Case Report, Jor Vol: 10 Issue: 4
New Onset Post-COVID-19 Tinnitus in a Young, Otherwise Healthy Male: Case Report
Angela Alnemri*, Tory McKnight and Dennis Fitzgerald
Department of Otolaryngology–Head and Neck Surgery, Thomas Jefferson University, Philadelphia, PA, USA
*Corresponding Author: Angela A
Department of Otolaryngology Head and Neck
Surgery, Thomas Jefferson University, Philadelphia, USA
Tel: 215-955-6760
E-mail: aea008@jefferson.edu
Received date: March 10, 2021; Accepted date: March 24, 2021; Published date: March 31, 2021
Citation: Angela Alnemri, Tory McKnight, and Dennis Fitzgerald (2021) New Onset Post-COVID-19 Tinnitus in a Young, Otherwise Healthy Male: Case Report. J Otol Rhinol 10:4.
Abstract
Coronavirus disease 2019 (COVID-19) is an infectious respiratory disease caused by the severe acute respiratory syndrome coronavirus 2 that may have lasting health sequela. While most people infected with COVID-19 have mild respiratory symptoms, there have been reports describing various manifestations of the virus in other organ systems including the neurological system, musculoskeletal system and peripheral nervous system. The impact of COVID-19 on structures of the inner ear is not well-understood.
Keywords: COVID-19; Tinnitus; Healthy male
Introduction
The connection between COVID-19 and acute onset tinnitus is a subject of current research and investigation. Tinnitus and equilibrium disorders (e.g. dizziness, vertigo) have been reported in patients infected with COVID-19. An Italian study of 185 patients diagnosed with COVID-19 across 15 hospitals reported 23.2% incidence of new onset subjective tinnitus, determined by patient-reported questionnaire [1].
Previous studies have also reported exacerbation of pre-existing tinnitus in patients during the COVID-19 pandemic; however, not all patients had COVID-19 suggesting a possible psychosocial source brought on by stress or social isolation. It is well-documented in medical literature that there is an association between tinnitus and psychiatric well-being [2].
There has been one prior case report on a previously healthy patient in Qatar who developed left-sided tinnitus with mild, high-frequency hearing loss following diagnosis with COVID-19. The current understanding of viral-induced tinnitus points to an intracochlear pathology, consistent with the findings of this prior case report [3]. We present a case of a previously healthy, young patient, with no prior history of tinnitus, hearing loss, or psychological disorders, who developed subjective tinnitus immediately following infection with COVID-19.
Case Report
A 30-year-old, previously healthy, white male presented to the Otolaryngology outpatient clinic with bilateral non-pulsatile tinnitus and aural fullness, right greater than left for two weeks. The patient had a history of nasopharyngeal swab-confirmed COVID-19 eight weeks prior. His symptoms during infection included anosmia, dysgeusia, and a maculopapular rash involving the palms and soles. Upon recovery, he experienced sequelae of shortness of breath and dizziness on exertion. While there was no significant personal or family psychiatric history, the patient reported experiencing additional psychosocial stress unrelated to the pandemic, brought on by the death of his partner’s mother. The patient had no prior history of tinnitus or hearing loss and no personal or family history of autoimmune disease. A detailed audiological evaluation was performed.
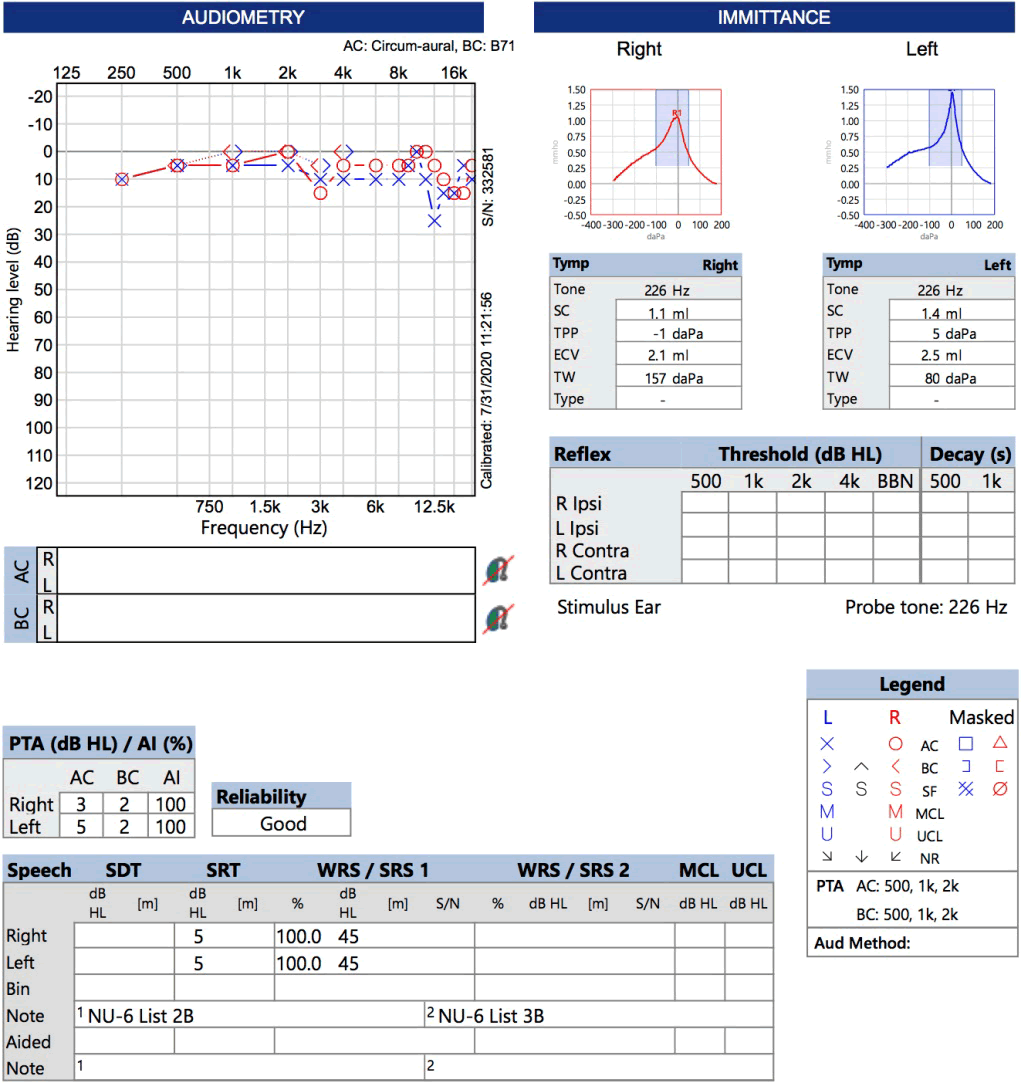
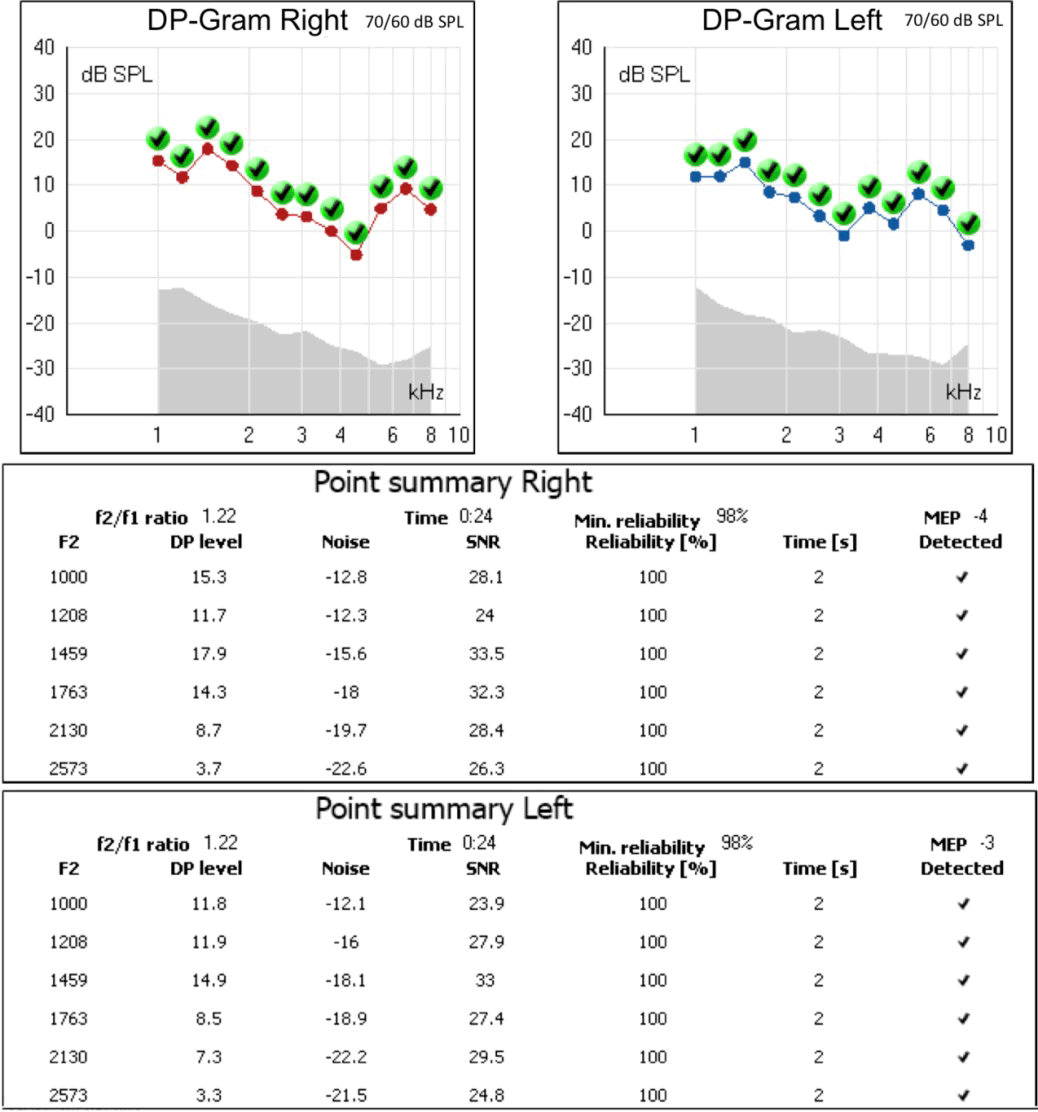
Pure Tone Audiogram (PTA) was carried out in sound booth (Figure 1). Frequencies from 250 Hz to 16 kHz were tested with results revealing normal hearing sensitivity in right and left ears. Speech recognition was 100% in both ears. Ultra-High-Frequency [UHF] testing showed normal results in right (UHF 0-15 dB HL) and left (UHF 0-25 dB HL) ears. Impedance audiometry revealed bilateral A type tympanogram. Pass Distortion Product Otoacoustic Emissions (DPOAEs) were consistent with the pure tone testing (Figure 2).
Figure 1: Results of tympanometry show bilateral Type A tympanometry. The right ear (AD) shows passed DPOAEs and normal hearing with excellent WRS and UHF of 0-15 dB HL. The left ear (AS) shows passed DPOAEs and normal hearing with excellent WRS and UHF of 0-25 dB HL. PTA: Pure Tone Audiometry; AD: right ear; AS: left ear; DPOAE: Distortion Product Otoacoustic Emissions; WRS: Word Recognition Score; UHF: Ultra-High Frequency.
As there was no apparent etiology for the new-onset tinnitus by audiologic evaluation, the treatment plan included a sound machine for sleeping. The patient has had no follow up visits with the Otolaryngology clinic since the first encounter, but on record review, he has been experiencing multiple post-COVID-19 sequelae including bilateral distal extremity paresthesia and a maculopapular rash on the palms and soles. These issues were brought to the attention of rheumatology and neurology, who suspected a possible autoimmune or immune complex deposition disease secondary to COVID-19; however, the workup to date has been negative.
Discussion
The timeline for this patient's tinnitus onset invites questions regarding its relevance to his COVID-19 infection. Intracochlear damage secondary to a viral infection should be reflected in his audiometry findings, particularly as reduced amplitude in DPOAE; however, this patient had normal DPOAE, and no audiometric evidence for tinnitus. Patients with constant tinnitus almost invariably have pure tone hearing loss, but this patient had normal pure-tone findings [3].
While auditory system damage secondary to viral infections is typically intracochlear, it can also affect the auditory brainstem. Intracochlear damage can include damage to the organ of Corti, stria vascularis, spiral ganglion, and include damage induced by the patient's own immune system, as seen in cytomegalovirus, measles, and in HIV-positive patients [4].
This case is unique due to the complex interplay between psychosocial distress and COVID-19 infection in the face of normal hearing. As the workup to date has been negative, the patient's life-stressors could have contributed to his new-onset tinnitus. However, his subsequent neurological and rheumatologic symptoms are concerning for a more complex etiology. Perhaps there was a central nervous system basis for the new-onset tinnitus that would relate to his recent development of a peripheral neuropathy. Further studies or case reports are needed to strengthen the cause-and-effect relationship between COVID-19 and tinnitus [5,6].
Conclusion
In summary, we present the first reported case in the United States of tinnitus occurring in a previously healthy young patient following infection with COVID-19. Ultimately, this case stresses the importance of a detailed work-up in patients experiencing post- COVID-19 symptoms, which should include referral to ENT and an audiometric examination in those presenting with otologic complaints.
References
- Viola P, Ralli M, Pisani D, Malanga D, Sculco D, et al. (2020) Tinnitus and equilibrium disorders in COVID-19 patients: preliminary results. Eur Arch Otorhinolaryngol 23: 1-6.
- Beukes EW, Baguley DM, Jacquemin L, Lourenco MPCG, Allen PM, et al. (2020) Changes in tinnitus experiences during the COVID-19 pandemic. Front Public Health 8: 592878.
- Chirakkal P, Al Hail AN, Zada N, Vijayakumar DS (2021) COVID-19 and tinnitus. Ear Nose Throat J 100: 160S-162S.
- Abramovich S, Prasher DK (1986) Electrocochleography and brain-stem potentials in Ramsay Hunt syndrome. Arch Otolaryngol Head Neck Surg 112: 925-928.
- McCormack A, Jones ME, Sarah S, Hall D (2016) A systematic review of the reporting of tinnitus prevalence and severity. Hear Res 337: 70-79.
- Xiong B, Liu Z, Liu Q, Peng Y, Wu H, et al. (2019) Missed hearing loss in tinnitus patients with normal audiograms. Hear Res 384: 107826.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi