Research Article, Arch Med Biotechnol Vol: 1 Issue: 1
Prevalence of Women Taking Iron-Folic Acid (IFA) During Pregnancy and its Impact on Child’s Birth Weight
Deo Sushma1, Pandey Shila2 and Kharel Sushil3*
1Department of Pharmacology, Gandaki Medical College and Teaching Hospital, Pokhara, Nepal
2Jaya Multiple Campus, Kathmandu, Nepal
3Department of Physiology, Kathmandu Medical College and Teaching Hospital, Kathmandu, Nepal
*Corresponding Author : Kharel Sushil
Department of Physiology, Kathmandu Medical College and Teaching Hospital, Kathmandu-44600, Nepal
Tel: +9771-4476152
E-mail: drsushilkharel@gmail.com
Received: April 02, 2018 Accepted: May 24, 2018 Published: May 30, 2018
Citation: Sushma D, Shila P, Sushil K (2018) Prevalence of Women Taking Iron-Folic Acid (IFA) During Pregnancy and its Impact on Child’s Birth Weight. Arch Med Biotechnol 1:1.
Abstract
1.1. Introduction
Pregnancy is a crucial period with increased metabolic demands. Vitamins, minerals and folic acids are the major determinants of not only the child’s health but also the pregnant woman.
1.2. Objective
To evaluate maternal intakes of iron-folic acids during pregnancy and assess its impact on child’s birth weight.
1.3. Materials and methods
A cross-sectional study was conducted among 290 women with live birth in Kathmandu, Nepal. In this study, maternal intake of iron-folic acid during pregnancy was assessed by a questionnaire and birth weight of child was verified by the certificate issued by the Hospital. The correlation between these intakes and birth weight were evaluated and analyzed.
1.4. Results
Prevalence of women taking iron-folic acid during pregnancy was 58.87%. This study found the positive association of the folic acid consumption of mothers on birth weight of their child, 79.65% of child with normal birth weight were the child whose mothers took iron-folic acid during the pregnancy whereas only 4.67% child were of normal birth weight whose mothers were not taking iron-folic acid during pregnancy. Folic acid intake during pregnancy was significantly associated with birth weight of child (P < 0.05).
Conclusion: Intake of folic acid by pregnant women was strongly related to normal birth weight of the child. So country level awareness campaign on iron-folic acid intake and other vitamins during pregnancy should be emphasized to make our society, country and the world healthy with normal birth weight child.
Keywords: Folic acid; Child birth weight; Pokhara
Introduction
Iron-Folic acid (FA) has been shown to be effective in decreasing the risk of neural tube defects (NTD) [1]. Folic acid plays a significant role in the physiological metabolism of nucleic acid synthesis and cell division [2]. During pregnancy, folic acid intake is essential for rapid cell and tissue growth of the placenta and the uterus, growth of the fetal child and increment of the maternal blood volume [3]. During pregnancy, folic acid requirements are 5- to 10-fold higher so pregnant women may be at the vulnerable risk for folic acid deficiency during pregnancy [4]. Daily prenatal use of iron with folic acid remarkably improves child’s birth weight, eventually reducing the risk of Low birth weight [5]. Folic acid consumption is prescribed before conception, to prevent development of spina bifida and other neural tube defects. It should be consumed at least 0.4 mg/day during the first trimester of pregnancy, 0.6 mg/day during the pregnancy, and 0.5 mg/day during breastfeeding with other eating foods rich in folic acid [6]. Folic acid deficiency might result in abnormal cellular growth and the effects are shown most on those tissues which grow most rapidly [7].
A good review by Fekete et al. [8] stated that an effect of FA supplementation on absolute birth weight. The Generation R study has found that the lowest folic acid levels are mostly correlated with lower placental weights and birth weight [9,10].
Different studies have focused on a positive correlation between the consumption of iron- folic acid supplements during pregnancy and birth-weight of child. Two follow-up studies of cluster randomized controlled trials from Nepal and China had evaluated the long term impact of iron-folic acid supplements on the physical growth status of children. A study from Bangladesh found a significantly higher incidence of childhood stunting in children whose mother did not use IFA (Iron-Folic acid) supplementation during pregnancy [11-14].
Methods
This was a cross-sectional study conducted in Kathmandu. The study was conducted in Feb-April, 2017. Before the examination, the purpose of the study was explained to all the participants and informed written consent was taken from the mothers before collecting any form of data. For the study, 290 mothers with live birth of different age group were selected randomly from different wards of Kathmandu. The mothers were given self-designed structured questionnaire. Hospital records for child’s birth weight were taken. During primary selection, all the subjects were interviewed thoroughly to know their medical history, food habits, economic status etc. Child under 2500 gm at the time of birth was considered as low birth weight [15]. All the mothers with live birth and who were cooperative were included in the study. The data was analyzed using SPSS version 21.Chi Square test was done to predict the P value. P<0.05 was considered statistically significant.
Results
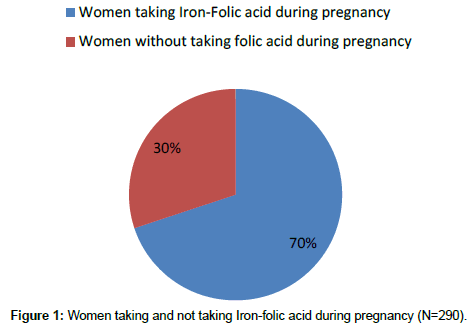
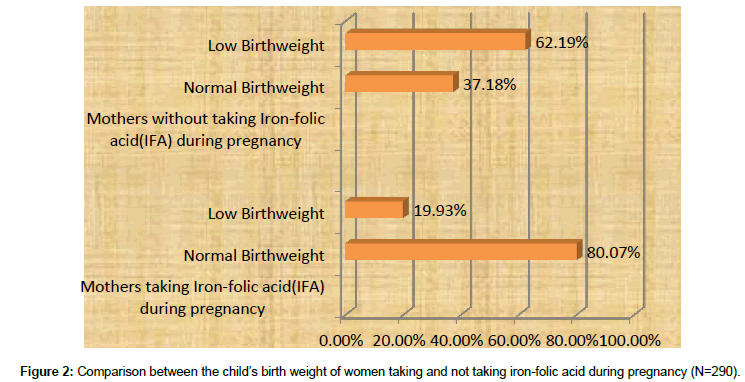
In our study, the mean age of mothers were 24 ± 2.86 those taking folic acid during pregnancy and 26 ± 5.97 not taking folic acid during pregnancy (Table 1). Prevalence of women taking folic acid during was 69.87% (Figure 1). Normal birth weight was seen in high percentage (80.07%) among the mothers who took folic acid during pregnancy. On the other hand, among mothers who did not take folic acid during pregnancy only 37.81% were the child with normal birth weight (Table 2). Even the mothers who took folic acid during the pregnancy gave low birth weight child which was 19.93% (55). This figure was significantly high in child (62.19%) whose mothers did not take folic acid during pregnancy (Figure 2).
| Variables (mothers) | Mothers taking Iron-folic acid (Mean ± SD) | Mothers not taking folic acid (Mean ± SD) |
|---|---|---|
| Age (Years) | 24 ± 2.86 | 26 ± 5.97 |
| Height (meters) | 1.55 ± 0.36 | 1.52 ± 0.27 |
| Weight (Kg) | 67 ± 8.86 | 63 ± 9.72 |
Table 1: Physical characteristics of mothers taking and not taking Iron-folic acid during pregnancy (N=290).
| Variables | No and % | Normal Birth weight (No and %) | Low Birth weight (LBW) <2,500 g (No and %) | P Value |
|---|---|---|---|---|
| Women taking Iron-Folic acid during pregnancy | 276 (69.87%) | 221 (80.07%) | 55 (19.93%) | P<0.05 |
| Women without taking folic acid during pregnancy | 119 (30.13%) | 45 (37.81%) | 74 (62.19%) | P<0.05 |
| Total | 395 (100%) | 266 (67.34%) | 129 (32.66%) | P<0.05 |
Table 2: Distribution of child birth weight among the study population (N=290).
Discussions
Numerous researches which support that iron-folic acid deficiency directly affect maternal health and child birth weight. The merits of iron-folic acid were recently stated in the Cochrane study [16]. Many researches were conducted to demonstrate the importance of maternal diet and iron-folic acid supplements in enhancing infant birth weight. Not only folic acid with iron but also daily intake of milk products and fruits by the mothers were significantly responsible with increase in the birth weight of their child compared with the birth weight of children whose mothers never or only occasionally consumed these products [17]. In our study also it showed that normal birth weight was seen in high percentage (80.07%) among the women who took iron-folic acid during pregnancy unlike the women who did not take iron-folic acid during pregnancy. Among the latter groups, only 37.81% were the child with normal birth weight.
Conclusion
This study showed a significant association between child birth weight and the consumption of iron-folic acid with other appropriate food items by the pregnant women. It seems that there is need for a huge social awareness campaign to improve the nutritional status of pregnant women in the country level. Educating the women during and before pregnancy with her family members to modify their nutritional habits would definitely help to improve mother’s and child’s health.
Acknowledgements
I express my deep sense of gratitude to my participants without their cooperation this study might not have been successful.
References
- Czeizel AE, Dudas I (1992) Prevention of the first occurrence of neural-tube defects by periconceptional vitamin supplementation. N Engl J Med 327: 1832-1835.
- Djukic A (2007) Folate-responsive neurologic diseases. J Pediatr Neurol 37: 387-397.
- Rondo PH, Tomkins AM (200) Folate and intrauterine growth retardation. Ann Trop Paediatr 20: 253-258.
- Antony AC (2007) In utero physiology: role of folic acid in nutrient delivery and fetal development. Am J Clin Nutr 85: 598S-603S.
- Haider BA, Olofin I, Wang M (2013) Anaemia, prenatal iron use, and risk of adverse pregnancy outcomes: systematic review and meta-analysis. British Medical Journal 346: f3443.
- Schaefer, Christof (2001) Drugs During Pregnancy and Lactation: Handbook of Prescription Drugs and Comparative Risk Assessment. 1st ed, Gulf Professional Publishing, Amsterdam, New York, USA.
- Institute of Medicine (2004) Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate. National Academies Press, Washington DC, USA.
- Fekete K, Berti C, Trovato M, Lohner S, Dullemeijer C, et al. (2012) Effect of folate intake on health outcomes in pregnancy: a systematic review and meta-analysis on birth weight, placental weight and length of gestation. Nutr J 11: 75.
- Bergen NE, Jaddoe VW, Timmermans S, Hofman A, Lindemans J, et al. (2012) Homocysteine and folate concentrations in early pregnancy and the risk of adverse pregnancy outcomes: the Generation R Study. BJOG 119: 739-751.
- Wang W, Yan H, Zeng L, Cheng Y, Wang D (2012) No effect of maternal micronutrient supplementation on early childhood growth in rural western China: 30 month follow-up evaluation of a double blind, cluster randomized controlled trial. Eur J Clin Nutr 66: 261-268.
- Stewart CP, Christian P, LeClerq SC, West KP, Khatry SK (2009) Antenatal supplementation with folic acid + iron + zinc improves linear growth and reduces peripheral adiposity in school-age children in rural Nepal. Am J Clin Nutr 90: 132-140.
- Grantham-McGregor S, Cheung YB, Cueto S, Glewwe P, Richter L, et al. (2007) Developmental potential in the first 5 years for children in developing countries. Lancet 369: 60-70.
- Nepal-Demographic and Health Survey (2011) Ministry of Health and Population (MOHP) Calverton, MA, USA.
- Black RE, Victora CG, Walker SP, Bhutta ZA, Christian P, et al. (2013) Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 38: 427-451.
- Birth Weight Classification (2011) WHO Statistical Information Systems (WHOSIS).
- Pena-Rosas JP, Viteri FE (2006) Effects of routine oral iron supplementation with or without folic acid for women during pregnancy. Cochrane Database Syst Rev 3: CD004736.
- Rao S, Kanade AN, Yajnik CS, Fall CH (2009) Seasonality in maternal intake and activity influence offspring’s birth size among rural Indian mothers-Pune Maternal Nutrition Study. Int J Epidemiol 38: 1094-1103.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi