Review Article, Int J Ophthalmic Pathol Vol: 7 Issue: 3
Subthreshold Micropulse Yellow Laser Treatment for Central Serous Chorioretinopathy
Aseel Hamoud1* and Saad Younis2
1Department of Ophthalmology Maidstone Hospital, Maidstone and Tunbridge Wells NHS Trust UK, Maidstone ME16 9QQ, United Kingdom
2Medical Retina Department, Western Eye Hospital-Imperial College Healthcare NHS Trust UK, Maidstone ME16 9QQ, United Kingdom
*Corresponding Author : Hamoud Aseel
FRCS Glasg, Department of Ophthalmology Maidstone Hospital, Maidstone and Tunbridge Wells NHS Trust UK, Maidstone ME16 9QQ, United Kingdom
Tel: +447470185991
E-mail: aseelhamoud@yahoo.com
Received: August 08, 2018 Accepted: September 29, 2018 Published: October 05, 2018
Citation: Hamoud A and Younis S (2018) Subthreshold Micropulse Yellow Laser Treatment for Central Serous Chorioretinopathy. Int J Ophthalmic Pathol 7:3. doi: 10.4172/2324-8599.1000223
Abstract
CSR is characterized by avascular focal leakage from the choriocapillaris through the retinal pigment epithelium (RPE), resulting in serous detachment of the neurosensory retina. It is usually self-limiting; in a small minority of cases chronic CSR may develop with the potential for progressive RPE atrophy and permanent visual loss. Treatment is challenging as focal laser can cause scarring and visual loss. Photodynamic therapy is not always effective. The Supra 577TM nm yellow micro pulse laser (Quantel medical) has been recently used for chronic CSR treatment. It is highly selective localizing the effect on the RPE, whilst sparing the fovea. The purpose of our study is to assess the efficacy and safety of the Supra 577TM MicroPulse (MP) laser treatment in cases of chronic and chronic recurrent central serous chorioretinopathy (cCSR) (rCSR). The aim was to document and measure the changes in the central retinal thickness (CRT) and best corrected visual acuity (BCVA) and the integrity of the fovea in a short period of time after treatment.
Keywords: Chorioretinopathy; Choriocapillaris; Subthreshold micropluse yellow laser treatment; Chronic central serous chorioretinopathy (CSCR)
Introduction
Chronic central serous chorioretinopathy (CSCR) is a posterior segment disease characterized by localized fluid accumulation underneath the neuro-retina. This can cause irreversible visual loss due to progressive and permanent photoreceptor damage and/or Retinal Pigment Epithelial (RPE) atrophy. The complex and multifactorial pathogenesis of CSCR is still uncertain and the effective treatment for CSCR is still unknown. Sub threshold micropulse yellow laser technology controls thermal elevation by cutting a continuous-wave beam into repetitive short pulses have been recently used to treat CSCR and have shown some efficacy in CSCR patients with subfoveal and extrafoveal leakage sites. Our research aims to assess the response and safety of subthreshold laser 577-nm treatment in patients with CSCR.
Case Report
We performed a retrospective observational review of the clinical notes of 11 eyes of 11 patients. Diagnosed usually made using OCT scan only. Treatment was applied with one session of an OCT-guided yellow laser. We apply the shots to leakage areas highlighted with the OCT scan [1]. We used the ‘Quantel Medical, Supra scan 577 nm laser’ for their macular condition. Patients received subthreshold micropulse yellow laser photocoagulation at 5% duty cycle at a reduced energy level from the micropulse laser test burns, to obtain this level of laser energy: we apply few laser burns to a peripheral retinal area, once we notice any retinal burn we stop. We then use half of that energy power to treat the leakage areas previously noticed with the OCT scan. Laser exposure time (duration) was 20 milliseconds, and the spot diameter was 160 microns. Inclusion criteria was CSCR suffered for minimum 6 months, no previous treatment for this condition, loss of vision and subretinal fluid secondary to CSCR when the treatment was performed. The evidence collected from the medical notes included: age, gender, laterality, duration of the CSCR, best corrected visual acuity (BCVA) pre and post treatment, central macular thickness (CMT) pre and post treatment, and retinal changes post-treatment.
The measurements were taken 6 weeks after treatment. Cirrus HDOCT scan or Heidelberg-OCT scan were used, fundus autofluorescence (FAF) and fundal colour photos were taken (Table 1) [2].
| Age | Gender | Laterality of the affected eye | Use of steroid |
|---|---|---|---|
| 54 | Male | Left | No |
| 41 | Male | Right | No |
| 61 | Male | Right | No |
| 39 | Male | Left | Yes |
| 53 | Female | Left | No |
| 35 | Male | Right | Yes |
| 48 | Male | Right | No |
| 45 | Male | Right | No |
| 53 | Male | Right | No |
| 77 | Male | Left | Yes |
| 54 | Male | Right | No |
Table 1: Table showing criteria of the patients’ sample.
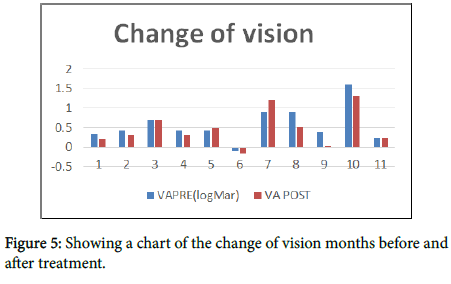
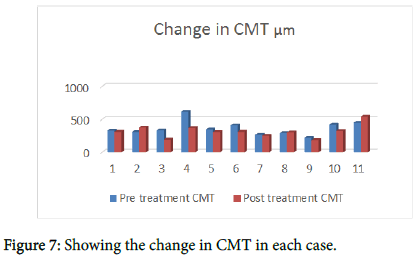
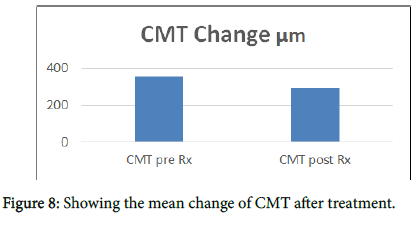
The Mean age of patients is 47 years (range 35-54). The mean duration of the CSCR was 26 months (range 9-52). Two thirds of the patients responded to treatment, improving the macula profile and reducing the subretinal fluid. The mean central macular thickness CMT measured by OCT pre-treatment changed from 364 +/-84 μm to 279 +/-67 μm post treatment (P<0.03), showing a 24% average reduction in fluid height. There was no evidence of RPE or retinal damage on SD-OCT and fundal florescent angiography. Never the less, three patients showed changes in the RPE with FAF. The BCVA changed from 0.35 +/-0.27 LogMAR pre-treatment to 0.33 +/-0.31 (p value is not significant, P<0.8).
Case 1
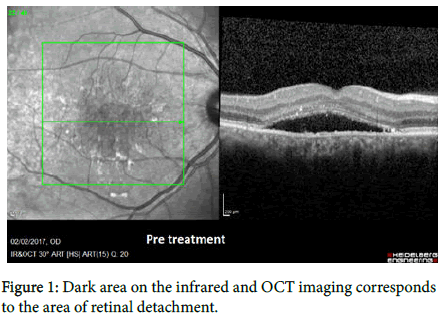
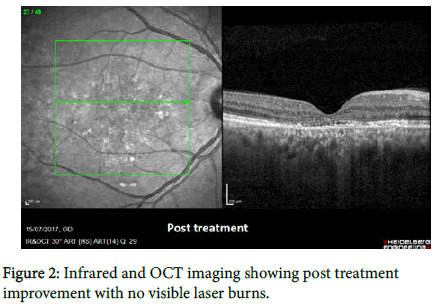
A 36-year-old male physician presented with reduced vision in the right eye over the previous 3 years. BCVA was 6/30 (0.7 logMAR) in the right eye and 6/6 in the left eye. Fundus exam showed a foveal retinal detachment and leakage near the fovea in the right eye (Figure 1). The patient was treated with 577-nm yellow laser, with a 0.2 msec pulse duration (400 mW), 200 μm spot size and 5% duty cycle. Fifteen shots were delivered to the centre of the macula, around the fovea over the location of the detachment. We followed the patient up for 5 months, although there was no improvement of his vision but anatomically the retina was flat again with a reduction of CMT from 332 to 193 after the period of follow-up. We could see subtle but definite improvement in the FAF (Figure 2). FFA shows that the leakage has resolved with no visible laser burns. Such rapid anatomic improvement after 5 months of treatment is remarkable (Table 2).
| Pre-treatment BCVA (logMar) | post-treatment BCVA | Pre-treatment CMT (μm) | Post-treatment CMT (μm) | Duration of the CSR | Number of MP laser shots | Notes |
|---|---|---|---|---|---|---|
| 0.32 | 0.2 | 329 | 312 | 52 months | 18 | |
| 0.44 | 0.3 | 309 | 375 | unknown | 26 | |
| 0.7 | 0.7 | 332 | 193 | 36 months | 15 | No visual improvement |
| 0.44 | 0.3 | 615 | 369 | unknown | 72 | |
| 0.44 | 0.5 | 346 | 308 | 3 years | 14 | Had laser twice |
| -0.1 | -0.16 | 411 | 312 | 4 years | 25 | |
| 0.9 | 1.2 | 265 | 250 | 3 years | 213 | Get dry then get fluid after 6/12 |
| 0.9 | 0.52 | 293 | 303 | 3 years | 18 | Amblyopic eye |
| 0.4 | 0.02 | 220 | 185 | 9 months | unknown | |
| 1.6 | 1.3 | 420 | 325 | 6 months | unknown | |
| 0.22 | 0.22 | 450 | 544 | 12 months | 35 | No response |
Table 2: Table showing patients’ characteristics.
Case 2
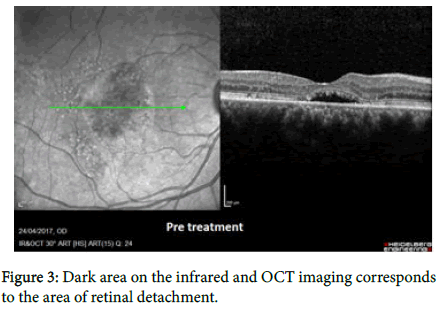
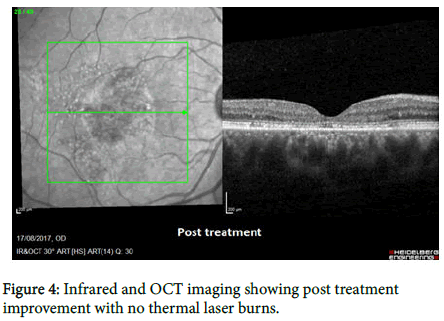
A 45-year-old male with a history of 3 years CSCR in the right eye, 2 courses of oral Spironolactone 50 mg were tried with no improvement in his vision. BCVA was 6/48 (0.9 logMAR) in his right eye, 6/6 in the left eye. Fundal exam showed a macular detachment (Figure 3). We decided to treat the patient with micropulse laser 0.2 msec pulse duration, 350 mW power, 100 μm spot size and 5% duty cycle. 18 laser shots were given. The BCVA improved to 6/19 (0.52 logMAR) three weeks after treatment. His FAF and OCT scan results are shown in (Figure 4).
Discussion
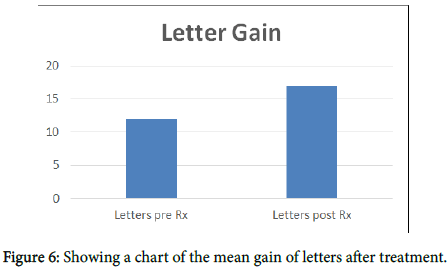
Studies compared the efficacy and safety of micropulse laser in treating CSCR with either photodynamic therapy (PDT) or with no treatment. Scholz in 2017 stated that micopulse laser was superior to PDT and no treatment. The decrease in CMT was highest with micropulse laser (-131 μm) as compared with PDT (-85 μm) or no treatment (-25 μm). 64% of patients treated with micropulse laser showed no fluid after treatment, 46% of the patients treated with PDT showed no fluid after treatment and only 8% of patients who got no treatment showed no fluid in their maculae. Micopulse pulse laser treatment had no side effects on the eyes treated, and was best effective if the site of leakage recognized with no atrophy of the RPE. There are few studies that discuss treating CSCR with the micropluse laser [3-5]. In 2010 Andre Maia conducted a series of case study of treating CSCR with the yellow 577 nm micropulse laser, he had 3 cases all from Brazil, they were all successfully treated with no retinal damage, some of them needed repeated treatment, but no major side effects were experienced. In our study, we proved that micropulpse laser is an effective Way of treating CSCR, although some of the cases didn’t have complete visual recovery, that probably due to the chronic nature of their disease with permanent damage to the photoreceptors (Figures 5-8).
Conclusion
Sub threshold micropluse yellow laser photocoagulation is a safe and effective treatment option for chronic CSCR. There was no evidence of retinal damage noticed with FAF and OCT after the treatment. The BCVA did not improve significantly and this likely to be because of the chronic nature of the disease in our patients. We may try this treatment with acute CSCR, and in such cases we would expect better results. Future research with larger samples and a longer period of time for treatment is required.
Conflict of Interest
We have no financial interest that may influence our interpretation of the results.
References
- André Maia (2010) A new treatment for chronic central serous retinopathy. Retina Today 2010.
- Scholz P, Altay L, Fauser S (2017) A review of subthreshold micropulse laser for treatment of macular disorders. Ophthalmologica 34: 1528-1555.
- Scholz P, Ersoy L, Boon CJ, Fauser S (2015) Subthreshold micropulse laser (577 nm) treatment in chronic central serous chorioretinopathy. Ophthalmologica 234: 189-194.
- Yadav NK, Jayadev C, Mohan A, Vijayan P, Battu R, et al. (2015) Subthreshold micropulse yellow laser (577 nm) in chronic central serous chorioretinopathy: Safety profile and treatment outcome. Eye 29: 258-265.
- Su D, Hubschman JP (2017) A review of subthreshold micropulse laser and recent advances in retinal laser technology. Ophthalmol Ther 6: 1-6.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi