Research Article, Jceog Vol: 9 Issue: 6
Secondary Malignant Neoplasms in Patients with Primary Hypopharyngeal Squamous Cell Carcinoma: An Analysis from SEER Database
Qingtong Liu1*, Yuan Wang1 and Gang Jin2
1Department of Gastroenterology, The Second Hospital of Shanxi Medical University. Shanxi, China
2Department of Oncology, The Second Hospital of Shanxi Medical University, Shanxi, China
*Corresponding Author: Qingtong Liu
M.D. Departments of Gastroenterology, The Second Hospital of Shanxi Medical University. NO. 382, Wuyi Road, Shanxi, 030001, China
Tel: +86-22-23345609 (O)
E-mail: mxy96510@163.com
Received: October 13, 2020 Accepted: October 22, 2020 Published: October 29, 2020
Citation: Liu Q, Wang Y, Jin G (2020) Secondary Malignant Neoplasms in Patients with Primary Hypopharyngeal Squamous Cell Carcinoma: An Analysis from SEER Database. J Clin Exp Oncol 9:6. doi: 10.37532/jceog.2020.9(6).256
Abstract
Purpose: An increasing attention has turned to the burden of secondary malignant neoplasms (SMNs) in long-term cancer survivors. The aim of this study was to describe the incidence, and survival outcomes of SMNs in primary hypopharyngeal squamous cell carcinoma (HSCC). Materials and Methods: Patients with primary diagnosis with HSCC and reported to the Surveillance, Epidemiology, and End Results (SEER) program between 1973 and 2016 were eligible for this study. Kaplan-Meier method was used to estimate the cumulative incidence of SMNs and survival rates. Standardized incidence ratios (SIRs) of SMNs after primary HSCC were also assessed. Results: A total of 8518 patients diagnosed with HSCC as their first malignancy were included (median follow-up: 142 months). 984 patients developed SMNs with a median time from primary diagnosis to an SMN diagnosis was 3.8 years. The cumulative incidences of any SMNs were 30% at 10 years, and 54% at 20 years. The top three common secondary tumors were lung, esophageal and oral cavity cancer, with cumulative incidence rates of 22%, 12% and 9% at 20 years, irrespectively. The SIR for SMNs in survivors of HSCC compared with the general population was 2.86 and 5-year overall survival (OS) rate after SMNS was 16%. Esophageal carcinoma as a SMN showed the highest SIR of 23.81 and presented with the lowest 5-year OS rate of 7%. Conclusions: Survivors of HSCC are at increased risks of developing SMNs compared with the baseline population. Patients developed oesophageal carcinoma as SMNs showed the highest SIR and shortest survival
Keywords: Second primary malignancy, Hypopharyngeal cancer, Cumulative incidence, Survival, Risk factor
Introduction
Head and neck cancer are the seventh most common cancer in the world and encompasses a group of malignancies arising from several mucosal sites. Most (95%) of histopathological types of head and neck cancer are squamous cell carcinoma (HNSCC) [1,2]. The important etiologist included alcohol, tobacco, and human papillomavirus (HPV)-infection, which have been confirmed with great association with incidence of HNSCC. Mounting evidences demonstrate that long-term survivors after HNSCCs are at high rates of subsequent second primary malignancy [3,4].
It has been reported that an excess risk of SMNs was existed in patients HNSCCs, with 2% to 3% per year and the risk remains constant throughout the lifetime [5]. The overall incidence of SMNs in HNSCC patients was observed to range from 9.1% to 19.0% [6]. To be noted that head and neck squamous cell cancer are consisted of tumour in different sites, including oral cavity, oropharynx, larynx, and hypopharynx. The incidences of SMNs in different locations varied largely [7,8]. Previous studies showed that anatomic site of index cancer is one of the most important factors associated with SMNs. Among different sites of head and neck cancer, hypopharyngeal cancer is identified with the highest risk of developing SMNs, about 2-folds than other sites in head and neck [6]. As to the most frequently SMNs after primary tumour, there are some inconsistencies among different studies [8,9]. Liu et al. and Chen et al. reported that the most common SMNs were localized in upper digestive tract [7,9], Leon X et al. demonstrated that the most common secondary neoplasm is head and neck cancer [10], while Milano et al. and Chuang et al. declared that lung cancer is the most frequent SMNs [3,8]. These inconsistencies might be due to the different sample sizes, data sources, and calculated methods.
Survival outcomes after HNSCC appears to be improved because of evolutions in the etiologist of disease, improvements in tobacco control, and advances in therapies. In patients survived from head and neck cancer, secondary primary malignancies had great adverse influence on their quality of life and long-term survival. Recent years, SMNs have been recognized as the leading long-term cause of mortality in HNSCCs [11,12]. Rennebohm et al. observed that the prognosis was poor for patients with SMNs, with the median survival was only 12 months [13]. Therefore, SMNs remain a major problem, and to understand the characteristics of SMNs after primary HPSCC is of vital clinical use.
In this study, we sought to examine the cumulative incidence of SMNs, to identify risk factors associated with SMNs occurrence and assess cause-specific mortality in a large cohort of recently diagnosed HSCC patients in SEER database.
Materials and Methods
Patients and Case Definition
Patient information was gathered from the 18 registries of the Surveillance, Epidemiology, and End Results (SEER) program of the United States National Cancer Institute, which included data from 1973 to 2016. Patients diagnosed with hypopharyngeal squamous cell carcinoma (international code disease-0-3 (ICD-0-3)/ world health organization (WHO) 2008 = hypopharynx, and ICD-0-3 hist/behave, malignant: 8052/3, 8053/4, 8070/3, 8071/3, 8072/3, 8073/3, 8074/3, 8075/3, 8076/3, 8077/3, 8078/3, 8083/3, 8084/3) was determined using the sequence number field in SEER. A total of 15650 patients with primary HSCC were selected, after excluding patients who had a malignancy before their HSCC diagnosis, patient with secondary malignancies within 6 months of their primary HSCC diagnosis, and also patients with a secondary benign neoplasm, 984 patients with a clear SMN and 7534 patients without SMN were identified. Leukaemia’s, myeloproliferative disease, myelodysplastic disease, and lymphomas were all considered to be hematologic malignancies. All other types of malignancies other than hematologic malignancies were considered to be solid tumour.
Analytic Variables
Evaluated predictor variables included age, gender, year of diagnosis, histology grade, surgery, exposure to radiotherapy, and exposure to chemotherapy. Primary outcomes included incidence of SMN and survival time after SMN.
Statistical Analysis
Time to events was from the day of initial diagnoses of index tumours to the first occurrence of events (SMNs and mortality). The cumulative incidence of SMNs and overall survival were estimated using the Kaplan-Meier methods. Standardized incidence ratios (SIRs) were calculated within the SEER database. The SEER database was accessed using SEER Stat version 8.3.6. Statistical analyses were performed using SPSS 23.0. No IRB/ethics committee approval or patient consent was needed to conduct this study as per SEER dataset requirements.
Results
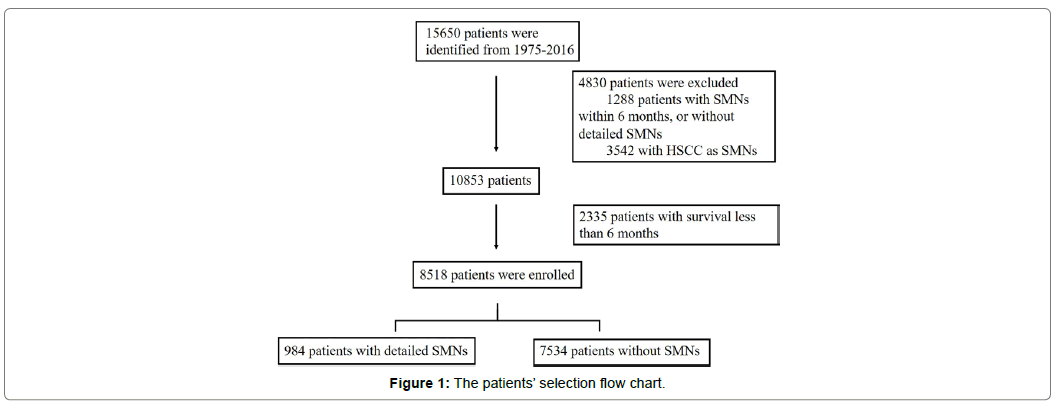
A total of 15650 patients with primary hypopharyngeal squamous cell carcinoma (HSCC) were reported in the SEER database. After excluding 5781 patients with tumours pre-existing than HSCC or within 6 months after HSCC, and patients with benign tumours, 9869 patients diagnosed with primary HSCC with or without clear SMNs were left. Since we only included patients developed malignancies more than 6 months after primary HSCC diagnosis, 2335 patients with survival less than 6 months were also excluded. Finally, a total of 8518 patients were enrolled in this study, including 984 patients with detailed SMNs and 7534 patients without SMNs. The patients’ selection flowchart is displayed in the Figure 1.
Incidence of SMNs after HSCC
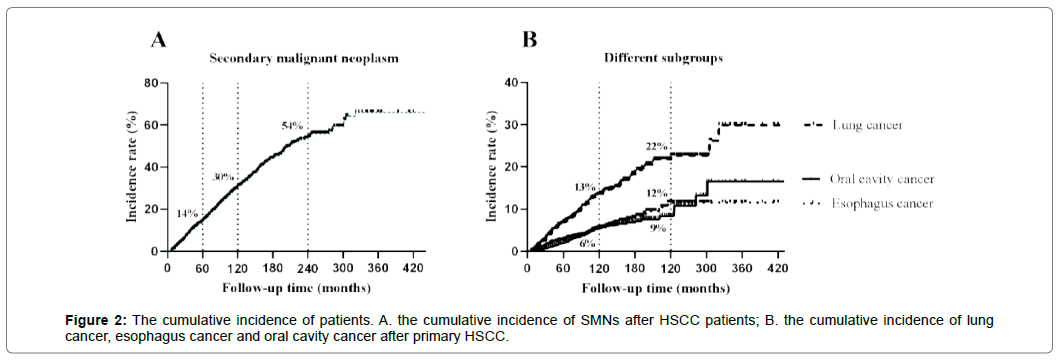
The median time of developing SMNs were 46 months. The cumulative incidence of any SMN was 14% at 5 years, 30% at 10 years, 54% at 20 years after the initial diagnosis of HSCC Figure 2A. Among them, the top three most common malignant tumours were lung, oesophageal, and oral cavity cancer, with median latencies of 39 months, 38 months and 55 months, irrespectively. The incidence of lung cancer as the secondary malignancy was13% at 10 years and 22% at 20 years, followed by oesophageal cancer with 6% at 10 years, and 12% at 20 years. And the third one was oral cavity cancer presented with 6% at 10 years, and 9% at 20 years, plotted in Figure 2B.
Compared with general population, HSCC patients were at a 2.86-fold increased risk of developing an SMN of any type (standard incidence ratio (SIR), 2.86; 95% CI, 2.7-3.03) in the observed period of 1973 through 2016 Table 1. Female showed higher risks than male (SIR was 3.30 in female, compared 2.77 in male). Among all the solid tumours, the highest SIR was found in oesophageal cancer, with SIR of 23.81 (19.89-28.27), and female showed higher SIR than male (SIRs was 53.13 in female and 21.16 in male), details showed in Table 2. The SIRs of oral cavity and lung cancer as SMNs were 20.47 and 6.17, respectively.
| Total | Male | Female | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Neoplasm | SIR | 95%CI | Excess risk | SIR | 95%CI | Excess risk | SIR | 95%CI | Excess risk |
| All sites | 2.86# | 2.7-3.03 | 347 | 2.77# | 2.6-2.96 | 359 | 3.30# | 2.89-3.75 | 308 |
| All solid tumor | 3.07# | 2.89-3.26 | 345 | 2.99# | 2.8-3.2 | 362 | 3.45# | 3-3.94 | 292 |
| Oral cavity and pharynx | 25.98# | 19.57-33.59 | 98 | 18.33# | 15.75-21.21 | 102 | 37.63# | 27.55-50.2 | 86 |
| Digestive System | 3.19# | 2.82-3.6 | 83 | 3.13# | 2.72-3.58 | 88 | 3.48# | 2.59-4.58 | 70 |
| Respiratory System | 6.10# | 5.54-6.69 | 168 | 5.69# | 5.11-6.32 | 173 | 8.41# | 6.77-10.33 | 153 |
| Bones and joints | 0 | 0-0 | 11.17 | 0 | 0-26.53 | -0.71 | 0 | 0-60.81 | -0.12 |
| Soft tissue including heart | 2.84 | 0.92-6.62 | 1.48 | 2.74 | 0.75-7.02 | 1.53 | 3.3 | 0.08-18.4 | 1.33 |
| Skins excluding basal and squamous | 0.72 | 0.35-1.33 | -1.74 | 1.07 | 0.03-5.96 | 0.33 | 0.54 | 0.01-3.03 | -1.6 |
| Breast | 0.78 | 0.44-2.8 | 3.34 | 1.47 | 0.04-8.18 | 0.19 | 0.75 | 0.42-1.24 | -9.45 |
| Female genital system | 0.6 | 0.19-1.4 | -1.53 | - | - | - | 0.6 | 0.19-1.4 | -6.4 |
| Male genital system | 0.9 | 0.73-1.1 | -6.26 | 0.9 | 0.73-1.1 | -6.26 | - | - | - |
| Urinary system | 1.33 | 0.98-1.75 | 5.63 | 1.32 | 0.96-1.76 | 6.53 | 1.4 | 0.46-3.28 | 2.75 |
| Eye and orbit | 3.48 | 0.42-12.56 | 0.65 | 2.12 | 0.05-11.79 | 0.32 | 9.76 | 0.25-54.38 | 1.72 |
| Brain and other nervous system | 0.51 | 0.06-1.83 | -0.9 | 3.07 | 0.08-17.12 | 3.45 | 0 | 0-5.13 | -1.38 |
| Endocrine system | 1.43 | 0.39-3.67 | 0.55 | 2.1 | 0.57-5.38 | 1.26 | 0 | 0-4.16 | -1.7 |
| Hemato | 0.74 | 0.47-1.1 | -3.84 | 0.71 | 0.43-1.11 | -4.67 | 0.89 | 0.29-2.07 | -1.22 |
| Mesothelioma | 0 | 0-2.84 | -0.59 | 0 | 0-3.02 | -0.73 | 0 | 0-47.86 | -0.15 |
| Kaposi sarcoma | 0 | 0-9.9 | -0.17 | 0 | 0-10.45 | -0.21 | 0 | 0-23.33 | -2.92 |
| Miscellaneous | 2.09# | 1.26-3.27 | 4.54 | 1.25 | 0.57-2.37 | 1.07 | 5.36# | 2.57-9.86 | 15.57 |
Table 1: SIR of SMNs in patients with primary hypopharyngeal squamous cell carcinoma #means with significant difference.
| Total | Male | Female | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Latency | Patients | SIR | 95%CI | Patients | SIR | 95%CI | Patients | SIR | 95%CI |
| Total | 130 | 23.81# | 19.89-28.27 | 106 | 21.16# | 17.33-25.6 | 24 | 53.13# | 34.04-79.05 |
| 6-11m | 13 | 23.45# | 12.48-40.1 | 10 | 19.43# | 9.32-35.74 | 3 | 75.22# | 15.51-219.83 |
| 12-59m | 67 | 29.18# | 22.62-37.06 | 58 | 27.36# | 20.77-35.37 | 9 | 51.24 | 23.43-97.27 |
| 60-119m | 31 | 22.16# | 15.05-31.45 | 23 | 18.02# | 11.42-27.04 | 8 | 65.14 | 28.12-128.36 |
| 120+m | 19 | 15.69# | 9.44-24.5 | 15 | 13.66# | 7.65-22.54 | 4 | 35.27 | 9.61-90.31 |
Table 2: SIR of esophageal carcinoma in patients with primary hypopharyngeal squamous cell carcinoma.
Features of patients with SMNs after HSCC
In order to identify risk features associated with SMNs after HSCC, patients were divided into two groups, with or without SMNs. The clinical characteristics and treatment data were showed in Table 3. There were no significantly difference between race, gender, age, and RT between two groups. However, compared with patients without SMN, patients with SMNs showed higher percentages in diagnosed in early year, lower histologic grade, surgery delivered, and without exposure to chemotherapy.
| HSCC without SMNs | HSCC with SMNs | p | ||||
|---|---|---|---|---|---|---|
| Cases Rates | Cases Rates | |||||
| Race | White | 5848 | 77.6% | 776 | 78.9% | 0.379 |
| Non-white | 1686 | 22.4% | 208 | 21.1% | ||
| Gender | Male | 5978 | 79.3% | 788 | 80.1% | 0.615 |
| Female | 1556 | 20.7% | 196 | 19.9% | ||
| Age | ≤60 yrs | 3276 | 43.5% | 447 | 45.4% | 0.259 |
| >60 yrs | 4258 | 56.5% | 537 | 54.6% | ||
| Years of diagnosis | 1975-1989 | 1865 | 24.8% | 427 | 43.4% | 0.000 |
| 1990-1999 | 1422 | 18.9% | 280 | 28.5% | ||
| 2000-2009 | 2542 | 33.7% | 211 | 21.4% | ||
| 2010-2016 | 1702 | 22.6% | 66 | 6.7% | ||
| Grade | Grade 1-2 | 3413 | 45.3% | 499 | 49.7% | 0.015 |
| Grade 3-4 | 2606 | 34.6% | 298 | 30.3% | ||
| UK | 1515 | 20.1% | 197 | 20.0% | ||
| Surgery | Yes | 2683 | 35.6% | 559 | 56.8% | 0.000 |
| No/Unknown | 4851 | 64.6% | 425 | 43.2% | ||
| Radiotherapy | Yes | 6403 | 85.0% | 833 | 84.7% | 0.783 |
| No/Unknown | 1131 | 15.0% | 151 | 15.3% | ||
| Chemotherapy | Yes | 3776 | 50.1% | 318 | 32.3% | 0.000 |
| No/Unknown | 3758 | 49.9% | 666 | 67.7% | ||
Table 3: Clinical characteristics in patients with primary HSCC with or without SMNs.
In univariate analysis, SMNs were significantly associated with gender (p=0.020), race (p=0.042), grade (p=0.005), year of diagnosis (p=0.000), surgery (p=0.000), and chemotherapy (p=0.000). While in multivariate analysis, only gender (p=0.000), race (p=0.000), grade (p=0.000) and year of diagnosis (p=0.000) were identified as significantly independent factors associated with SMNs Table 4. Compared with white patients, non-white patients showed 20.8% increasing in developing SMNs. High grade diseases demonstrated 14.8% decreasing in occurrence of SMNs than low grade diseases. And another significantly important factor associated with SMNs was years of diagnosis, compared with patients diagnosed in 1975-1989, patients diagnosed in years after 1989 showed a great decreasing in developing SMNs, with a large decreasing range from 20-60%.
| Factors | Univariate analysis | Multivariate analysis | |||||
|---|---|---|---|---|---|---|---|
| HR | 95%CI | p | HR | 95%CI | p | ||
| Race | No-white vs. white | 1.172 | 1.005-1.366 | 0.042 | 1.203 | 1.031-1.408 | 0.019 |
| Gender | Male vs. Female | 1.205 | 1.030-1.409 | 0.020 | 1.203 | 1.031-1.403 | 0.019 |
| AGE | >60 vs. ≤60 | 1.093 | 0.979-1.221 | 0.114 | - | - | - |
| Diagnostic year | Reference | 1 | 1 | ||||
| 1990-1999 | 0.812 | 0.698-0.944 | 0.007 | 0.818 | 0.702-0.954 | 0.010 | |
| 2000-2009 | 0.404 | 0.342-0.477 | 0.000 | 0.400 | 0.339-0.473 | 0.000 | |
| 2010-2016 | 0.417 | 0.320-0.543 | 0.000 | 0.408 | 0.313-0.532 | 0.000 | |
| Grade | 3-4 vs. 1-2 | 0.812 | 0.703-0.938 | 0.005 | 0.852 | 0.737-0.985 | 0.003 |
| Surgery | Yes vs. No/unknown | 1.405 | 1.237-1.597 | 0.000 | - | - | - |
| Radiotherapy | Yes vs. No/unknown | 0.936 | 0.787-1.114 | 0.459 | - | - | - |
| chemotherapy | Yes vs. No/unknown | 0.672 | 0.587-0.769 | 0.000 | - | - | - |
Table 4: Univariate and multivariate analysis of risk factors associated with SMNs and esophageal carcinoma in patients with primary HSCC.
Survival after SMNs
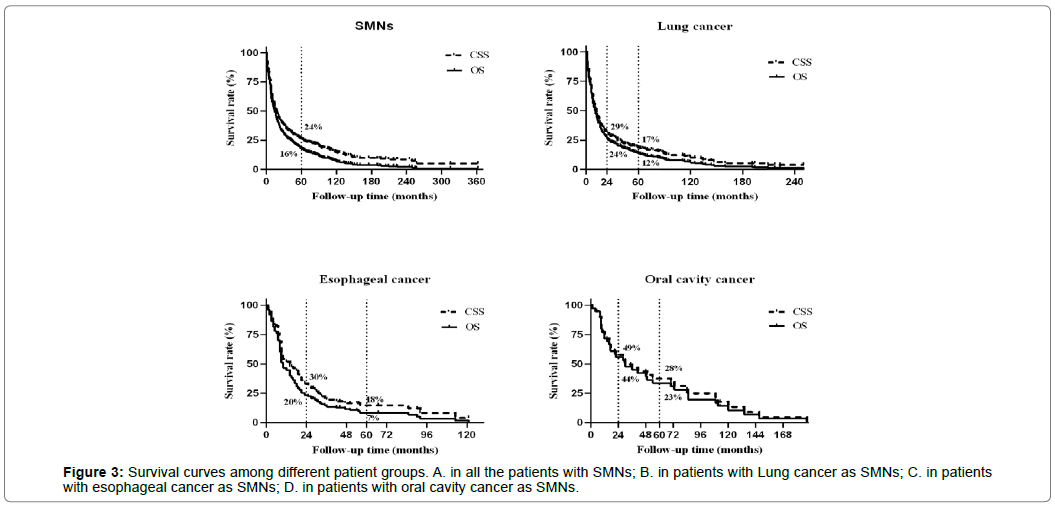
7534 HSCC patients without SMN showed a median survival of 22 months, and 5-year OS rate of 27%. However, the overall survival after SMNs in 984 patients were generally poor, with the median overall survival of 11 months, and 5-year OS rate of 16%. Among the top three common secondary tumors, the overall survival rate was lowest in patients developing oesophageal carcinoma, with an estimated 5-year OS of 7%, and a median survival time of 9 months. Patients diagnosed with lung cancer as SMN showed 5-year OS of 12%, and a median survival of 10 months. Patients with oral cavity cancer as SMNs showed 5-year OS of 25%, with a median survival of 20 months. Survival curves displayed in Figure 3.
Discussion
This is a retrospective analysis of secondary malignant neoplasms in hypopharyngeal squamous cell carcinoma from a populational database. The objective of this study was to assess the risk of SMNs and explore factors potentially affecting this risk within a large cohort of HSCC patients. Our results demonstrated survivors after HSCC are at a 2.86-fold increased risk of developing an SMN of any type compared with the baseline population, with a cumulative incidence of 30% at 10 years, and 54% at 20 years. The top three common SMNs were tumours in lung, esophagus and oral cavity. Among them, oesophageal cancer as a SMN after HSCC with the highest SIR of 23.8 and the shortest median survival of 9 months.
Head and neck cancers is a common cancer in the world and encompasses a group of malignancies arising from several mucosal sites [2]. Hypopharyngeal squamous cell carcinoma is not prevalent but represents a distinct clinical entity from other head and neck squamous cell carcinoma. Evidence have showed that head and neck cancer have high risks of developing SMNs [6]. Numerous researchers have attempted to identify the types of index tumour in head and neck and demonstrated that great variations existed in the risks of developing SMNs [5,14]. Lei et al. reported that the 10-year cumulative incidence of SMNs in hypopharyngeal squamous cell cancer was 42%, which was higher than other head and neck sites (laryngeal cancer was 23%, oral cavity was 17%, and oropharyngeal cancer was 19%) [6]. Form our results, the incidence of SMNs were 30% at 10 years and 54% at 20 years. These means that in HSCC patients survived more than 10 years, one in third will develop second malignancies, and in those survived more than 20 years, half of them will develop SMNs.
It has been well described that the most frequent type of synchronous malignancies in HSCC was esophageal cancer, about half of the synchronous diseases were esophageal cancer [15], however, less was known about the metachronous SMNs (SMNs developed more than 6 months after an index cancer diagnosis) [16]. In our study, in order to discover the patterns of SMNs after HSCC, only metachronous SMNs were included. Previously studies showed that in patients with index HNSCC, most cases of SMNs arouse in the head and neck regions [10]. There are also many literatures showed that esophagus cancer was the most common SMNs after primary HNSCC [3,9]. However, recent studies have shown that lung was the most common site of SMNs in patients with index HNSCC [3,8] and our data was in agreement with these findings. Our study demonstrated that lung cancer was with highest cumulative incidence among the second malignant neoplasms, with a cumulative incidence of 22% at 20 years. However, when compared the standard incidence ratio, esophagus cancer as SMNs presented with the highest SIR, suggesting a 24-fold increased risk than general population.
In the light of the significant risks of SMNs in HNSCC patients, it is crucial to refine our understanding of SMNs risk among patients with index HNSCC to optimize screening and follow-up strategies and improve long-term outcomes. To our best knowledge, studies has revealed a dramatic shift in the rates of SMNs development among patients with HNSCC [13]. Compared to other sites from head and neck region, especially oropharyngeal squamous cell carcinoma (OPSCC), HSCC itself harbours the highest risk of developing SMNs [14,17]. Exposure to alcohol and tobacco were also identified as strong predictors of development of SMNs [6,18]. Several studies have reported that male, young age, smaller index tumour, stage I/II primary tumour, no cervical lymph node metastasis were risk factors [13,19,20]. Regretfully, in our studies, we didn’t obtain the similar results. Male, race, low grade disease and diagnosed in early years were identified as independently significant risk factors associated with SMNs.
It has been well demonstrated that SMNs play a negative influence on survival, with a 5-year survival rates range from 9% to 19% [16,18]. In our study, patients developed SMNs of any type showed the 5-year OS and CSS of 16% and 24%. Among the top three common malignant neoplasms, the 5-year OS after developing oesophagus cancer was 7%, however, patients developed lung cancer and oral cavity cancer showed 5-year OS of 12% and 23%. From our study, HSCC showed high risk of developing SMNs, which played a vital role in influencing prognosis in HSCC. Therefore, it is quite necessary to define the incidence and patterns of SMNs in HSCC, which could be of extremely importance for physicians to design individual follow-up examination protocols. From our results, the highest SIR was found in oesophagus cancer and the shortest survival after SMNs diagnosed was also displayed in oesophagus carcinoma, it is extremely important to identify patients who developed oesophagus cancer in the early stage to improve long-term survival. Therefore, it might be of great help if modalities such as esophagoscopy were utilized to early detect oesophagus cancer in long-term survivors, which might be turned out to significantly improving patients’ outcomes.
The current study cohort of HSCC patients is, to our best knowledge, a large group to examine SMNs. Because of its size, we were able to perform statistical analysis to identify potential risk factors for developing an SMN after treatment of HSCC, and several important findings were obtained from this study. However, there are also limitations need to be noted. Firstly, the SEER registry provides a heterogeneous group of patients with HSCC from across the united states and is not limited to patients enrolled in a clinical trial. Second, the public SEER database does not include detailed information regarding to radiotherapy and chemotherapy. In addition, patients’ smoking and alcohol status couldn’t be obtained from the SEER database, which are of great pities that these two factors couldn’t be analysed in this study.
Conclusions
In conclusion, our study indicate that patients should be monitored indefinitely for SMNs after the completion of their treatment for HSCC. These patients are at a high risk of developing a range of second cancers compared with the general population. The findings of the current study may help to direct the type of surveillance screening for SMNs in this population, with an emphasis on lung, oesophageal and oral cavity cancer.
References
- Shield D, Jemal A, Sankaranarayanan R, Chaturvedi K, Bray F, et.al (2017) The global incidence of lip, oral cavity, and pharyngeal cancers by subsite in 2012. CA Cancer J Clin 67: 51-64.
- Fitzmaurice C, Abate D, Naghmeh A, Hedayat A, Foad A, et al (2019) Global, Regional, and National Cancer Incidence, Mortality, Years of Life Lost, Years Lived With Disability, and Disability-Adjusted Life-Years for 29 Cancer Groups, 1990 to 2017: A Systematic Analysis for the Global Burden of Disease Study. JAMA Oncol 5: 1749-1769.
- Chuang S, Hashibe M, Scelo G, David H, Eero P, et al (2008) Risk of second primary cancer among esophageal cancer patients: a pooled analysis of 13 cancer registries. Cancer Epidemiol Biomarkers Prev 17: 1543-1549.
- Lee K, Chang-Hsien L, Chen P, Jen-Tsun L, Cih-En H, et al (2009) The incidence and risk of developing a second primary esophageal cancer in patients with oral and pharyngeal carcinoma: a population-based study in Taiwan over a 25 year period. BMC Cancer 9: 373.
- Morris L, Sikora A, Patel S (2011) Second primary cancers after an index head and neck cancer: subsite-specific trends in the era of human papillomavirus-associated oropharyngeal cancer. J Clin Oncol 29: 739-746.
- Lee D, Roh J, Baek S (2013) Second cancer incidence, risk factor, and specific mortality in head and neck squamous cell carcinoma. Otolaryngol Head Neck Surg 149: 579-86.
- Chen M, Huang W, Chan C (2010) Impact of second primary esophageal or lung cancer on survival of patients with head and neck cancer. Oral Oncol 46: 249-54.
- Milano M, Peterson C, Zhang H, Deepinder P, Yuhchyau C et al (2012) Second primary lung cancer after head and neck squamous cell cancer: population-based study of risk factors. Head Neck 34:1782-1788.
- Liu W, Chang Y, Lin C (2014) Secondary primary cancer in patients with head and neck carcinoma: the differences among hypopharyngeal, laryngeal, and other sites of head and neck cancer. Eur J Cancer Care (Engl) 23: 36-42.
- Leon X, Quer M, Diez S (1999) Second neoplasm in patients with head and neck cancer. Head Neck 21:204-210.
- Lim H, Kim D, Jung H (2015) Clinical significance of early detection of esophageal cancer in patients with head and neck cancer. Gut Liver 9:159-65.
- Baxi S, Pinheiro L, Patil S, et al (2014) Causes of death in long-term survivors of head and neck cancer. Cancer 120:1507-1513.
- Rennemo E, Zatterstrom U, Boysen M (2008) Impact of second primary tumors on survival in head and neck cancer: an analysis of 2,063 cases. Laryngoscope 118:1350-1356.
- Gan S, Dahlstrom K, Peck B (2013) Incidence and pattern of second primary malignancies in patients with index oropharyngeal cancers versus index nonoropharyngeal head and neck cancers. Cancer 119: 2593-2601.
- Wang W, Lee C, Lee Y (2011) Risk factors for developing synchronous esophageal neoplasia in patients with head and neck cancer. Head Neck 33: 77-81.
- Erkal H, Mendenhall W, Amdur R (2001) Synchronous and metachronous squamous cell carcinomas of the head and neck mucosal sites. J Clin Oncol 19:1358-1362.
- Chaturvedi A, Engels E, Anderson W (2008) Incidence trends for human papillomavirus-related and -unrelated oral squamous cell carcinomas in the United States. J Clin Oncol 26: 612-619.
- Yamamoto E, Shibuya H, Yoshimura R (2002) Site specific dependency of second primary cancer in early stage head and neck squamous cell carcinoma. Cancer 94: 2007-2014.
- Jones A, Morar P, Phillips E (1995) Second primary tumors in patients with head and neck squamous cell carcinoma. Cancer 75:1343-1353.
- Schwartz L, Ozsahin M, Zhang N (1994) Synchronous and metachronous head and neck carcinomas. Cancer 74:1933-1938.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi