Case Report, Med Microbiol Rep Vol: 1 Issue: 1
Osteomyelitis of the Middle Distal Phalanx Caused by Arcanobacterium haemolyticum in an Adolescent Nail Biter
Sarah Becker, Tornia Wyllie, Maria Novo, Tarik Zahouani*, Shawn Lyo , Evelyn Erickson and Yekaterina Sitnitskaya
Department of Paediatrics, Lincoln Medical and Mental Health Center
*Corresponding Author : Zahouani T, MD
Department of Pediatrics, Lincoln Medical and Mental Health Center, 234E, 149 St. Bronx, NY 10451, USA
Tel: 718-579-5030
E-mail: tarikzahouani@gmail.com
Received: May 15, 2017 Accepted: June 15, 2017 Published: June 20, 2017
Citation: Becker S, Wyllie T, Novo M, Zahouani T, Sean L, et al. (2017) Osteomyelitis of the Middle Distal Phalanx Caused by Arcanobacterium haemolyticum in an Adolescent Nail Biter. Med Microbiol Rep 1:1.
Abstract
Human bites are the third leading cause of bite injuries leading to emergency room visits. Osteomyelitis is a dreaded complication of soft tissue infection contiguous to osseous structures and numerous cases of osteomyelitis due to human bites have been reported. Arcanobacterium haemolyticum is a known cause of pharyngitis in adolescents. We report a case of a 12 year old male with nail biting behavior who presented with cellulitis/abscess of the 3rd digit with MRI showing osteomyelitis and wound culture positive for Arcanobacterium haemolyticum. MRI should be considered in the evaluation of deep soft tissue infection of the finger.
Keywords: Osteomyelitis
Introduction
Human bites are the third leading cause of bite injuries leading to Emergency Room (ER) visits. While these lesions are less often penetrating, as compared to dog or cat bites, they have been associated with greater morbidity and more frequent complications [1]. Contiguous osteomyelitis secondary to soft tissue infection after human bites have been reported [2-4]. One multicenter prospective study showed that Streptococcus and Staphylococcus species, followed by Prevotella, Fusobacterium and Eikenella corrodens, were the predominant species isolated from wound cultures from infected human bites [5].
Arcanobacterium haemolyticum (A. haemolyticum) is an unusual cause of non-streptococcal bacterial pharyngitis in adolescents [6]. It has rarely been isolated from soft tissue and other sterile sites. However, it has not been previously isolated from infected human bite. Here we report the case of a 12 year old autistic boy with a habit of compulsive nail biting behavior, who developed cellulitis/abscess of the 3rd digit with associated underlying osteomyelitis of the adjacent bone caused by A. haemolyticum.
Case Presentation
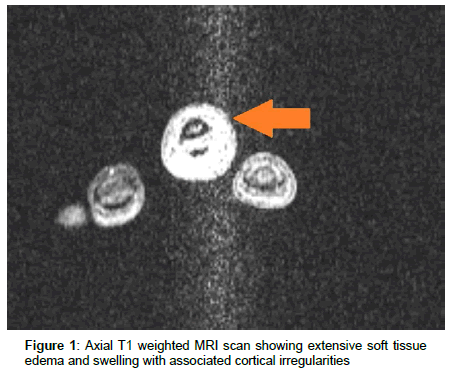
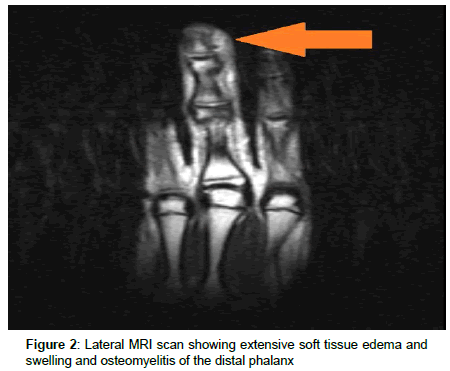
A 12 year old male with Autistic Spectrum Disorder (ASD) and habitual onychophagia presented with erythema, edema and pain in the left middle finger of 4 days duration. He had no fever, and was noted to have redness, swelling and abundant purulent discharge from the lateral aspect of the distal phalanx of the left middle finger. There was a decreased range of motion in the distal interphalangeal joint of the same finger. The WBC count was 15.5×109/mL and Procalcitonin was <0.05 ng/mL. Because of close proximity of the underlying bone, MRI was performed to rule out osteomyelitis by continuation. The imaging showed soft tissue edema and swelling with associated cortical irregularities in the distal phalanx (Figures 1 and 2). The wound culture grew A. haemolyticum. The wound was debrided. The patient was treated with IV ampicillin-sulbactam and clindamycin for 5 days. Three weeks of treatment were completed with oral clindamycin, in accordance with reported sensitivity of the causative organism. At the follow up examination one month later, there was full resolution of symptoms and signs.
Discussion
We report a case of osteomyelitis caused by A. haemolyticum, which had its probable origin in the oropharynx of a patient with no manifestations of pharyngitis. Infection inoculated through onychophagia is expected to have the same etiology as infection due to human bite, and to be caused by oral commensals [5]. A. haemolyticum is a rare cause of pharyngitis with extremely rarely reported systemic complications from sepsis to focal infection including osteomyelitis [6-11]. However, we found only one previous report of A. haemolyticum causing infection due to a bite (inflicted by a dog) [12]. Nevertheless, it makes sense that oropharyngeal bacteria may be inoculated into human bite wound. A. haemolyticum isolates are susceptible to penicillins, macrolides and Clindamycin [13,14]. Our initial choice of treatment included Ampicillin-Sulbactam and Clindamycin (for staphylococcal coverage) which resulted in prompt improvement.
A. haemolyticum rarely causes soft tissue infections, usually in old and/or immunocompromised individuals [8,11]. We believe that this is the first report of soft tissue infection in an immune competent pediatric patient. Furthermore, this case is unique because there was a complication of involvement of the underlying bone.
Osteomyelitis by continuation is a rare complication of human bite. On physical exam, it is not possible to determine whether cellulitis or abscess in the digit has extension to the bone, which is also extremely rare [9,10]. In contiguous osteomyelitis, fever usually is absent, and WBC count and inflammatory markers like CRP and Procalcitonin are more often normal rather than elevated. Our patient had no fever, his WBC count was only mildly elevated and procalcitonin was normal. All these findings do not exclude a diagnosis of underlying osteomyelitis. If MRI was not performed in this case, there would have been no recognition for the necessity of long antibiotic treatment because of the presence of osteomyelitis.
Conclusion
We have demonstrated that infection of distal finger secondary to onychophagia might be associated with extension to the underlying bone, and be caused by A. haemolyticum. MRI should be considered in the evaluation of deep soft tissue infection of the finger. In our case, empiric treatment with Ampicillin-Sulbactam and Clindamycin achieved prompt clinical resolution of the infection.
References
- Griego RD, Rosen T, Orengo IF, Wolf JE (1995) Dog, cat, and human bites: A review. J Am Acad Dermatol 33: 1019-1029.
- Gonzalez MH, P Papierski, RF Hall (1993) Osteomyelitis of the hand after a human bite. J Hand Surg Am 18: 520-522.
- Zahouani T, Lopez C, Burdea L, LaCruz AD, Polonio P, et al. (2016) Osteomyelitis of the fifth toe after human bite. Am J Med Case Rep 4: 346-348.
- Resnick D, Pineda CJ, Weisman MH, Kerr R (1985) Osteomyelitis and septic arthritis of the hand following human bites. Skeletal Radiol 14: 263-266.
- Talan DA, Abrahamian FM, Moran GJ, Citron DM, Tan JO, et al. (2003) Clinical presentation and bacteriologic analysis of infected human bites in patients presenting to emergency departments. Clin Infect Dis 37: 1481-1489.
- Mackenzie A, Fuite L A, Chan F T, King J, Allen U, et al. (1995) Incidence and pathogenicity of Arcanobacterium haemolyticum during a 2-year study in Ottawa. Clin Infect Dis21: 177-181.
- Gaston DA, Zurowski SM (1996) Arcanobacterium haemolyticum Pharyngitis and Exanthem. Three Case Reports and Literature Review. Arch Dermatol 132: 61-64.
- Kavitha K, Latha R, Udayashankar C, Jayanthi K, Oudeacoumar P, et al. (2010) Three cases of Arcanobacterium pyogenes-associated soft tissue infection. J Med Microbiol59: 736-739.
- Thean YT, Siew YN, Thomas H, Chan BK (2006) Archanobacterium haemolyticum bacteremia and soft tissue infections: Case report and review of literature. J Infect 53: 69-74.
- Therriault BL, Daniels LM, Carter YL, Raasch RH (2008) Severe sepsis caused by Arcanobacterium haemolyticum: a case report and review of the literature. Ann Pharmacother 42: 1697-702.
- Dobinsky S, Noesselt T, Rucker A, Maerker J, Mack D (1999) Three cases of Arcanobacterium haemolyticum associated with abscess formation and cellulitis. Eur J Clin Microbiol Infect Dis 18: 804-806
- Lee S, Roh KH, Kim CK, Chong Y et al. (2008) A Case of Necrotizing Fasciitis Due to Streptococcus agalactiae, Arcanobacterium haemolyticum, and Finegoldia magna in a Dog-bitten Patient with Diabetes. Korean J Lab Med 28: 191-195.
- Skov RL, Sanden AK, Danchell VH, Robertsen K, Ejlertsen T (1998) Systemic and deep-seated infections caused by Arcanobacterium haemolyticum. Eur J Clin Microbiol Infect Dis 17: 578-582.
- Linder R (1997) Rhodococcus equi and Arcanobacterium haemolyticum: two "coryneform" bacteria increasingly recognized as agents of human infection. Emerg Infect Dis 3: 145-153.
 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi