Review Article, J Spine Neurosurg Vol: 9 Issue: 2
The Growing Demand for Adult Spinal Deformity Surgery in England: A National Health Data Review
David C Kieser1*, Alan Silman2 and Dominique A Rothenfluh3
1Department of Orthopaedics and Musculoskeletal Medicine, University of Otago, Christchurch School of Medicine, Christchurch, New Zealand
2Nuffield Department of Orthopaedics, Rheumatology and Musculoskeletal Sciences, Oxford, England
3University of Oxford, Division of Spinal Surgery, Oxford, England
*Corresponding Author: David C Kieser,
Spinal Surgeon, Department of Orthopaedics and Musculoskeletal Medicine
University of Otago, Christchurch School of Medicine
Christchurch, New Zealand
Tel: +64 211499829
E-mail: kieserdavid@gmail.com
Received: July 29, 2019 Accepted: November 18, 2019 Published: November 26, 2019
Citation: Kieser DC, Silman A, Rothenfluh DA (2019) The Growing Demand for Adult Spinal Deformity Surgery in England: A National Health Data Review. J Spine Neurosurg 8:5.
Abstract
Objective: The rate of adult spinal deformity (ASD) surgery is increasing internationally. However, an understanding of the trends in England remains unknown. This study examines the trends in hospital admission and surgical intervention for complex ASD in order to predict the future health demands for NHS England.
Methods: Hospital episode statistics data for England were reviewed between 2005-2015 in order to determine the number of patients diagnosed and surgically treated for ASD. The future tenyear demand for surgery was modelled on demographic changes and admission trends, with the consequence on inpatient bed-days
and costs calculated.
Results: Over the time-course, the number of patients admitted has more than doubled, with an almost 3-fold increase in those older than 60-years. This contrasts the less than 10% increase in the adult population of England over the same time-period. The volume of ASD surgery has increased 3.5-fold, with the greatest increase in those older than 60years (6.4-fold increase).The average length of stay (LOS) has reduced from 10.1 to 8.4 days. If these trends continue, we estimate an additional 330
patients per year receiving ASD surgery, equivalent to an annual increase of 4.5 inpatients per day per year and additional financial cost of £8.1-11.5 million per year.
Conclusion: Severe ASD, unresponsive to conservative therapy, is a growing problem within England. The complex surgery required needs to be matched by the availability of the necessary expertise and considerable resources to meet this inevitable growing demand.
Keywords: Spinal deformity; Fusion; Kyphosis; Sagittal imbalance; Scoliosis; Alignment; Spine; surgery; Back pain
Abbreviations
ASD: Adult Spinal Deformity; CC: Complication Code; HES: Hospital Episode Statistics; HRG: Healthcare Resource Group; LOS: Length of Stay; NHS: National Health Service; QoL: Quality of life SVA: Sagittal Vertical Axis
Background
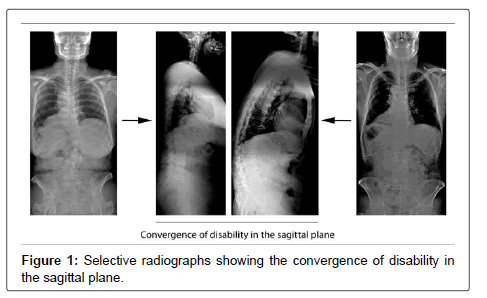
Spinal conditions are one of the most common groups of health disorders affecting adults [1]. Amongst spinal disorders adult spinal deformity (ASD) is predominantly a problem of older ages, with a reported prevalence of up to 32% of patients over the age of 50 years and 68% of patients aged over 70 years [2]. ASD is, however, an overarching term for a complex spectrum of spinal deformities [3,4]. Although frequently mild, when severe, it results in a persisting problem affecting a patient’s global spinal balance. This prevents the normal ‘economic’ resting posture resulting in increased physiological demands and subsequently fatigue, pain, neural compression and disability. The extent of these is directly related to the degree of spinal imbalance (Figure 1) [5-8].
The functional and quality of life (QoL) consequences of an imbalanced spine can be devastating [2,5-7,9]. Not surprisingly perhaps, compared to most other common long-term disorders, including arthritis, chronic lung disease, congestive heart failure, diabetes and ischaemic heart disease, ASD has a worse patient reported QoL and, hence, is the highest ranked disorder in estimates of global disease burden [10].
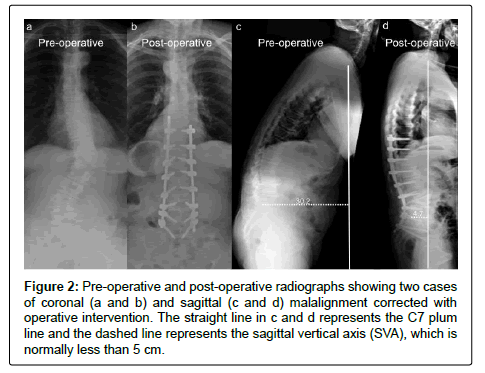
The treatment of severe ASD is challenging. Non-operative treatment has a limited role, especially when significant anatomical abnormality and spinal imbalance is present [11,12]. In contrast, operative management offers long-lasting benefit in improving pain, functional outcomes and QoL, but carries significant risk and expense [3,13-17]. The surgery for this condition has traditionally varied from single level neural decompression to global deformity correction. However, it is becoming clear that most patients with symptomatic ASD benefit from restoration of spinal balance (Figure 2) [8,18,19], although the surgery to achieve this is amongst the most complex of all planned surgical procedures.
Figure 2: Pre-operative and post-operative radiographs showing two cases of coronal (a and b) and sagittal (c and d) malalignment corrected with operative intervention. The straight line in c and d represents the C7 plum line and the dashed line represents the sagittal vertical axis (SVA), which is normally less than 5 cm.
Because of this growing body of evidence of the benefits of surgically restoring spinal balance, the number of complex operations being performed for ASD has doubled in the last decade in many countries, which contrasts with the 20% increase in all other spinal surgeries [4,20,21]. This growth suggested that there was a growing unmet demand [2], although this may have been fuelled by the availability of the resources to manage this disorder. In either event, if this trend were to continue it should be a concern to health policy planners.
Rational planning of current and future service provisions needs to have robust data on current and future demands and their likely consequences on the National Health Service (NHS). Yet, within England, there remains a paucity of data on the future demands of this condition and the challenges this condition will bear on the NHS. Our objectives were therefore firstly, to identify current trends in the burden of disease from severe ASD based on admission to hospital and surgical intervention, and secondly, to predict future demand based on these trends. Lastly, we consider the health economic implications of these predictions.
Methods
We used published anonymised data and therefore did not seek ethical approval or patient consent.
The latest eleven years of available annual aggregate health data for all hospital admissions and procedures in England, from 2005 to 2015, were retrieved from Hospital Episode Statistics (HES), available from the Health and Social Care Information Centre (https://digital.nhs.uk).
Patients were included in the analysis based on being as recorded for admission with ASD if any of the ICD10 diagnostic codes shown in Table 1. This range of codes largely reflects the variation in use of terms to describe the primary diagnosis related to ASD. The OPCS classification of interventions and procedures (version 8.4) was used as the procedural codes for complex ASD surgery (Table 1) [22]. In order to restrict the analysis to those with complex procedures, isolated decompressive procedures without instrumentation, were excluded. Prior to 2009 the procedural code V41.4 did not exist but was incorporated into one of the other codes listed. Similarly, V40.4 was only introduced in 2011. An accompanying code, V55 (level of spine) is sometimes used to add to the coding but this is supplementary to the main surgical procedure code and was therefore excluded.
| ICD10 diagnostic codes | OPCS operative codes | ||
|---|---|---|---|
| M40.1 | Other secondary kyphosis | V40.3 | Posterior instrumented fusion of the thoracic spine NEC |
| M40.2 | Other and unspecified kyphosis | V40.4 | Posterior instrumented fusion of the lumbar spine NEC |
| M41.1 | Juvenile idiopathic scoliosis | V41.1 | Posterior attachment of correctional instrument to spine |
| M41.2 | Other idiopathic scoliosis | V41.2 | Anterior attachment of correctional instrument to spine |
| M41.5 | Other secondary scoliosis | V41.4 | Anterior and posterior attachment of correctional instrument to spine |
| M41.9 | Scoliosis unspecified | V41.8 | Other specified instrumental correction of deformity of spine |
| V41.9 | Unspecified instrumental correction of deformity of spine | ||
Table 1: Diagnostic and procedural codes used in this analysis.
For the purposes of analysis, patients were separated, based on the available tabulations, into two age groups, namely 15-59 years and 60 years and older. Those older than 60 years were further subdivided in those under and over 75 years.
The main outcome of interest was the absolute number of (i) admissions and (ii) operations for complex ASD during the eleven years of observation. Secondly, using regression analysis, we modelled the linear trend, after allowing for any demographic change. We then predicted the probable future numbers over the next ten years, assuming the linear trend in demand persisted and also allowing for the predicted demographic changes.
The average length of hospital stay (LOS), was attained from the HES data for each procedural code and then averaged per year according to the number of patients treated for each procedural code. In order to estimate the average cost, we utilised the Healthcare Resource Group (HRG) codes, which is the national coding system determining tariff payments. This code is derived from the diagnosis (described above), the procedural code (described above) and the complication code (CC), which is an algorithmic derivative of the patient’s comorbidities. We included only two or more spinal levels and only “elective” codes. All “non-elective” codes were excluded. As the comorbidities and therefore CC code varies for each patient we presented the range of national tariffs for complex ASD procedures. Additionally, the age differs from the diagnostic and procedural codes and therefore we elected to include only those for 19 years and older. We also considered the costs of any revision procedure based on current data.
Statistical analysis
The raw data is presented for the diagnostic and operative volumes between 2005 and 2015. A trend line corresponding to the chronological change in operative volumes is incorporated and extrapolated to predict the future operative volumes in 2020 and 2025. Similarly, the change in LOS between 2005 and 2015 is extrapolated to 2025.
Results
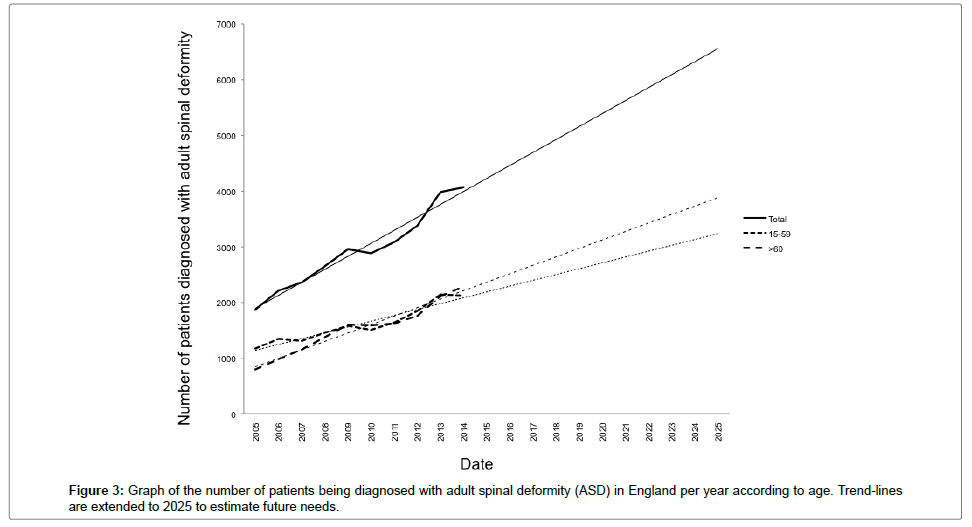
Within the last decade, based on the admissions to secondary care, the number of patients admitted with a diagnosis of ASD has more than doubled (2.2-fold increase), with the biggest change in those aged over 60 years (2.9-fold increase) (Figure 3).
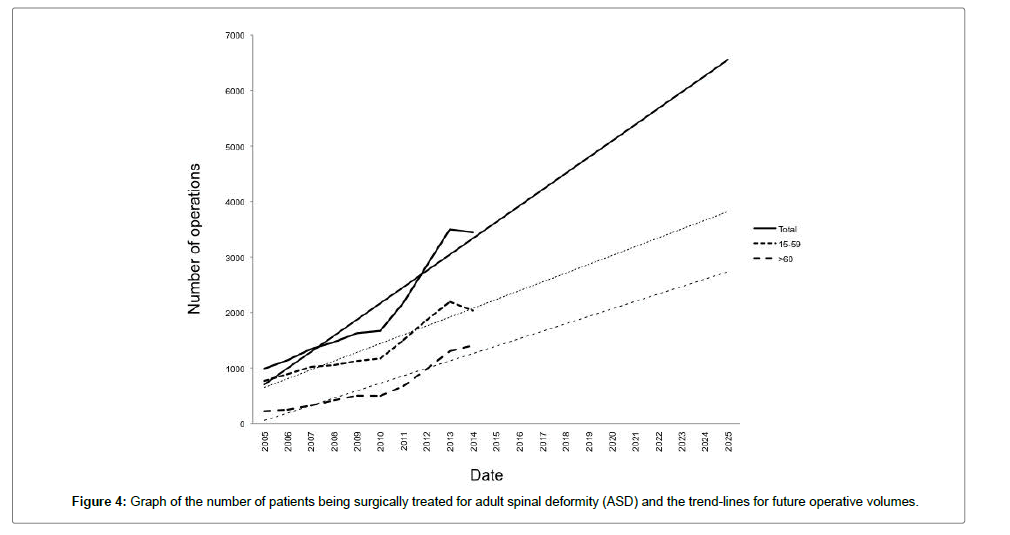
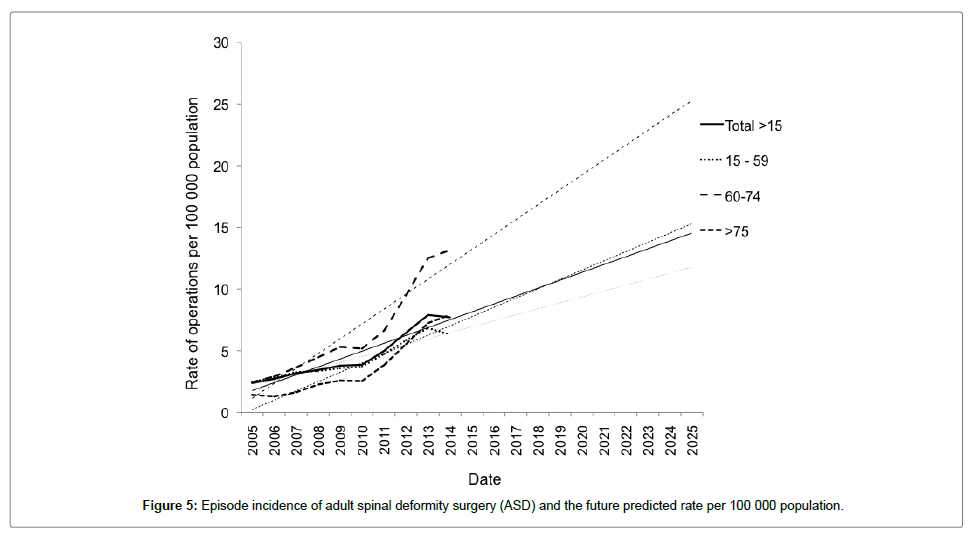
Figure 4 illustrates the number of patients surgically treated for ASD each year according to their age. This illustrates that within the last decade the number of patients treated with ASD has increased 3.5-fold and that the biggest change has been in those aged over 60 years (6.4-fold increase). If this trend continues it is estimated that by 2020, 5100 patients will require surgical intervention and by 2025, 6750 patients will receive ASD surgery, comprised of 3900 patients aged between 15 and 59 years and 2850 aged more than 60 years. When comparing the number of patients being surgically treated for ASD to the national population, the episode incidence of surgery continues to rise in all age groups (Figure 5).
The estimated LOS per patient has reduced from 10.1 days in 2005 to 8.4 days in 2015. If this trend continues, and considering the 3.5 fold increase in ASD operations in the last decade, it is estimated that the total number of inpatient days required in 2020 will be 38500 and in 2025 will be 45200. This equates to 124 inpatients every day nationally in 2025 and an annual increase of 4.5 inpatients per day from current volumes. More importantly, bed days are not all equal in terms of resource use and requirement for expert skills; with the peri-operative period being the period at greatest costs.
Despite the large number of combinations between diagnostic and procedural codes only four HRG codes are generated. The range of HRG codes and their national tariffs are shown in Table 2 [23]. There is an additional £224 per day funding for patients who exceed an expected LOS.
| HRG code | Description | National tariff (£) |
|---|---|---|
| HC50A | Very complex instrumented correction of spinal deformity | 33 374 |
| HC51A | Complex instrumented correction of spinal deformity, CC score 7+ | 34 704 |
| HC51B | Complex instrumented correction of spinal deformity, CC score 3-6 | 26 104 |
| HC51C | Complex instrumented correction of spinal deformity, CC score 0-2 | 24 568 |
Table 2: Healthcare resource group (HRG) codes (2018) for complex adult spinal deformity procedures and their national tariff [23].
Thus, the expected range of expenditure on national tariffs for ASD procedures in 2025 will be between £166 and 234 million based on the current prices. This represents an increase of £81-115 million from current spending.
As mentioned above there is also a need to account for the costs of any revision surgery. The national complication rate and breakdown of subsequent treatment is unclear. However, the costing for the tariffs for such revision procedures depends on the coding interpretation, however the cost may vary from £34 704 (HC51Acomplex instrumented correction of spinal deformity, CC score 7+) for removal of instrumentation and revision of correction, to £2 509 (WH07D-infections or other complications of procedures with single intervention, CC score 0-1) for wound washout and debridement.
Discussion
Surgical intervention for severe ASD, when indicated, is complex and the demands of a single case and impact on health services are disproportionately greater than those of other elective procedures, such as total hip joint replacement. These procedures can take over eight hours and can be associated with a large number of peri- and post-operative complications. However, for many severely affected patients, surgery offers the only option to improve quality of life.
Internationally, the diagnosis and treatment of ASD continues to increase at disproportionate rates to the increase in local populations [2]. If this increase in the occurrence of the underlying disorder is true, then it is not unexpected that at the severe end of the spectrum, there will be a growing demand for surgical intervention. Within England, we are experiencing a similar trend with the demand growing at a pace that is unsustainable with current resources, which include money, skilled surgeons and peri-operative teams, operating suites and hospital beds. Concerning, this is despite the baby boomer population only just entering the predominant age groups for this condition.
Our results suggest a 3.5-fold increase in patients requiring complex ASD surgery in the next decade with the biggest growth being in those aged over 60 years (6.4-fold increase). We calculate that this equates to an annual increase of 330 patients requiring surgery and 1644 inpatient days, even allowing for the trend of reducing LOS. Apart from age, there is no reason to believe there is an underlying increase in the incidence of ASD in the population, and thus the increase observed in our ten-year period, represents an increase in demand, possibly fuelled by increased availability of resources to manage this demand.
Our study did not address the non-operative costs of managing these patients. Within the published literature, there remains a lack of evidence supporting the use of non-operative therapy in ASD [11,12]. In contrast, the literature favours operative intervention in symptomatic patients and this has further fuelled the increased volume of complex ASD surgery being performed nationally and internationally [4,13,20,21]. Despite the paucity of data on non-operative care, the authors feel that the projected increasing demand in our study should not be interpreted as though surgery is mandatory but rather, that for many patients there remains no other option. Thus, ongoing research into alternative therapies, including preventative, treatment and peri-operative optimisation, the development of accurate treatment algorithms and cost saving strategies during surgical intervention should be developed.
Surgery for complex ASD is amongst the most expensive of all elective procedures. Within the USA, the average total hospital cost for a primary procedure is US$103 143, with the operating room cost (US$70 514) constituting the majority of this cost [15]. The costs of ASD surgery have not been well defined within the UK. This is because the cost relates to the surgical expense (including operating room costs, instrumentation and personnel), the cost of the hospital stay (including intensive care, anaelgesia, rehabilitation) and the complications. We utilised the HRG codes to determine the national tariffs of these procedures, which ranged from £24 568 - 34 704. However, all referral centres treating ASD have a local financial agreement, which supersedes the national tariffs, therefore, these values underestimate actual costs in England. Nonetheless, utilising the national tariffs we found the expected expenditure in 2025 to be £166-234 million, which equates to an annual increase of £8.1-11.5 million from current expenditure.
Management strategies are therefore necessary to control this increasing financial burden. Within the USA, the surgeon’s implant preference has been identified as the largest determinant of modifiable operating costs accounting for a US$14 780 difference between patients [15]. This is likely to be similar within the UK and suggests that there are avenues to improve expenditure with nationalisation of surgical resources.
It should be recognised that the surgical approach to this condition can vary, but that a restoration of spinal balance is important [8]. If this is not achieved there is a poorer patient outcome, higher complication rate and higher rate of revision [8,24,25]. Thus, undertaking minimal surgery without deformity correction in order to reduce initial costs may be counterintuitive.
Furthermore, it should be recognised that operative intervention in ASD has a high complication rate and patients don’t benefit equally [3,14,16,17]. The reported overall complication rate of ASD is 30-40%, with a major complication rate of 20% and a 30-day mortality of 2.4% [26,27]. Similarly, the revision rate for instrumented fusion in primary ASD is 9-26% [28,29]. The average total hospital cost of a readmission in the USA is US$67 262, equating to 70% of the initial cost of the patient’s treatment [15]. In addition, patients requiring revision have a worse longer-term outcome than those who do not require revision [29]. Therefore, it is in both the patient’s and the institutions best interest to optimise the first procedure, this being that although the initial costs may be greater, the longer-term costs will be lower. An approach to “getting it right first time” is therefore warranted [30]. This process may be enhanced by a process of certifying spinal surgery centres in Europe based on their performance based on a robust registration process. This is very much a ‘work in progress’ the debate for which, we hope this paper will contribute.
This analysis has a number of limitations. Firstly, patients diagnosed with ASD and registered with the Health and Social Care Information Centre are usually identified by the spinal surgeon, yet a number of patients with ASD may never seek surgical review, thus it is likely that this study significantly underestimates the national disease burden. Secondly, this study does not identify those patients with ASD who undergo less invasive procedures, such as isolated neural decompression. Thirdly, we have to rely on the accuracy of coding of the data within HES, an inevitable consequence of using routinely available secondary care data. We have attempted to cover all the codes used but changes in coding practice may, as always in these types of analysis, have influenced the trends. One small source of error for example is the use of the ‘V55’ code level of spine surgery but not indicating another procedure code. In fact, in our data this was only the case in 20 patients in the one year we checked (2014) and would not have affected the results. Fourthly, we offer future predictions based on the last decade’s trends, but these are only gross predictions and the fluctuations cannot be predicted. Indeed, the levels of activity are related to growing demand, predominantly based on age, but also on the changing surgical opinion and practice, which is harder to model. Fifthly, we are limited by the availability of the public data. For example, the HES data is based on including all those over 15, whilst the costs data are based on those aged over 19. In practice this discrepancy will not have influence the results in an important manner. Given the HES data we have included all patients over the age of 15 as an ‘adult deformity’. This cut off excludes ‘juvenile scoliosis’ (onset before age 10). More importantly, although surgery in late teens and early adult life are included, the data presented clearly shows that the growth in activity has been in those over aged 60, with a particular emphasis on those over 75. We have presented the early adult data for completeness. Sixthly, it is a challenging exercise to model the requirement for bed days. Indeed, LOS is reducing across many planned surgical procedures, but LOS is greater in those with the greatest health needs. Thus, any trend to intervene on more elderly frail patients, with greater needs, might arrest or increase the trend to a reduction in LOS. Seventhly, the national tariff does not cover all of the costs incurred for each patient and therefore each trust has its own local agreement, which is significantly more than the national tariff. Therefore, the financial costs described in this study are an underestimate of the actual costs. Lastly, we only assessed the data for England, however it is likely that this trend is replicated in developed and developing countries worldwide.
Conclusion
Severe ASD is an increasing health burden within England, particularly in those aged over 60 years. Although there will be a continuing debate on the role and value of non-surgical therapies for patients with such complex spinal problems it is sensible to attempt to predict the number of patients diagnosed and surgically treated to nearly double within the next decade. This conservatively equates to an additional 330 patients undergoing ASD per year and an additional annual increased requirement of 1644 inpatient days and between £8.1 and 11.5 million expenditure.
Declarations
Ethics approval and consent to participate: Ethical approval was sought but deemed unnecessary as it was a review of HES data.
Consent for Publication
Not applicable.
Availability of Data and Material
The datasets generated and/or analysed during the current study are available in the HES database.
Competing Interests
The authors declare that they have no competing interests. Funding
No funding was attained for this study.
Author’s Contribution
Kieser DC: Study design, data extraction and analysis, interpretation and write up.
Silman A: Data analysis, interpretation and write up.
Rothenfluh DA: Study design, data extraction and analysis, interpretation and write up.
All authors have read and approved the manuscript.
Acknowledgement
Chris Middlemass for his input into the national coding, Glynny Kieser for her editorial input
Competing Interest
The authors declare that they have no competing interests.
References
- Salomon JA, Haagsma JA, Davis A, de Noordhout CM, Polinder S, et al. (2015) Disability weights for the Global Burden of Disease 2013 study. Lancet Glob Health 3: e712-23.
- Schwab F, Dubey A, Gamez L, El Fegoun AB, Hwang K, et al. (2005) Adult scoliosis: prevalence, SF-36, and nutritional parameters in an elderly volunteer population. Spine 30: 1082-1085.
- Smith JS, Shaffrey CI, Fu KM, Scheer JK, Bess S, et al. (2013) Clinical and radiographic evaluation of the adult spinal deformity patient. Neurosurg Clin N Am 24: 143-156.
- Good CR, Auerbach JD, O'Leary PT, Schuler TC (2011) Adult spine deformity. Curr Rev Musculoskelet Med 4: 159-167.
- Glassman SD, Bridwell K, Dimar JR, Horton W, Berven S, et al. (2005) The impact of positive sagittal balance in adult spinal deformity. Spine 3: 2024-2029.
- Lafage V, Schwab F, Patel A, Hawkinson N, Farcy JP (2009) Pelvic tilt and truncal inclination: two key radiographic parameters in the setting of adults with spinal deformity. Spine 34: E599-606.
- Schwab FJ, Blondel B, Bess S, Hostin R, Shaffrey CI, et al. (2013) Radiographical spinopelvic parameters and disability in the setting of adult spinal deformity: a prospective multicenter analysis. Spine 38: E803-E812.
- Schwab F, Patel A, Ungar B, Farcy JP, Lafage V (2010) Adult spinal deformity-postoperative standing imbalance: how much can you tolerate? An overview of key parameters in assessing alignment and planning corrective surgery. Spine 35: 2224-2231.
- Schwab F, Dubey A, Pagala M, Gamez L, Farcy JP (2003) Adult scoliosis: a health assessment analysis by SF-36. Spine28: 602-606.
- Pellise F, Vila-Casademunt A, Ferrer M, Domingo-Sabat M, Bago J, et al. (2015) Impact on health related quality of life of adult spinal deformity (ASD) compared with other chronic conditions. Eur Spine J 24: 3-11.
- Glassman SD, Carreon LY, Shaffrey CI, Polly DW, Ondra SL, et al. (2010) The costs and benefits of nonoperative management for adult scoliosis. Spine 35: 578-582.
- Glassman SD, Berven S, Kostuik J, Dimar JR, Horton WC, et al. (2006) Nonsurgical resource utilization in adult spinal deformity. Spine 31: 941-947.
- Liu S, Schwab F, Smith JS, Klineberg E, Ames CP, et al. (2014) Likelihood of reaching minimal clinically important difference in adult spinal deformity: a comparison of operative and nonoperative treatment. Ochsner J14: 67-77.
- Baron EM, Albert TJ (2006) Medical complications of surgical treatment of adult spinal deformity and how to avoid them. Spine 31: S106-18.
- McCarthy IM, Hostin RA, Ames CP, Kim HJ, Smith JS, et al. (2014) Total hospital costs of surgical treatment for adult spinal deformity: an extended follow-up study. Spine J 14: 2326-2333.
- Smith JS, Shaffrey CI, Glassman SD, Berven SH, Schwab FJ, et al. (2011) Risk-benefit assessment of surgery for adult scoliosis: an analysis based on patient age. Spine 36: 817-824.
- Smith JS, Klineberg E, Lafage V, Shaffrey CI, Schwab F, et al. (2016) Prospective multicenter assessment of perioperative and minimum 2-year postoperative complication rates associated with adult spinal deformity surgery. J Neurosurg Spine 25: 1-14.
- Bridwell KH, Glassman S, Horton W, Shaffrey C, Schwab F, et al. (2009) Does treatment (nonoperative and operative) improve the two-year quality of life in patients with adult symptomatic lumbar scoliosis: a prospective multicenter evidence-based medicine study. Spine 34: 2171-2178.
- Scheer JK, Smith JS, Clark AJ, Lafage V, Kim HJ, et al. (2015) Comprehensive study of back and leg pain improvements after adult spinal deformity surgery: analysis of 421 patients with 2-year follow-up and of the impact of the surgery on treatment satisfaction. J Neurosurg Spine 22: 540-553.
- McCarthy I, O'Brien M, Ames C, Robinson C, Errico T, et al. (2014) Incremental cost-effectiveness of adult spinal deformity surgery: observed quality-adjusted life years with surgery compared with predicted quality-adjusted life years without surgery. Neurosurg Focus 36: E3.
- http://hcup-us.ahrq.gov/nisoverview.jsp.
- OPCS Classification of Interventions and Procedures (Version 4.8): NHS Digital; (2017).
- https://improvement.nhs.uk/resources/national-tariff-1719/.
- Kim YJ, Bridwell KH, Lenke LG, Rhim S, Cheh G (2006) Pseudarthrosis in long adult spinal deformity instrumentation and fusion to the sacrum: prevalence and risk factor analysis of 144 cases. Spine31: 2329-2336.
- Hostin R, McCarthy I, O'Brien M, Bess S, Line B, et al. (2013) Incidence, mode, and location of acute proximal junctional failures after surgical treatment of adult spinal deformity. Spine 38:1008-1015.
- Pateder DB, Gonzales RA, Kebaish KM, Cohen DB, Chang JY, et al. (2008) Short-term mortality and its association with independent risk factors in adult spinal deformity surgery. Spine 33: 1224-1228.
- Daubs MD, Lenke LG, Cheh G, Stobbs G, Bridwell KH (2007) Adult spinal deformity surgery: complications and outcomes in patients over age 60. Spine 32: 2238-2244.
- Pichelmann MA, Lenke LG, Bridwell KH, Good CR, O'Leary PT, et al. (2010) Revision rates following primary adult spinal deformity surgery: six hundred forty-three consecutive patients followed-up to twenty-two years postoperative. Spine 35: 219-226.
- Scheer JK, Tang JA, Smith JS, Klineberg E, Hart RA, et al. (2013) Reoperation rates and impact on outcome in a large, prospective, multicenter, adult spinal deformity database: clinical article. J Neurosurg Spine19: 464-470.
- Soroceanu A, Burton DC, Diebo BG, Smith JS, Hostin R, et al. (2015) Impact of obesity on complications, infection, and patient-reported outcomes in adult spinal deformity surgery. J Neurosurg Spine1-9.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi