Case Report, Int J Ophthalmic Pathol Vol: 12 Issue: 1
Postoperative Lens Material of the Eyelid after Cataract Surgery Masquerading as Phakomatous Choristoma
Keiko Inouye1, Harris Ahmed2*, Soungmin Cho2, Kelly Keefe2 and Douglas Van Putten2
1College of Osteopathic Medicine, Western University, Pomona, United States of America
2Department of Ophthalmology, Loma Linda University, Loma Linda, United States of America
*Corresponding Author: Harris Ahmed
Department of Ophthalmology, Loma
Linda University, Loma Linda, United States of America
E-mail: hahmed@llu.edu
Received date: 04 March, 2023, Manuscript No. IOPJ-23-91369;
Editor assigned date: 08 March, 2023, PreQC No. IOPJ-23-91369 (PQ);
Reviewed date: 22 March, 2023, QC No. IOPJ-23-91369;
Revised date: 29 March, 2023, Manuscript No. IOPJ-23-91369 (R);
Published date: 05 April, 2023, DOI: 10.4172/2324-8599.12.1.2
Citation: Inouye K, Ahmed H, Cho S, Keefe K, Putten DV (2023) Postoperative Lens Material of the Eyelid after Cataract Surgery Masquerading as Phakomatous Choristoma. Int J Ophthalmic Pathol 12:1.
Abstract
Cataract surgery is the most commonly performed surgery worldwide. Despite the prevalence in reports of retained lens tissue following surgery, there is no documentation of the tissue being deposited outside of the eye. Additionally, there are only a few reported cases of retained capsular tissue as a result of surgery. Here, we present a case of an elderly patient with an upper eyelid lesion containing a fragment of the basement membrane and proteinaceous lens-like material, initially mistaken as phakomatous choristoma that was later confirmed to be postoperative capsular material embedded into the eyelid.
Keywords: Lens; Capsule; Phakomatous choristoma; Cataract surgery
Introduction
Cataract surgery is the most commonly performed procedure worldwide with an estimated 20 million procedures done annually [1]. Complications of cataract surgery include posterior capsular rupture with vitreous loss, dropped or retained crystalline lens, infection, and inflammation. Retained lens fragments after cataract surgery can lead to a severe inflammatory reaction, increased intraocular pressure, macular or corneal edema, or event permanent vision loss [2,3]. Retained lens fragments are usually identified within days of the postoperative period, although there are reports of patients presenting with retained lens fragments as late as 65 years after the procedure [4].
In this report, we discuss a patient presenting approximately two years after surgery with a suspected chalazion that, upon biopsy, contained proteinaceous material resembling a crystalline lens and a fragment of smooth basement membrane resembling a lens capsule. Phakomatous choristoma, a rare tumor reported only in pediatric patients, was considered initially due to this lesion’s unusual histological appearance. Further evaluation showed that the lesion was more consistent with capsular tissue that had embedded into the tarsal conjunctiva following cataract surgery. Until now, there have been no documented reports of lens or capsular tissue being deposited outside of the eye following cataract surgery.
Case Presentation
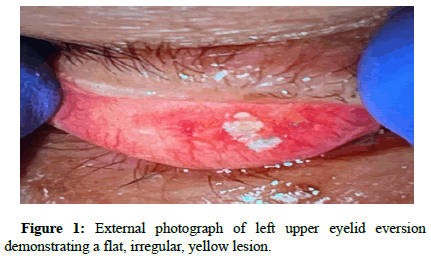
An 88-year-old female presented to the office after referral for a suspected chalazion of the left upper eyelid. Cataract surgery was performed approximately two years prior to the visit with no complications. The patient noted stable visual acuity and persistent itching but denied any eye pain. Slit lamp exam and upper lid eversion revealed a lesion thought to be a chalazion versus an embedded foreign body. The patient subsequently underwent excision in-office and the specimen was sent to pathology to rule out possible malignancy (Figure 1).
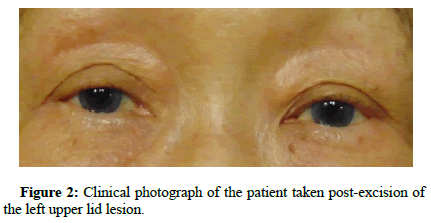
She accepted any risks associated with the procedure and agreed to proceed. The procedure was performed using topical and local anesthesia in the left upper eyelid. The lesion was excised with no complications and sent to pathology. She tolerated the procedure well and left in good condition (Figure 2).
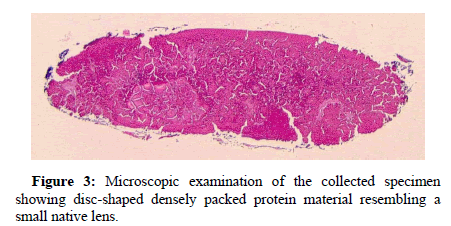
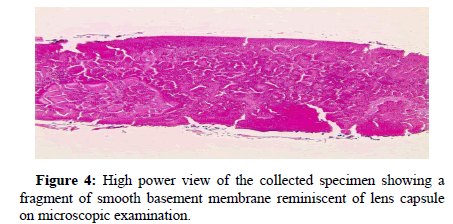
On gross examination, the specimen was less than 1 gram, 0.2 × 0.2 × 0.1 cm, and red-tan in color. Histological examination revealed a disc-shaped densely packed protein material resembling a small native lens (Figure 3). High power view showed a fragment of smooth basement membrane partially encompassing the proteinaceous material, reminiscent of lens capsule (Figure 4).
MRI of the brain was ordered as part of the initial evaluation to rule out other or concurrent orbital or extra ocular lesions. This imaging revealed moderate cerebral atrophy and non-specific white matter changes as well as changes possibly related to chronic hypertension, but no periocular or orbital lesions were present.
Results and Discussion
The patient was originally referred for a suspected chalazion. Chalazia generally present on the upper eyelid due to the increased concentration of meibomian glands on the tarsal plate of the upper lid. Like this patient, those presenting with chalazia may complain of nonspecific symptoms such as discomfort or a foreign body sensation [5].
The specimen collected during biopsy revealed densely-packed proteinaceous material resembling a crystalline lens encompassed by a small fragment of basement membrane, reminiscent of phakomatous choristoma. Although, phakomatous choristoma stain similar to lens tissue and epithelium, they do not take on the shape of a crystalline lens and are not composed of densely packed proteinaceous material. These tumors present on H & E staining with aggregates of cuboidal cells with surrounding pseudo-glandular structures and a characteristic Periodic Acid-Schiff (PAS)-positive basement surrounding the ectopic lens cells, resembling a lens capsule. Scarcities of cytoplasmic organelles and “bladder” or Wedl cells, which are found in cataractous lenses, have been noted [6-9]. Immunohistochemistry will stain positive for S-100 as well as crystalline and vimentin, which are specific to human lenticular tissue. They also stain negative for cytokeratin, which is present in other epithelial cells throughout the body [10,11]. Neuron specific enolase, which has moderate activity in lens epithelium during early stages of development, is found to be positive in these tumors [12,13]. Additionally, phakomatous choristoma usually involve the inferomedial eyelid or the anterior orbit and not the upper eyelid [7].
In this case, further review by an ophthalmic pathologist revealed that it was truly an unusual presentation of phakomatous choriostoma given the patient’s older age. The external photograph of the everted upper lid was also provided to the pathologist. Given its superficial location, patient age, and history, it was decided that this was more consistent with retained anterior capsule embedded into the tarsal conjunctiva following prior cataract surgery. Since the procedure was reportedly uncomplicated, it was theorized that the tissue removed from the anterior capsule following the capsulorhexis was deposited along the conjunctiva and eventually embedded as it healed. Additionally, the use of a wire versus plate speculum could have allowed the tissue to deposit in the lid due to the exposed conjunctiva. There is one other reported case of retained capsular material following an uncomplicated cataract surgery. In this case, the capsule adhered to the anterior chamber of the eye, masquerading as Descemet’s membrane detachment, and presented with corneal edema and decreased visual acuity [14].
Retained fragments of lens tissue are rare complications of cataract surgery. They occur most commonly due to low levels of surgical experience or complicated cases [15]. Smaller retained fragments or nuclear tissue may be treated conservatively with observation and corticosteroids, however, larger fragments are removed surgically. Depending on the location of the fragment, greater measures may be taken for removal; fragments depositing in the back of the eye often require vitrectomy to remove them [3]. In order to prevent retained fragments, measures must be taken to ensure that the nuclear material is cleared completely. Patients with smaller pupils are at higher risk of fragments depositing between the anterior capsule and posterior iris [16]. Retained fragments within the eye commonly present with irritation and edema. Even with the nuclear tissue being deposited outside of the eye, our patient presented with irritation and foreign body sensation. If left untreated, retained nuclear material can result in permanent vision loss.
Conclusion
Until now, there have been no reported cases of lens or capsular tissue depositing outside of the eye following cataract surgery. The tissue was likely deposited following the capsulorhexis in an otherwise uncomplicated procedure. In patients presenting with lesions of the upper eyelid following cataract surgery, embedded capsular tissue should be included on a list of possible diagnoses in addition to through history taking and slit lamp examinations.
Disclosure Statement
The authors have no conflicts of interest to disclose.
References
- Rossi T, Romano MR, Iannetta D, Romano V, Gualdi L, et al. (2021) Cataract surgery practice patterns worldwide: a survey. BMJ Open Ophthalmol 6: e000464.
[Crossref] [Google scholar] [Indexed]
- Tien T, Crespo MA, Milman T, Syed ZA (2022) Retained lens fragment presenting 32 years after cataract extraction. Am J Ophthalmol Case Rep 26: 101546.
[Crossref] [Google scholar] [Indexed]
- Salabati M, Mahmoudzadeh R, Wakabayashi T, Hinkle JW, Ho AC (2022) Indications for surgical management of retained lens fragments. Curr Opin Ophthalmol 33: 15-20.
[Crossref] [Google scholar] [Indexed]
- Barnhorst D, Meyers SM, Myers T (1994) Lens-induced glaucoma 65 Years After congenital cataract surgery. Am J Ophthalmol 118: 807-808.
[Crossref] [Google scholar] [Indexed]
- Gordon AA, Danek DJ, Phelps PO. (2020) Common inflammatory and infectious conditions of the eyelid. Dis Mon 6: 101042.
[Crossref] [Google scholar] [Indexed]
- Harris BF, Harris JP, Ducey TJ, Boden JH, Yakopson VS (2019) Phakomatous choristoma of the orbit with involvement of the inferior oblique muscle. Ophthalmic Plast Reconstr Surg 35: e10-e19.
[Crossref] [Google scholar] [Indexed]
- Jung EH, Avila SA, Gordon AA, de la Garza AG, Grossniklaus HE (2022) Phakomatous choristomas: A case report and review of literature. Ophthalmic Plast Reconstr Surg 38: 330-335.
[Crossref] [Google scholar] [Indexed]
- Tripathi RC, Tripathi BJ, Ringus J (1981) Phakomatous choristoma of the lower eyelid with psammoma body formation. Ophthalmology 88: 1198-1206.
[Crossref] [Google scholar] [Indexed]
- McMahon RT, Font RL, McLean IW (1976) Phakomatous choristoma of eyelid: Electron microscopical confirmation of lenticular derivation. Arch Ophthalmol 94: 1778-1781.
[Crossref] [Google scholar] [Indexed]
- Ellis FJ, Eagle RC, Shields JA, Shields CL, Fessler JN, et al. (1993) Phakomatous choristoma (zimmerman’s tumor):Immunohistochemical confirmation of lens-specific proteins. Ophthalmology 100: 955-960.
[Crossref] [Google scholar] [Indexed]
- Rafizadeh SM, Ghadimi H, Nozarian Z (2020) Phakomatous choristoma of the eyelid and orbit: A case report. Pediatr Dev Pathol 23: 296-300.
[Crossref] [Google scholar] [Indexed]
- Kamada Y, Sakata A, Nakadomari S, Takehana M. (1998) Phakomatous choristoma of the eyelid: Immunohistochemical observation. Jpn J Ophthalmol 42: 41-45.
[Crossref] [Google scholar] [Indexed]
- Shin HM, Song HG, Choi MY (1999) Phakomatous choristoma of the eyelid. Korean J Ophthalmol 13: 133-137.
[Crossref] [Google scholar] [Indexed]
- Sarkar P, Gandhi HC, Gupta MK, Tembhurde PM (2020) Retained anterior capsule: A masquerader of Descemet’s membrane detachment. Indian J Ophthalmol 68: 2528.
[Crossref] [Google scholar] [Indexed]
- Helayel HB, Alyahya AA, Owaifeer AMA, Khan AM, Zahrani ATA, et al. (2022) Risk factors, complications, and outcomes of phacoemulsification cataract surgery complicated by retained lens fragments in Asian eyes: A 10-year retrospective study. Saudi J Ophthalmol 36: 171-176.
[Crossref] [Google scholar] [Indexed]
- Devgan U (2019) Removing and preventing retained lens fragments. Ophthalmology Management 23: 60-64.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi