Review Article, J Physiother Rehabil Vol: 3 Issue: 1
Rehabilitation Challenges in Neuropathic Pain among Patients with Multiple Sclerosis: A Narrative Review
Mst Rabea Begum1* and Firoz Ahmed Mamin2
1Physiotherapy Department, Centre for the Rehabilitation of the Paralysed (CRP), Savar, Dhaka, Bangladesh
2Bangladesh Health Professions Institute (BHPI), CRP, Savar, Dhaka-1343, Bangladesh
*Corresponding Author : Mst Rabea Begum
Senior Clinical Physiotherapist, Physiotherapy Department, Centre for the Rehabilitation of the Paralysed (CRP), Savar, Dhaka-1343, Bangladesh
Tel: +8801675793257
E-mail: physio_miilee@yahoo.com, drrabea3@gmail.com
Received: March 22, 2019 Accepted: April 12, 2019 Published: April 22, 2019
Citation: Begum MR, Mamin FA (2019) Rehabilitation Challenges in Neuropathic Pain among Patients with Multiple Sclerosis: A Narrative Review. J Physiother Rehabil 3:1. doi: 10.4172/jptr.1000117
Abstract
Aim: The aim of the study was to find out the rehabilitation challenges in neuropathic pain among patients with multiple sclerosis.
Methodology: A narrative review was done for this study. The electronic database including PubMed and Google Scholar are used to find out the related study. International Classification of Functioning, Disability and Health (ICF) were used to find out the problems in patients with multiple sclerosis.
Findings: Studies found that drugs can affect adversely in depression, nausea, dizziness, constipation and lethargy. Physical activity improved functional capacity.
Conclusion: Neuropathic pain is a burden for patients with multiple sclerosis. This pain can negatively impact on individual’s life. The treatment of multiple sclerosis is a great challenging. It is very challenging to manage the symptoms of multiple sclerosis but to rehabilitate physiotherapy is very effective on managing the symptoms.
Keywords: Rehabilitation; Neuropathic pain; Multiple sclerosis
Introduction
Neuropathic pain is a common phenomenon in neurological disorder due to result from the dysfunction of central or peripheral nervous system [1]. In brain anatomy there are changes correlated with chronic pain due to changes in gray matter. In a study it is reported that the pathology of neuropathic and non-neuropathic is not similar. Due to changes of peripheral nerve injury and structural changes of thalamus neuropathic pain is occurred [2].
According to the International Association for the Study of Pain (IASP) report “neuropathic pain as pain initiated or caused by a primary lesion or dysfunction in the nervous system.” The international classification of diseases (ICD) is the usual diagnostic tools for clinical purpose as well as for epidemiology. According to ICD 11 chronic pain consists of chronic primary pain, chronic cancer pain, chronic postsurgical and posttraumatic pain, chronic neuropathic pain, chronic headache and orofacial pain, chronic visceral pain and chronic musculoskeletal pain [3].
In a study it is reported that most of chronic pains is reported in neuropathic type than non-neuropathic. This study was done in a general population. In this study most of the respondents were in middle aged group (50 to 64 years). In 7,522 respondents the prevalence was 31.7%. Women were more prevalent than men and occurred more at rural area than urban for developing chronic pain [4].
The common cause of neuropathic pain consists of diabetic polyneuropathy, spinal cord injury, stroke, multiple sclerosis, cancer and HIV infection. Health professionals are facing challenges to treat this chronic pain. Neuropathic pain may be classified as peripheral and central neuropathic pain [5].
To realize the definite neuropathic pain the professionals should correlate history, examination and then confirmatory test to reach a definite diagnosis which is shown in following flow chart [6].
In Multiple sclerosis occurring neuropathic pain is common characteristics. It is a chronic neurological disease that distinguished by inflammation, scarring and demyelination with most common in 20 to 40 years age. And 2.1 million people are affecting worldwide in this age group. The prevalence is 30 per 100,000 population and female are more prevalent than male [7].
In patients with multiple sclerosis neuropathic pain is frequent complaint with continued their life up to four decades. The pain in multiple sclerosis is associated with central neuropathic pain. In a systematic review the authors reported the central neuropathic pain and proposed a classification of pain in patients with multiple sclerosis (Table 1) [8].
| Pain condition | Examples |
|---|---|
| Continuous central neuropathic pain | Dysesthetic extremity pain |
| Intermittent central neuropathic pain | Lhermitte’s sign, trigeminal neuralgia |
| Musculoskeletal pain | Painful tonic spasms, low back pain, muscle spasms |
| Mixed neuropathic and non-neuropathic pain |
Headache |
Table 1: Classification of pain in patients with multiple sclerosis.
N.B: Dysesthetic extremity pain is unpleasant abnormal sensation of touch like burning, itching, pins and needles. It is found in mouth, scalp, skin, or legs.
Lhermitte’s sign is electric shock-like sensation felt in the back of the neck, lower back and occasionally in limbs. The Lhermitte’s phenomenon occurs with neck flexion and resolves with cessation of neck flexion.
Trigeminal neuralgia is a severe, sharp, electric shock like pain in one of the three divisions of the trigeminal nerve (the eye, cheek and jaw). The pain area of the eye is less frequent than cheek or the jaw.
Painful tonic spasm is sudden tightening of a limb, clawing of a hand or arm and kicking of a leg. This spasm is last less than 2 minutes.
For developing multiple sclerosis headache is common. In men and women migraine is 3 times more common that is created depression and sensory relating pain syndrome. It is associated with relapsingremitting type [9]. A central neuropathic pain is a chronic form of pain that resulted from the lesion of central nervous system. This pain is like burning, shooting, squeezing and altered sensation in temperature especially in cold. And also, parasthesia and allodynia is common. Due to central sensitization there is development of central pain and also sensitized spinothalamic pathway [10].
In a study it is reported that 27.5% of patient reported with central neuropathic pain in patient with multiple sclerosis. In 100 patients, 62 had bilateral lower extremity pain and 13 had unilateral pain. All patients had abnormal sensory alteration like complaint of decrease cold sensation. So in this study it is investigated that in patient with multiple sclerosis central neuropathic pain occurs resulted from the lesion of spinothalamic pathway [11].
Another study by Svendsen et al., (2005) reported that 58% participants suffered central neuropathic pain and the area of pain were lower extremities (96%), back (70%), and upper extremities (52%) with spinothalamic dysfunction.
The multiple sclerosis patients are rehabilitating in multidisciplinary approaches. Asian countries like Bangladesh, India, Pakistan and Sri Lanka are facing more or less same problem that is a huge population but having inadequate number of skilled and trained neurorehabilitation specialists [12].
Methodology
The electronic database including PubMed and Google Scholar are used to find out the related study. The inclusion criteria were study between the years 2000 to May 2017 and only chronic neuropathic pain in patients with multiple sclerosis.
Multiple sclerosis is a chronic condition and relapse-remitting is a more common than other type. The patients of multiple sclerosis suffered most common pain consists of headache, continuous burning pain in extremities, back pain, painful tonic spasm (cramping). The feeling of this neuropathic pain like consists of burning, tingling, aching and throbbing. Also worsen at night, increase in exercise and changes in temperature, hyperalgesia and allodynia [13].
To measure the disability there is a scale named Multiple Sclerosis Impact Scale (MSIS-29) that a valid and reliable scale for measuring the physical and psychological status of multiple sclerosis patients [14]. The treatment of painful neuropathy is a most important challenge and recent therapies are not adequate. Therapeutic approaches to reduce the neuropathic pain of multiple sclerosis are mainly in symptomatic.
In this circumstances evidence support the need of multidisciplinary approaches for needing appropriate rehabilitation [15]. The goal of treatment is maintenance of functional abilities, prevent further complication and physical limitation due to this chronic pain. There is low evidence for relief of long-term pain but not for short term pain [16]. The effective therapy helps to improve quality of life, reduction of chronic pain and disability in patients with multiple sclerosis. But physical activity increased the pain and sensory symptoms that create a big challenge for physiotherapist for manage this type of problem. The passive range of motion exercise is needed though there is no evidence to support for doing this but helpful for preventing contracture and deformity [17].
In acute stage physiotherapists focus on patient education for relieving the symptoms and involve caregiver with use of compensatory strategies. At advanced stage the severity is increasing. In this stage goal is to improve respiratory function, prevention strategies for contracture development or pressure sore, equipment prescription and educate to patient with the involvement of care giver for proper transfer techniques [18].
Quality of life
Neuropathic pain is a complex condition that negatively effect on mental, physical and professional quality of life that related with high economical cost [19]. Patients in neuropathic pain reported the low level of quality of life. The strong evidence supported that neuropathic pain associated with impairments that reduce quality of life. This pain is hidden and thus causes long term impact on person’s quality of life [20].
It is investigated that in patients with multiple sclerosis 40% have difficulty in working, 44% facing difficulty in sleeping and 34% have troubled in maintaining relationships [21].
A study by Pappalardo et al., [22] investigated that therapeutic intervention can improve the quality of life for patients with multiple sclerosis. This randomized control trial observes the effectiveness of inpatient and outpatient therapeutic rehabilitation on this population. After analysis it is concluded that outpatient rehabilitation showed statistically significant outcome in improving quality of life.
Bio psychosocial model
The neuropathic pain is a cause of disability. In Bio psychosocial model chronic neuropathic pain is well understood because in this model psychological factors are reported and it is evident that there is a strong relation between the psychological factors and chronic pain. Living with multiple sclerosis this chronic pain causes the chronic stress [23].
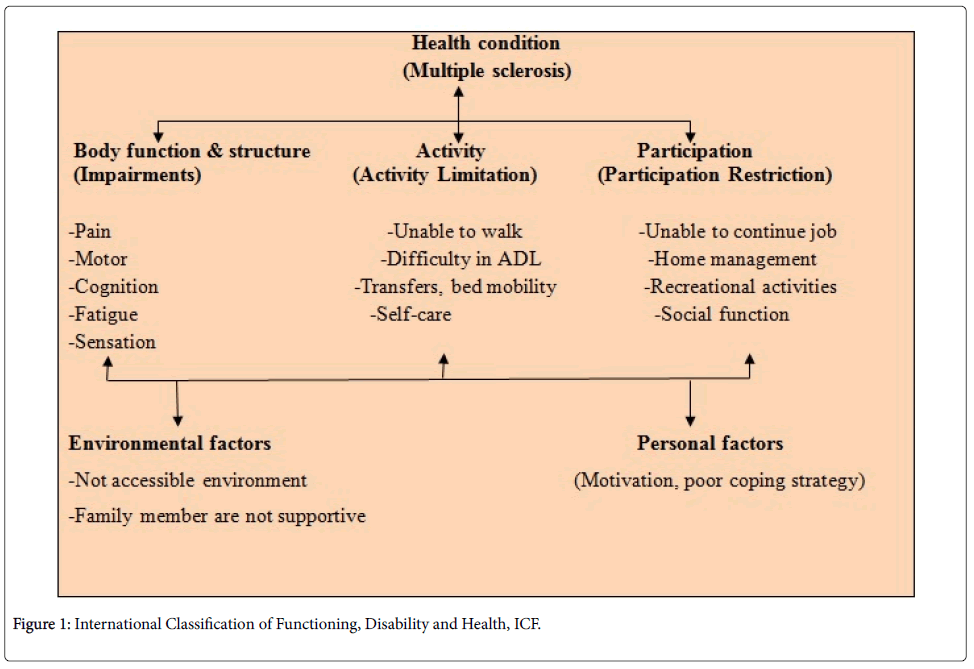
The neuropathic chronic pain contributes on International Classification of Functioning, Disability and Health (ICF). To manage and understanding the pain of multiple sclerosis through ICF it is more comprehensive which consist of increase physical and social activation, self-management of pain, reduce stress, reduce clinical symptoms and improvement of quality of life. The pain in multiple sclerosis is multidimensional phenomenon consist of physical, social and psychological impact on each individual. Mood, depression, anxiety, fatigue, sleep disturbance, poor coping and lack of social support influenced on pain intensity and contribute to disability. Developing coping strategies and how to accept pain may to reduction of pain intensity and impact of pain for multiple sclerosis patients. This pain can directly impact on participation of individuals and thus the physical discomfort causes the social withdrawal (Figure 1) [24].
Depression
In patients with multiple sclerosis depression and chronic pain are more prevalent. Depression and chronic pain has a negative impact on patients with multiple sclerosis on their living. Depression is associated with poor neuropsychological functioning, low quality of life as well as inactive in social activities. In this way, chronic pain in multiple sclerosis also impact on their activities in daily living. There is a correlation between depression and chronic pain. This depression and pain negatively impact on the effectiveness of treatment. For this type of problem multiple sclerosis patients need to take more visits from health professionals. There is no study proven the effectiveness of antidepressant drugs for depression in multiple sclerosis patients [23].
Use of drugs
Multiple sclerosis is a progressive disease. The aim of drug is to reduce the exacerbation and slow the progression of this condition. And rehabilitation aim is to improve and maintain the functional abilities and quality of life. Interdisciplinary team approaches of health care professionals are essential to reduce impairment, activity limitation and improve participation in family and society. Rehabilitation is a significant part from the diseases onset to end of life due to the diseases progression. Also its goal is to prevent the secondary complication of this disease. The rehabilitation of multiple sclerosis is very challenging. The challenge is in muscle contracture, return to employment and to manage chronic neuropathic pain in patients with multiple sclerosis [25].
Anti-depressive drugs are commonly used for managing chronic pain in patients with multiple sclerosis. Duloxetine is a serotonin norepinephrine reuptake inhibitor that has a therapeutic role in treating chronic pain due to multiple sclerosis but all patients are not able to tolerate this drug. A double blinded RCT was done by Brown and Slee [26] on 38 participants. After randomization one group received duloxetine (n=14) and another group (n=19) used placebo treatment. The dose was 30 mg daily for 1 week, then 60 mg daily for 5 weeks. The average age of participants was 55.5 years. The majority participants were in relapsing-remitting MS. After analysis author found that duloxetine reduced pain but not any change in depression or sleep. The experimental group who received duloxetine reduced their pain but showed adverse side effect including nausea, dizziness, fatigue, constipation, and urinary retention. Due to showing these effects some participants discontinued the trails. So from this study it is indicated that for reducing the clinical symptoms like chronic pain with depression, mood and sleep which are more common in multiple sclerosis by drugs it is more challenging.
The drugs that are used in multiple sclerosis carry a potential side effects as well as problems with dose and dependency. A nondrug treatment like physiotherapy is recommended for patients with multiple sclerosis and safe that is tolerable and does not interfere with sleep and daily activities [27].
Cost
The majority of multiple sclerosis patients diagnosed at the time of employment. After diagnosis 50% leave their job due to diseases progression. After diagnosis their cost is £17,000 per person but after leaving job the cost rising to over £25,000. There was significant association between cost, quality of life and disability. The high cost reduces the quality of life and disability in person with multiple sclerosis [28]. Similar result found a systematic review by Naci et al., [29]. In this review authors used cost related 29 studies in patients with multiple sclerosis. They concluded that increased costs associated with relapse occurrence and increasing the severity of diseases.
Neuropathic pain is more intense than non-neuropathic in patients with multiple sclerosis. This pain negatively impact on activities on daily living and quality of life. In this study neuropathic pain was 70.5% and 29.5% non-neuropathic pain. The neuropathic pain is higher in visual analogue scale (VAS) (p<0.05). There are positive relation with female and VAS [30].
Therapeutic challenges
Physiotherapy is a lifelong need due to its diseases progression. In rehabilitation the goal of physiotherapy is to improve the quality of life, prevent the further complication, and improve exercise tolerance and so on. It also depends on severity of diseases. In a systematic review by Rietberg et al., [31] mentioned that physiotherapy is a supportive treatment in case of multiple sclerosis patients. There is a strong evidence of muscle power, exercise tolerance, mobility related activities and prevent secondary complication. Moderate evidence is for changing mood. In this study there was small sample size and have type II error with lack of statistical power. So lastly the authors concluded that the effectiveness of physiotherapy is unclear but the symptoms are not increased by doing the therapy.
The motor and cognitive function improved the quality of life by enhancing structural and functional brain plasticity. This change is found in performance of function and changing in MRI findings [32]. The restoration and maintenance of functional capacities are relating to improve quality of life [33].
In a study Paltamaa et al., [34] reported that there is little evidence to support the progressive exercise and aerobic training had a positive effect on balance in case presence of chronic pain in patients with multiple sclerosis. In this case patients have fatigue depression which can affect the treatment. Already discussed mental health can effect on chronic pain.
Evidence reported that neurorehabilitation can improve symptoms, functional capacities, and social participation with maintain functional capacity. The treatment of multiple sclerosis is a great challenging because pharmacological and non-pharmacological management can influence the course of multiple sclerosis. This management can reduce the symptoms, slow the neurodegeneration but cannot stop the neurodegeneration [35].
There are some challenges faced by physiotherapist during treating in patients with multiple sclerosis. Weakness and fatigue are common caused by nerve conduction dysfunction that is increased by some factors like temperature, medication, disturbed sleep, stress, depression and also sometimes by some therapeutic intervention. Antiepileptic and Anti-depressive drugs are used for managing the symptoms of multiple sclerosis. Medication had a side effect including increasing the spasticity. Multiple sclerosis patient avoid physical activity because more physical activity worsening weakness, increased fatigue and other health problem. On the other hand limited physical loss. The cessations of exercise can recurrence of symptoms. Most of the patients come for rehabilitation when lost their most of function. In this situation this chronic pain slow and incomplete the improvements in patients with multiple sclerosis [36]. Activities worsen the spasticity, produce constipation and as well as contribute to bone.
Pain due to trigeminal neuralgia, painful tonic spasm antiepileptic is the first choice for managing pain. When pain related with spasticity physiotherapy is the first line management. According to expert opinion, NSAID should not be used for long time and also not response with combination of physiotherapy and NSAID. In that situation for management of this pain professionals need to identify the causes of pain otherwise it will be more challenging [37].
Summary
• Multiple sclerosis is a complex chronic progressive disorder.
• Compensatory strategies are used for rehabilitation.
• There are some hidden symptoms like fatigue, diplopia that cannot visible to others.
• The reflective sense of vulnerability, loss of control, frequently fall and poor coping status that related with management of neuropathic pain.
• Drugs can effect adversely in depression, nausea, dizziness, constipation, lethargy.
• Physical activity improved functional capacity but it can increase pain and sensory symptom.
To overcome these challenges for managing this chronic neuropathic pain a multidisciplinary team approaches means combination of psychological, pharmacological and physical therapies are the best approaches for managing chronic neuropathic pain in patients with multiple sclerosis [38]. Also early identification is important to delay this diseases progression and reduce the symptoms. At first the aim of rehabilitation is to educate that he has to accept this pain and cope with pain and then improve quality of life. Need to remember that this is a progressive disease thus treatment should not be so costly which affect the other family members of patients with multiple sclerosis [39].
Conclusion
Neuropathic pain is a burden for patients with multiple sclerosis. The challenges of multiple sclerosis is it affect the most peak age means their career age and childbearing years for women. This pain can negatively impact on individual’s life. For managing the neuropathic pain of multiple sclerosis used drugs due to its diseases progression but this drugs have more adverse effect other hand physiotherapy is safe and secure treatment for this type of patients therefore unable to stop the diseases progression and difficult to prevent the ongoing complication.
References
- International Association for the Study of Pain Taxonomy (2012) Accessed on May 2017, International Association for the Study of Pain Taxonomy.
- Gustin SM, Peck CC, Wilcox SL, Nash PG, Murray GM, et al. (2011) Different pain, different brain: Thalamic anatomy in neuropathic and non-neuropathic chronic pain syndromes. J Neurosci 31: 5956-5964.
- Treede RD, Rief W, Barke A, Aziz Q, Bennett MI, et al. (2015) A classification of chronic pain for ICD-11. Pain 156: 1003-1007.
- Bouhassira D, Lantéri-Minet M, Attal N, Laurent B, Touboul C (2008) Prevalence of chronic pain with neuropathic characteristics in the general population. Pain 136: 380-387.
- Attal N, Cruccu G, Haanpää M, Hansson P, Jensen TS, et al. (2006) EFNS guidelines on pharmacological treatment of neuropathic pain. Eur J Neurol 13: 1153-1169.
- Finnerup NB, Haroutounian S, Kamerman P, Baron R, Bennett DLH, et al. (2016) Neuropathic pain: An updated grading system for research and clinical practice. Pain 157: 1599-1606.
- World Health Organization (WHO) (2008) Atlas: Multiple sclerosis resources in the world. World Health Organization (WHO).
- O’Connor AB, Schwid SR, Herrmann DN, Markman JD, Dworkin RH (2008) Pain associated with multiple sclerosis: Systematic review and proposed classification. Pain 137: 96-111.
- Kister I, Caminero AB, Monteith TS, Soliman A, Bacon TE, et al. (2010) Migraine is comorbid with multiple sclerosis and associated with a more symptomatic MS course. J Headache Pain 11: 417-425.
- International Association for the study of Pain (IASP) (2014) Central neuropathic pain. Accessed on May 10, 2017, International Association for the study of Pain (IASP).
- Osterberg A, Boivie J, Thuomas KA (2005) Central pain in multiple sclerosis: prevalence and clinical characteristics. Eur J Pain 9: 531-542.
- Surya N (2015) Rehabilitation of multiple sclerosis patients in India. Ann Indian Acad Neurol 18: 43-47.
- Maloni H (2007) Multiple sclerosis and pain. Consortium for Multiple Sclerosis.
- Riazi A, Hobart JC, Lamping DL, Fitzpatrick R, Thompson AJ (2002) Multiple Sclerosis Impact Scale (MSIS-29): Reliability and validity in hospital based samples. J Neurol Neurosurg Psychiatry 73: 701-704.
- Kumar A, Pahwa D, Rinwa P (2013) Management of neuropathic pain: Challenges and opportunities. Int J Res Dev Pharm L Sci 3: 734-740.
- Bogduk N (2004) Management of chronic low back pain. Med J Aust 180: 79-83.
- Khan F, Pallant J (2007) Chronic pain in multiple sclerosis: Prevalence, characteristics, and impact on quality of life in an Australian community cohort. J Pain 8: 614-623.
- Provance P (2011) Physical Therapy in Multiple Sclerosis Rehabilitation. Accessed on May 23, 2017, A Clinical Bulletin from the Professional Resource Center of the National Multiple Sclerosis Society, New York.
- Langley PC, Van Litsenburg C, Cappelleri JC, Carroll D (2013) The burden associated with neuropathic pain in Western Europe. J Med Econ 16: 85-95.
- Doth AH, Hansson PT, Jensen MP, Taylor RS (2010) The burden of neuropathic pain: A systematic review and meta-analysis of health utilities. Pain 149: 338-344.
- Warnell P (1991) The pain experience of a multiple sclerosis population: A descriptive study. Axone 13: 26-28.
- Pappalardo A, D’Amico E, Leone C, Messina S, Chisari C, et al. (2016) Inpatient versus outpatient rehabilitation for multiple sclerosis patients: Effects on disability and quality of life. Multiple Scler Demyelinating Disord 1: 3.
- Alschuler KN, Ehde DM, Jensen MP (2013) Co-occurring depression and pain in multiple sclerosis. Phys Med Rehabil Clin N Am 24: 703-715.
- Jensen TS, Baron R, Haanpaa M, Kalso E, Loeser JD, et al. (2011) A new definition of neuropathic pain. Pain 152: 2204-2205.
- Burks JS, Bigley GK, Hill HH (2009) Rehabilitation challenges in multiple sclerosis. Ann Indian Acad Neurol 12: 296-306.
- Brown TR, Slee A (2015) A randomized placebo-controlled trial of duloxetine for central pain in multiple sclerosis. Int J MS Care 17: 83-89.
- Brown TR (2017) Challenges in pain management for MS patients. Real World Health Care.
- McCrone P, Heslin M, Knapp M, Bull P, Thompson A (2008) Multiple sclerosis in the UK: Service use, costs, quality of life and disability. Pharmacoeconomics 26: 847-860.
- Naci H, Fleurence R, Birt J, Duhig A (2010) Economic burden of multiple sclerosis: A systematic review of the literature. Pharmacoeconomics 28: 363-379.
- Grasso MG, Clemenzi A, Tonini A, Pace L, Casillo P, et al. (2008) Pain in multiple sclerosis: A clinical and instrumental approach. Mult Scler 14: 506-513.
- Rietberg MB, Brooks D, Uitdehaag BM, Kwakkel G (2005) Exercise therapy for multiple sclerosis. Cochrane Database of Syst Rev 25: CD003980.
- Prosperini L, Piattella MC, Gianni C, Pantano P (2015) Functional and structural brain plasticity enhanced by motor and cognitive rehabilitation in multiple sclerosis. Neural Plast 2015: 1-12.
- Khan F, Amatya B, Stokes LT (2011) Symptomatic therapy and rehabilitation in primary progressive multiple sclerosis. Neurol Res Int 2011: 1-22.
- Paltamaa J, Sjogren T, Peurala SH, Heinonen A (2012) Effects of physiotherapy interventions on balance in multiple sclerosis: A systematic review and meta-analysis of randomized controlled trials. J Rehabil Med 44: 811-823.
- Geng TC, Mark VW (2015) Clinical neurorestorative progress in multiple sclerosis. J Neurorestoratology 3: 83-90.
- Frohman TC, Castro W, Shah A, Courtney A, Ortstadt J, et al. (2011) Symptomatic therapy in multiple sclerosis. Ther Adv Neurol Disord 4: 83-98.
- Pollmann W, Feneberg W (2008) Current management of pain associated with multiple sclerosis. CNS Drugs 22: 291-324.
- Turk DC, Audette J, Levy RM, Mackey SC, Stanos S (2010) Assessment and treatment of psychosocial comorbidities in patients with neuropathic pain. Mayo Clin Proc 85: S42-S50.
- Scascighini L, Sprott H (2008) Chronic nonmalignant pain: A challenge for patients and clinicians. Nat Clin Pract Rheumatol 4: 74-81.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi