Short Communication, J Diagn Tech Biomed Anal Vol: 8 Issue: 1
The Turning Point for Maintaining Balance
Aasen T1,2*, Nordahl SHG1,3, Goplen FK1,2,3 and Knapstad MK1,2
1Norwegian National Advisory Unit on Vestibular Disorders, Haukeland University Hospital, Bergen, Norway
2Department of Otorhinolaryngology, Head and Neck Surgery, Haukeland University Hospital, Bergen, Norway
3Department of Clinical Medicine, University of Bergen, Bergen, Norway
*Corresponding Author : Aasen T
Norwegian National Advisory Unit on Vestibular Disorders, Haukeland University Hospital, Bergen, Norway
Tel: +4791750384
E-mail: torbjorn@aasens.net
Received: August 16, 2019 Accepted: August 26, 2019 Published: September 05, 2019
Citation: Aasen T, Nordahl SHG, Goplen FK, Knapstad MK (2019) The Turning Point for Maintaining Balance. J Diagn Tech Biomed Anal 8:1.
Abstract
Background: A method for detecting the critical time frame for reacting to postural sway in order to maintain balance has been previously proposed. However, this method requires subjective assessment, which reduces cost-efficiency and could introduce bias. In this article, we present a simple and robust algorithm to estimate the time window length, the turning point, during which the regulating functions for maintaining the upright position come into action.
Methods: Postural sway was measured using a static balance platform across four conditions (eyes open/closed, standing on bare platform/rubber foam) in a group of healthy subjects and a group of patients suffering from dizziness. The Hurst exponent is a measure of long-term memory of a time series. The turning point is estimated as the time where the derivative, the stepwise difference of the slope, of the Hurst scaling series crosses from higher to lower than 0.5 (i.e. switching from a positive to negative correlation).
Results: The turning point was increased in patients when standing on the bare platform with eyes open and closed.
Conclusion: An increased turning point may indicate delayed compensatory action to postural sway in some patients suffering from dizziness. This paper presents a new algorithm for estimating the turning point without the need for subjective data evaluation, increasing cost efficiency and reducing the potential for bias. The method is feasible for evaluating postural control and discriminates between patients with dizziness and healthy controls.
Keywords: Stabilometry; Hurst exponent; Information processing; Postural control; Dizziness
Introduction
The conceptual framework for this paper was obtained from Collins and De Luca [1]. They introduced a method known as stabilogram diffusion analysis to provide a quantitative statistical measure of the apparently random variations of Center-of-Pressure (COP) trajectories recorded during quiet upright stance in humans. The authors showed that the COP position series were positively correlated in the short term (i.e. over short observation times) but negatively correlated in the long term. Therefore, the time horizon between the short-and longrange regions was designated as the critical point and estimated as the intersection point of the straight lines fitted to the two regions of the linear-linear version of mean-square displacement (mm2) vs. time interval, which implies a degree of subjective assessment.
The aim of this study was to present a simple and robust algorithm to estimate the Turning Point (TP) that could be automated without the need for subjective assessment. We emphasize that the TP parameter is not an exact quantification of an essential property of the underlying physiological regulating system, but an estimate of some quality that gives information about the function of maintaining balance.
In order to assess the efficacy and utility of the TP algorithm, we applied it to patients with dizziness and compared the results to those from healthy controls.
Ethics
The project was part of a larger study approved by the Regional Committee for Health and Medical Research Ethics of South-Eastern Norway (REK 2017/783).
Materials and Methods
Subjects
We included 30 patients suffering from dizziness and were referred to a specialist unit for balance and dizziness disorders at a university hospital. Patients with severe orthopedic or neurologic disorders, known to influence balance, were excluded. The patients (70% female) had a mean age of 34.4 years (SD 14.0), with a range of 28 to 67. Additionally, a group of 30 healthy subjects was recruited among the hospital staff. The controls (63% female) had a mean age of 36.1 (SD 9.7), with a range from 21 to 54 years.
Computerized stabilometry
Stabilometry was evaluated by using the Synapsys Postugraphy System® (SPS®, SYNAPSYS, Marseille, France). Computerized Stabilometry (Posturography) used for documenting balance performance is non-invasive and causes no discomfort [2]. All participants were evaluated with the following protocol: Two tests of 20 s standing on a static platform, first standing upright with eyes open and second with eyes closed.
The same protocol was then preformed with the subjects placed on a foam balance board, making it harder to keep balance due to less proprioceptive input from the feet/ankles. The participants were told to stand with their feet aligned to the predetermined markings, corresponding to foot size and to stand with arms resting along the sides of their bodies.
Methods and analysis
The postural sway can be modeled as a correlated random walk [1,3] with the scaling properties
< Δx2 > = < (xi – xi-Δt)2 > ~ Δt2H
Where, < Δx2 > is the mean square displacement.
The scaling coefficient H, also called the Hurst exponent, is a measure of long-term memory of a time series with the three properties.
I. A time-integrated white noise time series (i.e. a random walk series) has a Hurst exponent of H=0.5.
II. A Hurst exponent that is higher than 0.5 (H>0.5) corresponds to a process which is trending (persistent), like a person moving away from the upright unstable equilibrium.
III. A Hurst exponent that is lower than 0.5 (H<0.5), corresponds to a mean reverting process (anti-persistent), like a person regulating back to the equilibrium, for the purpose of maintaining the balance.
In this study, we calculated the time horizon where the derivative, the stepwise difference of the slope of the scaling, crosses from positive correlation (II) H>0.5 to negative correlation (III) H<0.5.
The algorithm is simple. Instead of estimating the short-range and long-range scaling regions of the linear–linear plots of mean-square displacement (mm2) vs. time interval, we calculate the stepwise first differentiated series of the logarithm to the mean square displacement for increasing window size and the logarithm for the increasing window size, and estimate the shift, the Turning-Point (TP), as the time where the differentiated series crosses from higher to lower than 0.5.
The turning-point algorithm
We applied the algorithm to the shift of the Center of Pressure (COP) at the sole of the feet 20 s duration of body sway. The sample frequency was 100 Hz, which gave a time series recording of 2,000 data points.
We have a time series xi,
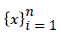
First, we calculate the mean square displacement < x2 > in mm for increasing the window size Δt.
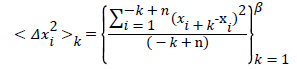
The window size is defined by the sampling frequency of 100 Hz, which sets the resolution to 10 ms. Increasing k increases the window size in steps of 10 ms. n is in our case 2,000 and we increment k until we span a window length of 5 s (β=500), long enough to fulfill the criteria of crossing 0.5 (if a subject does not reach the TP and activate the feedback mechanism to keep the upright position before a time span of 5 s, he/she will certainly fall).
Then, from the scaling properties, we find the slope si.
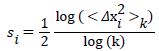
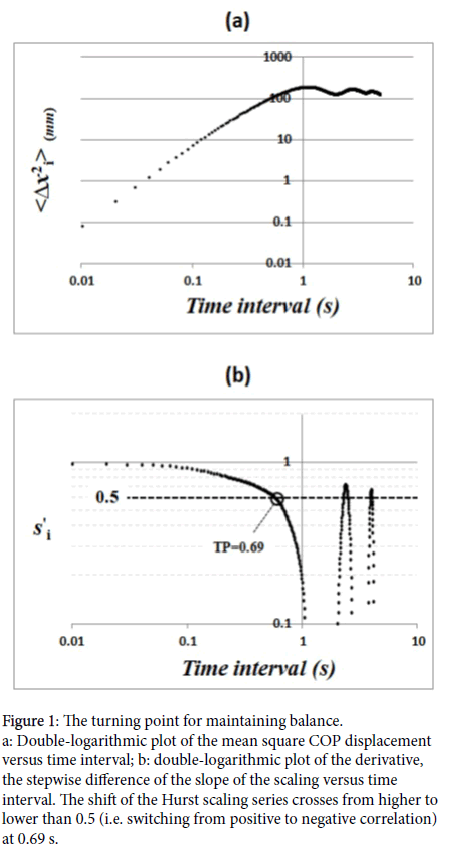
The TP is the time where the derivative 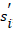 , the stepwise difference of the slope, crosses from higher to lower than 0.5 (Figure 1).
, the stepwise difference of the slope, crosses from higher to lower than 0.5 (Figure 1).
Figure 1: The turning point for maintaining balance. a: Double-logarithmic plot of the mean square COP displacement versus time interval; b: double-logarithmic plot of the derivative, the stepwise difference of the slope of the scaling versus time interval. The shift of the Hurst scaling series crosses from higher to lower than 0.5 (i.e. switching from positive to negative correlation) at 0.69 s.
Due to non-normality distribution of the TP, the median and Mann-Whitney U test was used to compare the TP values for the healthy and patient groups for the various test conditions.
Results
When applying the algorithm to the group of healthy subjects and the group of patients suffering from dizziness, we found a higher TP value for the patients in all four conditions. However, the difference was only significant for the easiest conditions, such as when standing on the platform without the foam mat (Table 1).
| Turning point (seconds) of center of pressure (COP) | |||
|---|---|---|---|
| Healthy | Patients | T-test | |
| EO | 0.49 | 0.77 | 0.018* |
| EC | 0.43 | 0.7 | 0.012* |
| F-EO | 0.42 | 0.55 | 0.052 |
| F-EC | 0.43 | 0.45 | 0.589 |
Table 1: EO: Eyes Open; EC: Eyes Closed; F: Foam; *p<0.05, Healthy n=60, Patients n=60. (n is the total number of two trials of 20 s for each person).
Discussion
A human body in upright position is in an unstable equilibrium. Like a pencil balancing on the tip, it will fall. The human mind is an information processing system with regulatory and compensatory mechanisms in place to maintain balance when it gets information that it is falling (sensory feedback). ‘When it gets information’ tell us there is a time delay before this information is provided and processed, and we present an algorithm to estimate this time delay, or time window, for a human regulating the balance turning-point. The TP is an estimate of the critical time to react and regulate back to the unstable equilibrium. This is an ongoing process to maintain balance. The TP is partially related to the information processing of cognitive functions, including several sensory, proprioception and vestibular functions.
We found that the TP was higher for patients with dizziness; however the difference only reached significance in the condition without the foam mat. A higher TP value could indicate a slower sensory feedback from the systems maintaining balance. This is often the case in patients with persistent dizziness.
The question in focus is not if the TP parameter is the true value of the information processing response and regulating reaction to proprioceptive inputs related to maintaining balance. Rather, we address whether this parameter captures the properties related to maintaining balance and can therefore be of possible use in the clinic in the future.
Despite the limitation of small sample size, this study suggests that the function of maintaining balance differentiates vertigo patients from healthy subjects. This encourages following up the study, applying the method to various groups of dizzy patients.
Conclusion
The algorithm we present for the turning point avoids subjective considerations and seems feasible to use for evaluating postural balance. It may also have the ability to discriminate between patients with dizziness and healthy controls.
References
- Collins JJ, De Luca CJ (1993) Open-loop and closed-loop control of posture: A random-walk analysis of center-of-pressure trajectories. Exp Brain Res 95: 308-318.
- Nordahl SHG, Aasen T, Owe JO, Dyrkorn BM, Eidsvik S, Molvær OI (2000) Static stabilometry and repeated testing in a normal population. Aviat Space Environ Med 71: 889-93.
- Collins JJ, De Luca CJ (1994) Random walking during quiet standing. Phys Rev Lett 73: 764-767.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi