Case Report, J Liver Disease Transplant Vol: 7 Issue: 1
Spontaneous Bacterial Empyema Caused by Haemophilus Influenzae in a Patient with Decompensated Alcoholic Liver Cirrhosis
Ushigusa T, Sasaki R*, Akazawa Y, Shibata H, Miuma S, Miyaaki H, Taura N and Nakao K
Department of Gastroenterology and Hepatology, Graduate School of Biomedical Sciences, Nagasaki University, Japan
*Corresponding Author : Ryu Sasaki
Department of Gastroenterology and Hepatology, Graduate School of Biomedical Sciences, Nagasaki University, Nagasaki City, Japan
Tel: +81-958-19-7481
E-mail: ryu03202501@yahoo.co.jp
Received: April 24, 2018 Accepted: May 16, 2018 Published: May 21, 2018
Citation: Ushigusa T, Sasaki R, Akazawa Y, Shibata H, Miuma S, et al. (2018) Spontaneous Bacterial Empyema Caused by Haemophilus Influenzae in a Patient with Decompensated Alcoholic Liver Cirrhosis. J Liver Disease Transplant 7:1 doi: 10.4172/2325-9612.1000161
Abstract
Introduction: Spontaneous bacterial empyema (SBEM) is an infection of a preexisting hydrothorax in patients with cirrhosis. Haemophilus influenzae (H. influenzae) is a Gram-negative bacteria that is commonly involved in upper and lower respiratory infections. Herein, we report our experience with SBEM in a patient with decompensated alcoholic liver cirrhosis caused by H. influenzae.
Case presentation: A 63-year-old man with alcoholic decompensated liver cirrhosis, Child-Pugh class C, and a Model for End-Stage Liver Disease score of 21, was admitted to our hospital. On admission day (day 1), the patient had jaundice with icteric conjunctiva, decreased lung sounds in entire right side of the chest. On the next day (day 2), the patient had fever of 39.2�??. A Gram stain of the pleural effusion revealed Gram-negative rods with remarkable leukocytosis. The blood and pleural effusion cultures were both positive for beta-lactamase-negative ampicillin-resistant H. influenzae. In spite of intensive care for septic shock, his comatose status and liver failure had not improved, and on day 21, the patient died of multiorgan failure.
Conclusion: Although H. influenzae is thought to be an indigenous microorganism in the respiratory tract, to our knowledge, there are no case reports of H. influenzae as a causative bacterium of SBEM. Our case suggests that it is essential to investigate the pathogenesis of hepatic hydrothorax in patients with cirrhosis as well as to offer systemic management and care for bacterial infections.
Keywords: Cirrhosis; Alcoholic liver disease; Hydrothorax; Empyema
Introduction
Late-stage liver cirrhosis often leads to peritoneal effusion and hepatic hydrothorax in some cases. Infection of the peritoneal effusion and hydrothorax lead to a critical condition in patients with liver cirrhosis. Spontaneous bacterial empyema (SBEM) is an infection of a preexisting hydrothorax in patients with cirrhosis and is reported to occur in 13% of such cases [1]. Clinical studies demonstrate a close relationship between the causative organisms of SBEM and spontaneous bacterial peritonitis (SBP). The major pathogenic bacteria in SBEM and SBP are aerobic Gram-negative bacilli, such as Escherichia coli and Klebsiella pneumoniae as well as aerobic Gram-positive cocci, such as Staphylococcus aureus and Enterococcus species [2]. Haemophilus influenzae (H. influenzae), belonging to the Pasteurellaceae family, is a Gram-negative bacteria that is commonly involved in upper and lower respiratory infections. However, SBP caused by H. influenzae is rare with few cases reported [3,4]. It is largely unknown whether H. influenzae causes SBEM. Herein, we report our experience with SBEM in a patient with decompensated alcoholic liver cirrhosis caused by H. influenzae.
Case Report
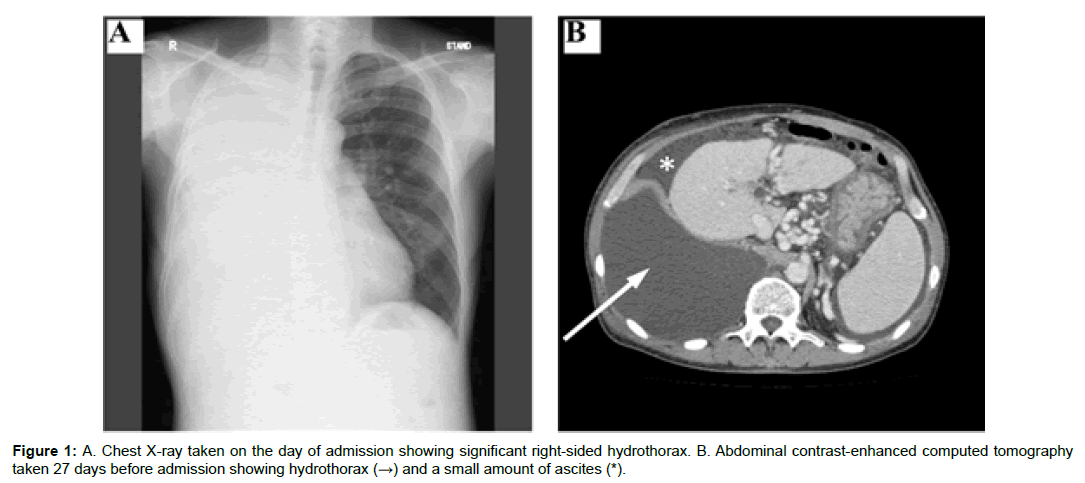
A 63-year-old man with alcoholic decompensated liver cirrhosis, Child-Pugh class C, and a Model for End-Stage Liver Disease score of 21, was admitted to our hospital. He had been drinking alcohol, approximately 1100 mL of distilled spirits (equal to 200 g ethanol) per day, for over 30 years. Seventeen months prior to hospitalization, the patient presented to a community hospital complaining of swelling in both lower legs. He had been treated several times for severe hepatic hydrothorax. On admission day (day 1), the patient had jaundice with icteric conjunctiva, decreased lung sounds in entire right side of the chest, and pitting edema in the bilateral lower legs without any sign of encephalopathy. Laboratory evaluation was notable for anemia with hemoglobin 12.7 g/dL, thrombocytopenia 58,000/mm3, prothrombin time-international normalized ratio 1.94, total protein 6.5 g/dL, albumin 1.6 g/dL, total bilirubin 5.6 mg/ dL, aspartate aminotransferase 47 IU/L, alanine aminotransferase 23 IU/L, and alkaline phosphatase 506 IU/L (Table 1). Further evaluation revealed a negative viral hepatitis panel and autoimmune panel. Viral infections such as CMV, HTLV-1, and HIV were ruled out. Initial infectious work-up with a throat swab, urine sample, and stool sample was negative. X-ray examination showed a remarkable right-sided hydrothorax. Abdominal contrast enhanced computed tomography (CT) demonstrated a cirrhotic liver with minimal ascites (Figure 1). On the next day (day 2), the patient had fever of 39.2°C. Blood cultures were performed, and ceftriaxone was administered as empiric therapy. He developed hypoxemia on day 2, and 900 mL of pleural fluid was aspirated. A Gram stain of the pleural effusion revealed Gram-negative rods with remarkable leukocytosis (23200/ μL, with segmented neutrophils of 95%), and the antibiotics were switched to ampicillin-sulbactam. In spite of the thoracentesis, on day 4, his dyspnea still remained, his tachypnea was aggravated, and his blood pressure had decreased. He was diagnosed with septic shock, and he was treated with meropenem, ciprofloxacin, catecholamines, and continuous hemodiafiltration in the intensive care unit. Hydrocortisone was also administered because of adrenal crisis. A catheter was placed in the right hemithorax for continuous drainage. There was not enough ascites detected by abdominal sonography to perform abdominocentesis. The blood and pleural effusion cultures were both positive for beta-lactamase-negative ampicillinresistant H. influenzae, for which meropenem and ciprofloxacin were administered. On day 8, chest CT detected pleural fluid with hematoma in the right lower hemithorax. Thoracoscopic debridement and pleural irrigation were performed. After the surgery, the sedative drug was discontinued, but his comatose status persisted. Head CT and magnetic resonance imaging revealed no significant intracranial hemorrhage or cerebral edema. In spite of intensive care for septic shock, his comatose status and liver failure had not improved, and on day 21, the patient died of multiorgan failure.
| Hematology | Blood chemistry | |||
|---|---|---|---|---|
| WBC | 8300/µl | TP | 6.5 | g/dl |
| Neutrophils | 78% | ALB | 1.6 | g/dl |
| Eosinophils | 8% | T.bil | 5.6 | mg/dl |
| Lymphocytes | 9% | AST | 47 | IU/l |
| RBC | 365/µl | ALT | 23 | IU/l |
| Hemoglobin | 12.7 g/dl | GGT | 43 | IU/l |
| Hematocrit | 36.8% | ALP | 506 | IU/l |
| Platelets | 58000/µl | LDH | 238 | IU/l |
| Coagulation | ChE | 63 | IU/l | |
| PT | 37% | Na | 139 | mEq/l |
| PT-INR | 1.94 | K | 4.1 | mEq/l |
| APTT | 70.3 s | Cl | 103 | mEq/l |
| Viral marker | BUN | 19 | mg/dl | |
| HBsAg | (-) | Cre | 1.12 | mg/dl |
| HBsAb | (-) | NH3 | 59 | µg/dl |
| HBcAb | (-) | Type 4 collagen | 344 | ng/ml |
| HCVAb | (-) | Hyaluronic acid | 3920 | ng/ml |
| HIVAb | (-) | HGF | 0.74 | ng/ml |
| Tumor marker | ß-D glucan | 8.4 | pg/ml | |
| AFP | 3.2 ng/ml | CRP | 0.71 | mg/dl |
| DCP | 1367 mAU/ml |
Table 1: Laboratory evaluation.
Discussion
Hepatic hydrothorax is defined as the presence of pleural fluid (usually greater than 500 mL) in a patient with cirrhosis in the absence of primary cardiac or pulmonary disease [5-7]. Hepatic hydrothorax occurs approximately 6–13% of patients with advanced cirrhosis and is often associated with alcoholic liver cirrhosis [8-10]. Patients with cirrhosis and hepatic hydrothorax are prone to spontaneous infection of pleural fluid [1,11]. In general, cirrhosis is an immunocompromised state that increases a patient’s susceptibility to the development of spontaneous bacterial infections and a variety of infections from uncommon pathogens [12,13]. SBEM is defined as infection of a preexisting hydrothorax in a patient with cirrhosis [1,11]. A diagnosis of SBEM is established if the pleural fluid cultures are positive and a polymorphonuclear count is >250 cells/μL. The patient in this case report met both these criteria [11]. Low pleural fluid opsonic activity and C3 levels are found in patients with cirrhosis, who are at high risk of SBEM [14]. In our case, the route of H. influenzae to the pleural fluid was uncertain; it was not clear whether it was from the respiratory tract or the gastrointestinal tract. Regarding liver cirrhosis, the major causative organisms of all bacterial infections are Gram-negative bacteria, while Gram-positive bacteria comprise about 20% and anaerobic bacteria only 3% [12]. A recent study reveals that Gram-positive cocci such as Staphylococcus, Enterococcus, and multi-resistant bacteria have become common pathogens [15]. Therefore, the etiology of bacterial infections in liver cirrhosis can be not only gastrointestinal tract sources but could also arise from other organs. The pathogenesis of SBEM, SBP, and spontaneous bacteremia is considered to be similar; they share the same types of common pathogens [16]. In our case, we could not rule out complications of SBP, as the patient’s ascites was too small to evaluate. However, SBEM can occur either with SBP (transdiaphragmatic spread) or without SBP (hematogenous spread) [16]. Therefore, it might be possible that bacteremia by H. influenzae results in SBEM. In previous reports, major causative microorganisms of SBEM were E. coli, Streptococcus species, Enterococcus species, and Klebsiella pneumonia [1,11]. These bacteria have been thought to originate from the gastrointestinal tract or to be systemic in origin [3]. Although H. influenzae is thought to be an indigenous microorganism in the respiratory tract, to our knowledge, there are no case reports of H. influenzae as a causative bacterium of SBEM [3]. Several reports reveal that H. influenzae is an indigenous bacterium in the human gastrointestinal tract [17- 19]. This fact might support that SBEM in this case occurred by the same pathway as the other major SBEM source. SBEM without ascites has been previously reported, and the pathogenic bacteria were E. coli, Pseudomonas stutzeri, and Enterococcus faecium [1]. If we take into account that H. influenzae is an indigenous bacterium of the intraperitoneal cavity, our case may support the hypothesis that enteric microorganisms reach the pleural fluid through bacteremia [1]. SBEM has a high recurrence rate (25-30%) and a poor prognosis [1]. For example, Xiol et al. reported that SBEM was fatal in 6 out of 16 cases [10]. Although SBEM is a rare common complication of liver cirrhosis, physicians should consider not only spontaneous bacterial peritonitis but also SBEM when a patient with cirrhosis and hydrothorax presents with infective symptoms such as fever and dyspnea. Moreover, these patients need to be intensively cared for because of their impaired immune systems, as they can very easily develop septic shock. In conclusion, we encountered a rare case of SBEM caused by H. influenzae. Our case suggests that it is essential to investigate the pathogenesis of hepatic hydrothorax in patients with cirrhosis as well as to offer systemic management and care for bacterial infections.
Acknowledgements
The authors do not have any disclosures to report.
References
- Xiol X, Castellvi JM, Guardiola J, Sese E, Castellote J, et al. (1996) Spontaneous bacterial empyema in cirrhotic patients: a prospective study. Hepatology 23: 719-723.
- Chen CH, Shih CM, Chou JW, Liu YH, Hang LW, et al. (2011) Outcome predictors of cirrhotic patients with spontaneous bacterial empyema. Liver Int 31: 417-424.
- Musher DM, Nichol AC, Rueda AM (2006) Nontypeable Haemophilus influenzae as a cause of spontaneous bacterial peritonitis. J Clin Microbiol 44: 2304-2306.
- Saadi T, Khoury S, Veitsman E, Baruch Y, Raz-Pasteur A (2013) Spontaneous bacterial peritonitis with a very high leukocyte count in ascitic fluid caused by Haemophilus influenzae. Int J Gen Med 6: 689-691.
- Kiafar C, Gilani N (2008) Hepatic hydrothorax: current concepts of pathophysiology and treatment options. Ann Hepatol 7: 313-320.
- Strauss RM, Boyer TD (1997) Hepatic hydrothorax. Semin Liver Dis 17: 227-232.
- Morrow CS, Kantor M, Armen RN (1958) Hepatic hydrothorax. Ann Intern Med 49: 193-203.
- Alberts WM, Salem AJ, Solomon DA, Boyce G (1991) Hepatic hydrothorax: Cause and management. Arch Intern Med 151: 2383-2388.
- Lazaridis KN, Frank JW, Krowka MJ, Kamath PS (1999) Hepatic hydrothorax: pathogenesis, diagnosis, and management. Am J Med 107: 262-267.
- Xiol X, Guardiola J (1998) Hepatic hydrothorax. Curr Opin Pulm Med 4: 239-242.
- Xiol X, Castellote J, Baliellas C, Ariza J, Gimenez RA, et al. (1990) Spontaneous bacterial empyema in cirrhotic patients: analysis of eleven cases. Hepatology 11: 365-370.
- Bunchorntavakul C, Chamroonkul N, Chavalitdhamrong D (2016) Bacterial infections in cirrhosis: a critical review and practical guidance. World J Hepatol 8: 307-321.
- Tandon P, Garcia-Tsao G (2008) Bacterial infections, sepsis, and multiorgan failure in cirrhosis. Semin Liver Dis 28: 26-42.
- Sese E, Xiol X, Castellote J, Rodriguez-Farinas E, Tremosa G (2003) Low complement levels and opsonic activity in hepatic hydrothorax: its relationship with spontaneous bacterial empyema. J Clin Gastroenterol 36: 75-77.
- Dever JB, Sheikh MY (2015) Review article: spontaneous bacterial peritonitis--bacteriology, diagnosis, treatment, risk factors and prevention. Aliment Pharmacol Ther 41: 1116-1131.
- Bunchorntavakul C, Chavalitdhamrong D (2012) Bacterial infections other than spontaneous bacterial peritonitis in cirrhosis. World J Hepatol 4: 158-168.
- Rajilić-Stojanović M, De Vos WM (2014) The first 1000 cultured species of the human gastrointestinal microbiota. FEMS Microbiol Rev 38: 996-1047.
- Justesen T, Nielsen OH, Hjelt K, Krasilnikoff PA (1984) Normal cultivable microflora in upper jejunal fluid in children without gastrointestinal disorders. J Pediatr Gastroenterol Nutr 3: 683-686.
- Ou G, Hedberg M, Horstedt P, Baranov V, Forsberg G, et al. (2009) Proximal small intestinal microbiota and identification of rod-shaped bacteria associated with childhood celiac disease. Am J Gastroenterol 104: 3058-3067.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi