Research Article, J Spine Neurosurg Vol: 8 Issue: 3
Surgical Approach to Access as Transciliar Resection for Anterior Cranial Fossa Meningiomas
Álvarez-Vázquez L1*, Vazquez-Nieves Jr4, Santos-Benitez H3, Rangel-Morales C2 and Vallejo-Moncada C2
1Neurosurgery Service, Hospital Hgr 220, Imss, Toluca, State of Mexico
2Neurosurgery Service, La Raza National Medical Center, Dr. Antonio Fraga Mouret, Mexico
3Unit of Neurosurgery and Spinal Surgery, Hospital Ruber, Madrid, Spain
4Neurosurgery Service, Adolfo López Mateos Medical Center, Toluca, State of Mexico
*Corresponding Author : Leonardo Alvarez Vazquez Toluca, CP 50160, State of México Tel: 722 217 0108 E-mail:lejamajm_729@hotmail.com
Received: January 28, 2019 Accepted: February 06, 2019 Published:February 13, 2019
Citation: Álvarez-Vázquez L, Vazquez- Nieves Jr, Santos- Benitez H, Rangel-Morales C, Vallejo- Moncada C (2019) Surgical Approach to Access as Transciliar Resection for Anterior Cranial Fossa Meningiomas. J Spine Neurosurg 8:1.
Abstract
Introduction: Meningiomas are meningothelial tumors originating from arachnoid cells, which are more frequent in the fifth and sixth decade of life, represent 30% of intracranial tumors. Multiple approaches have been described and developed for the resection of lesions of which the transciliary approach offers an adequate visualization of the anterior cranial fossa, of sellar, parasellar and suprasellar structures, with satisfactory resection results. Material and Method: Three cases of patients with a diagnosis of meningioma of the anterior cranial fossa were submitted to complete resection using a transciliary approach, plus repair technique with autologous bone graft and pericranial pedicle flap rotation to improve results aesthetics. Results: Two male patients (38 and 56 years) and a female of 52 years of age, with no relevant history, presented a history of chronic headache; in the two men with alteration in the campimetry, the resecction was performed using the technique described without complications and with good aesthetic results at 12 months follow up in the three cases. Conclusion: The transciliary approach is a good option for the management of anterior cranial fossa pathologies, allowing adequate resection in the case of meningioma, with reduced bleeding, retraction and lesion to the olfactory nerve, as well as better cosmetic results with the technique employed and a considerable reduction of the inpatient stay.
Keywords: Meningioma; Transciliar approach; Anterior cranial fossa
Introduction
Minimally invasive approaches reduce surgical morbidity in addition to shortening the hospital stay. The supraorbital transciliar approach provides adequate visualization of the anterior cranial fossa and sellar, parasellar and suprasellar structures. This technique has been used with satisfactory results in the management of pituitary macroadenoma, aneurysms, meningiomas and craniopharyngiomas [1].
The common symptoms of suprasellar lesions and lesions of the anterior cranial fossa are increased intracranial pressure, endocrine dysfunction, visual disturbances or subarachnoid hemorrhage in the case of aneurysms [2].
The surgeon should consider the diagnosis, the size and extent of the lesion, the location, and its relationship to the craniotomy before performing this approach [2,3].
Materials and Methods
A prospective study was carried out on three patients with a diagnosis of meningioma of the anterior floor to whom resection was performed using a transciliary approach.
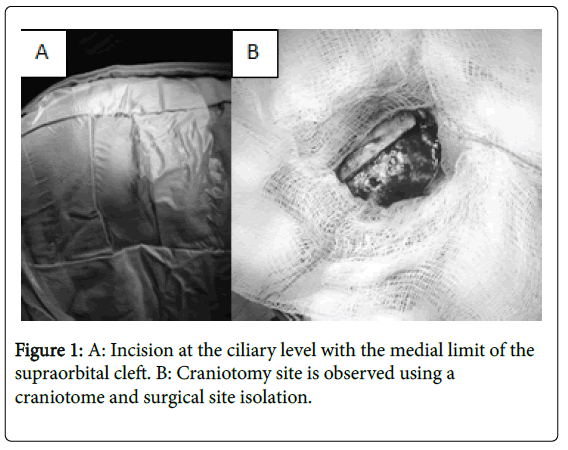
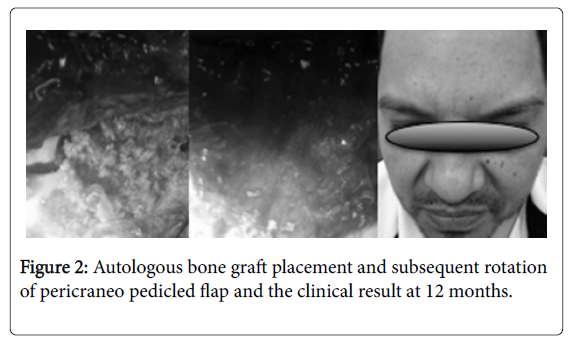
Surgical Technique: The skin incision was made along the upper edge of the eyebrow, ending at the level of the supraorbital recess, identifying and preserving the supraorbital nerve, continuing inside and up to the outer edge of the eyebrow. The pericranum on the frontal bone and the temporal fascia are exposed through a subcutaneous dissection. Silk sutures are used to retract the cutaneous flap. A Cshaped incision is made in the pericranium with its base at the orbital edge. This flap is continued with the periorbital, which rises from the orbital roof. The initial burr hole is performed in the pterion after the temporal muscle is detached. A supraorbital craniotomy is performed with craniotome, with dimensions of about 3.5cm width and 2.5cm high. Finally, the dura is open in curve sharpe [4-6] (Figure 1). After removing the lesion, the following repair and closure technique is performed: holes are made at the edges of the skull and the bony flap, fixed with polypropylene 3-0, the pericraneum pedicle flap is rotated to cover the edges of the craniotomy and finally facing the muscular and cutaneous planes (Figure 2).
Results
Case 1
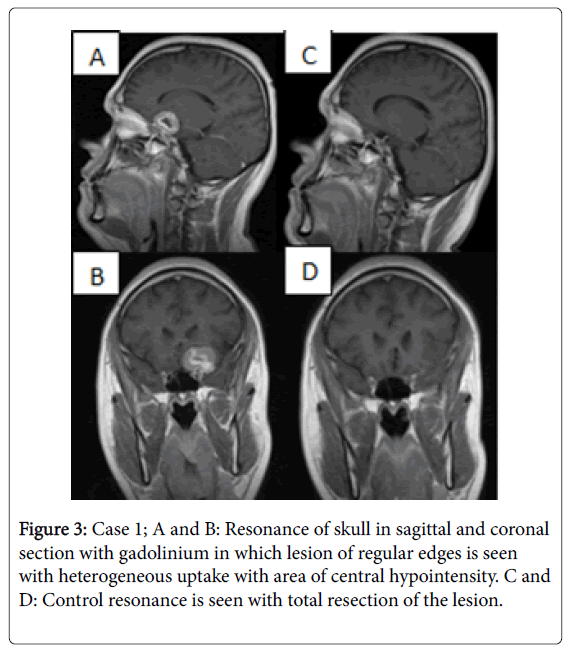
Male patient of 38 years of age, with no history of importance for his condition. Starts in 2011 with intermittent headache, generalized of puncture type which improves with common analgesics, exacerbation in January 2013 with an increase in intensity 9/10, nausea and vomiting, for which a tomography study was performed. Radiological findings are entered into our service to complete study protocol. Physical examination was patient oriented in the 3 spheres, mental functions conserved, with left temporal hemianopsia, normal fundus, without alterations of ocular movements. Clinoid meningioma resection is planned by transciliar approach. A transoperative finding of bleeding indurated lesion that is not very aspirable, with anterior clinoid implant compatible with meningioma, is completely resected. After surgery, patient was observed without complications. He leaves on the third postoperative day with control study without residual lesion, clinically with correction of visual deficit and without paresis for eyebrow lift (Figure 3).
Case 2
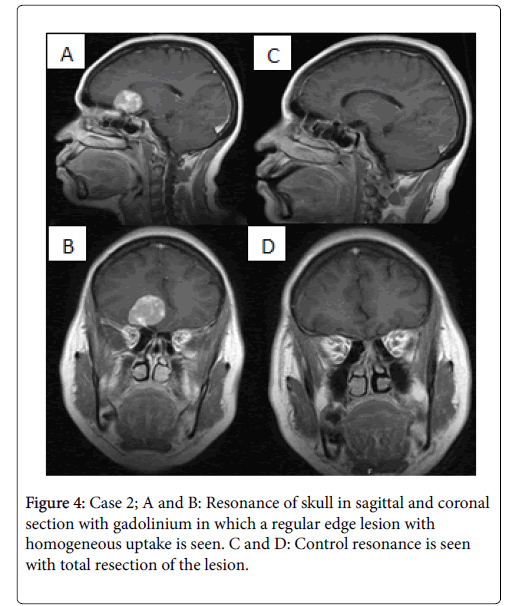
A 52-year-old female patient, history of systemic arterial hypertension under management with enalapril 10 mg every 12 hours. Began in 2009 with generalized occasional pulsed-type headache without irradiation, improve with analgesics. In March 2013 he presented a sudden loss of alertness, is taken to the emergency department of our unit where a tomography study is performed. With the findings of the CT we decided to enter our service to complement the MRI protocol. On physical examination the patient is oriented, preserved mental functions, right anosmia, papilledema ipsilateral, no alterations of eye movements, increased reflexes, present Babinski. Normal campimetry. Surgery is scheduled for resection of olfactory groove meningioma by transciliar approach with findings of an indurated, vascularized, little aspirable extraaxial lesion with a right olfactory groove implant compatible with meningioma, which is completely resected. After to a surgical event, the patient remained without complications and leaves on the third postoperative day with a control study at 6 months without residual lesión or paresis for elevation of the eyebrow (Figure 4).
Case 3
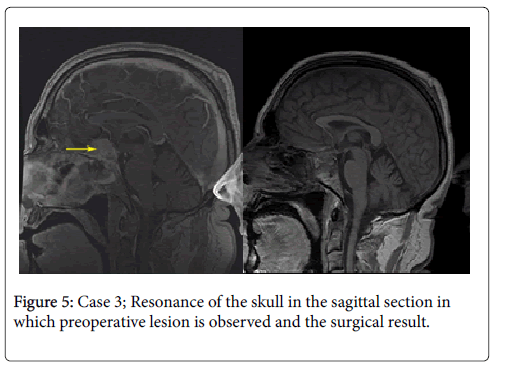
A 56-year-old male patient, history of hypertension and diabetes mellitus. Begins in 2012 with intermittent, generalized, puncture headache, visual deficit is added, so simple and contrasted tomography of head is performed. With radiological findings he entered into service to complete study protocol. A physical examination was found oriented in the 3 spheres, mental functions preserved, with bitemporal hemianopsia, normal fundus without alterations of ocular movements. He is programmed for resection of tuberculum sellar meningioma by transciliar approach. Transoperative finding of bleeding indurated lesion that is not aspirable, with implant in tuberculum sellar compatible with meningioma, is completely resected. Post-surgical patient presents with transient diabetes insipidus. He leaves the sixth postoperative day with control study without residual lesion, and adequate hormonal function. Clinically with correction of visual deficit and without paresis for elevation of the eyebrow (Figure 5).
Discussion
Introduced in 1908 by Krause [7], the supraorbital approach is part of the evolution of surgical approaches for pituitary tumors. McArthur (in 1912) and Frazier in 1913 reported that block removal of the supraorbital border with a portion of the orbital roof increased surgical exposure [8,9]. Other groups made slight modifications over the years, and for 1982, Jane and cols significantly improved the approach [10].
In 1978, Brock and Dietz led the development of minimally invasive approaches by introducing a small frontolateral approach with a curvilinear skin incision just behind the hairline that was smaller than that used in standard approaches [11]. In the early 1980s, Sánchez- Vázquez and Fukushima et al. [12] reported an incisión on the eyebrow that decreased the size of the supraorbital aperture.
Perneczky et al. have emphasized the advantages of microsurgical approaches, which eliminate the futility of major surgical exposures in conventional approaches [13].
Sánchez-Vázquez, reported 41 patients of whom 31 had pituitary adenomas, 2 patients had olfactory Groove meningiomas, 1 patient with a craniopharyngioma, 1 with aracnoid sellar, 6 patients had vascular lesions: an ophthalmic segment of internal carotid artery aneurysm, two posterior communicating artery aneurysms (PCoA), and 3 anterior communicating artery aneurysms (ACoA) who underwent a modified transciliary approach were observed for 3 months reporting 21 patients with hyposmia, 41 patients with decreased sensitivity in frontal region that persisted in 5 cases at 3 months and difficulty raising the eyebrow in the 41 patients however at 3 months all had an adequate elevation, no mortality reported in said series.
Patrick [14], reports 56 clipped aneurysms in 47 patients. Six patients presented with acute subarachnoid hemorrhage (SAH), bilateral supraorbital craniotomies were performed in 3 patients. Six patients with multiple aneurysms were treated by craniotomy. All aneurysms were visualized well under a microscope. Endoscopic assistance was not considered necessary. All were successfully clipped. In two cases there was a transoperative rupture. There was no direct mortality from surgery. One patient died later from bleeding from a ruptured posterior circulation aneurysm. One patient had a significant long-term deficit, but remained independent. There was no deficit for brow lift with adequate cosmetic results.
Prat-Acín [15] reports 6 patients with high-grade glioma who underwent a transciliary approach with supraorbital craniotomy: 3 patients with lesions in the rectus gyrus, 2 patients with lesions at the mid of the medial orbital gyrus and 1 patient in anterior portion of the orbital gyrus. The lesion was completely resected in 5 patients, 1 case of surgical site infection without subsequent complications, in the 6 cases a satisfactory cosmetic result was presented without deficit for eyebrow lift.
Jallo and Bognár [16] define the following: advantages: 1) shorter surgical procedure and less risk of injury to the neurovascular structures that irrigate/innervate the temporal muscle. 2) The incision of the supraciliar skin is hidden by the eyebrow and is cosmetically acceptable by the patients. There is minimal risk of alopecia or "double eye" image. 3) The craniotomy requires only a burr hole, which is covered by the temporal muscle, thus minimizing the poor cosmetic appearance. 4) Brain retraction is minimized when the opening includes the orbital roof. Disadvantages 1) The most important limitation of this approach is that it can never be a standard approach for all types of lesions. 2) The craniotomy should be evaluated for each specific tumor or type of vascular pathology to ensure that the target is reached by this small craniotomy approach. 3) The small size of the craniotomy could limit the view of the microscope. Some surgeons suggest osteotomy of the orbital roof to increase exposure. However, endoscopic surgery improves the surgical sight. 4) The craniotomy could penetrate the frontal sinus. This should be repaired before closing to avoid the risk of rhinorrhea and subsequent infection.
In comparison, the counterpart of this approach, (the pterional approach), however, is not without disadvantages. It requires a complete dissection of the temporalis muscle together with the presence of atrophy of the same and alterations in chewing; also frequently exposes large areas of the cortex unnecessarily. Poor results are common and this can be attributed to atrophy of temporal muscle and superficial fat or to injury of the frontal branch of the facial nerve [17].Whose alterations can be avoided by the transciliar approach.
Conclusion
The supraorbital transciliary approach allows a minimally invasive craniotomy in selected cases, with acceptable esthetic results for the patient, entails lower risks and post-operative sequelae, providing an excellent exposure of the anterior cranial fossa and thus the possibility of adequate resection of lesions in this region. However, it can not be used in all pathologies, so an adequate choice of case must be made, and the neurosurgeon's experience and ability to reduce morbidity and mortality are very important.
References
- Reisch R, Perneczky A (2005) Ten-year experience with the supraorbital sub-frontal approach through an eyebrow skin incision. Neurosurgery 57: 242-255.
- Ko Y, Yi H, Kim Y, Oh S, Kim K (2001) Eyebrow incision using tattoo for anterior fossa lesions: technical case reports. Minim Invasive Neurosurg 44: 17-20.
- Lee Warren W, Grant Gerald A (2009) Transciliary orbitofrontozygomatic approach to lesions of the anterior cranial fossa. Neurosurgery 64: 324-330.
- Van Lindert E, Perneczky A, Fries G, Pierangeli E (1998) The supraorbital keyhole approach to supratentorial aneurysms: concept and technique. Surg Neurol 49: 481-490.
- Reisch R, Perneczky A (2005) Ten-year experience with the supraorbital subfrontal approach through an eyebrow skin incision. Neurosurgery 57: 242-255.
- Sánchez-Vázquez MA, Barrera-Calatayud P, Mejia-Villela M, Palma-Silva JF, Juan-Carachure I, et al. (1999) Transciliary subfrontal craniotomy for anterior skull base lesions. Technical note. J Neurosurg 91: 892-896.
- Krause F (1908) Chirurgie des Gehirns und Rückenmarks nach eigenen Erfahrungen. Berlin: Urban & Schwarzenberg, Germany.
- McArthur LL (1912) An aseptic surgical access to the pituitary body and its neighborhood. J Am Med Assoc 58: 2009-2011.
- Frazier CH (1913) An approach to the hypophysis through the anterior cranial fossa. Ann Surg 57: 145-150.
- Jane JA, Park TS, Pobereskin LH, Winn HR, Butler AB (1982) The supraorbital approach: technical note. Neurosurgery 11: 537-542.
- Brock M, Dietz H (1978) The small frontolateral approach for the microsurgical treatment of intracranial aneurysms. Neurochirurgia 21: 185-191.
- Fukushima T, Miyazaki S, Takusagawa Y, Reichman M (1991) Unilateral interhemispheric keyhole approach for anterior cerebral artery aneurysms. Acta Neurochir Suppl 53: 42-47.
- Fries G, Perneczky A, van Lindert E, Bahadori-Mortasawi F (1997) Contralateral and ipsilateral microsurgical approaches to cartotid-ophthalmic aneurysms. Neurosurgery 41: 333-343.
- Patrick M, Vindlacheruvu R, Mahmood K, Ashpole R, Grivas A, et al. (2005) Supraorbital eyebrow minicraniotomy for anterior circulation aneurysms. Surgical Neurology 63: 47-51.
- Prat-Acín R, Galeano-Senabre I, Pancucci G, Evangelista R (2013) Supraorbital trans-eyebrow craniotomy and fluorescence-guided resection of fronto-basal high grade gliomas. Clinical Neurology and Neurosurgery 115: 1586-1590.
- Jallo G, Bognár L (2006) Eyebrow surgery: the supraciliary craniotomy: technical note. Neurosurgery 59: 157-158.
- Figueiredo EG, Deshmukh P, Nakaji P, Crusius MU, Crawford N, et al. (2007) The minipterional craniotomy: thechnical description and anatomic assessment. Neurosurgery 61: 256-265.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi