Review Article, J Womens Health Issues Care Vol: 6 Issue: 2
Antenatal Perineal Massage Improves Women’s Experience of Childbirth and Postpartum Recovery: A Review to Facilitate Provider and Patient Education on the Technique
Ellington JE1*, Rizk B2 and Criso S3
1BioOrigyn, LLC, Valleyford, WA, USA
2Professor and Head, Reproductive Endocrinology & Infertility, Department of Obstetrics & Gynecology, University of South Alabama, USA
3New Parent World, Sparta, NJ, USA
*Corresponding Author: JE Ellington
BioOrigyn, LLC, 17206 S Spangle Creek Rd, Valleyford, WA 99036, USA
Tel: 509 448 9013
E-mail: jellington@bioorigyn.com
Received: March 09, 2017 Accepted: April 24, 2017 Published: April 29, 2017
Citation: Ellington JE, Rizk B, Criso S (2017) Antenatal Perineal Massage Improves Women’s Experience of Childbirth and Postpartum Recovery: A Review to Facilitate Provider and Patient Education on the Technique. J Womens Health, Issues Care 6:2. doi: 10.4172/2325-9795.1000266
Abstract
Vaginal delivery during childbirth is associated with perineal trauma and damage in most women. Perineal damage during delivery can have significant long-term consequences for women, including decreased quality of birthing experience, persistent postpartum perineal pain and sexual dysfunction, as well as pelvic floor pathology. Many women fear such perineal trauma. In fact, obstetrical perineal damage and its long term consequences are some of the greatest concerns of patients. Even though evidencebased outcomes show antenatal perineal massage (APM) is an effective tool to reduce perineal trauma at childbirth, education of pregnant women about and subsequent application of the intervention remains low. This review details the potential physical
and psychological benefits of APM for most women, with a focus on helping the providers educate women and staff on the technique. Additionally, the impact of partner involvement in APM is discussed. Potential discussion topics are provided, to help care providers explain the benefits of APM to their patients. Revised, more flexible patient instructions for APM are also proposed. A discussion of vaginal physiology with regard to product choice during APM is reviewed. In spite of the mention of APM in many modern medical practice guidelines, detailed information to help providers teach the technique
and to encourage patient adoption is lacking. This review provides information to make APM a more accessible choice for providers and women in order to decrease chances of perineal damage during childbirth, along with related long-term morbidities, which can deleteriously impact the patients’ quality of life.
Keywords: Antenatal perineal massage; Perineal trauma; Intact perineum; Childbirth; Obstetrics; Postpartum pain; Perineal pain; Episiotomy
Background
Vaginal delivery during childbirth is associated with perineal trauma and damage in most women. In fact, in a recent meta-analysis of 17,674 women, only one out of four women (~27%) came through labor and delivery with an intact perineum [1]. And the risk of severe obstetric perineal lacerations increases 5-fold for first-time mothers [2].
The risk of perineal trauma during childbirth is not unexpected. During crowning, the perineum distends (stretches) by 170% in the transverse (side to side) direction and 40-60% in a vertical direction (front to back) [3,4]. Recent reports indicate that the chances of coming through vaginal delivery with an intact perineum are decreased for certain groups of women (in addition to primapara) including [2,3,5-8]:
• Older women (each year of age increases tearing risk by 7%);
• Delivery of larger or mal-positioned babies;
• Ethnicity (Asian and Hispanic women have higher rates of more severe trauma);
• Lack of sexual activity during the third trimester of pregnancy;
• Use of epidural anesthesia; and
• Use of instruments during delivery.
Episiotomy, which is widely practiced to improve outcomes during childbirth, is not protective for severe perineal laceration and in some cases, may increase perineal trauma rates and delay postpartum healing [2,3,9]. Practice guidelines do not recommend the routine use of episiotomies during normal labor and delivery [10].
Perineal damage during childbirth can have significant long-term consequences for women, including: decreased quality of birthing experience and early neonatal bonding; persistent postpartum perineal pain; increased rates of sexual dysfunction (e.g. poor desire; decreased arousal and lubrication; lower orgasm rate) and dyspareunia; pelvic floor weakness; and urinary or fecal incontinence and/or sphincter weakness [2,5,11-15].
Many women fear such perineal trauma and this fear ranks high as a reason for maternal request of a Caesarian section (C-section) delivery [16,17]. However, numerous studies have shown that persistent pain one year after delivery is actually far greater for women undergoing C-section versus vaginal delivery (22% vs. 8%; p<0.001) [18]. Women should be made aware of the risk of persistent pain and possible decreased quality of life, as well as mothering disruptions from C-sections versus vaginal delivery, so that informed choices can be made. A recent lay article highlighting perineal trauma risks has received widespread media coverage “The Scary Truth about Childbirth: Having a baby left you with a horrible, debilitating, embarrassing injury? You’re not alone” [19]. Unfortunately, the article dramatically downplayed morbidities associated with C-section delivery for moms and babies. While at the same time, it dramatized the risk of perineal trauma during vaginal delivery, and offered no medical options to optimize chances of an intact perineum. One main contention of the article was that providers don’t talk to women about potential perineal damage, and that the only outcome the provider seemed to care about is acute trauma management at birthing (usually termed “primary outcomes” around perineal trauma), versus the issues women are most concerned about (often labeled as “secondary outcomes” such as childbirth experience, persistent perineal pain and sexual dysfunction) [20].
Discussing perineal anatomy and physiology during pregnancy and delivery, as well as methods to improve chances for the best outcomes, should be a conversation between every healthcare provider and patient. This can include an explanation of the different types of perineal trauma. Specifically, women have the right to know that perineal trauma after childbirth is common and categorized as either: first degree (involving the fourchette, perineal skin and vaginal mucous membranes); second degree (involving the fascia and muscles of the perineal body); third degree (involving the anal sphincter) and fourth degree (involving the rectal mucosa) [21]. Discussion of the medical choices available during labor and delivery to help preserve perineal function can follow, which explain some of the balancing act required to ensure healthy outcomes for mom and baby while trying to preserve perineal function.
Women should also be informed as to why delivery with minimal perineal trauma is an optimal goal. Patients should be educated that those who give birth with an intact perineum report less postpartum pain at both one and 90 days postpartum; greater sexual satisfaction and sensation and a greater likelihood of orgasm at six months postpartum; and less pelvic floor muscle and anal sphincter damage, as compared to women who incur significant perineal damage during childbirth [5,15,22]. Having this conversation beforehand can help women develop trust that the care provider will perform episiotomies and other interventions only if medically necessary for the patient and her baby [23]. The provider can then also use this discussion to introduce ways to increase the woman’s chances of coming through childbirth with minimal perineal trauma. Several interventions have been associated with improved postpartum perineal and sexual outcomes according to recent meta-analysis reviews. These can include something as simple as maintaining sexual activity during pregnancy (there was a 20% increase in severe trauma for women who did not have sex in their third trimester; P<0.001).(5, 13) It can also include teaching about the use of digital antenatal perineal massage (APM) from approximately 35 weeks of gestation, to minimize perineal trauma and future pain (overall reduction in incidence of trauma p=0.0007; number needed to benefit=15) [20].
Specifically, a recent Cochrane review reported that APM reduced the incidence of perineal trauma at childbirth requiring suturing (mainly because of lower episiotomy rate); and the levels of postpartum pain at three months (regardless of whether or not an episiotomy was done) [20]. The report further stated that “Although there is some transient discomfort in the first few weeks, (APM) is generally well accepted by women. As such, women should be made aware of the likely benefit of perineal massage and provided with information on how to massage.” Benefits of APM appear to include both: 1) an increase in flexibility and elasticity of perineal tissues thereby decreasing severe tearing and/or the need for episiotomy; and 2) the method of helping women desensitize and relax through the unique sensations of perineal burning and pain that will be associated with labor.
The recent meta-analysis on the benefits of using APM to decrease perineal damage has been relied on to draft medical guidelines supporting a beneficial role of APM to lessen postpartum perineal morbidities [10,24-26]. However, many of these guidelines have focused mostly on the physiologic aspect of increasing perineal muscle flexibility to decrease trauma during birthing. Data on the benefits of APM for the woman’s psychological experience of childbirth, and her long-term pelvic and sexual health have not been as widely reported. While damage to the perineum is a critical event to be minimized, the secondary outcomes (as consequences of the perineal trauma) are actually the outcomes that women are most concerned about.Understanding the link between optimizing chances of an intact or less severely traumatized perineum and a positive birth experience or quicker postpartum recovery, can help motivate women to adopt the somewhat invasive, yet preventative perineal massage techniques. Reviewing these secondary outcomes, as well as the primary ones, may give healthcare providers better discussion tools for why and how APM can be beneficial for their obstetric patients.
APM improves perineal outcomes for both primapara and multipara
With regard to evidence for decreasing perineal trauma, a benefit of APM has been reported as a reduction in perineal trauma requiring suturing following vaginal birth, mostly through a reduction in the number of women having an episiotomy (p=0.007) [20]. This reduction was significant for women who had never had a vaginal delivery before (“primapara”; p=0.00067). For multiparous women, only limited data from one study (n=245 treatment arm) were available, with inadequate power to determine if a benefit of APM existed for these women. This finding has been incorrectly reported in some medical literature as a finding against the use of APM in multiparous women; however, this interpretation fails to take into account the improved secondary, long term benefit of APM in this sub-group. Specifically, for women who have previously had a vaginal delivery, APM significantly decreased the likelihood of perineal pain 90 days postpartum, whether they had had an episiotomy during delivery or not (p=0.02)[20].
More frequent APM leads to less postpartum pain
The 2013 meta-analysis also reported a significant increase in the incidence of an intact perineum for women who massaged less than 1/3 of the assigned days (assigned days=4 to 7 days/week) versus control women (p=0.01), primarily through a decrease in the episiotomy rate [20]. Oddly, this difference became only a trend for women who massaged more than 2/3 of the assigned days (p=0.13). However, in further communications, the review author states, “the original papers (and this analysis) are underpowered to reach conclusions that more frequent massage is ineffective… Generally, higher frequency of massage had similar point estimates (to lower frequency), but the confidence intervals crossed 1 (RR 0.94; 95% CI 0.86 to 1.02)”. (Personal Communication MM Beckmann 2017) Unfortunately, the lack of power in this analysis has been reported in some medical literature as a finding against more frequent massage. But in actuality, the reported secondary outcome does show a benefit of more frequent APM for women. In fact, the sub-group of women who massaged the most frequently (e.g. more than 2/3 of the days), showed the most benefit in terms of perineal pain reduction at 90 days (p=0.003). In conclusion, the meta-analysis found that “women who massage the most frequently may not be able to further reduce their chance of an episiotomy (versus women who massage less frequently) but may lessen their likelihood of perineal pain at three months.” The one study used in the meta-analysis that directly compared outcomes for women who massaged with more (>2/3 of assigned days) versus less frequency (<1/3 of days), also reported a dose dependent increase (p=0.03) in the percentage of women with an intact perineum (28% for most frequency of APM, 20% for least frequency of APM, 15% for controls). In follow up communications, the author noted, “In my opinion, perineal massage is like stretching of any other muscles. If you do it 3-4 times per week, or even more, you will get better flexibility than if you do it only once a week.” (Personal Communication, M Labrecque 2017) Women were in high agreement (88%) that they noticed the increased elasticity of the perineum as they performed regular APM [27].
APM increases sense of control during labor
During delivery, crowning is the critical moment that determines if tearing will occur or not. The communication between the healthcare provider and the woman, as well as an understanding of the physiologic events can help determine the outcome [23] Medical protocols with strict time limits during delivery, and women who push on demand of the medical staff versus when they feel a physiologic urge, may result in more tearing [23,28,29]. In fact, a recent study found that increasing the allowed labor time in primapara by 50% (from 2 to 3 hours) decreased C-section rates by more than half, without increasing adverse outcomes [28]. A slower, more controlled Stage 2 labor and delivery may allow perineal tissues to stretch, resulting in less perineal trauma without harming neonatal or maternal outcomes [3,28]. Interestingly, in the meta-analysis review of APM, Stage 2 labor times were increased in women who practiced massage most frequently (>2/3 of assigned days; p=0.02) [20]. Mean Stage 2 labor times increased for this group from 87 to 103 minutes (still within the definitions of normal labor times). The author proposed that women who regularly practiced APM may have become motivated to achieve a vaginal birth with an intact perineum, and may have been willing to work with their provider to slow down the labor process and resist an episiotomy unless medically required.
Overall, women who practice APM had a higher sense of control during childbirth than women who did not massage (e.g. the Labour Agentry Score; p=0.03) [30,31]. These women also reported they felt more positive about their “preparation for childbirth” (p<0.001) and a sense of pride in doing childbirth their “own way” (p=0.014) [32]. Most women agreed that APM helped prepare them for childbirth psychologically (80%) and physically (86%) [31]. Enthusiasm about the technique was highly correlated to how frequently they performed the massage (more massage equaled more enthusiasm), which also correlated with a lower rate of perineal trauma (p<0.001) [25,27]. Learning pelvic floor control during massage, including volitional relaxation of the perineum; and becoming desensitized to the burning sensations during perineal stretching are important benefits of APM [29]. Between 70% and 90% of women who used APM in preparation for labor, report that they would do the technique again and 60-87% would recommend it to another pregnant woman [7,31-33]. Midwives report that APM helps patients develop collaboration with the attendant for a slow, controlled delivery [29]. In fact, 57% of women agreed that APM helped them control delivery of the baby’s head [27].
In some literature, concerns are expressed that because APM isn’t 100% effective against perineal damage, women will become distressed if they don’t deliver without tearing. In fact, approximately three out of four women report they would use APM again in a future pregnancy, even though at least half of these women would not have come through delivery with an intact perineum [31]. This suggests that the benefits of APM are multi-factorial for women. The metaanalysis on APM reached the conclusion that “Most women find the practice of perineal massage acceptable and believe it helps them prepare for birth” [20].
APM is not associated with negative outcomes from “overstretching”
It is important for women to know that APM does not decrease perineal strength over time or cause an enlarged vaginal opening [27]. Like most muscle massage, the muscle is not lengthened during APM, but the elasticity is improved, as noticed by women practicing APM [25,27]. Reassuringly, APM did not increase postpartum fecal or urinary incontinence or decrease sexual satisfaction of the woman or her male partner after childbirth [12]. In fact, anal sphincter occult damage tended to be lower after childbirth for women over 30 who had practiced APM (p=0.07). Times to return to sexual function were the same for both women who do or do not practice APM [12].
Educating staff and women about APM determines success
Helping women adopt and comply with the APM technique can be a challenge. Over 50% of women felt that learning the technique was difficult [34]. And in most studies, only between 33% and 66% of women complied with the massage protocol as suggested [7,31,34]. Adoption was strongly correlated with instruction type (p<0.001), with childbirth class being better than no training and one-on-one midwife training being better than a classroom setting [29,34]. Use of a phone app to help women comply with APM instructions has recently been shown to be of interest to women [34].
Women commented that in the first few weeks, massage could be uncomfortable or unpleasant and even produced a painful or burning sensation [27]. This pain dissipated by the second or third week of massage, after which some women found the massage relaxing and easy. Learning to breathe and relax through the unusual sensation of perineal stretching is, of course, one of the benefits of APM. A majority of women (69%) reported that APM was useful for delivery by improving suppleness of the vaginal opening and increasing their tolerance for the burning discomfort during stretching [27].
Women who discontinued APM before childbirth reported several consistent concerns: resistance to touching themselves; a lack of knowledge about the technique; stickiness of provided oils; difficulty finding the right technique with a large abdomen or long fingernails; and cramping or tiring of the fingers or thumbs [27,34]. It is likely that discussing APM earlier than 34 weeks, before a large belly makes it difficult, could help women experiment with the technique. New instructions are proposed by the authors of this review (See Appendix), to better explain the goal of APM (pelvic floor relaxation and desensitization) and to encourage women to find the position and technique that works best for them, rather than an overly rigid approach [29,35].
Medical staff may have concerns about discussing APM with patients. However, more than half of women found the concept of APM acceptable, with only 25% finding the topic embarrassing [36]. Nevertheless, only one in six midwives regularly advised women about the benefits of APM [37]. Many providers may wait for the woman to bring up APM, but general knowledge among the lay public regarding the technique remains low at about 30% with only 11% knowing the correct time during pregnancy to start APM, and that it needs to be done regularly for best benefit [12].
Incorporating APM as part of best practice antenatal guidelines in clinics and institutions can increase awareness of, and enthusiasm for, APM as part of “evidence-based practice of management of perineal pain” [38]. Such incorporation of training and education in clinical settings, led to between 50 and 100% of women being specifically educated about APM, with a patient adoption rate of about 50%, and significant decreases in perineal trauma rates and postpartum perineal pain scores [37].
Many women value involving their partner in APM
Over half of women performed the APM with their partner [31]. A similar percentage of women reported that the partners involvement was important to them during massage (61%), and that the APM drew the couple closer together (55%) [27]. Women tended to report the APM was easier and more relaxing to do with a partner. And a benefit of motivation to comply with the schedule was found for partnered massage, although, some women did prefer to do the technique alone. Teaching the couple as a unit about APM can be beneficial, but is not required, as the technique can be equally successful when done by women themselves.
Sexual function and desire decrease in some women during the third trimester of pregnancy as compared to the first and second trimesters [39]. For some couples, APM may increase intimacy and can even lead to love-making. For other couples, it may cause tension around differing sexual desires. But given the association between women who are more sexually active during the third trimester of pregnancy and lower rates of severe perineal trauma during childbirth (p<0.001), couples should not be discouraged from allowing APM to transition into intimacy [5]. Couples can benefit from knowing about the association between a lack of sexual activity in the third trimester and more severe perineal trauma at childbirth, and then the subsequent link between perineal damage and higher levels of postpartum sexual dysfunction [5,22,39]. APM should be taught to couples (where the partner is welcomed by the woman), in a playful way that encourages experimentation to achieve the goals of stretching and perineal relaxation. The wife can read to the husband during the massage, or they can use the time to make plans (e.g. plan a vacation, review baby names, plan for the nursery). The couple should understand that the massage can enhance pair bonding [27].
Summary of potential benefits of APM on women’s health outcomes
Many studies on APM were not included in the recent metaanalysis because of: lack of randomization (women either wanted to be in the massage arm when they learned of it, or they stated they wouldn’t do massage even if assigned to treatment); high episiotomy rates across treatments obscuring any potential treatment effect; or lack of blinding for practitioners evaluating perineal trauma [20]. Even for studies included in the meta-analysis, only a subset of women (33%-66%) performed APM in 2/3 or more of the assigned days, which may have biased against the treated group [7,31,34,40]. However, a review of the findings from these additional studies and newer studies (since published), shows further consistency with the findings of the reports incorporated into the meta-analysis. The findings from studies used in the meta-analysis are italicized below. Data from additional supportive studies are not italicized.
Intact perineum rates
Increased intact perineum from 25% to 31% (p=0.07) [7].
Subgroup benefit for primapara over 30 yrs. decrease in tears of 12% (p=0.019)
Increased intact perineum from 12% to 19% (p=0.002) [31].
Subgroup benefit for primapara from 15% to 24% (p=0.001)
Subgroup benefit for increasing massage from <1/3 to >2/3 of days; 20% to 28% (p=0.003)
Increased intact perineum for multiparous women with previous episiotomy 35% to 64% (p=0.05) [41].
Decreased Episiotomies and/or Severe Lacerations (2nd degree or more)
Decreased severe trauma from 62% to 40% (p=0.03) [42]
Decreased episiotomy rate from 37% to 16% (p=0.09) [42]
Decreased severe lacerations from 60% to 29% (p<0.001) [43]
Decreased episiotomies from 43% to 24% (p=0.03) [43]
Decreased Postpartum Perineal Pain
Decreased perineal pain for multiparous women at 3 months postpartum (p=0.01) [12]
Decreased perineal pain scores at 1 and 15 days postpartum. (p<0.001) [43]
Improved perineal healing (REEDA Scale) at 1 and 15 days postpartum (p<0.001) [43]
Decreased perineal pain, day 3 postpartum (p=0.03) [40]
Improved Feelings About Childbirth
Higher confidence and control scores about labor and delivery (p=0.03) [27]
Frequency of APM related to how well it helped prepare for labor (p<0.0001) [27]
Higher sense of preparation for childbirth (p=0.001) [34]
Higher sense of self-efficacy (success and cont rol during childbirth); (p=0.014) [34]
Optimizing APM for patients
Open communication between healthcare providers and patients in order to teach the benefits of APM is a first step in helping women succeed at the technique. Older diagrams in APM instructions were difficult to understand and failed to accommodate a woman’s changing body or fatigue with the technique. New instructions adapted from several sources are presented in the Appendix to better help women understand the goals of APM and to give a variety of positions for ease of practice [35]. Patients should be encouraged to start APM at 34 or 35 weeks of pregnancy, although introducing the concept during early discussions on approach to pregnancy and birth plan development may be of benefit. Providing educational material on how to do APM prior to the last month of pregnancy can allow a woman to discuss the technique with other women and her partner. It can also encourage a discussion of the benefits of shorter fingernails for the woman during APM and later in caring for a newborn [44].
Most APM studies have recommended that massage be done daily, or at least 4 times per week [7,31,34]. Women should be educated on the decreased postpartum pain risk and potential for less perineal trauma found with increasing massage frequency. A vast majority of women (90%) agreed that APM did not require “much time” [27]. It is also important for women to know if they miss a day or two of massage, they should just return to the practice, and to call the clinic for support if they are having difficulty with the APM technique.
Tissue hydration for a gentle, lubricating massage helps create supple perineal tissues and allows for deeper stretching. Previously plant and nut-based oils or water-soluble lubricants have been recommended for APM [7,31,34,40]. However, it is critical to avoid inflammation and bacterial dysbiosis in pregnant women, to prevent bacterial vaginosis (BV) or other risk factors for inferior maternal and neonatal outcomes. Specifically, cytokine and inflammasome production in the vagina through vaginal product use has been associated with increased rates of BV [45,46]. So consideration of the products to be used during APM is warranted (e.g. not all products may meet the guideline of “do no harm”).
Over the past five years, significant advances have been made in understanding normal vaginal physiology and pathology [45-52]. Many of these advances have been through study of the impact of vaginal products and their ingredients on the vaginal mucosa and microbiome in sexually transmitted disease research [53-57]. A growing body of evidence has found that common vaginal products (e.g. KY Jelly, Astroglide) and/or specific ingredients in these products (e.g. glycerin, propylene glycol, parabens) can be toxic to vaginal ecosystem cells, including mucosal cells and beneficial acidproducing bacteria [53-57]. Such products increase interleukin and inflammasome production, thereby damaging mucosal cells and lactobacilli. Some of this toxicity appears to be related to hyperosmotic formulations of many vaginal products, and some a direct effect of specific ingredients. In order to avoid osmotic damage to the vaginal ecosystem, the World Health Organization has suggested that vaginal products be formulated isotonic to vaginal and seminal fluids (260- 380 mOsmo/kg) [58].
Although oils are commonly used for APM, the use of oils in the vagina has been associated with an 8-fold risk in vaginal infections [59]. Use of almond oils during pregnancy has been associated with an increase in pre-term labor [60]. Also, some women found the use of oils during APM sticky and uncomfortable [12]. Of concern is the chemistry of natural oils, which break down to contain varying levels of peroxidation products and pro-inflammatory chemicals. These breakdown chemicals can alter cell and bacterial physiology when applied topically [61,62]. The levels of peroxides and related cell-toxic chemicals differ in oils based on: oil product manufacturing process, storage exposure to light and room temperature, purity and oil type [61-63]. Vitamin E in oils can act as either a pro-oxidant or an antioxidant [63]. Unfortunately, consumers and providers have no way of knowing the level of oxidation and pro-inflammatory content in any given oil-based product.
Recently, virgin coconut oil has become popular for topical application. However, coconut oil has significant antimicrobial activity, and its impact on the vaginal microbiome is unknown [61]. Coconut oil also decreases water movement across membranes [61-64]. Constant mucus production and exfoliation of the vaginal mucosal barrier is a key factor in healthy vaginal physiology [49-52]. It is unknown how coating of the mucosa with an oil that changes water permeability of the tissues may impact normal healthy vaginal function. And natural products, such as Aloe vera gel, can contain high levels of heavy metals and endotoxins [65], both of which are very potent inflammation triggers when applied topically [66-68].
An isotonic, hydrogel for perineal massage, that does not contain glycerol, oils or parabens, has recently been introduced (BabyIt, Fairhaven Health, Bellingham, WA). In invertebrate toxicity testing it was found to have mild irritation potential, as compared to KY Jelly and other lubricants, which caused moderate to severe irritation potential (Table 1) (Personal Communication, E Adriaens 2017) [54].
| Product | Osmolality (mOsm/Kg)* | Total Mucus Production (% Body Weight)** | Irritation Classification** |
|---|---|---|---|
| BabyIt Perineal Massage Gel | 270 | 6.2 ± 2.8 | Mild |
| KY Jelly | 3631 | 19.0 + 0.7 | Severe |
| Astroglide | 2299 | 38.0 + 5.5 | Severe |
| Replens | 1177 | 16.5 + 2.5 | Mild |
**Mucosal irritation potency determined using the Slug Mucosal Irritation (SMI) assay.
Table 1: Irritation Potential of an Isotonic Massage Gel versus Common Lubricants [54,56,68].
Practitioners can remain aware of new findings in vaginal physiology and the impact of products or ingredients on inflammation markers in, and damage to, vaginal mucosal cells through medical literature searches in sexually transmitted disease research. Many such publications shed significant light on women’s health, but are rarely published in traditional gynecology journals.
Health care providers can review products available for APM to help women choose the best product for their situation. Whichever hydrating product is chosen for the massage, be sure the patient uses an adequate amount and reapplies as needed to ensure a comfortable massage for the 5-minute time period suggested.
Conclusion
The authors of the 2013 meta-analysis on the benefit of APM concluded that “… women who are instructed in perineal massage (either because they become more informed about birthing, episiotomies and the advantages of an intact perineum, or because of the act of massaging itself) are less likely to have an episiotomy, require perineal suturing or report ongoing perineal pain postpartum” [20]. Additional and newer studies as reviewed here further support the use of APM to optimize women’s experience of childbirth and to improve restoration of healthy postpartum perineal function.
Carefully explaining APM as a part of evidence-based methods to decrease perineal trauma and pain will continue to demystify the technique and may improve its more widespread use. Improved acceptance of APM can be achieved by helping medical staff and women understand its potential benefits and by encouraging sharing of patients’ experience with clinic staff.
Disclosure
JE Ellington discloses that she is a named inventor on a patent application for BabyIt perineal massage gel, a product mentioned in this paper, and a consultant for the manufacturer of the product.
References
- Sandall J, Soltani H, Gates S, Shennan A, Devane D (2015) Midwife-led continuity models versus other models of care for childbearing women. Cochrane Database Syst Rev 9:Cd004667
- Monteiro VM, Pereira GM, Aguiar RA, Azevedo RL, Correia-Junior MD, et al. (2016) Risk factors for severe obstetric perineal lacerations. Int Urogynecol J27:61-67.
- Kapoor DS, Thakar R, Sultan AH (2015) Obstetric anal sphincter injuries: review of anatomical factors and modifiable second stage interventions. Int Urogynecol J26:1725-1734.
- Meriwether KV, Rogers RG, Dunivan GC, Alldredge JK, Qualls C, et al. (2016) Perineal body stretch during labor does not predict perineal laceration, postpartum incontinence, or postpartum sexual function: a cohort study. Int Urogynecol J 27:1193-1200.
- Leeman L, Rogers R, Borders N, Teaf D, Qualls C (2016) The effect of perineal lacerations on pelvic floor function and anatomy at 6 months postpartum in a prospective cohort of nulliparous women. Birth 43:293-302.
- Dahlen HG, Ryan M, Homer CS, Cooke M (2007) An Australian prospective cohort study of risk factors for severe perineal trauma during childbirth. Midwifery 23:196-203.
- Shipman MK, Boniface DR, Tefft ME, McCloghry F (1997) Antenatal perineal massage and subsequent perineal outcomes: a randomised controlled trial. Br J Obstet Gynaecol 104:787-791.
- Grobman WA, Bailit JL, Rice MM, Wapner RJ, Reddy UM, et al. (2015) Racial and ethnic disparities in maternal morbidity and obstetric care. Obstet Gynecol 125:1460-1467.
- Carroli G, Mignini L (2009) Episiotomy for vaginal birth. Cochrane Database Syst Rev:Cd000081.
- American College of Obstetricians and Gynecologists (2016) Practice Bulletin No. 165 Summary: prevention and management of obstetric lacerations at vaginal delivery: Correction. Obstet Gynecol 128:411.
- McDonald E, Woolhouse H, Brown SJ (2015) Consultation about sexual health issues in the year after childbirth: a cohort study. Birth 42:354-361.
- Labrecque M, Eason E, Marcoux S (2000) Randomized trial of perineal massage during pregnancy: perineal symptoms three months after delivery. Am J Obstet Gynecol 182:76-80.
- Leeman LM, Rogers RG (2012) Sex after childbirth: postpartum sexual function. Obstet Gynecol 119:647-655.
- Barrett G, Pendry E, Peacock J, Victor C, Thakar R, et al. (2000) Women's sexual health after childbirth. BJOG 107:186-195.
- Signorello LB, Harlow BL, Chekos AK, Repke JT (2001) Postpartum sexual functioning and its relationship to perineal trauma: a retrospective cohort study of primiparous women. Am J Obstet Gynecol 184:881-888.
- Masoumi SZ, Kazemi F, Oshvandi K, Jalali M, Esmaeili-Vardanjani A, et al. (2016) Effect of training preparation for childbirth on fear of normal vaginal delivery and choosing the type of delivery among pregnant women in hamadan, Iran: a randomized controlled trial. J Family Reprod Health 10:115-121.
- Nieminen K, Wijma K, Johansson S, Kinberger EK, Ryding EL, et al. (2017) Severe fear of childbirth indicates high perinatal costs for Swedish women giving birth to their first child. Acta Obstet Gynecol Scand 96: 438-446.
- Kainu JP, Halmesmaki E, Korttila KT, Sarvela PJ (2016) Persistent pain after cesarean delivery and vaginal delivery: a prospective cohort study. Anesth Analg 123:1535-1545.
- Butler K (2017) The scary truth about childbirth. Mother Jones.
- Beckmann MM, Stock OM (2013) Antenatal perineal massage for reducing perineal trauma. Cochrane Database Syst Rev:Cd005123.
- Woodman PJ, Graney DO (2002) Anatomy and physiology of the female perineal body with relevance to obstetrical injury and repair. Clin Anat 15: 321-334.
- Ahmed WAS, Kishk EA, Farhan RI, Khamees RE (2016) Female sexual function following different degrees of perineal tears. Int Urogynecol J.
- Lindgren HE, Brink A, Klinberg-Allvin M (2011) Fear causes tears - perineal injuries in home birth settings. A Swedish interview study. BMC pregnancy childbirth 11:6.
- Seehusen DA, Raleigh M (2014) Antenatal perineal massage to prevent birth trauma. American family physician 89:335-336.
- Van Kampen M, Devoogdt N, De Groef A, Gielen A, Geraerts I (2015) The efficacy of physiotherapy for the prevention and treatment of prenatal symptoms: a systematic review. Int Urogynecol J 26:1575-1586.
- Hastings-Tolsma M (2014) Antenatal perineal massage decreases risk of perineal trauma during birth. Evidence-based Nursing 17:77.
- Labrecque M, Eason E, Marcoux S (2001) Women's views on the practice of prenatal perineal massage. BJOG 108:499-504.
- Gimovsky AC, Berghella V (2016) Randomized controlled trial of prolonged second stage: extending the time limit vs usual guidelines. Am J Obstet Gynecol 214: 361-366.
- Jones LE, Marsden N (2008) The Application of antenatal perineal massage: a review of literature to determine instruction, dosage and technique. J Assoc Chartered Physiotherapists Womens Health 102:8-11.
- Hodnett ED, Simmons-Tropea DA (1987) The Labour Agentry Scale: psychometric properties of an instrument measuring control during childbirth. Research in Nursing & Health 10:301-310.
- Labrecque M, Eason E, Marcoux S, Lemieux F, Pinault JJ, et al. (1999) Randomized controlled trial of prevention of perineal trauma by perineal massage during pregnancy. Am J Obstet Gynecol 180:593-600.
- Takeuchi S, Horiuchi S (2014) Why don't pregnant women practice antenatal perineal massage?: An empirical investigation. J Japan Acad Midwifery 28:173-182.
- Mei-dan E, Walfisch A, Raz I, Levy A, Hallak M (2008) Perineal massage during pregnancy: a prospective controlled trial. Isr Med Assoc J 10: 499-502.
- Takeuchi S, Horiuchi S (2016) Randomised controlled trial using smartphone website vs leaflet to support antenatal perineal massage practice for pregnant women. Women Birth 29:430-435.
- Oxford University Hospitals NHS Trust (2017)Antenatal perineal massage: information for women.
- Ismail SI, Emery SJ (2013) Patient awareness and acceptability of antenatal perineal massage. J Obstet Gynaecol33:839-843.
- Gomme C, Sheridan M, Bewley S (2003) Antenatal perineal massage: Part 1. British J Midwifery 11:707.
- Zhang Y, Huang L, Ding Y, Shi Y, Chen J, et al. (2017) Management of perineal pain among postpartum women in an obstetric and gynecological hospital in China: a best practice implementation project. JBI Database of Systematic Reviews and Implementation Reports 15:165-177.
- Ninivaggio C, Rogers RG, Leeman L, Migliaccio L, Teaf D, et al. (2016) Sexual function changes during pregnancy. Int UrogynecolJ.
- Eogan M, Daly L, O'Herlihy C (2006) The effect of regular antenatal perineal massage on postnatal pain and anal sphincter injury: a prospective observational study. J Matern Fetal Neonatal Med 19:225-229.
- Davidson K, Jacoby S, Brown MS (2000) Prenatal perineal massage: preventing lacerations during delivery. J Obstet Gynecol Neonatal Nurs 29:474-479.
- Shimada M (2005) A randomized controlled trial on evaluating effectivenss of perineal massage during pregnancy in primiparous women. J Jpn Acad Nurs Sci 25:22-29.
- Haef A (2015) Effects of prenatal perineal massage and kegel exercise on the episotomy rate. Journal of Nursing Health Science 4:61-70.
- Muschick KD, LaCroix R, McAdams J (2016) Fingernail carriage of methicillin-resistant staphylococcus aureus and possible correlation with soft tissue infections in children. South Med J 109:236-239.
- Alcaide ML, Rodriguez VJ, Brown MR, Pallikkuth S, Arheart K, et al. (2017) High levels of inflammatory cytokines in the reproductive tract of women with bv and engaging in intravaginal douching: a cross-sectional study of participants in the women interagency HIV study. AIDS Res Hum Retroviruses.
- Fashemi B, Delaney ML, Onderdonk AB, Fichorova RN (2013) Effects of feminine hygiene products on the vaginal mucosal biome. Microb Ecol Health Dis 24: 10.
- Hickey RJ, Zhou X, Pierson JD, Ravel J, Forney LJ (2012) Understanding vaginal microbiome complexity from an ecological perspective. Transl Res160:267-282.
- Anahtar MN, Byrne EH, Doherty KE, Bowman BA, Yamamoto HS, et al. (2015) Cervicovaginal bacteria are a major modulator of host inflammatory responses in the female genital tract. Immunity 42:965-976.
- Mirmonsef P, Modur S, Burgad D, Gilbert D, Golub ET, et al. (2015) Exploratory comparison of vaginal glycogen and Lactobacillus levels in premenopausal and postmenopausal women. Menopause 22:702-709.
- Oh JE, Kim BC, Chang DH, Kwon M, Lee SY, et al. (2016) Dysbiosis-induced IL-33 contributes to impaired antiviral immunity in the genital mucosa. Proc Natl Acad Sci USA 113:E762-E771.
- Shukair SA, Allen SA, Cianci GC, Stieh DJ, Anderson MR, et al. (2013) Human cervicovaginal mucus contains an activity that hinders HIV-1 movement. Mucosal Immunol 6:427-434.
- Nunn KL, Wang YY, Harit D, Humphrys MS, Ma B, et al. (2015) Enhanced trapping of hiv-1 by human cervicovaginal mucus is associated with lactobacillus crispatus-dominant microbiota. mBio 6:e01084-15.
- Gali Y, Delezay O, Brouwers J, Addad N, Augustijns P, et al. (2010) In vitro evaluation of viability, integrity, and inflammation in genital epithelia upon exposure to pharmaceutical excipients and candidate microbicides. Antimicrob Agents Chemother 54:5105-5114.
- Adriaens E, Remon JP (2008) Mucosal irritation potential of personal lubricants relates to product osmolality as detected by the slug mucosal irritation assay. Sex Transm Dis35:512-516.
- Dezzutti CS, Brown ER, Moncla B, Russo J, Cost M, et al. (2012) Is wetter better? An evaluation of over-the-counter personal lubricants for safety and anti-HIV-1 activity. PLoS One 7:e48328.
- Cunha AR, Machado RM, Palmeira-de-Oliveira A, Martinez-de-Oliveira J, das Neves J, et al. (2014). Characterization of commercially available vaginal lubricants: a safety perspective. Pharmaceutics 6:530-542.
- Hu M, Zhou T, Dezzutti CS, Rohan LC. (2016). The Effect of commonly used excipients on the epithelial integrity of human cervicovaginal tissue. AIDS Res Hum Retroviruses32:992-1004.
- World Health Organization (2012) Use and procurement of additional lubricants for male and female condoms: WHO/UNFPA/FHI. Geneva, Switzerland.
- Brown JM, Hess KL, Brown S, Murphy C, Waldman AL, et al. (2013) Intravaginal practices and risk of bacterial vaginosis and candidiasis infection among a cohort of women in the United States. Obstet Gynecol 121:773-780.
- Facchinetti F, Pedrielli G, Benoni G, Joppi M, Verlato G, et al. (2012) Herbal supplements in pregnancy: unexpected results from a multicentre study. Hum Reprod 27:3161-3167.
- Verallo-Rowell VM, Katalbas SS, Pangasinan JP (2016) Natural (mineral, vegetable, coconut, essential) oils and contact dermatitis. Curr Allergy Asthma Rep 16:51.
- Zarate J, Goicoechea E, Pascual J, Echevarria E, Guillen MD (2009) A study of the toxic effect of oxidized sunflower oil containing 4-hydroperoxy-2-nonenal and 4-hydroxy-2-nonenal on cortical TrkA receptor expression in rats. Nutr Neurosci 12:249-259.
- Auezova L, Saliba C, Hajj-Moussa E, Hosry LE, Yammine S, et al. (2012) A methodological approach to study almond oil stability in relation to α-tocopherol supplementation. Food and Nutrition Sciences 3:1710-1715.
- Noor NM, Khan AA, Hasham R, Talib A, Sarmidi MR, et al. (2016) Empty nano and micro-structured lipid carriers of virgin coconut oil for skin moisturisation. IET nanobiotechnology 10:195-199.
- Posadzki P, Watson L, Ernst E (2013) Contamination and adulteration of herbal medicinal products (HMPs): an overview of systematic reviews. Eur J Clin Pharmacol 69:295-307.
- Harijith A, Ebenezer DL, Natarajan V (2014) Reactive oxygen species at the crossroads of inflammasome and inflammation. Front Physiol 5:352.
- Baker B, Geng S, Chen K, Diao N, Yuan R, et al. (2015) Alteration of lysosome fusion and low-grade inflammation mediated by super-low-dose endotoxin. J Biol Chem 290:6670-6678.
- Begay O, Jean-Pierre N, Abraham CJ, Chudolij A, Seidor S, et al. (2011) Identification of personal lubricants that can cause rectal epithelial cell damage and enhance HIV type 1 replication in vitro. AIDS Res Hum Retroviruses 27:1019-1024.
Appendix
| Instructions for Perineal Massage During Pregnancy |
| Perineal massage during pregnancy is the gentle, manual stretching and massage of the back portion of the birth canal (the perineum), which is located between the vaginal opening and the rectum. There is good medical evidence that when done regularly, in the last 3 to 4 weeks of pregnancy, perineal massage can increase your chance of delivering a baby vaginally without tearing or damaging your perineum (including a decreased risk of episiotomy). Of course, perineal massage can’t totally remove any chance of perineal trauma, but it has been shown to decrease the chances of lasting damage to the perineum, which can negatively impact a woman’s quality of life and sexual health after having children. |
| Regular perineal massage during pregnancy also decreases your risk of developing postpartum pain. Women who practice this massage, also report feeling more confident and in control of their childbirth experience. Doing perineal massage during pregnancy helps women learn to relax and breathe through the burning sensation of perineal stretching (which is a natural part of childbirth). Perineal massage can be practiced by couples together or done on your own. Many women find that doing the massage with a partner makes it easier to do regularly and enhances bonding between the couple. |
| How to Perform Perineal Massage On Your Own The beneï¬Ã‚Âts of perineal massage can be achieved with as little as 5 minutes of massage each day or at least 4 times per week. Begin your regular massage routine at 34 to 35 weeksofpregnancy, after discussing it with your health care provider. Sticking to a regular massage schedule is best to promote greater elasticity of the tissues in the perineum. Don’tworry ifyoumissaday or two -justpickupthe next day. |
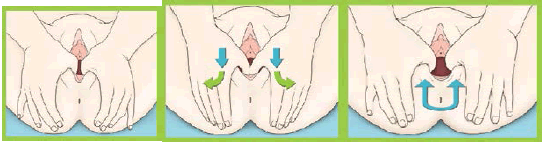
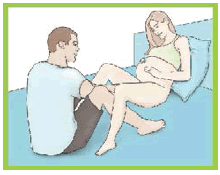
| 1.Before beginning perineal massage, wash your hands and trim your nails. 2.Find a comfortable position that allows you to reach your perineum, by reaching your hands in front of or behind you. Positions that work well include: a) Sitting propped up in bed with your knees bent; b) raising one leg such as on a shower bench or toilet; or c) squatting against a wall for support with or without the aid of a stack of books or a stool. Feel free to use diï¬Ã‚€erent positions on diï¬Ã‚€erent days or even change positions during your massage on any given day, if you become uncomfortable or tired.
4. Perineal massage may be done with your thumbs, or with your index or middle fingers. To start, insert your thumbs or fingers about one to two inches inside the vagina, resting your palms against your legs or bottom (depending on the position you choose). 5. Begin the massage by stretching the tissues at the back portion of the vaginal birth canal towards the rectum and also apart side-to-side, gliding down and out, and then back again during the massage. 6. You will continue the massage for up to 5 minutes, reapplying massage gel as needed.
8. Perineal massage should not be painful, but during the first couple of weeks it is normal to feel a slight uncomfortable burning or stretching sensation. Practicing awareness and breathing when you feel this discomfort will help you feel more in control when you feel these same sensations during delivery! Over time, increase the pressure you use during the massage, as you feel the tissue become less rigid and more elastic and flexible. |
|
How to Perform Perineal Massage with Your Partner
4. Women who have more sexual activity during the third trimester of pregnancy also have less chance of severe perineal trauma during delivery, and better sexual satisfaction after childbirth. As long as you are cleared for sexual activity by your healthcare provider (and a vast majority of women are), if perineal massage becomes erotic and leads to love-making, that is just fine! |
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi