Research Article, J Regen Med Vol: 7 Issue: 1
Simulation of Embryonic Environments Produced by the Effect of Estradiol on Induced Pluripotent Stem Cells
Sawako Sakai1, Daihachiro Tomotsune1,2, Kanji Hirashima1, Sakiko Takizawa3, Tadayuki Yokoyama3, Fengming Yue1, Rika Tani1, Ken Matsumoto4 and Katsunori Sasaki1,2*
1Department of Histology and Embryology, Shinshu University School of Medicine, Matsumoto 390-8621, Japan
2Department of Biotechnology and Biomedical Engineering, Institute for Biomedical Sciences, Interdisciplinary Cluster for Cutting Edge Research, Shinshu University Matsumoto, 3-1-1 Asahi, Matsumoto 390-8621, Japan
3Bourbon Corporation, 4-2-14 Matsunami, Kashiwazaki, Niigata 945-8611, Japan
4Nissui Pharmaceutical Co., Ltd., 1075-2 Hokunanmoro, Yuki, Ibaraki 307- 0036, Japan
*Corresponding Author : Katsunori Sasaki
Department of Histology and Embryology, Shinshu University School of Medicine, Matsumoto 390-8621, Japan
Tel: +81-263-37-2589
E-mail: katsmd@shinshu-u.ac.jp
Received: March 08, 2018 Accepted: July 20, 2018 Published: July 27, 2018
Citation: Sakai S, Tomotsune D, Hirashima K, Takizawa S, Yokoyama T, et al. (2018) Simulation of Embryonic Environments Produced by the Effect of Estradiol on Induced Pluripotent Stem Cells. J Regen Med 7:1. doi: 10.4172/2325-9620.1000144
Abstract
Estradiol (E2) is one of the sex steroid hormones, whose various well-known functions include control of the female reproductive system, causing breast cancers, and inhibiting arterial sclerosis. In this study to investigate how E2 affected cell differentiation of induced pluripotent stem cells (iPSCs), we used different methods to culture hiPSCs, the undifferentiated state, longterm culture without passages (natural differentiation), embryoid bodies (EBs), and accelerated differentiation by activin, focusing on marker gene expression, including Brachyury, hepatocyte nuclear factor (HNF) 3β, estrogen receptor α, and other markers. When iPSCs began to differentiate by responding to E2, Brachyury expression decreased regardless of the amount of E2, cell line, or protocol. Other markers were up or down-regulated, but did not show any tendency except in the early stage of EBs. The definite timing that E2 had the strongest effect on the aspect of differentiation was the EB stage analogous to gastrulation, in which E2 repressed Brachyury expression and induced HNF3β at its restricted amount. These results suggest that the first target of E2 is the gastrulation stage.
Keywords: E2; Brachyury; EB; Gastrulation; iPSC
Abbreviations
E2: Estradiol; hiPSC: human induced Pluripotent Stem Cells; HNF3β: Hepatocyte Nuclear Factor; ERα: Estrogen Receptor α; ESR1: Estrogen Receptor 1; EB: Embryoid Body; SIRT1: Sirtuin 1
Introduction
The embryo is exposed to estrogenic environments from the stage of implantation i.e. the blastocyst. Before maturity of fetoplacental circulation, the uterine gland fluid containing estrogen feeds an embryo, because it is secreted from the corpus luteum verum. After fetoplacental circulation is established, maternal blood contains a large amount of estrogen, which increases continuously, because it is secreted from trophoblasts of the placenta. Because of steroid hormone properties, it can pass through the plasma membrane and enter the embryo from the mother’s circulation. In the embryo, 17β-HSD (hydroxysteroid dehydrogenase) type 2, the enzyme that converts estradiol (E2) to estrone (E1), mainly expresses in the fetal liver, gastrointestinal tract and kidney [1]. These facts support that an embryo and/or fetus is continuously exposed to some amount of estrogen after its implantation into the uterus. The effects of E2 on cell differentiation have been studied widely. E2 accelerates morphologic maturation of the fetal rabbit lung [2] and affects the proliferation and differentiation of neural stem cells via estrogen receptors [3], but it is difficult to evaluate the effect of E2 on the extremely early stage of development, because research of human embryos is ethically limited.
hESCs (human embryonic stem cells) and hiPSCs (human induced pluripotent stem cells) similar to hESCs overcome these difficulties. Jung et al. indicated that continuous exposure of mES cells to estrogens resulted in increasing octamer-binding transcription factor 4 expression at the transcriptional level, which maintained their undifferentiated state [4]. Hong et al. revealed the ability of E2 to differentiate hESCs into endodermal marker-expressing cell types (α-fetoprotein, α1-Antitrypsin, GATA-4, and somatostatin) as well as enolase, nuclear factor-68Kda (ectoderm), and Brachyury (mesoderm)-expressing cells from the perspective of gene expression associated with the three germ layers and tissue types [5]. Kim et al. claimed that estradiol had the potential to differentiate hEBs into endodermal or mesodermal cells [6]. In addition, E2 differentiates EBs into osteoblast-like cells [7] hiPSCs, however, have not been target cells so far.
First, according to the above research of differentiation, although the results seemed to have some contradictions e.g. proliferation and maintenance of undifferentiated ES cells as well as promotion of their differentiation at the same time, we tried to differentiate hiPSCs into hepatocytes using E2, but failed to generate mature hepatocytes. This trial was however not meaningless, because we found that estrogen has a definite timing to work at least in early embryonic stages. In the present study, we investigated in detail when E2 affects differential aspects of hiPSCs at variously induced stages including the undifferentiated state, long-term culture without passaged (natural differentiation), embryoid body formation and outgrowth, before and after accelerated differentiation by activin followed by different concentrations of E2, and focused on marker gene expression and accounted for the role of a part of embryonic environments produced by estrogen.
Materials and Methods
hiPSCs and culture
hiPSC lines 201B7 and 253G1 [8] were cultured on a feeder cell layer of mouse embryonic fibroblasts (MEFs; Oriental Yeast Co, Tokyo, Japan) inactivated with mitomycin C (Kyowa Hakko Kirin Co, Tokyo, Japan) and were maintained by repeated passages. The culture medium consisted of 80% KnockOut™ Dulbecco’s minimal Eagle’s medium (DMEM; Gibco, Grand Island, NY, USA) supplemented with 20% KnockOut™ Serum Replacement (Gibco), 100 μM non-essential amino acids (Wako, Chuo-ku, Osaka, Japan), 2 mM L-glutamine (Wako), and 100 μM 2-mercaptoethanol (Sigma, St. Louis, MO, USA).
EB formation and EB outgrowth
Undifferentiated hiPSCs were cultured for 5 days and treated with collagenase IV (Invitrogen, Carlsbad, CA) for 4 min at 37°C. Detached hiPSC colonies were centrifuged and washed with phosphatebuffered saline (PBS). Washed hiPSC colonies were transferred into a non-adherent plate. Suspension cultures were maintained for 5 days in EB medium: 80% knockout DMEM, 100 μM non-essential amino acids, 2 mM L-glutamine, 100 μM 2-mercaptoethanol, and 20% fetal bovine serum (FBS; Hyclone, Logan, UT, USA). EBs were adhered to a gelatin-coated dish and cultured in the same EB medium for the planned number of days.
Activin stimulation
According to our previous report [9], hiPSC colonies were cultured in Roswell Park Memorial Institute media (RPMI) 1640 medium (Wako) containing 2% FBS (Gibco, BRL, USA) with 100 ng/ mL Activin A and 3 μM CHIR99021 for 24 h and then in 2% FBS/ RPMI1640 medium with 100 ng/mL Activin A for 48 h.
Treatment with E2
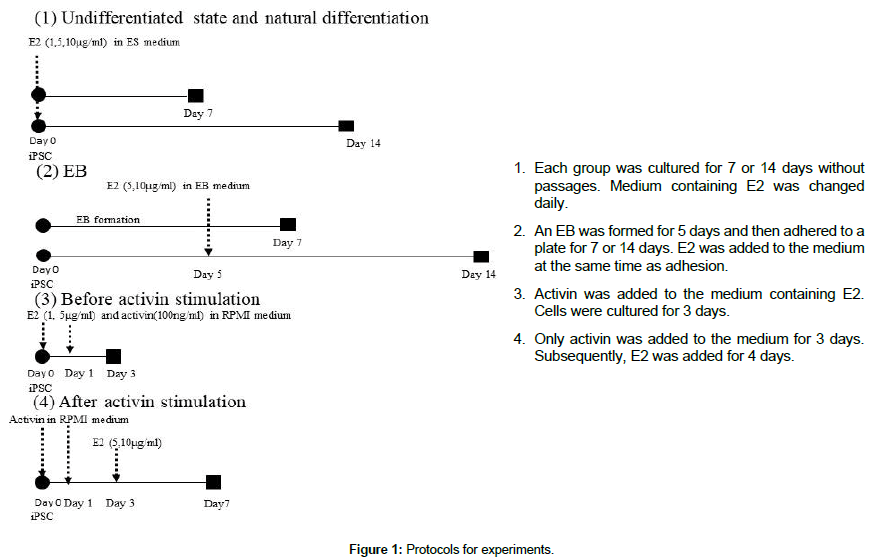
The cells were cultured with E2 (Sigma). The medium was exchanged daily. Acetonitrile was used for the control. The schemes of all experiments are presented in Figure 1.
Quantitative real-time RT-PCR
Total RNA was extracted using TRIzol reagent (Invitrogen) according to the manufacturer’s instructions. Quantitative polymerase chain reaction (PCR) analysis was performed using the Thermal Cycler Dice Real-Time System (Takara Bio, Otsu, Japan). Cycling was performed for 10 min at 95°C, followed by 40 cycles of 5 s at 95°C and 30 s at 60°C, which was the default conditions of Thermal Cycler Dice Real-Time System software TP 800 (version 5.11B). Primer sequences were as follows: HNF3β (Forward: 5′-TAT TGC CCC GTT GAG TGC-3′; Reverse: 5′-TCC CAG GGA AAC TGC AAG-3′), brachyury (5′- GAC AGG TAC CCA ACC CTG AGG A-3′; 5′-AGC ATG GAT AAA CAT GCA GGT GAG-3′), and estrogen receptor α (5′-TTA CTG ACC AAC CTG GCA GA-3′; 5′-ATC ATG GAG GGT CAA ATC CA-3′), and glyceraldehyde-3-phosphate dehydrogenase (GAPDH) (5′-TGG CAC CCA GCA CAA TGA A-3′; 5′-CTA AGT CAT AGT CCG CCT AGA AGC A-3′). PCR was performed in triplicate for each sample, and three independent experiments were carried out.
Immunohistochemistry of ERα
The cultured cells were fixed in 4% paraformaldehyde in 0.1 M phosphate buffer (PBS) (pH 7.4) for 30 min at room temperature, rinsed three times with 20 mM PBS (pH 7.4), and then prepared for immunostaining. The following primary antibody with an appropriate secondary antibody conjugated with Alexa Fluor 488 as well as 6-diamidino-2-phenylindole dihydrochloride (DAPI, Molecular Probes, Eugene, OR, USA) were used: anti-ESR1 (Bethyl Laboratories, Montgomery, TX, USA). For immunohistochemical controls, the primary antibody was omitted.
Statistical analysis
All values in figures and the text are expressed as means ± standard deviation. The significance of differences among mean values was evaluated by Student’s t-test. P<0.05 was considered to be significant.
Results
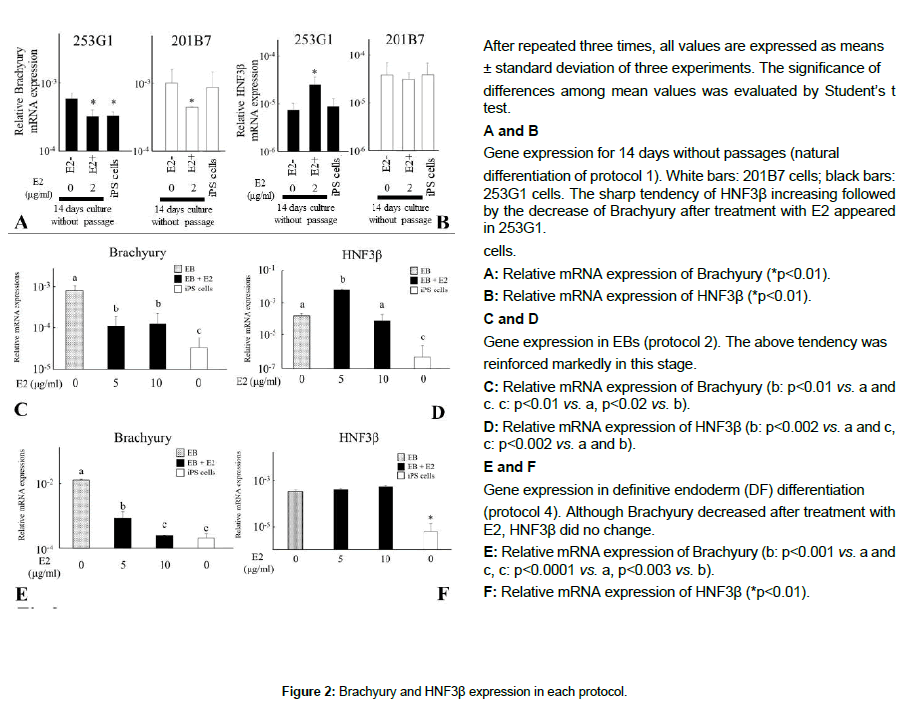
The undifferentiated stage (protocol 1) was near the inner cell mass in the blastocyst and almost showed no response in both cell lines to E2 in terms of cellular differentiation, especially within 1 week, although ERα was detected slightly (Figure 2). Two weeks later, germ layer markers appeared irregularly, depending on whether E2 (5 μg/mL) was added, but did not show any tendency. For example, although the expression level of Brachyury seemed to decrease, HNF3β was upregulated or did not change according to the cell line (Figures 2A and 2B).
The next stage (EB outgrowth protocol 2) was analogous to gastrulation consisting of three germ layers, when the definite timing for E2 to affect differentiation was found. Some germ layer markers were affected by 5 μg/mL E2 (Figures 2C and 2D). HNF3β expression was significantly (about 100 times) higher than in the control, and Brachyury expression was about 10 times lower than in the control. E2 (10 μg/mL) did not change the amount of Brachyury, but lowered HNF3β.
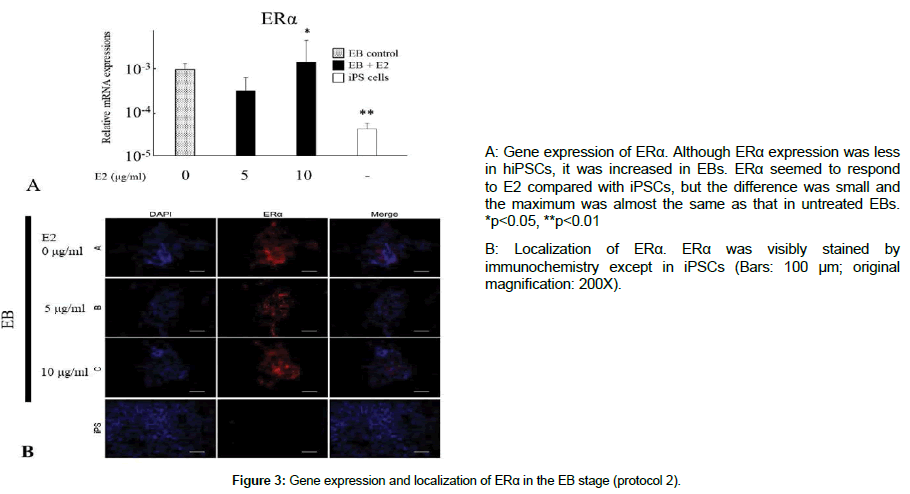
To confirm an interrelationship between E2 and ERs, ERα expression was investigated in RT-PCR and immunohistochemical analyses (Figure 3). ERα was apparently found at each stage (Figure 3A). It was obvious that EB outgrowth showed more ERα expression than hiPSCs. Moreover, the immunohistochemistry confirmed localization of ERα protein irrespective of E2 addition, which supported its gene expression (Figure 3B).
Before (protocol 3) and after (protocol 4) activin stimulation
E2 was added to RPMI1640 medium together with activin to confirm whether it accelerated definitive endoderm with activin (protocol 3), but cells treated with 5 μg/mL E2 did not survive to the end of the experiment. Therefore, cells were cultured in 1 μg/ mL E2-containing medium. The cells survived and expressed only a slightly lower level of Brachyury compared with the expression of other markers, but E2 did not promote differentiation of definitive endoderm.
Next, hiPSCs were stimulated with activin before addition of E2 and then cultured for 4 days in medium containing E2 to confirm whether E2 affected definitive endoderm induced by activin. The marked tendency seen in EBs was lost. Brachyury decreased with E2 treatment, while HNF3β did not change (Figures 2E and 2F).
Thus, addition of E2 decreased the level of Brachyury, but other markers showed only mild or no differences except in the EB stage in which the level of HNF3β was increased by almost 100 times with 5 μg E2 accompanied by the decrease in Brachyury to 1/10 that in the control. Two weeks later, EB outgrowth lost the interrelationship of the increase in HNF3β with the decrease in Brachyury. Only in EBs, especially at the early stage, the sharp tendency of gene expression was found.
Discussion
Definite effects of E2 seem to be limited to a time during development. Its effects were not all found in iPSCs, i.e. at the epiblast-like stage. Only at the early stage of EBs, E2 addition repressed Brachyury and increased HNF3β drastically. At a later stage or in specific tissue differentiation using activin, expression of differentiation markers was up or down-regulated and lost a defined tendency.
EBs are complex three-dimensional aggregates derived from hESCs or hiPSCs and has the ability to mimic post-implantation embryonic tissues [10]. It may be regarded as before the end of week 3 of human development, around day 17 or 18, when gastrulation begins, which establishes all three germ layers. Invagination, the migration of epiblast cells toward the primitive streak, occurs in this stage. Mesoderm and endoderm originate from these invaginating cells. This mesodermal specification needs regulation of Brachyury, one of the T-box family genes, which is expressed in the node, notochord precursor cells, and notochord, regulates the dorsal mesoderm formation in middle and caudal regions of the embryo, and is essential for cell migration through the primitive streak. Brachyury was repressed and expression of endoderm markers such as HNF3β was marked at the early stage of EBs. Based on these results, we elucidated that E2 plays the role of a switch from the limited epiblasts restricted to the primitive streak to endoderm by repressing Brachyury expression, and there is timing when E2 has the strongest effect i.e. the EB outgrowth stage analogous to the early stage of gastrulation.
ERα appeared clearly at the EB stage, but not on iPSCs. It is certain that the effects of E2 depend on ERs, because gene expression became marked at the EB stage, although it did not increase drastically by stimulation with E2. Therefore, ER is necessary for the effects of E2, but is independent of E2 stimulation.
Although the mechanism for E2 to convert the limited epiblasts into endoderm is beyond the scope of our study, the following mechanism may be extracted from several reports. According to a study by Wang’s group, one of the reasons why some types of breast cancers are tamoxifen resistant lies in overexpression of Brachyury [11]. This mechanism is explained by Brachyury downregulating the expression of sirtuin (SIRT) 1 that represses estrogen/estrogen receptor signaling and cell proliferation in estrogen-responsive breast cancer cells by downregulating B-cell leukemia/lymphoma (Bcl)-2 protein [12]. There is a study claiming that E2 upregulates expression of SIRT1 [13]. Consequently, we suggest the possibility that SIRT1 downregulates Brachyury. In almost all experiments of this study, we showed that expression of Brachyury was lower in E2-treated cells than in the control. This result suggests that SIRT1 inhibits Brachyury and the other way around.
In this short communication, we revealed the definite timing to add E2 most effectively was at the early stage of EBs. E2 may differentiate epiblasts, especially into endoderm, at the early stage of embryonic development through the repression of Brachyury.
Acknowledgements
We gratefully thank Ms. A. Yoshitome and Ms. J. Maruyama for their assistance. We thank M. Arico from Edanz Group (www.edanzediting.com/ac) for editing a draft of this manuscript. This work was supported by JSPS KAKENHI Grant Number JP24240076 and JP15H01803.
References
- Takeyama J, Suzuki T, Hirasawa G, Muramatsu Y, Nagura H, et al. (2000) 17 beta-hydroxysteroid dehydrogenase type 1 and 2 expression in the human fetus. J Clin Endocrinol Metab 85: 410-416.
- Khosla S, Smith J, Parks A, Rooney A (1981) Effects of estrogen on fetal rabbit lung maturation: morphological and biochemical studies. Pediatr Res 15: 1274-1281.
- Brannvall K, Korhonen L, Lindholm D (2002) Estrogen receptor-dependent regulation of neural stem cell proliferation and differentiation. Mol Cell Neurosci 21: 512-520
- Jung EM, Choi KC, Yu FH, Jeung EB (2010) Effects of 17beta-estradiol and xenoestrogens on mouse embryonic stem cells. Toxicol In Vitro 24:1538-1545.
- Hong SH, Nah HY, Lee J, Lee JW, Park JH, et al. (2004) Expression of estrogen receptor-alpha and beta, glucocorticoid receptor, and progesterone receptor genes in human embryonic stem cells and embryoid bodies. Mol Cells 18:320-325.
- Kim H, Kim Y, Ku Y, Kim H, Choi M, et al. (2012) The effect of estrogen compounds on human embryoid bodies. Reprod Sci 20: 661-669.
- Tielens S, Wymeersch F, Declercq H, Cornelissen M (2008) Effect of 17beta-estradiol on the in vitro differentiation of murine embryonic stem cells into the osteogenic lineage. In Vitro Cell Dev Biol Anim 44:368-378.
- Takahashi K, Tanabe K, Ohnuki M, Narita M, Ichisaka T, et al. (2007) Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell 131:861-872.
- Yoshie S, Yue F, Mogi A, Yokoyama T, Sasaki K, et al. (2013) FGF7 and cell density are required for final differentiation of pancreatic amylase-positive cells from human ES cells. Cell Tissue Res 354:751-759.
- Sadler TW (2015) Langman’s Medical Embryology (13rd edtn). Wolters Kluwer, Philadelphia,Baltimore,New York, London, Buenos Aires,Hong Kong, Sydney,Tokyo.
- Li K, Ying M, Feng D, Du J, Chen S, et al (2016) Brachyury promotes tamoxifen resistance in breast cancer by targeting SIRT1. Biomed Pharmacother 84:28-33.
- Kuo J, Lin Y, Chien Y, Chen R (2013) SIRT1 suppresses breast cancer growth through downregulation of the Bcl-2 protein. Oncol Rep 30:125-130.
- Han L, Wang P, Zhao G, Wang H, Wang M, et al. (2013) Upregulation of SIRT1 by 17beta-estradiol depends on ubiquitin-proteasome degradation of PPAR-gamma mediated by NEDD4-1. Protein Cell 4: 310-321.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi