Case Report, J Spine Neurosurg Vol: 7 Issue: 3
The Clinical Outcomes Of Patients With L1-L2 Disc Herniation Treated By Microsurgical Trans Facet Approach
Sharifi G1, Rahimzadeh A2*, Fereydonyan N3, Divanbeigi A4, Kasbkar H4, Ebrahimzadeh K1, Amiri S4 and Rezaei O1
1Department of Neurosurgery, Loghman Hakim Hospital, School of Medicine, Shahid Beheshti University of Medical Sciences, Tehran, Iran
2Department of Neurosurgery, Pars Hospital, Pars Advanced and Minimally Invasive Medical Manners Research Center, Affiliated to Iran University of Medical sciences, Tehran, Iran
3Department of Neurosurgery, Hazrat-e Rasool General Hospital, Iran University of Medical Sciences, Tehran, Iran
4Scientific Research Committee, Department of Neurosurgery, Loghman Hakim Hospital, Shahid Beheshti University of Medical Sciences, Tehran, Iran
*Corresponding Author : Abolfazl Rahimizadeh
Department of Neurosurgery, Pars Hospital, Pars Advanced and Minimally Invasive Medical Manners Research Center, Affiliated to Iran University of Medical sciences, Tehran, Iran
Tel: +98-9123226149
E-mail: a_rahimizadeh@hotmail.com
Received: July 05, 2018 Accepted: July 24, 2018 Published: July 31, 2018
Citation: Sharifi G, Rahimzadeh A, Fereydonyan N, Divanbeigi A, Kasbkar H, et al. (2018) The Clinical Outcomes of Patients with L1-L2 Disc Herniation Treated by Microsurgical Trans Facet Approach. J Spine Neurosurg 7:3. doi: 10.4172/2325-9701.1000302
Abstract
Background: In comparison to lower lumbar disc herniation, L1-L2 disc herniation has unique characteristics, which cause controversy in selection of surgical approach. The goal of this study was to evaluate the clinical outcomes for treatment of L1-L2 disc herniation by microsurgical transforaminal lumbar interbody fusion (TLIF) technique. Therefore, 37 symptomatic patients of L1-L2 disc herniation who were treated by TLIF, from 2008 to 2016, in three academic hospitals were reviewed retrospectively. Follow-up of these patients should significant clinical improvement following TLIF surgery (p-value <0.001) and acceptable bony union with respect to the results, we concluded that TLIF can be an effective, reproducible and safe technique for surgical treatment of L1-L2 disc herniation.
Keywords: L1-L2 disc herniation; Upper lumbar; Transforaminal lumbar interbody fusion; Microsurgery
Abbreviations
VAS: Visual Analogue Scale; ODI: Oswestry Disability Index; MIS-TILF: Minimally Invasive Transforaminal Lumbar Interbody Fusion; TLIF: Transforaminal lumbar Interbody fusion.
Introduction
Despite several studies published regarding the treatment of upper lumbar disc herniation, there is still controversy in selection of tailored surgical approach because of unique characteristics of these levels [1-4]. The incidence of disc herniation at upper lumbar levels including L1-L2, L2-L3 and L3-L4 is approximately 5% of all disc herniation’s [5-8]. Considering that 70% to 83% of these herniations are at L3-L4 level. Incidence of L1-L2 and L2-L3 disc herniation is close to 1% to 2% of all lumbar herniated discs [9-11]. Some of the previous studies about surgical treatment of upper lumbar disc herniation defined these levels as T12-L1 to L2-L3, beside other studies have reported them as L1-L2 and L2-L3 levels [2,8,12,13]. The posterior approach is the conventional transforaminal approach for these level, but there are others as well, such as Trans Dural, oblique Para spinal, anterolateral, and minimally invasive transforaminal interbody fusion surgery (MIS-TLIF). Although these approaches have some advantages, they might be associated with some complications and limitations [3-5,7,11]. In this retrospective study, the aim is to present and evaluate the clinical outcomes of patients with L1-L2 disc herniation treated by microsurgical transforaminal approach. According to a vast review of literature, there is no specific section focusing on surgical treatment of pure L1-L2 disc herniation and no exclusive study has been performed concerning this level alone.
Materials and methods
Subjects
Between 2011 and 2016, 37 patients underwent surgery for symptomatic disc herniation at L1-L2 level via microscopic transforaminal approach at three academic hospitals of Shahid Beheshti University of Medical Sciences and Iran University Medical Sciences in Tehran. These patients presented with back pain, radiating leg pain and neurological (motor and sensory) deficits. All patients were followed up for a mean period of 18.6 months (range 12-26 months) after the surgery. Inclusion criteria were symptomatic patients with disc herniation at the L1-L2 level who were recalcitrant to conservative treatment. Cases with one or more herniated discs at an adjacent segment to L1-L2 were excluded. All included patients were followed up for at least 12 months. The diagnosis of disc herniation was confirmed by an independent radiologist based on MRI and CT scan.
Surgical approach
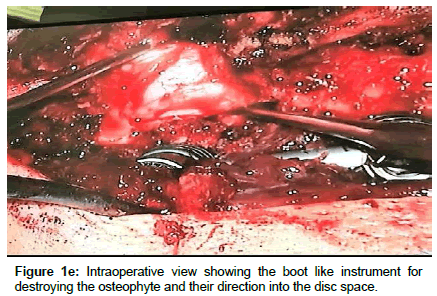
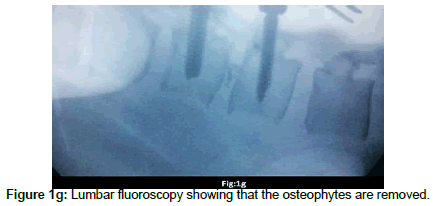
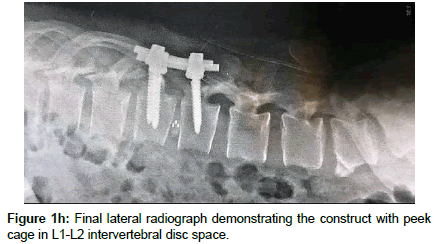
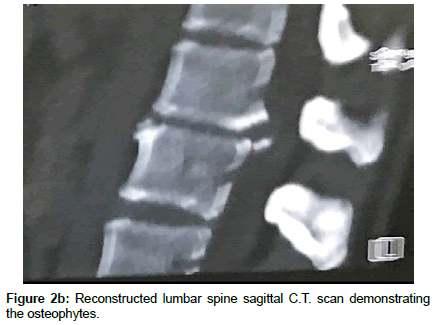
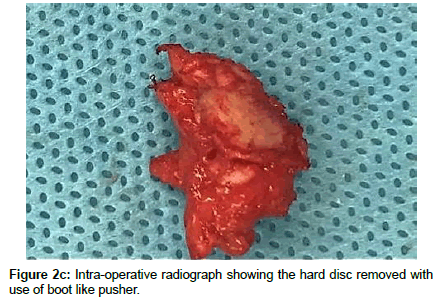
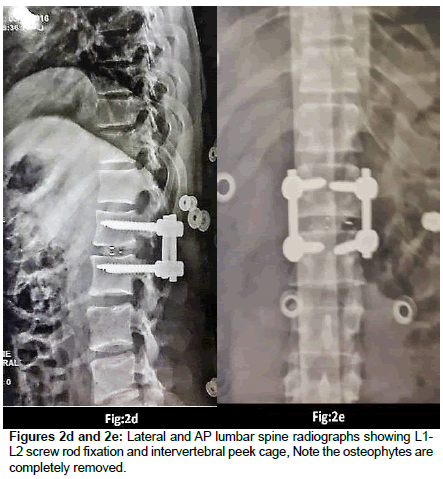
Microscopic transforaminal approach was used for all patients. Patients were positioned prone. All pressure points were padded. Then, midline incision was made from one level above to one level below the intended fusion levels. Para spinal muscles were splitted. Under fluoroscopic guidance, bilateral pedicle screws were inserted into L1 and L2. Partial interlaminar L1-L2 laminectomies were done. Unilateral or bilateral resection of the inferior facet of L1 and corresponding pars interarticularis were done Continuation of the procedure differs depending on the consistency of the herniated disc. In the case of hard disc herniations, this was done bilaterally where in the case of soft disc herniation ipsilateral facet -pars removal sufficed. Subsequently, L1 and L2 nerve roots were identified and meticulous hemostasis was obtained with bipolar coagulation of epidural veins and packing veins with hemostatic agents. Now the affected disc space can be easily visualized. If there was a sequestrated fragment, it was dissected softly from the dural sac and removed. This was followed with removal of the remaining contained disc. All steps were done without significant retraction of thecal sac. In the case of the hard calcified discs associated with large osteophyte, the annulus was incised at the extreme lateral side of the disc space and the contained disc material was removed as much as possible, the same scenario was repeated on controlateral side, at this time we aimed to the central part of the calcified disc. Initially, the procedure was started with destruction of L1 caudal osteophyte of tL1 vertebra with the aid of hammering on a boot-like instrument and pushing it into the disc space, The same was done for the osteophyte of L2, Thereafter, the same scenario was repeated on the controlateral side, till the dural sac became free of any compression. Subsequently, the disc space was cleaned from the debris of the broken calcified materials. Then, the rod was assembled on one side and after optimal distraction of the construct and wide opening of the disc space; a peek cage of an appropriate size was inserted into the space from the controlateral side. Of course the floor of the corresponding intervertebral disc space was packed with local bone grafts or demineralized allograft chips prior to insertion of the cage. Finally, the nuts of both constructs were tightened in compression, in order to secure the peek cage. In all these steps, rotating the table and angling the microscope were of great help for visualization of central part of the calcified disc without retracting the dural sac. Wound was closed in anatomical layers. Drain was removed in the first or second post-operative day depending on the amount of the blood drainage.
Outcome assessment
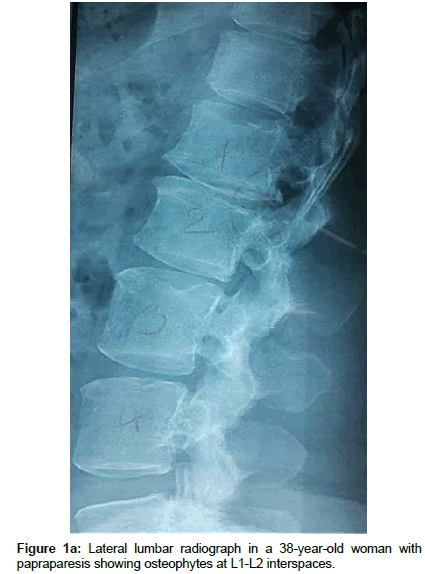
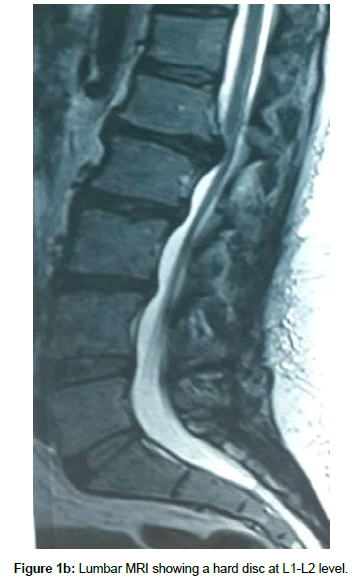
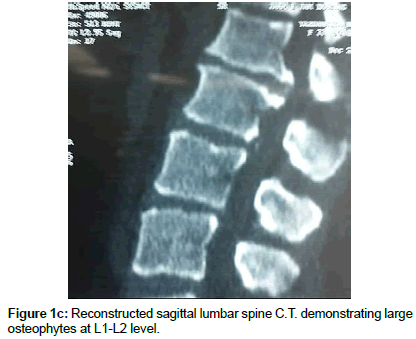
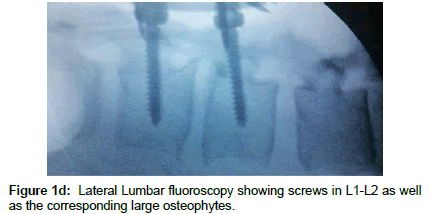
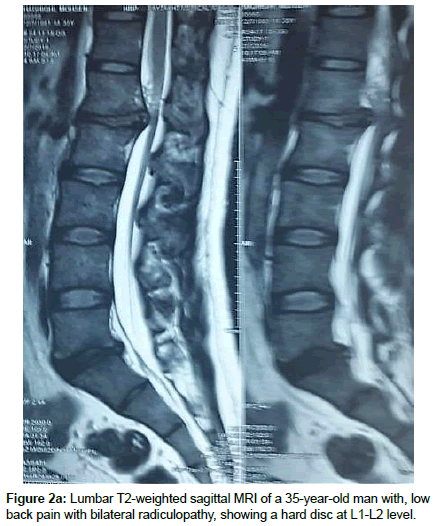
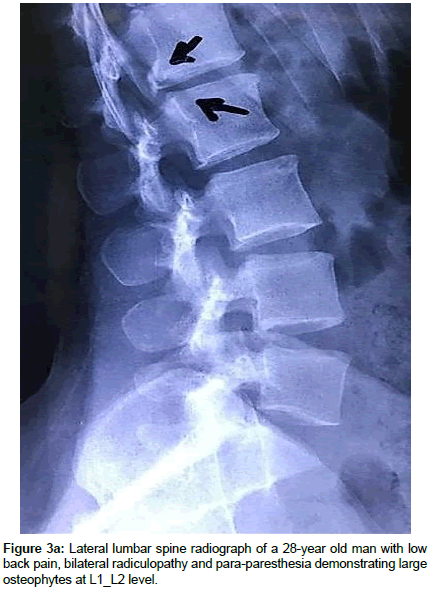
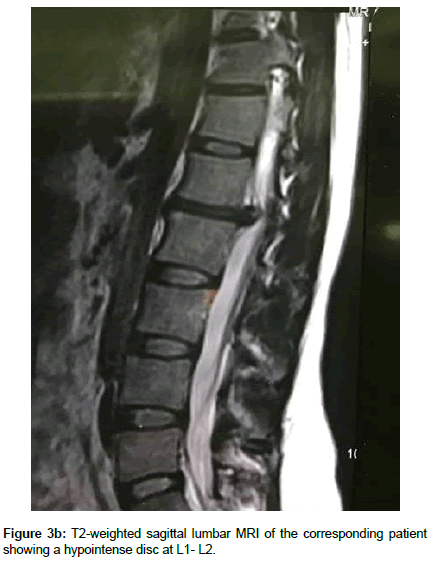
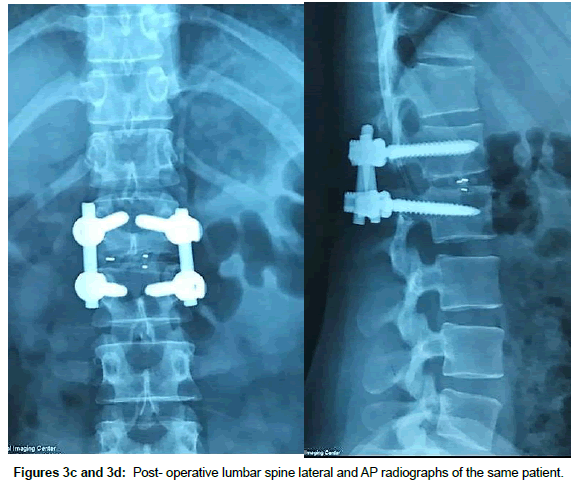
Operation time, the amount of intraoperative blood loss, and the post-operative time to return to routine work and daily life were documented. Clinical and radiological assessments were performed post-operatively and patients were followed up 1, 3 and 12 months after surgery. This follow up included a visiting at an outpatient clinic and telephone interview. As a radiological assessment, all cases had post-operative lumbar x-rays in early post-operative period and in 3, 6 and 12 months after surgery. An independent radiologist made radiographic evaluation based on dynamic lumbar x-rays, 3D CT scans and MRI. Clinical outcomes were collected and graded using the VAS for back and leg pain separately and functional outcomes were measured by ODI scores to quantify the impact of symptoms on patient’s everyday life [12,13]. Figures 1a-1h shows the clinical picture imaging studies and surgical results of three demonstrative patients (Figures 2a-2e and Figures 3a-3d).
Results
37 Subjects (19 males and 18 females) with a mean age 48.3 ± 13.9 years (range 23-83 years) were included in this study. Our average follow up period was 18.6 months (range 12-26). The mean operation time and intraoperative blood loss volume were 114 min (range 100- 145 min) and 371 ml (range 300-480 ml), respectively. Table 1 shows summary of patient’s demographics and clinical data.
| Patients (n) | 29 |
| Mean age ± standard deviation (years) | 48.3 ± 13.9 |
| Male [n (%)] | 15 (51.7%) |
| Female [n (%)] | 14 (48.3%) |
| Mean follow-up duration (months) | 18.6 |
| Preoperative symptoms and signs | |
| Back pain [n (%)] Radicular leg pain [n (%)] Sensory deficit [n (%)] Motor deficit [n (%)] |
23 (79.3%) 21 (72.4%) 15 (51.7%) 11 (37.9%) |
Table 1: Summary of patient’s demographics and clinical data.
Clinical outcomes
Prior to the surgery, the mean VAS for back and leg pain were 6.9 ± 1.1 and 7.7 ± 1.0, respectively. In the last follow up the mean VAS score for back and leg pain were significantly decreased to 1.8 ± 0.6 and 1.7 ± 0.5, respectively (p <0.001), as did the ODI scores which decreased from 68.1 ± 6.1% to 20.6 ± 3.1% (p <0.001) as shown in Table 2. 32 of 37 patients (86.4%) returned to their routine work and daily life within 2.4 months after the operation (ranging from 1.5 to 3.5 months).
| Pre-operative | Post-operative (last follow up) | p-value | |
|---|---|---|---|
| Mean ODI ± SD (%) | 68.1 ± 6.1 | 20.6 ± 3.1 | <0.001 |
| Mean VAS ± SD (leg) | 7.7 ± 1.0 | 1.7 ± 0.5 | <0.001 |
| Mean VAS ± SD (back) | 6.9 ± 1.1 | 1.8 ± 0.6 | <0.001 |
Table 2: Clinical outcomes based on VAS and ODI scores.
Radiological results
A review of post-operative lumbar dynamic x-rays, CT scans and MRIs showed adequate decompression also bony union was seen in 33 of 37 patients (89.6%). Solid fusion was not achieved in 3 cases; still they were asymptomatic. There were no cases of pseudoarthrosis and symptomatic adjacent segment degeneration.
Complications
One patient experienced acute surgical site hematoma and consequently a paraparesis, which symptoms resolved after hematoma removal. In two patients, dura was torn during discectomy which in both cases the dura was repaired and no CSF leakage was observed post-operatively. There were no other approach related complications such as pedicle screw malpositioning, neurological damage to spinal cord or nerve roots.
Discussion
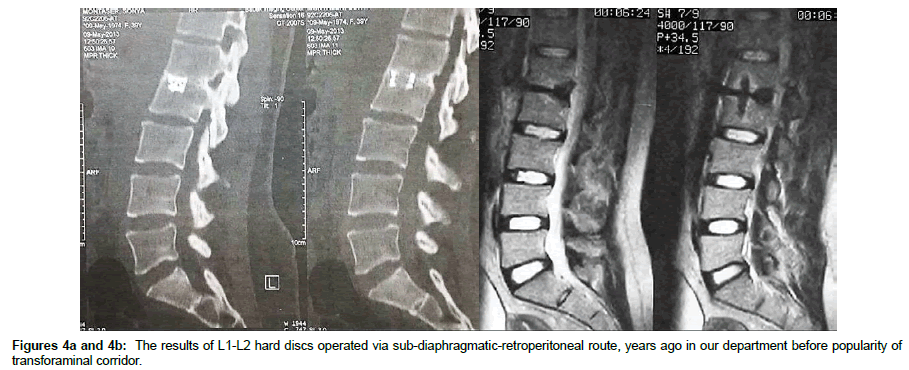
This study is in continuance of authors’ studies about microsurgical transforaminal approach of L1-L2 disc herniation [14,15]. To our knowledge this study is the largest series of surgically treated L1-L2 disc herniation alone. L1- L2 disc herniation is unique in several aspects in comparison to lower lumbar disc herniation. First, it hosts conus medullaris or is in close proximity to it making sac retraction and manipulation during surgery very hazardous. Also, spinal canal at this level is narrower compared to lower levels. Secondly, this level has special biomechanical characteristics. It is located at the point where thoracic kyphosis turns to lumbar lordosis and due to this characteristic, this level (L1-L2) is named as the “fulcrum disc” [1,2,16]. Additionally, sagittal orientation in this level allows only minimal facet resection without causing instability. Not uncommonly, L1-L2 disc herniation is accompanied with some conditions such as adjacent thoracic kyphosis, lumbar continuous or non-continuous disc herniation and/or canal stenosis [1]. This makes surgical plan even more complex. In comparison to lower lumbar disc herniation, L1-L2 herniation is more commonly calcified, making safe discectomy via simple laminectomy more critical. By comparison with thoracic disc herniation, L1-L2 doesn’t have rib cage support, resulting in more instability after discectomy. In addition, the root cannot be divided and sacrificed in posterior discectomy techniques. Compared to thoracic levels, dural sac retraction at L1-L2 may result in root and cauda injury in addition to spinal cord (conus) injury [3,5-8]. Consider above mentioned characteristics of L1-L2 disc herniation. This level needs special attention and considerations in choosing safe and optimal surgical technique. There are several approaches to address L1-L2 disc herniation. These are associated with potential complications. For example, Kim et al used oblique paraspinal approach [4]. Although they reported lesser instability and lower recurrence rates, this approach is not suitable for calcified discs and also narrow thecal sac visualization is provided for the surgeon. In another study, transdural approach was examined [11]. This approach is not possible at conus medullary level which is frequently located at L1-L2. Additionally, there is potential risk of complications related to CSF leakage. Ahn et al. performed endoscopic transfacet approach for L1-L2 disc herniations [16]. This approach is less invasive; however it requires special equipment and trained surgeons. In another minimally invasive approach, Wang et al described MIS-TLIF for thoracolumbar disc herniation [3]. 20% of their cases had non-union fixation and also this approach is not suitable for calcified discs. There is also the anterolateral approach, as we used to do so before popularity of transforaminal approach as we used to do so before popularity of transforaminal approach (Figures 4a and 4b). It is almost invasive and with difficult learning curve [1,7]. The significant advantage of transforaminal approach is its ability to be used for all types of L1-L2 disc herniations regardless of herniation type, disc consistency and conus level. Also, if there is stenosis in addition to disc herniation it can be addressed with a single posterior approach. The posterior approach is more convenient for most surgeons. With removing the inferior facets of cranial vertebra and pars, a surgeon can have a lateral access to disc space which allows him/her to remove the disc material with minimum thecal sac manipulation. Therefore, there is minimal risk for neural injury, especially when the conu is located at the L1-L2 or L1 level. Furthermore, the segmental or regional kyphosis can be corrected with this technique using translation and TLIF cages [15]. One drawback of this approach is the additional cost for instrumentation. Another disadvantage might be the long-term risk of developing adjacent level degeneration and disease, although with partial L1 laminectomy and good sagittal alignment, the chance of this complication can be reduced.
Conclusion
According to the results of this study and similarity to good clinical outcomes of other studies on lumbar disc herniation (L1 to S1) [17-19], we suggest that posterior transfacet microsurgical discectomy is a reproducible and safe technique to treat L1-L2 disc herniation.
Ethics
The ethical issues about all data of the patients in this retrospective study have been provided.
Conflict of interest
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Informed Consent
Written informed consent was obtained from three surgical examples.
References
- Sanderson SP, Houten J, Errico T, Forshaw D, Bauman J, et al. (2004) The unique characteristics of "upper" lumbar disc herniations. Neurosurgery 55: 385-389.
- Kim DS, Lee JK, Jang JW, Ko BS, Lee JH, et al. (2010) Clinical features and treatments of upper lumbar disc herniations. J Korean Neurosurg Soc 48: 119-124.
- Wang J, Zhou Y, Zhang ZF, Li CQ, Zheng WJ, et al. (2014) Disc herniation in the thoracolumbar junction treated by minimally invasive transforaminal interbody fusion surgery. J Clin Neurosci 21: 431-435.
- Kim JS, Lee SH, Moon KH, Lee HY (2009) Surgical results of the oblique paraspinal approach in upper lumbar disc herniation and thoracolumbar junction. Neurosurgery 65: 95-99.
- Hioki A, Miyamoto K, Hosoe H, Sugiyama S, Suzuki N, et al. (2011) Cantilever transforaminal lumbar interbody fusion for upper lumbar degenerative diseases (minimum 2 years follow up). Yonsei Med J 52: 314-321.
- Kido T, Okuyama K, Chiba M, Sasaki H, Seki N, et al. (2016) Clinical diagnosis of upper lumbar disc herniation: Pain and/or numbness distribution are more useful for appropriate level diagnosis. J Orthop Sci 21: 419-424.
- Ido K, Shimizu K, Tada H, Matsuda Y, Shikata J, et al. (1998) Considerations for surgical treatment of patients with upper lumbar disc herniations. J Spinal Disord 11: 75-79.
- Lee DS, Park KS, Park MS (2013) The comparative analysis of clinical characteristics and surgical results between the upper and lower lumbar disc herniations. J Korean Neurosurg Soc 54: 379-383.
- Hsu K, Zucherman J, Shea W, Kaiser J, White A, et al. (1990) High lumbar disc degeneration. Incidence and etiology. Spine 15: 679-682.
- Telfeian AE, Jasper GP, Oyelese AA, Gokaslan ZL (2016) Technical considerations in transforaminal endoscopic spine surgery at the thoracolumbar junction: report of 3 cases. Neurosurg Focus 40: E9.
- Choi JW, Lee JK, Moon KS, Hur H, Kim YS, et al. (2007) Transdural approach for calcified central disc herniations of the upper lumbar spine. J Neurosurg Spine 7: 370-374.
- Saberi H, Isfahani AV (2008) Higher preoperative Oswestry Disability Index is associated with better surgical outcome in upper lumbar disc herniations. Eur Spine J 17: 117-121.
- Mousavi SJ, Parnianpour M, Mehdian H, Montazeri A, Mobini B (2006) The Oswestry Disability Index, the Roland-Morris Disability Questionnaire, and the Quebec Back Pain Disability Scale: translation and validation studies of the Iranian versions. Spine 31: E454-459.
- Ebrahimzadeh K, Sharifi G, Shafizad M (2012) Surgical strategy for management of L1-L2 disc, based on unique differences with other lumbar levels. J Inj Violence Res 4: 74.
- Sharifi G, Abolhasani E, Hosseinzadeh M, Shafizadeh M, Mousavi A (2014) Neither a lumbar disc nor a thoracic disc; L1-L2 disc located in region of spine biomechanical and neural transition zone. Global Spine J 4: s-0034-1376665-s-1370034-1376665.
- Ahn Y, Lee SH, Lee JH, Kim JU, Liu WC (2009) Transforaminal percutaneous endoscopic lumbar discectomy for upper lumbar disc herniation: clinical outcome, prognostic factors, and technical consideration. Acta Neurochir 151: 199-206.
- Sedighi M, Haghnegahdar A (2014) Lumbar disk herniation surgery: outcome and predictors. Global Spine J 4: 233-244.
- Dewing CB, Provencher MT, Riffenburgh RH, Kerr S, Manos RE (2008) The outcomes of lumbar microdiscectomy in a young, active population: correlation by herniation type and level. Spine 33: 33-38.
- Dasenbrock HH, Juraschek SP, Schultz LR, Witham TF, Sciubba DM, et al. (2012) The efficacy of minimally invasive discectomy compared with open discectomy: a meta-analysis of prospective randomized controlled trials. J Neurosurg Spine 16: 452-462.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi