Research Article, Arch Transplant Vol: 4 Issue: 5
Estimates of Glomerular Filtration Rate in Liver Transplant Recipients are not Accurate: A Role for 24-Hour Urine Creatinine Clearance
Mark W Russo1*, Krista Bossi1, Gale Groseclose1, David M Levi2, Lon Eskind2, Bennett Noell2, Anderson WE3, Philippe J Zamor1 and Vincent Casingal2
1Division of Hepatology, Transplant Center -Carolinas Medical Center, Charlotte, NC, USA
2Division of Transplant Surgery, Carolinas HealthCare System, Charlotte, NC, USA
3Center for Outcomes Research and Evaluation, Carolinas HealthCare System, Charlotte, NC, USA
*Corresponding Author : Mark W Russo, MD MPH FAASLD
Transplant Center -Carolinas Medical Center, 6th Floor MMP, 1025 Morehead Medical Drive, Charlotte, NC, USA
E-mail: mark.russo@carolinashealthcare.org
Received: January 31, 2018 Accepted: February 22, 2018 Published: February 27, 2018
Citation: Russo MW, Bossi K, Groseclose G, Levi DM, Eskind L, et al. (2018) Estimates of Glomerular Filtration Rate in Liver Transplant Recipients are not Accurate: A Role for 24-Hour Urine Creatinine Clearance. Arch Transplant 2:1.
Abstract
Background: Kidney injury is common among liver transplant recipients. Equations estimating glomerular filtration rate were not developed in liver transplant recipients. Aim: To determine if GFR equations and 24-hour urine creatinine clearance accurately estimate GFR in liver transplant recipients. Methods: 30 subjects were enrolled within 6 months of transplant and obtained estimates of GFR. The iothalamate scan served as the gold standard and it was compared to GFR equations and 24- hour urine creatinine clearance. Results: The mean time to iothalamate scan was 110 + 50 days.The mean iothalamate GFR was 90 + 37 mL/min/1.73 m2. The GFR equations underestimated GFR with 47%-63% of estimates differing by more than 20% from the iothalamate GFR. Among the equations the CKD-EPI-Cys-Cr was the most accurate. 24-hour urine creatinine clearance both under and overestimated GFR, however it was the most concordant with the iothalamate scan in identifying subjects with GFR greater or less than 50 mL/min/1.73 m2. Conclusions: Within 6 months of liver transplant GFR equations and 24-hour urine collection do not accurately estimate GFR. 24-hour urine creatinine clearance may be the clinically most useful estimate of GFR because it most accurately identifies liver transplant recipients with GFR greater or less than 50 mL/min/1.73 m2.
Keywords: Kidney; Injury; Formulas
Introduction
Kidney injury is common after liver transplantation with up to 30% of liver transplant recipients developing stage 4 or 5 kidney disease within 5 years of liver transplantation [1]. Strategies to prevent kidney injury include minimizing or modifying immunosuppression such as reducing calcineurin inhibitor dosing with or without adding or replacing with mycophenolate mofetil, or an mTOR inhibitor [3]. Therefore, accurate measures of glomerular filtration rate (GFR) are needed because the presence of kidney injury may lead to modifications in immunosuppression.
The most accurate measures of GFR are determined from inulin or iothalamate clearance but these tests are invasive and costly. As a result, kidney equations have been developed to estimate GFR, but these equations were not originally validated in liver transplant recipients [3-6]. Studies that have evaluated GFR equations in liver transplant recipients have reported they do not accurately measure GFR but these studies either did not include 24-hour urine collection, the most recent formulas that estimate GFR or included a wide range of recipients, many of whom were several years post liver transplant [7-10]. Mindikoglu et al. developed a formula to estimate GFR specific for patients with cirrhosis, but this study did not include transplant recipients [11].
The goal of our study was to compare the GFR equations and 24- hour urine creatinine clearance to iothalamate scan GFR in the early post liver transplant period.
Methods
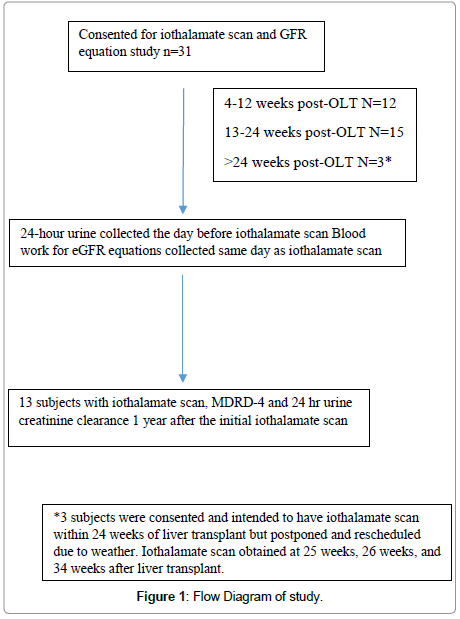
Adult (≥18 years-old) liver only transplant recipients within 6 months of liver transplant were invited to participate in the study. Serum creatinine was obtained on at least two occasions within 1 week prior to obtaining estimates of GFR, 24-hour urine creatinine and iothalamate scans. Patients were excluded if they had a multiorgan transplant, iodine allergy, estimated GFR less than 30 mL/min/1.73 m2, acute kidney injury, evidence of bleeding, acute infection, dehydration, diarrhea, volume contraction within at least 1 week of GFR measurement, or if they were taking or planned on initiating diuretics, or angiotensin converting enzyme inhibitors. Subjects underwent iothalamate scan, 24-hour urine creatinine clearance (24 hr CrCl), and blood work for MDRD-4, MDRD-6, CKD-EPI, CKD-EPI-cystatin, CKD-EPI-cystatin-Cr GFR, equations and eGFR equation developed in cirrhotics with refractory ascites [11]. The iothalamate scan and remaining studies were obtained within one day of each other. A flow diagram of the study is shown in Figure 1.
All study subjects received methylprednisolone 1 gram intravenously immediately after liver transplant followed by a steroid taper over 6 months and tacrolimus based immunosuppression with goal plasma levels of 6-10 ng/mL. Mycophenolate mofetil was added to tacrolimus in subjects with autoimmune hepatitis, primary sclerosing cholangitis and primary biliary cirrhosis. All study subjects received trimethoprim/sulfamethoxazole for pneumocystis jirovecii prophylaxis for the first year post liver transplant.
Iothalamate scans were performed following intravenous administration of 25 uCi of I-125 and three urine and blood plasma samples were obtained over a period of 2 to 3 hours, with volume and radioactivity count analysis performed. Global GFR calculations were performed utilizing all three sample data sets, with urine volume, urine flow rate, and body surface area information.
The study was approved by the Carolinas Healthcare System Institutional Review Board and registered with National Clinical Trials Registry [NCT02883400].
Statistical methods
Descriptive statistics were calculated. The primary analyses were based on the difference between each estimated GFR measure and iothalamate scan (the gold standard). The bias and precision of each GFR measure were calculated as the median and interquartile range difference, respectively [10-12]. Analyses were performed with the Wilcoxon sign rank test comparing the iothalamate result with each estimated GFR measure. Accuracy of each measure was assessed as the proportion of patients whose estimated GFR differed by more than 20% of iothalamate GFR. [10,12]. In addition, using 50 mL/min/1.73 m2 as the reference point, the proportion of discordant pairs was calculated for each GFR estimator as the proportion of patients with either estimated GFR <50 and iothalamate ≥ 50 mL/min/1.73 m2 or estimated GFR ≥ 50 mL/min/ 1.73 m2 and iothalamate <50 mL/min/ 1.73 m2. An estimated GFR <50 mL/min/1.73 m2 was used because estimates of GFR that fall below 40 and 60 mL/min/1.73 m2 have been advocated as cut offs to switch or add an mTOR inhibitor [13,14]. For the proportions referenced above, 95% confidence intervals were determined. Finally, modified versions of the graphs described in Bland and Altman plotted the difference scores against iothalamate GFR estimates [15]. SAS Enterprise Guide 6.1 (SAS Institute Inc., Cary, NC) was used for all statistical analyses. A p-value less than 0.05 was considered statistically significant.
Results
Characteristics of the study population (n=30) are shown in Table 1. The mean age was 55 ± 9 years-old years and most subjects were male. The most common indications for liver transplant were end stage liver disease from alcohol and nonalcoholic fatty liver disease followed by hepatitis C with a median MELD-Na at transplant of 23. The mean creatinine at transplant was 1.1 ± 0.4 mg /dL and 2 patients were on renal replacement therapy for less than 6 weeks prior to liver only transplant.
| Age, years (mean, SD) | 55 (9) |
| Male (%) | 24 (80) |
| Caucasian (%) | 26 (87) |
| BMI kg/m2 (mean, SD) | 32 (11) |
| Diabetes mellitus (%) | 8 (27) |
| Hepatitis C (%) | 8 (27) |
| Alcohol (%) | 9 (30) |
| NAFLD (%) | 9 (30) |
| HCC (%) | 11 (37) |
| MELD-Na at transplant (median, IQR) | 23 (4) |
| Creatinine at transplant mg/dL (median IQR) | 0.9 (0.4) |
| Cystatin C mg/L(median, IQR) | 1.2 (0.4) |
| Dialysis prior to liver transplant (< 6 weeks) (%) | 2 (7) |
| Median weeks from transplant to iothalamate scan (IQR, range)* | 15 (10), (6-35) |
Table 1: Characteristics of Subjects n=30.
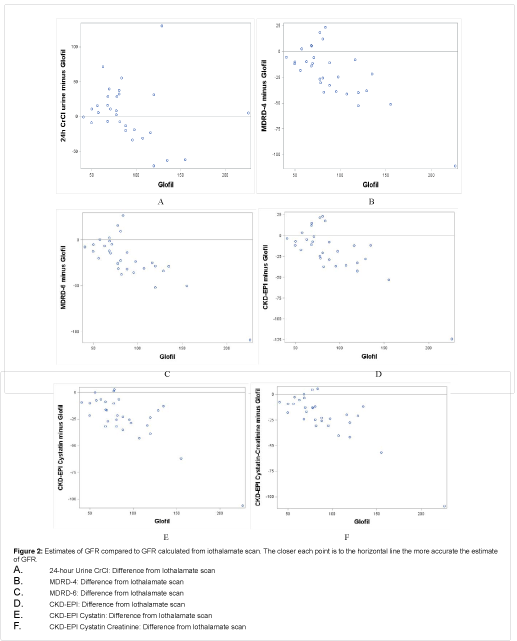
The estimated glomerular filtration rate (GFR) for iothalamate scan, GFR equations, and 24-hour urine creatinine clearance are shown in Table 2. The median time from transplant to iothalamate scan was 15 weeks (Table 1). The mean GFR for the study group by iothalamate scan was 90 ± 37 ml/min/1.73 m2. The mean 24- hour urine creatinine clearance best approximated the iothalamate scan results compared to the kidney formulas mean 96 ± 49 ml/ min/1.73 m2 followed by CKD-EPI formula 73 ± 24 mL/min/1.73 m2. However, the differences between 24-hour urine creatinine clearance and iothalamate scan results had high variability (IQR 47.4 for difference scores). The proportion of subjects where the difference between the GFR on the iothalamate scan and noninvasive tests was greater than 20% was similar among the 24-hour urine collection and GFR equations. The CKD-EPI-Cys-Cr was the least discordant GFR equation (Table 2). However, all the GFR equations significantly underestimated results from the iothalamate scan, with means ranging from 66-73 mL/min/1.73 m2 compared to 90 ml/min for the iothalamate scan (p<0.001 for each) (Table 2 and Figure 2). By contrast, the 24-hour urine creatinine clearance underestimated and overestimated the GFR about equally as often (Figure 2).
| Measure | Mean | Median | SD | Bias (precision): Median (IQR) difference | p-value (WSR Test) | Accuracy: Proportion differing by >20% iothalam. (95% CI) | Accuracy: Proportion Discordant at eGFR 50 (95% CI) |
|---|---|---|---|---|---|---|---|
| Iothalamate | 90.0 | 80.7 | 37.4 | -- | -- | -- | -- |
| 24hr CrCl urine | 95.6 | 81.0 | 49.0 | 5.2 (47.4) |
0.49 | 0.60 (0.41-0.77) |
0.03 (0.00-0.17) |
| MDRD-4 | 69.6 | 65.5 | 24.2 | -16.1 (31.9) |
<0.0001 | 0.63 (0.44-0.80) |
0.13 (0.04-0.31) |
| MDRD-6 | 69.5 | 66.5 | 23.4 | -21.4 (26.2) |
<0.0001 | 0.63 (0.44-0.80) |
0.13 (0.04-0.31) |
| CKD-Epi | 72.8 | 70.5 | 23.8 | -12.0 (25.3) |
0.0007 | 0.60 (0.41-0.77) |
0.10 (0.02-0.27) |
| CKD-Epi Cystatin | 66.8 | 62.0 | 24.3 | -21.7 (21.4) |
<0.005 | 0.63 (0.44-0.80) |
0.13 (0.04-0.31) |
| CKD-Epi Cystatin Creatinine | 69.2 | 65.0 | 23.1 | -17.4 (16.7) |
<0.005 | 0.47 (0.28-0.66) |
0.10 (0.02-0.27) |
| cirrhosis eGFR ref 11 | 66.1 | 64.3 | 18.1 | -19.2 (28.8) | <0.0001 | 0.57 (0.37-0.75) |
0.10 (0.02-0.27) |
Difference=estimated GFR minus iothalamate.
P-values are for comparisons of estimated GFR and iothalamate scan results.
Proportion outside 20% iothalamate is the proportion of patients whose estimated GFR differed by greater than 20% of iothalamate GFR result. Proportion discordant at 50 is the proportion of patients with either estimated GFR < 50 mL/min/1.73 m2 and iothlamate GFR ≥ 50 mL/min/1.73 m2 or estimated GFR ≥ 50 mL/min/1.73 m2 and iothalamate GFR< 50 mL/min/1.73 m2.
Table 2: Performance of estimates of GFR and creatinine clearance*.
Figure 2: Estimates of GFR compared to GFR calculated from iothalamate scan. The closer each point is to the horizontal line the more accurate the estimate of GFR.
A. 24-hour Urine CrCl: Difference from Iothalamate scan
B. MDRD-4: Difference from Iothalamate scan
C. MDRD-6: Difference from Iothalamate scan
D. CKD-EPI: Difference from Iothalamate scan
E. CKD-EPI Cystatin: Difference from Iothalamate scan
F. CKD-EPI Cystatin Creatinine: Difference from Iothalamate scan
We also determined the proportion of subjects where eGFR equation or 24-hour urine creatinine clearance GFR was either less than 50 mL/min/1.73 m2 but the results from the iothalamate scan were greater than or equal to 50 mL/min/1.73 m2, or vice versa (“discordant at 50”). We chose 50 mL/min/1.73 m2 because this is a threshold used to modify immunosuppression or add or switch from a calcineurin inhibitor to a mTOR inhibitor [13,14]. The 24-hour urine creatinine clearance was discordant in 3% of subjects while the formulas that estimate GFR were discordant in 10%-13% of subjects (Table 2).
There were two outliers with 24-hour urine creatinine clearance and iothalamate scan GFR >200 mL/min/1.73 m2. When excluding these two outliers, the results comparing iothalamate scan to the estimated measures were similar to the results from the entire cohort (paired t-test, p=0.85 for 24-hour CrCl urine, p ≤ 0.002 for the equations).
Table 3 shows the 13 subjects who agreed to an iothalamate scan one year after their initial iothalamate scan. Among these 13 subjects, the MDRD-4 underestimated GFR by ≥ 20 mL/min/1.73 m2 in 10 subjects. In contrast 24-hour urine creatinine clearance overestimated GFR ≥ 20 mL/min/1.73 m2 in 5 subjects and underestimated GFR in 2 subjects.
| Subject matched to Table 1 | Iothalamate GFR as mL/min/1.73m2 | MDRD-4 mL/min/1.73m2 | Tacrolimus level (ng/mL) | Serum Creatinine mg/dL | 24 hour urine Creatinine mL/min/1.73m2 |
|---|---|---|---|---|---|
| 1 | 98.6 | 55.0 | 4.5 | 1.33 | 107.0 |
| 3 | 154.7 | 82.0 | 8.5 | 0.97 | 166.0 |
| 4 | 55.4 | 69.0 | 6.8 | 0.87 | 109.0 |
| 6 | 76.6 | 59.0 | 8.0 | 1.27 | 93.0 |
| 7 | 85.3 | 50.0 | 8.5 | 1.41 | 47.0 |
| 8 | 123.4 | 78.0 | 8.8 | 1.03 | 140.0 |
| 9 | 87.9 | 62.0 | 5.3 | 1.14 | 87.0 |
| 11 | 113.4 | 93.0 | 6.9 | 0.83 | 126.0 |
| 12 | 88.7 | 56.0 | 6.0 | 1.30 | 71.0 |
| 13 | 49.6 | 43.0 | 7.5 | 1.28 | 91.0 |
| 14 | 197.0 | 130.0 | 6.7 | 0.74 | unable to calc |
| 15 | 86.0 | 50.0 | 9.2 | 1.46 | 120.0 |
| 16 | 86.4 | 55.0 | 6.3 | 1.24 | 139.0 |
Table 3: 1-year results comparing Iothalamate GFR to MDRD-4 and 24 hr urine creatinine clearance*.
Discussion
Kidney injury after liver transplantation is common and in the pre-MELD era 20%-30% of liver transplant recipients developed end stage renal disease within 5 years of liver transplantation [1,16]. Because creatinine is included in the MELD score, an increasing proportion of liver transplant candidates undergo liver transplant with impaired kidney function. In fact, 47% of candidates are listed with a serum creatinine greater than 2 mg/dL, and there was a 41% increase in wait listed candidates on dialysis following the introduction of MELD [16,17]. Thus, kidney dysfunction after liver transplant is one of the most common management issues encountered by transplant physicians.
Strategies to minimize kidney injury after liver transplant include modifying immunosuppression [2]. Changes in immunosuppression are based upon estimates of GFR. Thus, accurate estimates of glomerular filtration rate are important in liver transplant recipients so that appropriate changes can be implemented to preserve kidney function. Currently available equations used to estimate glomerular filtration rate (i.e. MDRD-4, MDRD-6, CKD-EPI creatinine-cystatin) were not developed in liver transplant recipients. Studies evaluating GFR equations in liver transplant recipients demonstrate these equations do no accurately estimate GFR after liver transplant. Gonwa et al. compared GFR estimated from the Cockcroft-Gault equation, MDRD-4-6 equations and Nank equation to GFR from I125-iothalamate clearance in 1,447 liver transplant recipients and reported that the equations were within 30% of GFR only 54.7%- 63.1% of the time [7]. The investigators did not evaluate 24-hour urine creatinine clearance or the CKD-EPI equations. A study of 401 liver transplant recipients found that CKD-EPIcr-cys performed the best compared to other GFR equations [10]. However, this study included recipients on average of 4 years post liver transplant, a much different population than the one included in the current study. Other studies of GFR equations in liver transplant recipients have similar limitations [8,9]. Perhaps not surprisingly, an eGFR formula developed in cirrhotic patients with refractory ascites performed no better than existing eGFR formulas in our patient population [11]. In our study of subjects within 6 months of liver transplant the GFR equations were discordant with results of the iothalamate mostly due to underestimating GFR.
At first glance it seemed that 24-hour urine creatinine clearance was best at approximating the GFR obtained from iothalamate scan, but 60% of subjects varied by more than 20% from iothalamate GFR. 24-hour urine creatinine clearance both under and overestimated GFR about equally as often. However, 24-hour creatinine clearance was the most concordant with estimating a GFR as either greater than or less than 50 mL/min/1.73 m2, a cutoff that may be used to add or switch to a mTOR inhibitor [13,14]. There are only a few strategies to protect the kidneys from injury after liver transplantation [2]. One strategy is to minimize calcineurin exposure either through dose reduction, or dose reduction and addition of mycophenolate mofetil or mTOR inhibitor, or conversion to mTOR inhibitor. Because it is not feasible or cost effective to regularly obtain an iothalamate scan, 24-hour urine creatinine clearance is more practical and could be obtained annually or more frequently if indicated. The number of subjects at 1-year followup was small but the same trend was seen where MDRD-4 underestimates GFR. It is apparent that better equations are needed to estimate GFR in liver transplant recipients.
Limitations of our study include the small sample size and the one time determination of estimated GFR without follow-up time points. However, despite the small sample size the results are consistent with prior studies reporting that the accuracy for estimating GFR using kidney equations is poor [7-10]. Our study adds to prior studies because we also evaluated new GFR equations and 24-hour urine creatinine clearance. We found that the accuracy for estimated GFR>50 mL/min/1.73 m2 was highest for 24 hour-urine creatinine clearance so from a practical standpoint obtaining a 24-hour urine creatinine clearance may be useful before changing immunosuppression. The eGFR equations underestimated GFR and a limitation is recipients were taking trimethoprim-sulfamethaxozole which blocks creatinine secretion in the renal tubules. Iothalamate scans were obtained during the first 6 months after liver transplant and muscle mass changes over this time which could affect results of estimated GFR.
In conclusion, GFR equations in liver transplant recipients and 24-hour urine creatinine clearance do not accurately estimate GFR in liver transplant recipients. 24-hour urine creatinine clearance may be useful for centers that use a threshold of 50 mL/min/1.732 to modify immunosuppression to prevent further kidney injury. The development and validation of GFR equations in liver transplant recipients is needed because changes in immunosuppression are based upon these estimates.
Acknowledgements
The study was supported by the Anne & Epes Robinson Fund for Liver Transplant Medicine. The authors thank Chris Fotiadis, MD, Metrolina Nephrology Associates, for serving as data safety monitor and input into study design
References
- Ojo AO, Held PJ, Port FK, Wolfe RA, Leichtman AB, et al. (2003) Chronic renal failure after transplantation of a nonrenal organ. N Engl J Med 349: 931-940.
- Levistsky J, O’Leary JG, Asrani S, Sharma P, Fung J, et al. (2016) Protecting the kidney in liver transplant recipients: Practice-based recommendations from the American Society of Transplantation Liver and Intestine Community of Practice. Am J Transpl 16: 2532-2544.
- Levey AS, Coresh J, Greene T, Stevens LA, Zhang YL, et al. (2006) Using standardized serum creatinine values in the modification of diet in renal disease study equation for estimating glomerular filtration rate. Ann Intern Med 145: 247-254.
- Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, et al. (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150: 604-612.
- Levey AS, Bosch JP, Lewis JB, Greene T, Rogers N, et al. (1999) A more accurate method to estimate glomerular filtration rate from serum creatinine:a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 130: 461-470.
- Stevens LA, Coresh J, Greene T, Levey AS (2006) Assessing kidney function-measured and estimated glomerular filtration rate. N Engl J Med 354: 2473-2483.
- Gonwa TA, Jennings L, Mai mL, Stark PC, Levey AS, et al. (2004) Estimation of glomerular filtration rates before and after orthotopic liver transplantation: evaluation of current equations. Liver Transpl 10: 301-309.
- Gerhardt T, Poge U, Stoffel-Wagner B, Ahrendt M, Wolff M, et al. (2006) Estimation of glomerular filtration rates after orthotopic liver transplantation: Evaluation of cystatin-C based equations. Liver Transpl 12: 1667-1672.
- Schuck O, Gottfriedova G, Maly J, Jabor A, Bruzkova I, et al. (2002) Glomerular filtration rate assessment in individuals after orthotopic liver transplantation based on serum cystatin c levels. Liver Transpl 8: 594-599.
- Allen AM, Kim RW, Larson JJ, Colby C, Therneau TM, et al. (2015) Serum cystatin C as an indicator of renal function and mortality in liver transplant recipients. Transplantation 99: 1431-1435.
- Mindikoglu AL, Dowling TC, Magder LS, Christenson RH, Weir MR, et al. (2016) Estimation of glomerular filtration rate in patients with cirrhosis by using new and conventional filtration markers and dimethylarginines. Clin Gastroenterol Hepatol 14: 624-632.
- Mindikoglu AL, Dowling TC, Weir MR, Seliger SL, Christenson RH, et al. (2014) Performance of chronic kidney disease epidemiology collaboration creatinine-cystatin C equation for estimating kidney function in cirrhosis. Hepatology 59: 1532-1542
- Abdelmalek MF, Humar A, Stickel F, Andreone P, Pacher A, et al. (2012) Sirolimus conversion regimen versus continued calcineurin inhibitors in liver allograft recipients: a randomized trial. Am J Transplant 12: 694-705
- De Simone P, Fagiouli S, Cescon M, De Carlis L, TIsone G, et al. (2017) Use of everolimus in liver transplantation: Recommendations from a working group. Transplantation 101: 239-251.
- Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 8: 307-310.
- Ruebner R, Goldbert D, Abt PL, Bahirwani R, Levine M, et al. (2013) Risk of end stage renal disease among liver transplant recipients with pre-transplant renal dysfunction. Am J Transplant 12: 2958-2965.
- Dellon ES, Galanko JA, Medapalli RK, Russo MW (2006) Impact of dialysis and older age on survival after liver transplantation. Am J Transplant 6: 2183-2190.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi