Commentary, Biomater Med Appl Vol: 2 Issue: 1
Different Interspinous Stabilization Systems: Market Evaluation
Iñaki Arrotegui*
Department of Neurosurgery, Hospital General Universitario de Valencia, Valencia-Spain
*Corresponding Author : Dr. Iñaki Arrotegui
Department of Neurosurgery, Hospital General Universitario de Valencia, Valencia-Spain
Tel: 00-34-627492961
E-mail: athbio@yahoo.es
Received: December 01, 2017 Accepted: December 21, 2017 Published: January 02, 2018
Citation: Arrotegui I (2018) Different Interspinous Stabilization Systems: Market Evaluation. Biomater Med Appl 2:1. doi: 10.4172/2577-0268.1000111
Abstract
The interspinous spacers are those devices that placed between the spinous processes of contiguous vertebrae, act by dynamically stabilizing the vertebral segment in the sagittal plane. The principle of implanting a spacer between adjacent spinous processes was used by F. Knowles in the 1950s to discharge the posterior ring in patients with herniated discs and thus achieve pain relief [1,2]. Senegas et al. [3] who in 1986 designed a system of dynamic normalization stabilization (mechanical normalization system) to stiffen the degenerated lumbar segment operated, using an interspinous titanium block to limit the extension and a tension band (Dacron) around the spinous processes, to Secure the implant and limit bending. This implant, which was designed as the first generation of the current Wallis, so that it restored more physiological mechanical conditions in the treated degenerate segment, could not only alleviate or prevent the pain related to instability but decrease the range of disc destruction at that level. It was also suggested that if the interspinous stabilization system preserved more mobility in the treated segment than a fusion would do, then the degenerative process at adjacent levels would progress more slowly [4,5].
Keywords: Interspinous spacers, spinal canal
Introduction
The interspinous spacers are those devices that placed between the spinous processes of contiguous vertebrae, act by dynamically stabilizing the vertebral segment in the sagittal plane. The principle of implanting a spacer between adjacent spinous processes was used by F. Knowles in the 1950s to discharge the posterior ring in patients with herniated discs and thus achieve pain relief [1,2]. Senegas et al. [3] who in 1986 designed a system of dynamic normalization stabilization (mechanical normalization system) to stiffen the degenerated lumbar segment operated, using an interspinous titanium block to limit the extension and a tension band (Dacron) around the spinous processes, to Secure the implant and limit bending. This implant, which was designed as the first generation of the current Wallis, so that it restored more physiological mechanical conditions in the treated degenerate segment, could not only alleviate or prevent the pain related to instability but decrease the range of disc destruction at that level. It was also suggested that if the interspinous stabilization system preserved more mobility in the treated segment than a fusion would do, then the degenerative process at adjacent levels would progress more slowly [4,5].
Several devices of this type have entered the market in recent years. In addition to the Wallis, mentioned above, there is the Coflex designed by Jacques Samani in 1994 and retaken today as U device, the Diam, X-Stop, Lixus etc [6]. All of them try to decrease the extension movement. Biomechanical studies have shown that certainly the extension decreases with the placement of the spacer while the flexion, axial rotation and lateral inclination remain unchanged [7]. These implants, by distracting the interspinous space and limiting the extension, reduce the posterior pressure of the annulus fibrosis. of the disc, the narrowing of the spinal canal, the bulging of the yellow ligament, and theoretically expand the intervertebral foramen and discharge the facets join [8-10]. For all these reasons, these implants are used in degenerative disc disorders and Lumbar Canal stenosis [11,12].
In a multicentre study for the treatment of lumbar stenosis with the X-Stop interspinous device, which produced interspinous distraction and indirectly decompression, reported a 59% satisfaction in relation to 12% in patients who had not undergone surgery [13].
Senegas et al. [3], in a retrospective analysis on the results of the placement of the interspinous dynamic stabilization device designed by them (first generation of the current Wallis), in 142 patients with degeneration of the lumbar segments reported an 80% permanence of the implant( 14 years follow- up), without needing a new reoperation. They attributed the good results to the long-term protection of the degeneration of the adjacent segment by the preservation of the movement since it is in itself a procedure of extra-articular nature in which, except the interspinous ligament, the rest of the elements remain intact, it is a reversible surgery and the rest of the surgical variants remain open.
In the report of Reyes Sánchez et al. on the result of corneal ligamentoplasty in the treatment of lumbosacral instability, 95% improvement was reported, with a single case that was reoperated because there was no variation in low back pain with respect to the preoperative period and an instrumented arthrodesis was performed. Another case presented wound dehiscence and soft tissue infection, which they attributed to the poor preparation of the skin [14]. In biomechanical studies performed for the evaluation of the U interspinous spacer as a lumbar stabilizer, it was determined that the models representing microsurgical decompression (partial laminectomy combined with partial fascetectomy) to release the root presented a partial instability, whereas Models with total laminectomy completely destabilized the vertebral segment and therefore required rigid transpedicular instrumentation to restore stability. It was concluded that U, by influencing the control of movement in the plane of flexion-extension and axial rotation, offered a non-rigid fixation and had the ability to return the destabilized samples in which it was inserted at its normal range of motion [15].
In our prospective control trial, historic group + a new device in a cohort of 100 patients with degenerative Lumbar disc degeneration 50 underwent surgical treatment in which the U device was placed and 50 control individuals were treated with discectomy alone.
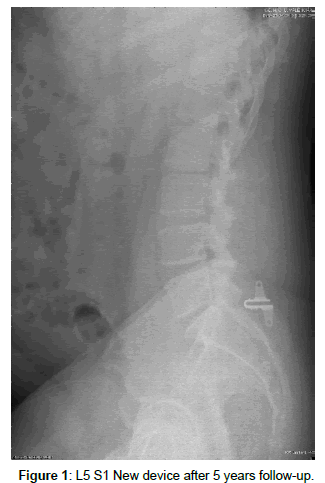
Patients underwent serial follow-up evaluations (clinical test). And radiographic assessment was used to determine outcome Up to ten years follow-up data were obtained in all patients. Aim: Use the device in order to prevent or delay the clinical symptoms after discectomy: LAST step Lumbar Instability. With a follow-up of Two years 90 % vs. 60 % without evidence of any clinical or radiological instability. We have five years follow up for the new device at L5 S1 with good results so far (Figure 1).
Conclusion
Our study shows that the U new device was more effective than discectomy Group in the management of degenerative lumbar disc herniation regarding lumbar instability.
The best to use was at l4/ L5, at L5 / S1, depends on the Spinous Process of S1 Now with our device 90 % of the patients have implant the device Vs. Historic device; you can perform up to 3 levels. Improvement with U new device was statistically significant p<0.01. To has real answers to know what happened after disc surgery and to avoid the next step: lumbar instability at the level of surgery. We are done 5 years follow up, with good results, but we think a long period of follow-up it will beneccesary in order to know if is useful or not.
References
- Boos N, Aebi M (2008) Fundamentals of diagnosis and treatment. Spinal disorders Berlin:Springer-Verlag: 83-568.
- Whiteside TE, (2003) The effect of an interspinous implant on intervertebral disc pressures. Spine 28:1906-1907
- Senegas J, Vital JM, Pointillart V, Mangione P (2007) Long-term actuarial survivorship analysis of an interspinous stabilization system. Eur Spine J 16:1279-1287.
- Ghiselli G, Wang JC, Bhatia NN, Hsu WK, Dawson EG (2004) The fate of the adjacent motion segments after lumbar fusion. J Bone Joint Surg Am 86:1497-1503.
- Gillet P (2003) The fate of the adjacent motion segments after lumbar fusion. J Spinal Disord Tech 16:338- 345.
- Sales J (2008) Implantes lumbares interespinosos. Neurocirugía contemporánea 2:1-7.
- Lindsey DP, Swanson KE, Fuchs P, Hsu KY, Zucherman JF, et al. (2003) The effects of an interspinous implant on the kinematics of the instrumented and adjacent levels in the lumbar spine. Spine 28: 2192-2197.
- Senegas J (2002) Mechanical supplementation by non-rigid fixation in degenerative intervertebral lumbar segments: the Wallis system. Eur Spine J 11:164-169.
- Christie SD, Song JK, Fessler RG (2005) Dynamic interspinous process technology. Spine 30: S73-78.
- Wiseman CM, Lindsey DP, Fredrick AD, Yerby SA (2005) The effect of an interspinous process implant on facet loading during extension. Spine 30: 903-907.
- Kondrashov DG, Hannibal M, Hsu KY, Zucherman JF (2006) Interspinous process decompression with the X-STOP device for lumbar spinal stenosis: a 4-year follow-up study. J Spinal Disord Tech 19:323- 327.
- Talwar V, Lindsey DP, Fredrick A, Hsu KY, Zucherman JF, (2006) Insertion loads of the X STOP interspinous process distraction system designed to treat neurogenic intermittent claudication. Eur Spine J 15: 908- 912.
- Zucherman JF, Hsu KY, Hartjen CA, Mehalic TF, Implicito DA, et al. (2004) A prospective randomized multi-center study for the treatment of lumbar spinal stenosis with the X STOP interspinous implant: 1-year results. Eur Spine J 13:22- 31.
- Reyes-Sánchez A, Villanueva Rivera P, Miramontes V, Rosales LM (1998) Ligamentoplastia interespinosa lumbar con corion para el tratamiento de la inestabilidad vertebral. Reporte de 4 años de seguimiento. Rev Mex Ortop Traum 12: 564-567.
- Tsai KJ, Murakami H, Lowery GL, Hutton WC (2006) A biomechanical evaluation of an interspinous device (Coflex device) used to stabilize lumbar spine. Paradigm Spine J : 167-72
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi