Research Article, J Trauma Stress Disor Treat Vol: 6 Issue: 2
Psychological Trauma, Substance Use and Mood Disorders and Level of Distress among Impaired Professionals: A Mediating Model of Comorbidity
Michael W. Brand1*, Ji Li2, Noeen Sarfraz1,2 and Julio Rojas1
1Department of Psychiatry and Behavioral Sciences, University of Oklahoma Health Sciences Center, USA
2Department of Biostatistics and Epidemiology, University of Oklahoma Health Sciences Center, USA
*Corresponding Author : Michael W. Brand, Ph.D.
Department of Psychiatry and Behavioral Sciences, College of Medicine, University of Oklahoma Health Sciences Center, 1100 N Lindsay Ave, Oklahoma City, OK, 73104, USA
Tel: 405-271-5700
E-mail: michael-brand@ouhsc.edu
Received: June 15, 2017 Accepted: June 22, 2017 Published: June 29, 2017
Citation: Brand MW, Li J, Sarfraz N, Rojas J (2017) Psychological Trauma, Substance Use and Mood Disorders and Level of Distress among Impaired Professionals: A Mediating Model of Comorbidity. J Trauma Stress Disor Treat 6:2. doi: 10.4172/2324-8947.1000171
Abstract
The prevalence of co-occurring psychiatric and substance use disorders is well established, yet, inadequately understood. Individuals with co-occurring psychiatric and substance use disorders display complex clinical presentations have poor prognosis, and institutional barriers hinder them from receiving treatment. To clarify our understanding of this common, yet complex, clinical presentation, we test the hypothesis that substance use disorder symptoms, mood disorders, and psychological trauma symptoms directly contribute to patient distress.
Material and methods
Between January 2006 and June 2010, participants were evaluated and treated in an outpatient setting on a health sciences center campus in Oklahoma City by the Department of Psychiatry and Behavioral Sciences. All participants were impaired professionals. Two groups of professionals participated: 1) health care providers (N=96) and 2) non-healthcare providers (N=44). We applied Structural Equation Modeling (SEM) techniques to the analysis.
Results
Mood disorder, substance use disorder, and trauma symptoms were all positively related to the level of distress. Symptoms of mood disorders had a total direct effect of 0.51 (p<0.0001) on level of distress. Trauma symptoms had a total effect of 0.46 (p<0.0001) on level of distress. This total effect includes 0.18 (p=0.05) direct effect on level of distress and 0.28 (p<0.0001) indirect effect through mood disorder symptoms leading to level of distress. Thus, mood disorder symptoms mediated the relationship between trauma symptoms and level of distress symptoms. The strongest positive direct paths were from symptoms of trauma to mood disorders, with a coefficient of 0.55, and from symptoms of mood disorders to level of distress, with a coefficient of 0.51.
Discussion
This approach challenges the existing treatment models, which targets diagnostic categories with prescribed treatment programsand regimens that may require abstinence before addressing trauma and mood symptoms. The effect of comorbid symptoms on patients’ levels of distress is more complicated than existing models of co-occurring typologies or treatment approaches would indicate. The results have clinical implications and contribute to advancing the fields’ current understanding of the relationship between co-occurring substance use disorders, mood disorders, posttraumatic stress disorder, and patients’ levels of distress, thereby improving treatment outcomes.
Keywords: Trauma; Substance use disorder; Structural Equation Modeling (SEM); Mediation; Impaired professionals; Comorbidity
Introduction
The prevalence of co-occurring psychiatric and substance use disorders is well established [1,2]. Although it is well-established, this relationship is not fully appreciated [3-5]. Thus, the treatment of this combination of disorders continues to be a vexing clinical problem encountered by most mental health and substance abuse treatment providers [3,6-10]. Individuals with co-occurring psychiatric and substance use disorders display more complex clinical presentations [5,9]. They have greater psychosocial problems, and, subsequently, poor prognosis [11-13]. Institutional barriers hinder patients with cooccurring disorders from receiving the treatment they need [9].
Recent studies indicated that individuals presenting with cooccurring psychiatric and substance use disorders share a common cluster of symptoms [14,15]. Clinicians then struggle with the dilemma of choosing which disorder to treat first. An early approach to solving this dilemma involved attempting to classify types of cooccurring disorders into two main typologies. The first classification describes four variations of co-occurring disorders: 1) secondary psychopathology, 2) secondary substance abuse, 3) common factor, and 4) bidirectional [8]. The second typology identifies three types of co-occurring disorders; 1) type one, primary mental health problems with substances used to medicate the mental health problems, 2) type two, primary substance use disorder with substance-induced mental health problems, and 3) type three, co-existing mental health and substance use disorders.
More recently, researchers have investigated the structure/ clustering of symptoms and disorders across patients [16-18]. Other groups have examined shared variance across symptoms and disorders that are taken into account in an outcome or criterion variable [14]. Providers often encounter the presence of co-occurring posttraumatic stress disorder, substance use, and mood disorders [11,19-21].
To help clarify our understanding of this common, yet complex, clinical presentation, our objective is to conduct a secondary data analysis of information from patients with co-occurring substance use and mood disorders with trauma symptoms. We used measures taken from standardized, psychometric, diagnostic testing, and applied Structural Equation Modeling (SEM) techniques to the analysis. We extended our previous research regarding the comorbidity of substance use, mood, and trauma disorder symptoms expressed by impaired professionals and their corresponding levels of distress by developing and testing a diagram of symptom effects. We anticipate that the results will help researchers and clinicians refine their thinking regarding the categories used to describe patients with co-occurring disorders. We also hope that the results will have clinical implications and contribute to advancing the fields’ current understanding of the relationship between co-occurring substance use disorders, mood disorders, posttraumatic stress disorder, and patients’ levels of distress, thereby improving treatment outcomes.
In his 1950’s book entitled Method in the Physical Sciences, von Neumann explains the use of models:
The sciences do not try to explain, they hardly even try to interpret, and they mainly make models. By a model is meant a mathematical construct which, with the addition of certain verbal interpretations, describes observed phenomena. The justification of such a mathematical construct is solely and precisely that it is expected to work-that is, correctly to describe phenomena from a reasonably wide area [22].
Structural equation modeling (SEM) is a theory-driven analytical tool that allows researchers to evaluate a priori hypothesized causal relationships between measured, observable variables and latent, conceptual variables [23]. SEM programs analyze hypothesized covariance structures, specifying the relationship between variables and the variables’ fit with the data’s original covariance matrix [24]. This approach is based on multiple linear regressions, which constructs a model consisting of an outcome variable and multiple predictor variables, resulting in a unique path diagram that predicts the criterion variable [23]. In addition, SEM is a Confirmatory Factor Analysis (CFA) tool that estimates the quality of measurement [25]. The SEM approach can be used in several ways; in the present study, SEM was used to generate a model that statistically fits the data well and is theoretically justifiable [26]. Specifically, this analysis sought to determine whether substance use disorder symptoms, mood disorder symptoms, and symptoms of psychological trauma directly predicted participants’ current levels of distress, or if mood disorder symptoms and/ or symptoms of psychological trauma mediated the effects of substance use disorder symptoms on participants’ current levels of distress.
Material and Methods
Participants
Participants were evaluated and treated in an outpatient setting on a health sciences center campus by the Department of Psychiatry and Behavioral Sciences in Oklahoma City. Participants were referred for evaluation by family friends and family members, employers, professional advocacy groups, or licensure boards in the state of Oklahoma (additional details) [27]. All participants were professionals confronted with difficulty at the workplace, such that it impaired their day-to-day work performance. They were evaluated between January 2006 and June 2010. Two groups of professionals participated: 1) health care providers and 2) non-healthcare providers. The healthcare provider participants (N=96) included medical doctors, nurses, dentists, and optometrists. The non-healthcare participant group (N=44) included business executives, lawyers, professors, and other professionals with advanced degrees and professional certifications (i.e., Certified Public Accountants). The prevalence of co-occurring disorders among impaired professionals is reported to be similar to that found in the general population [27,28]. The study was approved by the University of Oklahoma Health Sciences Center Institutional Review Board.
Procedures
All participants completed a clinical interview, a standard clinic questionnaire designed to capture biopsychosocial information, and the Personality Assessment Inventory (PAI). For the present study, the PAI data were used to test the hypothesis that substance use disorder symptoms, depression and anxiety, and psychological trauma symptoms significantly contribute to patient distress. The PAI is a self-administered objective test of personality and psychopathology designed to provide information on an individual’s level of functioning in a variety of domains. This measure is comprised of 344 items written at a fourth grade reading-level and is intended for use by those aged 18 and older. It takes 40 to 50 minutes to complete. The PAI was developed for use with clinical populations and was validated with a census-matched, normal population, a college student sample, and a clinical sample. Participants completed the computer-administered version of the PAI after receiving brief instructions [29].
Measurement
To test the hypothesis that substance use disorder symptoms, depression and anxiety, and psychological trauma symptoms directly contribute to patient distress, an SEM model was created. The model consisted of two latent factors: Addiction and Psychiatric Illness. Addiction was composed of two PAI scales derived from the PAI scales for Alcohol Problems and Drug Problems. The PAI Alcohol Problems scale (12 items) pertains to behaviors and effects of alcohol use, abuse, dependence, consequences of drinking, loss of control, and alcohol-related craving. The PAI Drug Problems scale (12 items) pertains to behaviors and effects of drug abuse, craving, loss of control, and consequences of drug use.
Psychiatric Illness is composed of two PAI scales. The PAI Depression scale (24 items) measures common cognitive, affective, and physiological symptoms of depression, while the Anxiety scale (24 items) assesses common clinical cognitive, affective, and physiological domains of anxiety.
Trauma was measured using the PAI Traumatic Stress subscale (4 items). This subscale identifies whether an individual has experienced a disturbing traumatic event that continues to cause clinical distress for that individual. The PAI traumatic Stress subscale is not specific to the type of traumatic event (i.e., sexual assault, natural disaster, motor vehicle accident, or combat).
The criterion or outcome variable was the score on the PAI Global Distress scale (12 items). The Global Distress scale captures an individual’s recent and current stressors, which may include family problems, finances, work-related difficulties, or other major life changes.
Statistical Analysis
Structural equation modeling (SEM) with latent variables was used to analyze the association among symptoms of mood disorders, substance use disorders, trauma, and level of distress. Different SEM models were generated, and the models’ fit were compared. The direct and indirect effect with the path coefficient was also tested on the final model. The analysis was conducted in SAS 9.4, with an alpha significance level of 0.05 [30].
Results
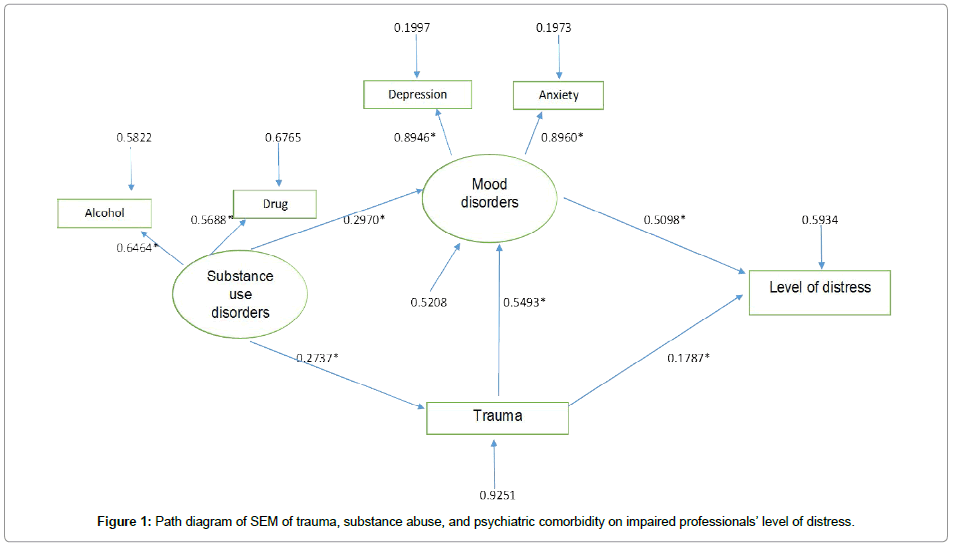
Across the different SEM path analysis, we observed no significant direct effect from substance use disorder on distress level. After adjusting the model for mediating effects, we constructed a final SEM model. Figure 1 displays the path diagram with the standardized regression coefficients for the effect of the paths in the final model. A significant path effect was indicated by an asterisk. This model fits the data well (GFI =0.98; 2=7.03; df=6, p-value=0.32; RMSEA=0.04; Bentler Comparative Fit Index=0.10).
Mood disorder, substance use disorder, and trauma symptoms were all positively related to the level of distress. Symptoms of mood disorders had a total direct effect of 0.51 (p<0.0001) on level of distress. This coefficient indicates that there was an increase of 0.51 standard deviation in the level of distress; T-score for each increase of 1 standard deviation in mood disorder symptoms. Trauma symptoms had a total effect of 0.46 (p<0.0001) on level of distress. This total effect includes 0.18 (p=0.05) direct effect on level of distress and 0.28 (p<0.0001) indirect effect through mood disorder symptoms leading to level of distress. Thus, mood disorder symptoms mediated the relationship between trauma symptoms and level of distress symptoms. Substance use disorder symptoms had no significant direct effect on level of distress. However, symptoms of substance use disorders had a significant total indirect effect of 0.28 (p=0.0002) on level of distress. Thus, mood disorder and trauma symptoms mediated the relationship between substance use disorder and level of distress symptoms.
The strongest positive direct paths were from symptoms of trauma to mood disorders, with a coefficient of 0.55, and from symptoms of mood disorders to level of distress, with a coefficient of 0.51. Table 1 shows the R2 values for the endogenous variables. Symptoms of mood disorders, trauma, and substance use disorders accounted for about 41% of the variance in level of distress. Substance use disorder and trauma symptoms accounted for about 48% of the variance in mood disorder symptoms. Substance use disorder symptoms accounted for about 7.5% of the variance in trauma symptoms.
| Variable | R-Square |
|---|---|
| Level of Distress Symptoms | 0.41 |
| Alcohol Disorder Symptoms | 0.42 |
| Drug Use Disorder Symptoms | 0.32 |
| Depression Symptoms | 0.80 |
| Anxiety Symptoms | 0.80 |
| Trauma Symptoms | 0.07 |
| Mood Disorder Symptoms | 0.48 |
Table 1: Results of SEM of trauma, substance abuse, and psychiatric comorbidity on impaired professionals’ level of distress.
Discussion
The present study presents a mathematically justified representation of the interaction of substance use, mood, and trauma disorder symptoms, which provides an empirically derived model describing the phenomena of comorbidity among a group of impaired professionals undergoing integrated substance use disorder and psychiatric outpatient treatment. We observed that the symptoms of substance use disorders make a significant, yet indirect, contribution to patients’ perceived levels of distress. Mood disorder and trauma symptoms had a direct effect on patients’ levels of distress. Thus, the model empirically supports the mediating effect of mood and trauma disorder symptoms on substance use disorder symptoms and patients’ levels of distress.
The model demonstrates that an increase in mood disorder and trauma symptoms is predicted by an increase in substance use disorder symptoms. However, it is the mood disorder symptoms primarily predict the patients’ levels of distress. The model describes a “confluence of symptoms” that predict level of distress. The word confluence is used to describe the merging of two or more bodies of water [31]. The model captures the complicated phenomenon of “symptom confluence”, depicting the avenues through which substance use, mood, and trauma symptoms merge to influence these patients’ levels of distress.
The prevailing typologies of co-occurring disorders appear to be too simplistic to adequately account for the relationships that the proposed model empirically represents [32]. The clinical presentation depicted by our SEM model suggests more than simply a mental health problem that is medicated through the use of substances, a mental health problem that is induced by substance use. While the current body of research establishes the correlation between substance use, mood disorders, and trauma, the present study proposes the avenues through which the symptoms of these disorders influence these patients’ levels of distress, revealing a much richer and more complicated picture than the existing typologies would indicate. By their very nature, the existing typologies lead researchers and clinicians to approach the problem of comorbidity as a “chicken or the egg” problem; which to treat first? Our proposed model suggests that the important question is how the symptoms of these various disorders come together to affect patients’ levels of distress and create life problems.
From a clinical perspective, the model challenges the common assumption that one must be free of all substance use before they can address their psychological trauma. Rather, helping the patient understand how the various symptoms contribute to their current level of distress and life problems may be a more beneficial approach than deciding which disorder to treat first. Here we propose “symptom mapping”, that is, allocating or mapping symptoms of the patient’s co-occurring disorders to their level of distress and life problems. As the proposed model indicates, substance use, mood disorders, and trauma uniquely and differentially impact patients’ levels of distress. Mapping specific symptoms to identified problems, such as family difficulties, finances, work-related problems, or other major life changes, allows clinicians and patients to identify how the symptoms of these disorders create their distress and then target interventions to either decrease symptoms or alleviate problems. This approach challenges the existing treatment model, which tends to target diagnostic categories with prescribed treatment programs and regimens. As the proposed model indicates, the effect of comorbid symptoms on patients’ levels of distress is more complicated than existing models of co-occurring typologies or treatment approaches would indicate.
While a number of researchers in the field of modeling research have reached similar conclusions, additional work is needed to replicate these findings with larger samples [14,15,18]. This type of modeling research and confirmatory factor analysis should be replicated with the general population using different types of indicators forming the same latent variables: substance use, mood disorders, and trauma. Finally, symptom-specific research that identifies how specific symptoms of the various co-occurring disorders contribute to patients’ problems and levels of distress is warranted.
References
- Kessler RC, Nelson CB, McGonagle KA, Edlud, MJ, Frank RG, et.al. (1996) The epidemiology of co-occurring addictive and mental disorders: Implications for prevention and service utilization. Am J Orthopsychiatry 66: 17-31.
- Warner LA, Kessler RC, Hughes M, Anthony JD, Nelson CB (1995) Prevalence and correlates of drug use and dependence in the United States. Arch Gen Psychiatry 52: 219-229.
- Andreas JB, Lauritzen G, Nordfjærn T (2015) Co-occurrence between mental distress and poly-drug use: A ten year prospective study of patients from substance abuse treatment. Addict Behav 48: 71-78.
- Delgadillo J, Kay-Lambkin F (2016) Closing the science-practice gap: Introduction to the special issue on psychological interventions for comorbid addictions and mental health problems. Advances in Dual Diagnosis 9: 1-5.
- Substance Abuse and Mental Health Services Administration (2015).
- Bergly TH, Grawe RW, Hagen R (2014) Domains and perceived benefits of treatment among patients with and without co-occurring disorders in inpatient substance use treatment. J Dual Diagn 10: 91-97.
- Minkoff K (1989) An integrated treatment model for dual diagnosis of psychosis and diction. Hosp Community. Psychiatry 40: 1031-1036.
- Mueser KT, Drake, RE, Turner W, McGovern M (2006) Comorbid substance use disorders and psychiatric disorders. (Eds.), Rethinking substance abuse: What the science shows, and what we should do about it (pp. 115-133). New York, NY: Guilford Press.
- Priester MA, Browne T, Iachini A, Clone S, DeHart D, et al. (2016) Treatment access barriers and disparities among individuals with co-occurring mental health and substance use disorders: an integrative literature review. J Subst Abuse Treat 61: 47-59.
- Swendsen J, Conway KP, Degenhardt L, Glantz M, Jin R, et al. (2010) Mental disorders as risk factors for substance use, abuse and dependence: results from the 10-year follow-up of the national comorbidity survey. Addiction 105: 1117-1128.
- Grant BF, Saha TD, Ruan WJ, Goldstein RB, Chou SP, et al. (2016) Epidemiology of DSM-5 drug use disorder results from the national epidemiologic survey on alcohol and related conditions–III. JAMA Psychiatry 73: 39-47.
- Mauroa PM, Furr-Holdena CD, Strainc EC, Crumd RM, Mojtabaia R (2016) Classifying substance use disorder treatment facilities with co-located mental health services: A latent class analysis approach. Drug Alcohol Depend 163: 108-115.
- Watkins KE, Susan M, Paddock SM, Hudson TJ, Ounpraseuth S, et al. (2016) Association between quality measures and mortality in individuals with co-occurring mental health and substance use disorders. J Subst Abuse Treat 69: 1-8.
- Rojas JR, Brand M, Li J (2013) Empirical examination of a Venn diagram heuristic for understanding the relationship between addiction, psychiatric comorbidity and trauma. Mental Health and Substance Use 7: 84-91.
- Urbanoski K, Kenaszchuk C, Veldhuizen S, Rush B (2015) The clustering of psychopathology among adults seeking treatment for alcohol and drug addiction. J Subst Abuse Treat 49: 21-26.
- Wang J, Kelly BC, Liu T, Hao W (2016) Studying psychosocial barriers to drug treatment among Chinese methamphetamine users using a 3-step latent class analysis. J Subst Abuse Treat 62: 89-95.
- Bergman A, Owens M, Kelter JD, Kong G (2016) Comorbidity in disconnected emerging adults with ADHD. Gavin Journal of Addiction Research and Therapy 2016: 17-25.
- Huynh C, Tremblay J, Fleury M (2016) Typologies of Individuals Attending an Addiction Rehabilitation Center Based on Diagnosis of Mental Disorders. Journal of Substance Abuse Treatment 71: 68-78.
- Cox DW, Buhr EE, Owen JJ, Davidson E (2015) Linking partner emotional support,partner negative interaction, and trauma with psychological distress: Direct and moderating effects. Journal of Social and Personal Relationships 33: 1-17.
- McGovern MP, Lambert-Harris C, Acquilano S, Xie H, Alterman AI, et al. (2009) A cognitive behavioral therapy for co-occurring substance use and posttraumatic stress disorders. Addict Behav 34: 892- 897.
- McGovern MP, Lambert-Harris C, Acquilano S, Xie H, Alterman AI, et al. (2011) A randomized controlled trial comparing integrated cognitive behavioral therapy versus individual addiction counseling for co-occurring substance use and posttraumatic stress disorders. J Dual Diagn 7: 207-227.
- Von Neumann J (1955) Method in the physical sciences. (Edtn.) The Neumann compendium: world series in 20th century mathematics; vol. 1 World Scientific Publishing Co, Singapore.
- Kline RB (2011) Principles of Practice of Structural Equation Modeling (2nd edtn) Guilford Press, New York, USA.
- Hoyle RH (2012) Handbook of Structural Equation Modeling. Guilford Press, New York, USA.
- Brown TA (2015) Confirmatory Factor Analysis for Applied Research. (2nd edtn), Guilford Press, New York, USA.
- Kline RB (2016) Principles of Practice of Structural Equation Modeling. (4th edtn), Guilford Press, New York, USA.
- Rojas JR, Brand M, Fareed S, Koos E (2012) Psychiatric comorbidity in healthcare professionals with substance use disorders. Addictive Disorders and their Treatment 12: 51-57.
- Angres DH, McGovern MP, Shaw MF, Rawal P (2003) Psychiatric comorbidity and physicians with substance use disorders: Between the 1980s-1990s. Journal of Addictive Diseases 22: 79-87.
- Morey LC (1991) Personality Assessment Inventory Professional Manual. Odessa, FL: Psychological Assessment Resources.
- SAS [computer program], release 9.4. Cary, NC: SAS Institute Inc; 2002-2012.
- Confluence (2017) In OxfordDictionaries.com.
- Haller M, Norman SB, Cummins K, Trim RS, Xu X, et al. (2016) Integrative cognitive behavioral therapy versus cognitive processing therapy for adults with depression, substance use disorder and trauma. J Subst Abuse Treat 63: 38-48.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi