Case Report, J Spine Neurosurg Vol: 6 Issue: 4
Relationship between Cutaneous Silent Period Characteristics and Lesion Site in the Cervical Spinal Cord
Tadokoro N*, Kiyasu K, Kasai Y, Kawasaki M, Takemasa R and Ikeuchi M
Department of Orthopedic Surgery, Kochi Medical School, Kochi University, Japan
*Corresponding Author : Dr. Nobuaki Tadokoro
Department of Orthopaedic Surgery, Kochi Medical School, Kochi University, Kohasu Oko-chou, Nankoku, 783-8505, Japan
Tel: +81-88-880-2386
Fax: +81-88-880-2388
E-mail: tadokoro.nobuaki@kochi-u.ac.jp; nobuaki.tadokoro@gmail.com
Received: July 05, 2017 Accepted: July 11, 2017 Published: July 20, 2017
Citation: Tadokoro N, Kiyasu K, Kasai Y, Kawasaki M, Takemasa R, et al. (2017) Relationship between Cutaneous Silent Period Characteristics and Lesion Site in the Cervical Spinal Cord. J Spine Neurosurg 6:4. doi: 10.4172/2325-9701.1000275
Abstract
Objective: The transient suppression of voluntary muscle contraction after nociceptive stimulation is termed the cutaneous silent period (CSP), and is thought to be a spinal inhibitory reflex mediated by A-delta fibers. In CSP testing using the abductor pollicis brevis (APB) muscle (C8-T1 myotome) and the index finger (C6-C7 dermatome), the intramedullary CSP circuit is thought to be localized to the C6-T1 spinal segments. Notably, CSPs are altered or abolished in cervical cord disorders. However, the association between the site of cord lesion and CSP changes is not clearly defined.
Methods: We prospectively reviewed the onset latency and duration of preoperative CSPs in 40 hands from 22 patients with cervical compression myelopathy (CCM) and single-level cord compression. CCM patients were divided into 2 groups: those with compression involving the C6-T1 spinal segments (CCM at the middle and lower cervical spine, the ML group; 10 hands) or other segments (CCM at the upper cervical spine; the U group, 30 hands).
Results: Onset latency was significantly delayed in the ML group compared to the U group (P = 0.0001), whereas duration was not significantly different between groups (P = 0.9).
Conclusion: Changes in the CSP onset latency were influenced by the CCM lesion site. The results of this study inform the evaluation of patients with cervical cord disorders when using CSP testing.
Keywords: Cervical compression myelopathy; Cutaneous silent period; Innervation; Pollicis brevis; Spinal inhibitory reflex; Spinal segment
Introduction
The cutaneous silent period (CSP) is a transient suppression of voluntary muscle contraction following nociceptive stimulation [1]. The afferent impulses that generate the CSP are mediated by the smaller, slower conducting A-delta fibers [2,3]. A-delta fibers enter the spinal cord via the lateral division of the dorsal root and divide into several branches in the tract of Lissauer. These branches terminate in the dorsal horn in laminae I and V of Rexed and connect to propriospinal projections that suppress motor nucleus activity. Clinically, CSP testing is useful for the detection of cervical cord disorders (e.g. intramedullary lesions such as syringomyelia or cervical spondylotic myelopathy based on the vulnerability of intramedullary A-delta fibers [4-7].
It is unknown whether CSP changes are detectable and altered in accordance with the lesion site of cervical cord disorders. The abductor pollicis brevis (APB) muscle (C8-T1 myotome) and index fingertip (C6-C7 dermatome) are commonly used sites for CSP testing [4,8- 12]. Afferent impulses travel along the C6 and C7 nerve roots, enter the spinal cord, and suppress activity in the motor nuclei of the C8 and T1 myotome via a spinal inhibitory reflex. Therefore, the presence of an intramedullary CSP reflex circuit is implicated at the C6-T1 level [13]. Because spinal segments extend one disc level higher than the intervertebral level (i.e., the C6 spinal segment is located at the C4- C5 intervertebral level) we hypothesized that CSP findings from the APB muscle and index finger would be most significantly influenced by cervical cord lesions between the C4-5 and C7-T1 intervertebral levels [14,15]. To test this hypothesis, we prospectively reviewed CSP changes in 2 cervical compression myelopathy (CCM) patient groups: a group with spinal cord compression at or below the C4- C5 intervertebral level (the ML group) and a group with spinal cord compression at or above the C3-C4 intervertebral level (the U group).
Materials and Methods
Patients
Ninety-five patients with CCM were surgically treated for progressive myelopathy symptoms at our institution between April 2014 and May 2016. Preoperative CSPs were recorded in all patients. We selected 22 patients (12 male patients and 10 female patients; mean age, 66 years; age range, 41–86 years) with transverse lesion-type myelopathy and single-level cord compression with an intramedullary T2 high-signal change confirmed by 1.5-T magnetic resonance imaging (MRI) and a manual muscle testing (MMT) APB score of ≥ 4. Three hands with a MMT APB score ≤ 3 were excluded because severe weakness prohibited the continuous muscle contraction needed for CSP recording. In cases of cord compression at a single site and unilateral APB weakness (MMT ≤ 3), the contralateral hand without weakness was used for the study. Patients with multiple cord compressions or a previous history of cervical spine surgery or cerebrovascular disease were also excluded [16]. Finally, we excluded individuals with peripheral nerve diseases because CSPs are influenced by these conditions [17].
A total of 40 hands met the inclusion criteria and were used for analysis: 30 hands were assigned to the ML group and 10 hands were assigned to the U group. The pathology of CCM was cervical spondylosis for 32 hands in 18 patients, extramedullary tumor for 4 hands in 2 patients, cervical disc herniation for 2 hands in 1 patient, and ossification of the posterior longitudinal ligament for 2 hands in 1 patient. The preoperative clinical severity of cervical myelopathy was evaluated using the Japanese Orthopaedic Association score of cervical myelopathy (JOA score), which is based on motor dysfunction of the upper and lower limbs, the degree of sensory deficits, and bladder dysfunction [18]. The total JOA score ranges from 0–17, with a maximum score of 17 reflecting normal function. This study was approved by the Ethical Review Board of Kochi Medical School. All participants provided written informed consent prior to study participation.
CSP testing
CSP was defined as an absence or a clear reduction (not exceeding 100 μV) of voluntary EMG activity at an appropriate post-stimulus latency. The onset and end of latencies and duration of the absent or reduced interference wave were measured. Sensory threshold intensities were also measured. The mean values of 5 responses were used for the analysis. When no visible CSPs were recorded for more than 2 out of 5 trials, the series of trials was categorized as CSP absent. Abnormal CSP findings included latency delay, shortened duration, and the absence of a CSP [4,6]. Because the end of the latency is influenced by the onset of the latency and its duration, we only analyzed the onset of latency and its duration in this study.
We recorded CSPs in the APB muscle following stimulation of the index fingertip. Single shocks were delivered to the index fingertip using a pair of ring electrodes. Electric stimuli were square waves of 0.2 m in duration with stimulus intensities 20 times stronger than the sensory threshold. The intensity of the sensory threshold was defined as the weakest stimulus intensity that the patient was able to feel subjectively [12]. Surface recording electrodes were attached at the APB muscle using the belly-tendon method. Patients were instructed to keep maximal voluntary contraction of the APB muscle against resistance during the examination. Stimulation was delivered during maximal voluntary contraction and we recorded subsequent transient suppression of muscle contraction interference. This procedure was repeated 5 times with the inter-trial interval varying randomly between 10–20 s. Five single sweeps of 500 ms in duration were recorded with the filter set at 20 and 5000 Hz. CSP testing was performed using standard electrodiagnostic equipment (Neuropack S1; Nihon Koden; Tokyo, Japan) [19-21].
Statistical analysis
To assess between-group differences, Mann-Whitney U tests were used for age, JOA score, sensory threshold intensity, CSP onset latency and CSP duration. All values are expressed as the mean ± standard deviation. JMP statistical software (version 12.01, SAS Institute, Cary, NC) was used for all statistical analyses. P-values<0.05 were considered to be statistically significant.
Results
Patient demographics and lesion characteristics
Table 1 summarizes the patient demographics for each group. No significant differences were observed between the 2 groups (P>0.05). The sites of cord compression were at C1-C2 in 2 patients (4 hands); C3-C4 in 4 patients (6 hands); C4-C5 in 9 patients (17 hands); C5-C6 in 6 patients (11 hands); and C6-C7 in 1 patient (2 hands). The site of the intramedullary T2 high signal change was identical to the cord compression site in all patients.
| Total | U group | ML group | P-value | |
|---|---|---|---|---|
| Number of patients | 22 | 6 | 16 | |
| Male:Female | 12:10 | 3:3 | 9:7 | |
| Age | 66.8 ± 12.1 | 63.8 ± 15.4 | 67.9 ± 11.0 | 0.50 |
| Total JOA score | 8.6 ± 2.5 | 7.8 ± 4.0 | 8.7 ± 1.8 | 0.27 |
Mann–Whitney U tests were used for between-group analyses
P<0.05 was the threshold for statistical significance
JOA score, Japanese Orthopaedic Association score for cervical myelopathy; ML group, cervical compression myelopathy at and below the C4-C5 intervertebral level; U group, cervical compression myelopathy at and above the C3-C4 intervertebral level
Table 1: Patient demographics.
CSP testing
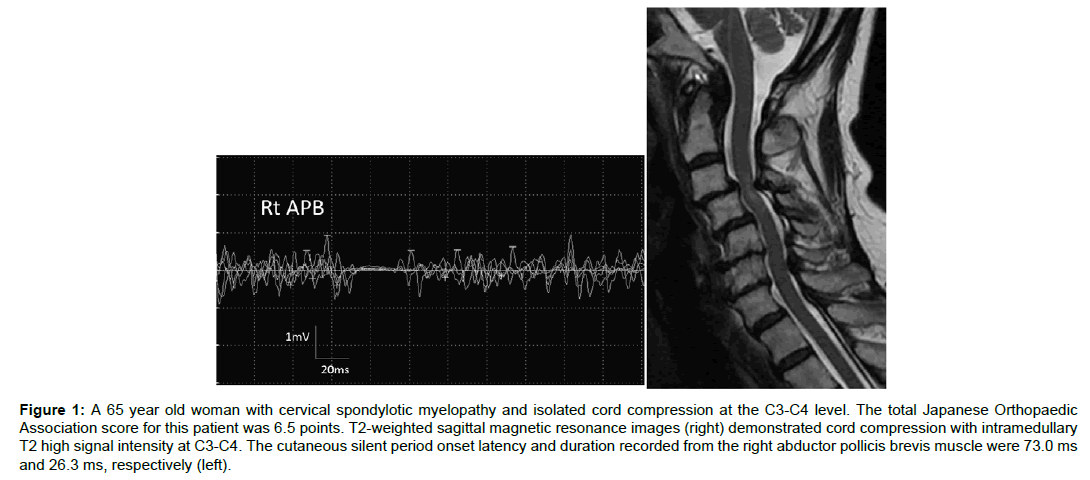
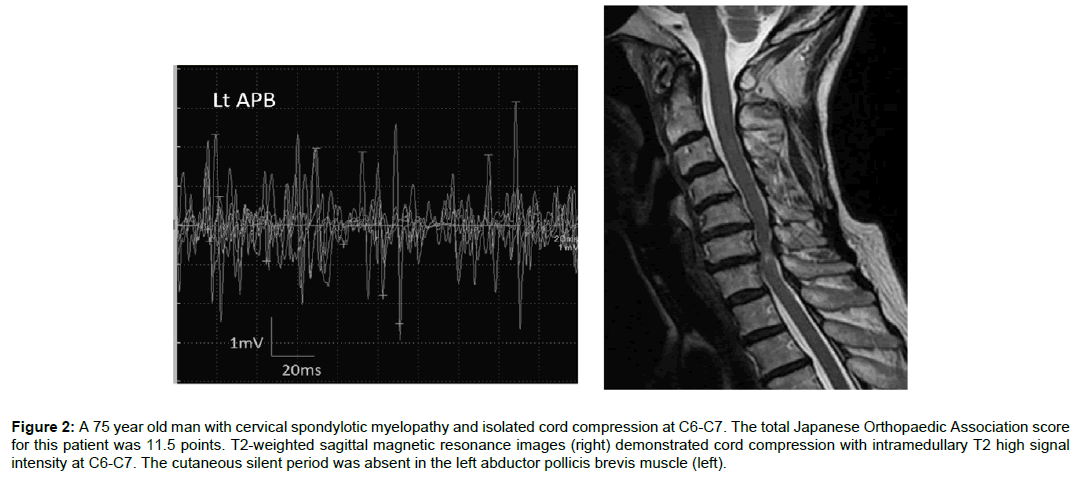
CSPs were recordable in all hands from the U group (Figure 1), but were absent in 8 hands from the ML group (2 hands from patients with C4-C5 compression, 4 hands from patients with C5-C6 compression, and 2 hands from patients with C6-C7 compression) (Figure 2). Table 2 shows CSP parameters in each group. The onset latency was significantly delayed in the ML group compared to the U group (P=0.0001), whereas CSP duration was not significantly between groups (P=0.9). Sensory thresholds in the U and ML groups were 2.9 ± 0.8 mA and 2.9 ± 0.7 mA, respectively (P=0.9).
Figure 1: A 65 year old woman with cervical spondylotic myelopathy and isolated cord compression at the C3-C4 level. The total Japanese Orthopaedic Association score for this patient was 6.5 points. T2-weighted sagittal magnetic resonance images (right) demonstrated cord compression with intramedullary T2 high signal intensity at C3-C4. The cutaneous silent period onset latency and duration recorded from the right abductor pollicis brevis muscle were 73.0 ms and 26.3 ms, respectively (left).
Figure 2: A 75 year old man with cervical spondylotic myelopathy and isolated cord compression at C6-C7. The total Japanese Orthopaedic Association score for this patient was 11.5 points. T2-weighted sagittal magnetic resonance images (right) demonstrated cord compression with intramedullary T2 high signal intensity at C6-C7. The cutaneous silent period was absent in the left abductor pollicis brevis muscle (left).
| U group (n=10) | ML group (n=22) | P-value | |
|---|---|---|---|
| Onset latency (ms) | 77.0 ± 5.6 | 94.5 ± 11.8 | 0.0001* |
| Duration (ms) | 42.9 ± 14.5 | 43.5 ± 24.2 | 0.9 |
P<0.05 was the threshold for statistical significance
ML group, cervical compression myelopathy at and below the C4-C5 intervertebral level; U group, cervical compression myelopathy at and above the C3-C4 intervertebral level
Table 2: Cutaneous silent period (CSP) parameters in each group.
Discussion
In this study, we found that CSP onset latencies were prolonged in patients with CCM in the middle and lower cervical spine. Twelve of 22 hands from the ML group showed had onset latencies longer than 92 ms, which is the longest upper limit for onset latency [4-7]. In contrast, the onset latency for the upper cervical CCM group reached 87.1 ms. Absent CSPs were only observed in the ML group. These findings support our hypothesis. The results of previous studies indicate that CSP abnormalities are specifically associated with the implicated cervical cord region. Stetkarova et al. evaluated CSP changes in mild cervical spondylotic myelopathy (CSM) and found nearly normal CSPs in 2 patients with cord compression at the C3- C4 intervertebral level [6]. Kofler et al. also reported normal CSPs in patients with thoracic myelopathy [5].
Stimulus strength and clinical severity influence CSP changes [3,19,20]. The sensory thresholds that defined the stimulus strength and JOA score were not different between groups. These findings also support our hypothesis.
The duration of the CSP was not different between groups. Lopergolo et al. found that axonal neuropathy was associated with decreased CSP durations and CSP absence, while demyelinating neuropathy was associated with prolonged CSP latencies [21]. Different patterns of CSP changes in various disease states should be examined in future studies.
The present study had the following limitations. First, the statistical power of our analysis was limited by a small sample size. Second, our cohort included patients with relatively heterogeneous diseases, including degenerative cervical myelopathy and extramedullary tumor. Nevertheless, this study demonstrates that CSP onset latency is affected by the site of spinal cord compression. The results of this study may help to evaluate the patients with cervical compression myelopathy using CSP testing.
Conflict of Interest
There is no conflict of interest in this study.
References
- Leis AA, Kofler M, Stetkarova I, Stokic DS (2011) The cutaneous silent period is preserved in cervical radiculopathy: significance for the diagnosis of cervical myelopathy. Eur Spine J 20: 236-239.
- Caccia MR, McComas AJ, Upton AR, Blogg T (1973) Cutaneous reflexes in small muscles of the hand. J Neurol Neurosurg Psychiatry 36: 960-977.
- Inghilleri M, Cruccu G, Argenta M, Polidori L, Manfredi M (1997) Silent period in upper limb muscles after noxious cutaneous stimulation in man. Electroencephalogr Clin Neurophysiol 105: 109-115.
- Roser F, Ebner FH, Liebsch M, Dietz K, Tatagiba M (2008) A new concept in the electrophysiological evaluation of syringomyelia. J Neurosurg Spine 8: 517-523.
- Kofler M, Kronenberg MF, Brenneis C, Felber A, Saltuari L (2003) Cutaneous silent periods in intramedullary spinal cord lesions. J Neurol Sci 216: 67-79.
- Stetkarova I, Kofler M (2009) Cutaneous silent periods in the assessment of mild cervical spondylotic myelopathy. Spine 34: 34-42.
- Lo YL, Tan YE, Dan YF, Leoh TH, Tan SB, et al. (2007) Cutaneous silent periods in the evaluation of cord compression in cervical spondylosis. J Neurol 254: 14-19.
- Levin KH, Maggiano HJ, Wilbourn AJ (1996) Cervical radiculopathies: comparison of surgical and EMG localization of single-root lesions. Neurology 46: 1022-1025.
- Chiba T, Konoeda F, Higashihara M, Kamiya H, Oishi C, et al. (2015) C8 and T1 innervation of forearm muscles. Clin Neurophysiol 126: 837-842.
- Rainville J, Laxer E, Keel J, Pena E, Kim D, et al. (2016) Exploration of sensory impairments associated with C6 and C7 radiculopathies. Spine J 16: 49-54.
- Lee MW, McPhee RW, Stringer MD (2008) An evidence-based approach to human dermatomes. Clin Anat 21: 363-373.
- Kofler M (2003) Functional organization of exteroceptive inhibition following nociceptive electrical fingertip stimulation in humans. Clin Neurophysiol 114: 973-980.
- Leis AA, Kofler M (2014) Silent Period. Silent Period In: Aminoff MJ and Daroff RB. Encyclopedia of the Neurological Sciences. (2nd edtn), Oxford: Academic Press 4: 164-168.
- Seichi A, Takeshita K, Kawaguchi H, Matsudaira K, Higashikawa A, et al. (2006) Neurologic level diagnosis of cervical stenotic myelopathy. Spine. 31: 1338-1343.
- Cadotte DW, Cadotte A, Cohen-Adad J, Fleet D, Livne M, et al. (2015) Characterizing the location of spinal and vertebral levels in the human cervical spinal cord. AJNR American journal of neuroradiology. 36: 803-810.
- Gilio F, Bettolo CM, Conte A, Iacovelli E, Frasca V, et al. (2008) Influence of the corticospinal tract on the cutaneous silent period: a study in patients with pyramidal syndrome. Neurosci Lett 433: 109-113.
- Koo YS, Park HR, Joo BE, Choi JY, Jung KY, et al. (2010) Utility of the cutaneous silent period in the evaluation of carpal tunnel syndrome. Clin Neurophysiol. 121: 1584-1588.
- Wada E, Suzuki S, Kanazawa A, Matsuoka T, Miyamoto S, et al. (2001) Subtotal corpectomy versus laminoplasty for multilevel cervical spondylotic myelopathy: a long-term follow-up study over 10 years. Spine. 26: 1443-1437.
- Leis AA, Stokic DS, Fuhr P, Kofler M, Kronenberg MF, et al. (2000) Nociceptive fingertip stimulation inhibits synergistic motoneuron pools in the human upper limb. Neurology. 55: 1305-1309.
- Aurora SK, Ahmad BK, Aurora TK (1998) Silent period abnormalities in carpal tunnel syndrome. Muscle Nerve. 21: 1213-1215.
- Lopergolo D, Isak B, Gabriele M, Onesti E, Ceccanti M, et al. (2015) Cutaneous silent period recordings in demyelinating and axonal polyneuropathies. Clin Neurophysiol. 126: 1780-1789.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi