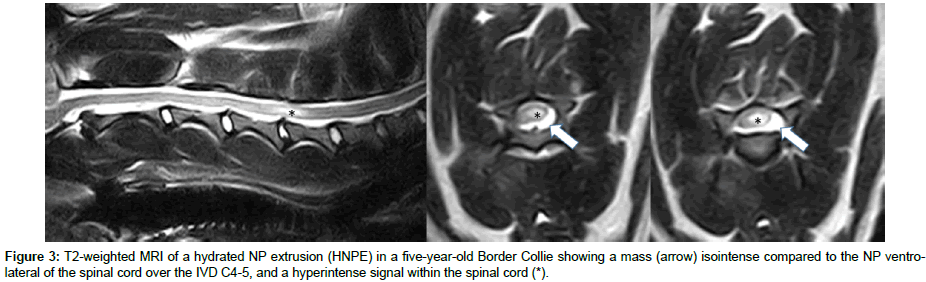
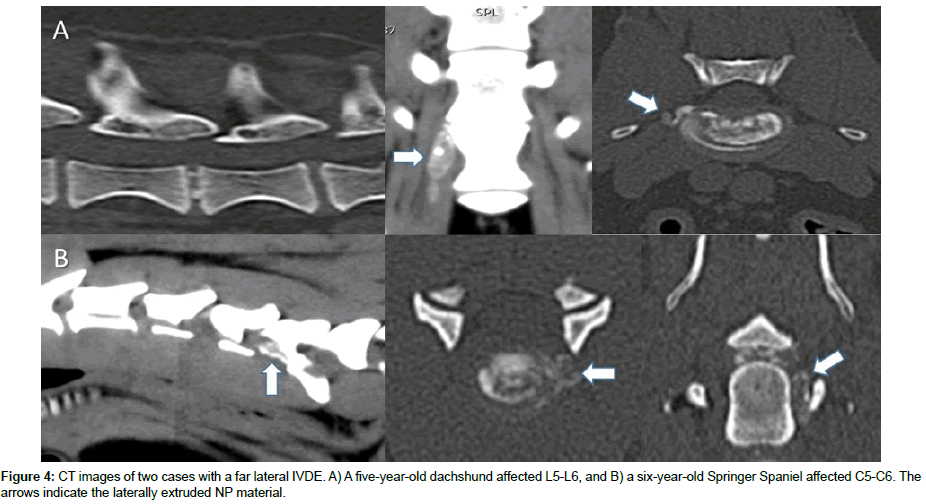
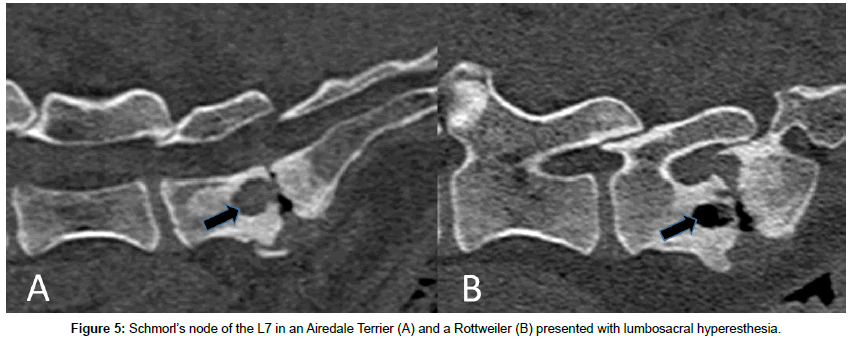
Another documented variation of canine IVDE, regarding the degenerative state of the extruded NP and the clinical features and treatment, is the hydrated NP extrusion (HNPE). More than 50 cases have been published of this type of herniation [16-21]. All cases, with one exception, were diagnosed in the cervical area and clinically most of them have a peracute/acute onset presented with severe signs (tetra paresis/paralysis). Remarkably no pain, or only mild pain, was observed and reported [16-18,20]. MRI has been shown to be the diagnostic imaging technique of choice in these cases, since the extruded NP is not mineralized and can therefore be difficult to assess with computer tomography (CT). The extruded NP mass is visible in MRI scans mostly ventral to the spinal cord with the same signal intensity as the NP (hyperintense in T2-weighted images), resulting in a mild to moderate ventral cord compression (Figure 3). The fast onset of signs in these patients suggests a pressurized extrusion with strong contusion of the spinal cord, often resulting in a hyperintense intramedullary signal in the T2-weighted sequence (Figure 3). Outcome of the reported cases has been shown favorable with both surgery and conservative treatment [16-21]. Extruded NP material from these patients showed viscous properties, and histologically mild degenerative signs [21]. When conservatively treated cases were rescanned after four weeks, the extruded NP material was absorbed which may explain the fast recovery shown in patients with a HNPE [19,20]. In 2013 Fadda described a Hansen IVDE type l to the lateral side of the IVD compromising the nerve root and the nerve passing through the foramen (Figure 4). This form of IVDE was in the publication named a far lateral disc extrusion [22]. Patients with a far lateral disc extrusion are presented with radicular pain, and surgical removal of the extruded NP may lead to a quick recovery to full function. Fluoroscopically guided perineural injections of methylprednisolone ± bupivacaine has recently been successfully used to treat the radicular pain caused by lateralized cervical disc extrusions [23]. A rare entity of NP extrusion has been described under the name of Schmorl´s node. This is described as a herniation of NP into the body of the vertebra through the endplate, leading to an inflammation with subsequent bone absorption (Figure 5) [24-27]. Most of these cystic lesions are incidental findings on CT or MRI scans. But clinical presentation can be caused by pain in the affected IVD and vertebra [25]. The limited information from the literature and from anecdotal cases of this rare extrusion does not allow today for an evidence based conclusion on the best treatment protocol.
Summary of the Hansen type l classification: In summary, the basic Hansen classification that distinguishes between NP extrusions (Hansen type l) and AF protrusions (Hansen type 2), is still useful. However, data collected in recent years show that there are distinct subtypes of the Hansen type l IVDE. These subtypes have different clinical presentation, and subsequently may benefit from different diagnostic techniques and therapy. Differences seen in the clinical picture of the Hansen type l subtypes are based on the degenerative state of the NP, but also on the velocity and localization of the extrusion. Clinical features of the six subtypes described in this review are summarized in table form as subtypes Hansen type l a-f (Table 1).
IVDD Hansen Type 2
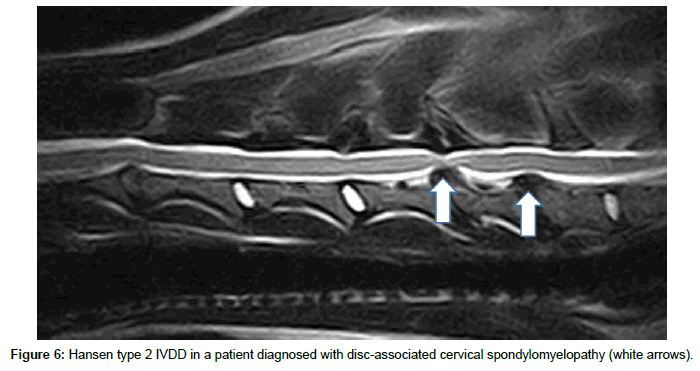
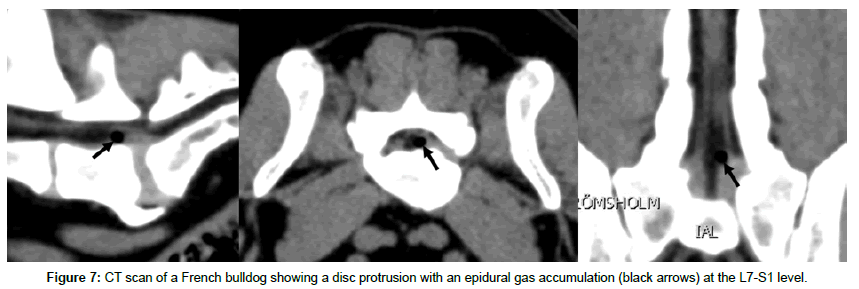
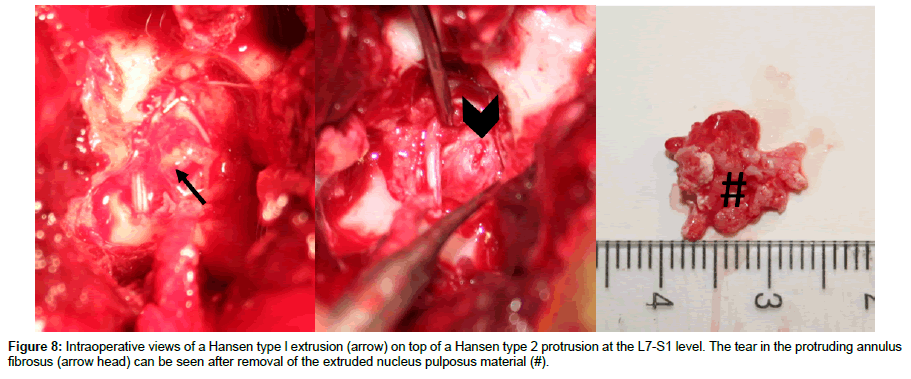
Hansen type 2 IVDD and protrusion is described as a fibroid degeneration and an age-related process that occurs in all breeds, but is documented mainly in nonchondrodystrophic dogs older than 7 years [1,28]. Hansen type 2 IVDD is characterized by a fibrous collagenization of the NP with concurrent degeneration of the AF, leading to partial ruptures and dorsal bulging of the AF ending in chronic mild-severe cord compression [1,28]. Signs are in most cases progressive, ranging from pain and ataxia to paresis and incontinence. Today, surgical decompression via corpectomy or ventral slot is recommended to relieve symptoms manifested in these patients [19-31]. Prognosis depends on (1) the degree of spinal cord damage, with mainly axonal atrophy and gliosis, often visible in T2-weighted MRI scans as a hyperintense signal, and (2) possible reperfusion injury following decompression. Rate of successful outcome has been shown to be lower for a chronic Hansen type 2 protrusion compared to a type la IVDE [32]. Type 2 IVDD sometimes occurs with biomechanical stress and/or instability, leading to degenerative changes of the spine including Hansen type 2 protrusion, spondylosis, ligament hypertrophy and facet joint changes such as intraspinal synovial cysts. Prevalence of these types of degenerative changes is higher in disc-associated cervical spondylomyelopathy (CSM) (Figure 6), and the degenerative lumbosacral syndrome (DLSS) [33-35]. Decompression of the spinal cord/nerve roots in these patients often needs not only removal of the protruding disc, but also release from the hypertrophied dorsal ligament and bone proliferations. Existing instability can be addressed by traction-fusion of the affected segment [33,36]. Additionally, in human spine surgery, a form of lumbar disk protrusion including a gas-containing cyst has been described [37,38]. Gas in the epidural space has been shown to be related to a disc vacuum phenomenon, and a one-way valve mechanism is suggested to be located between the gas in the disc and the epidural space. Clinically, human patients can suffer from lumbosacral radicular pain, often not responding to conservative treatment with rest and anti-inflammatory medication [37,38]. A similar form of gas-containing disc protrusion has recently been described in dogs with DLSS (Figure 7). The clinical significance of these epidural gas accumulations is unknown, but surgically treated DLSS patients with epidural gas accumulations have shown a good outcome retrieving their normal activity level postsurgery [39]. Hansen noted 1952 that in some cases it is not possible to histologically classify between type l and 2. It is logical to assume, that a type 2 partial AF rupture can protrude for some time and then rupture completely leading to an additional type l IVDE (‘one on two’) (Figure 8). There is a lack of evidence in the literature regarding prognosis of these specific cases, but surgical intervention is warranted if compression with neurologic deficits are present.
Prognosis of Patients with an IVDE
Most of the cases described in the literature are chondrodystrophic patients. These dogs often suffer from a IVDE with degenerated nucleus pulposus (Hansen type 1 a+b, Table 1). Prognosis of patients with an IVDE may be influenced by many factors such as severity of clinical signs, rate of onset, ambulation and deep pain perception (DPP).
Older and newer studies agree, that successful surgical outcome can be seen in 86-96% of non-ambulatory chondrodystrophic patients with intact DPP (Frankel score 3-1), finally regaining ambulation and bladder control [40-47]. However the success rate in larger breed dogs seems to be slightly lower than in chondrodystrophic dogs, with 78-85% [32,48]. A positive indicator for fast recovery of all IVDE patients is some motoric tonus or function shown after surgery [47]. Predicted recovery time and needed hospitalization is an important pre-operative information for the owner. Reported time until ambulation is around 7-14 days in chondrodystrophic patients [40,47]. In cases with more severe signs (Frankel score 1) it may take longer to recover [44,45]. Time needed to establish bladder control after hemilaminectomy is typically shorter than time needed for regaining ambulation, and has a correlation to severity of preoperative signs [44]. Evidence regarding healing time and final prognosis, in patients specifically affected by a Hansen type l IVDE with intact DPP (Frankel score 4-2, Table 2), shows some discrepancy when only based on anamnesis and clinical status. Most studies found a correlation between the severity of clinical signs and time to ambulation. Rate of onset of the symptoms seem to have only some effect on recovery time, but not all studies confirm this correlation [9,40-44]. Other studies investigating amount of compression through a non-dispersed IVDE type l visible on preoperative images, have shown no correlation to the outcome of surgical treatment [6,9,42,44]. And, no correlation was found between outcome and location of the IVDE [45].
| Score 5 | Normal gait with spinal hyperesthesia |
| Score 4 | Ambulatory paresis |
| Score 3 | Non-ambulatory paresis |
| Score 2 | Paralysis with intact pain perception |
| Score 1 | Paralysis with absent superficial pain perception |
| Score 0 | Paralysis with absent deep pain perception |
Table 2: The modified Frankel score.
Furthermore, disc extrusions with extensive hemorrhage (DEEH) seem to have a lower healing rate after decompression surgery. Buttin and colleges suggests that the lower healing rate may be due to the strong contusion of the spinal cord generated by the acute IVDE, but also due to the often-necessary extended surgery [9]. In contrast, Tartarelli and colleges did not confirm these findings with all DEEH patients with remaining DPP recovering to ambulation [7]. Cases with a hydrated NP extrusion (HNPE) show a fast recovery, taking in consideration the severity of the clinical signs. Both surgery and conservative treatment have for these cases shown to be successful [16-20].
Loss of DPP is controversial as a clear prognostic factor, as the testing is subjective and has been performed differently in studies. It is however considered as the only clinical sign, which negatively affects the prognosis of a Hansen IVDE type l consistently in all reported studies. The success rate in these patients after surgery is reported 0-76%, with an average around 50% [28,49]. Most of the studies show a higher success rate if the patient is operated within 24 hours after loss of DPP, however one study, does not confirm this time limit [41,50-53]. Loss of DPP as a prognostic factor is however problematic. For instance, the exact time point DPP is lost is often not clearly determined, therefore a ‘cut-off point’ cannot be established clinically. This puts the owner in a rather demanding situation. The owner’s decision to perform expensive surgery with an expected recovery time of four weeks or more is based on a ‘fifty-fifty’ prognosis, and the minimal waiting time after surgery is two weeks before the clinical prognosis can be more precise [12,54]. Recent publications however, using MRI scans to distinguish the prognosis in dogs with loss of DPP and an IVDE, found a strong correlation between surgery outcome and presence, or absence, of a hyperintense intramedullary signal in T2-weighted scans [6,13]. Length of the hyperintense signal subdivided prognosis even further. Dogs having loss of DPP (Frankel score 1 and 0) and no T2 signal recovered in 100% of the cases. Dogs having loss of DPP (Frankel score 1 and 0) and a short T2 signal recovered in 55% of the cases. Dogs having loss of DPP (Frankel score 1) and a T2 signal longer than three times the L2-vertebra recovered in 31% of the cases; and only in 10% of the cases with Frankel score 0 and a T2 signal longer than three times the L2-vertebra [13]. This suggests that using an MRI scan to evaluate dogs showing a Frankel score 1 or 0 may be recommended to provide a more exact prognosis helping the owner in this emotional situation.
A promising field of research is the investigation of biomarkers detected in the serum or cerebrospinal fluid (CSF). These potential biomarker molecules originate from nervous tissue, and could be used in the future to assess the severity of the damage to the spinal cord, as the use of liver enzymes assessing liver damage today [55-57].
Treatment of spinal cord injury (SCI) and IVDD is of large interest in human medicine. Unfortunately, there is today no established drug or cell treatment for acute or chronic SCI or IVDD in humans. The dog affected by an IVDD/IVDE can positively be used as a translational clinical animal model in search for new effective substances and procedures [58-63].
Surgical Treatment of IVDE
Most publications describing success of conservative treatment of IVDE are older, except for the publications of Levine et al. and Mann et al. [3,4,64-70]. One essential drawback of these studies is the lack of diagnostic proof that the dogs were actually suffering from an IVDE. The dogs had assumed IVDE, and no classification was possible. Several differential diagnoses exist such as fibrocartilaginous embolism, discospondylitis, neuritis, intraspinal cysts and tumors. Furthermore, patient care was different within the studies but also compared to conservative treatment today regarding medication and rehabilitation. Another fact making the comparison of these studies difficult, is the severity of clinical signs, reported 76,4% (50-100%) of the conservatively treated patients being ambulatory compared to 91,8% (66-100%) being non-ambulatory in the surgically treated cases [3,4,49,64-67,69-81]. Therefore it may be problematic to compare these conservative treatments with other publications reporting success rate of surgically treated dogs with IVDE. To our knowledge no controlled prospective trials have been published. In controlled studies, diagnostic imaging of all patients would be necessary to confirm the IVDE and to classify the type of IVDE. Since subtypes of IVDE have different prognoses and treatment options, it can be argued that they should also be differentiated in studies. Unfortunately, ethical concerns are high regarding a randomized prospective comparison between surgical decompression and conservative treatment, due to the reported high success rate of decompressive surgery [82]. Despite the lack of scientific evidence in publications regarding conservative treatment, success rates reported are quite uniform in all studies. It has been reported that 82-100% of ambulatory dogs (Frankel score 5 and 4) were treated successfully conservatively, but only 23-55% of non-ambulatory dogs [3,4,66,67,69,83]. In cases with a Frankel score 3 reported relapse rate during conservative treatment was 30-50%, thus lowering number of patients with a final successful outcome [5,12,66,67,70] For cases with a Frankel score 2-1 reported success rate of surgery is clearly superior to conservative treatment, and success of conservative treatment in cases with Frankel score 0 is close to zero [3,5,28,66,69].
Today we find a wide consent that surgical treatment of IVDE is recommended for spinal pain or paresis unresponsive to conservative treatment, but also for patients with recurrence of clinical signs during or after conservative treatment. Non-ambulatory patients are generally candidates for immediate imaging and decompressive surgery, with the aim of removing all extruded NP material [5,28].
Further evidence supporting surgical treatment
Newer studies confirm the cascade of events in the epidural space and within the cord that occur after an IVDE. Vascular compromise leads to tissue damage and focal myelomalacia in the cord, and persistent compression affects the lateral columns. Extruded NP induces an epidural inflammation leading to painful radiculitis [84-88]. Not only final treatment outcome, but also length of recovery and morbidity play a key role when choosing between surgical and conservative treatment. High rate of relapse during conservative treatment, leading to prolonged pain, may be considered as an argument for choosing surgical therapy instead of conservative treatment. During conservative treatment, the dog may compensate the loss of axonal function caused by the compression, but unfortunately this cannot be seen in all cases. Recovery with the ability to walk a few steps and urinate without help after surgery can be expected within 7-14 days in up to 96% of the cases [40,41,43-47]. The sooner the dog can move the affected legs and empty the bladder, the lower is the complication rate and loss of musculature. Relief of pain inflicted by epidural inflammation induced by NP material is fast after surgery when combined with modern analgesia. These factors seem to be valuable arguments for fast surgical decompression of nervous tissue in non-ambulatory patients. Less invasive surgical techniques are under development, making hemilaminectomy procedure less traumatic and painful [89,90]. In summary, evidence shows that ambulatory dogs with an IVDE can be treated conservatively, however, keeping in mind the considerable risk of relapse or incomplete remission with chronic pain making surgery necessary. Additionally, robust evidence shows that surgery is recommended in patients with a Frankel score 2,1 or 0. For cases with a Frankel score 3, however, evidence to do surgery is weaker due to lack of controlled studies. Importantly, high rate of reported relapse and epidural inflammation in Frankel score 3 cases are additional valid arguments for an immediate decompressive surgery also in these cases.
Recurrence rate of IVDE after surgical treatment
During the first days, up to four weeks after decompressive surgery, reherniation can occur at the same site as the original herniation. To assess this, immediate diagnostic imaging is recommended if unexpected pain or deterioration of neurologic status is detected in the postoperative period. Most cases can fortunately be reoperated with a successful outcome [91-94]. To prevent this complication, fenestration of the extruded IVD was recommended by some authors [46,95,96]. In two case series of 93 hemilaminectomies without and 252 with fenestration recurrence rate was 5%, all recurrent IVDE occurred at a new site [46,49]. In another large study involving 467 hemilaminectomies without fenestration, recurrence rate was reported 6,4%; 83% of reoperations were also here at a different site [91]. Another study using hemilaminectomy without fenestration, show a higher recurrence rate of 14,6% (41 cases out of 281), all cases with herniation of a different IVD [41]. Furthermore Aikawa and colleagues reported 662 operated cases using routinely fenestration T11-L1with a recurrence rate of 2,3% with a 2nd surgery. Additionally, 10% of these operated dogs were treated conservatively for signs of IVDE without radiological conformation. In this study, all recurrent IVDE were also at a different site, and significantly more common in non-fenestrated IVD [97].
Conclusion
Despite that intervertebral disc disease historically has been categorized into two main subtypes, Hansen type 1 and 2, it is significant to recognize and appreciate that we today further can subdivide IVDD and IVDE. These subtypes have different clinical presentation, and subsequently may benefit from different diagnostic techniques and therapy. Differences seen in the clinical picture of the Hansen type l subtypes are based on the degenerative state of the NP, but also on the velocity and localization of the extrusion.
Most of the cases described in the literature are chondrodystrophic patients. These dogs often suffer from a IVDE with degenerated nucleus pulposus. Today we find a wide consent supported by the evidence that surgical treatment of IVDE is recommended for non-ambulatory patients. Successful surgical outcome can be seen in 86-96% of these patients with intact DPP, finally regaining ambulation and bladder control. Less severe cases can be treated conservative keeping in mind the considerable risk of relapse or incomplete remission with chronic pain making surgery necessary. The pathologic events within the spinal canal and cord further advocate a surgical removal of extruded degenerated nucleus pulposus material.
References
- Hansen HJ (1952) A pathological study on disc degeneration in dog. Acta Orto Scand Suppl no XI: 1-117.
- Olson SE (1951) On disc protrusion in dog (enchondrosis intervertebralis); a study with special reference to roentgen diagnosis and to the value of disc fenestration. Acta Orto Scand Suppl 8: 1-95.
- Funkquist B (1962) Thoraco-lumbar disk protrusion with severe cord compression in the dog. 1. Clinical and pathoanatomic observations with special reference to the rate of development of the symptoms of motor loss. Acta Vet Scand 3: 256-274.
- Funkquist B (1970) Decompressive laminectomy in thoraco-lumbar disc protrusion with paraplegia in the dog. J Small Anim Pract 11: 445-451.
- Coates JR (2000) Intervertebral disk disease. Vet Clin North Am Small Anim Pract 30:77-110.
- Besalti O, Peckan Z, Sirin YS, Erbas G (2006) Magnetic resonance imaging findings in dogs with thoracolumbar intervertebral disk disease: 69 cases (1997-2005). J Am Vet Med Assoc 228: 902-908.
- Tartarelli CL, Baroni M, Borghi M (2005) Thoracolumbar disc extrusion associated with extensive epidural haemorrhage: a retrospective study of 23 dogs. J Small Anim Pract 46: 485-490.
- Olby NJ, Munana KR, Sharp NJ, Thrall DE (2000) The computed tomographic appearance of acute thoracolumbar intervertebral disc herniation in dogs. Vet Radiol Ultrasound 41: 396-402.
- Buttin P, Millet M, Cousin S, Carozzo C, Viguer E (2013) Computed tomographic measurements with and without myelography to characterise thoracolumbar extruded disc herniation. J Small Anim Pract 54: 521-530.
- De Risio L (2015) A review of fibrocartilaginous embolic myelopathy and different types of peracute non-compressive intervertebral disk extrusions in dogs and cats. Frontiers Vet Sci. 18: 2:24.
- Henke D, Gorga D, Flegel T, Vandevelde M, Lang J, et al. (2013) Magnetic resonance imaging findings in dogs with traumatic intervertebral disk extrusion with or without spinal cord compression: 31 cases (2006-2010). J Am Vet Med Assoc 242: 217-222.
- Griffin JF, Levine JM, Cole RC (2009) Canine thoracolumbar intervertebral disk disease: diagnosis, prognosis and treatment. Compend Contin Educ Vet. 3:E3.
- Ito D, Matsunga S, Jeffrey N, Sasaki N, Nishimura R, et al. (2005) Prognostic value of magnetic resonance imaging in dogs with paraplegia caused by thoracolumbar intervertebral disk extrusion: 77 cases (2000-2003). J Am Vet Med Assoc 227: 1454-1460.
- Chang Y, Dennis R, Platt SR, Penderis J (2007) Magnetic resonance imaging of traumatic intervertebral disc extrusions in dogs. Vet Rec 160: 795-799.
- De Risio L, Adams V, Dennis R, McConnel FJ (2009) Association of clinical and magnetic resonance imaging findings with outcome in dogs with presumptive acute noncompressive nucleus pulposus extrusion: 42 cases (2000-2007). J Am Vet Med Assoc 234: 495-504
- Beltram E, Dennis R, Doyle V, De Stefani A, Holloway A, et al. (2012) Clinical and magnetic resonance imaging features of canine compressive cervical myelopathy with suspected hydrated nucleus pulposus extrusion. J Small Anim Pract 53: 101-117.
- Hamilton T, Glass E, Drobatz K, Agnello KA (2014) Severity of spinal cord dysfunction and pain associated with hydrated nucleus pulposus extrusion in dogs. Vet Comp Orthop Traumatol 27: 313-318.
- Konar M, Lang J, Flühmann G, Forterre F (2008) Ventral intraspinal cysts associated with the intervertebral disc: magnetic resonance imaging observations in seven dogs. Vet Surg 37: 94-101.
- Kamishina H, Ogawa H, Katayama M, Tohyama K (2010) Spontaneous regression of a cervical intraspinal cyst in a dog. J Vet Med Sci 72: 349-52.
- Manunta ML, Evangelisti MA, Bergknut N, Grinwis GC, Ballocco I, et al. (2015) Hydrated nucleus pulposus herniation in seven dogs. Vet J 203: 342-344.
- Falzone C (2017) Canine acute cervical myelopathy: Hydrated nucleus pulposus extrusion or intraspinal cyst? Vet Surg 46: 376-80.
- Fadda A, Lang J, Forterre F (2013) Far lateral lumbar disc extrusion: MRI findings and surgical treatment. Vet Comp Orthop Traumatol 26: 318-322.
- Giambuzzi S, Pancotto T, Jeffrey R (2016) Perineural injection for treatment of root- signature signs associated with lateralized disk material in five dogs (2009-2013). Front Vet Sci. 27: 3:1.
- Baltzer WI, Hillebrand L, Smith TJ, Stieger-Vanegas SM (2012) Surgical management of a Schmorl’s node in an Airdaile Terrier and review of the literature. Vet Comp Orthop Traumatol 25: 167-171.
- Gaschen L, Lang J, Häni H (1995) Intravertebral disk herniation (Schmorl’s node) in five dogs. Vet Radiol Ultrasound 36:509-516.
- Gomez M, Mieres M, Thibaut J (2000) Cervical intravertebral disk herniation in a dog. Arch Med Vet 32: 115-119.
- Wise M, Faulkner R (1984) Unusual disc herniation in a dog: a case history report. Vet Radiol 25: 280-281.
- Brisson BA (2010) Intervertebral disc disease in dogs. Vet Clin North Am Small Anim Pract 40: 829-858.
- Flegel T, Böttcher IC, Ludewig E, Oechtering G, Böttcher P (2011) Partial lateral corpectomy of the thoracolumbar spine in 51 dogs: assessment of slot morphometry and spinal cord decompression. Vet Surg 40: 14-21.
- Moissonnier P, Meheust P, Carozzo C (2004) Thoracolumbar lateral corpectomy for treatment of chronic disk herniation: technique description and use in 15 dogs. Vet Surg 33: 620-628.
- Medl S, Reese S, Medl N (2011) Individualized mini-hemilaminectomy-corpectomy (iMHC) for the treatment of thoracolumbar intervertebral disc herniation in large breed dogs. Vet Surg 46: 422-32.
- Macias C, McKee WM. May C (2002) Thoracolumbar disc disease in large dogs: A study of 99 cases. J Small Anim Pract 43: 439-446.
- Fitzpatrick N, Fingeroth JM (2015) Is wobbler disease related to disc disease? Advances in Intervertebral Disc Disease in Dog and Cats. (1st ed), MA: Wiley Blackwell, Iowa, US.
- Da Costa R (2010) Cervical Spondylomyelopathy (Wobbler Syndrome) in Dogs. Vet Clin North Am Small Anim Pract 40: 881-913.
- Schmökel H, Rapp M (2016) Lameness caused by an extradural lumbosacral foraminal synovial cyst in three German Shepherd Dogs. Vet Comp Orthop Traumatol 29: 83-88.
- Farrell M, Fitzpatrick N (2015) Lumbosacral disc disease: Is vertebral stabilization indicated? Advances in Intervertebral Disc Disease in Dog and Cats. (1st ed), MA:Wiley Blackwell, Iowa, USA.
- Ryu K-S, Rathi NK, Shin M-H (2012) Gas-containing disc herniations: Dual nerve root compression at a single disc level. Neurol Med Chir (Tokyo) 52: 649-651.
- Yasuoka H, Nemoto O, Kawaguchi M (2009) Nerve root compression by gas containing lumbar disc herniation. Brain Nerve 61: 691-694.
- Skytte D, Schmökel H (2017) Epidural gas accumulation in connection with canine degenerative Lumbosacral Disease. Front Vet Sci. 18: 4:55.
- Ferreira AJA, Correia JHD, Jaggy A (2002) Thoracolumbar disc disease in 71 paraplegic dogs: influence of rate of onset and duration of clinical signs on treatment results. J Small Anim Pract 43: 158-163.
- NeÄÂas A (1999) Clinical aspects of surgical treatment of thoracolumbar disc disease in dogs. A retrospective study of 300 cases. Acta Vet Brno 68: 121-130.
- Penning V, Platt SR, Dennis R, Capello R, Adams V (2006) Association of spinal cord compression seen on magnetic resonance imaging with clinical outcome in 67 dogs with thoracolumbar intervertebral disc extrusion. J Small Anim Pract 47: 644-650.
- Sterna J, Burzykowski T (2007) The assessment of the usefulness of hemilaminectomy without fenestration in the treatment of thoracolumbar disc disease in chondrodystrophic dogs. Pol J Vet Sci 10:165-172.
- Skytte D, Schmökel H (2017) Average time until micturition and ambulation were regained after surgical treatment of thoracolumbar disc herniation in relation to the preoperative neurological score in 54 dogs.
- Ruddle TL, Allen DA, Schertel ER (2006) Outcome and prognostic factors in non-ambulatory Hansen type l intervertebral disc extrusion: 308 cases. Vet Comp Orthop Traumatol 19: 29-34.
- Brisson BA, Moffatt SL, Swayne SL, Parent JM (2004) Recurrence of thoracolumbar intervertebral disk extrusion in chondrodystrophic dogs after surgical decompression with or without prophylactic fenestration. J Am Vet Med Assoc 224: 1808-1814.
- Davis GJ, Brown DC (2002) Prognostic indicators for time to ambulation after surgical decompression in nonambulatory dogs with acute thoracolumbar disk extrusion: 112 cases. Vet Surg 31:513-8.
- Cudia SP, Duval JM (1997) Thoracolumbar intervertebral disk disease in large, non-chondrodystrophic dogs: a retrospective study. J Am Anim Hosp Assoc 33: 456-460.
- Muir P, Johnson KA, Manley PA, Dueland RT (1995) Comparison of hemilaminectomy and dorsal laminectomy for thoracolumbar intervertebral disc extrusion in dachshunds. J Small Anim Pract 36: 360-367.
- Duval J, Dewey C, Roberts R, Aron D (1996) Spinal cord swelling as a myelographic indicator of prognosis: a retrospective study in dogs with intervertebral disc disease and loss of deeppain perception. Vet Surg 25: 6-12.
- Laitinen OM, Puerto DA (2005) Surgical decompression in dogs with thoracolumbar intervertebral disc disease and loss of deep pain perception: a retrospective study of 46 cases. Acta Vet Scand 46: 79-85.
- Scott HW, McKee WM (1999) Laminectomy for 34 dogs with thoracolumbar intervertebral disc disease and loss of deep pain perception. J Small Anim Pract 40: 417- 422.
- Olby NJ, Levine J, Harris T, Munana KR, Skeen T, et al. (2003) Long-term functional outcome of dogs with severe injuries of the thoracolumbar spinal cord: 87 cases. J Am Vet Med Assoc 222:762-768.
- Griffin JF, Levine JM, Kerwin SC (2009) Canine thoracolumbar intervertebral disk disease: pathology, neurologic examination and emergency medical treatment. Compend Contin Educ Vet 31: E2.
- Martin-Vaquero P, Da Costa RC, Allen MJ, Moore SA, Keirsey JK, et al. (2015) Proteomic analysis of cerebrospinal fluid in canine cervical spondylopathy. Spine 40: 601-612.
- Mashita T, Kamishina H, Nakamoto Y, Akagai Y, Shaw G, et al. (2015) Combination of serum phosphorylated neurofilament heavy subunit and hyperintensivity if intramedullary T2W on magnetic resonance imaging provides better prognostic value of canine thoracolumbar intervertebral disc herniation. J Vet Med Sci 77: 433-438.
- Roerig A, Carlson R, Tipold A, Stein VM (2013) Cerebrospinal fluid tau protein as biomarker for severity of spinal cord injury in dogs with intervertebral disc herniation. Vet J 197: 253-258.
- Granger N, Blamires H, Franklin RJ, Jeffrey ND (2012) Autologous olfactory mucosal cell transplants in clinical spinal cord injury: a randomized double-blinded trial in a canine translational model. Brain 135: 3227-3237.
- Hiyama A, Mochida J, Iwashina T, Omi H, Watanabe T, et al. (2008) Transplantation of mesenchymal stem cells in a canine disc degeneration model. J Orthop Res 26: 589-600.
- Bach FC, Willems N, Penning LC, Keito I, Meij BP, et al. (2014) Potential regenerative treatment strategies for intervertebral disc degeneration in dogs. BMC Vet Res 10: 3.
- Levine JM, Cohen ND, Heller M, Fajt VR, Levine GJ, et al. (2014) Efficacy of a metalloproteinase inhibitor in spinal cord injured dogs. PLoS One 9: e96408.
- Kwon BK, Okon E, Hillyer J, Mann C, Teztlaff W (2011) A systematic review of non- invasive pharmacologic neuroprotective treatments for acute spinal cord injury. J Neurotraum 28: 1545-88.
- Kwon BK, Okon E, Blunet W, Baptiste D, Fouad K, et al. (2011) A systematic review of directly applied biologic therapies for acute spinal cord injury. J Neurotraum 28: 1589-1610.
- Funkquist B (1978) Investigations of the therapeutic and prophylactic effects of disc evacuation in cases of thoraco-lumbar herniated disc in dogs. Acta Vet Scand19: 441-457.
- Davies JV, Sharp NJHA (1983) Comparison of conservative treatment and fenestration for thoracolumbar intervertebral disc disease in the dog. J Small Anim Pract 24: 721-729.
- Levine JM, Levine GJ, Johnson SI, Hettlich BF, Fosgate GT (2007) Evaluation of the success of medical management for presumptive thoracolumbar intervertebral disk herniation in dogs. Vet Surg 36:482-491.
- Levine JM, Levine GJ, Johnson SI, Hettlich BF, Fosgate GT (2007) Evaluation of the success of medical management for presumptive cervical intervertebral disk herniation in dogs. Vet Surg 36:492-499.
- Scavelli TD, Schoen A (1989) Problems and complications associated with nonsurgical management of intervertebral disc disease. Problems Vet Med 1:402-414.
- Wilcox KR (1965) Conservative treatment of thoracolumbar intervertebral disc disease in the dog. J Am Vet Med Assoc 147:1458-1460.
- Mann FA, Wagner-Mann CC, Dunphy ED, Ruben DS, Rochat MC, et al. (2007) Recurrence rate of presumed thoracolumbar intervertebral disc disease in ambulatory dogs with spinal hyperpathia treated with anti-inflammatory drugs: 78 cases (1997–2000). J Vet Emerg Crit Care 17:53-60.
- Aikawa T, Fujita H, Kanazono S, Shibata M, Yoshigae Y (2012) Long-term neurologic outcome of hemilaminectomy and disk fenestration for treatment of dogs with thoracolumbar intervertebral disc herniation: 831 cases. J Am Vet Med Assoc 241: 1617-1626.
- Black AP (1988) Lateral spinal cord decompression in the dog: a review of 39 cases. J Small Anim Pract 29:581-588.
- Brown NO, Helphrey M, Prata RG (1977) Thoracolumbar disk disease in the dog: A retrospective analysis of 187 cases. J Am Anim Hosp Assoc 13: 665-672.
- Bush WW, Tiches DM, Kampard C, Murtaugh MJ, Bass CS (2007) Functional outcome following hemilaminectomy without methylprednisolone sodium succinate for acute thoracolumbar disk disease in 51 non-ambulatory dogs. J Vet Emerg Crit Care 17: 72-76.
- Hayashi AM, Matera JM, Fonseca Pinto AC (2007) Evaluation of electroacupuncture treatment for thoracolumbar intervertebral disk disease in dogs. J Am Vet Med Assoc 231:913-918.
- Jeffrey ND, Barker AK, Hu Z, Alcott CJ, Kraus KH et al. (2016) Factors associated with recovery from paraplegia in dogs with loss of pain perception in the pelvic limbs following intervertebral disk herniation. J Am Vet Med Assoc 248:386-394.
- Joaquim JG, Luna SP, Brondani JT, Torelli SR, Rahal SC, et al. (2010) Comparison of decompressive surgery, electroacupuncture, and surgery followed by electro- acupuncture for the treatment of dogs with intervertebral disk disease with long- standing severe neurological deficits. J Am Vet Med Assoc 236:1225-1229.
- McKee WM (1992) A comparison of hemilaminectomy (with concomitant disk fenestration) and dorsal laminectomy for the treatment of thoracolumbar disk protrusion in dogs. Vet Rec 130: 296-300.
- Knecht CD (1972) Results of surgical treatment for thoracolumbar disc protrusion. J Small Anim Pract 13:449-453.
- Loughin CA, Dewey CW, Ringwood PB, Pettigrew RW, Kent M, et al. (2005) Effect of durotomy on functional outcome of dogs with type I thoracolumbar disc extrusion and absent deep pain perception. Vet Comp Orthop Traumatol 18:141-146.
- Schulman A, Lipincott CL (1987) Dorsolateral hemilaminectomy in the treatment of intervertebral disc disease in dogs. Comp Small Anim Cont Educ 9:305-310.
- Freeman P, Jeffrey ND (2017) Re-opening the window on fenestration as a treatment for acute thoracolumbar intervertebral disc herniation in dogs. J Small Anim Pract 58:199-204.
- Hoerlein BF (1956) Further evaluation of the treatment of disc protrusion paraplegia in the dog. J Am Vet Med Assoc 129:495-502.
- Doita M, Kanatani T, Ozaki T, N Matsui; M Kurosaka et al. (2001) Influence of macrophage infiltration of herniated disc tissue on the production of matrix metalloproteinases leading to disc resorption. Spine 26: 1522-1527.
- Griffiths IR (1972) Some aspects of the pathology and pathogenesis of the myelopathy caused by disc protrusions in the dog. J Neurol Neurosurg Psychiatry 35:403-413.
- Fadda A, Oevermann A, Vandefelde M, Doherrr MG, Forterre F, et al. (2013) Clinical and pathological analysis of epidural inflammation in intervertebral disk extrusion in dogs. J Vet Intern Med 27:924-934.
- Royal AB, Chigerwe M, Coates JR, Berent LM (2009) Cytologic and histopathologic evaluation of extruded canine degenerated disks. Vet Surg 38:798-802.
- Shimizu J, Chigerwe M, Coates JR (2010) Inflammatory reaction in the herniated degenerative disc material in miniature dachshunds. J Vet Med Sci 72:81-84.
- Carozzo C, Maitre P, Genevois JP, Gabanou PA, Fau D, et al. (2011) Endoscope-assisted thoracolumbar lateral corpectomy. Vet Surg 40:738-742.
- Hwang Y-H, Lee H_C, Lee J-H (2016) Operative techiques and preliminary outcomes following percutaneous Endoscopic thoracolumbar pediculectomy in dogs. Vet Surg 45: 84-94.
- Dupah S, Glickman N, Waters D (1999) Reoperative neurosurgery in dogs with thoracolumbar disc disease. Vet Surg 28:421-428.
- Forterre F, Gorgas D, Dickomeit M, Jaggy A, Lang J, et al. (2010) Incidence of spinal compressive lesions in chondrodystrophic dogs with abnormal recovery after hemilaminectomy for treatment of thoracolumbar disc disease: a prospective magnetic resonance imaging study. Vet Surg 39: 165-172.
- Hettlich BF, Kermin SC, Levine JM (2012) Early reherniation of disk material in eleven dogs with surgically treated thoracolumbar intervertebral disk extrusion. Vet Surg 41:215-220.
- Stingen O, Ottesen N, Jäderlund KH (2010) Early recurrence of thoracolumbar intervertebral disc extrusion after surgical decompression: a report of 3 cases. Acta Vet Scand 52: 1-10.
- Forterre F, Konar M, Spreng D, Jaggy A, Lang J (2008) Influence of intervertebral disc fenestration at the herniation site in association with hemilaminectomy on recurrence in chondrodystrophic dogs with thoracolumbar disc disease: a prospective MRI study. Vet Surg 37: 399-405.
- Scott HW (1997) Hemilaminectomy for the treatment of thoracolumbar disc disease in the dog: a follow-up study of 40 cases. J Small Anim Pract 38:488-494.
- Aikawa T, Fujita H, Shibata M, Takahasi T (2012) Recurrent thoracolumbar intervertebral disc extrusion after hemilaminectomy and concomitant prophylactic fenestration in 662 chondrodystrophic dogs. Vet Surg 41: 381-90.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi