Research Article, Biomater Med Appl Vol: 9 Issue: 1
Comparison of Stability on Screw Placement with or without Polymethyl Methacrylate Filling in Porcine Mandible
Panchanok Janphong and Settakorn Pongpanich*
Department of Oral and Maxillofacial Surgery, Prince of Songkla University, Songkhla, 90110, Thailand
*Corresponding Author: Settakorn Pongpanich
Department of Oral and Maxillofacial Surgery, Prince of Songkla University, Songkhla, 90110, Thailand
E-mail: settakorn@gmail.com
Received date: 06 August, 2024, Manuscript No. BMA-24-144624;
Editor assigned date: 08 August, 2024, PreQC No. BMA-24-144624 (PQ);
Reviewed date: 22 August, 2024, QC No. BMA-24-144624;
Revised date: 28 February, 2025, Manuscript No. BMA-24-144624 (R);
Published date: 09 February, 2025, DOI: 10.35248/2577-0268.1000538
Citation: Janphong P, Pongpanich S (2025) Comparison of Stability on Screw Placement with or without Polymethyl Methacrylate Filling in Porcine Mandible. Biomater Med Appl. 9:1.
Abstract
Objective: To compare the stability of screw placement with or without Polymethyl Methacrylate (PMMA) in the porcine mandible.
Materials and Methods: A total of 13 porcine hemimandibles underwent Cone-beam 3D computed tomography for screw hole selection. One screw hole was determined on each hemimandible without overlapping vital structures. A 1.6 mm-diameter drill operated to a depth of 3 mm. Subsequently, 13 miniscrews (2.0 mm diameter, 5.5 mm length) were tightened. A dental implant stability meter (AnyCheck) recorded the IST values at the medial, distal and inferior sides of each miniscrew. To investigate loosened miniscrew stability, they were removed, and the 1.8 mm-diameter drill and miniscrews were used. IST values were recorded again. Lastly, after miniscrew removal, Haraeus Palacos® R+G PMMA was applied (1 ml per screw hole). Miniscrews were inserted and IST was recorded after 5 minutes for PMMA setting. All PMMA specimens were scanned.
Results: The median IST in the PMMA group significantly exceeded the loosening miniscrews group in all measured directions (p<0.05). There were no significant differences between the PMMA group and the tightened miniscrews group in all measured directions (p>0.05). Additionally, PMMA spread locally through cancellous bone from 1.3 mm to 3.3 mm using radiograph.
Conclusion: PMMA effectively restored primary stability of loosening miniscrews in the porcine mandible.
Keywords: Polymethyl Methacrylate (PMMA), Bone cement, Miniscrews, Stability, Mandible, Facial bone fracture, Othognathic surgery
Introduction
Internal fixation using miniplates and screws remains one of the surgical management options for maxillofacial bone fractures, including orthognathic surgery [1]. Some studies revealed that half of hardware complications required removal due to issues such as hardware loosening, nonunion, broken hardware, and severe pain [2-5]. Loosening screw could occasionally happen due to oversized bone drilling and complications from instability of the bone segments might be revealed. Typically, this could be corrected in the operative field with an emergency screw that had a larger outer thread diameter. Nevertheless, the emergency screw still might be loose and furthermore, space might be unavailable for a new position of the plate and screw fixation. Using bone cement for the loose screw fixation might be a solution. Currently, the most common bone cement is Polymethyl Methacrylate (PMMA), which is part of synthetic group. The advantages of this material are high bond strength, bone space filler and long bone adhesion [6].
The aim of this study being to investigate whether applying the bone cement to the hole of loose screw restores retention to acceptable level thus providing alternative to inserting a larger screw.
Materials and Methods
Study design/Sample
This was an in vitro experimental study performed in one day. Thirteen hemimandibles were obtained from porcine (average weight 50 kg) that had all been grown under similar settings. All specimens were stored at -20ºC with moisture. The sample size was analyzed by using the statistical software G*power, based on a previous study from Cankaya et al., [7]. The project was approved as non-human research by the research ethics community, Prince of Songkla University (No: NH6605-008). The study was divided into the pre-experimental procedure and the experimental procedure.
Pre-experimental procedure
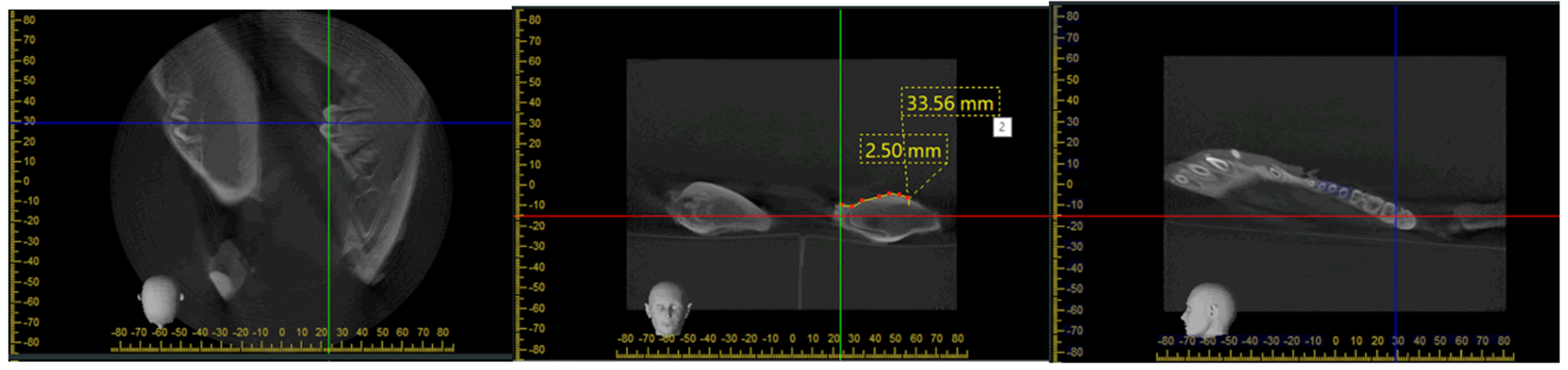
All specimens were scanned using a Cone-beam 3D computed tomography (3D Accuitomo®, Morita Co.) with Field of View (FOV) of 170 × 120 mm. For screw hole selection, each hemimandible was measured buccal cortex widths in axial, coronal and sagittal planes. The screw hole selection must be within the range of 1.98 mm-2.38 mm of buccal cortex width. One screw hole was determined on each hemimandible without overlapping dental roots or mental foramen (Figure 1).
Experimental procedure
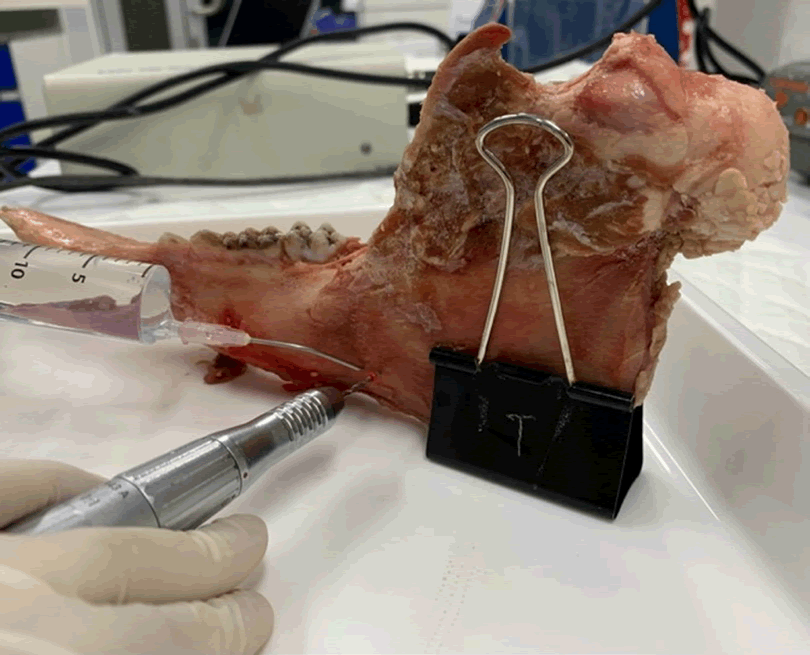
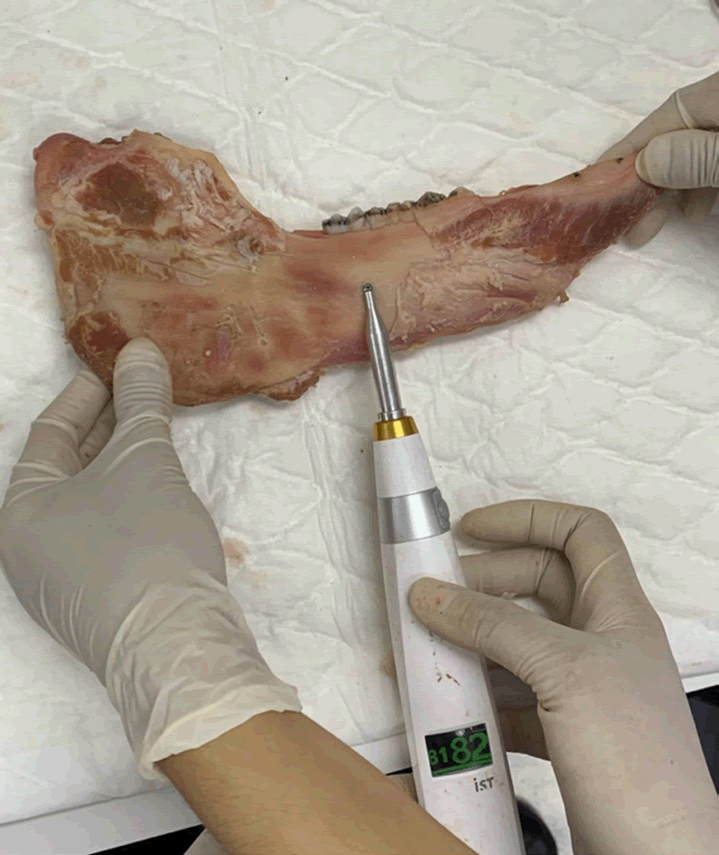
To create a screw hole, a drill with a 1.6 mm diameter (Medicon eG®) with a stopper was operated at 1,500 rpm to a depth of 3 mm at the screw hole marking. Normal saline was irrigated to the bone during drilling. Then, a mechanical screwdriver (Medicon eG®) was used to tighten 13 miniscrews, each 2.0 mm in diameter and 5.5 mm long (Medicon eG®) into the drilled holes. Next, AnyCheck® (IMT-100, DMS Co.,LTD.) was used to check the stability of the miniscrews, and the Implant Stability Test (IST) values were recorded at the medial, distal, and inferior sides of each miniscrew. From AnyCheck® instruction, IST values of 1-64 represented low stability, and IST values above 65 represented high stability. The measured values were calculated with scale increases by 4 according to screw height of 2 mm above the bone when operated (Figures 2 and 3).
To investigate the stability of the loosened miniscrews, all miniscrews were removed. In the same screw holes, the drill with a 1.8 mm diameter and stopper was operated again with irrigated normal saline at the same rate and depth. The same miniscrews were applied in the screw holes. Then, the IST value was recorded again.
In the final experiment, after removing the loosened miniscrews, an entire batch of Haraeus Palacos® R+G PMMA including 41.1 g of powder and 20 ml of liquid, was manually mixed for 3 mins with a bowl and spatula, according to the manufacturer's recommendations. Subsequently, 1 ml of the PMMA mixture was applied to all screw holes with a spatula. Afterward, the same miniscrews were put in and excess bone cement was removed. The IST was recorded after 5 mins to observe the PMMA setting.
Finally, all specimens with PMMA were scanned using a Conebeam 3D computed tomography to study the flow of PMMA-related cortical bone and cancellous bone.
Figure 1: A screw hole selection and reference point on each hemimandible.
Figure 2: A screw hole preparation with drill 1.6 mm in diameter and stopper on hemimandible.
Figure 3: IST value measurement with AnyCheck on miniscrew in inferior direction.
Data analyses
The statistical analysis was performed using SPSS (version 13, SPSS). p<0.05 was considered statistically significant. The IST value was presented as the median and Standard Deviation (SD). Differences in IST values between the dependent groups of the loosening miniscrews group and the PMMA group were analysed using Wilcoxon signed rank test due to non-normal distributions of data.
Result
Stability test outcome
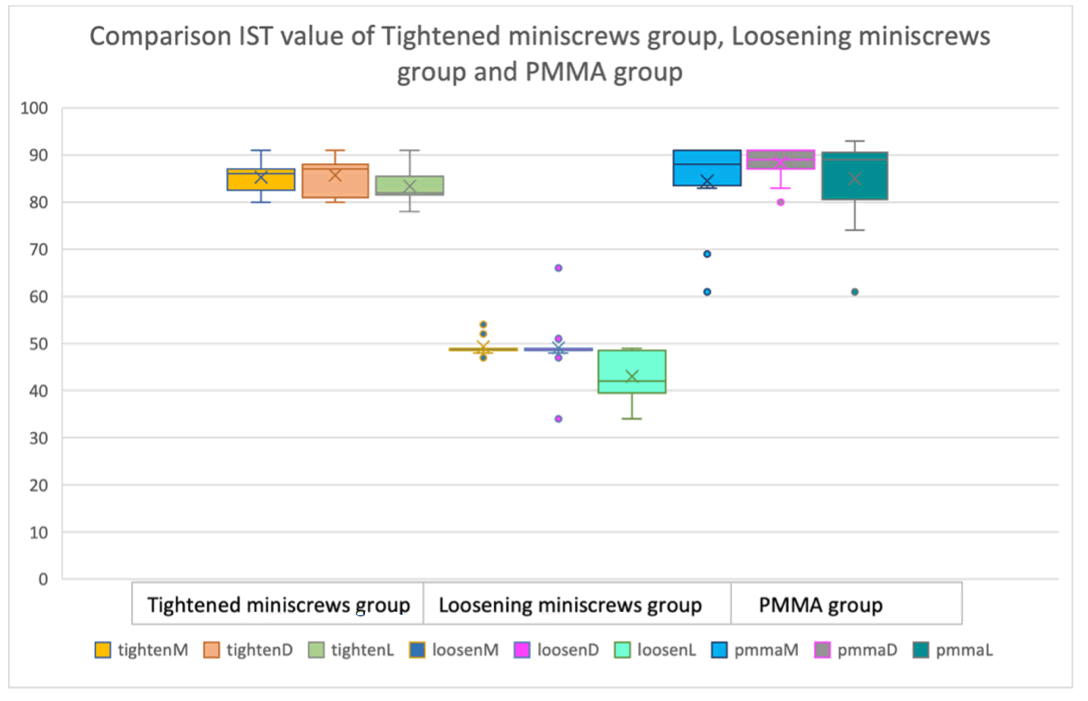
After the operation and the IST values were corrected, all IST values of the tighted miniscrew group were above 65. This defined that they had good stability. In the tightened miniscrew group, the median ± SD in the medial, distal and inferior directions were 86 ± 3.066, 87 ± 3.728, and 82 ± 3.798, respectively. In the loosening miniscrew group, the median ± SD of the medial, distal, and inferior directions were 49 ± 1.797, 49 ± 6.601, and 42 ± 5.339 respectively. In PMMA groups, the median ± SD in the medial, distal and inferior directions were 88 ± 9.252, 89 ± 3.453, and 89 ± 9.318 respectively. In all measured directions, the median of the tightened miniscrew group and the PMMA groups was higher than the median of the loosening miniscrew group (Figure 4).
Figure 4: Box and whisker plot of IST value in the tightened miniscrews group, loosening miniscrews group and PMMA group at medial, distal and inferior directions.
The median IST value in the PMMA group was statistically significantly higher than the loosening miniscrew group in all measured directions (p<0.05). There were no significant differences between the PMMA group and the tightened miniscrew group in all measured directions (p>0.05) (Table 1).
| Comparison groups | Z | P-value (2-tailed) | P-value (1-tailed) |
| PMMA-loosening miniscrews group (n=13) | |||
| Medial direction | -3.186 | 0.001 | 0.0005* |
| Distal direction | -3.191 | 0.001 | 0.0005* |
| Inferior direction | -3.185 | 0.001 | 0.0005* |
| Mean (all direction) | -3.183 | 0.001 | 0.0005* |
| PMMA-tightened miniscrews group (n=13) | |||
| Medial direction | -0.668 | 0.504 | 0.252 |
| Distal direction | -1.612 | 0.107 | 0.0535 |
| Inferior direction | -1.157 | 0.247 | 0.1235 |
| Mean (all direction) | -0.734 | 0.463 | 0.2315 |
| Note: *Significant p-value<0.05 | |||
Table 1: Comparison median of the PMMA group and the loosening miniscrews group and comparison median of the PMMA group and the tightened miniscrews group in medial, distal and inferior directions (Wilcoxon signed-rank test).
Radiographic outcome evaluation
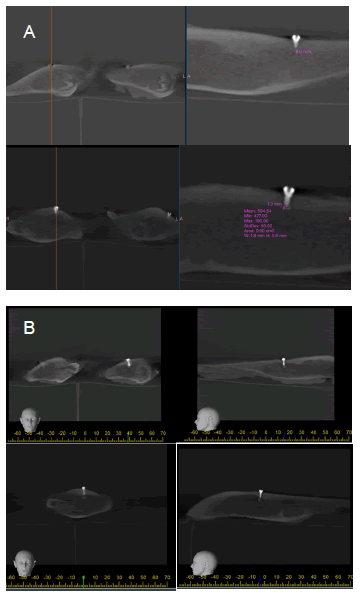
A total of 13 miniscrews and PMMA were placed. Each of the screw holes was filled with approximately 1.0 ml of PMMA. In the post-experimental Cone-beam 3D computed tomography, seven samples showed hyper density of PMMA around the miniscrews. However, six samples developed small cement infiltration into the cancellous bone (46.1%). There was no infiltration of PMMA into the entire cancellous bone or nerves. The PMMA material showed a hyperdense area with a Hounsfield unit about 614.41 (range 354.11- 847.75). This Hounsfield unit was between cancellous bone (range 111.66-331.73, mean 188.61) and cortex bone. (range 875.27- 1359.03, mean 1,047.02). The distance of PMMA leakage measured from the screw tip ranged from 1.3 mm to 3.3 mm (mean 2.1 mm) (Figure 5).
Figure 5: Cone-beam computed tomography imaging of postexperimental samples in the leakage PMMA groups. Note: A) CBCT images of Group A samples showing specific characteristics or measurements observed in Group A. Measurements include leakage distance of specific measurement, e.g., "9.6 mm" and area statistics; B) CBCT images of Group B samples showing specific characteristics or measurements observed in Group B. Measurements include leakage distance of specific measurement, e.g., "13 mm" and area statistics.
Discussion
PMMA was widely used in the surgical orthopaedic field including total hip joint and knee joint replacement but this was limitedly used in the maxillofacial field [6,8]. Many studies in orthopaedics have demonstrated the effectiveness of PMMA cements in enhancing stability with pedicle screws. Previous retrospective studies on osteoporotic spine patients by Sawakami et al., and Chang et al., concluded that PMMA augmentation of pedicle screws was safe, reliable and promoted bony fusion [9,10]. Orthopaedic studies utilised larger screw diameters (5.5 mm-6.5 mm), potentially impacting cement augmentation and stability. PMMA exhibits decreased viscosity and pseudoplastic behavior in the liquid phase during application. This pseudoplastic is non-Newtonian fluid, with viscosity decreasing as shear rate increases. At the working phase, the cement can be forced under pressure and infiltrate cancellous bone then perform mechanical interlocking. High-viscosity PMMA was most commonly used due to a long working phase of about 3-4 minutes and a short setting time of about 90-120 sec [11,12].
The PMMA experiment, an in vitro study, found that selfpolymerisation creates heat and toxicity. Consequently, tissue cells will be risk to heat injury [6,11]. Some studies found that the highest temperature of PMMA self-polymerisation was 48°C, which did not exceed the harmful tissue cell temperature [11,13,14]. Similarly, one study that experimented on rabbit (in vivo) found that the highest of PMMA self-polymerisation temperature was below animal body temperature [15]. Moreover, histopathological study of harvested rabbit bone, in which porous PMMA was applied, represented no tissue reaction, no tissue inflammation, and the presence newly formed bone [15,16].
We applied the implant stability meter, AnyCheck®, to be used for the screws stability assessment. The implant stability meter measures the stiffness of the alveolar bone-implant interface, which represents the bone-screw interface, through a tapping motion to evaluate the primary stability and osseointegration of the implant. The principle of stability is calculated by modified Damping Capacity Analysis (DCA). This calculates the deceleration at the tapping rod when it contacts the object and shown in IST value [17].
Furthermore, in this study, local PMMA infiltration through cancellous bone, ranging from 1.3 to 3.3 mm, was observed using cone-beam 3D computed tomography. These findings were consistent with the mechanical interlocking of PMMA and cancellous bone. This creates high bond strengths of PMMA cement [6,8,12]. Chang et al., identified key strategies to prevent significant cement leakage, emphasising the importance of factors such as PMMA viscosity, timing of cement injection, hardness, and duration of cement application. Using high-viscosity cement can likely help decrease cement leakage [10].
Conclusion
Based on our results, we concluded that the PMMA experimental group exhibited significantly greater stability in screw placement than the loosening miniscrew group. There were no significant differences between the PMMA group and the tightened miniscrew group in all measured directions. The PMMA exhibited to restore primary stability of the loosening miniscrews in the porcine mandible.
Therefore, further studies should examine the efficacy of PMMA with miniscrews together with surrounding bone formation in vivo.
Ethics statement/confirmation of patient permission
Non-human research by the research ethics community, Faculty of Dentistry, Prince of Songkla University (No: NH6605-008).
References
- Miloro M, Ghali GE, Larsen PE, Waite PD (2004) Peterson's principles of oral and maxillofacial surgery. Springer 1:37.
- Hernandez Rosa J, Villanueva NL, Sanati-Mehrizy P, Factor SH, Taub PJ (2016) Review of maxillofacial hardware complications and indications for salvage. Craniomaxillofac Trauma Reconstr 9(2):134-140.
[Crossref] [Google Scholar] [PubMed]
- Aramanadka C, Kamath AT, Srikanth G, Pai D, Singla N, et al. (2021) Hardware removal in maxillofacial trauma: a retrospective study. Sci World J 2021(1):9947350.
- Coletti DP, Salama A, Caccamese Jr JF (2007) Application of intermaxillary fixation screws in maxillofacial trauma. J Oral Maxillofac Surg 65(9):1746-1750.
[Crossref] [Google Scholar] [PubMed]
- Hashemi HM, Parhiz A (2011) Complications using intermaxillary fixation screws. J Oral Maxillofac Surg 69(5):1411-1414.
[Crossref] [Google Scholar] [PubMed]
- Heiss C, Kraus R, Schluckebier D, Stiller AC, Wenisch S, et al. (2006) Bone adhesives in trauma and orthopedic surgery. Eur J Trauma Emerg Surg 32:141-148.
[Crossref] [Google Scholar] [PubMed]
- Cankaya AB, Kasapoglu MB, Erdem MA, Kasapoglu C (2018) Effects of polymethylmethacrylate on the stability of screw fixation in mandibular angle fractures: A study on sheep mandibles. Int J Med Sci 15(13):1466.
[Crossref] [Google Scholar] [PubMed]
- Farrar DF (2012) Bone adhesives for trauma surgery: A review of challenges and developments. Int J Adhes Adhes 33:89-97.
- Sawakami K, Yamazaki A, Ishikawa S, Ito T, Watanabe K, et al. (2012) Polymethylmethacrylate augmentation of pedicle screws increases the initial fixation in osteoporotic spine patients. J Spinal Disord Tech 25(2):E28-35.
[Crossref] [Google Scholar] [PubMed]
- Webb JC, Spencer RF (2007) The role of polymethylmethacrylate bone cement in modern orthopaedic surgery. J Bone Joint Surg Br 89(7):851-857.
[Crossref] [Google Scholar] [PubMed]
- Sayeed Z, Padela MT, El-Othmani MM, Saleh KJ (2017) Acrylic bone cements for joint replacement. In Biomedical Composites. Woodhead Publishing 199-214.
[Crossref] [Google Scholar] [PubMed]
- Harving S, Søballe K, Bünger C (1991) A method for bone-cement interface thermometry: An in vitro comparison between low temperature curing cement palavit® and surgical simplex® p. Acta Orthopaedica Scandinavica. 62(6):546-548.
[Crossref] [Google Scholar] [PubMed]
- Reckling FW, Dillon WL (1977) The bone-cement interface temperature during total joint replacement. JBJS 59(1):80-82.
- Lye KW, Tideman H, Wolke JC, Merkx MA, Chin FK, et al. (2013) Biocompatibility and bone formation with porous modified PMMA in normal and irradiated mandibular tissue. Clin Oral Implants Res 24:100-109.
[Crossref] [Google Scholar] [PubMed]
- Sa Y, Yu N, Wolke JG, Chanchareonsook N, Goh BT, et al. (2017) Bone response to porous poly (methyl methacrylate) cement loaded with hydroxyapatite particles in a rabbit mandibular model. Tissue Engineering Part C: Methods. 23(5):262-273.
- Lee J, Pyo SW, Cho HJ, An JS, Lee JH, et al. (2020) Comparison of implant stability measurements between a resonance frequency analysis device and a modified damping capacity analysis device: An in vitro study. J Periodontal Implant Sci 50(1):56-66.
[Crossref] [Google Scholar] [PubMed]
- Chang MC, Liu CL, Chen TH (2008) Polymethylmethacrylate augmentation of pedicle screw for osteoporotic spinal surgery: A novel technique. Spine. 33(10):317-324.
[Crossref] [Google Scholar] [PubMed]
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi