Research Article, J Trauma Stress Disor Treat Vol: 7 Issue: 1
Pediatric Mood Disorders and Trauma: What are the Associations?
Yael Dvir1*, Hodge SM1, Michael Hill2 and Frazier JA1
1Department of Psychiatry, University of Massachusetts Medical School, USA
2Department of Emergency Medicine, University of Massachusetts Medical School, USA
*Corresponding Author : Yael Dvir, MD
Department of Psychiatry, University of Massachusetts Medical School, 55 Lake Avenue North, Worcester, MA 01655, USA
Tel: 508-856-5390
Fax: 508-856-5000
E-mail: Yael.Dvir@umassmed.edu
Received: January 22, 2018 Accepted: February 12, 2018 Published: February 19, 2018
Citation: Dvir Y, Hodge SM, Hill M, Frazier JA (2018) Pediatric Mood Disorders and Trauma: What are the Associations?. J Trauma Stress Disor Treat 7:1. doi: 10.4172/2324-8947.1000182
Abstract
Background: There is limited data on the effects of Childhood Maltreatment (CM) on pediatric mood disorders in general and pediatric Bipolar Disorder (BD) in particular. We aimed to compare clinical and family characteristics of youth with CM and Mood Disorder Not Otherwise Specified (MD) to youth with CM and BD and to follow the youth with MD longitudinally to determine their course of illness.
Methods: Twenty-two youths (ages 8-18 years) with mood symptoms (11 with BD and 11 with MD) and histories of CM prior to the age of 5 years were assessed using a structured clinical interview. A follow-up assessment was conducted with 8 of the 11 parents of youth with MD.
Results: 11 subjects (5 females, mean age 13 ± 2.4 sd) met DSMIV-TR criteria for BD and 11 subjects (4 females, mean age 12.5 ± 3.1 sd) met DSM-IV-TR criteria for MD. BD subjects had a higher number of lifetime major depressive episodes (BD=18.9 versus MD=4, z(20)=-2.5, p=0.01) and lifetime manic episodes (BD=17.7 MD=0.3, z(19)=-5.1,p<0.001). Age at first reported trauma exposure was similar for both groups youth with BD (BD=3.1 ± 1.7 MD 3.4 ± 1.8 t(19.9)=-0.4, p=0.7), as were types of trauma, number of incidents, and PTSD symptoms. There were higher rates of schizophrenia, BD and major depressive disorder in the families of youth with BD compared to youth with MD. At follow up, 4/8 (50%) youth with MD at baseline either received a different diagnosis (n=2), or experienced a manic episode (n=2).
Conclusions: The results suggest higher rates of schizophrenia, BD, and MDD in the families of youth with BD. These preliminary results suggest potential biological and genetic vulnerabilities, which may predispose children with histories of CM to develop specific mood disorders under certain circumstances.
Keywords: Childhood maltreatment; Pediatric mood disorders; Pediatric bipolar disorder; Mood disorder not otherwise specified; Major depressive episode; Manic episode; Post-traumatic stress disorder
Abbreviations
CM: Childhood Maltreatment; BD: Bipolar Disorder; MD: Mood Disorder Not Otherwise Specified; DSM: Diagnostic and Statistical Manual; PTSD: Post-Traumatic Stress Disorder
Introduction
There is ample evidence to suggest that childhood maltreatment (CM) contributes to mood dysregulation and is comorbid with psychiatric conditions in children and in adults [1-3]. Children who have experienced CM are at greater risk for both internalizing and externalizing disorders, and in adults, CM is found to increase the risk and severity of mood disorder, including depression and bipolar disorder [1-3]. CM is disproportionately reported in adults with Bipolar Disorder (BD): about half of adult patients with BD, across several studies, report CM [4,5]. Additionally, CM negatively influences the course and progression of BD in adults and is a predictor of unfavourable clinical outcomes such as delayed diagnosis, higher rates of hospitalizations, and decreased quality of life [6]. Adults with BD who report CM more frequently have prepubertal onset of affective symptoms [4,5,7,8] younger age at bipolar illness onset, and higher severity level of symptoms [5]. There appears to be a clear dose response effect between CM and BD severity in adults [9]. Few studies have examined the contribution of CM to the course of pediatric BD, but those that have, suggest significant interactions. For example, Romero and colleagues found a history of CM in 20% of 446 youth with BD (age: 7-17 years) as well as longer duration of illness and higher rates of Post-traumatic Stress Disorder (PTSD), and psychosis in the youth with CM [10]. In a New Zealand sample of 24 adolescents with BD (age: 13-17 years) 50% (compared to 10% of controls) reported CM [11]. Similarly, in a chart review, 35/66 (53%) of youth with BD seen in a community mental health outpatient clinic, experienced CM [12]. Finally, the multi-site Course and Outcome of Bipolar Youth (COBY) study, found that youth with BD and comorbid substance use disorders had a greater lifetime prevalence of physical and sexual abuse, as well as PTSD [13]. Given this apparent high prevalence of CM in BD youth, it is critical to better understand the implications of these common adverse psychosocial events on the development and clinical course of pediatric mood disorders, particularly on pediatric BD, as this has received little attention in the literature. Given that negative alterations in mood and reactivity (including irritable behaviour and angry outbursts) are among the DSM-5 the criteria for PTSD, it is not surprising that there is confusion when it comes to identifying and diagnosing BD in traumatized youth [14]. In the aftermath of trauma, mood dysregulation in children often is misdiagnosed within the clinical setting as BD and conversely, the diagnosis of BD is often overlooked in youth who have been traumatized. This situation results in a diagnostic quagmire that is critical to understand in more depth. It is also important to remember that not all traumatized children develop PTSD, and that the consequences of trauma may vary [15]. However, there is clear evidence to suggest that even when the diagnostic criteria for PTSD are not met in youth who experienced CM, there is a complex and bi-directional relationship between CM and mood dysregulation, and this relationship is associated with psychiatric comorbidities and impaired functioning across the lifespan [1]. Understanding the associations between trauma and the development of mood disorders will increase our knowledge of the effects of such events on youths’ emotional and behavioral development. Such distinctions have important implications in terms of treatment approaches and the study of biological markers and social/demographic factors.
To our knowledge, this is the first study to directly and longitudinally compare mood symptomatology, clinical correlates and demographics of traumatized, mood dysregulated youth with and without BD. Based on the literature, we expected that traumatized youth with mood dysregulation symptoms frequently would not meet criteria for either PTSD or BD, and that traumatized youth who meet full criteria for BD would be more likely to have a family history of BD, mood symptoms predating trauma and specific neurovegetative symptom clusters. We also hypothesized that traumatized mood dysregulated youth who progress to BD over the course of the followup period would have certain predictors of progression via specific identifiable symptom clusters.
Methods
The university’s institutional review board approved this pilot study, which was funded by the American Academy of Child and Adolescent Psychiatry supported by Lilly USA, LLC. Twenty-two youths (ages 8-18 years) with symptoms of mood dysregulation (11 with and 11 without BD) and histories of CM prior to the age of 5 years were recruited from outpatient units and referrals from clinicians at the University of Massachusetts Medical School/UMass Memorial Health care System. Parents signed informed consent and youth provided assent. Parents/primary caregivers were interviewed about the youths, and the youths were directly assessed by a trained child psychiatrist (board certified) or psychiatric nurse practitioner for a diagnosis of mood disorder using the following measures (Table 1): Structured Clinical Interview for DSM Disorders, Childhood Disorders Form (KID-SCID) mood module [16]. Additional information about the youth’s mood symptomatology was obtained using clinician administered Brief Psychiatric Rating Scale for Children (BPRS-C) [17], Young Mania Rating Scale (YMRS) [18], and Children’s Depression Rating Scale-Revised (CDRS-R) [19]. Information about CM was obtained from the interview with the parents and the youth’s self-report on the Childhood Trauma Questionnaire (CTQ) [20]. Common co-morbidities were assessed using the following self-report measures: PTSD Checklist –Civilian Version (PCL-C) [21], Attention Deficit Hyperactivity Disorder IV (ADHD-IV) rating scale [22], and a CRAFFT Substance Abuse screen [23]. Other information obtained during the psychiatric clinical assessment included demographic characteristics, number of medications and types, lifelong history of psychiatric hospitalization/out of home placement, and family history of psychiatric illness and substance use disorders based on parent report (Table 2). As the longitudinal portion of the study was specifically designed to identify the progression of MD to BD, the follow up assessment was conducted with MD subjects only and included assessments able to identify mania. A follow- up assessment was conducted through phone interviews with 8 of the 11 parents of youth with MD, within 1-2 years of the initial evaluation, and included interviewing for any change in diagnosis or medications, or interim hospitalizations, suicidality (ideations and attempt) and additional trauma exposure. The interviewer also repeated the administration of the SCID Mood Module, BPRS, and YMRS. Three subjects were lost to follow up.
| Rating Scale | Psychometric Properties | Time Period |
|---|---|---|
| Childhood Disorders Form (KID-SCID) mood module [16] | Structured interview, each module includes 4 sections with up to 9 questions per section | 1 month AND lifetime |
| Brief Psychiatric Rating Scale for Children (BPRS-C) [17] | 21-item clinician-based rating scale. Ratings based on 7- point Likert scale | 2-3 days |
| Young Mania Rating Scale (YMRS) [18] | 11-item clinician-administered scale. Ratings based on 5 point scale | 2 days |
| Children’s Depression Rating Scale-Revised (CDRS-R) [19] | 16-item semi-structured clinician rated scale. Ratings are measured on 7 point scales | 2 days |
| Childhood Trauma Questionnaire (CTQ) [20] | 28-item self-report measure | Lifetime |
| PTSD CheckList –Civilian Version (PCL-C) [21] | 17-item self-report measure | 1 month |
| Attention Deficit Hyperactivity Disorder IV (ADHD-IV) rating scale [22] | 18-item self-report measure | 6 months |
Table 1: Psychiatric Properties of Rating Scales.
| BD | MD-NOS | Statistic* | |
|---|---|---|---|
| Group size (N) | 11 | 11 | . |
| Gender (number of Females) | 5 | 4 | 0.7 |
| Ethnicity (% Caucasian) | 90 | 75 | 0.4 |
| Age at time of Interview (mean (SD)) | 13.0 (2.4) | 12.5 (3.1) | 0.7 |
| Number of Siblings (mean (SD)) | 2.2 (1.5) | 1.7 (1.3) | 0.5 |
Table 2: Basic demographics of the sample.
Data Analysis
Demographic, clinical, and family variables were compared between subjects with MD and those with BD at baseline assessment using Chi-Square likelihood statistics for categorical variables and proportions, t-tests (supported by non-parametric rank statistics, when appropriate) for continuous variables, and zero-inflated negative binomial models for count data. The severity and type of trauma and comorbid mood disorder were examined using t-tests for continuous trauma scales and chi-square tests for categorical trauma ratings. We examined correlations between clinical measures with parametric and rank correlations, and included an interaction term for a diagnostic group to determine slope equivalence when applicable. Due to the exploratory nature of the study, the alpha rate was set at 0.05 with no correction for multiple comparisons. All analyses were done using the R statistical computing environment [24] and the contributed packages “MASS” [25] and “ggplot2” [26].
Results
Twenty-two youth were assessed, 11 subjects (5 females, mean age 13 ± 2.4 sd) met DSM-IV-TR criteria for BD (I, II, and NOS per COBY study) [27], and the additional 11 youth (4 females, mean age 12.5 ± 3.1 sd) were diagnosed with DSM-IV-TR Mood Disorder Not Otherwise Specified (MD) [28]. Eight of the 11 youth with MD were assessed 11-28 months (mean 20.8 ± 6.2 sd) following the initial assessment via a phone interview with parents. There were no differences in clinical characteristics in the 3 youth were lost to follow up. Socioeconomic measures at baseline were similar for both groups, and included matched educational levels and ethnicity of parents, and household income. There was a significant difference in marital status of parents with 70% of the BD youth being married/living together, compared to 20% of the MD group (χ2=5.0, p=0.02). Both groups were taking a similar number of psychotropic medications (BD 3.6 ± 2.7 MD 2.7 ± 2.0, z(20)=-0.9, p=0.3) and had at least one out of home placement (8/11 for BD, 7/11 for MD, χ2=0.2, p=0.6).
Trauma exposure
Age at first reported trauma exposure was similar for youth with BD (3.1 ± 1.7) compared to youth with MD (3.4 ± 1.8) (t(19.9)=-0.4, p=0.7), as were the types of trauma and the number of incidents, as reported in the interview and on the CTQ (Table 1). There were also no significant differences between the two groups in PTSD symptoms: 5 subjects met criteria for PTSD (BD 3/11 MD 2/11, χ2=0.3, p=0.6) and the PCL-C Total score was similar between groups (BD 44.8 ± 9.4, MD 39.4 ± 12.9, t(18.3)=1.1, p=0.3). There were five new incidents of trauma among three of the subjects in the MD group at the follow up assessment (Table 3).
| Type of Trauma | BP | MD | MD Time 2 |
|---|---|---|---|
| Witnessed violence | 10 | 8 | 0 |
| Sexual assault or abuse | 8 | 6 | 1 |
| Physical abuse | 8 | 10 | 1 |
| Environmental exposure to trauma | 2 | 1 | 3 |
| Total Number of Incidents | 28 | 25 | 5 |
Table 3: Types of trauma experienced and the number of incidents by group.
Mood symptoms
At the time of initial assessment, 8 subjects met symptom threshold criteria for MDD episode (CDRS ≥ 40 BD 5/11 MD 3/11, χ2=0.8, p=0.4), and 6 for mania (YMRS ≥ 20 BD 4/11 MD 2/11, χ2=0.9, p=0.3). The two groups had similar age at onset of mood symptoms (BD 7.3 ± 2.6 versus MD 8.4 ± 1.7, t(15.4)=-1.1, p=0.3). There was a significant difference in the number of lifetime major depressive episodes (BD=18.9 versus MD=4, z(20)=-2.5, p=0.01), and in the number of lifetime manic episodes (BD=17.7 MD=0.3, z(19)=-5.1, p<0.001) (excluding one youth with MD whose manic episodes were “too indistinct or numerous to count”). There were also significant differences in current manic symptoms (past 2 days) as measured by the BPRS mania subscale scores (BD=7.4 ± 4.7 MD=2.2 ± 3.9, t(19.3)=2.8, p=0.01), and YMRS scores (excluding outlier) (BD=19.8 ± 10.7 MD=8.7 ± 8.8, t(18.8)=2.6, p<0.02). There were no differences between the two groups in rates of suicidal ideation (11/11 of BD youth vs 9/11 of MD youth, χ2=2.2, p>0.1) or attempts (9/11of BD youth vs 7/11 MD youth, χ2=0.9, p=0.3).
Family histories
There were higher rates of psychiatric disorders in the families of youth with BD (Table 2). There were significantly higher rates of at least one relative with schizophrenia, or two or more relatives with BD, MDD, and a trend towards higher rates of at least one relative with Anxiety Disorders. Both groups have high rates of substance abuse, although families of youth with BD have significantly more when the raw counts of the number of relatives are analysed (Table 2). There was no significant difference seen in family histories of legal involvement (Table 4).
| BD | MD | ||||||
|---|---|---|---|---|---|---|---|
| n=11 | n=11 | Chi-Square P-value | Chi-Square P-value | P-value * | |||
| History of… | 1 or more | 2 or more | 1 or more | 2 or more | 1 or more | 2 or more | All Counts |
| ADD/ADHD | 8 | 6 | 8 | 2 | 0.9 | 0.08 | 0.12 |
| Anxiety Disorder | 8 | 5 | 5 | 1 | 0.19 | 0.06 | 0.24 |
| Bipolar Disorder | 9 | 7 | 7 | 1 | 0.34 | 0.01 | 0.03 |
| Depression | 8 | 7 | 7 | 2 | 0.65 | 0.03 | 0.01 |
| PDD or Autism | 2 | 1 | 3 | 0 | 0.61 | 0.31 | 0.29 |
| Psychosis | 4 | 0 | 1 | 0 | 0.13 | . | 0.22 |
| Social Phobia | 4 | 0 | 1 | 0 | 0.13 | . | 0.22 |
| Schizophrenia | 6 | 1 | 1 | 0 | 0.02 | 0.31 | 0.07 |
| Substance Abuse | 7 | 5 | 9 | 6 | 0.34 | 0.67 | 0.02 |
| Trouble with the Law | 6 | 2 | 7 | 2 | 0.66 | 0.9 | 0.57 |
| Total Number (Mean, SD) | 11.8 | 7.9 | 6.5 | 4 | . | . | 0.001 |
Table 4: Family history: the number of family relatives with significant history. The values indicate the number of subjects who (1) have at least one relative with a positive history, and (2) have two or more relatives with a positive history. The total number indicates the average number of relatives for each subject across all diagnoses.
Comorbidity and Clinical Correlations
ADHD and PTSD
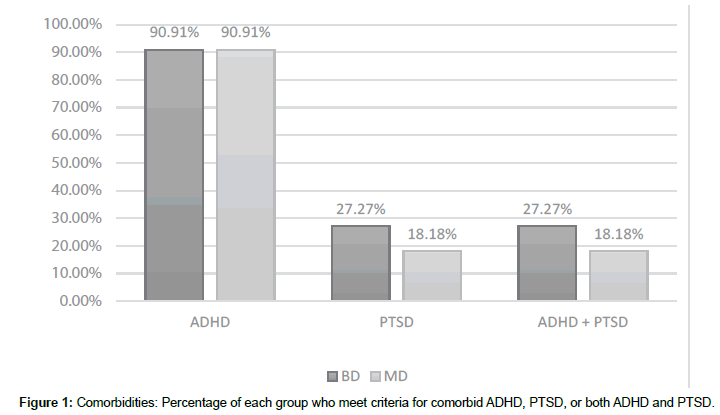
We found that the majority of subject had comorbid ADHD (BD 10/11, MD 10/11) and all subjects who met criteria for PTSD also had ADHD (BD 3/11, MD 2/11; see Figure 1). Subjects who had higher PTSD symptoms (as measured by the PCL-C) also had higher ADHD symptoms (as measured by ADHD-IV) (r(20)=0.8, p<0.001). There was no relationship between PTSD symptoms (as measured by PCL-C) and the number of reported traumatic events (as measured by CTQ) (r(20)=0.01, p=0.9).
Depression and mania
Subjects who had higher depressive symptoms (as measured by CDRS) and manic symptoms (as measured by YMRS), also had higher BPRS total scores (r(20)=0.83, p<0.001 and r(20)=0.69, p<0.001 respectively), suggesting that the severity of mood symptoms has a positive relationship with general behavioral symptoms. In the youth with BD, subjects who had higher depressive symptoms (as measured by CDRS) also had higher concurrent manic symptoms (as measured by YMRS), suggesting mixed episode/symptoms (r(20)=0.49, p=0.02) (Table 5).
| BD | MD | |||||
|---|---|---|---|---|---|---|
| Mean | ± | SD | Mean | ± | SD | |
| BPRS-C Total | 28.1 | ± | 16.7 | 19.6 | ± | 11.9 |
| BPRS-C Mania subscale | 7.4 | ± | 4.7 | 2.2 | ± | 3.9 |
| BPRS-C Depression subscale | 3.5 | ± | 3.8 | 3.6 | ± | 3.5 |
| BPRS-C Behavior subscale | 6.6 | ± | 4.7 | 5.7 | ± | 4.2 |
| YMRS Total* | 19.8 | ± | 10.7 | 8.7 | ± | 8.8 |
| CDRS-R Total | 39.9 | ± | 20.3 | 33.6 | ± | 14.6 |
| CTQ total | 57.4 | ± | 27.7 | 50.9 | ± | 23.6 |
| PCL-C Total | 44.8 | ± | 9.4 | 39.4 | ± | 12.9 |
| ARS-IV Total (Child) | 29.7 | ± | 14.1 | 22.0 | ± | 14.5 |
| ARS-IV Total (Parent) | 33.9 | ± | 12.5 | 33.5 | ± | 10.6 |
Table 5: Means and Standard Deviations (SD) for Rating Scales used in this study.
Number of comorbidities
Twelve subjects had more than two psychiatric disorders, and subjects in the BD group had on average two disorders while subjects in the MD group had on average 1.5 disorders, the most common being ADHD followed by depression. There was no significant difference in the number of comorbid psychiatric disorders between the groups (z=-0.8, p=0.4). However, the number of comorbidities directly correlated with BPRS Total scores (r(20)=0.79, p<0.001) (Figure 1).
Longitudinal data
In the follow up assessment of youth who were determined to have MD at baseline (n=8), parents of two subjects reported a new diagnosis (borderline personality disorder and schizoaffective disorder), and two other subjects (25%) were found to have had a manic episode in the interim. Given that this assessment was conducted by a phone interview with the parents, youth were not given a diagnosis of BD by study clinicians. We were not able to identify predictors for this diagnostic switch. When looking at factors that could be considered as measures of severity at initial assessment, there were no differences in the number of psychiatric medications (t(7.9)=-0.4, p=0.7), out of home placements (χ2=0.4, p=0.5), BPRS mania subscale scores (t(8.7)=0.3, p=0.7) and YMRS scores (t(8.3)=-1.0, p=0.3) in those four MD subjects who were found to have a change in diagnosis compared to the others in the MD group. Additionally, family history of BD or schizophrenia did not predict a diagnostic switch. The interim history suggested that three of those four subjects who switched diagnoses had three out of home placements and one hospitalization, but there continued to be no significant difference in the number of medications between the BD and the MD groups at follow up. There was a possible increase in measures of mania in the follow up assessment, with the BPRS mania subscale increasing by 4.5 points (paired t(7)=-3.2, p=0.01) while YMRS scores were not significantly increased (0.5 points, paired t(7)=-0.2, p=0.9). There was no significant change in BPRS depression and behaviour subscale when comparing the scores from the initial assessment and the follow up assessment of the MD subjects.
Discussion
This study aimed to compare mood symptomatology, clinical correlates and demographics of youth who experienced trauma and presented for treatment with mood symptomatology of two types: those who met diagnostic criteria for BD and those who at the time the study was conducted could best be described as having a mood disorder not otherwise specified. In general, demographics and other measures of clinical severity underscored that the youth in both groups appeared strikingly similar: matched demographics, number of psychotropic medications and out of home placements, age at first exposure to trauma and the types/number of traumatic exposures, age at onset of mood symptoms, and general symptomatology as measured by the BPRS total scores. Additionally, the two groups had similar rates of substance use and legal involvement in their families, suggesting that in general, they were matched in terms of psychosocial adversity that may lead to further traumatization. However, family histories differed in that there were higher rates of any psychiatric disorder in the families of youth with BD, and significantly higher rates of BD, depression, and schizophrenia in the families of youth with BD.
The two groups also differed significantly in other measures. Specifically, the assessment tools we utilized captured the differences in clinical presentations. It is not surprising that youth who met criteria for BD had significantly higher numbers of MDD and manic episodes and mixed symptoms; nevertheless, it is highly reassuring to learn that careful use of those measures can help us differentiate between mood dysregulation which is part of BD and mood dysregulation that is not part of BD. This finding has also been demonstrated in a recent study by the Diler et al. suggesting that measurement of sub-syndromal manic symptoms in youth with BD and unipolar depression during an acute depressive episode can serve to distinguish between the two conditions [29]. However, while the youth in the MD group had a lower rate of mood episodes (MDD, mania and mixed), their mood dysregulation was significant and impairing, as captured by YMRS scores (which captures the past two days of severity of symptoms characterized as mania, but is not diagnostic for manic episodes) and reported suicidality (ideation and attempts). The comorbidity between ADHD and PTSD highlighted important points: the significant clinical challenge of accurately assessing this highly complex group of youth with co-morbid disorders. It emphasizes the overlapping symptomatology that causes diagnostic confusion. The correlations between manic and depressive symptoms appeared in the BD group only and suggest a mixed mood state, further emphasizing the ability of those measures to differentiate between diagnostic groups. In addition, exposure to traumatic events in childhood is known to be correlated not only with PTSD but with other psychiatric disorders, including affective disorders and disruptive behaviour disorders [14].
Our longitudinal data, gathered in 8/11 youth with diagnosed with MD at baseline, showed that 4/8 (50%) youth either received a different diagnosis (n=2), or experienced a manic episode (n=2). This underscores the fact that mood disorder not otherwise specified (MD) is not a final diagnosis, rather a marker for significant evolving psychopathology or perhaps may represent a prodromal state [30].
When we set out to gather these data, we considered that traumatized youth in the MD group would frequently not meet criteria for either PTSD or BD, which we did find in our sample. We were able to confirm that traumatized youth who meet full criteria for BD were more likely to have a family history of BD; however, we did not find that they had mood symptoms predating trauma (rather a similar age at first trauma exposure and occurrence of mood symptoms in both groups), and were unable to identify specific neurovegetative symptom clusters. Additionally, we were unable to identify predictors of progression in MD youth with diagnostic switch, given our small N and the even smaller number of youth who switched.
This study’s limitations include a small N, a clinical evaluation which focused on mood disorders and common comorbidities (rather than using a more inclusive measure such as the K-SADS), lack of a measure assessing anxiety disorders and of a direct assessment of family psychopathology. Additionally, as is inherent in studies with a longitudinal design, we were unable to contact all of the subjects in the MD group and therefore we were only able to collect longitudinal data on 8/11 of our subjects in that group.
Conclusion
The results suggest differences in clinical presentation (higher number of lifetime episodes of MDD and mania and higher rates of current manic symptoms in BD group) and higher rates of schizophrenia, BD and MDD in the families with BD. Taken together, these preliminary results suggest potential biological and genetic vulnerabilities, which may predispose children with histories of CM to develop specific mood disorders under certain circumstances. Better understanding the association between trauma and the development of mood disorders will increase our knowledge of the diverse effects of such events on youths’ emotional and behavioral development. Identifying clinical correlates that help predict later development of BD in mood dysregulated, traumatized youth, will promote future research aimed at identifying biological markers that could aid in early identification and lay the foundation for preventive treatment interventions.
Clinical Significance
The most important and significant finding from our study is highly applicable to community clinicians, who frequently encounter youth with significant trauma histories and mood dysregulation. Clinicians who are at the forefront of treating those youth often face the challenging diagnostic question of wherever these youth also have comorbid BD. We found that a careful and structured diagnostic assessment and the use of clinician administered rating scales can help distinguish between mood dysregulation that is part of BD and therefore accompanied by distinct mood episodes (historically and at the time of the evaluation), and equally debilitating mood dysregulation that is part of other diagnostic entities (including but not limited to PTSD). This has important implications when designing a bio-psycho-social treatment planning.
Acknowledgement
We would like to acknowledge the youth who participated in this study and their families.
Grant Support
Funded by the American Academy of Child and Adolescent Psychiatry supported by Lilly USA, LLC.
References
- Dvir Y, Ford JD, Hill M, BS Frazier (2014) Childhood Maltreatment, Emotional Dysregulation, and Psychiatric Comorbidities. Harvard Rev Psychiat 22:149-161.
- Hovens JG1, Giltay EJ, Spinhoven P, van Hemert AM, Penninx BW (2015) Impact of childhood life events and childhood trauma on the onset and recurrence of depressive and anxiety disorders. J Clin Psychiatry 76: 931-938.
- Mandelli L, Petrelli C, Serretti A (2015) The role of specific early trauma in adult depression: A meta-analysis of published literature. Childhood trauma and adult depression. Eur Psychiatry 30: 665-680.
- Brown GR, McBride L, Bauer MS, Williford WO (2005) Cooperative Studies Program 430 Study Team. Impact of childhood abuse on the course of bipolar disorder: A replication study in U.S. veterans. J Affect Disord 89: 57-67.
- Garno JL, Goldberg JF, Ramirez PM, Ritzler BA (2005) Impact of childhood abuse on the clinical course of bipolar disorder. Br J Psychiatry. 186: 121-125.
- Daruy-Filho L, Brietzke E, Lafer B, Grassi-Oliveira R (2011) Childhood maltreatment and clinical outcomes of bipolar disorder. Acta Psychiatr Scan. 124: 427-434.
- Goldberg JF, Garno JL (2005) Development of posttraumatic stress disorder in adult bipolar patients with histories of severe childhood abuse. J Psychiatr Res 39: 595-601.
- Goldberg JF, Garno JL (2009) Age at onset of bipolar disorder and risk for comorbid borderline personality disorder. Bipolar Disord 11: 205-8.
- Sala R, Goldstein BI, Wang S, Blanco C (2014) Childhood maltreatment and the course of bipolar disorders among adults: Epidemiologic evidence of dose-response effects. J Affective Disord 165: 74-80.
- Romero S, Birmaher B, Axelson D, Goldstein T, Goldstein BI, et al. (2009) Prevalence and correlates of physical and sexual abuse in children and adolescents with bipolar disorder. J Affect Disord 112:144-150.
- Rucklidge JJ (2006) Psychosocial functioning of adolescents with and without paediatric bipolar disorder. J Affective Disord 91 (2-3): 181-188.
- Marchand WR, Wirth L, Simon C (2005) Adverse life events and pediatric bipolar disorder in a community mental health setting. Community Mental Health Journal 41: 67-75.
- Goldstein BI, Strober MA, Birmaher B, Axelson DA, Esposito-Smythers C, et al. (2008) Substance use disorders among adolescents with bipolar spectrum disorders. Bipolar Disord. 10: 496-478.
- American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders (5th ed.). Washington, DC: Author.
- Copeland WE, Keeler G, Angold A, Costello J (2007) Traumatic Events and Posttraumatic Stress in Childhood. Arch Gen Psychiatry. 64: 577-584.
- Matzner F, Silva R, Silvan M, Chowdhury M, Nastasi L (1997) Preliminary Test-retest Reliability of the KID-SCID, Scientific Proceedings, American Psychiatric Association Meeting.
- Faustman WO, Overall JE (1999) Brief Psychiatric Rating Scale. In: The Use of Psychological Testing for Treatment Planning and Outcome Assessment. 791-830.
- Young RC, Biggs JT, Ziegler VE, Meyer DA (1978) A rating scale for mania: Reliability, validity and sensitivity. Br J Psychiatry 133: 429-435.
- Overholser JC, Brinkman DC, Lehnert KL, Riccardi AM (1995) Children's depression rating scale-revised: Development of a short form. J Clin Child Psychol 24: 443-452.
- Bernstein DP, Fink L, Handelsman L, Foote J, Lovejoy M, et al (1990) Initial reliability and validity of a new retrospective measure of child abuse and neglect. Am J Psychiatry 151: 1132-1136.
- Weathers FW, Litz BT, Huska JA, Keane TM (1994) PTSD Checklist—Civilian version. Boston: National Center for PTSD, Behavioral Science Division.
- DuPaul GJ (1998) ADHD rating scale I-IV: Checklists, norms, and clinical interpretation. New York: Guilford Press 24(2).
- Knight J, Shrier L, Bravender T, Farrell M, VanderBilt J, et al. (1999) A new brief screen for adolescent substance abuse. Arch Pediatr Adolesc Med 153: 591-596.
- R Core Team (2017) R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria.
- Venables WN, Ripley BD (2002) Modern Applied Statistics with S-Plus. (4th edtn) Springer, New York, USA.
- Wickham H (2009) ggplot2: Elegant Graphics for Data Analysis. (2nd edtn) Springer-Verlag New York, USA.
- Birmaher B, Axelson D, Goldstein B, Strober M, Gill MK, et al. (2009) Four-year longitudinal course of children and adolescents with bipolar spectrum disorders: The course and outcome of bipolar youth (COBY) study. Am J Psychiatry 166: 795-804.
- American Psychiatric Association (2000) Diagnostic and statistical manual of mental disorders. (4th edtn) Washington, DC, USA.
- Diler RS, Goldstein TR, Hafeman D, Merranko J, Liao F, et al. (2017) Distinguishing Bipolar Depression from Unipolar Depression in Youth: Preliminary Findings. J Child Adolesc Psychopharmacol 27: 310-319.
- Correll CU, Penzner JB, Frederickson AM, Richter JJ, Auther AM, et al. (2007) Differentiation in the Preonset Phases of Schizophrenia and Mood Disorders: Evidence in Support of a Bipolar Mania Prodrome. Schizophrenia Bulletin 33: 703-714.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi