Research Article, J Pulm Med Vol: 5 Issue: 1
Physical Activity and Health Related Quality of Life in Relation to Allergic Disease among Adolescents: Results from a Crosssectional Study
Therese Sterner1,2*, Ada Uldahl1,2, Ake Svensson1, Alf Tunsater3, Cecilia Svedman4, Magnus Bruze4, Laura von Kobyletzki4, Hampus Kiotseridis3, Ann-Britt Zakrisson5, Jonas Bjork6
1Department of Dermatology, Skane University Hospital, Malmo, Sweden
2Department of Clinical Sciences Malmo, Lund University, Malmo, Sweden
3Department of Respiratory Medicine and Allergology, Lund University, Lund, Sweden
4Department of Occupational and Environmental Dermatology, Skane University Hospital, Malmo, Sweden
5University Healthcare Research Center, Orebro University, Orebro, Sweden
6Division of Occupational and Environmental Medicine, Lund University, Sweden, Philippines
*Corresponding Author: T SternerDepartment of Dermatology, Skane University Hospital, Malmo, Sweden Tel: +46 705 404075; E-mail: Therese.Sterner@med.lu.se
Received Date: 14 November, 2020; Accepted Date: 28 December, 2020; Published Date: 04 January, 2021
Citation: Therese S, Ada U, Ake S, Alf T, Cecilia S, et al. (2021) to Allergic Disease among Adolescents: Results from a Crosssectional Study. J Pulm Med 5:1
Abstract
Aim: The overall aim of was to investigate the impact of self-reported allergic disease on physical activity (PA) and health-related quality of life (HRQoL) among adolescents. Methods: A cross-sectional analysis of 1 181 adolescents aged 13-14 years (251 with current allergic disease), participating in the baseline investigation of the Southern Sweden allergy cohort, including a survey with questions on wheeze, rhinoconjunctivitis, eczema, PA and HRQoL. Results: Boys were more physically active than girls (mean total PA score 6.47 vs. 5.98, possible range 3-9). There were no noticeable differences in PA among adolescents with and without allergic disease (p ≥ 0.3 in all comparisons). Clear differences in HRQoL were observed depending on current or previous symptoms. In particular, adolescents with both current asthma and rhinoconjunctivitis scored lower HRQoL than the others. Conclusions: Our results support the importance of having health care measures directed towards promoting PA among adolescents with allergic disease as part of their treatment. The noticeable impaired HRQoL during pollen season in relation to self-reported symptoms Observed in the present study warrants further attention by health care.
Keywords: Adolescent health; Allergy; Asthma; Physical activity; Health-related quality of life
Abbreviations
The International Study of Asthma and Allergies in Childhood (ISAAC); The international Physical Activity Questionnaire (IPAQ); Health Related Quality of Life (HRQoL); Pediatric Allergic Disease Quality of Life Questionnaire (PADQLQ); Physical Activity (PA); Rhinoconjunctivitis (RC).
Introduction
Physical activity (PA) includes varying forms of activities such as sports, playing, gymnastics, exercise or outdoor activities during school-hours and leisure time [1]. The World Health Organization [1] and the Swedish National Board of Health and Welfare, Guidelines for Prevention and Treatment in Unhealthy Living [2] recommend that children and adolescents should accumulate at least 60 min of moderate to vigorous physical activity (PA) every day to achieve positive effects on their health and health-related quality of life (HRQoL). However, it has been reported in several studies that the vast majority (80%) of adolescents worldwide do not meet this recommendation [1,3]. It is known that PA is associated with health and improved psychological well-being among children [4,5]. It is also known that asthma, conjunctivitis and rhinitis are some of the most common allergic diseases worldwide, placing considerable burdens on the individuals and their families [6-8]. Studies have reported that childhood asthma may have negative impact on PA [9-12]. On the other hand, there is also empirical evidence suggesting that PA may protect against asthma symptoms due to the increase of aerobic capacity [13]. However there are little research in associations between PA, HRQoL and allergic disease [14]. HRQoL defines the perceived physical and mental health over time at individual or group level, and is commonly used to investigate the impact of health status on quality of life [14,15]. A general finding from previous research in this area is that allergic disease may have marked consequences in terms of HRQoL among children and adolescents [7,16].Several studies have shown significantly reduced HRQoL in children and adolescents with grass pollen allergy during the pollen season [17,18]. However, research in this field has mainly been focused on individuals with verified allergy-diagnosis, excluding those with self-reported allergic conditions [12]. Thus the overall aim of this study was to investigate the impact of self-reported allergic disease on PA and HRQoL among adolescents.
Methods
Study design
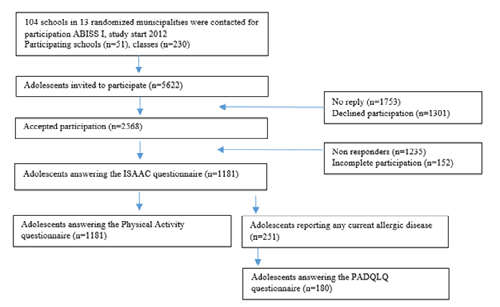
The present study was approved by the Regional Ethics Board in Lund, Sweden (No. 2011/753). It is a cross-sectional analysis of adolescents aged 13-14 years, participating in the baseline investigation of the Southern Sweden allergy cohort, which has been described in detail previously [19]. The cohort was established from a random sample of schools in 13 of 52 municipalities (300 schools for the selected age group) in four counties in southern Sweden. Stratified sampling was done in order to obtain data from both small and large municipalities and from costal as well as rural counties. The location of the school was used as a proxy for the living area (large city, city and countryside), since most children live close to their elementary school in Sweden. Information on the study was sent to the heads and school nurses of 104 schools in 2012. Each head was contacted personally by telephone in order to elicit the school’s participation in the study, resulting in the participation of 51 schools (230 classes in grade 7 and 8). Written information about the study was delivered to the adolescents at school and sent home to their parents. The web-based survey used in this study was completed during school hour in the fall semester (September-November) under the supervision of the school nurse or a teacher. Written informed consent from their guardians were required in order to participate, which was obtained for 2 568 (46%) of the 5622 eligible adolescents attending the participating schools. A flow chart describing recruitment and participation with a total of 1 181 participating adolescents is presented in Figure 1.
Survey
The web-based survey was constructed and provided by Clinical Studies Sweden, Forum South, Skane University Hospital, and Lund, Sweden. The survey comprised mainly of questions from international, validated questionnaires, but a few study-specific questions were also included (see further below). The questionnaire modules for asthma, eczema and rhinoconjunctivitis (RC) from the International Study of Asthma and Allergies in Childhood (ISAAC) [20] were used. The ISAAC questionnaire was designed as a tool for epidemiological research in asthma and allergic diseases, and has been widely used during the past decade [7]. In order to assess HRQoL, we used the Swedish version (LILA) of the disease-specific and validated, Pediatric Allergic Disease Quality of Life Questionnaire (PADQLQ) [21]. This questionnaire was only answered by those who reported any pollen related symptoms. PADQLQ has 26 questions in three domains: 1) Practical domain with questions about symptoms that affect concentration, sleep, hearing, breathing and physical activity (question Q1-7, 26). 2) Physical domain with questions about physical allergy symptoms on airways, eyes, nose, skin, tiredness and thirst (Q8-22). 3) Emotional domain with questions about irritation and fear of having an asthma attack (Q23-25). Each question was answered on a 7 point Likert scale where 0 denotes “not troubled at all” and 6 “extremely troubled”. A mean score (with range 0-6) was calculated for each participant in each of the three domains in PADQLQ.
Three questions about PA designed by the research group specifically for this study were used: I). Think of what you have done during break time at school during the past seven days; how many of these days have you been warm and sweaty after physical activity? Answers were scored as: Low (1)=No day or one day, Medium (2)=Two or three days, High (3)=four or five days. II). Think of what you do after the school day; how many times a week do you exercise and become warm and sweaty? Answers were scored as: Low (1)=Never, more seldom or once a month, Medium (2)=Once a week, High (3)=More than once a week or every day III). Think of the last three days that were not school days; how many of these days did you exercise so that you became warm and sweaty? Answers were scored as: Low (1)=Never, more seldom or once a month, Medium (2)=Once a week, High (3)=More than once a week or every day III). Think of the last three days that were not school days; how many of these days did you exercise so that you became warm and sweaty? Answers were scored as: Low (1)=No day, Medium (2)=One to two days, High (3)=three days. The answers of these three questions were summed up in a total PA score, 3-9. Data on symptoms related to asthma, RC and eczema were obtained from the questionnaire using the definitions given in Table 1.
| Current RC | Current RC | Previous asthma and/or RC | Current eczema |
|---|---|---|---|
| If the respondent answered yes to rhinitis (sneezing, runny or blocked nose | If the respondent answered yes to rhinitis (sneezing, runny or blocked nose without a cold) and conjunctivitis (itchy and/or watery eyes) at any time in their life and during the past year | If the respondent answered yes to asthma and orrhinitis/conjunctivitis, at any time in their life but not during the past year. | If the child answered yes to itching, rash/eczema for six months at any time during their life, and during the past year |
Table 1: Definitions of current allergic symptoms used in this study.
Statistical analysis
Statistical analysis was conducted using SPSS Statistics 25.0 for Windows (SPSS Inc., Chicago, IL, USA). P<0.05 was regarded as statistically significant. D ifferences in PA be tween sy mptom-groups we re te sted using Mann-Whitney test. Differences in mean P ADQLQ scores between symptom-groups were tested using one-way ANOVA overall and independent t-test for subsequent two group comparisons. The Spearman’s rank-correlation coefficient was calculated as a measure of the association between total PA score and PADQLQ.
Results
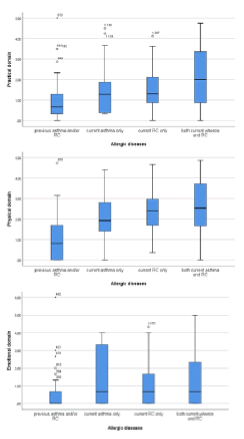
The study population of 1181 participating adolescents consisted of 50% girls, mean age was 13.5 years, 96% were born in Sweden and 12% were exposed to smoking within the family. Data on school location, eczema and BMI are presented in Table 2 in four groups with current symptoms (n=251 in total): Current asthma-only (6.9%), current RConly (10.2%), both current asthma and RC (4.2%) and neither RC nor asthma currently (78.7%). There were no clear differences in symptoms across school locations. The prevalence of eczema was significantly higher in all symptom groups than in the non-symptomatic group (p<0.001 in all three comparisons). The mean BMI [22] of the participants in this study was in the normal range and there were no apparent differences across the symptom groups. Boys were more physically active than girls (mean total PA score 6.47 vs. 5.98, possible range 3-9; Table 3). There were no noticeable differences in PA among adolescents with and without allergic disease (p ≥ 0.3 in all comparisons). When the analysis was conducted separately for boys and girls, still no differences in PA were apparent across the groups (results not shown). The proportion of participants reporting PA classified as high was 19% for school breaks, 67% after school and 29% for school-free days (Table 3). Only 29% of the boys and 22% of the girls reported PA classified as high both after school and during school free days. There were 180 participants with allergic symptoms during pollen season who answered the PADQLQ about HRQoL. The ANOVA test showed strong empirical evidence for differences in all three dimensions of HRQoL depending on current or previous symptoms (p≤0.004) (Table 4). Likewise, there were strong empirical evidence suggesting that adolescents with both current asthma and RC (n=29) had lower HRQoL in all three domains compared to those with only one current or no current symptom (n=152; p≤0.005; not in tables) the differences between the groups in the three domains are further illustrated in Figure 2. The correlation between total PA score and the three domains of HRQoL was consistently low (Spearman´s rank-correlation coefficient -0.14, -0.11 and -0.08, respectively).
| Current asthma only |
Current RC only | Both current asthma and RC |
No asthma or RC | All Participants |
||
|---|---|---|---|---|---|---|
| n | 81 | 120 | 50 | 930 | 1 181 | |
| Gender, n(%) | Female 38 | (46.9) | 62 (51.7) | 23 (46.0) | 469 (50.4) | 592 (50.1) |
| Male | 43 (53.1) | 58 (48.3) | 27 (54.0) | 461 (49.5) | 589 (49.9) | |
| BMI* mean (range) | 20.48 (14-29) | 19.44 (14-28) | 19.44 (13-28) | 19.77 (12-35) | 19.77 (12-35) | |
| School-location, n(%) | Large city) | 20 (24.7) | 27 (22.5) | 10 (20.0) | 214 (23.0) | 271 (22.9 |
| City | 39 (48.1) | 61 (50.8) | 28 (56.0) | 448 (48.1) | 576 (48.8) | |
| Countryside | 22 (27.2) | 32 (26.7) | 12 (24.0) | 268 (28.8) | 334 (28.3) | |
| Eczema, n(%) | 22 (27.2) | 30 (25.0) | 18 (36.0) | 145 (15.6) | 215 (18.2) | |
| *BMI: age 13 male<21.90, female 22.57, age 14 male<22.61, female<23.33 (limits for overweight) | ||||||
Table 2: Basic characteristics of the study population (n=1 181 respondents), stratified by self-reported current allergic symptoms.
| Physical activity | Current asthma only |
Current RC only 1 missing |
Both current asthma and RC |
No current asthma or RC |
All participan ts |
p-value | |
|---|---|---|---|---|---|---|---|
| n | 81 | 119 | 50 | 925-927 | 1175-1177 | ||
| PA total score, mean (SD) range 3-9 |
Boys | 6.47 (1.50) | 6.46 (1.64) | 6.44 (1.89) | 6.47 (1.67) | 6.47 (1.66) | 0.3 |
| Girls | 6.00 (1.25) | 5.92 (1.57) | 5.70 (1.49) | 6.00 (1.47) | 5.98 (1.47) | 0.4 | |
| PA during break time at school *n=1177(%) 4 missing |
Low | 40 (49.3) | 72 (60.5) | 26 (52.0) | 502 (54.2) | 640 (54.3) | 0.5 |
| Medium | 27 (33.3) | 26 (21.8) | 14 (28.0) | 249 (26.8) | 316 (26.8) | ||
| High | 14 (17.2) | 21 (17.6) | 10 (20.0) | 176 (18.9) | 221 (18.8) | ||
| PA after school day **n=1176 (%) 5missing |
Low | 10 (12.3) | 23 (19.3) | 13 (26.0) | 173 (18.6) | 219 (18.6) | 0.3 |
| Medium | 16 (19.7) | 18 (15.1) | 7 (14.0) | 130 (14.0) | 171 (14.5) | ||
| High | 55 (67.9) | 78 (65.5) | 30 (60.0) | 623 (67.2) | 786 (66.8) | ||
| PA during the previous 3 schoolfree days *** n=1175 (%) 6 missing |
Low | 16 (19.7) | 21 (17.6) | 12 (24.0) | 177 (19.1) | 226 (19.2) | 0.4 |
| Medium | 48 (59.2) | 58 (48.7) | 22 (44.0) | 480 (51.7) | 608 (51.7) | ||
| High | 17 (20.9) | 40 (33.6) | 16 (32.0) | 268 (28.0) | 341 (29.0) | ||
| *Low=No day or one day, Medium=Two or three days, High=four or five days. ** Low=Never, more seldom or once a month, Medium=Once a week, High=More than once a week or every day. *** Low=No day, Medium=One to two days and High=three days | |||||||
Table 3: Self-reported physical activity (PA) among the study participants, stratified by selfreported current allergic symptoms.
| n=180 *Likert scale 0-6 |
Current asthma only | Current RC only | Both current asthma and RC |
Previous asthma and/or RC |
p-value |
|---|---|---|---|---|---|
| n | 18 | 62 | 29 | 71 | |
| Practical domain mean (range) |
1.62 (0.30-4.50) | 1.56 (0-4.13) | 2.24 (0-4.75) | 0.93 (0-5.0) | <0.001 |
| Physical domain mean (range) |
2.12 (0-4.40) | 2.39 (0.36-4.67) | 2.63 (0-4.87) | 0.99 (0-4.73) | 0.004 |
| Emotional domain mean (range) |
1.29 (0-4.00) | 1.04 (0.0-4.33) ” |
1.51 (0.0-5.0) | 0.47 (0-6.0) | 0.001 |
| *0=“not troubled at all” and 6=“extremely troubled | |||||
Table 4: HRQoL scores obtained from the PADQLQ-questionnaire in relation to selfreported current or previous allergic symptoms.
Figure 2: Differences between the symptom groups; previous asthma and/or RC, current asthma only, current RC only, and current asthma and RC, in the three domains of HRQoL. a) Practical domain, b) Physical domain and c) Emotional domain. HRQoL scores from the 7-point Likert scale used in the PADQLQ-questionnaire are given on the Y-axis were 0 denotes “not troubled at all” and 6 “extremely troubled”.
Discussion
There were two salient findings in the present study. Firstly, there were no noticeable differences in PA among adolescents with or without allergic disease. Secondly, clear differences in HRQoL were observed depending on current or previous symptoms. In particular, adolescents with both current asthma and RC scored lower HRQoL than the others. Our results support the importance of having health care measures directed towards promoting PA among adolescents with allergic disease as part of their treatment [2]. Adherence to such recommendations and guidelines could be one of the reason why adolescents with and without allergic disease were equally active in the present study. Both current and previous asthma were associated with lower PA in a cross-sectional study of adolescents in 2002 in Denmark [23]. This is a finding that could not be confirmed in our study. Our study was smaller and thus more statistically uncertain, but another potential explanation for the differences could be that our study represents more recent birth cohorts where PA among individuals with allergic disease has been promoted. Other studies on PA and asthma control among adolescents reported similar results with no associations between asthma symptoms and PA in line with the present study [11,24]. Adolescents who participate regularly in physical activities are more likely to have better general health than those who never participate in physical activities [12,25,26]. The finding that adolescents with both current asthma and RC had lower HRQoL in all three domains during the pollen season, compared to those with only one current or no current symptom, is in line with previous studies [7,14,16,27,28]. The newly updated, ARIA (Allergic Rhinitis and its Impact on Asthma) guidelines with the approach to provide an active and healthy life to this patient group and to stress the importance of HRQoL instruments in clinical practice to evaluate and treat symptoms, using mobile technology [29]. PA during the school day may have many positive effects. As an example frequent PA at school was associated with higher final grades for boys in a recent study [30]. Many of the adolescents in our study were not physically active during break time at school that might have been due to short pauses or not enough stimulating environment in the schoolyards. It is thus important to promote PA at school, which could be done by investments in both school and surrounding environments [31].
Strengths and limitations
A major strength of the present study was the population-based design, with a broad range of questions covering previous and current symptoms resulting from respiratory allergy, daily PA and HRQoL during the pollen season. Validated questionnaires, ISAAC and PADQLQ were to a large extent used to ensure that the results of the study were comparable to those from other investigations. The PADQLQ is a disease specific questionnaire used to obtain an overview of the HRQoL among a large population. The questionnaire is not specific to each individual, and important information could therefore be missed [21]. Another limitation was that the questions about PA were study-specific and not validated. On the other hand, the expected higher PA level among boys than among girls was confirmed in our study, and the associations found were in line with other studies [11,24]. The study size made it impossible to assess PA using accelerometers. An additional noteworthy limitation was the low rate of participation regarding both the number of schools that agreed to participate, and the number of adolescents participating from each school. Finally, as this is a cross-sectional study, no firm conclusions about causality can be drawn.
Conclusions
Our results support the importance of having health care measures directed towards promoting PA among adolescents with allergic disease as part of their treatment. The noticeable impaired HRQoL during pollen season in relation to allergic disease observed in the present study warrants further attention by health care. The finding that only a minority of both boys and girls, irrespective of allergic disease, reported PA classified as high both after school and during school-free days also calls for further investigations.
Acknowledgements
The authors would like to thank Elisabeth Holmner, asthma and allergy nurse at Skåne University Hospital, for the coordination and implementation of this study and her great enthusiasm, and professor Leif Bjermer for his invaluable help in study planning.
Conflict of interest
All authors declare no conflicts of interest.
Funding
This work was supported by a scholarship to the main author from The Swedish Asthma, Allergy-and COPD nurses Association (ASTA).
References
- WHO. Global Strategy on Diet, Physical Activity and Health. Intensity of physical activity.
- Socialstyrelsen (2017) Swedish National Board of Health and Welfare, Guidelines for Prevention and Treatment in unhealthy living. Swedish.
- Guthold R, Stevens GA, Riley LM (2020) Global trends in insufficient physical activity among adolescents: A pooled analysis of 298 population-based surveys with 1.6 million participants. Lancet Child Adolesc Health 4: 23-35.
- White J, Jago Rs (2013) Fat distribution, physical activity and cardiovascular risk among adolescent girls. Nutr Metab Cardiovasc Dis 23: 189-195.
- Sebire SJ, Haase AM, Montgomery AA (2014) Associations between physical activity parenting practices and adolescent girls’ selfperceptions and physical activity intentions. J Phys Act Health 11: 734-740.
- Hellgren J, Cervin A, Nordling S, Bergman A, Cardell LO, et al. (2010) Allergic rhinitis and the common cold high cost to society. Allergy 65: 776-783.
- Blaiss MS, Hammerby E, Robinson S, Kennedy-Martin T, Buchs S (2018)The burden of allergic rhinitis and allergic rhinoconjunctivitis on adolescents: A literature review. Ann Allergy Asthma Immunol 121: 43-52
- Bousquet J (2019) The Msg. Correction to: Guidance to 2018 good practice: ARIA digitally enabled, integrated, person-centred care for rhinitis and asthma. Clin Transl Allergy; 9: 52.
- Yiallouros PK, Economou M, Kolokotroni O (2015) Gender differences in objectively assessed physical activity in asthmatic and non-asthmatic children. Pediatr Pulmonol 50: 317-326.
- Wanrooij VH, Willeboordse M, Dompeling E (2014) Exercise training in children with asthma: A systematic review. Br J Sports Med 48:1024-1031.
- Strom MA, Silverberg JI (2016) Associations of Physical Activity and Sedentary behavior with Atopic Disease in United States Children. J Pediatr 174:247-253-e243.
- Mitchell EA, Beasley R, Bjorksten B, Crane J, Garcia-Marcos, et al. (2013) Isaac Phase Three Study Group. The association between BMI, vigorous physical activity and television viewing and the risk of symptoms of asthma, rhinoconjunctivitis and eczema in children and adolescents: ISAAC Phase Three. Clin Exp Allergy 43.
- Crosbie A (2012) The effect of physical training in children with asthma on pulmonary function, aerobic capacity and health-related quality of life: a systematic review of randomized control trials. Pediatr Exerc Sci 24: 472-489.
- Solans M, Pane S, Estrada MD, Serra-Sutton V, Berra S, et al. (2008) Health-related quality of life measurement in children and adolescents: A systematic review of generic and disease specific instruments. Value Health 11:742-764.
- Wallander JL, Schmitt M, Koot HM (2001) Quality of life measurement in children and adolescents: Issues instruments, and applications. J Clin Psychol 57: 571-585.
- Jonsson M, Bergstrom A, Egmar AC (2016) Asthma during adolescence impairs health-related quality of life. J Allergy Clin Immunol Pract 4: 144-146
- Kiotseridis HCCM, Bjermer L, Aurivillius M, Jacobsson H, Dahl A, et al. (2013) Grass pollen allergy in children and adolescentssymptoms, health related quality of life and the value of pollen prognosis. Clin Transl Allergy 3:19.
- Sterner T, Uldahl A, Svensson A, Bjork J, Svedman C, et al. (2018) The Southern Sweden Adolescent Allergy-Cohort: Prevalence of allergic diseases and cross-sectional associations with individual and social factors. J Asthma 1-9.
- Asher MI, Keil UAHR, Beasley R, Crane J, Martinez F, et al. (1995) International Study of Asthma and Allergies in Childhood (ISAAC): Rationale and methods. Eur Respir J 8:483-491.
- Kiotseridis HCCM, Bjermer L, Aurivillius M, Jacobsson H, Dahl A, et al. (2011) Swedish translation and validation of the Pediatric Allergic Disease Quality of Life Questionnaire (PADQLQ). Acta Paediatr 100: 242-247.
- Cole TJ, Bellizzi MC, Flegal KM (2000) Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 320: 1240-1243.
- Lochte L, Petersen PE, Nielsen KG (2018) Associations of physical activity with childhood asthma, a population study based on the WHO health behaviour in school-aged children survey. Asthma Res Pract 4: 6.
- Matsunaga NY, Oliveira MS, Morcillo AM, Ribeiro JD, Ribeiro Mago, et al. (2017) Physical activity and asthma control level in children and adolescents. Respirology 22: 1643-1648.
- Groth SW, Rhee H, Kitzman H (2016) Relationships among obesity, physical activity and sedentary behavior in young adolescents with and without lifetime asthma. J Asthma 53:19-24.
- Wafa SW, Shahril, Ahmad, Zainuddin, Ismail, et al. (2016) Association between physical activity and health-related quality of life in children: a cross-sectional study. Health Qual Life Outcomes 14: 71.
- Hallstrand TS, Curtis, Aitken, Sullivan (2003) Quality of life in adolescents with mild asthma. Pediatr Pulmonol 36: 536-543.
- Cibella FFG, Cuttitta G, Bucchieri S, Melis MR, La Grutta S, et al. (2015) The burden of rhinitis and rhinoconjunctivitis in adolescents. Allergy Asthma Immunol Res 7: 44-50.
- Bousquet J, Hellings PW, Agache I (2019) Allergic Rhinitis and its Impact on Asthma (ARIA) Phase 4 (2018): Change management in allergic rhinitis and asthma multimorbidity using mobile technology. J Allergy Clin Immunol 143: 864-879.
- Coster ME, Fritz J, Karlsson C, Rosengren BE, Karlsson, et al. (2018) Extended physical education in children aged 6-15 years was associated with improved academic achievement in boys. Acta Paediatr 107: 1083-1087.
- Ketteridge A, Boshoff K (2008) Exploring the reasons why adolescents participate in physical activity and identifying strategies that facilitate their involvement in such activity. Aust Occup Ther 55: 273-282.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi