Editorial, Arch Transplant Vol: 1 Issue: 1
Is C4d Deposits Detection a Real Marker for the Diagnosis of Chronic Rejection in Renal Allografts? Is Further Revise of its Diagnostic Criteria Not Required?
Satoshi Teraoka*
Executive Director, International University of Health and Welfare, Tokyo, Japan
*Corresponding Author : Satoshi Teraoka
Former Executive director, International University of Health and Welfare, Shimoochiai, Shinjuku-ku, Tokyo, Japan 161-0033
Tel: 090-3090-0383
E-mail: teraoka@iuhw.ac.jp
Received: November 07, 2017 Accepted: November 09, 2017 Published: November 13, 2017
Citation: Teraoka S (2017) Is C4d Deposits Detection a Real Marker for the Diagnosis of Chronic Rejection in Renal Allografts? Is Further Revise of its Diagnostic Criteria not Required?. Arch Transplant Stud 1:1.
Abstract
Outcomes of kidney transplantation have been improved during the last decade mainly by the new potent immunosuppressants. Main causes of graft loss are chronic humoral rejection (CHR), calcineurin inhibitor (CNI) nephrotoxicity (CNINT), de novo or recurrent glomerulonephritis (GN) and the death with functioning graft (DWFG). Nowadays acute cellular rejection has been almost overcome by its prevention and early treatment using potent and selective T cell-based immunosuppressants based upon the early and accurate diagnosis, which was developed and standardized by Banff criteria
Keywords: Renal allograft
Outcomes of kidney transplantation have been improved during the last decade mainly by the new potent immunosuppressants. Main causes of graft loss are chronic humoral rejection (CHR), calcineurin inhibitor (CNI) nephrotoxicity (CNINT), de novo or recurrent glomerulonephritis (GN) and the death with functioning graft (DWFG). Nowadays acute cellular rejection has been almost overcome by its prevention and early treatment using potent and selective T cell-based immunosuppressants based upon the early and accurate diagnosis, which was developed and standardized by Banff criteria [1].
The histological diagnosis of CNINT and de novo or recurrent GN was established by immunohistochemical, fluorescent and electron microscopic imaging in addition to conventional microscopic findings using various staining technology. On the other hand, the establishment of the histological diagnostic criteria of CHR remained still in the process. In 1993 the novel category “chronic allograft nephropathy (CAN)” was introduced by Banff classification [1], which was featured as chronic transplant glomerulopathy, glomerular basement membrane (GBM) duplication, mesangial cell proliferation, fibrous intimal thickening, interstitial fibrosis and tubular atrophy (IF/TA), and arteriolar hyalinization. “CAN” was considered to include several entities inclusive of CHR, chronic CNINT, hypertensive changes, chronic infection and others. The introduction of “CAN” meant that it was not able to differentiate CHR from CNINT by histological findings. It could be taken a kind of “concede defeat” of the specialty of pathology. Furthermore the introduction of this new category caused a certain kind of confusion in the diagnosis and the statistics of graft failure/loss in the clinical field, so that it led to more than 10-year-delay in taking countermeasures for CHR.
Banff classification was revised and “CAN” was eliminated in 2005, in which the new category, chronic active antibodymediated rejection (CAAMR) was introduced as a novel definition of conventional CHR [2]. CAAMR was featured as IF/TA with transplant glomerulopathy (GBM duplication, increased mesangial matrix), loss of peritubular capillary (PTC), multilamination of PTC basement membrane (BM) and arterial intimal fibrosis in addition to C4d deposition and circulating donor-specific antibody (DSA) positivity.
Although the elimination of “CAN” and the introduction of CAAMR should be appreciated, there is still room for consideration on the newly prescribed criteria of CAAMR. The detection of circulating DSA belongs to just clinical entity. The detection of C4d deposits does not always mean the activation of the whole process of the classical pathway of complement cascades leading to the production of membrane attack complex (MAC, 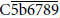 ), a terminal product of complement cascades which leads to cell lysis by cylindrical pore formation in cell membranes, but it means the degradation of
), a terminal product of complement cascades which leads to cell lysis by cylindrical pore formation in cell membranes, but it means the degradation of 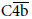 into C4c and C4d by C4b inactivator (C4b-binding protein, C4BP) following the activation of initial process of complement cascades, C1r,Þq,s,
into C4c and C4d by C4b inactivator (C4b-binding protein, C4BP) following the activation of initial process of complement cascades, C1r,Þq,s, 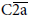 and
and 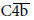 [3]. Additionally in case of ABO-incompatible kidney transplantation, C4d deposition is almost always detected and shows no harmful effect [4]. It was reported that the detection of C4d in the absence of C3d may represent effective complement regulation [5], suggesting that this activation was well regulated and did not proceed to the level of C3 cleavage [6]. When C4b is not cleaved and not inactivated, C3 is split into C3a and C3b by C3 convertase (
[3]. Additionally in case of ABO-incompatible kidney transplantation, C4d deposition is almost always detected and shows no harmful effect [4]. It was reported that the detection of C4d in the absence of C3d may represent effective complement regulation [5], suggesting that this activation was well regulated and did not proceed to the level of C3 cleavage [6]. When C4b is not cleaved and not inactivated, C3 is split into C3a and C3b by C3 convertase (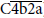 ) and following the inactivation of C3b (iC3b) by C3b inhibitor, iC3b is degraded to C3c and C3d by C3b inhibitor, so that both C4d and C3d detection suggest that the process of classical pathway of complement cascade has proceeded at least to C3 activation by C3 convertase (
) and following the inactivation of C3b (iC3b) by C3b inhibitor, iC3b is degraded to C3c and C3d by C3b inhibitor, so that both C4d and C3d detection suggest that the process of classical pathway of complement cascade has proceeded at least to C3 activation by C3 convertase (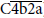 ). Thus, C3d may be more specific than C4d as a marker of complement activation and antibody-mediated rejection [5,7]. Moreover both C4d and C3d detection are considered to be more confirmative. However C3d detection merely means that the complement activation proceeds to the level of C3 activation followed by C3b inactivation and its cleavage into C3c and C3d.
). Thus, C3d may be more specific than C4d as a marker of complement activation and antibody-mediated rejection [5,7]. Moreover both C4d and C3d detection are considered to be more confirmative. However C3d detection merely means that the complement activation proceeds to the level of C3 activation followed by C3b inactivation and its cleavage into C3c and C3d.
This doesn't necessarily deny the efforts and contributions achieved by Banff meetings. In fact the standardization of graft pathology criteria contributed tremendously to the improvement in outcomes of organ transplantation and no one can deny it, on the contrary we all should appreciate their achievement. That’s exactly why the further revise of Banff criteria is required, isn’t that?
References
- Solez K, Axelsen RA, Benediktsson H, Burdick JF, Cohen AH, et al. (1993) International standardization of criteria for the histologic diagnosis of renal allograft rejection: The Banff working classification of kidney transplant pathology. Kidney Int 44: 411-22.
- Solez K, Colvin RB, Racusen LC, Sis B, Halloran PF, et al. (2007) Banff '05 meeting report: Differential diagnosis of chronic allograft injury and elimination of chronic allograft nephropathy (‘CAN’). Am J Transplant 7: 518-26.
- Blom AM, Villoutreix BO, Dahlback B (2004) Complement inhibitor C4b-binding protein-friend or foe in the innate immune system? Molecular immunology 40: 1333-1346.
- Haas M (2010) The significance of C4d staining with minimal histologic abnormalities. Curr Opin Organ Transplant 15: 21-27.
- Stites E, Le Quintrec M, Thurman JM (2015) The Complement System and Antibody-Mediated Transplant Rejection. J Immunol 195: 5525-5531.
- Brandon Renner, Derek Strassheim, Claudia R. Amura, Liudmila Kulik, Danica Ljubanovic, et al. (2010) B cell subsets contribute to renal injury and renal protection after ischemia/reperfusion. J Immunol 185: 4393-4400.
- Haas M, Rahman MH, Racusen LC, Kraus ES, Bagnasco SM, et al. (2006) C4d and C3d staining in biopsies of ABO- and HLA-incompatible renal allografts: correlation with histologic findings. Am J Transplant 6:1829-1840.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi